Abstract
Previous in vitro studies of cord blood platelets from full-term and preterm neonates have demonstrated decreased responses to most physiologic agonists. This hyporesponsiveness is, in part, related to both deficient synthesis of, and response to, an important mediator of platelet function, thromboxane A2(TxA2). The poor response of neonatal platelets to TxA2 is not due to differences in TxA2 receptor binding characteristics, when compared with platelets from adult controls. Therefore, the postreceptor signal transduction pathway was investigated. The TxA2 receptor is linked via the trimeric GTP-binding protein, Gq, to phospholipase C-β (PLCβ), and stimulation of platelets with the stable TxA2 mimetic, U46619, leads to activation of PLCβ and subsequent intracellular signaling events. U46619-induced 32P-phosphatidic acid formation, an index of PLCβ activation, was decreased in platelets of neonates (166 ± 10%) when compared with adult controls (206 ± 22%) (p < 0.05). Mobilization of intracellular calcium was impaired in platelets of newborns (175 ± 49 nM) in comparison to adult controls (506 ± 130 nM) (p < 0.01), after stimulation with U46619. U46619-stimulated GTPase activity was blunted in platelet membrane fractions from full-term neonates and almost absent in platelet membranes from preterm infants. Immunoblotting studies of the platelet membrane fractions, quantified by densitometric analysis, showed that levels of the Gαq subunit were not significantly different between adult and neonate, and were not the cause of the marked differences in GTPase activity. These data suggest that signal transduction through the TxA2 receptor is affected by decreased activity of Gq in platelets of neonates, and that this defect in signal transduction through PLCβ contributes to the observed poor response of newborns' platelets to TxA2 and consequently to TxA2-dependent agonists such as collagen.
Similar content being viewed by others
Main
The transient physiologic alteration in the neonatal hemostatic system is of clinical importance to those caring for the newborn. The abnormalities in the coagulation cascade and fibrinolytic system have been extensively studied(1–3). Studies of neonatal platelet function have been hampered by the need for relatively large volumes of blood for standardized studies. Therefore, most of the information available about the activity of neonatal platelets has been obtained from studies done on umbilical cord blood platelets collected at the time of delivery. These cord blood platelets respond differently to activation stimuli than platelets of either older children or adults(4–7). We, and others, have described decreased activation responses in cord blood platelets from full-term newborns to agonists including thrombin, ADP, epinephrine, collagen and U46619 (a stable mimetic of thromboxane A2; TxA2)(8–10). The activation parameters found to be deficient have included aggregation, granule secretion, calcium flux, fibrinogen receptor expression, and TxA2 production.
Premature infants, particularly those under 1500 g in weight, often have serious medical problems that increase their risk of hemorrhage. The levels of clotting factors at birth are lower in premature infants than in full-term newborns(11,12). To evaluate the contribution of platelets to this increased risk of bleeding in premature infants, we examined the function of their cord blood platelets. In comparison to full-term neonatal platelets, the premature platelets showed poorer responses to all agonists studied(13,14). We also confirmed that platelets of premature neonates, like their full-term counterparts, produce less TxA2 than adult platelets(10,14). This platelet hypofunction may put this group of infants at increased risk of bleeding, particularly in the presence of additional risk factors such as asphyxia or infection(15).
TxA2, the product of platelet arachidonic acid metabolism and an important endogenous platelet activator, is essential for full platelet activation by agonists such a collagen and low concentrations of thrombin. The decreased TxA2 production was a result of decreased conversion of arachidonic acid to TxA2 in the neonatal platelets(10).
