Abstract
Hypoxic/ischemic (H/I) brain injury is thought to be mediated via the N-methyl-D-aspartate receptor complex, which can be blocked by the magnesium ion. Striatal medium spiny neurons abundantly express N-methyl-D-aspartate receptors and are known to be injured after H/I. Thus, the aim of this study was to investigate the effect of postinjury magnesium treatment on the total number of medium spiny neurons in the striatum after perinatal H/I injury in the rat. Anesthetized postnatal day (PN) 7 rats underwent common carotid artery ligation followed 2 h later by exposure to hypoxia for 1.5 h. Contralateral hemispheres served as controls as did animals exposed to normoxia. Immediately after hypoxia or normoxia, the magnesium groups received s.c. injections of 300 mg/kg MgSO4. Control, hypoxic or normoxic animals received NaCl injections. This continued daily until PN13. Eleven matched-for-weight H/I pups were injected in total. A power calculation showed that 11 pups per treatment group would permit detection of a treatment difference of 32% or more. Animals were killed on PN18, and 40-µm serial sections were cut through each entire striatum. The total number of the predominant medium spiny neurons within each striatum was stereologically determined via the use of an unbiased optical dissector/Cavalieri combination. It was found that postinjury magnesium treatment did not improve neuronal survival by 32% or more in the striatum. The results suggest that magnesium treatment after perinatal H/I damage in the rat is not markedly neuroprotective for striatal medium spiny neurons.
Similar content being viewed by others
Main
Perinatal cerebral hypoxia-ischemia is a major cause of acute perinatal brain injury leading ultimately to neurologic dysfunction manifest as cerebral palsy, mental retardation, and epilepsy (1,2). There is an emerging consensus that excitatory amino acids such as glutamate play a critical role in the pathogenesis of perinatal H/I brain injury (3,4). Most attention has been focused on the NMDA subtype of the glutamate receptor that is coupled to a calcium-permeable cationic channel. NMDA-mediated elevation of intracellular calcium is throught to be pivotal in the initiation of neuronal cell death (5). Both competitive and noncompetitive NMDA-receptor antagonists afford neuroprotection in animal models of brain injury [for a review, see Meldrum (6)]. Neurotoxicity (7) and behavioral side effects (8) limit the therapeutic use, however, of many of these compounds.
Magnesium is a voltage-dependent antagonist of the NMDA receptor (9). Magnesium has been in clinical use for over 60 y in the treatment of preeclampsia in pregnancy (10), and more recently in stroke (11) and infants with birth asphyxia (12). It therefore has an established safety profile. The magnesium ion is involved in many cellular bioenergetic processes (13,14). It may regulate ATP concentrations, and an adequate magnesium concentration is a prerequisite for ATP regeneration after ischemia and reperfusion (15). There is a well documented decrease in intracellular magnesium that persists for up to 5 d after brain injury (16,17). In addition, delayed cell death resulting from calcium overload may occur up until several days after an ischemic insult (18). Thus, a relatively long window of opportunity for interventional therapy may exist after brain injury.
Postinjury therapy is particularly relevant to H/I brain injury in the third trimester because detection of the insult is difficult in utero but much more likely once the fetus is born. Studies suggest that postinjury magnesium administration reduces NMDA-mediated brain injury in perinatal rats (19,20). Thordstein et al. (21) reported that a combination of magnesium and free radical scavengers given immediately after H/I in perinatal rats offered neuroprotection. However, the effect of postinjury treatment with magnesium alone after H/I in perinatal rats is unknown.
This investigation therefore aims to explore the possible benefits of postinjury treatment with MgSO4 on neuronal survival in the striatum after perinatal H/I brain injury. The striatum was chosen because it is one of the main sites of injury after perinatal H/I in both the rat (22–24) and human (25). In humans, this injury is associated with the choreoathetotic movement disorders of cerebral palsy (26). The predominant medium spiny neurons of the striatum were investigated because they are postsynaptic to glutamatergic input from the cerebral cortex (27,28) and are particularly rich in NMDA receptors (29). Total neuronal numbers were determined using some of the available unbiased stereologic techniques. This allowed reliable comparisons to be made between control and injured animals (30,31).
