Abstract
There is evidence that fetal growth restriction is associated with impaired nephrogenesis and reduced numbers of mature nephrons at birth. It has been proposed that such impairment of renal growth may contribute to increased blood pressure in later life. Although prostaglandins (PG) play a key role in kidney development, it is unknown whether a poor fetal substrate supply alters the synthesis or actions of PG within the fetal kidney. Using real-time reverse transcriptase PCR, we have measured the effect of chronic placental restriction (PR) on the renal expression of PG endoperoxide G/H synthase-2 (PGHS-2), PGE2 receptors EP2 and EP4, and renin mRNA in the sheep fetus in late gestation. Restriction of placental growth reduced fetal body weight (PR: 3.2 ± 0.2 kg, control: 4.8 ± 0.2 kg) and total kidney weight (PR: 19.7 ± 1.8 g, control: 25.1 ± 1.3 g). Mean fetal arterial Po2 was reduced by PR (PR: 15.03 ± 0.67 mm Hg, control: 21.3 ± 0.87 mm Hg). Renal PGHS-2 mRNA was increased in the PR group (PR: 2.26 ± 0.38, control: 1.20 ± 0.31) and was inversely related to mean fetal arterial Po2 in the PR and control groups [PGHS-2: −0.17 (Po2) + 4.69, r2 = 0.26]. PR also increased renal EP2 (PR: 1.57 + 0.24, control: 0.82 + 0.13) but not EP4 mRNA. Renin mRNA was directly related to renal EP2 [renin = 0.37 (EP2) + 0.97, r2 = 0.29] and EP4, [renin = 0.75 (EP4) + 0.44, r2 = 0.38] mRNA expression. Thus, the restriction of placental growth and associated chronic hypoxemia appear to increase the renal capacity to synthesize and respond to PG, which may play an important role in maintaining renin mRNA expression in the growth-restricted fetus.
Similar content being viewed by others
Main
A worldwide series of epidemiologic studies has demonstrated that low birth weight is associated with an increased risk of hypertension and cardiovascular disease in later life (1–3). The associations between low birth weight and poor adult health outcomes have been articulated in the “fetal origins of adult disease hypothesis.” This hypothesis states that the physiologic adaptations that enable the fetus to survive a period of intrauterine deprivation result in a permanent reprogramming of the development of key organ systems and pathologic consequences in adult life (3, 4). There is evidence that fetal growth restriction is associated with impaired nephrogenesis and reduced numbers of mature nephrons (5–7). It has been proposed that such impairment of renal growth may contribute to increased blood pressure in later life (5–7). The mechanisms by which a poor fetal substrate supply alters renal growth and development are, however, poorly understood.
There is clear evidence that prostaglandins, in particular those produced by the prostaglandin synthetic enzyme, prostaglandin endoperoxide synthase-2 (PGHS-2), are essential for normal renal development and function (8–15). In mice with a null mutation of the gene for PGHS-2, there is a severe reduction in the number of functional nephrons developed in the fetal kidney (9). Administration of indomethacin, an inhibitor of prostaglandin synthesis, to women in threatened preterm labor also results in abnormalities in glomerular and tubular morphology in the fetal kidney and a loss of fetal and neonatal urine production (10, 11). Similarly, chronic suppression of prostaglandin synthesis in the pregnant Rhesus monkey during late gestation resulted in fetal renal dysgenesis (13). Although prostaglandins play a key role in the growth and development of the fetal kidney, it is unknown whether poor fetal substrate supply results in an alteration in the synthesis or actions of prostaglandins, mediated through their specific receptor subtypes in the fetal kidney.
There is evidence that the expression of PGHS-2 is developmentally regulated in the fetal kidney, and intense PGHS-2 expression has been localized to a subset of thick ascending limb cells near the macula densa during nephrogenesis in the rat kidney (16). Although all biologically active prostaglandins are produced through further enzymatic modification of PGHS metabolites, prostaglandin E2 (PGE2) has been identified as the major renal prostaglandin produced in the fetal sheep kidney during late gestation (17). There is evidence that PGE2, acting via either the EP2 or EP4 receptor subtype, increases renin synthesis and secretion in the adult kidney (18). Renin mRNA levels are high in the fetal sheep kidney (19), and activity of the renin angiotensin system is essential for normal growth (20) and function (21) of the kidney in utero. There is some evidence that prostaglandins may increase renin secretion in the fetal kidney (14, 15), and one preliminary report has indicated that EP4 mRNA is expressed in the kidney of the late gestation fetal sheep (22). There is no information, however, on whether the EP2 receptor subtype is expressed in the developing kidney, whether restriction of fetal growth is associated with a change in the renal expression of PGHS-2 or the EP2 or EP4 receptor subtype, or whether the expression of either receptor subtype is related to renin expression.
