Abstract
Background/Objectives:
Individually, genetic variants only moderately influence cardiometabolic (CM) traits, such as lipid and inflammatory markers. In this study we generated genetic risk scores from a combination of previously reported variants influencing CM traits, and used these scores to explore how adiposity levels could mediate genetic contributions to CM traits.
Subjects/Methods:
Participants included 1649 women from the 2005 Cebu Longitudinal Health and Nutrition Survey. Three genetic risk scores were constructed for C-reactive protein (CRP), high-density lipoprotein cholesterol (HDL-C) and triglycerides (TGs). We used linear regression models to assess the association between each genetic risk score and its related trait. We also tested for interactions between each score and measures of adiposity.
Results:
Each genetic risk score explained a greater proportion of variance in trait levels than any individual genetic variant. We found an interaction between the TG genetic risk score (2.29–14.34 risk alleles) and waist circumference (WC) (Pinteraction=1.66 × 10−2). Based on model predictions, for individuals with a higher TG genetic risk score (75th percentile=12), having an elevated WC (⩾80 cm) increased TG levels from 1.32 to 1.71 mmol l−1. However, for individuals with a lower score (25th percentile=7), having an elevated WC did not significantly change TG levels.
Conclusions:
The TG genetic risk score interacted with adiposity to synergistically influence TG levels. For individuals with a genetic predisposition to elevated TG levels, our results suggest that reducing adiposity could possibly prevent further increases in TG levels and thereby lessen the likelihood of adverse health outcomes such as cardiovascular disease.
Similar content being viewed by others
Introduction
Recent studies in both European and Asian cohorts have found multiple genetic variants relating to cardiometabolic (CM) traits such as lipid and inflammation levels.1, 2, 3, 4, 5 Individually, the identified genetic variants only moderately influence these trait levels and are thought to provide only limited information in clinically assessing an individual’s risk. However, the combination of genetic variants, each with a relatively small effect, may better explain the variability of such complex traits.6 Thus, the use of a genetic risk score has been proposed to better capture the effect of associated genetic variants on trait variability of an individual.7, 8, 9, 10
Genetic variants may interact with diet, environmental and anthropometric factors to influence CM phenotypes; accounting for synergistic effects may also help explain some of the variability of these traits.6 Excess adiposity is one of the strongest predictors of CM disease and risk.11, 12, 13, 14 Previous work suggests that measures of adiposity interact with specific genetic variants and predict CM traits.15, 16, 17
However, synergistic effects are not well understood, especially in low-middle-income populations undergoing rapid nutritional and lifestyle changes. Coinciding with economic development and urbanization, these changes include increased consumption of fats, caloric sweeteners and meats, along with greater sedentary behavior.18 Such lifestyle changes contribute to a growing burden of overweight, visceral adiposity and thus associated CM diseases.19, 20 These concerns are especially pertinent for Asians; compared with Caucasians, Asians have increased visceral adiposity and greater insulin resistance at similar levels of body mass index (BMI).21, 22, 23 In addition, the World Health Organization concluded that the risk of CM-based diseases is elevated for Asians with a BMI >23 kg m−2, suggesting the use of a lower cutpoint for overweight (OW).24
In this study we sought to: create genetic risk scores relating to inflammatory and lipid traits, examine the ability of these scores to explain the variation in such traits and test whether the genetic risk scores interact with measures of adiposity to influence trait levels. We chose to specifically look at C-reactive protein (CRP), high-density lipoprotein cholesterol (HDL-C) and triglycerides (TGs) because previous research suggests that these traits interact with various measures of adiposity.25, 26, 27 To accomplish this, we used an at-risk Asian population, from the 2005 Cebu Longitudinal and Health and Nutrition Survey (CLHNS), undergoing a nutrition and lifestyle transition. In particular, this cohort of women based in the Philippines showed a sixfold increase in prevalence of overweight and obesity associated with nearly 20 years of substantial and continuing socioeconomic modernization.28 This rapid transition allows us to capture changes one cannot capture so readily in the United States.
Subjects and methods
Survey design
The women in this study are participants in the CLHNS that is described in detail elsewhere.29 The CLHNS is a community-based cohort of women and their index children followed since 1983. In 2005, fasting blood was drawn for biomarkers and genetics. Here we use cross-sectional data from the mother cohort participating in the 2005 CLHNS. All data were collected under conditions of informed consent with institutional review board approval from the University of North Carolina at Chapel Hill (Chapel Hill, NC, USA).
