Abstract
Plasma somatostatin and cholecystokinin are two gut peptides with opposite functions which are regulated by two different parts of the autonomic nervous system. Previously we have shown that plasma somatostatin and cholecystokinin levels are higher in preterm infants during the 1st d of life than in adults or in their mothers, and that plasma somatostatin is negatively correlated to gestational age. We have longitudinally studied these two peptides in 28 preterm infants, 17 boys and 11 girls, up until the age of 2 y. The mean (SD) gestational age was 32.3 (2.8) wk, the mean birth weight was 1877 (515) g, and the mean birth length was 42.8 (3.8) cm. Blood samples were taken on the 1st d of life, at 6 wk, and at 3, 6, 12, and 24 mo of age. Plasma was analyzed by specific somatostatin and cholecystokinin RIAs. The median plasma somatostatin and cholecystokinin levels were lowest at 3 mo (somatostatin = 17.4/cholecystokinin = 10.5 pmol/L) and highest at 6 mo (somatostatin = 37.3/cholecystokinin = 27.1 pmol/L). At 24 mo plasma somatostatin remained at the same level, and cholecystokinin had decreased to half that level. After the 1st d of life plasma somatostatin and cholecystokinin levels were not correlated to gestational age or attained weight or length. The plasma somatostatin level at 3 mo of age was negatively correlated to the increment in knee-heel distance between 3 and 6 mo of age.
Similar content being viewed by others
Main
Somatostatin and cholecystokinin are two of many known gut peptides(1, 2). Our knowledge of the function of these peptides in term and preterm infants is sparse. Previously, we have shown that just after birth and during the 1st d of life, plasma somatostatin and cholecystokinin levels are higher in the infants than in plasma from their mothers(3, 4). The infant plasma somatostatin and cholecystokinin levels increased during the 1st d of life, and plasma somatostatin levels were inversely related to gestational age, although this was not the case for cholecystokinin levels(4).
Our knowledge of the regulation and the levels of these peptides after the neonatal period is also incomplete. What roles do somatostatin and cholecystokinin play during the postneonatal period of rapid somatic growth and how are the somatostatin and cholecystokinin levels affected by different feeding patterns?
The first aim of this work was to study up to the age of 2 y the plasma levels of somatostatin and cholecystokinin in preterm infants. Some of these infants were previously investigated in the neonatal period(3, 4). The second aim was to relate the levels to attained weight and length and knee-heel distance and to growth rate.
METHODS
Material. The study included 28 preterm infants with gestational ages ranging from 25 to 36 wk [mean 32.3 (SD) 2.8]. Gestational age was based on ultrasound at 18 gestational weeks in 20 mothers(5). For the remainder, gestational age was based on the mother's recollection of the 1st d of her last menstrual period. The birth weights ranged from 733 to 2840 g (mean 1877, SD 515 g) and the birth lengths from 30.5 to 47.0 cm (mean 42.8, SD 3.8 cm). There were 21 singletons and seven twins from a total of four twin pregnancies. Twenty-five infants were appropriate for gestational age (AGA; ≥ -2 SD to ≤ +2 SD) and three infants were small for gestational age (SGA; < -2 SD) according to the classification of Karlberg and Priolisi(6).
All infants were admitted to the intensive care nursery. According to the nursery policy, oral feeding with human milk is introduced within the 1st d of life for almost all preterm infants. The 1st d volumes ranged from 1 to 5 mL/kg per meal. Mothers are actively encouraged to start feeding with breast milk by breast or by nasogastric tube as soon as possible after the delivery. Donor's milk, coded human milk, is used until mothers' milk production is adequate. In general, about 90% of all infants are breast-fed at the time of discharge from the intensive care nursery. Table 1 shows the number of infants in this study who were breast-fed at varying time points. At 3 mo, 14 infants (50%) were exclusively breast-fed and six infants(21%) were on mixed feedings.
Table 2 shows the health conditions and medical treatment of the infants during their first 2 mo of life. Respiratory problems and hyperbilirubinemia were the predominant problems. One infant had pronounced clinical symptoms of transient neonatal thyrotoxicosis caused by stimulating thyroid receptor antibodies acquired from the mother. The infant was successfully treated with thyrostatics for 3 mo. Seven infants received continuous positive airway pressure and five infants were ventilated on a respirator.
Postneonatally, six children developed chronic diseases. Four of them had bronchial asthma, one suffered from cow's milk allergy, and one child developed a moderate right-sided hemiplegia without feeding problems. Of the four children with asthma, two children also had gastroeosophageal reflux.
