Abstract
The objective was to investigate whether there is any correlation between signs of central and peripheral immune stimulation in victims of sudden infant death syndrome (SIDS), the former expressed by IL-6 in cerebrospinal fluid (CSF), the latter by IgA, IgG, and IgM immunocytes, T lymphocytes, and HLA-DR expression in laryngeal mucosa. Seventeen SIDS cases with low CSF IL-6 levels (≤5 pg/mL) and 20 cases with high CSF IL-6 levels (≥30 pg/mL) were subjected to immunohistochemical quantitation of IgA, IgG, and IgM immunocytes; semiquantitative scoring of T lymphocytes in the mucosa of epiglottis and larynx, and semiquantitative evaluation of HLA-DR expression. SIDS cases with IL-6 levels ≥30 pg/mL had a significantly higher number of IgA immunocytes in laryngeal mucosa (p = 0.007) and in epiglottis (p = 0.03) than cases with IL-6 levels ≤5 pg/mL. Furthermore, laryngeal HLA-DR expression was significantly more extensive in SIDS cases with IL-6 levels ≥30 pg/mL than in those with levels ≤5 pg/mL (p = 0.05). No differences were found for IgG and IgM immunocytes or for T cells. In addition, babies found prone more often had symptoms of slight infection before death and had a higher number of IgA immunocytes in the larynx (p = 0.02) than babies sleeping on their side or back. Because IL-6 levels ≥30 pg/mL correspond to the levels found in infants who die from infectious diseases such as meningitis/septicemia and pneumonia, the findings favor the hypothesis that many SIDS cases may be caused by an "overreaction" of the immune system to an otherwise harmless infection.
Similar content being viewed by others
Main
SIDS deaths occur more often during wintertime than during the summer(1–3), and the frequency is also higher during periods with epidemics of upper respiratory infection(4). Approximately half of SIDS cases have had signs of an upper respiratory infection before death(1,5). Many of them also show mucosal immune stimulation in the lungs, trachea(6,7), duodenum(7), and salivary glands(8). However, to our knowledge, the larynx and epiglottis have not been systematically studied in SIDS.
We have previously shown that SIDS cases have elevated levels of IL-6 in CSF(9) and postulated a possible relationship between such central immune response indicated by CSF IL-6 levels and peripheral immune stimulation(9).
In the present study the larynx was chosen because it is an organ that is important with regard to obstructive apneas and the laryngeal reflex(10). Moreover, a respiratory tract infection is quite common in SIDS babies. Several studies have shown that laryngeal stimulation affects respiration(11,12), and Lindgren and Grøgaard(13) have shown that laryngeal stimulation in RSV-infected infants results in disturbances in the regulation of breathing.
Our hypothesis was therefore that immune reactions in the laryngeal mucosa may induce a central immune response with elevated levels of IL-6 in SIDS.
We thus wanted to examine whether there is a relationship between central immune response in SIDS, indicated by increased CSF IL-6 levels, and peripheral immune stimulation as expressed by the presence of IgA, IgG, and IgM immunocytes and T lymphocytes (CD3) in the laryngeal mucosa and HLA-DR expression in the surface epithelium and in the glands of the wall.
METHODS
Subjects. Seventeen SIDS cases with low CSF IL-6 levels (≤5 pg/mL) and 20 SIDS cases with high CSF IL-6 levels (≥30 pg/mL) were studied. IL-6 concentrations in CSF had been measured by ELISA technique (Biotrak Amersham). Fewer than half of the results of these measurements have been published elsewhere(9,14). All SIDS cases originated from the Institute of Forensic Medicine in the period July 1992 through April 1997. In this period, 70 SIDS cases were examined. However, 13 cases had to be excluded because of a postmortal time >48 h, and in 11 of the cases appropriate tissue samples or CSF was not available. The rationale for selecting the SIDS cases exclusively on the basis of CSF IL-6 levels was to compare the immune response in cases with obvious IL-6 elevation with cases with low normal values to detect any differences between these two groups. Five girls and four boys with a similar age range as those investigated were thus excluded. Forty-four percent of all the SIDS cases measured had clearly elevated IL-6 levels >30 pg/mL, whereas 37% had low normal levels <5 pg/mL.
There were 12 girls and 25 boys in the present material. The median age was 3.5 mo (range 1 wk to 19 mo). Further clinicopathologic information about the subjects is given in Tables 1 and 2. All information was obtained from medical records and police reports.