In the present study, we hypothesized that restriction of placental and, hence, fetal growth may decrease mRNA levels of PGHS-2, EP2, and EP4 in the kidney of the fetal sheep during late gestation. We also postulated that any changes in PGHS-2 and EP2 and EP4 receptor subtype expression would be directly related to changes in renal renin expression in the growth-restricted sheep fetus.
METHODS
Animals and surgery.
All procedures were approved by the Adelaide University Animal Ethics Committee. In 12 Merino ewes, the majority of endometrial caruncles were surgically removed from the uterus before mating to restrict subsequent placental cotyledon formation, restricting placental and, hence, fetal growth, as described previously (23). Ewes were observed for 4–7 d postsurgery, and were allowed at least 10 wk recovery after surgery before mating. Pregnancy was confirmed by ultrasound at approximately 60 d gestation. In 12 placentally restricted (PR) ewes, and seven control ewes, vascular catheters filled with 50 IU/mL heparinized saline were inserted into both a fetal and maternal carotid artery and jugular vein between 102 and 120 d gestation. All surgical procedures were performed under general anesthesia induced with an injection of sodium thiopentone (25 g i.v., Boehringer Ingelheim, North Ryde, NSW, Australia), and maintained with 3–4% inhalational halothane in oxygen. Fetal catheters were exteriorized through an incision in the ewe's flank. During surgery, antibiotics (penicillin, 250 mg/mL, and procaine hydrochloride 20 mg/mL, Lyppards, Adelaide, Australia) were administered intramuscularly to the ewe (2 mL) and fetus (2 mL), respectively. Ewes were housed in individual pens within animal holding rooms, with a 12-h light-dark cycle. Water was available ad libitum, and ewes were fed once daily.
A recovery period of at least 4 d was allowed after surgery before blood sampling commenced. Fetal arterial blood samples (0.5 mL) were taken three times per week, and Po2, Pco2, pH, O2 saturation, and Hb content were determined (ABL 520 analyzer, Radiometer, Copenhagen, Denmark).
Postmortem and tissue collection.
In addition to the pregnant ewes described above, two pregnant ewes carrying normally grown singleton fetuses that did not undergo surgery were also used for collection of fetal tissues. Ewes and fetuses were killed with an overdose of sodium pentobarbitone (Lyppards, Castle Hill, NSW, Australia) between 139 and 145 d gestation. Fetal sheep were delivered by hysterectomy, weighed, and decapitated. Fetal kidneys were weighed and a mid-glandular section of one kidney was collected from each fetus. These samples were snap frozen in liquid nitrogen and stored at −80°C.
Real-time reverse transcriptase (RT)-PCR.
To ensure that the relative contribution of renal cortical and medullary RNA to the whole kidney RNA sample examined was equal, total RNA was extracted from 50 to 100 mg of each tissue using Tri-Reagent (Sigma Chemical, St. Louis, MO, U.S.A.), as described previously (24). Extracted RNA was resuspended in Tris-EDTA buffer (TE: 10 mM Tris, 1 mM EDTA, pH 7.4), and the RNA concentrations determined by spectrophotometry. Renal cortical and medullary RNA from each kidney were then combined in equal proportions, treated twice with DNase I (Ambion DNA-free, Ambion, Austin, TX, U.S.A.), and RNA concentration determined by spectrophotometry. Primers for each gene (Table 1) were designed with the assistance of Primer Premier 5.0 Software (Premier Biosoft International, Palo Alto, CA, U.S.A.) and were optimized for annealing temperature (64–70°C) and RT RNA concentration. Correct product size and sequence were confirmed by agarose gel electrophoresis and sequencing.
