Abstract
Stromal–epithelial interactions dictate prostate tumorigenesis and response to castration. Hydrogen peroxide-inducible clone 5 (Hic-5/ARA55) is a transforming growth factor-beta (TGF-β)-induced coactivator of androgen receptor (AR) expressed in the prostate stroma. Interestingly, following castration, we identified epithelial expression of Hic-5/ARA55 in mouse and human prostate tissues. To determine the role of epithelial Hic-5 in prostate cancer progression and castration responsiveness, we compared LNCaP cells having Hic-5 stably expressed with the parental LNCaP cells following tissue recombination xenografts with mouse prostate stromal cells. We previously identified knocking out prostate stromal TGF-β signaling potentiated castrate-resistant prostate tumors, in a Wnt-dependent manner. The LNCaP chimeric tumors containing prostate fibroblasts conditionally knocked out for the TGF-β type II receptor (Tgfbr2-KO) resulted in larger, more invasive, and castration-resistant tumors compared those with floxed (control) stromal cells. However, the LNCaP-Hic5 associated with Tgfbr2-KO fibroblasts generated chimeric tumors with reduced tumor volume, lack of invasion and restored castration dependence. Neutralization of canonical Wnt signaling is shown to reduce prostate tumor size and restore regression following castration. Thus, we hypothesized that epithelial Hic-5/ARA55 expression negatively regulated Wnt signaling. The mechanism of the Hic-5/ARA55 effects on castration was determined by analysis of the c-myc promoter. C-myc luciferase reporter activity suggested Hic-5/ARA55 expression inhibited c-myc activity by β-catenin. Sequential ChIP analysis indicated β-catenin and T-cell-specific 4 (TCF4) bound the endogenous c-myc promoter in the absence of Hic-5 expression. However, the formation of a TCF4/Hic-5 repressor complex inhibited c-myc promoter activity, by excluding β-catenin binding with TCF4 on the promoter. The data indicate Hic-5/ARA55 expression in response to castration-enabled epithelial regression through the repression of c-myc gene at the chromatin level.
Similar content being viewed by others
Introduction
Prostate cancer is the most commonly diagnosed cancer and is increasing with the expanding aging population. As the prostate is an androgen-dependent organ, various methods of androgen depletion have therapeutic benefit for prostate cancer. However, castrate-resistant prostate cancer is common and is the second leading cause of cancer-related death in men in the United States (Jemal et al., 2009). The microenvironment has a critical role in the emergence and progression of prostate cancer. Cancer-associated fibroblasts contribute to the progression of prostate and other epithelial cancers (Chung et al., 2005; Hwang et al., 2008; Taylor and Risbridger, 2008). In a reciprocal manner, paracrine signals from the epithelial compartment contribute to stromal differentiation (Mukaratirwa et al., 2005; Kass et al., 2007; Cunha, 2008). The prostate stromal cells, like the prostate luminal epithelia, express androgen receptor (AR) and depend on androgens for growth, survival and differentiation (Cunha, 2008). However, on androgen depletion, such as through castration, the stromal compartment regresses only a fraction of the epithelial compartment (Uke et al., 1983; Johansson et al., 2007; Placencio et al., 2008). Androgen signaling of the prostate stroma is identified as a mediator for epithelial androgen responsiveness (Cunha, 2008; Kurita et al., 2001). More recently, transforming growth factor-beta (TGF-β) responsiveness of the stromal fibroblasts was observed to enable prostate epithelial regression following castration (Placencio et al., 2008). A better understanding of stromal–epithelial interactions is emerging to be especially critical for the regulation of prostate cancer progression and castrate resistance.
The prostate requires androgens in development for proliferation and differentiation. Androgens are shown to be important in maintaining prostate epithelial quiescence following maturation (Niu et al., 2008). However, it is less clear what enables prostate regression in the absence of androgens. A mouse model with a conditional stromal knockout of the TGF-β type II receptor (Tgfbr2fspKO) indicates the stromal fibroblasts contribute to prostate tumor initiation, progression, and responsiveness to androgens (Bhowmick et al., 2004; Placencio et al., 2008). The knockout TGF-β responsiveness of stroma resulted in the constitutive expression of Wnt ligands, including Wnt3a, from the stroma stimulating epithelial Wnt target genes (Li et al., 2008). The canonical Wnt pathway is associated with the stabilization and binding of β-catenin with the lymphoid enhancer binding factor/T-cell-specific factor transcription factors to activate Wnt target genes (Moon, 2005). Constitutive epithelial Wnt signaling stimulated prostate proliferation, regardless of androgen status in Tgfbr2fspKO mice. The exogenous neutralization of canonical Wnt/β-catenin signaling restored both adult prostate epithelial quiescence and response to castration in Tgfbr2fspKO mice (Li et al., 2008; Placencio et al., 2008). As expected, the control, Tgfbr2floxE2/floxE2 mice prostate regressed following androgen ablation. However, the control stromal cells expressed canonical Wnt ligands (Placencio et al., 2008). Thus, we hypothesized an endogenous mechanism for antagonizing β-catenin/Wnt signaling in the prostate epithelia enables castration responsiveness.
In this study, we sought to explain a mechanism for castration-dependent prostate regression. β-catenin and T-cell-specific 4 (TCF) proteins interact with the AR to support androgen-dependent transcriptional activity and promote castration-independent survival and proliferation of prostate epithelia (Truica et al., 2000; Schweizer et al., 2008; Wang et al., 2008). On the basis of the data in Xenopus that suggest the protein hydrogen peroxide-inducible clone 5 (Hic-5) could bind and antagonize TCF-dependent signaling (Ghogomu et al., 2006), we focused on this originally described stromal-specific protein. The human homolog of Hic-5 was identified as a TGF-β1-inducible gene that associates with AR (ARA55) (Shibanuma et al., 1994; Fujimoto et al., 1999; Heitzer and DeFranco, 2006, 2007). ARA55 expression is elevated during cellular senescence of normal human fibroblastic cells. Hic-5/ARA55 binds to and potentates signaling by many nuclear steroid receptors, including the androgen receptor (Thomas et al., 1999; Zhang et al., 2000; Guerrero-Santoro et al., 2004; Shibanuma et al., 2004; Drori et al., 2005; Heitzer and DeFranco, 2006). In a surprising finding, we observed that Hic-5/ARA55 was expressed in the epithelial compartment of both mouse and human prostate tissues following androgen deprivation. Experiments of exogenous Hic-5 expression in LNCaP prostatic epithelia inhibited tumor growth in vivo and restored regression after androgen ablation in chimeric tumors of LNCaP epithelia and Tgfbr2-KO stromal cells. The mechanism elucidated in this study suggests that epithelial Hic-5/ARA55 represses the Wnt target, c-myc gene promoter in an androgen-dependent manner. Further, androgen deprivation potentiated β-catenin-mediated c-myc activity in prostate epithelia can be inhibited by Hic-5/ARA55 expression in a TCF4-dependent and -independent manner.
