Abstract
Background:
Comprehensive molecular characterization of cancer that has metastasized to bone has proved challenging, which may limit the diagnostic and potential therapeutic opportunities for patients with bone-only metastatic disease.
Methods:
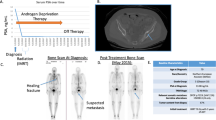
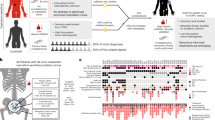
We describe successful tissue acquisition, DNA extraction, and whole-exome sequencing from a bone metastasis of a patient with metastatic, castration-resistant prostate cancer (PCa).
Results:
The resulting high-quality tumor sequencing identified plausibly actionable somatic genomic alterations that dysregulate the phosphoinostide 3-kinase pathway, as well as a theoretically actionable germline variant in the BRCA2 gene.
Conclusions:
We demonstrate the feasibility of diagnostic bone metastases profiling and analysis that will be required for the widespread application of prospective ‘precision medicine’ to men with advanced PCa.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 4 print issues and online access
$259.00 per year
only $64.75 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Roychowdhury S, Iyer MK, Robinson DR, Lonigro RJ, Wu YM, Cao X et al. Personalized oncology through integrative high-throughput sequencing: a pilot study. Sci Translational Med 2011; 3: 111ra21.
Wagle N, Berger MF, Davis MJ, Blumenstiel B, Defelice M, Pochanard P et al. High-throughput detection of actionable genomic alterations in clinical tumor samples by targeted, massively parallel sequencing. Cancer Discovery 2012; 2: 82–93.
de Bono JS, Logothetis CJ, Molina A, Fizazi K, North S, Chu L et al. Abiraterone and increased survival in metastatic prostate cancer. N Engl J Med 2011; 364: 1995–2005.
Scher HI, Fizazi K, Saad F, Taplin ME, Sternberg CN, Miller K et al. Increased survival with enzalutamide in prostate cancer after chemotherapy. N Engl J Med 2012; 367: 1187–1197.
Grasso CS, Wu YM, Robinson DR, Cao X, Dhanasekaran SM, Khan AP et al. The mutational landscape of lethal castration-resistant prostate cancer. Nature 2012; 487: 239–243.
Mehra R, Kumar-Sinha C, Shankar S, Lonigro RJ, Jing X, Philips NE et al. Characterization of bone metastases from rapid autopsies of prostate cancer patients. Clin Cancer Res 2011; 17: 3924–3932.
Febbo PG, Thorner A, Rubin MA, Loda M, Kantoff PW, Oh WK et al. Application of oligonucleotide microarrays to assess the biological effects of neoadjuvant imatinib mesylate treatment for localized prostate cancer. Clin Cancer Res 2006; 12: 152–158.
Fisher S, Barry A, Abreu J, Minie B, Nolan J, Delorey TM et al. A scalable, fully automated process for construction of sequence-ready human exome targeted capture libraries. Genome Biol 2011; 12: R1.
Drier Y, Lawrence MS, Carter SL, Stewart C, Gabriel SB, Lander ES et al. Somatic rearrangements across cancer reveal classes of samples with distinct patterns of DNA breakage and rearrangement-induced hypermutability. Genome Res 2013; 23: 228–235.
Van Allen E, Wagle N, Kryukov G, Ramos A, Getz G, Garraway L . A heuristic platform for clinical interpretation of cancer genome sequencing data. J Clin Oncol 2012; (suppl; abstr 10502).
Quayle SN, Lee JY, Cheung LW, Ding L, Wiedemeyer R, Dewan RW et al. Somatic mutations of PIK3R1 promote gliomagenesis. PloS One 2012; 7: e49466.
Forbes SA, Bindal N, Bamford S, Cole C, Kok CY, Beare D et al. COSMIC: mining complete cancer genomes in the Catalogue of Somatic Mutations in Cancer. Nucleic Acids Res 2011; 39: D945–D950.
Barbieri CE, Baca SC, Lawrence MS, Demichelis F, Blattner M, Theurillat JP et al. Exome sequencing identifies recurrent SPOP, FOXA1 and MED12 mutations in prostate cancer. Nat Genet 2012; 44: 685–689.
Exome Variant Server, NHLBI GO Exome Sequencing Project (ESP). Seattle, WA, USA 2012.
Farrugia DJ, Agarwal MK, Pankratz VS, Deffenbaugh AM, Pruss D, Frye C et al. Functional assays for classification of BRCA2 variants of uncertain significance. Cancer Res 2008; 68: 3523–3531.
Yang D, Khan S, Sun Y, Hess K, Shmulevich I, Sood AK et al. Association of BRCA1 and BRCA2 mutations with survival, chemotherapy sensitivity, and gene mutator phenotype in patients with ovarian cancer. JAMA 2011; 306 (14): 1557–1565.