We excluded women who were pregnant at the time of blood draw, not fasting at the time of blood draw and with CRP levels >95.24 nmol l−1 (10 mg l−1; a level representing current/recent illness rather than low-level basal inflammation).30 A total of 1649 women had complete biomarker, genetic, diet, socioeconomic and anthropometric data. Medication use in this population was low: 0.1% took statins, 1.75% took diabetes medication and 4% took antihypertensive medications. A sensitivity analysis showed that exclusion of these individuals did not affect the results, and hence we did not exclude anyone taking medication.
CM biomarkers
After a 12-h overnight fast, blood samples were collected using EDTA-coated tubes. Frozen blood samples were shipped to the Emory Lipid Research Laboratory (Atlanta, GA, USA) for lipid analysis. Total lipids were measured by enzymatic methods using reagents from Beckman Diagnostics (Palo Alto, CA, USA) on a CX5 chemistry analyzer. HDL-C was determined using the homogenous assay direct HDL-C (Genzyme Corporation, Exton, PA, USA). CRP concentrations were determined using a high-sensitivity immunoturbidimetric method (Synchron LX20, Beckman Coulter, Inc., Brea, CA, USA, lower detection limit: 0.95 nmol l−1).
The cutpoints used to define elevated risk for each trait were: >28.57 nmol l−1 (3.0 mg l−1) for CRP, <1.29 mmol l−1 (50 mg dl−1) for HDL-C and >1.69 mmol l−1 (150 mg dl−1) for TG levels. These were based on recommendations from the International Diabetes Federation (IDF) and the American Heart Association.30, 31, 32, 33
Anthropometry
Body weight, height and waist circumference (WC) were measured using standard techniques.34 BMI was calculated as the ratio of weight (kg) to height (m2). We used cutpoints for Asians to define normal weight as BMI <23 kg m−2, OW as 23 kg m−2 ⩽BMI < 27.5 kg m−2, obese as BMI ⩾27.5 kg m−2 and central adiposity as WC ⩾80 cm.24, 31
Dietary data
Dietary data were derived from two 24-h dietary recalls; mean energy and mean saturated fat intake was used in the analyses. Data were collected during in-home interviews performed by highly trained local field staff. A nutritionist reviewed all dietary recalls immediately after collection. When implausible values were found, interviewers revisited respondents for verification. Energy and saturated fat intakes were calculated using the Philippines Food Composition Tables.35, 36
Sociodemographic and lifestyle characteristics
Highly trained interviewers collected reproductive history data; this included menopausal status beginning in the 1991 survey.
Socioeconomic status was measured by a factor score based on a principal components analysis of household ownership of key assets such as television, vehicles and furniture.37
Infectious illness was measured by asking participants if they were currently experiencing any symptoms of infection, consistent with prior research on CRP.38 Symptoms included runny nose, cough, fever, diarrhea and sore throat, as well as the more general categories of flu, cold and sinusitis. Responses were used to construct a summary variable indicating the presence or absence of any infectious symptoms at the time of blood collection.
Environmental cleanliness and household hygiene was measured by a hygiene score based on data on the interviewer’s rating of cooking area, immediate area around the house, toilet type and water source. The score ranges from 0 to 9, with larger values indicating greater cleanliness.38
Genotyping, quality controls and imputation
The complete methods for direct single-nucleotide polymorphism (SNP) genotyping, quality control and SNP imputation have been described previously.39 Briefly, genotyping was performed with the Affymetrix Genome-Wide Human SNP Array 5.0 (Affymetrix, Inc., Santa Clara, CA, USA). Quality control procedures excluded: samples with <97% genotyping call rate; members of estimated first-degree relative pairs; SNPs with a call rate <90%; SNPs with a deviation from Hardy–Weinberg equilibrium (P<10−6); SNPs with ⩾3 discrepancies among duplicate pairs; SNPs with Mendelian inheritance errors among five CEPH trios and/or CEPH sample genotype discrepancies with HapMap. Genotype imputation was conducted with MACH using phased haplotypes from the 1000 Genomes Project in both CEU and CHB+JPT samples (June 2010 Release).40 In addition, we excluded any SNP with poor imputation quality (MACH r2<0.3) or estimated minor allele frequency) ⩽0.01.
Genetic marker selection
The process of choosing SNPs is depicted in Figure 1. The SNPs used to create the genetic risk scores were selected by finding SNPs associated with the individual CM traits of interest: CRP, HDL-C and TGs. We selected these SNPs from (1) genome-wide association studies conducted with our own study population,3, 41 (2) published genome-wide association studies of East and South East Asian cohorts1, 42 and (3) published genome-wide association studies of European descent cohorts,4 if the specific trait lacked studies conducted in populations of Asian descent. We limited our selection of studies to cohort-based studies and meta-analyses; case–control studies were not considered because we wanted to choose SNPs associated with the individual CM trait rather than disease state. From the studies identified, we selected SNPs with a P<5 × 10−8 in the original study population for further analysis; we increased this threshold to a P<5 × 10−5 for those studies conducted in our own study population because of the smaller sample size in the CLHNS.