RNA (500 ng) was reverse transcribed using the TaqMan RT Reagents kit (Applied Biosystems, Foster City, CA, U.S.A.), containing 1× RT buffer (TaqMan RT buffer), 5.5 mM MgCl2, 500 μM of each deoxyNTP, 2.5 μM random primers, 0.4 U/μL RNase inhibitor, and 1.25 U/μ RT (MultiScribe). Control mixtures were prepared for each RNA sample containing no RT and a no-template control also included. A six-point standard curve was constructed by serial dilution of an RNA sample from one control animal and was reverse transcribed in parallel with the experimental samples. The RT thermal cycle was conducted using the Bio-Rad iCycler (Bio-Rad, Hercules, CA, U.S.A.) as follows: 25°C (10 min), 48°C (30 min), then 95°C (5 min) before freezing at −20°C.
PCR reaction mixtures (50 μL) were prepared containing 1× SYBR Green buffer, 3 mM MgCl2, 1 mM dNTP mix with dUTP substituted for dTTP, 0.025 U/μL Taq polymerase (AmpliTaq Ddd), 0.01 U/μL Uracil N Glycosylase (Amp Erase UNG), 0.2 μM sense primer, 0.2 μM antisense primer, and 2 μL cDNA using the SYBR Green PCR Core Reagents kit (PE Biosystems, Warrington, U.K.). Aliquots (3 × 50 μL) of each cDNA sample were transferred to a 96-well optical plate (iCycler iQ PCR plates, Bio-Rad). Wells were sealed using optical grade tape (iCycler iQ, Bio-Rad), and the plate centrifuged briefly. Fluorescence measurements for each experimental run were standardized either using the experimental plate or an external well factor plate. The thermal cycle protocol used for amplification, using the Bio-Rad iCycler, was as follows: 50°C (2 min), 95°C (10 min), and 40 × 95°C (15 s), 70°C (60 s), or appropriate annealing temperature (30 s) followed by 72°C (30 s). Sample fluorescence was measured each cycle during either the 70°C or 72°C step. Melt curve data were then collected immediately, using the thermal protocol 95°C (1 min), 55°C (1 min), and then fluorescence was measured as sample temperature was increased by 1°C increments every 12 s.
Data analysis.
After the PCR run was completed, melt curve analysis was used to confirm that there was one amplified product. Baseline fluorescence was determined, and a threshold value assigned at 10 SD above the mean baseline fluorescence. This was used to assign a threshold cycle (TC) for each well. The mean TC was then calculated for each sample in triplicate. A maximum variation between the TC measurements of the three aliquots was set at 0.6 TC, and data points outside this value were excluded from further analysis. The difference in the mean abundance of renal 18S rRNA between the PR and control groups was 0.3 TC, and 18S rRNA was therefore used as the reference gene. The ratio of target gene mRNA abundance, relative to 18S rRNA abundance, was determined using a modification of the data analysis method recently developed, and validated for real-time PCR measurement of relative gene expression (25). The PCR reaction efficiency for each primer set was determined from the slope of the standard curve. The mean relative gene mRNA expression for each group was then determined:
MATH
where Etarget = the real-time PCR reaction efficiency of the gene of interest, and E18S = the real-time PCR reaction efficiency of 18S, which were calculated as E = 10[−1/slope of standard curve] for each reaction. ΔTC = the difference in mean TC between a control sample on the plate and each experimental sample on that plate. The control sample was one sample of renal cDNA included in all PCR runs.

A mean arterial blood gas value was calculated for each fetus from all of the blood gas data collected for that fetus during late gestation. Data are expressed as mean ± SEM, and results from the PR and control groups were compared using a t test and linear regression analysis. A probability level of 5% (p ≤ 0.05) was considered significant.
RESULTS
Fetal Blood Gas Status and Outcomes
Mean fetal arterial Po2 and O2 saturation were significantly lower in the PR group when compared with controls. There was no difference, however, in mean fetal arterial Hb content, Pco2, or pH between the PR and control fetuses (Table 2). Placental restriction significantly reduced fetal body weight (PR: 3.2 ± 0.2 kg, n = 12; control: 4.8 ± 0.2 kg, n = 9, p < 0.001) and fetal kidney weight (PR: 19.7 ± 1.8 g, control: 25.1 ± 1.3 g, p = 0.04), whereas the proportion of kidney weight to body weight was unaltered (PR: 0.62 ± 0.05%, control: 0.53 ± 0.03%, p > 0.05).
