Abstract
Adrenergic input influences renal cell replication/differentiation and the development of excretory function. Kidney cells make adrenoceptors before the arrival of the majority of nerve terminals, and the current study examines whether thyroid hormone plays a role in receptor development. Propylthiouracil(PTU) was given to pregnant and neonatal rats from gestational d 17 through postnatal d 5, a treatment that obtunds thyroid hormone levels throughout the first 2-3 wk postpartum. The PTU group showed significant deficits in the number of α1-receptors, and values resolved to normal in parallel with hormone level recovery. The effects were not secondary to alterations in cell differentiation or growth, as the period of receptor abnormalities did not correspond to that of growth inhibition. Similarly, the effects were selective for the α1-receptor, as no comparable effects were seen for total membrane protein or for α2-receptors. The role of thyroid hormone in α1-receptor ontogeny involved a critical developmental window; later in development neither treatment with PTU nor with large doses of thyroid hormone had any impact on α1-receptors. Studies of mRNAs encoding the α1-receptor subtypes indicated that hypothyroidism targets the α1a-subtype, which has been implicated in the transduction of neurotrophic signals; α1a-receptor mRNA also showed the largest proportional developmental increase compared with those encoding other α1-subtypes. Accordingly, thyroid hormone is likely to set the stage for the subsequent trophic control of renal development by neural input, and hypothyroidism during this critical window can be expected to result in abnormal renal functional development and increased perinatal risk.
Similar content being viewed by others
Main
In the adult, sympathetic nerves play an important role in the control of renal hemodynamics, renin secretion, and electrolyte and water excretion. During development, however, adrenergic activity is also essential for programming cell development and for establishing the set point for future reactivity of the kidney to sympathetic stimulation(1–6). Although the newborn rat kidney has only minimal concentrations of norepinephrine(7), lesioning of sympathetic nerves at this stage interferes with the acquisition of cells, with the establishment of renal responses to diverse neuronal and hormonal trophic stimuli, and with the ontogeny of urine concentrating mechanisms and water reabsorption(2, 8–13). Although some of the denervation-induced defects in basal excretory function are eventually compensated later in life(13), the concentrating mechanisms fail to develop full function, so that factors such as excessive salt intake result in death(12); in addition, the defective renal trophic responses are apparently permanent(10). Sympathetic nerves can supply multiple factors to influence target organ cell differentiation and function, but the most important role is likely provided by the neurotransmitter, norepinephrine, because the same defects can be elicited with neonatal brain lesions that leave the peripheral sympathetic nerves intact but obturate impulse activity(2, 8, 12).
The participation of norepinephrine as a trophic signal for developing cells in the kidney requires not only the presence of sympathetic nerve terminals but also of the appropriate adrenergic receptor populations. Specifically, if early neonatal sympathetic input is so critical to cell development and to the ontogeny of excretory function, cells must acquire the proper receptor populations in advance of the arrival of the majority of nerve terminals. Therefore, it is critical to assess how the development of adrenergic receptor proteins is controlled in the newborn. There are two likely mechanisms: trophic control by sympathetic nerves themselves or by hormonal factors. The first hypothesis, that sympathetic nerves themselves evoke receptor acquisition, is unlikely to be correct. Receptors are present on target cells well before the arrival of the majority of nerve terminals, and denervation does not blunt receptor development(2, 9, 14–16). Based on work done in the heart, hormonal control of receptor ontogeny would be a more likely possibility, as both thyroid and steroid hormones have been shown to promote cardiac β-adrenergic receptor development(17–21) and, to a lesser extent, that of α1-receptors(22). Nevertheless, it is clear that receptor regulation in the developing kidney follows a different scheme, as neither thyroid nor steroid hormones influenceβ-receptor ontogeny in this tissue(19, 23–26). However, there is virtually no information about hormonal regulation of α-adrenergic receptors in developing kidney, and it is these receptors that are most likely to mediate positive trophic influences on cell replication and differentiation(27–29).
The current study examines the role of thyroid hormone in the ontogeny of renal α-adrenergic receptors in the neonatal rat. We have used well established models of perinatal hypothyroidism and neonatal hypo- and hyperthyroidism elicited by PTU or T3 treatments(17–20, 23, 30–33). To characterize the critical period for thyroid hormone's effects, we have contrasted the effects of PTU given during the immediate perinatal period (gestational d 17 through postnatal d 5) with PTU or T3 given on postnatal d 11 through 15, after the ontogenetic rise of thyroid hormone levels (1st postnatal wk)(20, 30) and during the establishment of sympathetic innervation (2nd to 4th wk)(7). If there is a specific developmental role for thyroid hormone in adrenergic receptor ontogeny, such effects should be limited to the earlier period. Contrasting the effects of hypo- or hyperthyroidism on the two classes of α-adrenergic receptors, theα1- and α2-receptors, enables a distinction to be made between specific promotion or repression of receptor genes compared with the generalized effects of thyroid hormones on cell differentiation and growth(22). Because both receptor classes increase in concentration with renal cell development(14, 16), effects exerted on differentation and growth will be reflected in parallel actions on both classes, whereas specific effects exerted on individual genes will show separable actions on α1- orα2-receptors. Finally, we determined whether effects exerted onα1-receptor protein, as exemplified by ligand binding, reflected ubiquitous effects on the mRNAs encoding the multiple α1-subtypes or rather indicated a targeting of a specific subtype.
METHODS
Animals and treatments. Timed pregnant Sprague-Dawley rats(Zivic-Miller Laboratories, Allison Park, PA) were shipped by climate-controlled truck (transit time, 12 h) and were housed individually, with a 12-h light-dark cycle and free access to food and water. After birth, all pups within a given treatment group were randomized and redistributed to the nursing dams with a litter size of 10-12 pups, and the randomization procedure was repeated at intervals of 2-3 d. For each experiment, animals of both sexes were selected from several different cages. Runts, defined as those whose body weights were more than 2 SD below those of their littermates, were culled. Weaning occurred at 23 d.