Choosing of genetic variants to include in the genetic risk scores. (a) Schematic representation describing the process of choosing SNPs associated with CRP, HDL-C and TGs. Parentheses indicate the specific study population in which analyses were conducted. Numbers refer to reference papers. The r2<0.3 indicates poor SNP imputation quality. *rs1268004 was not genotyped and no HapMap or 1000 Genomes imputed data were available. See Subjects and Methods for further details.
The original studies were used to identify the risk allele. We designated the risk allele as the allele associated with an increased level of the specified trait, except in the case of HDL-C, for which we assigned the allele associated with lower levels of the trait. We coded SNPs as the number of copies of the risk allele (a continuous number between 0 and 2).
Three genetic risk scores were constructed, one for each CM trait, CRP, HDL-C, and TG. Before creating each genetic risk score, we chose a subset of SNPs with nominal significance (P<0.1) and directional consistency of the effect estimate in our study population. This was based on adjusted linear regression models of the natural log-transformed CM trait on the individual SNP (see model 2 in Subjects and methods). Then, for each CM trait, we pruned this subset of SNPs for redundancy because of linkage disequilibrium (r2 >0.2). To do this we first used the clump procedure in PLINK to create ‘clumps’ of correlated SNPs.43 Each clump was represented by the index SNP, designated as the SNP with the lowest P-value (see model 2 in Subjects and methods). Using these index SNPs, we calculated each genetic risk score by summing the risk alleles of each index SNP associated with the specific trait. We created an unweighted score instead of weighting by the effect of each SNP because: (1) the current literature does not provide stable effect estimates of each SNP for each trait; (2) the outcomes (and thus effects) across studies were noncomparable (for example, log-transformed trait vs nontransformed trait); (3) studies used populations of various sample sizes and ethnicities; and (4) using weights from the CLHNS data itself would have introduced bias.
Statistical analysis
Linear regression models, with each of the three CM traits as a continuous outcome, were used. All traits were natural log-transformed to satisfy model assumptions of normally distributed residuals. Given the markedly skewed distribution of CRP concentrations and the presence of many values below the detectable level (0.95 nmol l−1), CRP values were natural log-transformed after adding the constant 0.95.
We constructed principal components (PCs) using the software EIGENSOFT to capture population substructure among CLHNS subjects.44 We assessed the association between each of the first 10 PCs and each log-transformed CM trait to identify any potential ancestry explanatory PC; the 7th PC was significantly associated with CRP and HDL-C (no PCs were significantly associated with log TG levels), and thus the first 7 PCs were included as covariates in the linear regression models.
Two different models were examined; in both models the outcome was either log-transformed CRP, HDL-C and TG levels. Model 1 was a linear regression model adjusted for age (categorical: ⩽44, 45–49, 50–54 and ⩾55 years) and population substructure. Model 2 included covariates adjusted for in model 1 plus additional adjustment for postmenopausal status (yes/no), OW/obese status (BMI ⩾23 kg m−2), high WC (WC ⩾80 cm), % energy intake from saturated fat, energy intake, environmental hygiene, reported infectious illness (yes/no) and socioeconomic status. The covariates chosen for adjustment in model 2 were based on prior published studies in the CLHNS on these lipid and inflammatory traits.37, 38, 45 We categorized age, BMI and WC to account for their nonlinear relationship with the log CM trait levels.
Models 1 and 2 were applied to test for the association between each candidate SNP and its related log-transformed CM trait (assuming an additive genetic model). Then both models were applied to test for the association between each genetic risk score (continuous) and its related log-transformed CM trait. In addition, we examined the proportion of variance explained (Rsq) in the log-transformed CM trait by the genetic risk score vs the most strongly associated individual SNP in model 2 (see online-only Supplementary Table S1 and Supplementary Methods).
Finally, for each CM trait we looked at interactions between the genetic risk score and measures of adiposity. We examined a genetic risk score × elevated WC interaction, both unadjusted and adjusted for BMI (using a three-categorical dummy variable for normal weight, OW and obese). We adjusted for BMI to better isolate visceral fat’s effect on CM trait levels. Then we examined a genetic risk score × OW/obese status interaction, both unadjusted and adjusted for elevated WC. We adjusted for WC to better examine how overall fatness (regardless of fat distribution around the waist) influences CM trait levels. Each interaction was looked at separately while adjusting for the same covariates as model 2.