Renal PGHS-2 mRNA Expression
The relative expression of PGHS-2 mRNA.
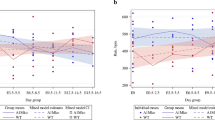
In the fetal kidney, 18S rRNA was significantly greater in the PR group (PR: 2.26 ± 0.38, control: 1.20 ± 0.31, p = 0.05) (Fig. 1A). There was also an inverse relationship between the relative expression of PGHS-2 mRNA in the fetal kidney and the mean fetal arterial Po2 during late gestation [PGHS-2 = −0.17 (Po2) + 4.69, r2 = 0.26, p = 0.03] (Fig. 1B).
(A) The renal expression of PGHS-2 mRNA/18S rRNA in PR fetal sheep (filled bar, n = 12) compared with control (open bar, n = 9) fetal sheep at 139–145 d gestation (p = 0.05). Data are shown as mean ± SEM. *Significant difference (p ≤ 0.05) between the PR and control groups. (B) The relative expression of PGHS-2 mRNA/18S rRNA is inversely related to the mean fetal arterial Po2 throughout late gestation [PGHS-2 = −0.17 (Po2) + 4.69, r2 = 0.26, p = 0.03] in the PR (filled circles, n = 12) and control (open circles, n = 7) groups combined.
Renal EP2 and EP4 receptor mRNA expression.
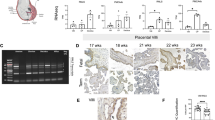
The expression of EP2 receptor mRNA was significantly greater in the PR group (PR: 1.57 ± 0.24, control: 0.82 ± 0.13, p = 0.02) (Fig. 2A). There was a trend for an inverse relationship between the relative renal expression of EP2 mRNA and the mean arterial Po2 throughout late gestation (p = 0.06). The restriction of placental growth did not alter the renal expression of EP4 receptor mRNA (PR: 1.81 ± 0.23, control: 1.29 ± 0.27, p > 0.05) (Fig. 2B), and there was no relationship between renal EP4 mRNA expression and mean fetal arterial Po2.
(A) The renal expression of EP2 mRNA/18S rRNA in PR fetal sheep (filled bar, n = 12) compared with control (open bar, n = 9) fetal sheep at 139–145 d gestation (p = 0.02). Data are shown as mean ± SEM. *Significant difference (p ≤ 0.05) between the PR and control groups. (B) Renal expression of EP4 mRNA/18S rRNA in PR (filled bar, n = 12) and control (open bar, n = 9) fetal sheep at 139–145 d gestation (p > 0.05). Data are shown as mean ± SEM.
Renal renin mRNA expression.
There was no difference between the PR and control groups in the expression of renin mRNA in the fetal kidney (PR 1.56 + 0.20, control: 1.23 + 0.21, p > 0.05). Renal renin mRNA expression was not correlated with fetal mean arterial Po2. There were, however, significant positive relationships between the relative expression of renin mRNA and EP2 mRNA [renin = 0.37 (EP2) + 0.97, r2 = 0.29, p = 0.05] (Fig. 3A) and EP4 mRNA [renin = 0.75 (EP4) + 0.44, r2 = 0.38, p = 0.02] (Fig. 3B). There was also a trend for a direct relationship between relative renin mRNA expression and the expression of PGHS-2 mRNA (p = 0.09).
(A) There is a significant relationship between EP2 mRNA/18S rRNA expression and renin mRNA/18S rRNA expression in the PR (filled circles, n = 9) and control (open circles, n = 5) groups at 139–145 d gestation [renin = 0.37 (EP2) + 0.97, r2 = 0.29, p = 0.05]. (B) There is a significant relationship between EP4 mRNA/18S rRNA expression and renin mRNA/18S rRNA expression in the PR (filled circles, n = 9) and control (open circles, n = 5) groups combined [renin = 0.75 (EP4) + 0.44, r2 = 0.38, p = 0.02].