One of the asthmatic children inhaled salbutamol and three inhaled budesonide. One child intermittently received 1000-2000 μg of budesonide daily. During the periods of high steroid dosage, the daily increment in knee-heel distance decreased. One child with gastroeosophageal reflux was being treated with cisapride. Cow's milk was eliminated from the diet of the child with cow's milk allergy.
Information on birth weight, birth length, and head circumference at birth was extracted from the hospital records. At the time of blood sampling, the weight, length, head circumference, type of feeding, health status, and medical treatment were prospectively recorded. Supine length was measured on a sturdy wooden board by hospital personal as a part of the admission routines. Weight and length were compared with Karlberg's(7) growth standard and expressed in SD scores. Chronologic age was corrected for gestational age at birth. Nineteen infants followed normal growth curves (≥-2 SD ≤ +2 SD). The attained growth of the remaining nine children was outside the normal range (< -2SD to > +2SD) on one or more occasions(“abnormal growth”). Six of these children had serious neonatal morbidity, and three were SGA. The range of growth for the nine children with abnormal growth are shown in Table 3. Only two of the total number of children in the study were outside the normal range at 2 y of corrected age. One of these children had respiratory distress and a chronic condition (asthma), and the other child had a neonatal problem.
Knee-heel distance(8) was measured by one of the authors (C.J.T.). Table 4 shows the difference in knee-heel distance in paired samples between different time points from 6 wk up to 2 y of age. Age was not corrected for gestational age at birth.
The study was approved by the Ethical Committee of the Medical Faculty, Umeå University. The mothers/parents received verbal and written information and gave her/their consent for participation in the investigation.
Procedure. Initial blood samples (arterial, venous, or capillary) for plasma somatostatin and cholecystokinin were taken from the infants just before the first meal at 1-6 h of age (mean 3.3 h). Subsequent blood samples (venous or capillary) were taken at the mean (SD) age of 6 (0.7) wk, and at 3 (0.5), 6 (0.5), 12 (1.5), and 24 (1.2) mo of age. In agreement with Fitz-Patrick and Patel(9) we did not find any difference between somatostatin levels from arterial and venous blood. Neither there was any difference between venous and capillary blood. The same results was found for cholecystokinin levels. All sample were taken shortly before a meal, representing preprandial peptide levels. None of the children was acutely ill at the time of blood sampling. There was not always sufficient blood on all occasions to measure both peptides. The n values may consequently differ in the tables.
One milliliter of blood was put into ice-chilled heparin/trasylol/chlorbutanol-prepared tubes(3) and immediately centrifuged (20 °C, 10 min, 2000 rpm). The plasma was frozen at (-20 °C or -80 °C) until analyzed. The plasma was concentrated by semichromatography(10) and analyzed as double samples at two different occasions. Samples taken on the 1st d and at 6 wk, and half of the samples taken at 3 mo were analyzed on the first occasion. Half of the samples taken at 3 mo and all samples taken at 6, 12, and 24 mo were analyzed on the second occasion. The somatostatin RIA method measures somatostatin 14 and 28. The cholecystokinin RIA method measures the N-terminal end of sulfated cholecystokinin 8, 33, and 39 as earlier described(3). The RIA interassay coefficients of variation was 9% for somatostatin and 15% for cholecystokinin.
Statistics. All calculations were performed at the Institute of Mathematical Statistics, Umeå University. The SYSTAT(11) and MINITAB(12) computer programs were used to carry out descriptive statistics and Wilcoxon's signed ranks test. Holm's method for correction of mass significance was used for correlations(13). p values less than 0.05 were considered statistically significant.
There was no association between plasma levels of somatostatin or cholecystokinin for the children in each sets of twins. In the statistical analysis, values obtained from twins have therefore been treated together with values obtained from singletons.
RESULTS
There were no differences between the median levels of somatostatin and cholecystokinin of children with normal growth compared with children with abnormal growth. The two groups have therefore been investigated together.
Table 5 shows the median plasma somatostatin and cholecystokinin values at different time points up to 2 y of age. The time points are not corrected for gestational age at birth. The lowest plasma somatostatin values were found at 3 mo. At 6 mo the median plasma somatostatin level was twice as high, and it remained at this level at 12 and 24 mo of age. The difference at 3 mo was significant compared with 6 wk and 6, 12, and 24 mo. The decline from 6 wk to 3 mo failed to reach statistical significance, however, when correction for mass significance was applied.