METHODS
Animal treatment. Pregnant albino Sprague-Dawley rats (from the University of Otago Animal Breeding Station) were housed individually with food and water provided ad libitum under stable environmental conditions. All procedures were approved by the Animal Ethics Committee at the University of Otago. On PN7 (day of birth designated as day 0) 28 male pups from seven litters weighing 17.6 ± 1.3 g (mean ± SD) were treated according to a variation of the Rice et al. (22) model of H/I injury during the human third trimester equivalent. Four male pups were paired according to weight per litter. Under ether anesthesia, the right common carotid artery of each pup was ligated with sterile 5-0 surgical silk. Two hours after completion of the last surgery the experimental pups were exposed to an hypoxic environment of humidified 8% oxygen/92% nitrogen for 1.5 h at 37°C. This procedure was repeated six times to yield 24 H/I-treated pups. In addition, the contralateral hypoxic hemisphere was used as a control (32,33). A hypoxic exposure of 1.5 h was chosen for this study, as it causes brain pathology of moderate to severe neuronal loss within the ipsilateral but not the contralateral striatum (23,24), with minimal pup mortality (33).
An additional four, paired male pups from another litter were exposed to a normoxic condition of high purity humidified air. This resulted in 22 H/I right cerebral hemispheres (out of an initial 24, see "Results") and eight control hemispheres (i.e. two hypoxic alone, four ischemic alone, and two normoxic alone hemispheres) being used in this study. After 1.5 h, of either H/I or normoxic exposure, half of the pups from either the H/I or normoxic groups were injected with MgSO4 and half with placebo. The pups were removed from the hypoxic environment and sequentially injected immediately with 300 mg/kg (i.e. 1.60 mM/kg) sterile MgSO4 solution for one of th matched-for-weight pair and sterile NaCl of equivalent molarity and volume for the other animal. The injections were s.c. in the back of the neck at the same time each day from PN7 to 13.
Eleven matched-for-weight H/I pup pairs were injected in total. A power calculation showed that 11 pups per H/I treatment group would give an 80% chance of detecting, at the 5% level for a 2-tailed test, a treatment difference of 32% or more (34). This power calculation was based on a SD of 25% around the mean total number of medium spiny neurons for PN7 H/I rats, with this level of variability being determined from our initial pilot experiments using the same animal model.
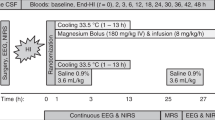
The MgSO4 dosage of 300 mg/kg was chosen to mimic Thordstein et al. (21) (see Introduction). In a study assessing a range of doses, 300 mg/kg was the maximum dose at which the general condition of PN5 rats could be maintained (35). In PN5 mice, a dose of 600 mg/kg produced paralysis (20). We acknowledge, however, that a dose escalation design would have been optimal for the current study. The effect of a lower dosage (150 mg/kg) was not studied due to the time needed for careful quantitation, which is a hallmark of the current study (see "Stereology" and "Discussion"). Our strategy of daily dosing differed from the single dose given by Thordstein et al. (21). Yet, neuroprotection is seen after either daily dosing of 600 mg/kg for adult rats (36) or a single dose of 60-300 mg/kg (20,36,37) and daily dosing permitted a greater opportunity for possible intervention therapy (see Introduction). A previous study has demonstrated that a dose of 300 mg/kg MgSO4 given intraperitoneally results in an immediate and substantial elevation in serum magnesium levels (35), which are still elevated at 2 h postinjection [see Nakajima et al. (35), their Fig. 1].
Temperature measurements were not monitored because 1) previous studies have demonstrated that both brain and core (i.e. rectal) temperatures correlate well for H/I and normoxic rats in the same thermal environment (38,39); 2) brain and rectal temperatures correlate well for H/I rats recovered in the same thermal environment of 31°C after H/I (39); and 3) rectal temperatures are similar for MgSO4- or placebo-treated neonatal rats kept in the same thermal environment (of 24°C) after H/I (40). However, because we did not measure our post-H/I ambient room temperature, it is possible that it differed from 24 or 31°C. Each treatment could therefore have altered each pup's brain and rectal temperature to varying degrees (through physiologic factors like vasodilation) and confounded the results. Neuroprotection from hypothermia is evident (39,41), although this effect is seen only if hypothermia is given during, and not after, H/I. A confounding effect by temperature therefore seems unlikely.