For regression analyses we used a statistical significance criteria of P<0.05 (two sided). For interaction terms we considered P<0.1 as nominally significant. After applying a Bonferroni correction for three independent tests, these significance criteria became P<0.033. All regression analyses were performed with Stata 12.0 (Stata Corporation, College Station, TX, USA).
Results
The characteristics of 1649 women participants in the 2005 CLHNS are presented in Table 1. In 2005, participants had a mean (s.d.) age of 48.41 (6.03) years. Approximately 39% of women were postmenopausal, 52% had elevated WC, 60% were OW, 20% had elevated CRP, 82% had low HDL-C and 29% had elevated TGs.
Our selection strategy for candidate SNPs relating to CRP, HDL-C and TGs resulted in 46, 19 and 13 usable variants (Figure 1). After pruning to eliminate correlated SNPs in linkage disequilibrium (by trait), 6 CRP, 9 HDL-C and 9 TG index SNPs were used in the construction of the genetic risk scores (Figure 1 and Supplementary Table S2). Among participants, each genetic risk score was normally distributed (Supplementary Figure S1). The mean score (s.d.) and range of number of risk alleles for CRP was 3.32 (1.37) with a range from 0.12 to 8.51; for HDL-C it was 5.95 (1.58) with a range from 1.61 to 11.66; and for it was TG 9.42 (1.85) with a range from 2.29 to 14.34.
The regression results from model 2 for each candidate SNP and its respective CM trait are shown in Supplementary Table S2 (results from model 1 were similar and thus not shown). Using model 2, the individual SNP most strongly associated with CRP was rs876537 at the CRP loci (β=0.33, 95% confidence interval (CI) 0.24, 0.42, P=2.27 × 10−12), with HDL-C it was rs12708980 at the CETP loci (β=−0.05, 95% CI −0.08, −0.03, P=6.61 × 10−7), and with TG it was rs964184 at the APOC3 loci (β=0.15, 95% CI 0.11, 0.19, P=3.37 × 10−15). The same SNPs were found to be most strongly associated with each trait in model 1 as well.
As expected, each of the three genetic risk scores was associated with its respective log-transformed trait (Table 2). Specifically in model 2, each additional CRP risk allele resulted in an estimated 18% increase in CRP levels (β=0.18, 95% CI 0.14, 0.23); each additional HDL-C risk allele resulted in an estimated 4% decrease in HDL-C levels (β= −0.04, 95% CI −0.05, −0.04); each additional TG risk allele resulted in an estimated 7% increase in TG levels (β= 0.07, 95% CI 0.06, 0.08).
We compared the proportion of variance explained (Rsq) in the log-transformed CM trait by the genetic risk score vs the most strongly associated individual SNP in model 2 (Figure 2). For all three traits, Rsq of genetic risk score >Rsq of individual SNP; ∼4% of log CRP levels, 7% of log HDL-C levels and 6% of log TG levels were explained by the genetic risk score alone (Table 2).
The proportion of variance explained by genetic risk score vs individual genetic variant most strongly associated with trait. The proportion of variance in the cardiometabolic trait explained by the genetic risk score vs the individual SNP most strongly associated with the trait. The individual SNP most strongly associated with CRP was rs876537, with HDL-C was rs12708980 and with TGs was rs964184.
We found significant interactions between measures of adiposity and the TG genetic risk score on log TG levels, whereas we found no evidence of such interactions on log CRP or log HDL-C levels (Supplementary Tables S3 and S4).
Stratifying by normal WC (<80 cm) and elevated WC (⩾80 cm), the estimated % increase in TG levels for each additional TG risk allele was 5% (β=0.05, 95% CI 0.03, 0.07) in normal WC individuals, but increased to 8% (β=0.08, 95% CI 0.06, 0.10) in elevated WC individuals (Pinteraction=1.66 × 10−2; Table 3). Here we present BMI-adjusted results; we found no difference between the effect estimate and P-value of the unadjusted model (results not shown).
Similarly, stratifying by normal weight (<23 kg m−2) and OW/obese (⩾23 kg m−2), the estimated % increase in TG levels for each additional TG risk allele was 5% (β=0.05, 95% CI 0.03, 0.07) in normal-weight individuals, but increased to 8% (β=0.08, 95% CI 0.06, 0.09) in OW/obese individuals (Pinteraction=2.73 × 10−2; Table 3). Here we present WC-adjusted results; we found no difference between the effect estimate and P-value of the unadjusted model (results not shown).