Results
Hic-5/ARA55 is expressed in prostate epithelia following castration
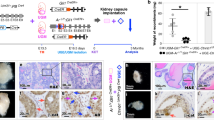
TGF-β is upregulated in the prostate following castration (Kyprianou and Isaacs, 1989; Muir et al., 1994). Previous reports suggest that the stromal response to TGF-β supports epithelial regression in a paracrine manner (Placencio et al., 2008). However, the direct epithelial response to TGF-β in the microenvironment has not been clearly identified. As Hic-5/ARA55 is induced by TGF-β and an AR cofactor, we examined its expression in mouse prostates following castration. Immunohistochemical localization of Hic-5/ARA55 in intact wild-type C57BL/6 mice indicated exclusive expression in the prostate stromal compartment, as previously reported (Heitzer and DeFranco, 2007). However, 3 and 7 days following castration, Hic-5/ARA55 was detected in both the epithelial and stromal compartments (n=12, Figure 1).
Encouraged by the consistent data in mice, this finding was verified in human prostate tissue. Prostate cancer and adjacent benign tissue from nine patients had a mean pathological Gleason score of 6.9±0.6 and presurgical prostate-specific antigen (PSA) of 5.0 μg/ml±1.8. The benign and cancer tissues from each patient were xenografted in contralateral kidneys of two male severe combined immunodeficient (SCID) mice for 1 week. All grafts were collected from mice 7 days following castration or the same period of time from intact mice. All benign and prostate cancer tissue grafts from intact hosts had only stromal Hic-5/ARA55 expression. Following castration, seven out of nine grafts had both epithelial and stromal Hic-5/ARA55 expression (Figure 2). Both prostate cancer and benign tissue had similar patterns of Hic-5/ARA55 expression. The Fisher's exact test suggested castration-dependent Hic-5/ARA55 epithelial expression is significant (P-value=0.003).
Human prostate epithelia expressed ARA55 in response to androgen ablation. ARA55 was localized in the prostate stroma of benign and cancer tissues xenografted in intact host mice. ARA55 was in addition detected in the epithelial compartment of benign and cancer prostate tissues harvested from hosts mice following 7 days of castration. Scale bar indicates 50 μm.
Hic-5 expression in LNCaP cells reduced prostate tumor growth and restored castrate responsiveness
The novel identification of Hic-5/ARA55 in the prostate epithelia associated with castration-dependent regression in both mouse and human tissues initiated this study on its epithelial function. As LNCaP cells do not express Hic-5, LNCaP cells were made to stably express Hic-5 (LNCaP-Hic5) by lentiviral transduction. The expression of Hic-5 protein was confirmed by western blot analysis (Figure 3a). To determine the role of Hic-5/ARA55 expression in prostate cancer tumorigenesis and responsiveness to androgen, we xenografted tissue recombinants of LNCaP or LNCaP-Hic5 epithelia with Tgfbr2-flox or Tgfbr2-KO prostate stroma cells. After the grafts established in 4 weeks, half of the host SCID mice were castrated. After a further 3 weeks, the castrated and control host mice were killed. The representative tumor growth is illustrated and quantitated in Figure 3b and c (n=6 for each chimeric tumor group). Parental LNCaP recombinant tumors with Tgfbr2-KO prostate stromal cells developed tumors fourfold larger in volume compared with control recombinants with Tgfbr2-flox prostate stroma cells (P<0.001). None of the LNCaP/Tgfbr2-flox recombinant grafts in castrated-host mice had detectable tumors. However, the chimeric LNCaP/Tgfbr2-KO tumors in intact and castrated-host mice had similar tumor volumes. These results confirmed our previous study in Tgfbr2fspKO mice having castration-resistant prostate growth (Placencio et al., 2008). Further, there was no detectible tumor growth in any of the LNCaP-Hic5/Tgfbr2-flox recombinants. The LNCaP/Tgfbr2-KO recombinants were 4.4-fold larger than LNCaP-Hic5/Tgfbr2-KO tumors (P<0.001). Importantly, the LNCaP-Hic5/Tgfbr2-KO recombinants in castrated-host mice showed no tumor growth. As the LNCaP-Hic5 tumors were undetectable in multiple groups in this study, we repeated the identical experiment in host mice that were supplemented with testosterone, with expected greater tumor size (see Supplementary Figure 1). Regardless of the status of testosterone supplementation, LNCaP-Hic5 cells had reduced tumor growth.
Hic-5 inhibited LNCaP tumorigenicity and restored responsiveness to castration. (a) western blot indicated no Hic-5 expression in LNCaP cells, but strong Hic-5 expression in LNCaP-Hic5 cells. (b) Representative images of chimeric tumors generated from LNCaP and LNCaP-Hic5 epithelia recombined with either Tgfbr2-flox or Tgfbr2-KO mouse prostate stromal cells in intact or castrated (Cx) SCID host mice. Scale bar indicate 3 mm. (c) The tumor volumes were quantitated. ANOVA analysis suggested significant differences in LNCaP/Tgfbr2-KO tumors from intact (In) and castrated (Cx) mice compared with other recombinants (n=48, P<0.001). However, the growth of LNCaP/Tgfbr2-KO tumors had no significant difference in intact and castrated-host mice. The following chimeric tumors had no detectible growth: intact host mice with LNCaP-Hic5/Tgfbr2-flox recombinants and castrated-host mice with LNCaP/Tgfbr2-flox, LNCaP-Hic5/Tgfbr2-flox and LNCaP-Hic5/Tgfbr2-KO recombinants. A red horizontal line indicated the mean of six calculated tumor volumes per group.
The chimeric tumor margins differed when associated with Tgfbr2-flox versus Tgfbr2-KO stromal cells, although with similar cellular tumor histology (Figure 4a). The LNCaP and LNCaP-Hic5 cells were best detected by immunohistochemical localization of human mitochondria. The Tgfbr2-flox stroma-associated tumors had no detectible extracapsular invasion (Figure 4b). However, the LNCaP/Tgfbr2-KO recombinant tumors in the intact and castrated hosts had positively stained LNCaP cells invade into the kidney parenchyma. In contrast, the LNCaP-Hic5/Tgfbr2-KO recombinants had distinct tumor margins, in which no LNCaP-Hic5 cells were detected in the kidney parenchyma.