On PN18, the rats were anesthetized with Hypnorm/Hypnovel (3.3 mL/kg) and perfused intracardially with 4% paraformaldehyde and 0.1% glutaraldehyde in 0.1 M phosphate buffer (pH 7.2). The brains were dissected from the skull, partitioned into right and left cerebral hemispheres and hindbrain, weighed, transferred immediately into postfixative (4% paraformaldehyde) for 5 d, and stored in 0.1 M phosphate buffer at 4°C.
Histologic preparation. Each cerebral hemisphere was embedded in toto in glycomethacrylate as previously described (31). Serial, 40-µm coronal sections were cut through the entire striatum on a Reichert-Jung 2050 Supercut Microtome. After a random start, every fourth section from section number 1 to 150 (at this point the striatum was no longer present) was mounted on gelatin-coated slides, stained with 0.002% cresyl violet, dehydrated, and coverslipped as previously described (31).
Stereology. Stereologic quantitation was carried out on every eight 40-µm section of the brain containing the striatum. An optical dissector/Cavalieri combination as described in Oorschot (31) was used to estimate the total numbers of medium spiny neurons in the striatum. The Cavalieri method was used to determine the total reference volume (V). The number of medium spiny neurons per unit volume of the striatum (i.e. the neuronal density or Nv) was determined using the optical dissector method. The boundaries of the striatum (i.e. caudate putamen) and the identification of a medium spiny neuron were defined as in Oorschot (31). An unbiased estimate of the total number of medium spiny neurons, N, was then obtained by N = V × Nv.
Statistical analysis. With data derived from a set of systematically sampled sections from an individual, it is possible to estimate the precision of the estimates made on that individual (31,42,43). These estimates of precision, termed the CE of the estimates, were calculated as described in West and Gundersen (42). All quantitative data were compared using the Mann-Whitney U test.
RESULTS
Two H/I rat pups died in this study yielding an 8% mortality rate. One animal died immediately upon reperfusion and the other as a result of the dam and not H/I. The controls used were H/I pups treated with NaCl and normoxic/ischemic pups treated with either MgSO4 or NaCl. The hypoxic hemisphere also served as an internal control for the H/I hemispheres. Histologically, H/I rats showed gliosis (44), neuronal loss, and infarct zones to varying degrees of severity. This pathology was most marked in the striatum, globus pallidus, cerebral cortex, and thalamus. Neuronal cell death was also evident in the hippocampus and medial habenula (45).
There was a significant 9% (p < 0.05) decrease in the weight of the H/I cerebral hemispheres for both the MgSO4- and NaCl-treated groups in comparison with the controls (Table 1). Total number data revealed that there was a significant difference in the total number of medium spiny neurons in the striatum for the H/I MgSO4-treated group (43% decrease, p < 0.01) and H/I NaCl-treated group (45% decrease, p < 0.01) in comparison with the MgSO4- and NaCl-treated control (C) animals (Table 1). Similarly, there were significant decreases in the V and Nv for both the H/I MgSO4- and H/I NaCl-treated groups in comparison with the controls (p < 0.05 and p < 0.01, respectively, see Table 1). However, these parameters have not been corrected for treatment and/or processing-induced shrinkage and thus strictly speaking should not be compared. It is only the product N that is shrinkage-independent, because both V and Nv were measured in the same sections at the same stage of tissue processing (30).
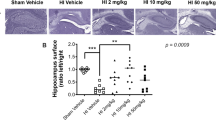
There was no significant difference in the total number of medium spiny neurons within the striatum in the H/I MgSO4-treated animals the H/I NaCl-treated animals (p ≫ versus 0.05) (Fig. 1 and Table 1). The CEs for the precision of the V, Nv, and the total number measurements ranged from 1-4%, 1-6%, and 2-8%, respectively. Because these CEs are less than 10%, reliable estimates were obtained (46).
There appears to be some degree of variability in the total neuronal number between the hypoxic, ischemic, and normoxic conditions for both the MgSO4- and NaCl-treated animals (Fig. 2). This probably reflects the small number of animals used for each specific control condition. When these control values are pooled, the variability is similar to a previous control study on the total number of medium spiny neurons within the rat striatum (31).