To achieve perinatal hypothyroidism, pregnant rats were given daily s.c. injections of 20 mg/kg PTU (Sigma Chemical Co., St. Louis, MO) dissolved in 0.1 N NaOH and titrated with HCl to a final pH of 9.3, starting at gestational d 17 (5 d before birth) and continued through postnatal d 5; pups also received PTU from postnatal d 1 through 5. With this regimen, thyroid hormone levels are severely reduced at birth, begin to recover at postnatal d 10, and are within 75% of normal levels by d 20(30). To achieve hypothyroidism during a later developmental period, the same treatments were begun on postnatal d 11 and continued through postnatal d 15(33). Finally, a third group of animals was rendered hyperthyroid during the later developmental period by administration of daily s.c. injections of 0.1 mg/kg T3 (Sigma Chemical Co.), beginning on postnatal d 11 and continued through postnatal d 15(18, 34). This dose regimen is effective for eliciting alterations of peripheral noradrenergic function or for replacement therapy in neonatal hypothyroidism(18, 20, 30, 32, 34) and causes minimal growth impairment; hormone levels return approximately to normal within 3 d of the end of treatment(30). Control dams and pups for each treatment regimen received equivalent volumes of alkaline saline vehicle (1 mL/kg) on the same schedules.
All experimental treatments and protocols involving live animals were approved by the Institutional Animal Care and Use Committee of Duke University Medical Center and conformed to guidelines set out in the NIH Guide for the Care and Use of Laboratory Animals.
Membrane preparation. Animals were weighed and decapitated, and kidneys were rapidly dissected, weighed, flattened between two sheets of aluminum foil, frozen immediately in liquid nitrogen, and stored at -45°C; with these conditions, preliminary experiments showed no deterioration of receptor binding capabilities. Tissues were thawed and homogenized(Polytron, Brinkmann Instruments, Westbury, NY) in 39 volumes of ice-cold buffer containing 145 mM NaCl, 2 mM MgCl2, 20 mM Tris (pH 7.5) and were filtered through several layers of cheesecloth to remove connective tissue. The homogenates were then sedimented at 40 000 × g for 15 min, the supernatant solution was discarded, and the pellets were washed twice by resuspension (Polytron) in homogenization buffer followed by resedimentation. The final pellet was dispersed with a smooth glass homogenizer fitted with a Teflon pestle, in 4 volumes (based on original wet weight of tissue) of 250 mM sucrose, 2 mM MgCl2, 50 mM Tris (pH 7.5), and the suspension was then used for studies of ligand binding and for protein analysis(35). The properties of this membrane preparation in developing rat kidney have been described in detail previously(14, 16).
Receptor binding assays. Receptor binding capabilities were assessed by methods described in earlier publications(16, 36–38). The overall strategy was to examine binding in preparations from every animal at a single ligand concentration below full saturation of the binding site. The selection of a single concentration for the receptor analysis enables the detection of drug-induced changes in either Kd or Bmax but does not permit distinction between the two possible mechanisms. At a point of robust alteration caused by treatment, Scatchard analyses were done to identify whether binding alterations resulted from changes in Kd or Bmax. This strategy was necessitated by the requirement to measure binding of two different receptor types in six different treatment groups, each involving up to nine different time points and 12 individual animals in each treatment at each time point (a total of over 1000 separate tissue determinations).
Radioligands were incubated with the tissue membrane preparation in a total volume of 250 μL. Incubations were stopped by dilution with 3 mL of ice-cold buffer, and the labeled membranes were trapped by rapid vacuum filtration onto Whatman GF/C filters, which were then washed with additional buffer and counted by liquid scintillation spectrometry.α1-Receptor binding was determined with 2.2 nM[3H]prazosin (DuPont NEN, Boston, MA; specific activity, 74 Ci/mmol). Duplicate aliquots of membrane preparation (containing up to 0.18 mg of protein) were incubated with radioligand in 10 mM MgCl2, 50 mM Tris (pH 7.5) on ice for 50 min. The subsequent Scatchard analysis covered a[3H]prazosin concentration range from 0.1 to 3 nM.α2-Receptor binding was evaluated similarly, using 2.5 nM[3H]rauwolscine (DuPont NEN; specific activity 79 Ci/mmol), incubated for 20 min at room temperature. For both receptor types, nonspecific binding was determined in the presence of an excess concentration (10 μM) of phentolamine (Sigma Chemical Co.) and was typically 15-30% of the total; before postnatal d 10, when receptor binding was lowest, nonspecific binding was higher (40-50% of total binding).
Because adrenergic receptors are integral membrane proteins, increases or decreases in cell size can influence the numbers of these molecules exclusive of any age- or drug-induced effects on the specific development of these proteins. Accordingly, measurements of receptor binding were determined both on the basis of milligrams of membrane protein and on the basis of grams of tissue. Because the objective of this study was to determine whether there are specific alterations in receptors over and above effects of hypo- or hyperthyroidism on all membrane constituents, values corrected for membrane protein are the relevant values and are presented in the“Results.” None of the treatments caused significant changes in membrane protein concentrations (data not shown), so that conclusions were the same with either measure of receptor binding.
Preparation of RNA, cDNA constructs and probes. Tissues were harvested rapidly, immersed in liquid nitrogen, and stored at -45 °C. Total RNA was extracted from rat tissues using RNazol (Teltest Inc., Friendswood, TX). Each sample was quantitated spectrophotometrically at 260 and 280 nm and stored at -70 °C as an ethanol precipitate for later use.
