Abstract
Infants are subjected to both endogenous and exogenous corticosteroids in the pre- and postnatal periods. Stress to the mother before birth, or to the child postpartum, can give rise to high, chronic endogenous corticosteroid levels caused by activation of the hypothalamic-pituitary-adrenal (HPA) axis. Physician-administered exogenous corticosteroids are also used in the management of a wide spectrum of pre- and postnatal conditions. The long-term effects of corticosteroids in developing humans are not well known. Studies in animals, however, indicate that both natural stress and exogenous corticosteroids can have long-lasting and deleterious effects on the body, brain, behavior, and hypothalamic-pituitary-adrenal axis of developing infants. These data suggest that exogenous corticosteroids should be administered with caution, after careful benefit/risk analyses, and that, as far as possible, the developing brain should be protected against the effects of pre- and postnatal stress.
Similar content being viewed by others
The Developing Nervous System: A Series of Review Articles
The following is the fifth in our series of review articles on the developmental biology of the nervous system and its relation to diseases and disorders that are found in newborn infants and children. In this article Drs. Edwards and Burnham examine the effect of corticosteroids on brain development. Since steroids are frequently used to prevent or treat disease in the fetus and newborn infant, it is of utmost importance to determine whether such therapy has any effect on the developing brain.
Alvin Zipursky
Editor-in-Chief
Infants are subjected to both endogenous and exogenous corticosteroids in the pre- and postnatal periods. When pregnant women undergo prolonged stress, for instance, such as that caused by family discord or the death of a spouse, the unborn infant is subjected to high, chronic levels of endogenous corticosteroids (1, 2). This is a result of repeated activation of the mother's HPA axis (1). Postnatally, traumatic events in the child's life give rise to high, chronic corticosteroid levels, resulting from activation of the child's own HPA axis (3).
Exogenous glucocorticoids are also used in the management of a wide spectrum of pediatric diseases. Prenatally—and in the early postnatal period—their primary use is in the promotion of lung maturation and, thus, the prevention of respiratory distress syndrome in preterm infants (4–6). Postnatally, corticosteroids are used for a variety of diseases, such as autoimmune hemolytic anemia (7), hypoglycemia (8), CNS trauma, meningitis, and myoclonic seizures (9–11).
The long-term effects of corticosteroids in the pre- and postnatal period in humans are not known. Studies in animals, however, indicate that both antenatal stress and repeated glucocorticoid treatment can have deleterious effects. The present review summarizes animal studies of how exogenous corticosteroids and pre- and postnatal stress affect the developing brain. The review of the literature will be preceded by a discussion of the HPA axis, and its development in early life, and will conclude with results of the limited human clinical studies.
THE HYPOTHALAMIC-PITUITARY-ADRENAL AXIS
A schematic representation of the HPA axis is shown in Figure 1. The limbic system, primarily via the hippocampus, forms a major inhibitory input to the PVN of the hypothalamus by activating GABAergic interneurons (12). The PVN neurons release CRH and, to a lesser extent, AVP into the hypophyseal portal circulation. In the anterior pituitary, CRH and AVP synergistically stimulate the corticotroph cells of the anterior lobe to release ACTH (13). ACTH, transported in the systemic circulation, interacts with the adrenal cortex to cause steroidogenesis and elevation of plasma glucocorticoids. The primary glucocorticoid in humans and most other mammals is cortisol, but in rats and mice it is corticosterone (13).
Glucocorticoid feedback occurs at the level of the hippocampus, hypothalamus, and pituitary, to inhibit further HPA activity. It involves two populations of receptors: MR and GR (14) (Table 1). MR are highly concentrated in the hippocampus and septal area (15) and have a 10-fold higher affinity for circulating glucocorticoids than GR (15, 16). MR are therefore occupied (∼80%) at low, basal corticosterone levels—seen in nonstress periods (16)—and are responsible for the maintenance of basal HPA activity (15). In contrast, GR are widely distributed in the brain, being most abundant in hypothalamic CRH neurons and pituitary corticotrophs (13–16). During acute stress, rising corticosterone levels cause MR to saturate and GR to become occupied (16). GR-mediated effects restore stress-induced increases in HPA activity to basal levels. They also modify neurotransmitter release from the raphe nuclei, the nucleus tractus solitarius, and the locus ceruleus (17, 18). These in turn can alter the number of GR binding sites in the hippocampus and hypothalamus (19), thereby altering feedback regulation of the HPA axis.
With prolonged stress, chronic activation of GR causes profound changes in neuronal integrity and function—resulting in altered HPA neuroendocrine regulation and behavior (20, 21). These will be discussed below.
DEVELOPMENT OF THE HPA AXIS IN EARLY LIFE
The ontogeny of MR and GR in the brain, and the development of corticosteroid feedback control, have been studied primarily in rats. As shown in Figure 2, MR (found primarily on neurons) are largely indistinguishable from adult levels by the end of the first week of life (22, 23). High levels of MR allow the quick establishment of baseline HPA function (23). GR, on the other hand, are approximately 30% of adult values during the first few weeks of life, being found primarily on neurons (22–25). As the brain continues to develop and glial cell density increases, levels of GR in the brain increase (GR are also expressed on glia), reaching adult levels by about 30 d of life (22, 23, 25). Consistent with the slow developmental profile of GR in the brain, the ability to “rapidly turn off” a stress response does not develop fully for several weeks after birth (25, 26).
Developmental profile of MR and GR in the rat hippocampus. The concentration of MR is largely indistinguishable from adult levels by the end of the first week of life (26, 27). In contrast, GR are approximately 30% of adult levels at birth, and do not reach adult levels until approximately 4 wk of life (25–28). Thus, the ratio of MR/GR is much higher during the first few weeks of life in the rat.
The profile of GR development in the brain lags behind that of MR; thus, there is an increased ratio of MR/GR in the rat brain during the first few postnatal weeks. The most rapid brain growth—characterized by neuronal proliferation, synaptogenesis, dendritic arborization, and increased weight (27, 28)—occurs in this early postnatal period when MR occupation predominates over GR. These neuronal events seem to be depressed by GR activation (28), which may explain the low GR levels seen at that time. Thus, dysregulation of the MR/GR balance may lead to abnormalities in the brain, behavior, and endocrine response (29–35).
EFFECTS OF ENDOGENOUS GLUCOCORTICOIDS ON DEVELOPMENT
Exposure to uncontrollable stress during pregnancy results in elevated maternal and fetal plasma corticosteroid levels (36).