DISCUSSION
This study examined the effect of postinjury MgSO4 treatment on striatal neuronal survival after perinatal H/I brain injury in the rat. It was found that MgSO4 treatment did not significantly improve striatal neuronal survival (Table 1, Figs. 1 and 2) by 32% or more compared with placebo. A substantial improvement in striatal neuronal survival is not evident, therefore, after postinjury treatment with MgSO4. A lack of substantial improvement after postinjury treatment with MgSO4 has also been recently reported for hypoxic fetal lambs (47) and hypoxic newborn piglets (48).
These results are in contrast to earlier reports (19–21). One explanation could be that, in the current study, MgSO4 did not reach the striatal synapses in sufficient concentration to inhibit the NMDA receptors and prevent calcium influx. However, protection has been reported in the PN7 and mature rat brain at an equivalent or lower dose of MgSO4, and similar injection route, to the current study (19–21,37). In addition, MgSO4 has been shown to cross the blood-brain barrier and the blood-cerebrospinal fluid barrier in neonatal piglets (49,50) and the blood-brain barrier in fetal rats (51). Furthermore, blood-brain barrier permeability is considered to be greater after H/I brain injury (35). Thus, although the evidence is indirect, the results of the current study are unlikely to be due to inadequate delivery of MgSO4 to the target tissue of interest.
An alternative, and more likely explanation is that neuroprotection by MgSO4 may be evident when the insult is entirely excitotoxic (19,20,36), but may not be evident when NMDA receptor activation is only one of a range of possible deleterious biochemical reactions triggered by immature H/I brain injury (52). Any beneficial effect of NMDA blockade after H/I could have been overwhelmed by the adverse effects of other reactions (48).
The timing of MgSO4 treatment may also be significant. Pretreatment with MgSO4 is protective for hypoxic piglets (53), whereas posttreatment is not protective for hypoxic rat pups (current study), lambs, and piglets (47,48). These findings suggest that glutamate release and NMDA receptor activation may be an initial cause of H/I neuronal injury (which pretreatment, and simultaneous treatment, with magnesium can protect against) (53), but that postinjury magnesium treatment is too late to be markedly protective.
Yet, Thordstein et al. (21) found that posttreatment with MgSO4, in combination with free radical scavengers, ameliorates brain damage after H/I in perinatal rats. It is noteworthy, however, that posttreatment with a scavenger of free radicals alone is protective after H/I in perinatal rats (54). Thus, free radical scavengers may possibly be the key to the postinjury neuroprotection reported by Thordstein et al. (21).
As far as we are aware, the current study is the only investigation that has fully quantified the response of the injured brain to magnesium in terms of the total number of surviving neurons. Previous studies have used indirect measures for determining neuronal survival, namely brain weight (19,21), or qualitative scoring of neuronal injury (20,37,47). Neither of these measures may necessarily reflect the total, or absolute, number of surviving neurons (30). This is because brain weight is likely to reflect glial cell dynamics as well as neuronal cell dynamics postinjury, whereas qualitative scoring of neuronal injury from a few selected sections through the brain structure of interest may not reflect significant volume changes that directly affect the total number of surviving neurons (30,55,56). As an example of the effect of glial cell dynamics, there was only a 9% reduction in the hemisphere weight post-H/I in the current study, compared with a 45% reduction in the total number of medium spiny neurons. Marked post-H/I astrogliosis (44) would contribute to the smaller reduction in hemisphere weight. Thus, the way to be absolutely sure of the presence or absence of neuroprotection is to determine the absolute number of neurons using unbiased stereologic methods as described in the current study.
The statistical power of the current study does not permit the detection, if present, of a smaller (i.e. <32%), but perhaps clinically significant, difference in striatal neuronal loss after postinjury MgSO4 treatment. Moreover, a lack of substantial protection for striatal medium spiny neurons in the current study does not preclude the possibility that MgSO4 might be effective in protecting less vulnerable neurons in the immature H/I brain.
