Abstract
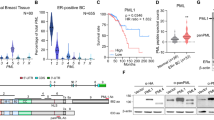
Crosstalk between estrogen receptor (ER) and the inflammatory nuclear factor κB (NFκB) pathway in ER+ breast cancers may contribute to a more aggressive phenotype. Pleckstrin Homology-Like Domain, Family A, member 1 (PHLDA1), a target gene of ER-NFκB crosstalk, has been implicated in cell survival and stem cell properties. 17β-estradiol (E2), acting through ERα, and pro-inflammatory cytokines, acting through NFκB, increase the nascent transcript and PHLDA1 messenger RNA stability, indicating both transcriptional and post-transcriptional control of PHLDA1 expression. We show that PHLDA1 is a direct target of miR-181 and that mature miR-181a and b, as well as their host gene, are synergistically downregulated by E2 and tumor necrosis factor α, also in an ER- and NFκB-dependent manner. Thus, ER and NFκB work together to upregulate PHLDA1 directly through enhanced transcription and indirectly through repression of miR-181a and b. Previous studies have suggested that PHLDA1 may be a stem cell marker in the human intestine that contributes to tumorigenesis. Our findings that PHLDA1 is upregulated in mammospheres (MS) of ER+ breast cancer cells and that PHLDA1 knockdown impairs both MS formation and the expansion of aldehyde dehydrogenase (ALDH)-positive population, suggest that PHLDA1 may play a similar role in breast cancer cells. Upregulation of PHLDA1 in MS is largely dependent on the NFκB pathway, with downregulated miR-181 expression a contributing factor. Over-expression of miR-181 phenocopied PHLDA1 knockdown and significantly impaired MS formation, which was reversed, in part, by protection of the PHLDA1 3′ untranslated region (UTR) or overexpression of PHLDA1 lacking the 3′UTR. Furthermore, we find that elevated PHLDA1 expression is associated with a higher risk of distant metastasis in ER+ breast cancer patients. Altogether, these data suggest that high PHLDA1 expression is controlled through an ER-NFκB-miR-181 regulatory axis and may contribute to a poor clinical outcome in patients with ER+ breast tumors by enhancing stem-like properties in these tumors.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 50 print issues and online access
$259.00 per year
only $5.18 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout








Similar content being viewed by others
References
Zhou Y, Eppenberger-Castori S, Marx C, Yau C, Scott GK, Eppenberger U et al. Activation of nuclear factor-kappaB (NFkappaB) identifies a high-risk subset of hormone-dependent breast cancers. Int J Biochem Cell Biol 2005; 37: 1130–1144.
Zhou Y, Yau C, Gray JW, Chew K, Dairkee SH, Moore DH et al. Enhanced NF kappa B and AP-1 transcriptional activity associated with antiestrogen resistant breast cancer. BMC Cancer 2007; 7: 59.
Jones RL, Rojo F, A'Hern R, Villena N, Salter J, Corominas JM et al. Nuclear NF-kappaB/p65 expression and response to neoadjuvant chemotherapy in breast cancer. J Clin Pathol 2011; 64: 130–135.
deGraffenried LA, Chandrasekar B, Friedrichs WE, Donzis E, Silva J, Hidalgo M et al. NF-kappa B inhibition markedly enhances sensitivity of resistant breast cancer tumor cells to tamoxifen. Ann Oncol 2004; 15: 885–890.
Riggins RB, Zwart A, Nehra R, Clarke R . The nuclear factor kappa B inhibitor parthenolide restores ICI 182,780 (Faslodex; fulvestrant)-induced apoptosis in antiestrogen-resistant breast cancer cells. Mol Cancer Ther 2005; 4: 33–41.
Frasor J, Weaver A, Pradhan M, Dai Y, Miller LD, Lin CY et al. Positive cross-talk between estrogen receptor and NF-kappaB in breast cancer. Cancer Res 2009; 69: 8918–8925.