The rat α1a-receptor cDNA construct, obtained from Dr. Carina Tan (Merck, Rahway, NJ), consists of a 299-bp (XbaI/XbaI) fragment inserted into a SpeI/XbaI site in pGEM-9zf(Promega Corp., Madison, WI) corresponding to nucleotides 1133-1432 (accession no. U13368) of the receptor cDNA(39). Ratα1b- and α1d-receptor cDNA constructs were obtained from Dr. James E. Faber (University of North Carolina School of Medicine, Chapel Hill, NC). The α1b construct consists of a 306-bp(BamHI/PstI) fragment in pGEM-3Z (Promega) and is identical to the reported cDNA sequence(40) from nucleotides 469-775 (accession no. M60655). The α1d cDNA construct consists of a 276-bp (BglI/BamHI) fragment in pGEM-4Z (Promega) corresponding to nucleotides 1104-1380 (accession no. L31771) of the previously reported cloned rat cDNA(40). The rat β-actin cDNA construct consists of a 126-bp(KpnI/EcoRI) insert in pTRIPLEscript vector (Ambion, Austin, TX) corresponding to nucleotides 2682-2779 (accession no. J00691)(41). Linearized cDNA constructs were used to synthesize high specific activity, radiolabeled, antisense RNA probes, using T7 RNA polymerase and [α-32P]CTP (DuPont NEN) as described previously(42).
RNase protection assays. Hybridization of gel-purified RNA probes to total cellular rat RNA was performed as modified from previously reported methods(43). In brief, 20 μg of total RNA were hybridized simultaneously with 300 000 cpm of gel-purified receptor riboprobe and 150 000 cpm of β-actin riboprobe, for 16 h at 48 °C. RNase A (5 μg/mL) and T1 (100 units/mL) were added to each sample and incubated at 37 °C for 30 min. After digestion, RNA samples were precipitated with ethanol and resuspended in gel loading buffer, heated to 95°C for 4 min, and fractionated on a denaturing 6% polyacrylamide-8.3 M urea gel (National Diagnostics, Atlanta, GA) at 70 W for 2 h. Gels were dried on filter paper and quantitated on a PhosphorImager (Molecular Dynamics, Sunnyvale, CA) using an exposure time of 72 h. All values were normalized to the reading of the corresponding β-actin band and corrected for the different length of each probe. In addition, to enable reliable comparisons to be made between receptor subtypes and across ages and treatments, samples to be compared with each other were always run on the same gel.
Data analysis. Data are reported as means and SE. For each variable, initial statistical comparisons were carried out by ANOVA with factors of treatment and age; data were logtransformed whenever variance was heterogeneous. When the initial test indicated an effect of treatment or an interaction of treatment × age, post hoc comparisons were carried out using Fisher's protected least significant difference. Effects of T3 and PTU treatment on body and tissue weights were evaluated similarly using two-factor ANOVA and Fisher's protected least significant difference. Significance for all tests was assumed at the level p< 0.05. For convenience, some data are presented as percentages of control values, or as control developmental curves pooled across the three different control sets. However, statistical analyses were conducted only on unmanipulated values, and each treatment group was compared only to its matched control cohort.
Scatchard plots were fitted by linear regression analysis. Each set of Scatchard determinations was conducted pairwise; that is, a determination from membrane preparations from control animals of the appropriate cohort was always run concurrently with the determination from the treated group.
RESULTS
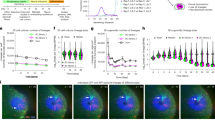
Receptor binding capabilities in kidneys of control animals across all three cohorts displayed a marked increase between birth and the end of the 5th postnatal wk (Fig. 1). Both α1- andα2-receptors were low immediately after birth, but the subsequent rise in α1-receptors was much larger than forα2-receptors (4-5-fold compared with 2-fold). The greatest rate of rise of α1-receptors was during the first 10 d postpartum, corresponding to the ontogenetic increase in thyroid hormone levels(20, 30); in contrast, the rate of rise in receptor binding was lower during the 2nd to 4th wk, the period of most rapid sympathetic neuronal ingrowth(7). The pattern in the kidney of an ontogenetic increase in receptor binding for both theα1 and α2 classes differs substantially from that in heart or liver, where α2-receptors are higher in the fetus and neonate and decline with the rise in hormone levels and the ingrowth of sympathetic neurons(33, 36, 38). The scatter of values for receptor binding with age is indicative of some variability from cohort to cohort, partially reflecting the use of a single ligand concentration that is sensitive both to changes in receptor number and affinity. Accordingly, data shown below for the effects of PTU and T3 are given along with their specifically matched control cohorts. Similarly, because the single ligand concentration and the receptor Kd differ for the α1 and α2 ligands used, the current data alone do not permit comparisons of the absolute numbers ofα1 compared with α2 receptors. There are discrepancies in the literature as to which receptor class predominates in the adult kidney(16, 44, 45), partially reflecting differing Kd values among laboratories. In the current report, the effects of PTU and T3 thus are considered relative to the appropriate control values, but are not compared with each other in absolute terms.
If endogenous thyroid hormone plays a role in the maximal rate of rise ofα1-receptors, then administering PTU from gestational d 17 through postnatal d 5 should affect receptor development, as this treatment severely attenuates thyroid hormone levels through the first 2 wk postpartum(20, 30). Perinatal PTU treatment significantly reduced α1-receptor binding overall (Fig. 2, top left panel) and the effect was distinctly age-dependent (significant interaction of treatment × age). Accordingly, values were divided into those obtained during the period of maximal hypothyroidism, i.e. through postnatal d 18, and after reestablishment of thyroid hormone levels, d 23-35(20, 30). With this subdivision, it was evident that reductions in α1-receptor binding were limited to the early, hypothyroid period. Additionally, the detrimental effects of perinatal PTU treatment were restricted to the α1-receptors, asα2-receptor binding did not show significant decrements and actually displayed a slight, statistically significant overall increase (Fig. 2, top right panel). The decrease in binding forα1-receptors was statistically distinguishable from the increase in that for α2-receptors (three-factor ANOVA, interaction of treatment × receptor type, p < 0.0001; interaction of treatment × receptor type × age, p < 0.003). Although the PTU treatment also produced significant, age-dependent retardation of body and kidney growth (Fig. 2, bottom panels), the largest deficits in growth occurred after the third postnatal week, when receptor binding had returned to normal. Perinatal PTU treatment had no significant effect on litter size, sex ratio, or neonatal survival (data not shown).