Microbiologic examination. In all the cases but one, a nasopharyngeal aspiration was performed during autopsy, and smears were made. After air-drying and fixation in acetone for 10 min, the slides were kept at -70° before staining. After applying FITC-conjugated MAb to influenza A and B viruses, a mixture of three MAb specific to parainfluenza virus types 1, 2, and 3, and MAb to RSV and adenovirus, the specimens were examined by a blind trial for respiratory viruses by a direct immunofluorescence technique. All antibodies were supplied by Dako, Cambridgeshire, United Kingdom. Blood, CSF, and tissue from lung, liver, spleen, and kidney were examined for bacterial growth. Culture specimens from bronchial tree secretions were obtained when present.
Tissue preparation and immunohistochemical staining. A longitudinal section from the larynx including the epiglottis was obtained by autopsy, which in all cases was performed within 48 h after death. The sections were approximately 2 mm thick and were either fixed directly in 96% cold alcohol(15) or extracted in cold PBS for 24 h to remove diffusable extracellular immunoglobulins before alcohol fixation and paraffin embedding(16). Serial sections from the PBS-extracted tissue samples were cut at 6 µm and evaluated by paired immunohistochemical staining with fluorochrome-conjugated polyclonal rabbit anti-human antisera to the immunoglobulin isotypes IgA, IgM, and IgG (Dako A/S, Copenhagen, Denmark). The directly fixed tissue samples were also cut into serial sections and either stained with fluorescein-conjugated rabbit anti-human pan T (CD3) cell (Dako A/S) or with a mouse monoclonal anti-human antibody to the nonpolymorphic site of the HLA-DR determinant (Becton Dickinson, Sunnyvale, CA). The latter two antigens were visualized by a three-step immunofluorescence method applying biotinylated goat anti-rabbit IgG (Dako A/S) and biotinylated goat anti-mouse IgG2a (Southern Biotechnology Associates, Birmingham, AL), respectively, and fluorescein-labeled avidin (Vector Laboratories, Burlingame, CA) (Table 3).
Quantitation of IgA, IgG, and IgM immunocytes, semiquantitative scoring of T lymphocyte density in the mucosa of the epiglottis and larynx, and semiquantitative evaluation of epithelial HLA-DR expression were performed with a Leitz Aristoplan fluorescence microscope (Leica Microscopie and Systeme GmbH, Wetzlar, Germany) equipped with a Ploem-type epilluminator for narrow-band excitation and selective filtration of green and red emission colors. Cell counting of immunocytes density was based on the counting of 30 grid fields. Scoring of the T cell density was based on dividing the mean cell counts into three categories: in the larynx, 0-15 cells per grid was given a score of 1, 16-29 cells per grid was given a score of 2, and ≥30 cells per grid was given a score of 3. For the epiglottis the scores were as follows: 0-9 cells per grid scored 1, 10-14 cells per grid scored 2, whereas ≥15 cells per grid corresponded to a score of 3. In most cases stable means for immunocyte counts and T cell scores were obtained after evaluation of 25 grid fields. HLA-DR expression was scored in the following way: intense positive staining in surface epithelium (squamous and columnar) was given a maximum score of 2, no staining in the surface epithelium was scored 0, intermediate staining was scored 1, no staining in the glandular epithelium was scored 0, staining of 50% of the glands was scored 2, and intense staining of most of the glands (≥75%) was scored 4. Intermediate staining patterns received scores of 1 or 3.
Reproducibility of cell counting. Interindividual reproducibility of cell counts was tested by counting 30 grids for the three immunocyte isotypes independently and another 30 grids for the immunocyte isotype IgA and IgG by two observers (Å.V. and T.O.R.). Intraindividual reproducibility of staining and morphometric evaluation was tested by an evaluation of IgA-positive immunocytes in the epiglottis and larynx in adjacent sections in 22 cases, by blind trial.
Statistical analyses. For comparison between groups, the Mann-Whitney U test was applied and for reproducibility testing, the κ test was used. To evaluate whether there were differences in symptoms before death according to sleeping position when found dead, and whether there were more infants with symptoms in the group with high CSF IL-6 levels than in the group with low CSF IL-6 levels, the χ2 test was applied.