Platelets have a single class of high affinity TxA2-binding sites (500-2500 per platelet)(16–18). The platelet TxA2 receptor belongs to the superfamily of GTP binding protein-coupled receptors, which have seven hydrophobic transmembrane domains(19). It is linked via a pertussis toxin-insensitive G protein (Gq) to phosphatidylinositol-specific phospholipase C-β (PLCβ)(19–21), which generates the intracellular second messengers, inositol 1,4,5-trisphosphate (IP3) and diacylglycerol. These second messengers stimulate intracellular calcium flux and protein kinase C activation, respectively(21–24), leading to platelet granule secretion and aggregation(20,22,25). The decreased response of premature newborn platelets, and to a lesser extent those of the full-term newborn platelets, to the TxA2 analogue, U46619, suggested either a defect in the TxA2 receptor or in receptor-coupled events(14). No significant differences in binding affinity or number of binding sites were found when comparing adult and neonatal platelets. Therefore we have evaluated postreceptor events including U46619-induced calcium flux, inositol phospholipid turnover, and the GTPase activity of the α-subunit of Gq.
METHODS
Subjects. Studies were performed on cord venous blood from 12 full-term infants (gestational age ≥37 wk) and from 4 preterm infants (gestational age 34 ± 1 wk). Mothers had no history of bleeding diathesis, alcohol, or ASA ingestion for 2 wk before delivery. In some studies, the results of all neonates, full-term and preterm, were combined. Control platelets were obtained from 10 healthy nonsmoking adults with no history of drug or alcohol ingestion.
Blood collection and preparation. Blood was collected from the umbilical vein immediately after clamping of the cord; 40-60 mL of cord blood were drawn into plastic syringes containing ACD (1.9: 8.1; ACD:blood; v:v). Blood from adult controls was obtained by venipuncture and drawn into ACD (1.9: 8.1; ACD:blood; v:v). Platelet-rich plasma was prepared by centrifugation of the citrated whole blood at 800 g for 5 min at 20°C. Platelet counts were conducted on a Coulter counter (model JT2, Coulter Electronics, Hialeah, FL), and platelets were then washed and resuspended in physiologic buffers before study(26). All experiments were conducted within 2 h of blood collection.
Phosphoinositide metabolism. Platelet-rich plasma from four adults and four full-term neonates was labeled with 100 µCi/mL [32P]-orthophosphate for 90 min at 37°C. The platelets were washed by centrifugation at 800 g for 10 min After stimulation with 1 µM U46619, 1U/mL thrombin, or buffer control for 3 min, the lipids were extracted and separated by thin-layer chromatography, autoradiographed, and quantified by radiochromatogram scanning(27). All samples were run in triplicate. Under the experimental conditions used, the [32P]-orthophosphate is preferentially incorporated into the highly metabolically active phosphoinositides rather than the more abundant phosphatidylcholine and the formation of [32P]-phosphatidic acid reflects the effects of the phosphoinositide-specific phospholipase C (PLCβ) rather than nonspecific phospholipase C or D. Therefore [32P]-phosphatidic acid formation was monitored as an indirect index of phosphoinositide metabolism(28). The results of stimulated samples were compared with unstimulated controls.
Measurement of cytosolic free calcium concentrations. Changes in cytosolic free calcium concentration was measured using Fura 2(29). Briefly, platelet-rich plasma was incubated with 3 µM Fura 2 AM, at 37°C for 30 min. Platelets were washed by centrifugation and resuspended in Tyrode's-HEPES buffer (134 mM NaC1, 12 mM NaHCO3, 2.9 mM KC1, 0.34 mM Na2HPO4, 1 mM MgC12, 10 mM HEPES, 5 mM dextrose, 0.3% BSA, pH 7.4), at a final concentration of 2 × 108/mL. Two milliliter aliquots were dispensed into quartz cuvettes, 1 mM CaC12 added, and while the sample stirred, U46619 (0.1-1.0 µM) was added. The fluorescence was monitored continuously at 339 nm excitation and 500 nm emission wavelengths in a Shimadzu-5000 spectrofluorophotometer (Hadley Tek-science, Oakville Ontario). After 5 min, digitonin (375 µM) was added, followed by 7.5 mM EDTA to obtain the maximum (Fmax) and minimum (Fmin) Fura 2 fluorescence values, respectively. Cytosolic calcium concentration was quantified using the method of Pollock et al.(30).