How fetal corticosteroid levels rise is somewhat controversial. The first possibility is that there is a direct transfer of maternal corticosteroids across the placenta (37). Some authors, however, report that access of maternal endogenous corticosteroids to the fetus is low because of the placental expression of the enzyme 11β-HSD, which converts corticosteroids to inactive products (cortisone, 11-dehydrocorticosterone) (38). Unlike endogenous corticosteroids, 11β-HSD has a low affinity for synthetic glucocorticoids (39), and so dexamethasone and betamethasone pass rapidly from mother to fetus.
The second possibility is that maternal CRH released by the hypothalamus during times of stress may cross the placenta and activate the fetal HPA axis directly, which would explain the elevated fetal levels. Studies in rats, however, indicate that the transfer of maternal CRH across the placenta is restricted (40).
Lastly, recent studies in humans suggest that elevated maternal glucocorticoids can stimulate the production of placental CRH—which is identical to hypothalamic CRH in structure, immunoreactivity, and bioactivity (41). Placental CRH may therefore enter the fetus and activate the HPA axis (42).
Effects on the body.
In the primate, guinea pig, rat, and mouse, chronic maternal stress during late gestation permanently alters fetal growth and development (27, 43–45). In rhesus monkeys, early prenatal stress reduces fetal birth weight and does so more than mid- to late prenatal stress (46). In rats, male offspring of stressed mothers, or mothers treated with exogenous CRH during late gestation, show signs of demasculinization. They have shorter anogenital distances at birth (47), and have a 20% reduction in size of the suprachiasmatic nucleus in the brain—a structure involved in neuroendocrine control of male sexual behavior in rodents (48).
Effects on the brain.
Late-gestation restraint stress (4 h/day, d 15–17) in rats causes neurotoxic changes of neurons in the fetal PVN such that neural processes are shortened and apoptosis of neurons is increased (49). Prenatal stress also has been shown to have postnatal effects on neurotransmitters, including serotonin (50) and the catecholamines (51). Development of forebrain cholinergic systems is altered by prenatal stress, because hippocampal acetylcholine release in adult male and female rats is increased in response to mild stress (52).
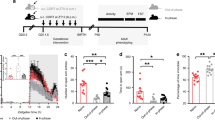
Recent studies in our laboratory have shown that prenatal stress (i.e. restraint stress under bright light for 1 h, three times per day) during early or late pregnancy in the rat significantly lowers seizure threshold in the dorsal hippocampus of 14-d-old male and female offspring (Fig. 3A [Edwards et al., submitted for publication]). We also found that prenatal stress during late, but not early, gestation also significantly facilitates the development of kindled seizures (Fig. 3B). These data suggest that prenatal stress increases excitability of the brain, which enhances its vulnerability to developing seizures.
Rats were stereotaxically implanted with a chronic indwelling bipolar electrode in the right dorsal hippocampus on postnatal d 13. They were allowed 1 d recovery. (A) After-discharge thresholds were significantly lowered in postnatal d 14 offspring of mothers who were stressed during early (d 5–12) or mid- to late gestation (d 12–19). Dams were stressed via repeated restraint under bright light, three times per day. After-discharge threshold was defined as the minimum stimulus intensity to provoke a “spike and wave” pattern of at least 3 s on the EEG. The stimulus consisted of a 1-s train of 1 ms, 60 Hz biphasic (+ve and −ve going) square-wave pulses generated by a Grass Model S88 stimulator coupled to two Grass PSIU6 stimulus-isolation constant-current units (Grass Instruments, Quincy, MA, U.S.A.). Stimulation was begun at 20 μA and increased in steps of 20 μA until an afterdischarge was triggered. The interval between stimulations was 1 min. A Grass Model 7D polygraph was used to record electroencephalographic activity. (B) Kindling rates were significantly lowered in offspring of mothers who were stressed during mid-late gestation (d 12–19). Kindling involved suprathreshold stimulations (100 μA above threshold) every 15 min over a 2-d period (postnatal d 14–15). Convulsive responses, when they developed, were scored accordingly: stage 1 (mouth clonus), stage 2 (head nodding), stage 3 (forelimb clonus), stage 4 (rearing), stage 5 (loss of postural control). Stimulations were continued until three stage 5 seizures had been evoked. Data for A and B were statistically similar between male and female pups, and were thus combined. Parentheses indicate the number of animals tested in each experimental group. Asterisks indicate significant difference from control animals (Duncan's multiple range test;p < 0.05).
Effects on behavior.
Stress during pregnancy (i.e. immobilization, restraint, crowding, repeated electric tail shocks, or noise) in rats and primates results in offspring with sleep disturbances (53), reduced juvenile play and social interaction (54), increased frequency of mutual clinging (55), attention deficits (56), decreased exploratory behavior in a novel environment (57), and enhanced fear (54). Increased levels of fear and anxiety may relate to a decrease in amygdaloid GABAergic activity resulting from prenatal stress (58, 59). Fear and anxiety are normally inhibited by agents that facilitate GABAergic transmission (58).
Effects on neuroendocrine function.
Chronic maternal stress during late gestation in the primate and rat permanently alters HPA function in the offspring (43). Offspring of prenatally stressed rhesus monkeys (unpredictable noise during mid- to late gestation [d 90–145]), for instance, have higher ACTH and cortisol levels than control offspring (60). In the rat, elevated maternal glucocorticoid levels during the third week of gestation (pregnancy = 21 d) produce a permanent 70% reduction in MR and a 30% reduction in GR in the hippocampus of prenatally stressed offspring (61). This reduction was not seen on postnatal d 3 (neonatal period), but was apparent by postnatal d 21 (weanling age) (61). Down-regulation of receptors as a result of prenatal stress must therefore occur gradually over the course of development.
These rat offspring—once born—have an altered “set point” for negative feedback, giving rise to higher basal secretion of CRH and adrenal corticosterone (31, 32). They also have enhanced sensitivity to stress-induced ACTH, giving an exaggerated stress response (31, 32, 62). Such increases in basal corticosterone levels accelerate the appearance of age-related neural and cognitive deficits in rats, including atrophy of dendritic processes and cell death (63, 64). The underlying mechanism is thought to involve energy deprivation (65), excitotoxicity (65), and disturbed calcium homeostasis (65, 66). In addition, neuronal defense mechanisms and repair by neurotrophins are impaired by corticosteroids (65). All of these changes can be prevented by blocking the mother's stress-response during pregnancy (67).
Reversal of stress effects.