Hic-5 expression inhibited LNCaP recombinant tumor invasion and restored responsiveness to castration. (a) Representative H and E staining of the tissue recombinants xenografted under the renal capsule indicated areas of vascularity and graft/kidney interface. Note that no tumors were detected in LNCaP-Hic-5/Tgfbr2-flox recombinants from intact or castrated-host mice. ‘K’ indicates host SCID mice kidney tissue. (b) Immunohistochemistry of human mitochondrial marker distinguished the LNCaP and LNCaP-Hic-5 tumor epithelia from the mouse tissue. The LNCaP/Tgfbr2-flox and LNCaP-Hic5/Tgfbr2-KO chimeric tumors had distinct tumor margins (uninterrupted dashed line). The LNCaP/Tgfbr2-KO chimeric tumors invaded the host kidney under both intact and castration conditions (arrows). (c) Immunohistochemistry of phosphorylated-histone H3 was performed and cells undergoing mitosis were identified. Scale bar indicates 50 μm for panels (a–c). (d) The mitotic cells determined by phosphorylated-histone H3 staining were quantitated for each chimeric tumor in intact and castrated-host mice. No positive cells were found in the groups without any tumor growth. ANOVA significant differences of *P<0.05 and ***P<0.001 were identified.
The stark differences in tumor size and invasion mediated by the stromal TGF-β responsiveness and epithelial Hic-5 expression, suggested differences in tumor cell proliferation. To identify mitotic cells, we performed immunohistochemistry for phosphorylated-histone 3 (Figure 4c). Correlated with tumor volume, the quantitation of mitotic cells suggested a significant increase in proliferation when the LNCaP tumors were associated with Tgfbr2-KO prostate stroma compared with Tgfbr2-flox stromal cells (P<0.001). Castration had little effect on proliferation of the LNCaP/Tgfbr2-KO tumors compared with those in intact mice (Figures 4c and d). LNCaP-Hic5 cells had significantly fewer proliferating cells in Tgfbr2-KO-associated tumors compared with those LNCaP/Tgfbr2-flox or LNCaP/Tgfbr2-KO (P<0.001) and most prominently caused a loss of proliferation following castration (P<0.001). LNCaP-Hic5 cells were more proliferative than the parental LNCaP line in culture (data not shown). However, Hic-5 expression inhibited LNCaP tumor proliferation in vivo, restored the responsiveness to castration of LNCaP tumors, otherwise refractile to castration when associated with Tgfbr2-KO prostate stroma cells.
The findings with LNCaP-Hic5 cells were tested in PC3 prostate cancer cells, which have endogenous Hic-5/ARA55 expression. Further, PC3–AR cells, with exogenous expression of AR were tested (Litvinov et al., 2006a). First, we compared the expression of AR, β-catenin and Hic-5/ARA55 in LNCaP, LNCaP-Hic5, PC3 and PC3–AR cells, in vitro, under the conditions of control, dihydrotestosterone (DHT) and bicalutamide (Bic) treatment (Supplementary Figure 2). The treatment of LNCaP cells with DHT or Bic did not induce the expression of Hic-5/ARA55 in vitro. The exogenous expression of Hic-5/ARA55 in LNCaP cells was 1.5-fold of the physiological expression level in PC3 cells. Interestingly, exogenous AR expression in PC3 cells significantly reduced Hic-5/ARA55 expression. The expression level of β-catenin was consistent in all the cells, regardless of treatment. Tissue recombination of PC3 with Tgfbr2-Flox and Tgfbr2-KO prostate stromal cells similarly developed large castrate-resistant tumors (Supplementary Figure 3). However, no tumor growth was detected in recombinants of PC3–AR cells with either of the prostate stromal cell type (Supplementary Figure 3). Thus, we focused on LNCaP and LNCaP-Hic5 cells for further Hic-5/ARA55 mechanistic studies on tumor growth and castration dependence.
Hic-5 antagonizes c-myc activity
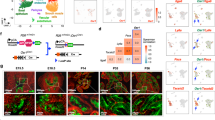
Upregulation of epithelial Wnt signaling in human and Tgfbr2fspKO mouse model has been associated with increased tumorigenicity and castrate-independent response in prostate cancer cells (Li et al., 2008; Placencio et al., 2008; Wang et al., 2008). Thus, the role of epithelial Hic-5 expression in response to castration was explored in terms of regulation of the Wnt pathway. We initially verified the AR–coactivator function of Hic-5 using the PSA luciferase reporter. DHT treatment resulted in a tenfold PSA luciferase activity induction in LNCaP cells compared with control, and a further 23-fold induction in LNCaP-Hic5 cells (Figure 5a; P<0.001). The coexpression of constitutively active β-catenin (S37Y mutant) doubled PSA reporter activity over control in the presence or absence of Hic-5 expression. However, in the presence of DHT, the added expression of β-catenin had little effect on PSA luciferase activity. We speculated the significant increase of PSA luciferase activity by Hic-5 was because of induced AR expression in LNCaP-Hic5 cells, however, both western and immunohistochemistry analyses showed no difference in AR expression level (Supplementary Figure 2), and location between LNCaP and LNCaP-Hic5 cells (data not shown). As expected, Bic and DHT had respective inhibitory and stimulatory effects on PSA luciferase activity. Hic-5 expression further potentiated PSA luciferase activity by DHT compared with that in parental LNCaP cells (P<0.001), as previously reported (Fujimoto et al., 1999).
Hic-5 coactivated AR- and inhibited c-myc-transcriptional activity. (a) Luciferase reporter assay for the PSA promoter indicated androgen transcriptional activity of LNCaP (empty bars) and LNCaP-Hic5 (filled bars) cells under control (vehicle treated), bicalutamide (10−5 M Bic), dihydrotestosterone (10−8 M DHT) treatment and/or cotransfected with constitutively active S33Y β-catenin (β-cat). (b) Canonical Wnt signaling was measured by the c-myc promoter luciferase reporter assay in LNCaP and LNCaP-Hic5 cells under the same conditions as in panel A. (c) C-myc luciferase assays was performed on LNCaP and LNCaP-Hic5 cells following incubation with conditioned media from Tgfbr2-flox or Tgfbr2-KO prostate stromal cells. Data shown in panels (a–c) is representative of at least three separate experiments performed in triplicate. The luciferase activities are normalized to protein concentration. ANOVA significant differences of **P<0.01, and ***P<0.001 were identified.
Next, the effect of Hic-5 regulation on canonical Wnt target gene reporter, c-myc-luciferase construct, was tested under the same conditions of the PSA luciferase assay (Figure 5b). Bic, DHT treatment alone or Hic-5 expression in LNCaP cells did not affect the c-myc luciferase activity. The exogenous expression of S37Y–β-catenin upregulated c-myc reporter activity in LNCaP cells sixfold over control (P<0.001) and was further enhanced twofold by the supplementation of DHT (P<0.001). However, the expression of Hic-5 inhibited c-myc luciferase activity induced by β-catenin (P<0.001).