Fong PC, Boss DS, Yap TA, Tutt A, Wu P, Mergui-Roelvink M et al. Inhibition of poly(ADP-ribose) polymerase in tumors from BRCA mutation carriers. N Engl J Med 2009; 361: 123–134.
Nakabayashi M, Werner L, Courtney KD, Buckle G, Oh WK, Bubley GJ et al. Phase II trial of RAD001 and bicalutamide for castration-resistant prostate cancer. BJU Int 2012; 110: 1729–1735.
Van Allen EM, Pomerantz M . Moving toward personalized medicine in castration-resistant prostate cancer. Urol Clinics North Am 2012; 39: 483–490.
Carver BS, Chapinski C, Wongvipat J, Hieronymus H, Chen Y, Chandarlapaty S et al. Reciprocal feedback regulation of PI3K and androgen receptor signaling in PTEN-deficient prostate cancer. Cancer Cell 2011; 19: 575–586.
Spritzer CE, Alfonso PD, Vinson EN, Turnbull JD, Morris KK, Foye A et al. Bone marrow biopsy: RNA isolation with expression profiling in men with metastatic castration-resistant prostate cancer - factors affecting diagnostic success. Radiology 2013; 269: 816–823.
Brenner JC, Ateeq B, Li Y, Yocum AK, Cao Q, Asangani IA et al. Mechanistic rationale for inhibition of poly(ADP-ribose) polymerase in ETS gene fusion-positive prostate cancer. Cancer Cell 2011; 19: 664–678.
Ateeq B, Tomlins SA, Laxman B, Asangani IA, Cao Q, Cao X et al. Therapeutic targeting of SPINK1-positive prostate cancer. Sci Translational Med 2011; 3: 72ra17.
Cibulskis K, McKenna A, Fennell T, Banks E, DePristo M, Getz G . ContEst: estimating cross-contamination of human samples in next-generation sequencing data. Bioinformatics 2011; 2718: 2601–2602.
McKenna A, Hanna M, Banks E, Sivachenko A, Cibulskis K, Kernytsky A et al. The Genome Analysis Toolkit: a MapReduce framework for analyzing next-generation DNA sequencing data. Genome Res 2010; 20: 1297–1303.
Cibulskis K, Lawrence MS, Carter SL, Sivachenko A, Jaffe D, Sougnez C et al. Sensitive detection of somatic point mutations in impure and heterogeneous cancer samples. Nat Biotechnol 2013; 31: 213–219.
Acknowledgements
This work was supported by Stand Up To Cancer, Prostate Cancer Foundation, Prostate Dream Team Translational Cancer Research Grants, made possible by the generous support of the Movember Foundation (EMV, AF, LAG, PGF), the Prostate Cancer Foundation (EMV, PGF), the Starr Cancer Consortium (I4-A424; LAG), the NIH (5 U01 CA157703; PGF), and the Department of Defense (W81XWH-10-PCRP-SIDA; LAG). Stand Up To Cancer is a program of the Entertainment Industry Foundation administered by the American Association for Cancer Research. The authors acknowledge Deborah Farlow for her project management contribution to this effort.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Competing interests
Levi A Garraway is an equity holder and consultant in Foundation Medicine, a consultant to Novartis, Millenium/Takeda, and Boehringer Ingelheim, and a recipient of a grant from Novartis. Phillip G Febbo is the principal investigator on a Novartis supported trial and speaker and consultant for Janssen and Dendrion. The remaining authors declare no conflict of interest.
Additional information
Supplementary Information accompanies the paper on the Prostate Cancer and Prostatic Diseases website
Rights and permissions
About this article
Cite this article
Van Allen, E., Foye, A., Wagle, N. et al. Successful whole-exome sequencing from a prostate cancer bone metastasis biopsy. Prostate Cancer Prostatic Dis 17, 23–27 (2014). https://doi.org/10.1038/pcan.2013.37
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/pcan.2013.37
Keywords
This article is cited by
-
SIUrO best practice recommendations to optimize BRCA 1/2 gene testing from DNA extracted from bone biopsy in mCRPC patients (BRCA Optimal Bone Biopsy Procedure: BOP)
Virchows Archiv (2023)
-
Mitochondrial DNA analysis efficiently contributes to the identification of metastatic contralateral breast cancers
Journal of Cancer Research and Clinical Oncology (2021)
-
Lysosomal acid ceramidase ASAH1 controls the transition between invasive and proliferative phenotype in melanoma cells
Oncogene (2019)
-
The prognostic utility of the transcription factor SRF in docetaxel-resistant prostate cancer: in-vitro discovery and in-vivo validation
BMC Cancer (2017)
-
Gene expression analysis of bone metastasis and circulating tumor cells from metastatic castrate-resistant prostate cancer patients
Journal of Translational Medicine (2016)