Although the potential consequences of prenatal stress are great, environmental events such as maternal care and handling during the postnatal period reverse the prenatal stress-induced deficits in hippocampal corticosteroid receptors and the alterations in HPA hormone secretion (43, 68). For example, fostering of prenatally stressed pups onto other dams prevents the decrease in hippocampal MR and the rise in basal glucocorticoid levels, lowers hypothalamic CRH levels, and enhances open-field exploration-an indication of decreased anxiety in animals (43, 69–71). This occurs as a result of the foster mother spending more time than the biologic mother in pup-directed activity (71). Early postnatal handling by experimenters (15 min daily for the first few weeks of life) similarly reverses the effects of prenatal stress, by altering the behavior of the mother upon the pups' return (i.e. increased licking and grooming of the pups) (70). Available data indicate that maternal care triggers thyroid hormone release, which appears to activate ascending serotonergic projections to the hippocampal region of the brain (72). Serotonin causes long-lasting increases in GR number in hippocampal neurons, enhancing the negative feedback sensitivity to circulating corticosteroid levels (72, 73). This promotes the rapid recovery of HPA function.
EFFECTS OF EXOGENOUS GLUCOCORTICOIDS ON DEVELOPMENT
Mammals exposed to chronic high levels of exogenous glucocorticoids during early development exhibit morphologic, physiologic, and behavioral modifications in later life. The precise nature of these is dependent on the dose of the steroid, the developmental stage at which the exposure occurs (74, 75), and the species studied (76–78). In animals that give birth to relatively mature young (sheep, guinea pigs, and primates), maximal brain growth and a large proportion of neuroendocrine maturation (including corticosteroid receptor development) takes place in utero (76, 77). In species that give birth to immature young (rats, rabbits, and mice), much neuroendocrine development occurs in the postnatal period (78). Thus, glucocorticoid treatment will impact on different stages of brain development depending on the species.
The discussions below will first consider the effects of prenatal and then postnatal exposure.
PRENATAL EXPOSURE
Effects on the body.
In rhesus monkeys, daily administration of betamethasone (i.m.) to pregnant animals during the last trimester causes a significant reduction in brain, lung, liver, pancreas, heart, and adrenal weight in the fetus (79). Similarly, chronic administration of betamethasone (0.5 mg/kg) in sheep, or dexamethasone (0.1 mg/kg) in rats, during late gestation causes fetal growth retardation (80, 81). In mice, maternal treatment with prednisolone on d 13–18 of pregnancy causes offspring to have delayed development of eye opening, lifting, walking, and gripping (82).
Effects on the brain.
Administration of even a single dose of dexamethasone to pregnant rhesus monkeys during the last trimester produces dose-dependent neuronal degeneration in the hippocampal CA1–CA3 fields of offspring (83). The degeneration is more severe with multiple injections than with single injections of the same total dose (83). In addition, when pregnant monkeys receive multiple dexamethasone treatments, their offspring (at 20 mo of age) have 30% fewer hippocampal neurons than control offspring (84).
In rats, antenatal glucocorticoids administered on d 17–19 of pregnancy have been shown to promote early maturation of the dopamine systems in the forebrain (51). As well, dexamethasone exposure (0.1 mg/kg) in the last week of gestation causes decreased serotonin turnover in the neocortex, hippocampus, hypothalamus, and midbrain in offspring at 3 and 14 wk of life (50). It also reduces norepinephrine turnover in the cerebellum and forebrain (51), and norepinephrine content in the hippocampus and neocortex (50). Concentrations of GR mRNA and MR mRNA in the hippocampus are reduced by >20% (80). These alterations in corticosteroid receptor levels would be expected to alter the feedback control of glucocorticoid secretion.
Effects on behavior.
Infants of pregnant rhesus monkeys exposed to ACTH for 2 wk show impairments in motor coordination and muscle tone, have shorter attention spans, and are more irritable and difficult to console than control animals (85).
In rats, chronic treatment of pregnant dams during the last trimester with corticosterone results in sex-specific alterations in motor activity in adult offspring (86). Exploratory activity in a novel environment, for instance, is increased in adult male, but not female, offspring (86). Also, daily dexamethasone treatment (0.1 mg/kg) during the last week of gestation alters sexual behavior, such that male offspring become demasculinized and somewhat feminized (87). In mice, a single injection of dexamethasone on gestational d 14 causes differences in anxiety, memory, and socialization in the offspring (45).
Effects on neuroendocrine function.
A single injection of dexamethasone (5 mg/kg) to pregnant rhesus monkeys at 132–133 d of gestation induces an irreversible degeneration of hippocampal dentate granule neurons and CA3 pyramidal neurons (84). This attenuates corticosteroid negative feedback, thereby permanently elevating basal and stress stimulated cortisol levels in the juvenile offspring (84).
In rats, dexamethasone treatment during late gestation causes pups to have permanently decreased glucocorticoid feedback and, hence, increased basal plasma corticosterone concentrations (32, 50, 80). As a consequence, the offspring of dexamethasone-treated mothers have high blood pressure (80) and suppressed immune function (88).
Thus, both rat and primate studies show that exposure to prenatal glucocorticoids leads to long-term increases in HPA tone. Increased HPA tone throughout life has a significant impact on adult health, because of the chronic exposure of tissues to glucocorticoids. In humans, elevated concentrations of cortisol are associated with atherosclerosis, heart disease, immunosuppression, diabetes, and cognitive impairment (89, 90).
Postnatal Exposure.
The effects of postnatal exposure are less dramatic than the effects of prenatal exposure, but can be significant in species where large amounts of neural growth take place after birth.
Effects on the body.
In the neonatal rat, a single injection of dexamethasone (0.2 or 1 mg/kg s.c. on postnatal d 7) causes an acceleration of developmental landmarks such as incisor eruption, eye opening, and motor skill, and a retardation of body growth and vaginal opening (91). It also reduces whole brain and regional weights (frontal cortex, cerebellum, and brain stem) as measured on postnatal d 28 (92). Repeated neonatal dexamethasone (1 mg/kg) treatment causes a significant increase in surfactant protein D content in the rat lungs (93). It also increases bone mineral density and bone mineral content in male, but not female, rats (94).
Effects on the brain.
Administration of glucocorticoids can be neuroprotective against hypoxia-ischemia in the early postnatal period (95). This effect seems to involve a GR-mediated decrease in basal metabolic energy requirements and/or an increase in the availability or efficiency of glucose utilization (95). Also, cortisone treatment in neonates seems to prevent excessive astrocytic proliferation in response to hypoxia-ischemia by stimulating the activity of microglial cells through enhanced expression of MHC class I antigens (96).