Previously we published that elevated Wnt ligands expression by Tgfbr2fspKO prostate stromal cells promote prostate tumorigenesis and by Tgfbr2-flox prostate stromal cells following Bic treatment (Li et al., 2008; Placencio et al., 2008). Note, that most Wnt ligands of mouse can bind to frizzled receptors of human origin. Further we found that Wnt3a neutralizing antibody could inhibit c-myc reporter activity and block LNCaP cell proliferation, induced by conditioned media from Tgfbr2-KO mouse prostate stromal cells (Li et al., 2008). We tested the role of Tgfbr2-flox and Tgfbr2-KO prostate stromal cell-derived factors on myc-reporter activity in LNCaP and LNCaP-Hic5 cells, by incubation with stromal-conditioned media. In LNCaP cells, the activation of c-myc luciferase reporter was elevated 2.6-fold when the cells were treated with Tgfbr2-KO stromal-conditioned media compared with that of Tgfbr2-flox stromal cells (P<0.05, Figure 5c). No significant induction of c-myc luciferase activity was observed in LNCaP-Hic5 cells with conditioned media from Tgfbr2-flox or Tgfbr2-KO stromal cells (P>0.05). Together, expression of Hic-5 inhibited the direct and paracrine-mediated c-myc activation in prostate epithelia.
Hic-5 inhibits c-myc gene by forming a suppressor complex
We next chose to identify how Hic-5 affected endogenous canonical Wnt transcriptional target, c-myc, in the context of androgen signaling agonists and antagonists. Chromatin immunoprecipitation (ChIP) and sequential ChIP analyses were performed on the human c-myc promoter in LNCaP and LNCaP-Hic5 cells. The c-myc promoter has two closely spaced TCF binding elements at −1156 bp TCF4 binding element (TBE1) and −589 bp (TBE2); each account for 50% of c-myc gene activation when β-catenin binds to TCF4 on the DNA (He et al., 1998). We observed similar occupancy of the transcriptional complex on these TBE1 and TBE2. The sequential ChIP experiments represented in this study were for the TBE2 c-myc promoter region (Figure 6). The specificity of ChIP and sequential ChIP analysis were confirmed by pull–down assay with normal mouse immunoglobulin G (Figures 6 and 7) and PCR amplification with exon 2 of c-myc gene (Figure 7). (Supplementary Figure 4 illustrates full gel images of the ChIP and sequential ChiP assays in Figure 6.) First, TCF4 occupation of the c-myc promoter in LNCaP and LNCaP-Hic5 cells were similar, regardless of treatment conditions. The coincident binding of TCF4 and β-catenin on the TBEs, suggestive of c-myc gene activation was prominent following either Bic or DHT treatment in LNCaP cells in subsequent sequential ChIP analysis. LNCaP-Hic5 cells had no coincident TBE binding of TCF4 and β-catenin under any treatment condition. In further effort to delineate how Hic-5 inhibited c-myc gene transcription, we found TBEs occupied by AR through TCF4 in LNCaP cells with Bic and DHT treatment. In LNCaP-Hic5 cells, only control conditions had cooperative occupation of AR and TCF4 on the c-myc promoter. Sequential ChIP analyses indicate Hic-5 occupancy of TCF4/TBEs under control and DHT-treated conditions in LNCaP-Hic5 cells, but not after Bic treatment. Thus, Hic-5 inhibited c-myc activity by binding with TCF4 on the TBEs in the promoter to prevent activation by β-catenin.
Hic-5 and TCF4 co-occupy the c-myc promoter in an androgen-dependent manner. LNCaP and LNCaP-Hic5 cells were treated with vehicle (con), DHT (10−8 M) or Bic (10−5 M) for 3 h. PCR products in the input panel were amplified using diluted chromatin that was not immunoprecipitated. Preimmune mouse IgG was used to detect nonspecific immunoprecipitated DNA. PCR products shown in gel are representatives of three separate experiments.
Hic-5 binds to the TBEs of the c-myc promoter in the presence of bicalutamide. The chromatin–protein complexes were pulled down by antibody for Hic-5. (a) PCR products in the input panel were amplified using diluted chromatin that was not immunoprecipitated. A mouse IgG was used to detect any nonspecific immunoprecipitated DNA. PCR products shown in gel are representatives of three separate experiments. (b) Relative changes in Hic-5 recruitment to the TBEs of c-myc promoter were quantitated by real-time qPCR, normalized by the input. Data are shown as an average of TBE1 and TBE2 binding of at least three independent experiments. ANOVA significant differences of **P<0.05.
Owing to the apparent differences in mechanism of c-myc transcriptional inhibition by Hic-5/ARA55 with Bic and DHT treatment, the possibility of Hic-5/ARA55 binding TBEs, independent of TCF4 was explored. We conducted individual ChIP analysis for TBEs of the c-myc promoter with antibodies for AR, β-catenin or Hic-5. The ChIP qPCR results were averaged for TBE1 and TBE2 to ease presentation (Figure 7). As previously reported, the individual ChIP results of AR and β-catenin were similar to that detected in the sequential ChIP analysis with TCF4, to suggest that AR and β-catenin associates with TBEs through TCF4 on the c-myc promoter (Truica et al., 2000). However, the individual ChIP of Hic-5 revealed the greatest TBE binding following Bic treatment, compared with that of control and DHT. This suggested that Hic-5 binds to TBEs on the c-myc promoter independent of TCF4 in the situations of androgen ablation by Bic. Thus, the suggested mechanism of Hic-5 inhibition of c-myc activation were through Hic-5/AR or Hic-5 exclusion of β-catenin binding with TCF4 on TBEs under control or DHT treatment, respectively, or through Hic-5 directly occupation of TBEs instead of TCF4 in the present of Bic.
Discussion
The role of Hic-5/ARA55 in stromal AR-mediated gene expression has been identified as a coactivator and was therefore initially suggested to promote prostate cancer cell growth (Rahman et al., 2003; Fujimoto et al., 2007). However, more recently Hic-5/ARA55 was reported inhibiting the androgen responsive for keratinocyte growth factor (Heitzer and DeFranco, 2007). The link of Hic-5/ARA55 to prostate cancer has been debated (Fujimoto et al., 2001, 2007; Mestayer et al., 2003; Miyoshi et al., 2003). In whole prostate tissue extracts, Hic-5/ARA55 expression was decreased when associated with prostate cancer, compared with benign tissue (Mestayer et al., 2003). However, this finding is likely not reflective of expression levels, as the ratio of stroma to epithelia also decreases in prostate cancer (Ayala et al., 2003). Immunohistochemical localization of Hic-5/ARA55 in benign and prostate cancer-associated stromal compartment was similar in human tissues (Figure 2). Previous reports suggest Hic-5/ARA55 expression contribute to prostate stromal responsiveness to androgens and mediates adjacent epithelial differentiation and growth (Heitzer and DeFranco, 2006). The first in vivo indication of Hic-5/ARA55 epithelial expression was found in the mouse and human prostate tissues following castration of host mice (Figures 1 and 2). This was an especially interesting finding as Hic-5/ARA55 regulates both TGF-β and AR activity—two established signaling pathways critical for prostate regression on castration. We had previously reported that mouse prostate stromal cells express Wnt ligands following castration or Bic treatment in vitro (Placencio et al., 2008). The paracrine activation of Wnt/β-catenin signaling in prostate epithelia contributes to epithelial survival following castration (Placencio et al., 2008). As prostates and prostate cancer normally respond to castration (at least initially), the observed Hic-5/ARA55 expression in the epithelia may be a means of inhibition of Wnt, specifically the c-myc gene at the chromatin level, to enable regression. On the basis of potential TCF4 repressor function of Hic-5/ARA55 for Wnt target genes in Xenopus development (Ghogomu et al., 2006), we hypothesized Hic-5/ARA55 could antagonize canonical Wnt signaling in human prostate tumorigenesis and regression in response to castration.