Stanculescu A, Bembinster LA, Borgen K, Bergamaschi A, Wiley E, Frasor J . Estrogen promotes breast cancer cell survival in an inhibitor of apoptosis (IAP)-dependent manner. Horm Cancer 2010; 1: 127–135.
Toyoshima Y, Karas M, Yakar S, Dupont J, Lee H, LeRoith D . TDAG51 mediates the effects of insulin-like growth factor I (IGF-I) on cell survival. J Biol Chem 2004; 279: 25898–25904.
Sakthianandeswaren A, Christie M, D'Andreti C, Tsui C, Jorissen RN, Li S et al. PHLDA1 expression marks the putative epithelial stem cells and contributes to intestinal tumorigenesis. Cancer Res 2011; 71: 3709–3719.
Van Laere S, Limame R, Van Marck EA, Vermeulen PB, Dirix LY . Is there a role for mammary stem cells in inflammatory breast carcinoma?: a review of evidence from cell line, animal model, and human tissue sample experiments. Cancer 2010; 116: 2794–2805.
Ben-Porath I, Thomson MW, Carey VJ, Ge R, Bell GW, Regev A et al. An embryonic stem cell-like gene expression signature in poorly differentiated aggressive human tumors. Nat Genet 2008; 40: 499–507.
Choi WY, Giraldez AJ, Schier AF . Target protectors reveal dampening and balancing of Nodal agonist and antagonist by miR-430. Science 2007; 318: 271–274.
Bridge G, Monteiro R, Henderson S, Emuss V, Lagos D, Georgopoulou D et al. The microRNA-30 family targets DLL4 to modulate endothelial cell behavior during angiogenesis. Blood 2012; 120: 5063–5072.
Kim K, Madak-Erdogan Z, Ventrella R, Katzenellenbogen BS . A MicroRNA196a2* and TP63 circuit regulated by estrogen receptor-alpha and ERK2 that controls breast cancer proliferation and invasiveness properties. Horm Cancer 2013; 4: 78–91.
Knauss JL, Bian S, Sun T . Plasmid-based target protectors allow specific blockade of miRNA silencing activity in mammalian developmental systems. Front Cell Neurosci 2013; 7: 163.
Makino K, Jinnin M, Aoi J, Hirano A, Kajihara I, Makino T et al. Discoidin domain receptor 2-microRNA 196a-mediated negative feedback against excess type I collagen expression is impaired in scleroderma dermal fibroblasts. J Invest Dermatol 2013; 133: 110–119.
Ouyang YB, Lu Y, Yue S, Giffard RG . miR-181 targets multiple Bcl-2 family members and influences apoptosis and mitochondrial function in astrocytes. Mitochondrion 2012; 12: 213–219.
Maillot G, Lacroix-Triki M, Pierredon S, Gratadou L, Schmidt S, Benes V et al. Widespread estrogen-dependent repression of micrornas involved in breast tumor cell growth. Cancer Res 2009; 69: 8332–8340.
Ponti D, Costa A, Zaffaroni N, Pratesi G, Petrangolini G, Coradini D et al. Isolation and in vitro propagation of tumorigenic breast cancer cells with stem/progenitor cell properties. Cancer Res 2005; 65: 5506–5511.
Charafe-Jauffret E, Monville F, Ginestier C, Dontu G, Birnbaum D, Wicha MS . Cancer stem cells in breast: current opinion and future challenges. Pathobiology 2008; 75: 75–84.
Li X, Lewis MT, Huang J, Gutierrez C, Osborne CK, Wu MF et al. Intrinsic resistance of tumorigenic breast cancer cells to chemotherapy. J Natl Cancer Inst 2008; 100: 672–679.
O'Brien CS, Howell SJ, Farnie G, Clarke RB . Resistance to endocrine therapy: are breast cancer stem cells the culprits? J Mammary Gland Biol Neoplasia 2009; 14: 45–54.
Clarke MF, Dick JE, Dirks PB, Eaves CJ, Jamieson CH, Jones DL et al. Cancer stem cells—perspectives on current status and future directions: AACR Workshop on cancer stem cells. Cancer Res 2006; 66: 9339–9344.