Postnatal administration of glucocorticoids can, however, have deleterious effects on brain development (20, 97). Rates of neurogenesis, neuronal migration, and cell death reach maximal levels during the stress hyporesponsive period in the rat (postnatal d 2–14) when circulating corticosterone is low (28). Acute administration of glucocorticoids during this period causes atrophy of dendrites in various hippocampal subfields (20), permanently decreases cerebral cholesterol levels, and causes an irreversible decrease in brain weight and myelination of fibers (98). In the dentate gyrus, acute postnatal glucocorticoid treatment inhibits neurogenesis and decreases cell death (28). Thus, although the number of granule neurons appears constant, electrophysiologic studies indicate their function to be abnormal (99). Specifically, early glucocorticoid treatment alters the normal spatial extent of the perforant pathway distribution to the dentate gyrus, measured by extracellular field potential negativity of granule cell neurons (99). It also reduces the ability of entorhinal afferents to activate dentate granule cells, measured by stimulus response functions (99). Such chronic abnormalities in dentate gyrus electrophysiology might explain, at least in part, the behavioral impairments on spatial learning tests in those same animals (100).
In the rat, postnatal glucocorticoid treatment causes different populations of neurons to survive in the dentate gyrus than would normally do so (28). This may reflect an impairment of neuronal migration (101, 102), in as much as corticosteroids decrease the production of radial glia (28), and newly generated neurons preferentially migrate along radial glia (28, 102). Alterations in neural migration may predispose the infant brain to pathologic conditions, such as cortical dysplasia. Rats with cortical dysplasia, induced by intrauterine injections of methylazoxymethanol acetate, are susceptible to developing seizures (see (103) for a review). Clinically, cortical dysplasia is often found in patients with a history of medically refractory epilepsy (104). Taken together, we hypothesize that glucocorticoids may cause abnormalities in neuronal migration and cortical dysplasia, thereby altering seizure vulnerability. No clinical studies to date have tested this hypothesis, although studies in animals are currently underway in our laboratory.
Effects on behavior.
Exposing the developing nervous system to hormones of the HPA axis can produce marked long-term effects on behavior. Male rat pups injected with 25 μg of ACTH on d 2–7 postpartum exhibit poor learning performance in a shuttle box as adults, are slow to acquire reversal learning, and exhibit an exaggerated startle response (105). Rat pups treated daily with glucocorticoids during the first two postnatal weeks show delayed development of the startle reflex, of swimming ability, and of cortical evoked responses to auditory, visual, and sciatic nerve stimulation (106–108). As adults, glucocorticoid-treated animals show increased voluntary running in activity wheels and decreased motor coordination (109). They also demonstrate increased immobility in closed-field tests and enhanced defensive burying activity (110).
Effects on neuroendocrine function.
A single injection of dexamethasone to 7-d-old rats results in a significant depletion of GR from the cytosol of the brain. The effect is dose-dependent, beginning with the dose of 0.04 mg/kg (s.c.), which is far lower than the clinical dose used in obstetrics (0.4–0.5 mg/kg) (92). Repeated injections of dexamethasone (on postnatal d 1, 3, and 5) in the rat similarly cause down-regulation of GR in the brain (111).
Unaltered MR expression might explain why basal levels of circulating corticosterone are not affected by postnatal glucocorticoid treatment (110, 111)—a result that contrasts sharply with the prenatal effects of exogenous glucocorticoid treatment.
IMPLICATIONS FOR HUMANS
In animals, pre- and postnatal stress, as well as exogenous administration of glucocorticoids during pregnancy, lead to long-lasting effects on the function of the HPA axis in the offspring. Although the clinical data are limited, they suggest that similar effects may occur in humans, and that they may create the substrate for later developmental, behavioral, and mood disorders.
Clinical studies on the effects of maternal prenatal stress, for instance, suggest that repeated activation of the HPA axis—and the resultant high serum levels of endogenous corticosteroids—can cause a variety of long-term sequelae in infants (43). Maternal stress during the third trimester of pregnancy is associated with adverse birth outcomes, which include preterm birth (1), fetal growth retardation (112), delays in early motor development (42), behavioral abnormalities (3, 113, 114), and sleep disturbances in the infant (43). Maternal stress has also been linked to the development of psychiatric disorders, such as schizophrenia and depression in later life (3). Abnormal HPA regulation in the unborn child, and hence glucocorticoid secretion, has been linked to the acceleration of behavioral sensitization and drug-seeking behavior, to increased emotionality, shyness and avoidance behavior, and to decreased sociability of young children (114, 115). No effect on cognitive ability was seen (114). Thus, prenatal stress in mothers has important effects on HPA function and on the later physical and mental health of the unborn child.
With regard to postnatal stress, there is evidence that links parental loss during early childhood to an increased risk for major depression and generalized anxiety disorders (2, 3, 43, 113). These children also show a permanent elevation in plasma cortisol, which may enhance their vulnerability to disease later in life (i.e. atherosclerosis, diabetes, etc.) (42, 89, 90, 113).
Studies on the effects of exogenous corticosteroids are few in number, and have been limited to the effects of prenatal administration. Randomized trials have shown no apparent neurologic or cognitive effects in children treated prenatally with a single course of corticosteroids (4–6). The current trend in clinical practice, however, is to increase the number of corticosteroid treatments when the risk of preterm delivery persists (10). Such repeated glucocorticoid treatment in pregnant women has been shown to reduce head circumference in children (44). It has also been associated with subtle effects on neurologic function, including reduced visual closure and visual memory, in 6-y-old children (116). Lastly, repeated dexamethasone treatment in early pregnancy—because of increased risk of congenital adrenal hyperplasia—results in children with increased emotionality, unsociability, avoidance, and behavioral problems (114).
Both endogenous and exogenous corticosteroids can have significant and deleterious effects in animals. Although there are, as yet, relatively few data on the long-term effects of corticosteroids in developing humans, the data that do exist suggest that humans show effects similar to those seen in animals. These data suggest that glucocorticoids should be administered with caution.
There are, however, circumstances in which the benefits of administering corticosteroids outweigh the risks. For example, autoimmune hemolytic anemia results from the self-destruction of red blood cells. Left untreated, the accumulation of bile pigment causes severe jaundice that subsequently leads to brain damage. As development proceeds, a pattern of cerebral palsy emerges at approximately 6 mo with uncoordinated movement, deafness, disturbed vision, and speech difficulties (117). This condition is preventable because corticosteroid administration modifies the immune response and, thus, resolves the hemolytic crisis (118). As another example, hypoglycemia—common in infancy and childhood—can cause long-term neurologic damage and mental retardation (119). Neonatal administration of exogenous corticosteroids promotes glucose homeostasis and, thus, protects the brain from hypoglycemia-induced injury (120). Lastly, ACTH and prednisone can be enormously valuable in the treatment of early childhood epilepsy, particularly infantile spasms (121, 122). If untreated, repeated seizures may cause serious brain damage (123).