The activation of Wnt/β-catenin signaling is observed in 90% of human prostate cancer clinical samples, with upregulation of Wnt-responsive genes such as c-myc and Twist (Kwok et al., 2005; Gurel et al., 2008). The suppression of Wnt/β-catenin signaling inhibits prostate cancer progression and castration-resistant prostate cancer growth (Wang et al., 2008; Lu et al., 2009). The data in this study would support epithelial Hic-5 expression inhibit c-myc activity, an inherent response to androgen ablation (Placencio et al., 2008). However, immunohistochemistry for Hic-5/ARA55 also did not show elevation in LNCaP xenografts, following castration of host mice. As LNCaP cells do not express the TGF-β type II receptor (Guo and Kyprianou, 1999), and Hic-5 is a TGF-β1-dependent gene (Fujimoto et al., 1999), it was not surprising that Hic-5/ARA55 expression was not found in the LNCaP cells in vitro or in vivo.
Stromal–epithelial interactions are critical in prostate development and tumorigenesis. The previously generated Tgfbr2fspKO mice developed prostatic intraepithelial neoplasia lesions, with elevated expression of the Wnt target gene, c-myc in the epithelium (Bhowmick et al., 2004). More recent studies revealed Tgfbr2fspKO mice develop prostate adenocarcinoma (Li et al., 2008). Of the differentially regulated paracrine factors resulting from the TGF-β receptor knockout in the prostate stroma, Wnt3a was shown to be critical for tumor growth. Importantly, the Tgfbr2fspKO model resembles the clinical situation, in which 69% of the human prostate cancer tissues lose TGF-β type II receptor stromal expression (Li et al., 2008). Thus, the chimeric prostate tumors of control, Tgfbr2floxE2/floxE2 and Tgfbr2fspKO prostate stroma cells with LNCaP epithelia, provided a relevant recombinant model for prostate cancer. We had previously observed that Tgfbr2-KO prostate stroma cells promote approximately four fold greater LNCaP tumor growth in vivo than Tgfbr2-flox stromal cells (Li et al., 2008). Notably, the prostate cancer derived-LNCaP cells rarely develop tumors in subcutaneous or subrenal capsule grafts unless they are recombined with stromal fibroblasts (Gleave et al., 1991). In this study, we discovered that Hic-5 expression in LNCaP cells decreased Tgfbr2-KO fibroblast-associated recombinant tumor growth near to that observed with control stromal cells (Figure 3b and Supplementary Figure 1). Further, we observed significant regression of LNCaP-Hic5/Tgfbr2-KO tumors following castration (Figure 3b). The gross chimeric tumor size in intact and castrated-host mice directly correlated with the number of cells undergoing mitosis (Figures 3c and 4d). The stromal regulation of tumor size, proliferation and androgen responsiveness was dependent on epithelial Hic-5 expression. Together, it would suggest epithelial expression of Hic-5/ARA55 supports castration responsiveness, but the dominant role of prostate androgen responsiveness remains in the stromal compartment (Cunha, 2008; Placencio et al., 2008).
Epithelial Hic-5 expression prevented invasion of the LNCaP tumors. Interestingly, the highly metastatic prostate cancer cell line, PC3, has high Hic-5/ARA55 expression (Mestayer et al., 2003). Silencing Hic-5/ARA55 in prostate epithelial, DU145, cells inhibit TGF-β-mediated epithelial to mesenchymal transdifferentiation (Mestayer et al., 2003). In human breast epithelia, MCF10A, Hic-5/ARA55 promotes TGF-β-mediated epithelial to mesenchymal transdifferentiation through the downregulation of E-cadherin (Tumbarello and Turner, 2007). Thus, it has been suggested that ectopic expression of Hic-5/ARA55 in prostate carcinoma may stimulate tumor cell migration and invasion (Wang et al., 2008). On the contrary, this in vivo study confirmed in cells that have intact androgen signaling, exogenous expression of Hic-5 inhibited tumor invasion of LNCaP cells. It is noteworthy that the proliferation and tumorigenesis in AR-deficient PC3 is significantly diminished when AR is overexpressed as reported before and this study in the recombination with prostate stroma cells (Litvinov et al., 2006a, 2006b; Niu et al., 2008). Hic-5/ARA55 was previously reported to inhibit both Smad3 (TGF-β signaling mediator) and Smad7 (TGF-β signaling antagonist) through direct protein–protein interaction (Wang et al., 2005, 2008). Wang et al. suggested that the net result of blocking both Smad3 and Smad7 by Hic-5/ARA55 was likely associated with Smad2 transcriptional activity in stromal fibroblasts. Thus, similar Smad2-specific signals could be promoted in the prostate epithelia during prostate regression. However, the parental LNCaP cells do not respond to TGF-β (Jakowlew et al., 1997; Zhu et al., 2008). Hence, the lack of observed tumor invasion by LNCaP-Hic5 cells might be due to the inhibition of Wnt/β-catenin signaling, prominently associated proliferation and epithelial to mesenchymal transdifferentiation promotion.
To better understand the mechanism of Hic-5/ARA55 inhibition of c-myc activity in prostate epithelia, the results from luciferase, ChIP and sequential ChIP analyses need to be considered together. The inhibition of c-myc luciferase activity by Hic-5 expression in LNCaP cells and Hic-5 occupation of TBEs on c-myc promoter through TCF4 or directly would suggest, Hic-5 is a transcriptional suppressor of Wnt target genes by binding DNA directly or as Hic-5/TCF4 or Hic-5/AR/TCF4 complex in an androgen-dependent manner (Figures 5, 6 and 7). Interestingly, we found DHT stimulated β-catenin-induced c-myc luciferase activity in LNCaP cells. There are reports of DHT inhibiting TOPFlash (TCF/β-catenin) activity (not c-myc reporter) in the presence of androgen receptor expression (Chesire and Isaacs, 2002; Mulholland et al., 2003; Schweizer et al., 2008). Apart from the different reporter construct used, other cell lines such as SW480 cells (with a mutant antigen-presenting cells) (Chesire and Isaacs, 2002; Kaur et al., 2010), PC3 cells (with no exogenous β-catenin expression) (Mulholland et al., 2003) were the basis of their conclusions. As no one cell line can model the in vivo situation of stromal–epithelial interaction, we relied on the castration response, mouse and human prostate tissues demonstrated for the basis of the further mechanistic studies on Hic-5/ARA55. It is provocative to think that Hic-5/ARA55 expression may be a means of increasing sensitivity to ultralow concentrations of androgens in AR antagonist-treated patients (Rahman et al., 2003). However, we found that Hic-5 can inhibit c-myc in TCF4-dependent and independent mechanisms. Hic-5/ARA55 expression in prostate epithelia enables prostate regression in the absence of androgens. A future direction in prostate cancer therapeutics could involve combination treatment of androgen ablation and Hic-5/ARA55 protein or Hic-5/ARA55 mimics. Such therapy could eliminate a population of castration-resistant prostate cancers cells. Hic-5/ARA55 is a multifunctional protein interacting with multiple hormone receptors, as well as in focal adhesion complex proteins that shuttle between the cytoplasm and nucleus. This study identified the novel role for Hic-5/ARA55 on c-myc promoter activation through its interactions with TCF4 and AR. The role of Hic-5/ARA55 on other hormone receptors and cell–cell interactions would be important future studies.