In conclusion, this is the first known study to investigate the neuroprotective effect of magnesium in a model of perinatal H/I brain injury in the rat. This is also the first known study to use unbiased stereology to quantify the response of the injured brain to magnesium. The findings are significant as they suggest that MgSO4 treatment after perinatal H/I damage in the rat is not markedly neuroprotective for striatal medium spiny neurons.
Abbreviations
- NMDA:
-
N-methyl-D-aspartate
- CE:
-
coefficient of error
- H/I:
-
hypoxic/ischemic
- Nv:
-
neuronal density
- PN:
-
postnatal day
References
Blair E, Stanley FJ 1988 Intrapartum asphyxia: a rare cause of cerebral palsy. J Pediatr 112: 515–519
Nelson KB 1988 What proportion of cerebral palsy is related to birth asphyxia? J Pediatr 112: 572–574
McDonald JW, Johnston MV 1990 Physiological and pathophysiological roles of excitatory amino acids during central nervous system development. Brain Res Rev 15: 41–70
Vannucci RC 1990 Experimental biology of cerebral hypoxic-ischemia: relation to perinatal brain damage. Pediatr Res 27: 317–326
Choi DW 1985 Glutamate neurotoxicity in cortical cell culture is calcium dependent. Neurosci Lett 58: 293–297
Meldrum B 1989 Excitotoxicity in ischemia: an overview. In: Ginsberg MD, Dietrich WD (eds) Cerebrovascular Diseases. Raven, New York, pp 47–60.
Olney JW, Labruyere J, Price MT 1989 Pathological changes induced in cerebrocortical neurons by phencyclidine and related drugs. Science 244: 1360–1362
Albers GW, Glodberg MP, Choi DW 1989 N-Methyl-D-aspartate antagonists: ready for clinical trial in brain ischemia? Ann Neurol 25: 398–403
Nowak L, Bergestowski P, Ascher P, Prochiantz A 1984 Magnesium gates glutamate activated channels in mouse central neurons. Nature 307: 462–465
Pritchard JA, Pritchard SA 1975 Standardised treatment of 154 consecutive cases of eclampsia. Am J Obstet Gynecol 123: 543–552
Muir KW, Lees KR 1995 A randomized double-blind placebo-controlled pilot trial of intravenous magnesium sulfate in acute stroke. Stroke 26: 1183–1188
Levene M, Blennow M, Whitelaw A, Hanko E, Fellman V, Hartley R 1995 Acute effects of two different doses of magnesium sulfate in infants with birth asphyxia. Arch Dis Child 73: F174–F177
Ebel H, Gunther T 1980 Magnesium metabolism: a review. J Clin Biochem 182: 257–270
Aikawa JK 1981 Magnesium: Its Biological Significance. CRC Press, Boca Raton, FL, pp 21–29.
Altura BM, Barbour RL, Dowd TL, Wu F, Altura BT, Gupta RK 1993 Low extracellular magnesium induces intracellular free magnesium deficits, ischemia, depletion of high energy phosphates and cardiac failure in intact working rat hearts: a 31P NMR study. Biochim Biophys Acta 1182: 188–193
Tsuda T, Kogure K, Nishioka K, Watanabe T 1991 Mg2+ administered up to 24 hours following reperfusion prevents ischemic damage of the CA1 neurons in the rat hippocampus. Neuroscience 44: 335–341
Vink R, Heath DL, McIntosh TK 1996 Acute and prolonged alterations in brain free magnesium following fluid-percussion-induced brain trauma in rats. J Neurochem 66: 2477–2483
Pulsinelli WA, Brierly JB, Plum F 1982 Temporal profile of neuronal damage in a model of transient forebrain ischemia. Ann Neurol 11: 491–499
McDonald JW, Silverstein FS, Johnston MV 1990 Magnesium reduces N-methyl-D-aspartate (NMDA)-mediated brain injury in perinatal rats. Neurosci Lett 109: 234–238
Marret S, Gressens P, Gadisseux J-F, Evrard P 1995 Prevention by magnesium of excitotoxic neuronal death in the developing brain: an animal model for clinical intervention studies. Dev Med Clin Neurol 37: 473–484
Thordstein M, Bagenholm R, Thiringer K, Kjellmer I 1993 Scavengers of free oxygen radicals in combination with magnesium ameliorate perinatal hypoxic-ischemic brain damage in the rat. Pediatr Res 34: 23–26
Rice JE, Vannucci RC, Brierly JB 1981 The influence of immaturity on hypoxicischemic brain damage in the rat. Ann Neurol 9: 131–141
Johnston MV 1983 Neurotransmitter alterations in a model of perinatal hypoxicischemic brain injury. Ann Neurol 13: 511–518
Towfighi J, Yager JY, Housman C, Vannuci RC 1991 Neuropathology of remote hypoxic-ischemic damage in the immature rat. Acta Neuropathol 81: 578–587
Volpe JJ 1992 Perinatal hypoxic-ischemic brain injury: Overview. In: Fukuyama Y, Suzuki Y, Kamoshita S, Casaer P (eds) Fetal and Perinatal Neurology. Karger, Basel, pp 232–252.