In conclusion, the available literature indicates that exogenous corticosteroids should be administered only after careful consideration of the benefits and risks, and that, as far as possible, the developing brain should be protected against the effects of pre- and postnatal stress.
Abbreviations
- HPA:
-
hypothalamic-pituitary-adrenal axis
- PVN:
-
paraventricular nucleus
- CRH:
-
corticotropin-releasing hormone
- POMC:
-
proopiomelanocortin
- GR:
-
glucocorticoid receptor
- MR:
-
mineralocorticoid receptors
- GABA:
-
gamma amino butyric acid
- MHC:
-
major histocompatibility complex
- 11β-HSD:
-
11β-hydroxysteroid dehydrogenase
References
Stott DH 1973 Follow-up study from birth of the effects of prenatal stresses. Dev Med Child Neurol 5: 770–787
Huttenen MO, Niskanen P 1978 Prenatal loss of father and psychiatric disorders. Arch Gen Psychiatry 35: 429–431
Meier A 1985 Child psychiatric sequelae of maternal war stress. Acta Psychiatr Scand 72: 505–511
Liggins GS, Howie RN 1972 A controlled trial of antepartum glucocorticoid treatment for the prevention of the respiratory distress syndrome in premature infants. Pediatrics 50: 515–525
Crowley P 1995 Antenatal corticosteroid therapy: a meta-analysis of the randomized trials, 1972–1994. Am J Obstet Gynecol 173: 332–335
Smolders-de Haas H, Neuvel J, Schmand B, Treffers PE, Koppe JG, Hoeks J 1990 Physical development and medical history of children who were treated antenatally with corticosteroids to prevent respiratory distress syndrome: a 10–12 year follow-up. Pediatrics 86: 65–70
Ezekowitz RAB, First LR 1994 Hematology. In: Avery ME, First LR (eds) Pediatric Medicine, 2nd Ed. Williams & Wilkins, Baltimore, pp 575–577
Robinson A, Goodman SI, O'Brien D 1984 Genetic and chromosomal disorders, including inborn errors of metabolism. In: Kempe CH, Silver HK, O'Brien D (eds) Current Pediatric Diagnosis and Treatment, 8th Ed. Lange Medical Publications, Los Altos, CA, pp 1012–1015
Nellhaus G, Stumpf DA, Moe PG 1984 Neurologic and muscular disorders. In: Kempe CH, Silver HK, O'Brien D (eds) Current Pediatric Diagnosis and Treatment, 8th Ed. Lange Medical Publications, Los Altos, CA, pp 635–771
Huang WL, Dunlop SA, Harper CG 1999 Effect of exogenous corticosteroids on the developing central nervous system: a review. Obstet Gynecol Surv 54: 336–342
Snead OC, Benton JW, Myers GJ 1983 ACTH and prednisone in childhood seizure disorders. Neurology 33: 966–970
Sutanto W, Handelman G, De Bree F, De Kloet ER 1989 Multifacetted interaction of corticosteroids with the intracellular receptors and with membrane GABA-A receptor complexes in the rat brain. J Neuroendocrinol 1: 243–247
Herman JP, Cullinan WE 1997 Neurocircuitry of stress: central control of the hypothalamo-pituitary-adrenocortical axis. Trends Neurosci 20: 78–84
McEwen BS, De Kloet ER, Rostene WE 1986 Adrenal steroid receptors and actions in the nervous system. Physiol Rev 66: 1121–1188
Funder JW 1992 Glucocorticoid receptors. J Steroid Biochem Molec Biol 43: 389–394
Reul JMHM, De Kloet ER 1985 Two receptor systems for corticosterone in rat brain: microdistribution and differential occupation. Endocrinology 117: 2505–2511
MacArthur BA, Howie RN, Dezoete JA, Elkins J 1982 School progress and cognitive development of 6 year old children whose mothers were treated antenatally with betamethasone. Pediatrics 70: 99–105
Levitt NS, Lindsay RS, Holmes MC, Seckl JR 1996 Dexamethasone in the last week of pregnancy attenuates hippocampal glucocorticoid receptor gene expression and elevates blood pressure in the adult offspring in the rat. Neuroendocrinology 64: 412–418
Towle AC, Sze PY, Lauder JM 1982 Cytosol glucocorticoid binding in monoaminergic cell groups. Dev Neurosci 5: 458–464
McEwen BS, Magarinos AM 1997 Stress effects on morphology and function of the hippocampus. Ann N Y Acad Sci 821: 271–84
Checkley S 1996 The neuroendocrinology of depression and chronic stress. Br Med Bull 52: 597–617
Bohn MC, Dean D, Hussain S, Giuliano R 1994 Development of mRNAs for glucocorticoid and mineralocorticoid receptors in rat hippocampus. Dev Brain Res 77: 157–162
Vazquez DM, Lopez JF, Morano MI, Kwak SP, Watson SJ, Akil H 1998 α, β, and γ mineralocorticoid receptor messenger ribonucleic acid splice variants: differential expression and rapid regulation in the developing hippocampus. Endocrinology 139: 3165–3177
Liggins GC 1994 The role of cortisol in preparing the fetus for birth. Reprod Fertil Dev 6: 141–150
Yi SJ, Masters JN, Baram TZ 1994 Glucocorticoid receptor mRNA ontogeny in the fetal and postnatal rat forebrain. Mol Cell Neurosci 5: 385–393
Meaney MJ, Sapolsky RM, McEwen BS 1985 The development of the glucocorticoid receptor system in the rat limbic brain. I. Ontogeny and autoregulation. Dev Brain Res 18: 159–164
Sands J, Dobbing J, Gratrix CA 1979 Cell number and cell size: organ growth and development and the control of catch-up growth in rats. Lancet 2: 503–505
Gould E 1994 The effects of adrenal steroids and excitatory input on neuronal birth and survival. Ann N Y Acad Sci 743: 73–92
Van Eckelen JAM, Rots NY, Sutanto W, Oitzl MS, De Kloet ER 1991 Brain corticosteroid receptor gene expression and neuroendocrine dynamics during aging. J Steroid Biochem Mol Biol 40: 679–683
Morano MI, Vazquez DM, Akil H 1994 The role of the hippocampal mineralocorticoid and glucocorticoid receptors in the hypothalamo-pituitary-adrenal axis of the aged Fisher rat. Mol Cell Neurosci 5: 400–412
Takahashi LK, Kalin NH 1991 Early developmental and temporal characteristics of stress-induced secretion of pituitary-adrenal hormones in prenatally stressed rat pups. Brain Res 558: 75–78