Materials and methods
Human tissues
Prostate cancer and adjacent benign tissue were separated from fresh radical prostatectomy samples from patients undergoing surgery at Vanderbilt University Medical Center in 2009. Patients who had undergone hormone ablation therapy before surgery were excluded. All subjects were annotated based on age, presurgical serum PSA, pathological Gleason score, pathological stage, extracapsular involvement and surgical margin status (Supplementary Table). All samples were deidentified according to the Institutional Review Board, Vanderbilt University.
Animals
Tgfbr2floxE2/floxE2 and Tgfbr2fspKO mice bred on the C57BL/6 background were generated and maintained as previously described (Bhowmick et al., 2004). Adult male SCID mice and C57BL/6 mice were purchased from Harlan (Indianapolis, IN, USA). Vanderbilt Institutional Animal Care and Use Committee approved the animal procedures.
Cell culture
Primary mouse prostate stromal cell cultures were generated from 6- to 8-week-old Tgfbr2floxE2/floxE2 or Tgfbr2fspKO mice as described before (Li et al., 2008). Prostate stromal fibroblastic cells derived from Tgfbr2floxE2/floxE2 and Tgfbr2fspKO mice are termed Tgfbr2-flox and Tgfbr2-KO, respectively.
LNCaP, PC3 cells were purchased from ATCC (Manassas, VA, USA). LNCaP-Hic5 cells were generated by lentivirus transduction of parental LNCaP cells with Hic-5 cDNA, according to manufacturer directions (Invitrogen, Carlsbad, CA, USA). PC3–AR cells were derived from PC3 cells (Dr John T Isaacs, Johns Hopkins University). In the experiments with dihydrotestosterone DHT and Bic treatment, the cells were cultured in phenol red-free RPMI medium with 10% charcoal-stripped fetal bovine serum to reduce steroids from the media.
Tissue recombination and subrenal capsule xenografting
Tissue recombinants were generated by combining 100 000 prostate cancer epithelia with 250 000 Tgfbr2-flox or Tgfbr2-KO prostatic stromal cells in 50 μl of rat-tail collagen. The tissue recombinants were grafted under the renal capsule of SCID mice as previously described (Li et al., 2008). At 4 weeks following grafting, half of the host SCID mice were castrated for an additional 3 weeks. After a total 7 weeks following grafting, the mice were killed. The grafts were then removed, photographed and processed for histology evaluation. The tumors were measured and the volume calculated by the formula: volume=width × length × 0.52 using Image J program (developed by National Institutes of Health). It is noteworthy that the formula underestimates the volume of invasive tumors, and accordingly underestimates differences between small noninvasive and larger invasive tumors. Statistical significance of results was determined by analysis of variance.
Live human prostate tissues were grafted under the renal capsule of male SCID mice supplemented with testosterone-containing silastic tubing. Following 1 week of grafting, the host mice were either left intact or castrated, and the silastic tubing removed for an additional 7 days. All grafts were collected and histochemically evaluated 14 days following xenografting.
Immunohistochemistry
Immunohistochemical staining on paraffin-embedded tissue sections (5 μm) were conducted using antibodies against: phosphorylated-histone H3 (1:1000, Millipore, Billerica, MA, USA), and human mitochondria (1:100, Millipore). Appropriate HRP-conjugated secondary antibodies and DAB incubation (Dako North America, Carpinteria, CA, USA) was used for visualization. All sections were nuclear counter-stained with Hematoxylin Gill3 (Fisher, Pittsburgh, PA, USA). All slides were photographed on a Nikon Coolscope (Nikon instruments, Lewisville, TX, USA).
Transfection and luciferase assay
Prostate cancer cells were transfected with the PSA (Lee et al., 2000) or c-myc (He et al., 1998) reporter luciferase construct, alone or together, with constitutive active β-catenin (S37Y) cDNA construct using Lipofectamine LTX (Invitrogen), according to the manual. Next day, the cells were treated with DHT, Bic or with conditioned media from primary cultured Tgfbr2floxE2/floxE2 or Tgfbr2fspKO mice prostate stromal cells for 24 h before the cells were collected and analyzed for firefly luciferase activity, normalized to protein concentration. Statistical significance of results was determined by analysis of variance.
The PSA luciferase construct contains an enhancer region of PSA from −5824 to −3738 with three AREs and promoter regions of PSA from −320 to +12 with one ARE (Dr Robert Matusik, Vanderbilt University). The positive and negative controls in the PSA–luciferase experiments were the addition of DHT and Bic, respectively. The c-myc luciferase construct contains a 2.5 kb region of the c-myc promoter, which includes two TCF4 binding elements and two antigen-presenting cell-responsive regions (Dr Bert Vogelstein, The Johns Hopkins Oncology Center). The transfection of constitutive active β-catenin was the positive control for the activation of the c-myc-luc reporter.
Chromatin immunoprecipitation
Prostate cancer, LNCaP and LNCaP-Hic5 cells were treated 3 h with DHT or Bic before crosslinking, lysis and sonication, as described previously (Li et al., 2008). Chromatin fragments were immunoprecipitated with TCF4, β-catenin, AR or Hic-5/ARA55 antibodies (Santa Cruz, Santa Cruz, CA, USA) or preimmune mouse immunoglobulin G overnight at 4 °C. After immunoprecipitation, protein G agarose was added into each reaction tube to pull down the chromatin/protein–antibody complex as indicated by the EZ ChIP kit (Millipore). For sequential ChIPs, complexes immunoprecipitated with anti-TCF4 were eluted by incubation with 10 mM dithiothreitol for 10 min at 37 °C in ChIP dilution buffer, followed by reimmunoprecipitation with antibodies for AR, β-catenin, Hic-5/ARA55 or immunoglobulin G. PCRs were performed with 2 μl purified DNA for 30 cycles of amplification. The primers for the TBEs of the c-myc promoter were forward: 5′-GTGGCAATGCGTTGCTGGGTTATT-3′, reverse: 5′-ATAAATCATCGCAGGCGGAACAGC-3′ for TBE1; and forward: 5′-ACGTTTGCGGGTTACATACAGTGC-3′, reverse: 5′-GAGTCAGCAGAGACCCTTGTGAAA-3′ for TBE2. The forward primer 5′-CCCTCAACGTTAGCTTCACCAACA-3′, and reverse primer 5′-GCAGCAGCTCGAATTTCTTCCAGA-3′ for the internal region (exon 2) of c-myc were used as negative control. The quantification of precipitated-TCF4 binding site between groups was analyzed by ΔΔCt method, and normalized by input for the single ChIP and immunoglobulin G for the sequential ChIP. Statistical significance was determined by analysis of variance. The final PCR amplified-TBE fragments were also run on 1% agarose gels and visualized by ethidium bromide.