Platelet membrane preparation. Platelet pellets were resuspended in 10 mM Tris-HCl (pH 7.5) and 1 mM EDTA, sonicated for 15-25 sec and the homogenate was centrifuged at 30,000 g for 15 min at 4°C. The resulting pellet was resuspended in ice-cold 10 mM Tris-HCl/1 mM EDTA and centrifuged a second time before the membrane pellet was resuspended in 10 mM Tris-HCl (pH 7.5) and stored at -70°C(31). Before assay, the membranes were thawed and the protein concentration determined.
GTPase activity. Platelet membrane GTPase activity was measured by quantitating the liberation of 32Pi from [γ-32P] GTP, using the methods of Houslay et al.(32). The assay mixture contained 0.4 µM [γ-32P] GTP, 5 mM MgCl2, 100 mM NaCl, 1 mM DTT, 0.5 mM EGTA, 1 mM ATP, 50 units of creatine kinase, 12 mM phosphocreatine and 50 mM Tris-HCl (pH 7.4) in a 100 µL volume. To this cocktail, increasing concentrations of U46619 (0.01-10 µM) and platelet membranes (10 µL) or appropriate buffer controls were added. All samples were assayed in triplicate. The samples were incubated together for 10 min at 37°C, and the reaction was terminated by the addition of 0.5 mL of 20 mM NaPO4 buffer with 5% activated charcoal. The samples were centrifuged at 6000 g for 10 min and the 32Pi in 100 µL aliquot of supernatant was counted using a Beckman LS 7800 scintillation counter. GTPase activity was calculated as the difference between total and nonspecific hydrolysis (defined with 50 µM unlabeled GTP), and expressed as pmol of 32Pi liberated per min per mg of protein.
Immunoblotting of Gαq. Immunoblots were performed as previously described(14). Briefly, platelet membranes were solubilized and aliquots, each containing 25 µg of protein, were separated by 10% SDS-PAGE and transferred to nitrocellulose. The nitrocellulose was incubated with polyclonal antibody to the C-terminal decapeptide of Gαq (Calbiochem, San Diego CA) overnight at 4°C. The nitrocellulose was washed with Tris-buffered saline/Tween, incubated with peroxidase-conjugated goat anti-rabbit IgG and visualized by enhanced chemoluminescence (Amersham, Oakville, Ontario). The radiography film was scanned and subjected to densitometry analysis (Quantiscan).
Statistical analysis. Means, standard deviations, standard errors, and tests of significance (t test) were calculated with the spreadsheet program, Excel (Microsoft, Redmond, WA).
RESULTS
Agonist-induced phosphoinositide metabolism. U46619 stimulated 32P-phosphatidic acid formation, an index of PLCβ activation, in platelets of neonates (165 ± 10%) and adult controls (206 ± 21%), compared with unstimulated platelets (Table 1). Phosphatidic acid formation was, however, significantly less in the neonatal samples compared with the adult controls (p < 0.05). PA formation in response to thrombin was greater than to U46619 but was also significantly less in neonatal platelets than in the adult controls.
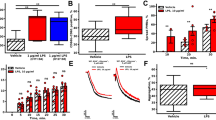
U46619-induced changes in intracellular calcium. The neonatal platelets had basal intracellular calcium levels of 139 ± 29 nM (mean ± SD; n = 8) that was not significantly different to that measured in the adult controls, 143 ± 21 nM (n = 9). The increase in intracellular calcium levels in response to U46619 was deficient in the neonatal platelets, when compared with the adult controls (175 ± 49 nM versus 506 ± 130 nM; p < 0.01) (Fig. 1). Similar decreased responses were also observed when 1U/mL thrombin was used as the agonist, although the absolute change in intracellular calcium was much higher (1181 ± 144 nM versus 3063 ± 371 nM).
Changes in intracellular calcium concentration in response to 1 µM U46619. Intracellular calcium flux was measured in Fura 2 - loaded platelets monitored in a spectrofluorophotometer after addition of agonist. Data points represent the difference between the basal and peak calcium levels for each sample. In adult platelets (n = 9) intracellular calcium concentration increased by 506 ± 130 nM, in neonates (n = 8) by 175 ± 49 nM. The difference between the means was significant at p < 0.01.