Hill A 1991 Current concepts of hypoxic-ischemic cerebral injury in the term newborn. Pediatr Neurol 7: 317–325
Herrling PL, Morris R, Salt TE 1983 Effects of excitatory amino acids and their antagonists on membrane and action potentials of caudate neurons. J Physiol 339: 207–222
Cherubini E, Herrling PL, Lanfumey L, Stanzione P 1988 Excitatory amino acids in synaptic excitation for rat striatal neurons in vitro. J Physiol 400: 677–690
Landwehrmeyer GB, Standaert DG, Testa CM, Penney JB, Young AB 1995 NMDA receptor subunit mRNA expression by projection neurons and interneurons in rat striatum. J Neurosci 15: 5297–5307
Oorschot DE 1994 Are you using neuronal densities, synaptic densities or neurochemical densities as your definitive data? There is a better way to go. Prog Neurobiol 44: 233–247
Oorschot DE 1996 Total number of neurons in the neostriatal, pallidal, subthalamic, and substantia nigral nuclei of the rat basal ganglia: a stereological study using the Cavalieri and optical dissector methods. J Comp Neurol 366: 580–599
Burke RE, Kent J, Kenyon N, Karanas A 1991 Unilateral hypoxic-ischemic injury in neonatal rat results in a persistent increase in the density of striatal tyrosine hydroxylase immunoperoxidase staining. Dev Brain Res 58: 171–179
Romijn HJ, van Marle J, Janszen AWJW 1993 Permanent increase of the GAD67/synaptophysin ratio in rat cerebral cortex nerve endings as a result of hypoxicischemic encephalopathy sustained in early postnatal life: a confocal laser scanning microscope study. Brain Res 630: 315–329
Cochran WG, Cox GM 1992 Experimental Designs. 2nd Ed. John Wiley & Sons, New York, pp 17–23.
Nakajima W, Ishida A, Takada G 1997 Magnesium attenuates a striatal dopamine increase induced by anoxia in the neonatal rat brain: an in vivo microdialysis study. Pediatr Res 41: 809–814
Wolf G, Keilhoff G, Fischer S, Hass, P 1990 Subcutaneously applied magnesium protects reliably against quinolinate-induced N-methyl-D-aspartate (NMDA)-mediated neurodegeneration and convulsions in rats: are there therapeutical implications? Neurosci Lett 117: 207–211
Wolf G, Fischer S, Hass P, Abicht K, Keilhoff G 1991 Magnesium sulphate subcutaneously injected protects against kainate-induced convulsions and neurodegeneration: an in vivo study on the rat hippocampus. Neuroscience 43: 31–34
Wasterlain CG, Adams LM, Schwartz PH, Hattori H, Sofia RD, Wichmann JK 1993 Posthypoxic treatment with felbamate is neuroprotective in a rat model of hypoxia-ischemia. Neurology 43: 2303–2310
Yager J, Towfighi J, Vannucci RC 1993 Influence of mild hypothermia on hypoxicischemic brain damage in the immature rat. Pediatr Res 34: 525–529
Gilland E, Bona E, Levene M, Hagberg H 1997 Magnesium and the N-methyl-D-aspartate receptor antagonist dizocilpine maleate neither increase glucose use nor induce a 72-kilodalton heat shock protein expression in the immature rat brain. Pediatr Res 42: 472–477
Towfighi J, Housman C, Heitjan DF, Vannucci RC, Yager JY 1994 The effect of focal cerebral cooling on perinatal hypoxic-ischemic brain damage. Acta Neuropathol 87: 598–604
West MJ, Gundersen HJG 1990 Unbiased stereological estimation of the number of neurons in the human hippocampus. J Comp Neurol 296: 1–22