Weinstock M, Matlina A, Maor GI, Rosen H, McEwen BS 1992 Prenatal stress selectively alters the reactivity of the hypothalamic-pituitary-adrenal system in the female rat. Brain Res 595: 195–200
De Kloet ER, Vreugdenhil E, Oitzl MS, Joels M 1998 Brain corticosteroid receptor balance in health and disease. Endocr Rev 19: 269–301
Brady LS, Whitfield HJ, Fox RJ, Gold PW, Herkenham M 1991 Long-term antidepressant administration alters corticotropin-releasing hormone, tyrosine hydroxylase, and mineralocorticoid receptor gene expression in rat brain. Therapeutic implications. J Clin Invest 87: 831–837
Reul JMHM, Stec I, Soder M, Holsboer F 1993 Chronic treatment of rats with the antidepressant amitriptyline attenuates the activity of the hypothalamic-pituitary-adrenocortical system. Endocrinology 133: 312–320
Takahashi LK, Turner JG, Kalin NH 1998 Prolonged stress-induced elevation in plasma corticosterone during pregnancy in the rat: implications for prenatal stress studies. Psychoneuroendocrinology 23: 571–581
Reznikov AG, Nosenko ND, Tarasenko LV 1999 Prenatal stress and glucocorticoid effects on the developing gender-related brain. J Steroid Biochem Mol Biol 69: 109–115
Edwards CR, Benediktsson R, Lindsay RS, Seckl JR 1996 11 beta-Hydroxysteroid dehydrogenases: key enzymes in determining tissue-specific glucocorticoid effects. Steroids 61: 263–269
Seckl JR 1997 Glucocorticoids, feto-placental 11 beta-hydroxysteroid dehydrogenase type 2, and the early life origins of adult disease. Steroids 62: 89–94
Williams MT, Davis HN, McCrea AE, Hennessy MB 1998 The distribution of radiolabeled corticotropin-releasing factor in pregnant rats: an investigation of placental transfer to the fetuses. Int J Dev Neurosci 16: 229–234
Petraglia F, Volpe A, Genazzani R, Rivier J, Sawchenko PE, Vale W 1990 Neuroendocrinology of the human placenta. Front Neuroendocrinol 11: 6–37
Sandman CA, Wadhwa PD, Chicz-DeMet A, Dunkel-Schetter C, Porto M 1997 Maternal stress, HPA activity, and fetal-infant outcome. Ann N Y Acad Sci 814: 266–275
Weinstock M 1997 Does prenatal stress impair coping and regulation of hypothalamic-pituitary-adrenal axis?. Neurosci Biobehav Rev 21: 1–10
French NP, Hagan R, Evans SF, Godfrey M, Newnham JP 1999 Repeated antenatal corticosteroids: size at birth and subsequent development. Am J Obstet Gynecol 180: 114–121
Rayburn WF, Christensen CL, Gonzalez CL 1997 A placebo-controlled comparison between betamethasone and dexamethasone for fetal maturation: differences in neurobehavioral development of mice offspring. Am J Obstet Gynecol 176: 842–850
Schneider ML, Roughton EC, Koehler AJ, Lubach GR 1999 Growth and development following prenatal stress exposure in primates: an examination of ontogenetic vulnerability. Child Dev 70: 263–274
Secoli SR, Teixeira NA 1998 Chronic prenatal stress affects development and behavioral depression in rats. Stress 2: 273–280
Anderson DK, Rhees RW, Fleming DE 1985 Effects of prenatal stress on differentiation of the sexually dimorphic nucleus of the preoptic area (SDN-POA) of the rat brain. Brain Res 332: 113–118
Fujioka T, Sakata Y, Yamaguchi K, Shibasaki T, Kato H, Nakamura S 1999 The effects of prenatal stress on the development of hypothalamic paraventricular neurons in fetal rats. Neuroscience 92: 1079–1088
Muneoka K, Mikuni M, Ogawa T, Kitera K, Kamei K, Takigawa M, Takahashi K 1997 Prenatal dexamethasone exposure alters brain monamine metabolism and adrenocortical response in rat offspring. Am J Physiol 273: R1669–R1675
Slotkin TA, Lappi SE, McCook EC, Tayyeb MI, Eylers JP, Seidler FJ 1992 Glucocorticoids and the development of neuronal function: effects of prenatal dexamethasone exposure on central noradrenergic activity. Biol Neonate 61: 326–336
Day JC, Koehl M, Deroche V, Le Moal M, Maccari S 1998 Prenatal stress enhances stress- and corticotropin-releasing factor-induced stimulation of hippocampal acetylcholine release in adult rats. J Neurosci 18: 1886–1892
Rao U, McGinty DJ, Shinde A, McCracken JT, Poland RE 1999 Prenatal stress is associated with depression-related electroencephalographic sleep changes in adult male rats: a preliminary report. Prog Neuropsychopharmacol Biol Psychiatry 23: 929–939
Takahashi LK, Haglin NH, Kalin NH 1992 Prenatal stress potentiates stress-induced behavior and reduces propensity to play in juvenile rats. Physiol Behav 51: 319–323
Clarke AS, Schneider ML 1993 Prenatal stress has long-term effects on behavioral responses to stress in juvenile rhesus monkeys. Dev Psychobiol 26: 293–304
Schneider ML, Coe CL 1993 Repeated social stress during pregnancy impairs neuromotor development in the primate infant. J Dev Behav Pediatr 14: 81–87
Schneider ML 1992 Prenatal stress exposure alters postnatal behavioral expression under conditions of novelty challenge in rhesus monkey infants. Dev Psychobiol 25: 529–540
Fride E, Dan Y, Gavish M, Weinstock M 1985 Prenatal stress impairs maternal behavior in a conflict situation and reduces hippocampal benzodiazepine receptors. Life Sci 36: 2103–2109
Makino S, Gold PW, Schulkin J 1994 Corticosterone effects on corticotropin-releasing hormone mRNA in the central nucleus of the amygdala and the parvocellular region on the paraventricular nucleus of the hypothalamus. Brain Res 640: 105–112
Clarke AS, Wittwer DJ, Abbott DH, Schneider ML 1994 Long-term effects of prenatal stress on HPA axis activity in juvenile rhesus monkeys. Dev Psychobiol 27: 257–269
Henry C, Kabbaj M, Simon H, Le Moal M, Maccari S 1994 Prenatal stress increases the hypothalamo-pituitary-adrenal axis response in young and adult rats. J Neuroendocrinol 6: 341–345