References
Ayala G, Tuxhorn JA, Wheeler TM, Frolov A, Scardino PT, Ohori M et al. (2003). Reactive stroma as a predictor of biochemical-free recurrence in prostate cancer. Clin Cancer Res 9: 4792–4801.
Bhowmick NA, Chytil A, Plieth D, Gorska AE, Dumont N, Shappell S . (2004). TGF-beta signaling in fibroblasts modulates the oncogenic potential of adjacent epithelia. Science 303: 848–851.
Chesire DR, Isaacs WB . (2002). Ligand-dependent inhibition of beta-catenin/TCF signaling by androgen receptor. Oncogene 21: 8453–8469.
Chung LW, Baseman A, Assikis V, Zhau HE . (2005). Molecular insights into prostate cancer progression: the missing link of tumor microenvironment. J Urol 173: 10–20.
Cunha GR . (2008). Mesenchymal–epithelial interactions: past, present, and future. Differentiation 76: 578–586.
Drori S, Girnun GD, Tou L, Szwaya JD, Mueller E, Xia K et al. (2005). Hic-5 regulates an epithelial program mediated by PPARgamma. Genes Dev 19: 362–375.
Fujimoto N, Miyamoto H, Mizokami A, Harada S, Nomura M, Ueta Y et al. (2007). Prostate cancer cells increase androgen sensitivity by increase in nuclear androgen receptor and androgen receptor coactivators; a possible mechanism of hormone-resistance of prostate cancer cells. Cancer Invest 25: 32–37.
Fujimoto N, Mizokami A, Harada S, Matsumoto T . (2001). Different expression of androgen receptor coactivators in human prostate. Urology 58: 289–294.
Fujimoto N, Yeh S, Kang HY, Inui S, Chang HC, Mizokami A et al. (1999). Cloning and characterization of androgen receptor coactivator, ARA55, in human prostate. J Biol Chem 274: 8316–8321.
Ghogomu SM, van Venrooy S, Ritthaler M, Wedlich D, Gradl D . (2006). HIC-5 is a novel repressor of lymphoid enhancer factor/T-cell factor-driven transcription. J Biol Chem 281: 1755–1764.
Gleave M, Hsieh JT, Gao CA, von Eschenbach AC, Chung LW . (1991). Acceleration of human prostate cancer growth in vivo by factors produced by prostate and bone fibroblasts. Cancer Res 51: 3753–3761.
Guerrero-Santoro J, Yang L, Stallcup MR, DeFranco DB . (2004). Distinct LIM domains of Hic-5/ARA55 are required for nuclear matrix targeting and glucocorticoid receptor binding and coactivation. J Cell Biochem 92: 810–819.
Guo Y, Kyprianou N . (1999). Restoration of transforming growth factor beta signaling pathway in human prostate cancer cells suppresses tumorigenicity via induction of caspase-1-mediated apoptosis. Cancer Res 59: 1366–1371.
Gurel B, Iwata T, Koh CM, Jenkins RB, Lan F, Van Dang C et al. (2008). Nuclear MYC protein overexpression is an early alteration in human prostate carcinogenesis. Mod Pathol 21: 1156–1167.
He TC, Sparks AB, Rago C, Hermeking H, Zawel L da Costa LT, Morin PJ et al. (1998). Identification of c-MYC as a target of the APC pathway. Science 281: 1509–1512.
Heitzer MD, DeFranco DB . (2006). Hic-5/ARA55, a LIM domain-containing nuclear receptor coactivator expressed in prostate stromal cells. Cancer Res 66: 7326–7333.
Heitzer MD, DeFranco DB . (2007). Hic-5/ARA55: a prostate stroma-specific AR coactivator. Steroids 72: 218–220.
Hwang RF, Moore T, Arumugam T, Ramachandran V, Amos KD, Rivera A et al. (2008). Cancer-associated stromal fibroblasts promote pancreatic tumor progression. Cancer Res 68: 918–926.
Jakowlew SB, Moody TW, Mariano JM . (1997). Transforming growth factor-beta receptors in human cancer cell lines: analysis of transcript, protein and proliferation. Anticancer Res 17: 1849–1860.
Jemal A, Siegel R, Ward E, Hao Y, Xu J, Thun MJ . (2009). Cancer statistics, 2009. CA Cancer J Clin 59: 225–249.
Johansson A, Jones J, Pietras K, Kilter S, Skytt A, Rudolfsson SH et al. (2007). A stroma targeted therapy enhances castration effects in a transplantable rat prostate cancer model. Prostate 67: 1664–1676.
Kass L, Erler JT, Dembo M, Weaver VM . (2007). Mammary epithelial cell: influence of extracellular matrix composition and organization during development and tumorigenesis. Int J Biochem Cell Biol 39: 1987–1994.
Kaur M, Velmurugan B, Tyagi A, Agarwal C, Singh RP, Agarwal R . (2010). Silibinin suppresses growth of human colorectal carcinoma SW480 cells in culture and xenograft through down-regulation of beta-catenin-dependent signaling. Neoplasia 12: 415–424.
Kurita T, Wang YZ, Donjacour AA, Zhao C, Lydon JP, O′Malley BW et al. (2001). Paracrine regulation of apoptosis by steroid hormones in the male and female reproductive system. Cell Death Differ 8: 192–200.
Kwok WK, Ling MT, Lee TW, Lau TC, Zhou C, Zhang X et al. (2005). Up-regulation of TWIST in prostate cancer and its implication as a therapeutic target. Cancer Res 65: 5153–5162.
Kyprianou N, Isaacs JT . (1989). Expression of transforming growth factor-beta in the rat ventral prostate during castration-induced programmed cell death. Mol Endocrinol 3: 1515–1522.
Lee SE, Jin RJ, Lee SG, Yoon SJ, Park MS, Heo DS et al. (2000). Development of a new plasmid vector with PSA-promoter and enhancer expressing tissue-specificity in prostate carcinoma cell lines. Anticancer Res 20: 417–422.
Li X, Placencio V, Iturregui JM, Uwamariya C, Sharif-Afshar AR, Koyama T et al. (2008). Prostate tumor progression is mediated by a paracrine TGF-beta/Wnt3a signaling axis. Oncogene 27: 7118–7130.