RESULTS
Clinical symptoms. In total, there were 18 infants with symptoms of a mild upper respiratory infection (a common cold with rhinitis and/or cough and/or fever) and 19 without such symptoms. Among the infants with high CSF IL-6, 12 had signs of an infection, whereas the corresponding number in the group with low CSF IL-6 was six.
Nineteen of the babies were found dead in a prone position. Significantly more prone sleeping babies had symptoms before death than the babies sleeping on their side or back (p = 0.02). Babies found prone also had a higher number of IgA immunocytes in the larynx (p = 0.02). Furthermore, infants with symptoms before death had a higher number of IgA immunocytes in the laryngeal mucosa (p = 0.01).
Microbiologic examination. In three of the cases with high CSF IL-6 levels, respiratory viruses were found, whereas no such viruses were found in the low CSF IL-6 group. In one of the cases with respiratory viruses a potentially pathogenic bacteria was also found in the lung tissue. Furthermore, bacterial growth that might be of significance was found in six additional cases (Table 4). However, five of the cases with low IL-6 levels also showed bacterial growth with potential significance (Table 5).
Reproducibility. Cell counts by two different observers showed a high degree of reproducibility (κ = 0.89). Reproducibility of the staining procedure and scoring system applied by the same observer (Å. V. I and Å. V. II) was also substantial (κ = 0.72).
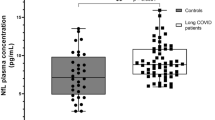
IgA, IgG, and IgM immunocytes. SIDS cases with IL-6 levels ≥30 pg/mL had a significantly higher number of IgA immunocytes in the epiglottis (p = 0.03) (Fig. 1a) and in the laryngeal mucosa (p = 0.007) (Fig. 1b) than cases with IL-6 levels ≤5 pg/mL. No differences were found for IgG and IgM immunocytes. Sections from larynx with IgA and IgG immunocytes, and IgA and IgM immunocytes, respectively, are shown in Figure 2, a and b.
Mean immunocyte counts in the epiglottis (a) and the laryngeal mucosa (b) in SIDS cases with high CSF IL-6 levels (≥30 pg/mL) and low CSF IL-6 levels (≤5 pg/mL). SIDS cases with high IL-6 levels had significantly higher IgA cell numbers per tissue unit (mm2) in the epiglottis (p = 0.03), as well as in the larynx (p = 0.007), than those with low IL-6 levels.
Microscopic sections from laryngeal mucosa in a case with high CSF IL-6 values. a, Immunocytes stained green for IgA and red for IgG. b, Immunocytes stained green for IgA and red for IgM (magnification ×200). c, Routine stained section (hematoxylin and eosin) of laryngeal glands. d, Adjacent section stained green for HLA-DR (magnification ×200).
HLA-DR expression and T cells. Sections from the larynx with laryngeal glands stained green for HLA-DR are shown in Figure 2, c and d. HLA-DR expression in laryngeal glandular epithelium was more extensive in SIDS cases with IL-6 levels ≥30 pg/mL than in those with levels ≤5 pg/mL (p = 0.05) (Fig. 3).
No differences were found for T cells. When combining the scores for HLA-DR and CD3 in the larynx, however, the scores showed a more pronounced stimulation in the group with high levels of IL-6 in the CSF, the p value being close to significance (p = 0.05).
DISCUSSION
To our knowledge, the present paper demonstrates for the first time a link between an immune response in the laryngeal wall and high IL-6 levels in the CNS in SIDS. The normal upper limit of IL-6 in CSF is reported to be 5 pg/mL(17). This is in accordance with our previous studies, in which we have found the CSF IL-6 levels in acute, violent deaths to be <5 pg/mL(9,14). Steinmetz et al.(18) claim that serum IL-6 levels >30 pg/mL should be considered clearly elevated. In the absence of a specific reference value for CSF, this cutoff value was also chosen for CSF in the present study. Several studies of the prevalence of cytokines in CSF in cases of various types of meningitis and septic shock or bacteremia report the IL-6 levels to be very high(19,20), in most cases >100 pg/mL, with a median of several thousand picograms per milliliter. If we only include cases with values >100 pg/mL in the present material, the link between SIDS cases with high IL-6 and an immune stimulation in the larynx still shows the same trend.