Effects of PTU treatment from gestational day(G) 17 through postnatal day (PN) 5 on α-adrenergic receptor binding and on body and kidney weights. Data represent means and standard errors obtained from 13-16 membrane preparations in each group at each age. ANOVA for each variable is shown within the panels. Asterisks denote individual ages at which the PTU group differs significantly from controls. For α1-receptors, ANOVA is also shown for two age brackets, corresponding to the period in which thyroid hormone levels are suppressed by PTU (PN2-18) and the period after recovery (PN23-35).
To determine whether the deficit in α1-receptor binding in the perinatal PTU group reflected a change in receptor number or affinity, Scatchard determinations were carried out on postnatal d 14(Fig. 3), a point at which robust differences were found in the single ligand concentration studies. The reduction in binding caused by PTU treatment reflected a change in number and not in affinity, as evidenced by reduced Bmax without a change in Kd.
If the role of thyroid hormone in α-receptor development is restricted to the period of rapid rise in hormone levels before the onset of sympathetic innervation, then PTU should have no effect when administered later. When PTU was given from postnatal d 11 through 15, there were no significant effects on either α1- or α2-receptor binding (Fig. 4, top panels). Although there were statistically significant effects of this later PTU treatment on body weight, the effects were much smaller than those of perinatal treatment, and kidney weights showed little or no effect (Fig. 4, bottom panels).
Effects of PTU treatment from postnatal day(PN) 11 through 15 on α-adrenergic receptor binding and on body and kidney weights. ANOVA for each variable is shown within the panels. Data represent means and standard errors obtained from 11-14 determinations in each group at each age. Asterisk denotes individual age at which the PTU group differs significantly from controls, determined only for the variable showing a significant effect by ANOVA (body weight).
In addition, to determine whether there was any reactivity ofα-receptor binding capabilities to thyroid hormone during the later developmental period, we administered 0.1 mg/kg T3 on postnatal d 11 through 15, a dose sufficient to raise hormone levels severalfold above normal and to suppress endogenous thyroid hormone production(30). There was no effect on α1-receptors, but in this case, α2-receptors were affected (Fig. 5, top panels). Because of the significant interaction of treatment × age for the effects of T3 onα2-receptors, we subdivided the data into the period of elevated hormone levels (d 12 and 15) and subnormal to normal levels (d 18 through 29).α2-Receptor binding was reduced during the period of elevated hormone levels and enhanced during the subsequent period. The presence of changes in α2-receptor binding was distinguishable from the absence of such changes in α1-receptors (three-factor ANOVA, interaction of treatment × receptor type × age, p < 0.0001). These changes occurred without significant effects on body weight and with only small overall elevations in kidney weight (Fig. 5, bottom panels).
Effects of T3 treatment from postnatal day(PN) 11 through 15 on α-adrenergic receptor binding and on body and kidney weights. ANOVA for each variable is shown within the panels. Data represent means and standard errors obtained from 12-13 membrane preparations in each group at each age. Asterisks denote individual ages at which the T3 group differs significantly from controls, determined only for the variables showing a significant effect by ANOVA(α2-receptor binding, body weight). Forα2-receptors, ANOVA is also shown for two age brackets, corresponding to the period in which T3 levels are elevated (PN12-15) and the period after return to subnormal or normal levels (PN18-29).
We also compared 10-d-old kidney to adult kidney for levels of the mRNAs encoding the three α1-receptor genes, α1a,α1b, and α1d, as defined with the most current nomenclature(46). Representative lanes for separation of the protected mRNAs corresponding to each of the receptor subtypes appear in Figure 6. In each case, the band for the appropriate receptor message was readily discernible, as was a distinctly higher mRNA level in adult compared with neonatal kidney. In keeping with earlier findings(47), the α1a band was a doublet, representing mRNAs differing by only 1 or 2 nucleotides. The doublet can be attributed to either partial digestion of the end of the RNA-RNA hybrid or to protection of nearly identical but separate fragments due to variation in probe length brought about by premature termination of the in vitro transcription process. It is unlikely that the doublet represents two distinct but highly homologous subtypes (differing in only 1 or 2 nucleotides), as in our hands, simply changing the type of RNase used in the assay can result in a single band but does not change the quantitative distribution in rat or human tissues(47). Indeed, this type of multiple banding is seen even in cells stably transfected with a single receptor gene(47).
Representative gel lanes for determination of mRNAs encoding the three α-receptor subtypes in kidneys from adult and postnatal day (PN) 10 control rats. Entire lanes are shown, with expanded views of the relevant bands (arrows) corresponding to hybridized receptor probe. Note lower levels of α1a- andα1b-receptor mRNA in neonatal vs adult rats and predominance of these two subtypes over α1d-receptor mRNA. Although the β-actin bands are much darker than the corresponding receptor bands, the actual PhosphorImager readings for β-actin were within the linear range.
The mRNA bands were quantitated by phosphorimaging (Fig. 7, top panel). In keeping with earlier results(47, 48), adult kidney exhibited mRNAs encoding all three subtypes with the rank order, α1a > α1b>> α1d. Compared with the adult, 10-d-old kidney showed much lower mRNA levels for the α1a and α1b subtypes but not for the α1d subtype. Thus, the 3-fold increase in receptor binding that occurs between d 10 and adulthood is most likely accounted for by increases in either gene transcription or mRNA stability(49) of two of the subtypes. As a corollary, the preference for α1a and α1b compared withα1d is much less prominent in the neonatal kidney than in the adult.
mRNAs encoding the different α-receptor subtypes in adult kidney and in kidneys of 10-d-old rats from control and early PTU treatment groups (treatment from gestational d 17 through postnatal d 5). Data represent means and SE obtained from four preparations in each group; relative units are the phosphorimage density relative to the that of the β-actin band in the same lane. ANOVA is shown within the panels, and asterisks denote individual subtypes for which differences are present for neonatal vs adult rats (top panel) and for control vs PTU-treated neonates (bottom panel).