The lowest cholecystokinin values were found at 3 mo. The plasma levels were highest at 6 mo and subsequently decreased. The differences between 3 mo compared with 6 wk and 6 and 12 mo were significant. The decrease from 6 to 24 mo of age was not significant when correction for mass significance was applied. Plasma somatostatin and cholecystokinin levels after birth were not correlated to attained weight or attained length at any time point.
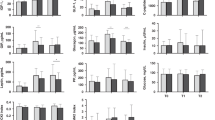
Figures 1 and 2 show individual plasma somatostatin and cholecystokinin levels from the 1 d of life up to 2 y of age. Age is not corrected for gestational age at birth. Both figures show the decrease in plasma somatostatin and cholecystokinin levels at 3 mo and the increase at 6 mo. There was generally no tracking, but it can be noted that two children, who were classified as SGA at birth and who exhibited poor catch up in growth, had particularly high plasma somatostatin values, whereas the third SGA child, who had a normal catch up, had plasma somatostatin values that were lower. The plasma somatostatin values of the child with neonatal thyrotoxicosis were high throughout the study period.
Figure 3,A and B, shows individual plasma somatostatin values during the 1st y of life for infants at 25 to 31 gestational wk and for infants at 32 to 36 gestational wk. Age is not corrected for gestational age. The temporal patterns were similar in the two groups. Thus, the lowest values were recorded at 3 mo of chronologic age, regardless of the gestational age at birth. Similarly, the plasma cholecystokinin values were independent of gestational age (not shown).
Figure 4 shows plasma somatostatin values at 3 mo and the average daily increment in knee-heel distance from 3 to 6 mo. A significant negative correlation was found. The lower the values of plasma somatostatin at 3 mo, the greater was the daily increment from 3 to 6 mo. However, when excluding the two SGA infants, the significance disappeared(r = -0.44; p = 0.058). There were no significant correlations between the knee-heel increment or distance and plasma somatostatin levels at any other time points. There were no significant associations between plasma cholecystokinin values and knee-heel increment or distance at any time points.
There were no differences in the temporal pattern or in the median plasma somatostatin and cholecystokinin levels of children who were breast-fed at the time of blood sampling compared with those who were not. Nor were the median values of the six children with chronic conditions significantly different from those who were healthy at any time point.
DISCUSSION
In spite of immaturity and low birth weight, the attained weight and height of most children were entirely normal at all time points when chronologic age was corrected for gestational age. Moreover, of nine children with abnormal measurements at some time point, only two were outside the normal range at 2 y of corrected age. Thus, the material represents a cohort of children with a pattern of growth which may not be much different from that of normal term infants.
The most remarkable finding of this study was the significant decrease in both plasma somatostatin and cholecystokinin levels at 3 mo of age followed by a significant rise of both peptides at 6 mo. These results could not be explained by methodologic factors. The plasma was stored frozen for different lengths of time before analysis. If the peptide levels had decreased due to storage, the lowest values would have been found in samples collected during the 1st d and at 6 wk. However, this was not the case. Nor could the results be explained by the fact that the samples were analyzed at two occasions. The RIA interassay coefficients of variation, 9% for somatostatin and 15% for cholecystokinin, were too small to explain the differences obtained in the peptide levels. Moreover, half of the 3-mo samples were analyzed on the first occasion and half on the second, but as seen in Table 5 the plasma levels at 3 mo varied within only a narrow range. The changes in plasma somatostatin and cholecystokinin levels during the first 6 mo could not be related to whether the child was breast-fed or formula-fed.
In a nonlinear model of growth in the 1st y of life, Giani et al.(14) found a growth spurt during the first 2 mo of life followed by a decreased growth rate up to 6 mo of age. The decline in the plasma somatostatin level between 6 wk and 3 mo, which was found in our study, seems to be in agreement with this growth model. Low plasma somatostatin levels at 3 mo might promote growth due to the lack of inhibition by somatostatin on gastrointestinal growth and function. The relationship between somatostatin levels and growth was also demonstrated in our AGA and SGA infants by the negative correlation between plasma somatostatin levels at 3 mo and the daily increment in knee-heel distance from 3 to 6 mo. However, the significant correlation disappeared when the two SGA infants were excluded.