Diehn M, Cho RW, Lobo NA, Kalisky T, Dorie MJ, Kulp AN et al. Association of reactive oxygen species levels and radioresistance in cancer stem cells. Nature 2009; 458: 780–783.
Murohashi M, Hinohara K, Kuroda M, Isagawa T, Tsuji S, Kobayashi S et al. Gene set enrichment analysis provides insight into novel signalling pathways in breast cancer stem cells. Br J Cancer 2010; 102: 206–212.
Cao Y, Luo JL, Karin M . IkappaB kinase alpha kinase activity is required for self-renewal of ErbB2/Her2-transformed mammary tumor-initiating cells. Proc Natl Acad Sci USA 2007; 104: 15852–15857.
Iliopoulos D, Hirsch HA, Struhl K . An epigenetic switch involving NF-kappaB, Lin28, Let-7 MicroRNA, and IL6 links inflammation to cell transformation. Cell 2009; 139: 693–706.
Charafe-Jauffret E, Ginestier C, Iovino F, Tarpin C, Diebel M, Esterni B et al. Aldehyde dehydrogenase 1-positive cancer stem cells mediate metastasis and poor clinical outcome in inflammatory breast cancer. Clin Cancer Res 2010; 16: 45–55.
Fillmore CM, Gupta PB, Rudnick JA, Caballero S, Keller PJ, Lander ES et al. Estrogen expands breast cancer stem-like cells through paracrine FGF/Tbx3 signaling. Proc Natl Acad Sci USA 2010; 107: 21737–21742.
Baumgarten SC, Frasor J . Inflammation: an instigator of more aggressive estrogen receptor (ER) positive breast cancers. Mol Endocrinol 2012; 26: 360–371.
Pradhan M, Baumgarten SC, Bembinster LA, Frasor J . CBP mediates NF-kappaB-dependent histone acetylation and estrogen receptor recruitment to an estrogen response element in the BIRC3 promoter. Mol Cell Biol 2012; 32: 569–575.
Pradhan M, Bembinster LA, Baumgarten SC, Frasor J . Proinflammatory cytokines enhance estrogen-dependent expression of the multidrug transporter gene ABCG2 through estrogen receptor and NF{kappa}B cooperativity at adjacent response elements. J Biol Chem 2010; 285: 31100–31106.
Frasor J, Weaver AE, Pradhan M, Mehta K . Synergistic up-regulation of prostaglandin E synthase expression in breast cancer cells by 17beta-estradiol and proinflammatory cytokines. Endocrinology 2008; 149: 6272–6279.
Meier-Noorden M, Flindt S, Kalinke U, Hinz T . A CpG-rich bidirectional promoter induces the T-cell death-associated gene 51 and downregulates an inversely oriented transcript during early T-cell activation. Gene 2004; 338: 197–207.
Croker AK, Allan AL . Cancer stem cells: implications for the progression and treatment of metastatic disease. J Cell Mol Med 2008; 12: 374–390.
Velasco-Velazquez MA, Popov VM, Lisanti MP, Pestell RG . The role of breast cancer stem cells in metastasis and therapeutic implications. Am J Pathol 2011; 179: 2–11.
Hollier BG, Evans K, Mani SA . The epithelial-to-mesenchymal transition and cancer stem cells: a coalition against cancer therapies. J Mammary Gland Biol Neoplasia 2009; 14: 29–43.
Johnson EO, Chang KH, de Pablo Y, Ghosh S, Mehta R, Badve S et al. PHLDA1 is a crucial negative regulator and effector of Aurora A kinase in breast cancer. J Cell Sci 2011; 124: 2711–2722.
Taylor MA, Sossey-Alaoui K, Thompson CL, Danielpour D, Schiemann WP . TGF-beta upregulates miR-181a expression to promote breast cancer metastasis. J Clin Invest 2013; 123: 150–163.