The coexistence of signs of infection before death and an increased number of IgA immunocytes in the laryngeal mucosa in many SIDS cases pinpoints the significance of the larynx as an important anatomic site for possibly dangerous immune reactions in the pathogenesis of SIDS. Moreover it has been demonstrated that respiratory tract infections may interfere with respiratory control mechanisms(13). Thus, vagal reflexes may induce bradycardia and apnea(21). Lindgren and Grøgaard(13) recently showed that laryngeal stimulation in RSV-infected infants resulted in a reinforced reflex apnea response compared with noninfected infants. It is feasible that other infectious agents may act in the same way. Experiments in animals have shown that laryngeal stimulation may induce prolonged and even fatal apneas(11,12). In addition, stimulation of chemoreceptors and free nerve endings in the upper airway induces reflex apnea in infants(21,22).
Three of the SIDS cases in the group with high IL-6 levels are ≥12 months. They were included, however, because it has been shown that there is no relationship between age or sex of patients and the ability to produce IL-6(14,23,24). Furthermore, both mature and immature neonates may produce IL-6 as a response to life-threatening infection(24).
The fact that babies who were found dead in a prone position were more likely to have had symptoms of infection before death and to have increased laryngeal IgA response fits with the observation of a marked increase in the risk of dying from SIDS when factors such as prone sleeping position, upper airway infection, and heat stress, caused by either overwrapping or excessive environmental temperature, are all present(25,26).
Several studies have shown that levels of IL-6 in CSF are elevated in meningitis(19,20) and that IL-6 is an endogenous pyrogen(27). The link between peripheral immunologic organs and the CNS may be blood-borne mediators(28–30) or be caused by retrograde axonal transport(31). Thus, Maehlen et al.(31) have shown that peripheral stimulation may alter the immune response locally within the CNS through retrograde axonal transport. It is therefore possible that laryngeal stimulation may stimulate centers in the brain stem and thereby provoke a production of IL-6 in the CNS. Both microglia and astrocytes(32), as well as endothelial cells(33), are capable of producing IL-6. It is also possible that IL-6 may be produced locally and then, through retrograde axonal transport, reach the CNS. One might also speculate whether IL-6 in the cerebrospinal fluid could be a result of leakage from autolytic cells after death. In a previous study(14), CSF was sampled at two different times after death in 26 subjects. The median IL-6 level increased from 73 to 116.5 pg/mL in 18 h. In half of the subjects a postmortem increase was seen, whereas one third showed a decrease. Only one of the cases would have been transferred from the high IL-6 group to the low IL-6 group, whereas two cases would have been included if the second sample had been chosen for the study. Exclusion of the first case would not have influenced the results of the study.
To rule out the possibility of passive leakage-especially of IgG-into immunoglobulin-producing cells, paired immunohistochemical staining was applied, with double staining for IgA and IgM. No double staining was seen, except in two cases, in which a few scattered cells showed mixed fluorescence. These cells were excluded.
Noah et al.(34) found markedly elevated levels of the cytokines IL-1β, IL-1γ, IL-6, and TNF-α in nasal lavage fluid in infants and children with acute upper respiratory disease. They furthermore state that increased cytokine production in nasal secretions is a general phenomenon in viral upper respiratory infection and that it is not specific to certain pathogens. IL-6 may be produced by a wide variety of cells, including epithelial cells. Infection by several different viruses and bacteria may also enhance the IL-6 production in fibroblasts and monocytes. A production of IL-6 in laryngeal mucosa could therefore be a possible source of the observed IL-6 levels in CSF in our cases, transmitted either by retrograde axonal transport(31) or by blood. However, Waage et al.(19) and Chavanet et al.(20) have shown that the systemic circulation and the CNS represent separate compartments, and that cells normally present in the CNS may release the cytokines.
In three of our cases with high CSF IL-6 levels who were found prone and in whom there had been light infectious symptoms before death, viruses were detected in the nasopharyngeal secretions (RSV, adenovirus, and parainfluenza virus). It has also been shown that both lambs and infants will respond to heat stress with increased respiratory rate(35). In infants irregular breathing was almost always noted when the body temperature reached 37-37.1°C, and this was seen before any other sign of thermoregulation. There was also an increased frequency of apneic episodes.