U46619-induced GTPase activity. GTPase activity in the platelet membranes of full-term neonates, preterm neonates and adult controls is shown in Fig. 2. In the adult samples GTPase activity increased in a dose-dependent manner in response to U46619. These results are similar to those reported by Shenker et al.(33), including a basal activity of 7.2 ± 1.8 pmol Pi/min/mg protein. In contrast, the neonatal platelet membranes showed a significantly lower basal level of GTPase activity, 1.7 ± 0.7 pmol Pi/min/mg protein. In response to increasing concentrations of U46619, GTPase activity of platelets from full-term infants was blunted, with a plateau at 0.1 µM, in comparison to the GTPase activity in the adult platelets, which was still increasing at this concentration of U46619 (p < 0.05). Most striking was the almost absent response of GTPase to stimulation by U46619 in the preterm platelets (Fig. 2); the GTPase activity was significantly less than the activity in adult platelets at all concentrations of U46619 (p < 0.05).
Stimulation of GTPase activity by U46619 in platelet membranes from full-term neonates (n = 6), preterm neonates (n = 4) and adult controls (n = 4). Activity was quantified by the measurement of 32Pi released from [γ-32P]- GTP in the presence of agonist and platelet membranes. Data points represent the mean ± SEM. (*) Data points significantly different (p < 0.05) than adult controls. Each platelet membrane sample was assayed in triplicate.
Gαq immunoblot analysis. Platelet membranes from preterm and full-term neonates and adult controls were analyzed using specific antibodies against Gαq (Fig. 3). Under conditions with equivalent protein loading, densitometry analysis of the Gαq band from four immunoblots showed values (in arbitrary units) as follows: preterm 990 ± 73 (60%); full-term 1523 ± 190 (86%); adult controls 1650 ± 103 (100%). The values for platelets from preterm and full-term neonates were not significantly different from adult controls.
Representative immunoblot of Gαq from adult (A), full-term neonatal (FT) and preterm neonatal (PT) platelet membranes. 25 µg aliquots of solubilized platelet protein were separated on a 10% SDS-PAGE gel, transferred to nitrocellulose and detected using anti-Gαq anti-serum, peroxidase conjugated goat anti-rabbit IgG and enhanced chemoluminescence. Gαq was detected as a single 43 kD band.
DISCUSSION
Cord blood platelets from full-term and preterm infants have been shown to have both deficient synthesis of, and response to, TxA2(6,8,10,14). The TxA2 receptor was found to be present, and have binding characteristics similar to that found in platelets of adult controls(14). Therefore in the present study we have examined post-TxA2 receptor events in these platelets. Receptor activation, and consequent activation of PLCβ, leads to internal calcium release and the activation of protein kinase C, which are required for granule secretion and expression of fibrinogen receptors. Failure of this signal transduction pathway leads to impaired platelet activation as can be demonstrated both by the effects of PLC inhibitors such as U73122(34) and by the clinical bleeding symptoms of individuals identified to have defects in this pathway(35,36).
Phosphatidic acid production, an index of PLCβ activity and phosphoinositide metabolism, was decreased in neonatal platelets stimulated with U46619. We have previously demonstrated that phosphoinositide metabolism was decreased in these platelets in response to collagen stimulation(10), which is consistent with the TxA2-dependence of collagen-induced platelet activation(30,37,38).
Changes in intracellular calcium concentration after platelet activation result from both the release of calcium from the dense tubular system mediated by IP3, and the influx of extracellular calcium across the plasma membrane, which may also be mediated in part by inositol phosphates(23). Gelman et al.(9) demonstrated that mobilization of intracellular calcium by neonatal platelets was impaired after stimulation of platelets by both thrombin and collagen. In the present study we have demonstrated that a similar impairment occurs when using U46619, the TxA2 analogue, as agonist, and this supports the conclusion that deficient IP3 production results in decreased calcium mobilization. Basal levels of calcium in the neonatal platelets were found to be no different from that of adult controls.