Neel JC, Lebrun JJ . Activin and TGFbeta regulate expression of the microRNA-181 family to promote cell migration and invasion in breast cancer cells. Cell Signal 2013; 25: 1556–1566.
Bisso A, Faleschini M, Zampa F, Capaci V, De Santa J, Santarpia L et al. Oncogenic miR-181a/b affect the DNA damage response in aggressive breast cancer. Cell Cycle 2013; 12: 1679–1687.
Lobry C, Oh P, Mansour MR, Look AT, Aifantis I . Notch signaling: switching an oncogene to a tumor suppressor. Blood 2014; 123: 2451–2459.
Thorner AR, Parker JS, Hoadley KA, Perou CM . Potential tumor suppressor role for the c-Myb oncogene in luminal breast cancer. PLoS ONE 2010; 5: e13073.
Dontu G, Abdallah WM, Foley JM, Jackson KW, Clarke MF, Kawamura MJ et al. In vitro propagation and transcriptional profiling of human mammary stem/progenitor cells. Genes Dev 2003; 17: 1253–1270.
Gupta PB, Onder TT, Jiang G, Tao K, Kuperwasser C, Weinberg RA et al. Identification of selective inhibitors of cancer stem cells by high-throughput screening. Cell 2009; 138: 645–659.
Seiler CY, Park JG, Sharma A, Hunter P, Surapaneni P, Sedillo C et al. DNASU plasmid and PSI:Biology-Materials repositories: resources to accelerate biological research. Nucleic Acids Res 2014; 42: D1253–D1260.
Cormier CY, Park JG, Fiacco M, Steel J, Hunter P, Kramer J et al. PSI:Biology-materials repository: a biologist's resource for protein expression plasmids. J Struct Funct Genomics 2011; 12: 55–62.
Cormier CY, Mohr SE, Zuo D, Hu Y, Rolfs A, Kramer J et al. Protein Structure Initiative Material Repository: an open shared public resource of structural genomics plasmids for the biological community. Nucleic Acids Res 2010; 38: D743–D749.
Yang X, Boehm JS, Yang X, Salehi-Ashtiani K, Hao T, Shen Y et al. A public genome-scale lentiviral expression library of human ORFs. Nat Methods 2011; 8: 659–661.
Gyorffy B, Lanczky A, Szallasi Z . Implementing an online tool for genome-wide validation of survival-associated biomarkers in ovarian-cancer using microarray data from 1287 patients. Endocr Relat Cancer 2012; 19: 197–208.
Acknowledgements
We thank Shuangping Zhao, Bryant Marure and Tuan-Ahn Tran for technical assistance. We are grateful for the financial support provided by the National Institute of Health (R01 CA130932-05 to JF), the University of Illinois at Chicago through the Chancellor’s Discovery Fund (JF), and by a postdoctoral fellowship grant from Susan G Komen for the Cure to IK (PDF12229484).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies this paper on the Oncogene website
Supplementary information
Rights and permissions
About this article
Cite this article
Kastrati, I., Canestrari, E. & Frasor, J. PHLDA1 expression is controlled by an estrogen receptor-NFκB-miR-181 regulatory loop and is essential for formation of ER+ mammospheres. Oncogene 34, 2309–2316 (2015). https://doi.org/10.1038/onc.2014.180
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/onc.2014.180
This article is cited by
-
PHLDA1 is a P53 target gene involved in P53-mediated cell apoptosis
Molecular and Cellular Biochemistry (2023)
-
microRNA Regulation in Estrogen Receptor-Positive Breast Cancer and Endocrine Therapy
Biological Procedures Online (2018)
-
Circ_0027599/PHDLA1 suppresses gastric cancer progression by sponging miR-101-3p.1
Cell & Bioscience (2018)
-
MiR-181 family-specific behavior in different cancers: a meta-analysis view
Cancer and Metastasis Reviews (2018)
-
Full antagonism of the estrogen receptor without a prototypical ligand side chain
Nature Chemical Biology (2017)