Mistchenko et al.(36) show that in adenovirus infection in children, the serum IL-6 concentration is related to the severity of the disease. In moderately ill patients, there was no IL-6 production. We have previously shown that in a group of children dying of violent deaths there were significantly lower CSF IL-6 levels than in both the SIDS group and the group with infectious deaths(9,14). In the SIDS babies, the cytokines produced may give hyperpyrexia, which, when added to the increased temperature caused by known risk factors such as prone position and overwrapping, may induce irregular breathing(35) and thus hypoxia and finally coma and death. Laryngeal reflexes in the presence of hypoxemia have cardioinhibitory effects(37). The present study is in accordance with these findings.
We have previously looked at the development of immune response markers in the tracheal wall in fetal life and the first year after birth.(38). No IgA immunocytes were present until 2 wk after birth, from which time the number increased. A few IgG-, IgM-, and CD3-positive cells were seen throughout the period studied, with a significant increase of CD3- and IgM-positive cells after birth. The number of IgA-positive cells seemed stable after the fourth postnatal week. In one of our cases the infant was 1 wk old and did not have any IgA-positive cells, which is in accordance with these findings. All other subjects were 3 wk or older and should thus not be subject to variations owing to age with regard to IgA-positive cells. Gleeson et al.(39) have presented a paper that favors the hypothesis of an immunologic overreaction. They demonstrated an infant who ultimately died of SIDS and who had a more prolonged and intense immune response compared with control infants with the same upper respiratory infection.
Several researchers have reported evidence of similarities between SIDS and infectious deaths(7,14,40,41). We believe that the rapid development of mucosal immunity in the first months after birth(38) may cause a vulnerability for an immunologic overreaction; i.e. the babies may react in an inappropriately strong manner to minor immunologic stimuli, such as slight upper respiratory infections(42). This could be the reason for the striking discrepancy between the high IL-6 levels in the CSF in many SIDS cases and the lack of correspondingly severe clinical symptoms. A recent report in animal experiments(43) suggests a two-stage scenario: an initial sympathoexcitation with profuse sweating and tachycardia followed by sympathoinhibition, and enhanced vagal outflow inducing bradycardia and hypotension.
High doses of IL-6 have been given to humans, inducing fever and headache, but not hypotension(44). However, Minghini et al.(45) have recently reported that IL-6 and IL-1 are potent dilating agents for skeletal muscle resistance vessels under in vivo conditions, acting together with parenchymal or intravascular factors. Parents often report their babies found dead in SIDS to be extremely warm and sweaty(14). The fever-inducing effects of IL-6 could induce apnea and irregular breathing, which eventually could lead to hypoxic apnea and death. A possible effect of IL-6 on the vasculature and thus the blood pressure is a question that apparently is still not solved.
Abbreviations
- CSF:
-
cerebrospinal fluid
- RSV:
-
respiratory syncytial virus
- SIDS:
-
sudden infant death syndrome
References
Andersen M, Arnestad M, Rognum TO, Vege Å 1995 Cot death in eastern part of Norway 1984-92. Tidsskr Nor Laegeforen 115: 34–37.
Murphy MFG, Campbell MJ 1987 Sudden infant death syndrome and environmental temperature: an analysis using vital statistics. J Epidemiol Community Health 41: 63–71.
Beal S, Porter C 1991 Sudden infant death syndrome related to climate. Acta Paediatr 80: 278–287.
Froggatt P, Lynas MA, Marshall TK 1968 Sudden infant death in babies: epidemiology. Am J Cardiol 22: 457–468.
Valdes-Dapena M 1998 A pathologist's perspective on possible mechanisms in SIDS. Ann NY Acad Sci 533: 31–36.
Forsyth KD, Weeks SC, Kohl L, Skinner J, Bradley J 1989 Lung immunoglobulins in the sudden infant death syndrome. BMJ 298: 23–26.
Stoltenberg L, Saugstad OD, Rognum TO 1992 Sudden infant death syndrome victims show local immunoglobulin M response in tracheal wall and immunoglobulin A response in duodenal mucosa. Pediatr Res 31: 372–375.
Thrane PS, Rognum TO, Brandtzaeg P 1994 Up-regulated epithelial expression of HLA-DR and secretory component (SC) in salivary glands: reflection of mucosal immunostimulation in sudden infant death syndrome (SIDS). Pediatr Res 35: 625–628.
Vege Å, Rognum TO, Scott H, Aasen AO, Saugstad OD 1995 SIDS cases have increased levels of Interleukin-6 in the cerebrospinal fluid. Acta Paediatr 84: 193–196.