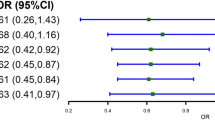
To better visualize these interactions (Figure 3), we predicted TG levels at the 25th and 75th percentile values of the genetic risk score (7 and 12, respectively) at varying levels of adiposity while holding all other covariates in model 2 at the mean. Based on model predictions, for individuals with a higher TG genetic risk score (=12), having an elevated WC (⩾80 cm) increased TG levels from 1.32 to 1.71 mmol l−1. However, for individuals with a lower score (=7), having an elevated WC made no significant impact on TG levels (1.05 vs 1.18 mmol l−1). Similar results were seen at varying levels of BMI.
Predicted TG levels at the 25th and 75th percentile values of the genetic risk score, stratified by levels of adiposity. Predicted geometric means (95% CI) of TGs at the 25th and 75th percentile values of the genetic risk score (7 and 12, respectively) at varying levels of WC and BMI: (a) Predicted levels of TG stratified by WC ⩾80 cm. (b) Predicted levels of TG stratified by overweight/obese (BMI ⩾23 kg m−2).
We also examined all the above interactions with each individual SNP included in the TG genetic risk score, but none of these interactions were significant (results not shown).
Discussion
In this study we used a genetic risk score to combine the relatively small additive effects of individual SNPs to better capture the complex relationship between genetics, adiposity and CM risk. We found that the genetic risk score more strongly predicted log-transformed CRP, HDL-C and TG levels than any individual SNP. In addition, the genetic risk score explained a greater proportion of variance in the specified trait than any given individual SNP. Finally, we found that for individuals with a higher TG genetic risk score, having either an elevated WC or being OW/obese amplified the genetic risk score’s effect by further increasing TG levels. However, for individuals with a lower TG genetic risk score, measures of adiposity made almost no difference in TG levels. Interestingly, for those women with a low TG genetic risk score and elevated levels of adiposity, their predicted levels of TG equaled those of women with a high genetic risk score without any adverse levels of adiposity. Overall, these results demonstrate that combinations of multiple genetic loci better explain the variation in CRP, HDL-C and TG levels and that the TG genetic risk score seemed to interact with measures of adiposity to influence TG levels in this study population.
In support of our results, recent work using the same study population found that central obesity might accentuate the effect of the TG-increasing allele of an APOA5 variant.3 In addition, previous research has implicated several variants in the LPL gene (a gene included in our genetic risk score) as having an interactive effect with central adiposity on TG levels and the ratio of TG to HDL-C.25, 26 However, we did not find significant interactions between these individual loci and adiposity on TG levels, perhaps indicating that the interactive effect is driven by a collective result of all SNPs in the TG genetic risk score.
We observed that both WC (adjusted for BMI) and OW/obese (adjusted for WC) interacted significantly with the TG genetic risk score. This suggests that visceral adiposity (as proxied by WC) and overall fatness both strengthen the effect of the genetic risk score on TG levels. However, it is interesting to note that the residuals of WC regressed on BMI also significantly interacted with the TG genetic risk score (results not shown). Previous studies have implicated visceral adiposity as a stronger predictor of TG levels and hypertriglyceridemia compared with subcutaneous adipose tissue.46, 47
From a clinical perspective, individuals with both a high TG genetic risk score and elevated WC had predicted TG levels that meet the American Heart Association’s level of ‘borderline high risk’ (1.69 mmol l−1 or 150 mg dl−1).32 This combination of elevated WC along with increased TG levels has been previously described as the ‘hypertriglyceridemic waist’ phenotype. Individuals with this phenotype have a higher risk of increased visceral adiposity, CVD, insulin resistance and other related outcomes.13, 48, 49, 50 This is of particular concern for Asian populations, for whom increased levels of visceral adiposity are present at normal BMIs.21, 22, 23 However, it is not clear how to specifically reduce visceral adiposity using lifestyle and diet modifications. Our results suggest that reducing overall fatness may also lessen the genetic risk score’s effects on TG levels. Work from Pollin et al.51 reinforces this concept by finding that an intensive lifestyle intervention that focused on weight loss appeared to partially mitigate the effect of the rs1260326 risk allele in the GCKR gene (a locus included in our genetic risk score) on higher TG levels. Further research, especially clinical trials in larger populations, is needed to know whether such weight loss interventions could be useful, especially across different ethnicities and different genetic risk profiles.
Limitations of our study merit consideration. In our literature search we found differing numbers of candidate SNPs for each trait. Although we used the same criteria in our search regardless of the CM trait, the variation in the number of candidate SNPs could reflect the current state of the literature. In addition, there is concern with choosing SNPs from a European sample and applying them to an Asian sample, especially in terms of tagging the appropriate functional variant. We tried to mitigate this by choosing SNPs with nominal significance and directional consistent effect estimates in our study population; however, because of the limited sample size in the CLHNS we may have lacked the power to detect the SNPs true effect. In addition, using a threshold of r2 <0.2 for linkage disequilibrium still allows SNPs to partially tag the same underlying signal, potentially including some redundancy in the genetic risk score. Although we used an unweighted approach to create our genetic risk scores, it may be possible in the future to obtain stable and accurate estimates of genetic variants for use in a weighted risk score that could improve predictability of CM risk.