As phosphoinositide hydrolysis was decreased in neonatal platelets in response to both U46619 and thrombin, we examined Gq, the heterotrimeric G protein involved in signal transduction from the TxA2 receptor to PLCβ(33). Gq is also one of the G proteins (in addition to Gi) involved in thrombin activation of PLCβ(39,40), and may be involved in signaling through other surface receptors(41). Upon receptor activation, the αβγ-GDP complex of the G protein dissociates and GDP is replaced with GTP on the α-subunit. The α-subunit has intrinsic GTPase activity, which hydrolyses the GTP and results in reassociation of the α-subunit with the βγ subunits and termination of the activation signal. The function of the G protein can be evaluated by measuring agonist-stimulated GTPase activity. The membranes of cord blood platelets from full-term and preterm neonates had lower basal GTPase activity, as well as blunted or absent increases in activity after stimulation by U46619. Immunoblots detected levels of Gαq protein in the membranes of platelets from preterm infants, which were 60% of adult controls, whereas platelets from full-term infants had Gαq protein content 86% of adult controls. These small differences in the quantity of Gαq protein do not account for the significantly decreased GTPase activity in neonatal platelets.
The deficient Gαq activity associated with abnormal platelet function is supported by two recent reports. Gabbeta et al.(42) described a single patient, with a lifelong bleeding diathesis associated with decreased platelet aggregation and secretion responses when stimulated by collagen, epinephrine, ADP and U46619, who had an isolated, partial deficiency of G αq. In addition, Gαq knock-out mice have recently been described by Offermanns et al.(41). The Gαq-/-mice have a bleeding diathesis, markedly prolonged bleeding times and platelets that do not aggregate or mobilize calcium in response to U46619, thrombin, collagen, or ADP. This suggests that functional Gαq is required by each of these agonists for effective platelet activation.
The situation in the newborn differs from the two described above, as the Gαq deficiency is qualitative, rather than quantitative, and may be the result of upstream defects in signal transduction from the TxA2 receptor to Gq, as suggested by the blunted response to U46619; or decreased intrinsic activity of the enzyme, as suggested by the lower basal GTPase activity in the unstimulated membranes. In addition, this defect is transient (as is the decreased platelet function) and most likely represents a point on the maturational continuum.
This finding of this defect in signal transduction in cord blood platelets may explain many of the previously described abnormalities in platelet function of newborn infants, including poor aggregation and secretion responses, decreased PLC activity, impaired calcium mobilization, and decreased thromboxane production. As Gq appears to transduce signals from agonist receptors for thrombin and TxA2, it may provide a unified explanation for the hyporesponsiveness of neonatal platelets to several physiologic platelet activators.
Abbreviations
- ACD :
-
citrate/citric acid/dextrose
- PLCβ :
-
phospholipase C-β
- IP3 :
-
inositol trisphosphate
- TxA 2 :
-
thromboxane A2
References
Andrew M, Paes B, Johnston M 1990 Development of the hemostatic system in the neonate and young infant. Am J Pediatr Hematol Oncol 12: 95–104.
Beardsley DS 1991 Hemostasis in the perinatal period: approach to the diagnosis of coagulation disorders. Sem Perinatol 15( suppl 2): 25:334.
Andrew M, Mitchell L, Vegh P, Ofosu F 1994 Thrombin regulation in children differs from adults in the absence and presence of heparin. Thromb Haemost 72: 836–842.
Mull MM, Hathaway HE 1970 Altered platelet function in newborns. Pediatr Res 4: 229–237.
Corby DG, O'Barr TP 1981 Decreased α-adrenergic receptors in newborn platelets: cause of abnormal response to epinephrine. Dev Pharmacol Ther 2: 215–225.
Stuart MJ, Dusse J, Clark DA, Walenga RW 1984 Differences in thromboxane production between neonatal and adult platelets in response to arachidonic acid and epinephrine. Pediatr Res 18: 823–826.
Whaun JM 1973 The platelet of the newborn infant. Thromb Diath Hemorrh 30: 327–333.