According to the infant-child-puberty model of Karlberg et al.(15), infant growth from 6 mo of age is largely dependent on growth hormone. Growth hormone secretion is stimulated by growth hormone-releasing hormone and inhibited by somatostatin(16). The high plasma somatostatin levels at 6 mo and later in life might be a consequence of the increase in growth hormone secretion. There might be a secondary increase in the plasma somatostatin levels to balance the increase in growth hormone, as well as to balance the growth rate, which is rather constant after 1 y of age. It is well known that the secretion of growth hormone varies during a 24-h period. The 24-h variation in somatostatin level is not known, and we have not found any significant variation in the somatostatin levels in the morning compared with the levels in the evening (our unpublished observations).
It is known that some SGA infants have a lack of growth hormone and benefit from growth hormone therapy(17). In this context it is of interest to note that the plasma somatostatin levels were particularly high at 12 and 24 mo in the two children who were SGA at birth and had a poor catch up in growth.
We have found that there is a strong negative correlation between plasma somatostatin levels and gestational age during the 1st d of life(4). In the present study, plasma somatostatin levels after the 1st d of life were unrelated to gestational age at birth. It seems that the plasma somatostatin levels might be related to the biologic maturity of the infant early in life, whereas later, exogenous factors, such as light, noise, sleep patterns, nutrients, caretaker-infant interaction, and so forth, might be more important determinants of the plasma levels. Similarly, in preterm infants the secretion of other gut hormones, such as glucagon, gastrin, and secretin, the secretion of enzymes from the exocrine pancreas, and the maturation of renal function and of the skin all depend on postnatal rather than on postconceptional age(18–23).
With the exception of the study by Jain et al.(24), there are no longitudinal studies of plasma somatostatin during the 1st y of life. Postnatal changes of plasma somatostatin were followed by these authors (Jain et al.)(24) in 62 infants (gestational age 25-35 wk), but only during the 1st mo of life. Plasma somatostatin levels were highest in the 2nd wk and gradually declined during the 3rd and 4th wk. In a cross-sectional study, Alfvén et al.(25) analyzed plasma somatostatin in children aged 1-15 y. There was a significant decrease in plasma somatostatin levels with increasing age, and it was concluded that the level was twice as high at 1-2 y of age compared with that of children older than 10 y. The study provided no details, however, of changes during the 2nd y of life. In our study the plasma somatostatin level remained stable during the 2nd y.
To our knowledge there are only two published studies of plasma cholecystokinin levels in children. In the cross-sectional study of Alfvén et al.(25), the plasma cholecystokinin levels were not significantly different in children 1-8 y of age compared with children 8-15 y of age. However, they found an age-related negative correlation for plasma cholecystokinin levels in boys, but not in girls, but provided no details about the changes during the 2nd y of life. At this age we found a decrease in the cholecystokinin levels, which, however, did not reach statistical significance.
We found the lowest plasma cholecystokinin levels at 3 mo of age. Even these levels, however, were high compared with those of children 1-7 y of age(25) and with those of healthy school children(26). The fact that cholecystokinin secretion is stimulated by protein and fat(2) and that both human milk and formula contain relatively more fat during the 1st y may be an explanation for the high plasma cholecystokinin levels up to 1 y of age.
In conclusion, after the neonatal period, the somatostatin and cholecystokinin levels decreased in preterm infants to a minimal level at 3 mo of age followed by a significant rise at 6 mo of age. These variations in plasma somatostatin but not in plasma cholecystokinin levels at 3 mo of age were correlated to the daily increment in knee-heel distance (growth rate) from 3 to 6 mo of age. The variations in plasma levels were not correlated to gestational age, attained weight and length, breast-feeding or formula-feeding, and weaning.
Abbreviations
- AGA:
-
appropriate for gestational age
- SGA:
-
small for gestational age
References
Delvalle J, Yamada T 1990 The gut as an endocrine organ. Annu Rev Med 41: 447–55.
Walsh JH 1994 Gastrointestinal hormones. In: Johnson LR(ed) Physiology of the Gastrointestinal Tract, 3rd Ed, Vol 1. Raven Press, New York, pp 1–128.
Törnhage C-J, Serenius F, Uvnäs-Moberg K, Lindberg T 1995 Plasma somatostatin and cholecystokinin levels in preterm infants and their mothers at birth. Pediatr Res 37: 771–776.
Törnhage C-J, Serenius F, Uvnäs-Moberg K, Lindberg T 1996 Plasma somatostatin and cholecystokinin levels in preterm infants during the first day of life. Biol Neonate 70: 311–321.
Campell S 1969 The prediction of fetal maturity by ultrasonic measurement of the biparietal diameter. J Obstet Gynaecol Br Commonw 76: 603–609.