Bonthius DJ, Bonthius NE, Napper RMA, West JR 1992 Early postnatal alcohol exposure acutely and permanently reduces the number of granule cells and mitral cells in the olfactory bulb: a stereological study. J Comp Neurol 324: 557–566
Oorschot DE, Galvin KA 1995 The effect of hypoxic-ischemic brain injury on the total number of astrocytes in the rat basal ganglia: is there hyperplasia? Proc Aust Neurosci Soc 6: 234
Oorschot DE, Mexted MJ, Rangi F, Scarr E 1997 Fos expression after immature hypoxic-ischemic brain injury. Int J Neurosci 94: 136
Gundersen HJG, Jensen EB 1987 The efficiency of systematic sampling in stereology and its prediction. J Microsc 147: 229–263
de Haan HH, Gunn AJ, Williams CE, Heymann MA, Gluckman PD 1997 Magnesium sulfate therapy during asphyxia in near-term fetal lambs does not compromise the fetus but does not reduce cerebral injury. Am J Obstet Gynecol 176: 18–27
Penrice J, Amess PN, Punwani S, Wylezinska M, Tyszczuk L, D'Souza P, Edwards AD, Cady EB, Wyatt JS, Reynolds EOR 1997 Magnesium sulfate after transient hypoxia-ischemia fails to prevent delayed cerebral energy failure in the newborn piglet. Pediatr Res 41: 443–447
Rivera LI, Gootman PM, Lin RH, Gootman N 1991 Effects of elevated plasma magnesium concentration on cerebrospinal fluid levels of magnesium in neonatal swine. Proc Soc Exp Biol Med 197: 98–101
Gee JB II, Corbett RJT, Perlman JM, Garcia D, Silmon S, Laptook AR 1996 Magnesium (Mg) increases to comparable levels in brain extracellular fluid (ECF) in newborn (NEW) and older (OLD) swine during systemic administration of magnesium sulfate. Pediatr Res 39: 374A
Hallak M, Cotton DB 1993 Transfer of maternally administered magnesium sulfate into fetal compartment of the rat: assessment of amniotic fluid, blood and brain concentrations. Am J Obstet Gynecol 169: 427–431
Volpe JJ 1995 Neurology of the Newborn. 3rd Ed. WB Saunders, Philadelphia, pp 228–237.
Hoffman DJ, Marro PJ, McGowan JE, Mishra OP, Delivoria-Popadopoulos M 1994 Protective effect of MgSO4 infusion on NMDA receptor binding characteristics during cerebral cortical hypoxia in the newborn piglet. Brain Res 644: 144–149
Palmer C, Towfighi J, Roberts RL, Heitjan DF 1993 Allopurinol administered after inducing hypoxia-ischemia reduces brain injury in 7-day-old rats. Pediatr Res 33: 405–411
Gundersen HJG 1986 Stereology of arbitrary particles. A review of unbiased number and size estimators and the presentation of some new ones, in memory of William R. Thompson. J Microsc 143: 3–45
Swaab DF, Uylings HBM 1987 Density measures: parameters to avoid. Neurobiol Aging 8: 574–576
Author information
Authors and Affiliations
Additional information
Supported by the Dean of the Otago Medical School's Health Research Council Fund (D.E.O.) and a University of Otago Postgraduate Scholarship (K.A.G.).
Rights and permissions
About this article
Cite this article
Galvin, K., Oorschot, D. Postinjury Magnesium Sulfate Treatment Is Not Markedly Neuroprotective for Striatal Medium Spiny Neurons after Perinatal Hypoxia/Ischemia in the Rat. Pediatr Res 44, 740–745 (1998). https://doi.org/10.1203/00006450-199811000-00017
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-199811000-00017
This article is cited by
-
Nonoperative management of spasticity in children
Child's Nervous System (2007)