DISCUSSION
The restriction of placental growth reduced mean fetal arterial Po2, O2 saturation, fetal body weight, and total kidney mass. There was no change, however, in the proportion of kidney mass to body weight, indicating that the growth of the kidney was restricted in proportion to body size in the PR animals. PGHS-2 mRNA expression was increased in the PR fetus, and was inversely related to mean fetal arterial Po2. In addition to the increased expression of mRNA for this prostaglandin synthetic enzyme, there was also an increase in expression of mRNA for the PGE2 receptor, EP2, whereas there was no change in the expression of mRNA for either the EP4 receptor or renin in the kidney of the placentally restricted fetus. Renin mRNA expression was directly related to the expression of EP2 and EP4 mRNA. It has previously been demonstrated that an up-regulation of EP2 receptor mRNA in rat glomeruli, after induction of mesangioproliferative glomerulonephritis, is correlated with both an increase in receptor protein and an increase in cAMP production in response to PGE2(26). Our results therefore indicate that there may be an increase in the capacity of the kidney in the growth-restricted fetus to synthesize and respond to prostaglandins. It is possible that this response is an important fetal adaptation to placental restriction, acting to maintain proportionate renal growth.
Our results demonstrated that the relative renal expression of PGHS-2 mRNA increased in response to placental restriction, and was inversely related to mean arterial Po2 during late gestation. The inverse relationship between PGHS-2 mRNA and mean arterial Po2 suggests that hypoxia may directly stimulate PGHS-2 expression in the fetal sheep kidney. There is evidence that prostaglandins play a role in the fetal renal response to hypoxia in vivo. Millard et al. (27) reported that administration of indomethacin to fetal sheep caused a significantly greater decrease in renal blood flow when fetal hypoxia was induced. Interestingly, Bauer et al. (28) demonstrated that in growth-restricted newborn piglets, the decrease in renal blood flow in response to severe hypoxia was smaller when compared with normally grown newborns, suggesting that adaptations in the growth-restricted fetal kidney improve its capacity to maintain renal blood flow during hypoxia. Based on data from the present study, it would be pertinent to determine the effects of blockade of the EP2/EP4 receptor subtypes on renal blood flow and renin mRNA expression in the growth-restricted fetus.
Hypoxia has been demonstrated to increase the expression of PGHS-2 mRNA in cultured vascular endothelial cells in vitro(29). This latter study also demonstrated that the mechanism by which hypoxia stimulates increased PGHS-2 mRNA expression includes increased binding of nuclear factor (NF)-κB p65 to one of two NF-κB consensus elements present in the PGHS-2 promoter region (29). There is also the potential for other oxygen-sensing mechanisms, such as hypoxia inducible factor 1 (HIF-1) to contribute to the increased PGHS-2 expression that is induced by hypoxia (30). In cultured adult rat renal mesangial cells, an increase in PGE2 production has been demonstrated in response to severe hypoxia in vitro(23, 31, 32).
Although decreasing oxygen supply may act directly to increase the renal expression of PGHS-2 mRNA, it is possible that other factors, such as circulating glucose or IGF-1 concentrations, which also reflect the severity of growth restriction, influence renal PGHS-2 mRNA expression and contribute to the inverse relationship observed between mean arterial Po2 and PGHS-2 mRNA expression. The expression of other important regulators of fetal renal development, including components of the nitric oxide, or bradykinin pathways, may also be affected when fetal growth is restricted. Changes in the activity of these pathways may mediate or compensate for the effect of growth restriction on the renal prostaglandin system or RAS. Our data suggest that, regardless of the nature of the cellular mechanisms involved, an increase in prostaglandin production in the kidney forms part of the renal response to a restriction in substrate supply.
We have also demonstrated that restriction of placental and fetal growth increased EP2 receptor mRNA expression in the fetal sheep kidney. There was a trend for the increased EP2 mRNA expression to be inversely related to mean fetal arterial Po2 throughout late gestation. This is the first report of EP2 mRNA expression in the fetal kidney, and also the first investigation into the impact of a suboptimal intrauterine environment on the renal expression of the EP2 receptor in fetal development. The role of EP2 in adult renal function is controversial. EP2 is localized in the nephron of the adult rat kidney to the descending thin limb of the loop of Henle, and outer medulla vasa recta (33), and to the renal cortical arteries and arterioles in the human kidney (34). At present, the specific role of the EP2 receptor in the adult or fetal kidney is unclear, although two gene deletion studies have suggested a role for this receptor in the regulation of renal salt reabsorption (35, 36).