Karlberg P, Priolisi A 1977 Clinical evaluation of similarities and dissimilarities between two city surveys. In: Falkner F. (ed) Fundamentals of Mortality Risks during the Perinatal Period and Infancy, Vol 9. Karger, Basel, pp 165–192.
Karlberg Taranger J, Engström I, Lichtenstein H, Svennberg-Redegren I 1976 The somatic development of children in a Swedish urban community. A prospective longitudinal study. I. Physical growth from birth to 16 years and longitudinal outcome of the study during the same age period. Acta Paediatr Scand Suppl 258: 7–76.
Fleischer Michaelsen K, Skov L, Badsberg JH, Jörgensen M 1991 Short-term measurement of linear growth in preterm infants:validation of a hand-held knemometer. Pediatr Res 30: 464–468.
Fitz-Patrick D, Patel YC 1979 Measurement, characterization and source of somatostatin-like immunoreactivity in human amniotic fluid. J Clin Invest 63: 737–742.
Bidlingmeyer BA 1984 Guidelines for proper usage of solid-phase extraction devices. LC GC Magazine of Liquid and Gas Chromatography 2: 578–80.
Wilkinson, Leyland 1989 SYSTAT. The system for statistics, Version 5:2, Evanston, IL, pp 48–557.
MINITAB 1994 Reference manual, release 10 for Windows, 8: 1–12.
Holm S 1979 A simple sequentially rejective multiple test procedure. Scand J Stat 6: 65–70.
Giani U, Filosa A, Causa P 1996 A non-linear model of growth in the first year of life. Acta Paediatr Scand 85: 7–13.
Karlberg J, Engström I, Karlberg P, Fryer JG 1987 Analysis of linear growth using a mathematical model. I. From birth to three years. Acta Paediatr Scand 76: 478–488.
Tannenbaum GS 1988 Somatostatin as physiological regulator of pulsatile growth hormone secretion. Horm Res 29: 70–74.
Albanese A, Stanhope R 1993 Growth and metabolic data following growth hormone treatment of children with intrauterine growth retardation. Horm Res 39: 8–12.
Marchini G, Persson B, Uvnäs-Moberg K 1990 Plasma gastrin and somatostatin levels in infants during the first four postnatal days. J Dev Physiol 14: 157–162.
Rogers M, Davidson DC, Lawrence J, Ardill Joy, Buchanan KD 1974 Neonatal secretion of gastrin and glucagon. Arch Dis Child 49: 796–800.
Lucas A, Adrian TE, Bloom SR, Aynsley-Green A 1980 Plasma secretin in neonates. Acta Paediatr Scand 69: 205–210.
Nakamura KT, Matherne GP, McWeeny OJ, Smith BA, Robillard JE 1987 Renal hemodynamics and functional changes during the transition from fetal to newborn life in sheep. Pediatr Res 21: 229–234.
Lane AT 1987 Development and care of the preterm infant's skin. Pediatr Dermatol 4: 1–5.
Zoppi G, Andreotti G, Pajno-Ferrara F, Njai DM, Gaburro D 1972 Exocrine pancreas function in premature and fullterm neonate. Pediatr Res 6: 880–886.
Jain L, Del Valle J, Gelhar D, Levy P, Mc Culloch K, Vidyasagar D 1995 Somatostatin in preterm infants:postnatal changes and response to stress. Biol Neonate 68: 81–86.
Alfvén G, Gustavsson P, Uvnäs-Moberg K 1995 Age-related decrease in plasma levels of gastrin, cholecystokinin and somatostatin. Acta Paediatr 84: 1344–1346.
Alfvén G, Uvnäs-Moberg K 1993 Elevated cholecystokinin concentrations in plasma in children with recurrent abdominal pain. Acta Paediatr 82: 967–970.
Acknowledgements
The authors thank Peter Anton and Leif Nilsson, Institute of Mathematical Statistics, Umeå University, for the statistical calculations and creating the figures. We also thank Reneé Anderson for technical assistance and Professor Petter Karlberg for help with the classification of growth.
Author information
Authors and Affiliations
Additional information
Supported by grants from the Foundation of First of May Flower Annual Campaign and the Medical Faculty, Umeå University, Umeå, Sweden.
Rights and permissions
About this article
Cite this article
Törnhage, CJ., Serenius, F., Uvnäs-Moberg, K. et al. Plasma Somatostatin and Cholecystokinin Levels in Preterm Infants during Their First Two Years of Life. Pediatr Res 41, 902–908 (1997). https://doi.org/10.1203/00006450-199706000-00017
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-199706000-00017