Litvinov IV, Antony L, Dalrymple SL, Becker R, Cheng L, Isaacs JT . (2006a). PC3, but not DU145, human prostate cancer cells retain the coregulators required for tumor suppressor ability of androgen receptor. Prostate 66: 1329–1338.
Litvinov IV, Vander Griend DJ, Antony L, Dalrymple S, De Marzo AM, Drake CG et al. (2006b). Androgen receptor as a licensing factor for DNA replication in androgen-sensitive prostate cancer cells. Proc Natl Acad Sci USA 103: 15085–15090.
Lu W, Tinsley HN, Keeton A, Qu Z, Piazza GA, Li Y . (2009). Suppression of Wnt/beta-catenin signaling inhibits prostate cancer cell proliferation. Eur J Pharmacol 602: 8–14.
Mestayer C, Blanchere M, Jaubert F, Dufour B, Mowszowicz I . (2003). Expression of androgen receptor coactivators in normal and cancer prostate tissues and cultured cell lines. Prostate 56: 192–200.
Miyoshi Y, Ishiguro H, Uemura H, Fujinami K, Miyamoto H, Miyoshi Y et al. (2003). Expression of AR associated protein 55 (ARA55) and androgen receptor in prostate cancer. Prostate 56: 280–286.
Moon RT . (2005). Wnt/beta-catenin pathway. Sci STKE 2005: cm1.
Muir GH, Butta A, Shearer RJ, Fisher C, Dearnaley DP, Flanders KC et al. (1994). Induction of transforming growth factor beta in hormonally treated human prostate cancer. Br J Cancer 69: 130–134.
Mukaratirwa S, Koninkx JF, Gruys E, Nederbragt H . (2005). Mutual paracrine effects of colorectal tumour cells and stromal cells: modulation of tumour and stromal cell differentiation and extracellular matrix component production in culture. Int J Exp Pathol 86: 219–229.
Mulholland DJ, Read JT, Rennie PS, Cox ME, Nelson CC . (2003). Functional localization and competition between the androgen receptor and T-cell factor for nuclear beta-catenin: a means for inhibition of the Tcf signaling axis. Oncogene 22: 5602–5613.
Niu Y, Altuwaijri S, Lai KP, Wu CT, Ricke WA, Messing EM et al. (2008). Androgen receptor is a tumor suppressor and proliferator in prostate cancer. Proc Natl Acad Sci USA 105: 12182–12187.
Placencio VR, Sharif-Afshar AR, Li X, Huang H, Uwamariya C, Neilson EG et al. (2008). Stromal transforming growth factor-beta signaling mediates prostatic response to androgen ablation by paracrine Wnt activity. Cancer Res 68: 4709–4718.
Rahman MM, Miyamoto H, Lardy H, Chang C . (2003). Inactivation of androgen receptor coregulator ARA55 inhibits androgen receptor activity and agonist effect of antiandrogens in prostate cancer cells. Proc Natl Acad Sci USA 100: 5124–5129.
Schweizer L, Rizzo CA, Spires TE, Platero JS, Wu Q, Lin TA et al. (2008). The androgen receptor can signal through Wnt/beta-Catenin in prostate cancer cells as an adaptation mechanism to castration levels of androgens. BMC Cell Biol 9: 4.
Shibanuma M, Kim-Kaneyama JR, Sato S, Nose K . (2004). A LIM protein, Hic-5, functions as a potential coactivator for Sp1. J Cell Biochem 91: 633–645.
Shibanuma M, Mashimo J, Kuroki T, Nose K . (1994). Characterization of the TGF beta 1-inducible hic-5 gene that encodes a putative novel zinc finger protein and its possible involvement in cellular senescence. J Biol Chem 269: 26767–26774.
Taylor RA, Risbridger GP . (2008). Prostatic tumor stroma: a key player in cancer progression. Curr Cancer Drug Targets 8: 490–497.
Thomas SM, Hagel M, Turner CE . (1999). Characterization of a focal adhesion protein, Hic-5, that shares extensive homology with paxillin. J Cell Sci 112 (Pt 2): 181–190.
Truica CI, Byers S, Gelmann EP . (2000). Beta-catenin affects androgen receptor transcriptional activity and ligand specificity. Cancer Res 60: 4709–4713.
Tumbarello DA, Turner CE . (2007). Hic-5 contributes to epithelial-mesenchymal transformation through a RhoA/ROCK-dependent pathway. J Cell Physiol 211: 736–747.
Uke E, Lee C, Grayhack JT . (1983). The effect of CIS hydroxyproline on ventral prostatic growth in rats. J Urol 129: 171–174.
Wang G, Wang J, Sadar MD . (2008). Crosstalk between the androgen receptor and beta-catenin in castrate-resistant prostate cancer. Cancer Res 68: 9918–9927.
Wang H, Song K, Krebs TL, Yang J, Danielpour D. . (2008). Smad7 is inactivated through a direct physical interaction with the LIM protein Hic-5/ARA55. Oncogene 27: 6791–6805.
Wang H, Song K, Sponseller TL, Danielpour D . (2005). Novel function of androgen receptor-associated protein 55/Hic-5 as a negative regulator of Smad3 signaling. J Biol Chem 280: 5154–5162.
Zhang J, Zhang LX, Meltzer PS, Barrett JC, Trent JM . (2000). Molecular cloning of human Hic-5, a potential regulator involved in signal transduction and cellular senescence. Mol Carcinog 27: 177–183.
Zhu ML, Partin JV, Bruckheimer EM, Strup SE, Kyprianou N . (2008). TGF-beta signaling and androgen receptor status determine apoptotic cross-talk in human prostate cancer cells. Prostate 68: 287–295.
Acknowledgements
We thank Drs Robert Matusik, Roger Jackson and Veronica Placencio for help in the preparation of this paper. The work was supported through Department of Defense (DAMD17-02-1-0063, PC081246) and NIH grants (CA108646, CA126505). The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Cancer Institute or the National Institutes of Health.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies the paper on the Oncogene website
Rights and permissions
This work is licensed under the Creative Commons Attribution-NonCommercial-Share Alike 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-sa/3.0/
About this article
Cite this article
Li, X., Martinez-Ferrer, M., Botta, V. et al. Epithelial Hic-5/ARA55 expression contributes to prostate tumorigenesis and castrate responsiveness. Oncogene 30, 167–177 (2011). https://doi.org/10.1038/onc.2010.400
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/onc.2010.400
Keywords
This article is cited by
-
A Targeted Bivalent Androgen Receptor Binding Compound for Prostate Cancer Therapy
Hormones and Cancer (2019)
-
A reciprocal role of prostate cancer on stromal DNA damage
Oncogene (2014)
-
Genistein cooperates with the histone deacetylase inhibitor vorinostat to induce cell death in prostate cancer cells
BMC Cancer (2012)
-
Hic-5 controls BMP4 responses in prostate cancer cells through interacting with Smads 1, 5 and 8
Oncogene (2012)