In contrast to EP2, we found that EP4 receptor mRNA expression in the fetal sheep kidney was not altered by placental restriction, and there was no relationship between the expression of EP4 mRNA and mean fetal arterial Po2. In the adult, expression of the EP4 receptor has been localized to the renal glomerulus, where it is believed to mediate the stimulatory action of PGE2 on the synthesis and secretion of renin (37). The EP2 and EP4 receptors share several characteristics. Importantly, both bind PGE2 with a similar affinity (38), and both increase intracellular cAMP production (39). It may be of relevance, however, that the EP4 receptor undergoes rapid, agonist-induced desensitization within minutes by being internalized into the cell, whereas the EP2 receptor subtype is only down-regulated by long-term agonist exposure (40). The specific increase in both the enzyme PGHS-2 and EP2 receptor mRNA may therefore represent a requirement for prolonged prostaglandin signaling in the kidney of the growth-restricted fetus.
There was no significant change in the expression of renin mRNA in the kidney in response to placental restriction. This contrasts with the previous findings of Zhang et al. (41), who reported that renin mRNA was reduced in the kidney of placentally restricted fetal sheep. Consistent with the results of Zhang et al., it has been demonstrated that, in the rat, restriction of maternal protein intake during pregnancy suppressed renin mRNA levels in the kidneys of offspring (42). This demonstrates that, in the rat, the renin angiotensin system can be suppressed by protein restriction, in the absence of hypoxemia. Edwards and co-workers (43), however, reported that infusion of an angiotensin-converting enzyme inhibitor, which blocked activity of the renin angiotensin system, resulted in a greater hypotensive response in placentally restricted fetal sheep. These authors concluded that the renin angiotensin system plays a greater role in the maintenance of fetal arterial blood pressure in the PR, compared with the normally grown fetus.
In the present study, we have demonstrated that the relative expression of renin mRNA was directly related to the relative expression of both EP2 and EP4 receptor mRNA. It has been demonstrated that inhibition of prostaglandin synthesis decreases plasma renin activity in late-gestation fetal sheep (14, 15) and prostaglandin-mediated increase in cAMP production is also an established promoter of renin synthesis and secretion in the adult kidney (18, 37). The relationships we observed between renin and the components of the prostaglandin system may therefore suggest that renin mRNA synthesis is indeed regulated, in part, by prostaglandins in the late-gestation fetal sheep.
In summary, our results demonstrated that there is an increase in PGHS-2 mRNA expression in the kidney of the placentally restricted fetal sheep, and that renal PGHS-2 mRNA expression is inversely related to mean fetal arterial Po2. Placental restriction significantly increased EP2 receptor mRNA, and there was also a trend for this increase to be inversely related to mean fetal arterial Po2 during late gestation. Placental restriction did not affect EP4, or renin mRNA expression, however, the relative expression of renin mRNA was directly related to both EP2 and EP4 receptor mRNA expression. Thus, the restriction of placental growth and associated chronic hypoxemia appear to increase the renal capacity to synthesize and respond to prostaglandins, which may play an important role in maintaining renin mRNA expression in the growth-restricted fetus.