Applying the same approach to animals treated with PTU from gestational d 17 through postnatal d 5, hypothyroidism interfered with the mRNA of only one of the three genes, namely that encoding the α1a-receptor (Fig. 7, bottom panel). The lack of significant effect of PTU on α1b-receptor mRNA was statistically distinguishable from the presence of significant differences for the α1a-receptor mRNA(treatment × subtype interaction, p < 0.02). For theα1d-receptor mRNA, however, the absence of significant differences with PTU treatment needs to be interpreted with caution, as the values were not distinguishable from the change elicited inα1a-receptor mRNA (treatment × subtype interaction, NS); in this case, the basal level was sufficiently low that further decreases attributable to PTU might not be detectable even if they were of the same magnitude as those for the α1a-receptor mRNA.
DISCUSSION
Our results indicate that thyroid hormone plays a significant role in the ontogeny of renal α1-receptors during a critical developmental period. Perinatal PTU treatment obtunded the developmental rise ofα1-receptor binding during the first 2-3 wk, corresponding to the period of maximal hypothyroidism(20, 30), and receptor binding returned to normal coincidentally with the recovery of thyroid hormone. As there is only one ligand binding site per receptor molecule, and as perinatal PTU evoked changes in receptor number and not affinity, thyroid status is affecting the amount of receptor protein present in renal cell membranes. The existence of a critical period for thyroid control of α1-receptor development was demonstrated by the absence of significant effects when PTU was administered on postnatal d 11-15, just after the ontogenetic rise in thyroid hormone levels and during the arrival of the majority of sympathetic nerve terminals(7, 20, 30). Indeed, after this point, even massive doses of thyroid hormone (T3 given on postnatal d 11-15) failed to alter α1-receptors.
Because perinatal hypothyroidism also affects growth and cell differentiation, it is essential to establish whether the effect onα1-receptors is simply an epiphenomenon of these general developmental effects as opposed to specific hormonal control of receptor ontogeny. In the first case, it would be expected thatα2-receptor development and total membrane protein concentration would also be blunted. However, we did not find any decrement inα2-receptor binding with perinatal PTU treatment (in fact there was a slight increase); the membrane protein concentration was unaffected(data not shown). Furthermore, the greatest changes in receptor binding were seen in the period in which body and kidney growth deficits were minimal; instead, the shortfalls in weight became most notable after receptor binding had returned to normal. Thus, the role of thyroid hormone in the specific control of renal α1-receptor development is distinct from its role in general cell differentiation and growth.
Despite the deficits in α1-receptors caused by perinatal PTU treatment, hypothyroidism did not prevent the ontogenetic rise in receptors completely. There are two possible explanations for this result: the role of thyroid hormone may be superimposed on a basic ontogenetic pattern that is either an autochthonous property of renal cells or is controlled primarily by other factors, or alternatively, thyroid hormone may have a relatively large impact on just one α1-receptor subtype. Recent studies using molecular cloning have identified three different α1-receptor sequences(39, 40, 50) with subtypes regulated individually by stimuli such as hypoxia or trophic factors(51, 52). Although there is no prior information about individual α-receptor subtype regulation by thyroid hormone, these hormones are known to control the β-receptor subtype differentially(53–55). In the developing heart, theβ1-receptor subtype shows an absolute requirement for thyroid hormone so that perinatal PTU treatment leads to complete arrest of receptor ontogeny during the period of subnormal thyroid hormone levels(20, 23); in the liver, whereβ2-receptors predominate, no such effects are seen(33). Accordingly, we examined both the developmental differences in mRNAs encoding the α1-receptor subtypes as well as the effects of perinatal PTU treatment. Both the adult and neonatal rat kidney were found to contain predominantly the α1a and α1b subtypes and much less α1d, in keeping with earlier work(47, 48, 56). However, the preference ratios were substantially different with age, with only a three-fold range in the neonate compared with a 10-fold range in the adult. Thus, the elaboration of separate receptor subtypes is a developmentally distinct event involving preferential increases in mRNAs for α1a > α1b>> α1d. It is of equal interest that PTU treatment interfered almost exclusively with the α1a-receptor subtype. In myocytes, this subtype has recently been shown to be regulated by mechanisms distinct from those of the other subtypes and is postulated to be specifically responsible for transduction of neurotrophic responses(57). Our finding that this subtype is specifically dependent on the ontogenetic rise of thyroid hormone that occurs in the first postnatal week(30) thus provides a necessary link between the early development of adrenergic receptors before the ingrowth of the majority of sympathetic nerve terminals, and the subsequent control of target cell differentiation and ultimately of renal excretory function by sympathetic input(2, 8–13).
Because readings for mRNAs encoding the α-receptor subtypes were corrected for the amount of β-actin mRNA, it is important to note that thyroid hormone can potentially affect β-actin gene mRNA levels(58). It is unlikely, however, that such effects account for the changes seen here in receptor mRNA, as a change in the“denominator” term for the mRNA comparisons would cause parallel alterations in all three subtypes. Instead, we found a specific targeting of the α1a mRNA. Furthermore, because β-actin is keyed to general structural development, gene effects that are indexed to β-actin would always be reflected in the tissue growth pattern, which in this case was clearly dissociated from effects on α-receptors. Our results do not rule out the possibility, however, that the targeting of α1a-receptors involves selective effects on kidney subregions or specific cell types. The different α-receptor subtypes do show distinct cortical-medullary differences in their distribution and may be concentrated in different cell populations(48, 59). It would therefore be worthwhile to conduct studies of the regional development of α-receptors and mRNA, as well as the effects of thyroid deficiency on the numbers and sizes of cells containing each receptor subtype. If the effects of thyroid insufficiency during the critical developmental period are indeed concentrated on one region or cell type, then the deficits in receptor mRNA and receptor binding are likely to be much larger than when the effects are “washed out” by noninvolved regions or cells as determined here in whole kidney.