Johnson P, Salisbury DM, Storey AT 1975 Apnea induced by stimulation of sensory receptors in the larynx. In: Bosma JF, Showacre J, eds. Development of the Upper Respiratory Anatomy and Function. Washington, DC, US Dept of Health, Education, and Welfare, Publication NIH 75-941, 160–183.
Harding R, Johnson P, McClelland ME 1978 Liquid-sensitive laryngeal receptors in the developing sheep, cat and monkey. J Physiol 277: 409–422.
Lucier GE, Storey AT, Sessle BJ 1979 Effects of upper respiratory tract stimuli on neonatal respiration: reflex and single neuron analyses in the kitten. Biol Neonate 35: 82–89.
Lindgren C, Grögaard J 1996 Reflex apnoea response and inflammatory mediators in infants with respiratory tract infection. Acta Paediatr 85: 798–803.
Vege Å, Rognum TO, Aasen AO, Saugstad OD 1998 Are elevated cerebrospinal fluid levels of IL-6 in sudden unexplained deaths, infectious deaths and deaths due to heart/lung disease in infants and children due to hypoxia?. Acta Paediatr 87: 819–824.
Sainte-Marie G 1962 A paraffin embedding technique for studies employing immunofluorescence. J Histochem Cytochem 10: 250–260.
Brandtzaeg P 1974 Mucosal and glandular distribution of immunoglobulin components. Immunohistochemistry with a cold ethanol-fixation method. Immunology 26: 1101–1114.
Matsuzono Y, Nraita M, Akutsu Y, Togashi T 1995 Interleukin-6 in cerebrospinal fluid of patients with central nervous system infections. Acta Paediatr 84: 879–883.
Steinmetz HT, Herbertz A, Bertram M, Diehl V 1995 Increase in interleukin-6 serum level preceding fever in granulocytopenia and correlation with death from sepsis. J Infect Dis 171: 225–228.
Waage A, Halstensen A, Shalaby R, Brandtzæg P, Kierulf P, Espevik T 1989 Local production of tumor necrosis factor α, interleukin 1, and interleukin 6 in meningococcal meningitis. J Exp Med 170: 1859–1867.
Chavanet P, Bonnotte B, Guiguet M, Zeller V, Solary E, Maurice L, Casanovas O, Caillot D, Waldner A, Kisterman JP, Portier H 1992 High concentrations of intrathecal interleukin-6 in human bacterial and nonbacterial meningitis. J Infect Dis 166: 428–431.
Wennergren G, Hertzberg T, Milerad J, Bjure J, Lagercrantz H 1989 Hypoxia reinforces laryngeal reflex bradycardia in infants. Acta Paediatr Scand 78: 11–17.
Perkett EA, Vaughan RL 1982 Evidence for a laryngeal chemoreflex in some human preterm infants. Acta Paediatr Scand 71: 696–672.
de Bont ESJM, Martens A, van Raan J, Samson G, Fetter WPF, Okken A, de Leij LHMF, Kimpen JLL 1994 Diagnostic value of plasma levels of tumor necrosis factor α (TNFα) and interleukin-6 (IL-6) in newborns with sepsis. Acta Paediatr 83: 696–699.
Groll AH, Meiser A, Weise M, Rettwitz-Volk W, von Loewenich V, Gussetis ES, Kornhuber B 1992 Interleukin 6 as early mediator in neonatal sepsis. Pediatr Infect Dis J 11: 496–497.
Ponsonby A-L, Dwyer T, Gibbons LE, Cochrane JA, Wang Y-G 1993 Factors potentiating the risk of sudden infant death syndrome associated with the prone position. N Engl J Med 329: 377–382.
Fleming PJ, Gilbert R, Azaz Y, Berry PJ, Rudd PT, Stewart A, Hall E 1990 Interaction between bedding and sleeping position in the sudden infant death syndrome: a population based case-control study. BMJ 301: 85–89.
Dinarello CA 1989 Interleukin-1 and its biologically related cytokines. Adv Immunol 44: 153–205.
Guntheroth WG 1989 Interleukin-1 as intermediary causing prolonged sleep apnea and SIDS during respiratory infections. Med Hypotheses 28: 121–123.
Krueger JM, Walter J, Dinarello CA, Wolff SM, Chedid L 1984 Sleep-promoting effects of endogenous pyrogen (interleukin-1). Am J Physiol 246:R994–R999.