References
Barker DJ 1995 Fetal origins of coronary heart disease. BMJ 311: 171–174
Barker D 1998 Mothers, Babies and Health in Later Life. Churchill Livingstone, Edinburgh, Scotland, p 217
Barker DJP 1999 Fetal programming and public health. In: O'Brien PMS, Wheeler T, Barker DJP (eds) Fetal Programming: Influences on Development and Disease in Later Life. RCOG Press, London, pp 3–11
Lucas A 1991 Programming by early nutrition in man. In: Bock GR, Whelen J (eds) The Childhood Environment and Adult Disease. John Wiley & Sons, Chichester, England, pp 38–55
Hinchliffe SA, Lynch MR, Sargent PH, Howard CV, Van Velzen D 1992 The effect of intrauterine growth retardation on the development of renal nephrons. Br J Obstet Gynaecol 99: 296–301
Bassan H, Trejo L, Kariv N, Bassan M, Berger E, Fattal A, Gozes I, Harel S 2000 Experimental intrauterine growth retardation alters renal development. Pediatr Nephrol 15: 192–195
Vehaskari VM, Aviles DH, Manning J 2001 Prenatal programming of adult hypertension in the rat. Kidney Int 59: 238–245
Gleason CA 1987 Prostaglandins and the developing kidney. Semin Perinatol 11: 12–21
Dinchuk JE, Car BD, Focht RJ, Johnston JJ, Jaffee BD, Covington MB, Contel NR, Eng VM, Collins RJ, Czerniak PM 1995 Renal abnormalities and an altered inflammatory response in mice lacking cyclooxygenase II. Nature 378: 406–409
van der Heijden BJ, Carlus C, Narcy F, Bavoux F, Delezoide AL, Gubler MC 1994 Persistent anuria, neonatal death, and renal microcystic lesions after prenatal exposure to indomethacin. Am J Obstet Gynecol 171: 617–623
Kaplan BS, Restaino I, Raval DS, Gottlieb RP, Bernstein J 1994 Renal failure in the neonate associated with in utero exposure to non-steroidal anti-inflammatory agents. Pediatr Nephrol 8: 700–704
Komhoff M, Wang JL, Cheng HF, Langenbach R, McKanna JA, Harris RC, Breyer MD 2000 Cyclooxygenase-2-selective inhibitors impair glomerulogenesis and renal cortical development. Kidney Int 57: 414–422
Novy MJ 1978 Effects of indomethacin on labor, fetal oxygenation, and fetal development in rhesus monkeys. Adv Prostaglandin Thromboxane Res 4: 285–300
Matson JR, Stokes JB, Robillard JE 1981 Effects of inhibition of prostaglandin synthesis on fetal renal function. Kidney Int 20: 621–627
Stevenson KM, Lumbers ER 1992 Effects of indomethacin on fetal renal function, renal and umbilicoplacental blood flow and lung liquid production. J Dev Physiol 17: 257–264
Zhang MZ, Wang JL, Cheng HF, Harris RC, McKanna JA 1997 Cyclooxygenase-2 in rat nephron development. Am J Physiol 273: F994–F1002
Pace-Asciak CR 1977 Prostaglandin biosynthesis and catabolism in the developing fetal sheep kidney. Prostaglandins 13: 661–668
Breyer MD, Harris RC 2001 Cyclooxygenase 2 and the kidney. Curr Opin Nephrol Hypertens 10: 89–98
Zhang DY, Lumbers ER, Simonetta G 1996 Changes in renal renin gene expression in fetal sheep. Clin Exp Pharmacol Physiol 23: 682–684
Tufro-McReddie A, Romano LM, Harris JM, Ferder L, Gomez RA 1995 Angiotensin II regulates nephrogenesis and renal vascular development. Am J Physiol 269: F110–F115
Lumbers ER, Burrell JH, Menzies RI, Stevens AD 1993 The effects of a converting enzyme inhibitor (captopril) and angiotensin II on fetal renal function. Br J Pharmacol 110: 821–827
Takae K, Wu WX, Nathanielsz PW Characterization of developmental changes of prostaglandin (PG) E and F receptor subtypes in the fetal sheep kidney in late gestation. Proceedings of the Society for Gynecologic Investigation, Chicago, IL, pp
Robinson JS, Kingston EJ, Jones CT, Thorburn GD 1979 Studies on experimental growth retardation in sheep. The effect of removal of endometrial caruncles on fetal size and metabolism. J Dev Physiol 1: 379–398
McMillen IC, Warnes KE, Adams MB, Robinson JS, Owens JA, Coulter CL 2000 Impact of restriction of placental and fetal growth on expression of 11beta-hydroxysteroid dehydrogenase type 1 and type 2 messenger ribonucleic acid in the liver, kidney, and adrenal of the sheep fetus. Endocrinology 141: 539–543