In conclusion, using a study population of middle-aged Filipino women undergoing a nutrition and lifestyle transition, we found that CRP, HDL-C and TG genetic risk scores explained a greater variance of the associated trait compared with a single SNP. We also found that the TG genetic risk score interacted with adiposity to synergistically influence TG levels. For individuals with a high genetic predisposition to elevated TG levels, our results suggest that reducing adiposity could possibly prevent increases in TG levels and thereby reduce the likelihood of adverse health outcomes such as CM diseases. Replication of these results in larger study populations is needed to support the potential clinical and public health utility of targeted prevention efforts using genetic profiling.
References
Teslovich TM, Musunuru K, Smith AV, Edmondson AC, Stylianou IM, Koseki M et al. Biological, clinical and population relevance of 95 loci for blood lipids. Nature 2010; 466: 707–713.
Kim MH, Kim MK, Choi BY, Shin YJ . Prevalence of the metabolic syndrome and its association with cardiovascular diseases in Korea. J Korean Med Sci 2004; 19: 195.
Wu Y, Marvelle AF, Li J, Croteau-Chonka DC, Feranil AB, Kuzawa CW et al. Genetic association with lipids in Filipinos: waist circumference modifies an APOA5 effect on triglyceride levels. J Lipid Res 2013; 54: 3198–3205.
Ridker PM, Pare G, Parker A, Zee RY, Danik JS, Buring JE et al. Loci related to metabolic-syndrome pathways including LEPR,HNF1A, IL6R, and GCKR associate with plasma C-reactive protein: the Women’s Genome Health Study. Am J Hum Genet 2008; 82: 1185–1192.
Curocichin G, Wu Y, McDade TW, Kuzawa CW, Borja JB, Qin L et al. Single-nucleotide polymorphisms at five loci are associated with C-reactive protein levels in a cohort of Filipino young adults. J Hum Genet 2011; 56: 823–827.
Manolio TA . Cohort studies and the genetics of complex disease. Nat Genet 2009; 41: 5–6.
Aulchenko YS, Ripatti S, Lindqvist I, Boomsma D, Heid IM, Pramstaller PP et al. Loci influencing lipid levels and coronary heart disease risk in 16 European population cohorts. Nat Genet 2009; 41: 47–55.
Paynter NP, Chasman DI, Pare G, Buring JE, Cook NR, Miletich JP et al. Association between a literature-based genetic risk score and cardiovascular events in women. JAMA 2010; 303: 631–637.
Ripatti S, Tikkanen E, Orho-Melander M, Havulinna AS, Silander K, Sharma A et al. A multilocus genetic risk score for coronary heart disease: case-control and prospective cohort analyses. Lancet 2010; 376: 1393–1400.
Dehghan A, Dupuis J, Barbalic M, Bis JC, Eiriksdottir G, Lu C et al. Meta-analysis of genome-wide association studies in >80 000 subjects identifies multiple loci for C-reactive protein levels. Circulation 2011; 123: 731–738.
Rexrode KM, Carey VJ, Hennekens CH, Walters EE, Colditz GA, Stampfer MJ et al. Abdominal adiposity and coronary heart disease in women. JAMA 1998; 280: 1843–1848.
Adair LS . Dramatic rise in overweight and obesity in adult Filipino women and risk of hypertension. Obesity 2004; 12: 1335–1341.
Tanko LB, Bagger YZ, Qin G, Alexandersen P, Larsen PJ, Christiansen C . Enlarged waist combined with elevated triglycerides is a strong predictor of accelerated atherogenesis and related cardiovascular mortality in postmenopausal women. Circulation 2005; 111: 1883–1890.
Yusuf S, Hawken S, Ounpuu S, Bautista L, Franzosi MG, Commerford P et al. Obesity and the risk of myocardial infarction in 27,000 participants from 52 countries: a case-control study. Lancet 2005; 366: 1640–1649.
Wang X, Ding X, Su S, Spector TD, Mangino M, Iliadou A et al. Heritability of insulin sensitivity and lipid profile depend on BMI: evidence for gene-obesity interaction. Diabetologia 2009; 52: 2578–2584.
Surakka I, Isaacs A, Karssen LC, Laurila PP, Middelberg RP, Tikkanen E et al. A genome-wide screen for interactions reveals a new locus on 4p15 modifying the effect of waist-to-hip ratio on total cholesterol. PLoS Genet 2011; 7: e1002333.