Rajasekhar D, Kestin AS, Bednarek FJ, Ellis PA, Barnard MR, Michelson A 1994 Neonatal platelets are less reactive than adult platelets to physiological agonists in whole blood. Thromb Haemost 72: 957–963.
Gelman B, Setty BNY, Chen D, Amin-Hajani S, Stuart MJ 1996 Impaired mobilization of intracellular calcium in neonatal platelets. Pediatr Res 39: 696–696.
Israels SJ, Daniels M, McMillan EM 1990 Deficient collagen-induced activation in the neonatal platelet. Pediatr Res 27: 337–343.
Andrew M, Paes B, Milner R, Johnston M, Mitchell L, Tollefson DM, Castle V, Powers P 1988 Development of the human coagulation system in the healthy premature infant. Blood 72: 1651–1657.
Forrestier F, Daffos F, Galacteros F, Bardakjian J, Rainaut M, Benzard Y 1986 Hematological values of 163 normal fetuses between 18 and 30 wk of gestation. Pediatr Res 20: 342–346.
Rajasekhar D, Barnard MR, Bednarek FJ, Michelson AD 1997 Platelet hyporeactivity in very low birth weight neonates. Thromb Haemost 77: 1002–1007.
Israels SJ, Odaibo FS, Robertson C, McMillan EM, McNicol A 1997 Deficient thromboxane synthesis and response in platelets from premature infants. Pediatr Res 41: 218–223.
Kuhne T, Imbach P 1998 Neonatal platelet physiology and pathophysiology. Eur J Pediatr 157: 87–94.
Mais DE, Burch RM, Saussy DL Jr, Kochel PJ, Halushka PV 1985 Binding of a thromboxane A2/prostaglandin H2 receptor antagonist to washed human platelets. J Pharmacol Exp Ther 235: 729–734.
Kattelman EJ, Venton DL, Le Breton GC 1986 Characterization of U46619 binding in unactivated, intact human platelets and determination of binding site affinities of four TXA2/PGH2 receptor agonists. Thromb Res 41: 471–481.
Liel N, Mais DE, Halushka PV 1987 Binding of a thromboxane A2/prostaglandin H2 agonist [3H]U46619 to washed human platelets. Prostaglandins 33: 789–97.
Hirata M, Hayashi Y, Ushibuki F, Yokota Y, Kageyama R, Nakanishi S, Narumiya S 1991 Cloning and expression of cDNA for a human thromboxane A2 receptor. Nature 349: 617–620.
Brass LF, Shaller CC, Belmonte EJ 1987 Inositol 1:4,5-trisphophate-induced granule secretion in platelets. Evidence that the activation of phospholipase C mediated by platelet thromboxane receptors involves a guanine nucleotide binding protein-dependent mechanism distinct from that of thrombin. J Clin Invest 79: 1269–1275.
McNicol A, Israels SJ, Gerrard JM 1993 Recent Advances in Blood Coagulation. Churchill Livingston, Edinburgh,. pp 17: 49
Israels SJ, Robinson P, Docherty J, Gerrard JM 1985 Activation of permeabilized platelets by inositol 1:4,5-trisphosphate. Thromb Res 40: 499–509.
Berridge MJ 1993 Inositol trisphosphate and calcium signalling. Nature 361: 315–325.
Gerrard JM, Israels SJ, Friesen LL 1985 Protein phosphorylation and platelet secretion. Nouv Rev Fr Hematol 27: 267–275.
Gerrard JM, Beattie LL, Park J et al. 1989 A role for protein kinase C in the membrane fusion necessary for platelet granule secretion. Blood 74: 2405–2413.
McNicol A 1996 Platelets: A Practical Approach. Oxford University Press, Oxford,. pp 1: 25
McNicol A, Robertson C, Gerrard JM 1993 Vanadate activates platelets by enhancing arachidonic acid release. Blood 81: 2329–2338.
Holmsen H, Dangelmaier CA, Rogved S 1984 Tight coupling of thrombin-induced acid hydrolase secretion and phosphatidate synthesis to receptor occupancy in human platelets. Biochem J 222: 157–167.