Koehl M, Darnaudery M, Dulluc J, Van Reeth O, Le Moal M, Maccari S 1999 Prenatal stress alters circadian activity of hypothalamo-pituitary-adrenal axis and hippocampal corticosteroid receptors in adult rats of both gender. J Neurobiol 40: 302–315
Euchs E, Uno H, Flugge G 1995 Chronic psychosocial stress induces morphological alterations in hippocampal neurons of the tree shrew. Brain Res 673: 275–282
Arbel I, Kadar T, Silbermann M, Levy A 1994 The effects of long-term corticosterone administration on hippocampal morphology and cognitive performance of middle-aged rats. Brain Res 657: 227–235
Sapolsky RM 1996 Stress, glucocorticoids, and damage to the nervous system: the current state of confusion. Stress 1: 1–19
Landfield PW 1987 Modulation of brain aging correlates by long-term alterations of adrenal steroids and neurally-active peptides. Prog Brain Res 72: 279–300
Barbazanges A, Piazza PV, Le Moal M, Maccari S 1996 Maternal glucocorticoid secretion mediates long-term effects of prenatal stress. J Neurosci 16: 3943–3949
Takahashi LK 1998 Prenatal stress: consequences of glucocorticoids on hippocampal development and function. Int J Dev Neuroscience 16: 199–207
Maccari S, Piazza PV, Kabbaj M, Barbazanges A, Simon H, Le Moal M 1995 Adoption reverses the long-term impairment in glucocorticoid feedback induced by prenatal stress. J Neurosci 15: 110–116
Vallee M, Mayo W, Dellu F, Le Moal M, Simon H, Maccari S 1997 Prenatal stress induces high anxiety and postnatal handling induces low anxiety in adult offspring: correlation with stress-induced corticosterone secretion. J Neurosci 17: 2626–2636
Meaney MJ, Diorio J, Francis D, Widdowson J, LaPlante P, Caldji C, Sharma S, Seckl JR, Plotsky PM 1996 Early environmental regulation of forebrain glucocorticoid receptor gene expression: implications for adrenocortical responses to stress. Dev Neurosci 18: 49–72
Meaney MJ, Diorio J, Francis D, LaRocque S, O'Donnell D, Smythe JW, Sharma S, Tannenbaum B 1994 Environmental regulation of the development of glucocorticoid receptor systems in the rat forebrain. The role of serotonin. Ann N Y Acad Sci 746: 260–273
Sapolsky RM 1997 The importance of a well-groomed child. Science 277: 1620–1621
Clarke AS 1993 Social rearing effects on HPA axis activity over early development and in response to stress in rhesus monkeys. Dev Psychobiol 26: 433–446
Levine S, Johnson DF, Gonzalez CA 1985 Behavioral and hormonal responses to separation in infant rhesus monkeys and mothers. Behav Neurosci 99: 399–410
Matthews SG, Challis JRG 1996 Regulation of the hypothalamo-pituitary-adrenocortical axis in fetal sheep. Trends Endocrinol Metab 7: 239–246
Matthews SG 1998 Dynamic changes in glucocorticoid and mineralocorticoid receptor mRNA in the developing guinea pig brain. Dev Brain Res 107: 123–132
Sapolsky RM, Meaney MJ 1986 Maturation of the adrenocortical stress response: neuroendocrine control mechanisms and the stress hyporesponsive period. Brain Res Rev 396: 64–76
Johnson JW, Mitzner W, Beck JC, London WT, Sly DL, Lee PA, Khouzami VA, Cavalieri RL 1981 Long-term effects of betamethasone on fetal development. Am J Obstet Gynecol 141: 1053–1064
Levitt NS, Lindsay RS, Holmes MC, Seckl JR 1996 Dexamethasone in the last week of pregnancy attenuates hippocampal glucocorticoid receptor gene expression and elevates blood pressure in the adult offspring in the rat. Neuroendocrinology 64: 412–418
Jobe AH, Newnham J, Willet K, Sly P, Ikegami M 1998 Fetal versus maternal and gestational age effects of repetitive antenatal glucocorticoids. Pediatrics 102: 1116–1125
Gandelman R, Rosenthal C 1981 Deleterious effects of prenatal prednisolone exposure upon morphological and behavioral development of mice. Teratology 24: 293–301
Uno H, Lohmiller L, Thieme C, Kemnitz JW, Engle MJ, Roecker EB, Farrell PM 1990 Brain damage induced by prenatal exposure to dexamethasone in fetal rhesus macaques. I. Hippocampus. Brain Res Dev Brain Res 53: 157–167
Uno H, Eisele S, Sakai A, Shelton S, Baker E, DeJesus O, Holden J 1994 Neurotoxicity of glucocorticoids in the primate brain. Horm Behav 28: 336–348
Schneider ML, Coe CL, Lubach GR 1992 Endocrine activation mimics the adverse effects of prenatal stress on the neuromotor development of the infant primate. Dev Psychobiol 25: 427–439
Diaz R, Fuxe K, Ogren SO 1997 Prenatal corticosterone treatment induces long-term changes in spontaneous and apomorphine-mediated motor activity in male and female rats. Neuroscience 81: 129–140
Holson RR, Gough B, Sullivan P, Badger T, Sheehan DM 1995 Prenatal dexamethasone or stress but not ACTH or corticosterone alter sexual behavior in male rats. Neurotoxicol Teratol 17: 393–401
Bakker JM, Schmidt ED, Kroes H, Kavelaars A, Heijnen CJ, Tilders FJ, van Rees EP 1995 Effects of short-term dexamethasone treatment during pregnancy on the development of the immune system and the hypothalamo-pituitary adrenal axis in the rat. J Neuroimmunol 63: 183–191
Munck A, Naray-Fejes-Toth A 1994 Glucocorticoids and stress: permissive and suppressive actions. Ann N Y Acad Sci 746: 115–120
Lupien SJ, McEwen BS 1997 The acute effects of corticosteroids on cognition: integration of animal and human model studies. Brain Res Brain Res Rev 24: 1–27
Benesova O, Pavlik A 1989 Perinatal treatment with glucocorticoids and the risk of maldevelopment of the brain. Neuropharmacology 28: 89–97
Ferguson SA, Holson RR 1999 Neonatal dexamethasone on day 7 causes mild hyperactivity and cerebellar stunting. Neurotoxicol Teratol 21: 71–6