Although comparable information about thyroid hormone's effects on specificα1-receptor subtypes is not available for other tissues, the same differential effects on individual subtypes may be operating to produce apparent tissue selectivity. In the heart, α1-receptors show a similar profile of sensitivity to perinatal PTU, and of critical period closure by the 2nd wk, just as found here for the kidney(22). However, the liver is much less affected(33). In comparing the effects of PTU on other receptor populations, it is apparent that development of β-receptors andα2-receptors is particularly sensitive to thyroid status in the heart compared with other tissues(19, 23, 33). These differences may all reflect differential control of specific receptor subtypes whose proportions differ in each tissue. Alternatively, because the effects of thyroid hormone involve a specific developmental window, it is also possible that each tissue has a defined period in which receptor development is responsive to thyroid hormone. It will thus be necessary to evaluate the subtypes at earlier stages of development to determine which of these hypotheses is correct. We and others have found that some adrenergic receptor subtypes are especially abundant in the fetus(28, 36, 38, 60); thyroid hormone regulation of receptor development in these stages may thus be a fruitful area of pursuit.
One puzzling finding was that T3 given in the late treatment period, postnatal d 11-15, produced initial suppression and a subsequent rebound elevation of renal α2-receptor binding capabilities. Suppression of α2-receptors in this period by excess thyroid hormone has also been seen in the liver(33), but the effects are opposite in the heart(22). Again, the likely explanations are either that there are different subtype proportions in each tissue or that the tissues differ in their critical windows for reactivity of receptor development to thyroid hormone. In the current study, the effects of excessive T3 are probably not relevant to normal physiology (but may be so for neonatal hyperthyroidism), as attenuation of endogenous thyroid hormone with PTU in the same period did not alter α2-receptor binding.
Regardless of how widespread thyroid control of α-adrenergic receptor development extends, the functional consequences seen in the kidney are likely to be meaningful. In the perinatal period and particularly during parturition, a surge of adrenergic stimulation is known to play a key role in cardiovascular and metabolic adaptations necessary to the transition from fetal to neonatal life(61). During this period, interference with adrenergic stimulation of renal cells, and particularly with the receptor subtype thought to mediate neurotrophic responses(57), results in lasting deficits in trophic responses to neuronal and hormonal factors, compromises the excretory response to vasopressin, and disrupts cell formation(1, 2, 8, 10–13). Thyroid hormone may thus play a vital role in enabling a successful transition to neonatal life and postnatal development, as well as in the programming of neonatal receptor ontogeny.
Abbreviations
- ANOVA:
-
analysis of variance
- PTU:
-
propylthiouracil
- T3:
-
triiodothyronine
References
Slotkin TA, Whitmore WL, Orband-Miller L, Queen KL, Haim K 1987 β-Adrenergic control of macromolecule synthesis in neonatal rat heart, kidney and lung: relationship to sympathetic neuronal development. J Pharmacol Exp Ther 243: 101–109.
Slotkin TA, Seidler FJ, Haim K, Cameron AM, Antolick L, Lau C 1988 Neonatal central catecholaminergic lesions with intracisternal 6-hydroxydopamine: effects on developmental of presynaptic and postsynaptic components of peripheral sympathetic pathways and on the ornithine decarboxylase/polyamine system in heart, lung and kidney. J Pharmacol Exp Ther 247: 975–982.
Nakamura KT, Klinkefus JM, Smith FG, Sato T, Robillard JE 1989 Ontogeny of neuronally released norepinephrine on renin secretion in sheep. Am J Physiol 257:R765–R770.
Smith FG, Smith BA, Guillery EN, Robillard JE 1991 Role of renal sympathetic nerves in lambs during the transition from fetal to newborn life. J Clin Invest 88: 1988–1994.
Robillard JE, Smith FG, Segar JL, Merrill DC, Jose PA 1992 Functional role of renal sympathetic innervation during fetal and postnatal development. News Physiol Sci 7: 130–133.
Rosenberg ME, Hostetter TH, Kren S, Chmielewski D 1993 Effect of angiotensin II and norepinephrine on early growth response genes in the rat kidney. Kidney Int 43: 601–609.
Grignolo A, Seidler FJ, Bartolome M, Kuhn CM, Slotkin TA, Schanberg SM 1982 Norepinephrine content of the rat kidney during development: alterations induced by perinatal methadone. Life Sci 31: 3009–3016.
Slotkin TA, Levant B, Orband-Miller L, Queen KL, Stasheff S 1988 Do sympathetic neurons coordinate cellular development in the heart and kidney? Effects of neonatal central and peripheral catecholaminergic lesions on cardiac and renal nucleic acids and proteins. J Pharmacol Exp Ther 244: 166–172.
Slotkin TA, Lau C, Kavlock RJ, Gray JA, Orband-Miller L, Queen KL, Baker FE, Cameron AM, Antolick L, Haim K, Bartolome M, Bartolome J 1988 Role of sympathetic neurons in biochemical and functional development of the kidney: neonatal sympathectomy with 6-hydroxydopamine. J Pharmacol Exp Ther 246: 427–433.
Hou Q-C, Eylers JP, Lappi SE, Kavlock RJ, Slotkin TA 1989 Neonatal sympathectomy compromises development of responses of ornithine decarboxylase to hormonal stimulation in peripheral tissues. J Dev Physiol 12: 189–192.
Hou Q-C, Baker FE, Seidler FJ, Bartolome M, Bartolome J, Slotkin TA 1989 Role of sympathetic neurons in development ofβ-adrenergic control of ornithine decarboxylase activity in peripheral tissues: effects of neonatal 6-hydroxydopamine treatment. J Dev Physiol 11: 139–146.
Gray JA, Kavlock RJ, Seidler FJ, Slotkin TA 1991 Neural factors in the development of renal function: effect of neonatal central catecholaminergic lesions with 6-hydroxydopamine. J Dev Physiol 15: 325–330.
Appenroth D, Bräunlich H 1981 Effect of sympathectomy with 6-hydroxydopamine on the renal excretion of water and electrolytes in developing rats. Acta Biol Med Ger 40: 1715–1721.
Sripanidkulchai B, Wyss JM 1987 The development ofα2-adrenoceptors in the rat kidney: correlation with noradrenergic innervation. Brain Res 400: 91–100.