McNicol A 1993 The effects of genistein on platelet function are due to thromboxane receptor antagonism rather than inhibition of tyrosine kinase. Prostaglandins Leukot Essent Fatty Acids 48: 379–384.
Pollock WK, Rink TJ, Irvine RF 1986 Liberation of [3H]-arachidonic acid and changes in cytosolic free calcium in fura-2-loaded human platelets stimulated by ionomycin and collagen. Biochem J 235: 869–877.
Krishnamurti S, Wheeler-Jones CPD, Kakkar VV 1989 Effect of phorbol ester treatment on receptor-mediated versus G-protein-activator-mediated responses in platelets. Biochem J 262: 77–81.
Houslay MD, Bojanic D, Wilson A 1986 Platelet activating factor and U44069 stimulate GTPase activity in human platelets which is distinct from the regulatory proteins Ns and Ni. Biochem J 234: 737–740.
Shenker A, Goldsmith P, Unson CG, Spiegel AM 1991 The G protein coupled to the thromboxane A2 receptor in human platelets is a member of the novel Gq family. J Biol Chem 266: 9309–9313.
Bleasdale JE, Thakur NR, Gremban RS, Bundy GL, Fitzpatrick FA, Smith RJ, Bunting S 1990 Selective inhibition of receptor-coupled phospholipase C-dependent processes in human platelets and polymorphonuclear neutrophils. J Pharmacol Ther 255: 756–768.
Lages B, Weiss HJ 1988 Impairment of phosphatidylinositol metabolism in a patient with a bleeding disorder associated with defects of initial platelet responses. Thromb Haemost 59: 175–179.
Rao AK, Kowalska MA, Disa J 1989 Impaired cytoplasmic ionized calcium mobilization in inherited platelet secretion defects. Blood 74: 664–672.
Rittenhouse SE, Allen CL 1982 Synergistic activation by collagen and 15-hydroxy-9a,11a-peroxidoprosta- 5:13dienoic acid (PGH2) phosphatidylinositol metabolism and arachidonic acid release in human platelets. J Clin Invest 70: 1216–1224.
McNicol A, Nickolaychuk BR 1995 Inhibition of collagen-induced platelet activation by arachidonyl trifluromethyl ketone. Biochem Pharmacol 50: 1795–1802.
Akkerman JWN, van Willigen G 1996 Platelet activation via trimeric GTP-binding proteins. Haemostasis 26( Suppl 4): 199:20209.
Brass LF, Mannign DR, Cichowski K, Abrams CS 1997 Signaling through G proteins in platelets: to the integrins and beyond. Thromb Haemost 78: 581–589.
Offermanns S, Toombs CF, Simon MI 1997 Defective platelet activation in Gαq-deficient mice. Nature 389: 183–186.
Gabbeta J, Yang X, Kowalska MA, Sun L, Dhanasekaran N, Rao AK 1997 Platelet signal transduction defect with Gα subunit dysfunction and diminished Gαq in a patient with abnormal platelet responses. Proc Natl Acad Sci USA 94: 8750–8755.
Acknowledgements
The authors thank F. Vicente for aid with preparation of the manuscript and the staff of the Labour Suite at the Health Sciences Centre, Winnipeg for aid in collection of cord blood specimens.
Author information
Authors and Affiliations
Additional information
Supported by Grants from the Heart and Stroke Foundation of Canada and the Children's Hospital Foundation of Manitoba, including a Children's Hospital Foundation studentship to T.C.
Rights and permissions
About this article
Cite this article
Israels, S., Cheang, T., Roberston, C. et al. Impaired Signal Transduction in Neonatal Platelets. Pediatr Res 45 (Suppl 5), 687–691 (1999). https://doi.org/10.1203/00006450-199905010-00014
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-199905010-00014
This article is cited by
-
Neonatal thrombocytopenia: Thrombin generation in presence of reduced platelet counts and effects of rFVIIa in cord blood
Scientific Reports (2019)
-
Neonatal platelets: mediators of primary hemostasis in the developing hemostatic system
Pediatric Research (2014)