Lamina C, Forer L, Schonherr S, Kollerits B, Ried JS, Gieger C et al. Evaluation of gene-obesity interaction effects on cholesterol levels: a genetic predisposition score on HDL-cholesterol is modified by obesity. Atherosclerosis 2012; 225: 363–369.
Drewnowski A . Nutrition transition and global dietary trends. Nutrition 2000; 16: 486–487.
Popkin BM, Adair LS, Ng SW . Global nutrition transition and the pandemic of obesity in developing countries. Nutr Rev 2012; 70: 3–21.
Lim SS, Vos T, Flaxman AD, Danaei G, Shibuya K, Adair-Rohani H et al. A comparative risk assessment of burden of disease and injury attributable to 67 risk factors and risk factor clusters in 21 regions, 1990-2010: a systematic analysis for the Global Burden of Disease Study 2010. Lancet 2012; 380: 2224–2260.
McKeigue PM, Shah B, Marmot MG . Relation of central obesity and insulin resistance with high diabetes prevalence and cardiovascular risk in South Asians. Lancet 1991; 337: 382–386.
Deurenberg-Yap M, Chew SK, Deurenberg P . Elevated body fat percentage and cardiovascular risks at low body mass index levels among Singaporean Chinese, Malays and Indians. Obes Rev 2002; 3: 209–215.
Wang J, Thornton JC, Russell M, Burastero S, Heymsfield S, Pierson RN Jr . Asians have lower body mass index (BMI) but higher percent body fat than do whites: comparisons of anthropometric measurements. Am J Clin Nutr 1994; 60: 23–28.
WHO Expert Consultation. Appropriate body-mass index for Asian populations and its implications for policy and intervention strategies. Lancet 2004; 363: 157–163.
Li J, Huang A, Hu Y, Chen D . Association of the lipoprotein lipase gene T+495G polymorphism with central obesity and serum lipids in a twin study. Ann Epidemiol 2008; 18: 760–767.
Senti M, Bosch M, Aubo C, Elosua R, Masia R, Marrugat J . Relationship of abdominal adiposity and dyslipemic status in women with a common mutation in the lipoprotein lipase gene. The REGICOR investigators. Atherosclerosis 2000; 150: 135–141.
Eiriksdottir G, Smith AV, Aspelund T, Hafsteinsdottir SH, Olafsdottir E, Launer LJ et al. The interaction of adiposity with the CRP gene affects CRP levels: age, gene/environment susceptibilty-Reykjavik study. Int J Obes (Lond) 2009; 33: 267–272.
Adair LS . Dramatic rise in overweight and obesity in adult Filipino women and risk of hypertension. Obesity 2004; 12: 1335–1341.
Adair LS, Popkin BM, Akin JS, Guilkey DK, Gultiano S, Borja J et al. Cohort profile: the Cebu longitudinal health and nutrition survey. Int J Epidemiol 2011; 40: 619–625.
Pearson TA, Mensah GA, Alexander RW, Anderson JL, Cannon RO, Criqui M et al. Markers of inflammation and cardiovascular disease: application to clinical and public health practice: a statement for healthcare professionals from the Centers for Disease Control and Prevention and the American Heart Association. Circulation 2003; 107: 499–511.
Alberti KG, Zimmet P, Shaw J, IDF Epidemiology Task Force Consensus Group. The metabolic syndrome—a new worldwide definition. Lancet 2005; 366: 1059–1062.
National Cholesterol Education Program (NCEP) Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel III). Third Report of the National Cholesterol Education Program (NCEP) Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel III) final report. Circulation 2002; 106: 3143.
Stern SE, Williams K, Ferrannini E, DeFronzo RA, Bogardus C, Stern MP . Identification of individuals with insulin resistance using routine clinical measurements. Diabetes 2005; 54: 333–339.
Lohman TG, Roche AF, Martorell R . Anthropometric Standardization Reference Manual. Human Kinetics Books: Champaign, 1988.
Food and Nutrition Research Institute. Food Composition Tables Recommended for Use in the Philippines. Food and Nutrition Research Institute, Department of Science and Technology: Metro Manila, Philippines, 1997.
Food and Nutrition Research Institute. Philippine Nutrition Facts and Figures. Food and Nutrition Research Institute, Department of Science and Technology: Manila, Philippines, 2001.
Zubair N, Kuzawa CW, McDade TW, Adair LS . Cluster analysis reveals important determinants of cardiometabolic risk patterns in Filipino women. Asia Pac J Clin Nutr 2012; 21: 271–281.
McDade TW, Rutherford JN, Adair L, Kuzawa C . Adiposity and pathogen exposure predict C-reactive protein in Filipino women. J Nutr 2008; 138: 2442–2447.