Grignolo A, Kuhn CM, Schanberg SM 1982 Maturation of growth hormone stimulation of kidney ornithine decarboxylase in the rat. Life Sci 30: 383–390.
Slotkin TA, Kavlock RJ, Cowdery T, Orband L, Bartolome M, Whitmore WL, Bartolome J 1986 Effects of neonatal methylmercury exposure on adrenergic receptor binding sites in peripheral tissues of the developing rat. Toxicology 41: 95–106.
Lau C, Slotkin TA 1980 Maturation of sympathetic neurotransmission in the rat heart. II. Enhanced development of presynaptic and postsynaptic components of noradrenergic synapses as a result of neonatal hyperthyroidism. J Pharmacol Exp Ther 212: 126–130.
Pracyk JB, Lappi SE, Slotkin TA 1991 Role of thyroid hormone in the development of beta adrenergic control of ornithine decarboxylase in rat heart and kidney. J Pharmacol Exp Ther 256: 757–766.
Pracyk JB, Slotkin TA 1991 Thyroid hormone differentially regulates development of β-adrenergic receptors, adenylate cyclase and ornithine decarboxylase in rat heart and kidney. J Dev Physiol 16: 251–261.
Lau C, Slotkin TA 1982 Maturation of sympathetic neurotransmission in the rat heart. VIII. Slowed development of noradrenergic synapses resulting from hypothyroidism. J Pharmacol Exp Ther 220: 629–636.
Slotkin TA, Lau C, McCook EC, Lappi SE, Seidler FJ 1994 Glucocorticoids enhance intracellular signaling via adenylate cyclase at three distinct loci in the fetus: a mechanism for heterologous teratogenic sensitization?. Toxicol Appl Pharmacol 127: 64–75.
Metz LD, Seidler FJ, McCook EC, Slotkin TA 1996 Cardiacα-adrenergic receptor expression is regulated by thyroid hormone during a critical developmental period. J Mol Cell Cardiol 28: 1033–1044.
Pracyk JB, Slotkin TA 1992 Thyroid hormone regulates ontogeny of β-adrenergic receptors and adenylate cyclase in rat, heart and kidney: effects of propylthiouracil-induced perinatal hypothyroidism. J Pharmacol Exp Ther 261: 951–958.
Bian X-P, Seidler FJ, Bartolome J, Kavlock RJ, Bartolome M, Slotkin TA 1990 Dose-dependent effect of prenatal dexamethasone treatment of β-adrenergic receptor coupling to ornithine decarboxylase and cyclic AMP. J Dev Physiol 14: 125–130.
Bian X-P, Seidler FJ, Slotkin TA 1992 Promotional role for glucocorticoids in the development of intracellular signalling: enhanced cardiac and renal adenylate cyclase reactivity to β-adrenergic and non-adrenergic stimuli after low-dose fetal dexamethasone exposure. J Dev Physiol 17: 289–297.
Kudlacz EM, Navarro HA, Kavlock RJ, Slotkin TA 1990 Regulation of postnatal β-adrenergic receptor/adenylate cyclase development by prenatal agonist stimulation and steroids: alterations in rat kidney and lung after exposure to terbutaline or dexamethasone. J Dev Physiol 14: 273–281.
Duncan CP, Seidler FJ, Lappi SE, Slotkin TA 1990 Dual control of DNA synthesis by α- and β-adrenergic mechanisms in normoxic and hypoxic neonatal rat brain. Dev Brain Res 55: 29–33.
Lidow MS, Goldman-Rakic PS, Rakic P 1991 Synchronized overproduction of neurotransmitter receptors in diverse regions of the primate cerebral cortex. Proc Natl Acad Sci USA 88: 10218–10221.
Lidow MS, Rakic P 1995 Neurotransmitter receptors in the proliferative zones of the developing primate occipital lobe. J Comp Neurol 360: 393–402.
Pracyk JB, Seidler FJ, McCook EC, Slotkin TA 1992 Pituitary-thyroid axis reactivity to hyper- and hypothyroidism in the perinatal period: ontogeny of regulation and long-term programming of responses. J Dev Physiol 18: 105–109.
Rastogi RB, Singhal RL 1979 Effect of neonatal hypothyroidism and delayed L-triiodothyronine treatment on behavioural activity and norepinephrine and dopamine biosynthetic systems in discrete regions of rat brain. Psychopharmacology 62: 287–293.
Rastogi RB, Singhal RL 1976 Neonatal hyperthyroidism: alterations in behavioural activity and the metabolism of brain norepinephrine and dopamine. Life Sci 18: 851–858.
Rao GS, Seidler FJ, Slotkin TA 1995 Modulation of hepatic adrenergic receptor ontogeny by thyroid hormone. Res Commun Mol Pathol Pharmacol 87: 27–42.
Lau C, Slotkin TA 1980 Regulation of ornithine decarboxylase activity in the developing heart of euthyroid of hyperthyroid rats. Mol Pharmacol 18: 247–252.
Lowry OH, Rosebrough NJ, Farr AL, Randall R 1951 Protein measurement with the Folin phenol reagent. J Biol Chem 193: 265–270.
McMillian MK, Schanberg SM, Kuhn CM 1983 Ontogeny of rat hepatic adrenoceptors. J Pharmacol Exp Ther 227: 181–186.
Huff RA, Seidler FJ, Slotkin TA 1991 Glucocorticoids regulate the ontogenetic transition of adrenergic receptor subtypes in rat liver. Life Sci 48: 1059–1066.
Lin W, Seidler FJ, McCook EC, Slotkin TA 1992 Overexpression of α2-adrenergic receptors in fetal rat heart: receptors in search of a function. J Dev Physiol 17: 183–187.
Stewart AF, Rokosh DG, Bailey BA, Karns LR, Chang KC, Long CS, Kariya K, Simpson PC 1994 Cloning of the ratα1C-adrenergic receptor from cardiac myocytes: α1C,α1B and α1D mRNAs are present in cardiac myocytes but not in cardiac fibroblasts. Circ Res 75: 796–802.