Ogasawara Y, Kuroki Y, Tsuzuki A, Ueda S, Misaki H, Akino T 1992 Pre- and postnatal stimulation of pulmonary surfactant protein D by in vivo dexamethasone treatment of rats. Life Sci 50: 1761–1767
Karabelyos C, Horvath C, Hollo I, Csaba G 1998 Effect of neonatal glucocorticoid treatment on bone mineralization of adult nontreated, dexamethasone-treated or vitamin D3-treated rats. Gen Pharmacol 31: 789–791
Tuor UI 1997 Glucocorticoids and the prevention of hypoxic-ischemic brain damage. Neurosci Biobehav Rev 21: 175–179
McRae A, Bona E, Hagberg H 1996 Microglia-astrocyte interactions after cortisone treatment in a neonatal hypoxia-ischemia model. Brain Res Dev Brain Res 94: 44–51
McEwen BS, Angulo J, Cameron H, Chao HM, Daniels D, Gannon MN, Gould E, Mendelson S, Sakai R, Spencer R, Woolley C 1992 Paradoxical effects of adrenal steroids on the brain: protection versus degeneration. Biol Psychiatry 31: 177–199
Gumbinas M, Oda M, Huttenlocher P 1973 The effects of corticosteroids on myelination of the developing rat brain. Biol Neonate 22: 355–366
Vicedomini JP, Nonneman AJ, DeKosky ST, Scheff SW 1985 Perinatal glucocorticoids alter dentate gyrus electrophysiology. Brain Res Bull 15: 111–116
Vicedomini JP, Nonneman AJ, DeKosky ST, Scheff SW 1986 Perinatal glucocorticoids disrupt learning: a sexually dimorphic response. Physiol Behav 36: 145–149
Rickmann M, Amaral DG, Cowan WM 1987 Organization of radial glial cells during the development of the rat dentate gyrus. J Comp Neurol 264: 449–479
Altman J, Bayer SA 1990 Migration and distribution of two populations of hippocampal granule cell precursors during the perinatal and postnatal periods. J Comp Neurol 301: 365–381
Sperber EF, Veliskova J, Germano IM, Friedman LK, Moshe SL 1999 Age-dependent vulnerability to seizures. Adv Neurol 79: 161–169
Mishel PS, Nguyen LP, Vinters HV 1995 Cerebral cortical dysplasia associated with pediatric epilepsy: review of neuropathological features and proposal for a grading system. J Neuropathol Appl Neurobiol 54: 137–153
McGivern RF, Rose G, Berka C, Clancy AN, Sandman CA, Beckwith BE 1987 Neonatal exposure to a high level of ACTH4-10 impairs adult learning performance. Pharmacol Biochem Behav 27: 133–142
Golub MS 1982 Maze exploration in juvenile rats treated with corticosteroids during development. Pharmacol Biochem Behav 17: 473–479
Pavlovska-Teglia G, Stodulski G, Svendsen L, Dalton K, Hau J 1995 Effect of oral corticosterone administration on locomotor development of neonatal and juvenile rats. Exp Physiol 80: 469–75
Salas M, Schapiro S 1970 Hormonal influences upon the maturation of rat brains responsiveness to sensory stimuli. Physiol Behav 5: 7–11
Howard E, Granoff DM 1968 Increased voluntary running and decreased motor coordination in mice after neonatal corticosterone implantation. Exp Neurol 22: 661–673
Felszeghy K, Sasvari M, Nyakas C 1993 Behavioral depression: opposite effects of neonatal dexamethasone and ACTH-(4–9) analogue (ORG 2766) treatments in the rat. Horm Behav 27: 380–396
Felszeghy K, Gaspar E, Nyakas C 1996 Long-term selective down-regulation of brain glucocorticoid receptor after neonatal dexamethasone treatment in rats. J Neuroendocrinol 8: 493–499
Cliver SP, Goldenburg RL, Cutter GR, Hoffman HJ, Copper RL, Gotlieb SJ, Davis RO 1992 The relationships among psychosocial profile, maternal size, and smoking in predicting fetal growth retardation. Obstet Gynecol 80: 262–267
Clements AD 1992 The incidence of attention deficit-hyperactivity disorder in children whose mothers experienced extreme psychological stress. Georgia Educational Researcher 91: 1–14
Trautman PD, Meyer-Bahlburg HF, Postelnek J, New MI 1995 Effects of early prenatal dexamethasone on the cognitive and behavioral development of young children: results of a pilot study. Psychoneuroendocrinology 20: 439–49
Prasad C, Prasad A 1995 A relationship between increased voluntary alcohol preference and basal hypercorticosteronemia associated with an attenuated rise in corticosterone output during stress. Alcohol 12: 59–63
MacArthur BA, Howie RN, Dezoete JA, Elkins J 1982 School progress and cognitive development of 6 year old children whose mothers were treated antenatally with betamethasone. Pediatrics 70: 99–105
Avery ME, Als H, Coulter DM 1994 Neonatology. In: Avery ME, First LR (eds) Pediatric Medicine, 2nd Ed. Williams & Wilkins, Baltimore, pp 231–232
Ezekowitz RAB, First LR 1994 Hematology. In: Avery ME, First LR (eds) Pediatric Medicine, 2nd Ed. Williams & Wilkins, Baltimore, pp 575–577
Halamek LP, Benaron DA, Stevenson DK 1997 Neonatal hypoglycemia. Part 1: Background and definition. Clin Pediatr 36: 675–680
Silver HK, Gotlin RW, Klingensmith GJ 1984 Endocrine disorders. In: Kempe CH, Silver HK, O'Brien D (eds) Current Pediatric Diagnosis and Treatment, 8th Ed. Lange Medical Publications, Los Altos, CA, pp 774–777
Chutorian AM 1982 Corticosteroids and corticotrophin in the treatment of neurologic disorders, with emphasis on neurologic disorders of childhood. Clin Neuropharm 5: 239–265
Snead OCI, Benton JW, Myers GL 1983 ACTH and prednisone in childhood seizure disorders. Neurology 33: 966–970
Haines ST, Casto DT 1994 Treatment of infantile spasms. Ann Pharmacother 28: 779–790
Author information
Authors and Affiliations
Corresponding author
Additional information
Support, in part, by a grant from the Bloorview Childrens Hospital Foundation to W.M.B.
Rights and permissions
About this article
Cite this article
Edwards, H., Burnham, W. The Impact of Corticosteroids on the Developing Animal. Pediatr Res 50, 433–440 (2001). https://doi.org/10.1203/00006450-200110000-00003
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-200110000-00003