Lange LA, Croteau-Chonka DC, Marvelle AF, Qin L, Gaulton KJ, Kuzawa CW et al. Genome-wide association study of homocysteine levels in Filipinos provides evidence for CPS1 in women and a stronger MTHFR effect in young adults. Hum Mol Genet 2010; 19: 2050–2058.
Li Y, Willer CJ, Ding J, Scheet P, Abecasis GR . MaCH: using sequence and genotype data to estimate haplotypes and unobserved genotypes. Genet Epidemiol 2010; 34: 816–834.
Wu Y, McDade TW, Kuzawa CW, Borja J, Li Y, Adair LS et al. Genome-wide association with C-reactive protein levels in CLHNS: evidence for the CRP and HNF1A loci and their interaction with exposure to a pathogenic environment. Inflammation 2012; 35: 574–583.
Kim YJ, Go MJ, Hu C, Hong CB, Kim YK, Lee JY et al. Large-scale genome-wide association studies in East Asians identify new genetic loci influencing metabolic traits. Nat Genet 2011; 43: 990–995.
Purcell S, Neale B, Todd-Brown K, Thomas L, Ferreira MAR, Bender D et al. PLINK: a tool set for whole-genome association and population-based linkage analyses. Am J Hum Genet 2007; 81: 559–575.
Price AL, Patterson NJ, Plenge RM, Weinblatt ME, Shadick NA, Reich D . Principal components analysis corrects for stratification in genome-wide association studies. Nature 2006; 38: 904–909.
Feranil AB, Duazo PL, Kuzawa CW, Adair LS . Coconut oil is associated with a beneficial lipid profile in pre-menopausal women in the Philippines. Asia Pac J Clin Nutr 2011; 20: 190–195.
Nazare JA, Smith JD, Borel AL, Haffner SM, Balkau B, Ross R et al. Ethnic influences on the relations between abdominal subcutaneous and visceral adiposity, liver fat, and cardiometabolic risk profile: the International Study of Prediction of Intra-Abdominal Adiposity and Its Relationship With Cardiometabolic Risk/Intra-Abdominal Adiposity. Am J Clin Nutr 2012; 96: 714–726.
Fox CS, Massaro JM, Hoffmann U, Pou KM, Maurovich-Horvat P, Liu CY et al. Abdominal visceral and subcutaneous adipose tissue compartments: association with metabolic risk factors in the Framingham Heart Study. Circulation 2007; 116: 39–48.
Sam S, Haffner S, Davidson MH, D'Agostino RB Sr., Feinstein S, Kondos G et al. Hypertriglyceridemic waist phenotype predicts increased visceral fat in subjects with type 2 diabetes. Diabetes Care 2009; 32: 1916–1920.
Lemieux I, Pascot A, Couillard C, Lamarche B, Tchernof A, Almeras N et al. Hypertriglyceridemic waist: a marker of the atherogenic metabolic triad (hyperinsulinemia; hyperapolipoprotein B; small, dense LDL) in men? Circulation 2000; 102: 179–184.
Bos G, Dekker JM, Heine RJ, Hoom s . Non-HDL cholesterol contributes to the “hypertriglyceridemic waist” as a cardiovascular risk factor: the Hoorn study. Diabetes Care 2004; 27: 283–284.
Pollin TI, Jablonski KA, McAteer JB, Saxena R, Kathiresan S, Kahn SE et al. Triglyceride response to an intensive lifestyle intervention is enhanced in carriers of the GCKR Pro446Leu polymorphism. J Clin Endocrinol Metab 2011; 96: E1142–E1147.
Acknowledgements
We thank the Office of Population Studies Foundation research and data collection teams and the study participants who generously provided their time for this study. This research was supported by National Institutes of Health Grants R01-HL085144-03, R01-HD054501 and R01-TW05596.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies this paper on the Nutrition & Diabetes website
Supplementary information
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivs 3.0 Unported License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/3.0/
About this article
Cite this article
Zubair, N., Mayer-Davis, E., Mendez, M. et al. Genetic risk score and adiposity interact to influence triglyceride levels in a cohort of Filipino women. Nutr & Diabetes 4, e118 (2014). https://doi.org/10.1038/nutd.2014.16
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nutd.2014.16
This article is cited by
-
Polygenic risk for triglyceride levels in the presence of a high impact rare variant
BMC Medical Genomics (2023)
-
Gene-environment interactions due to quantile-specific heritability of triglyceride and VLDL concentrations
Scientific Reports (2020)
-
Detection of gene-environment interactions in the presence of linkage disequilibrium and noise by using genetic risk scores with internal weights from elastic net regression
BMC Genetics (2017)