Lomasney JW, Cotecchia S, Lorenz W, Leung WY, Schwinn DA, Yang-Feng TL, Brownstein M, Lefkowitz RJ, Caron MG 1991 Molecular cloning and expression of the cDNA for the α1A-adrenergic receptor. J Biol Chem 266: 6365–6369.
Nudel U, Zakut R, Shani M, Neuman S, Levy Z, Yaffe D 1983 The nucleotide sequence of the rat cytoplasmic β-actin gene. Nucleic Acids Res 11: 1759–1771.
Titus DE 1992 Transcription in vitro. In: Titus DE (ed) Promega Protocols and Applications Guide. Promega Corp, Madison, WI, pp 59–61.
Zinn K, DiMaio D, Maniatis T 1983 Identification of two distinct regulatory regions adjacent to the human β-interferon gene. Cell 34: 865–879.
Yamada S, Yamamura HI, Roeske WR 1986 Effects of chemical sympathectomy with 6-hydroxydopamine on α- andβ-adrenoceptors and muscarinic cholinoceptors in rat kidney. Eur J Pharmacol 121: 345–353.
Sundaresan PR, Fortin TL, Kelvie SL 1987 α- andβ-adrenergic receptors in proximal tubules of rat kidney. Am J Physiol 253:F848–F856.
Michel MC, Kenny B, Schwinn DA 1995 Classification ofα1-adrenoceptor subtypes. Naunyn-Schmiedebergs Arch Pharmacol 352: 1–10.
Price DT, Chari RS, Berkowitz DE, Meyers WC, Schwinn DA 1994 Expression of α1-adrenergic receptor subtype mRNA in rat tissues and human SK-N-MC neuronal cells: implications forα1-adrenergic receptor subtype classification. Mol Pharmacol 46: 221–226.
Meister B, Dagerlind Å, Nicholas AP, Hökfelt T 1994 Patterns of messenger RNA expression for adrenergic receptor subtypes in the rat kidney. J Pharmacol Exp Ther 268: 1605–1611.
Kanasaki M, Matsubara H, Murasawa S, Masaki H, Nio Y, Inada M 1994 cAMP Responsive element-mediated regulation of the gene transcription of the α1B adrenergic receptor by thyrotropin. J Clin Invest 94: 2245–2254.
Rokosh DG, Bailey BA, Stewart AF, Karns LR, Long CS, Simpson PC 1994 Distribution of α1C-adrenergic receptor mRNA in adult rat tissues by RNase protection assay and comparison withα1B and α1D . Biochem Biophys Res Commun 200: 1177–1184.
Knowlton KU, Michel MC, Itani M, Shubeita HE, Ishihara K, Brown JH, Chien KR 1993 The α1A-adrenergic receptor subtype mediates biochemical, molecular, and morphologic features of cultured myocardial cell hypertrophy. J Biol Chem 268: 15374–15380.
Li HT, Long CS, Rokosh DG, Honbo NY, Karliner JS 1995 Chronic hypoxia differentially regulates α1-adrenergic receptor subtype mRNAs and inhibits α1-adrenergic receptor-stimulated cardiac hypertrophy and signaling. Circulation 92: 918–925.
Moalic JM, Bourgeois F, Mansier P, Machida CA, Carré F, Chavalier B, Pitarque P, Swynghedauw B 19931 β1-Adrenergic receptor and GαS mRNAs in rat heart as a function of mechanical load and thyroxine intoxication. Cardiovasc Res 27: 231–237.
Birk E, Tyndall MR, Erickson LC, Rudolph AM, Roberts JM 1992 Effects of thyroid hormone on myocardial adrenergic β-receptor responsiveness and function during late gestation. Pediatr Res 31: 468–473.
Revelli JP, Pescini R, Muzzin P, Seydoux J, Fitzgerald MG, Fraser CM, Giacobino J-P 1991 Changes in β1- andβ2-adrenergic receptor mRNA levels in brown adipose tissue and heart of hypothyroid rats. Biochem J 277: 625–629.
McCune SK, Voigt MM 1991 Regional brain distribution and tissue ontogenic expression of a family of α-adrenergic receptor mRNAs in the rat. J Mol Neurosci 3: 29–37.
Rokosh DG, Stewart AFR, Chang KC, Bailey BA, Karliner JS, Camacho SA, Long CS, Simpson PC 1996 α1-Adrenergic receptor subtype mRNAs are differentially regulated by α1-adrenergic and other hypertrophic stimuli in cardiac myocytes in culture and in vivo: repression of α1B and α1D but induction ofα1C . J Biol Chem 271: 5839–5843.
Gick GG, Ismail-Beigi F, Edelman IS 1988 Thyroidal regulation of rat renal and hepatic Na,K-ATPase gene expression. J Biol Chem 263: 16610–16618.
Takatori K, Ogura T, Katayama E, Ota Z, Mizukawa K, Ogawa N 1991 Autoradiographic localization and computerized quantification ofα1- and α2-adrenoceptors in spontaneously hypertensive rat kidney: [3H]bunazosin and [3H]yohimbine binding studies. J Int Med Res 19: 153–160.
Slotkin TA, Lau C, Seidler FJ 1994 β-Adrenergic receptor overexpression in the fetal rat: distribution, receptor subtypes and coupling to adenylate cyclase via G-proteins. Toxicol Appl Pharmacol 129: 223–234.
Lagercrantz H, Slotkin TA 1986 The “stress” of being born. Sci Am 254: 100–107.
Acknowledgements
The authors thank E. C. McCook for technical assistance.
Author information
Authors and Affiliations
Additional information
Supported by U.S. Public Health Service Grants HD-09713 (T.A.S.), HL-49103(D.A.S.), and AG-00745 (D.A.S.).
Rights and permissions
About this article
Cite this article
Tan, J., Seidler, F., Schwinn, D. et al. A Critical Period for the Role of Thyroid Hormone in Development of Renalα-Adrenergic Receptors. Pediatr Res 42, 93–102 (1997). https://doi.org/10.1203/00006450-199707000-00015
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-199707000-00015