Pfaffl MW 2001 A new mathematical model for relative quantification in real-time RT-PCR. Nucleic Acids Res 29: 2002–2007
Hartner A, Pahl A, Brune K, Goppelt-Struebe M 2000 Upregulation of cyclooxygenase-1 and the PGE2 receptor EP2 in rat and human mesangioproliferative glomerulonephritis. Inflamm Res 49: 345–354
Millard RW, Baig H, Vatner SF 1979 Prostaglandin control of the renal circulation in response to hypoxemia in the fetal lamb in utero. Circ Res 45: 172–179
Bauer R, Walter B, Zwiener U 2000 Effect of severe normocapnic hypoxia on renal function in growth-restricted newborn piglets. Am J Physiol 279: R1010–R1016
Schmedtje JFJ, Ji YS, Liu WL, DuBois RN, Runge MS 1997 Hypoxia induces cyclooxygenase-2 via the NF-kappaB p65 transcription factor in human vascular endothelial cells. J Biol Chem 272: 601–608
Semenza GL 2001 HIF-1 and mechanisms of hypoxia sensing. Curr Opin Cell Biol 13: 167–171
Kurtz A, Jelkmann W, Pfeischifter J, Bauer C 1985 Role of prostaglandins in hypoxia-stimulated erythropoietin production. Am J Physiol 249: C3–C8
Phillips ID, Simonetta G, Owens JA, Robinson JS, Clarke IJ, McMillen IC 1996 Placental restriction alters the functional development of the pituitary-adrenal axis in the sheep fetus during late gestation. Pediatr Res 40: 861–866
Jensen BL, Stubbe J, Hansen PB, Andreasen D, Skott O 2001 Localization of prostaglandin E(2) EP2 and EP4 receptors in the rat kidney. Am J Physiol 280: F1001–F1009
Morath R, Klein T, Seyberth HW, Nusing RM 1999 Immunolocalization of the four prostaglandin E2 receptor proteins EP1, EP2, EP3, and EP4 in human kidney. J Am Soc Nephrol 10: 1851–1860
Tilley SL, Audoly LP, Hicks EH, Kim HS, Flannery PJ, Coffman TM, Koller BH 1999 Reproductive failure and reduced blood pressure in mice lacking the EP2 prostaglandin E2 receptor. J Clin Invest 103: 1539–1545
Kennedy CR, Zhang Y, Brandon S, Guan Y, Coffee K, Funk CD, Magnuson MA, Oates JA, Breyer MD, Breyer RM 1999 Salt-sensitive hypertension and reduced fertility in mice lacking the prostaglandin EP2 receptor. Nat Med 5: 217–220
Breyer M, Breyer R 2000 Prostaglandin E receptors and the kidney. Am J Physiol 279: F12–23
Narumiya S, Sugimoto Y, Ushikubi F 1999 Prostanoid receptors: structures, properties, and functions. Physiol Rev 79: 1193–1226
Coleman RA, Smith WL, Narumiya S 1994 International Union of Pharmacology classification of prostanoid receptors: properties, distribution, and structure of the receptors and their subtypes. Pharmacol Rev 46: 205–229
Nishigaki N, Negishi M, Ichikawa A 1996 Two Gs-coupled prostaglandin E receptor subtypes, EP2 and EP4, differ in desensitization and sensitivity to the metabolic inactivation of the agonist. Mol Pharmacol 50: 1031–1037
Zhang DY, Lumbers ER, Simonetta G, Wu JJ, Owens JA, Robinson JS, McMillen IC 2000 Effects of placental insufficiency on the ovine fetal renin-angiotensin system. Exp Physiol 85: 79–84
Woods LL, Ingelfinger JR, Nyengaard JR, Rasch R 2001 Maternal protein restriction suppresses the newborn renin-angiotensin system and programs adult hypertension in rats. Pediatr Res 49: 460–467
Edwards LJ, Simonetta G, Owens JA, Robinson JS, McMillen IC 1999 Restriction of placental and fetal growth in sheep alters fetal blood pressure responses to angiotensin II and captopril. J Physiol 515: 897–904
Author information
Authors and Affiliations
Corresponding author
Additional information
Supported by a grant from the Molly Towell Perinatal Research Foundation, the Canadian Institutes of Health Research, the Alberta Heritage Foundation for Medical Research, and the National Health and Medical Research Council of Australia.
Rights and permissions
About this article
Cite this article
Williams, S., McMillen, I., Zaragoza, D. et al. Placental Restriction Increases the Expression of Prostaglandin Endoperoxide G/H Synthase-2 and EP2 mRNA in the Fetal Sheep Kidney during Late Gestation. Pediatr Res 52, 879–885 (2002). https://doi.org/10.1203/00006450-200212000-00012
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-200212000-00012