Stoltenberg L, Sundar T, Almaas R, Storm H, Rognum TO, Saugstad OD 1994 Changes in apnea and autoresuscitation in piglets after intravenous and intrathecal interleukin-1β injection. J Perinatal Med 22: 421–432.
Maehlen J, Olsson T, Zachau A, Klareskog L, Kristensson K 1989 Local enhancement of major histocompatibility complex (MHC) class I and II expression and cell infiltration in experimental allergic encephalomyelitis around axotomized motor neurons. J Neuroimmunol 23: 125–132.
Lee SC, Liu W, Dickson DW, Brosnan CF, Berman JW 1993 Cytokine production by human fetal microglia and astrocytes. J Immunol 150: 2659–2667.
Kishimoto T 1989 The biology of interleukin-6. Blood 74: 1–10.
Noah TL, Henderson FW, Wortman IA, Devlin RB, Handy J, Koren HS, Becker S 1995 Nasal cytokine production in viral upper respiratory infection of childhood. J Infect Dis 171: 584–592.
Riesenfeld T, Hammarlund K, Norsted T, Sedin G 1996 Irregular breathing in young lambs and newborn infants during heat stress. Acta Paediatr 85: 467–470.
Mistchenko AS, Diez RA, Mariani AL, Robaldo J, Maffey AF, Bayley-Bustamante G, Grinstein S 1994 Cytokines in adenoviral disease in children: association of interleukin-6, interleukin-8, and tumor necrosis factor alpha levels with clinical outcome. J Pediatr 124: 714–720.
Wennergren G, Bjure J, Hertzberg T, Lagercrantz H, Milerad J 1993 Laryngeal reflex. Acta Paediatr Scand Suppl 389: 53–56.
Stoltenberg L, Thrane PS, Rognum TO 1993 Development of immune response markers in the trachea in the fetal period and the first year of life. Pediatr Allergy Immunol 4: 13–19.
Gleeson M, Clancy RL, Cripps AW 1993 Mucosal immune response in a case of sudden infant death syndrome. Pediatr Res 33: 554–556.
Blackwell CC, Weir DM, Busuttil A 1995 Infectious agents, the inflammatory responses of infants and sudden infant death syndrome (SIDS). Mol Med Today 1: 72–78.
Vege Å, Chen Y, Opdal SH, Saugstad OD, Rognum TO 1994 Vitreous humor hypoxanthine levels in SIDS and infectious death. Acta Paediatr 83: 634–639.
Rognum TO, Saugstad OD 1993 Biochemical and immunological studies in SIDS victims. Clues to understanding the death mechanism. Acta Paediatr Suppl 389: 82–85.
Harper RM 1998 Neural basis for cardiovascular signs during fatal SIDS events. Abstract. Proceedings of the 5th SIDS International Conference, Rouen, France, 7
Dinarello CA 1997 Proinflammatory and anti-inflammatory cytokines as mediators in the pathogenesis of septic shock. Chest 112:( suppl): 321S–329S.
Minghini A, Britt LD, Hill MA 1998 Interleukin-1 and interleukin-6 mediated skeletal muscle arteriolar vasodilation: in vitro and in vivo studies. Shock 9: 210–215.
Author information
Authors and Affiliations
Additional information
Supported by the Norwegian SIDS Society and the Research Council of Norway.
Rights and permissions
About this article
Cite this article
Vege, Å., Rognum, T. & Ånestad, G. IL-6 Cerebrospinal Fluid Levels Are Related to Laryngeal IgA and Epithelial HLA-DR Response in Sudden Infant Death Syndrome. Pediatr Res 45, 803–809 (1999). https://doi.org/10.1203/00006450-199906000-00004
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-199906000-00004
This article is cited by
-
Age-related cytokine imbalance in the thymus in sudden infant death syndrome (SIDS)
Pediatric Research (2023)
-
Altered gene expression and possible immunodeficiency in cases of sudden infant death syndrome
Pediatric Research (2016)
-
Candidate gene variants of the immune system and sudden infant death syndrome
International Journal of Legal Medicine (2016)
-
Gene variants predisposing to SIDS: current knowledge
Forensic Science, Medicine, and Pathology (2011)
-
Interleukin-6 and the serotonergic system of the medulla oblongata in the sudden infant death syndrome
Acta Neuropathologica (2009)