Abstract
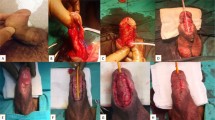
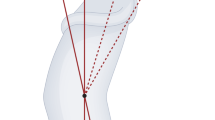
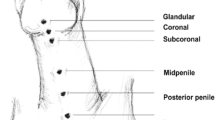
Hypospadias is one of the most common congenital malformations of the male genitalia. Severe cases present with associated curvature greater than 30° and the meatus opening proximally to the penoscrotal junction. The perioperative management of patients with primary severe hypospadias is variable. Systematic evaluation of the upper urinary tract and the search for enlarged prostatic utricles seem unnecessary in patients with isolated primary severe hypospadias, and should be limited to severe cases with associated extraurinary malformations. Detection of a disorder of sex development is key for gender assignment and prognosis, but the identification of cases warranting a full work-up and the influence of such a diagnosis on the success of hypospadias repair is controversial. Preoperative hormonal stimulation allows for penile growth irrespective of the administration route. Associated morbidity is minimal, but its influence on the success of surgery is still unknown. An age of 6–18 months is generally recommended for surgery, but no trial data support this policy. Second-layer coverage of the urethroplasty and postoperative urinary drainage seem to reduce the complications of surgery, whereas postoperative antibiotic prophylaxis and type of dressing have minimal impact on surgical success. Overall, most interventions are based on weak evidence, and their influence on the outcomes of repair is ill-defined. Clinicians should be made aware of the evidence supporting any single intervention in order to standardize their management policies. We hope the issues outlined here will prompt researchers to design new studies to address the clinically relevant questions.
Key Points
-
Systematic evaluation of the upper urinary tract and investigation for enlarged prostatic utricles seem unnecessary in patients with isolated primary severe hypospadias
-
Diagnosis of a disorder of sex development is key, but the identification of cases warranting a full work-up and the influence of diagnosis on the success of surgery are controversial
-
Preoperative hormonal stimulation allows for penile growth irrespective of the administration route; associated morbidity is minimal, but its influence on the success of surgery is still unknown
-
An age of 6–18 months is generally recommended for surgery, but no trial data support this policy
-
Second-layer coverage of the urethroplasty and postoperative urinary drainage seem to reduce the complications of surgery
-
Postoperative antibiotic prophylaxis and type of dressing have minimal impact on the success of surgery
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Baskin, L. S. & Ebbers, M. B. Hypospadias: anatomy, etiology, and technique. J. Pediatr. Surg. 41, 463–472 (2006).
Castagnetti, M. & El-Ghoneimi, A. Surgical management of primary severe hypospadias in children: systematic 20-year review. J. Urol. 184, 1469–1474 (2010).
Valla, J. S. et al. Single-stage correction of posterior hypospadias (178 cases). Comparison of three techniques: free skin graft, free bladder mucosal graft, transverse pedicle preputial graft. Eur. J. Pediatr. Surg. 1, 287–290 (1991).
Flack, C. E. & Walker, R. D. 3rd. Onlay-tube-onlay urethroplasty technique in primary perineal hypospadias surgery. J. Urol. 154, 837–839 (1995).
Fossum, M., Svensson, J., Kratz, G. & Nordenskjöld, A. Autologous in vitro cultured urothelium in hypospadias repair. J. Pediatr. Urol. 3, 10–18 (2007).
Hayashi, Y. et al. Neo-modified Koyanagi technique for the single-stage repair of proximal hypospadias. J. Pediatr. Urol. 3, 239–242 (2007).
Kajbafzadeh, A. M. et al. Proximal hypospadias with severe chordee: single stage repair using corporeal tunica vaginalis free graft. J. Urol. 178, 1036–1042 (2007).
Manzoni, G. A. & El-Ghoneimi, A. Posterior hypospadias. Dial. Pediatr. Urol. 29, 1–11 (2008).
Cerasaro, T. S., Brock, W. A. & Kaplan, G. W. Upper urinary tract anomalies associated with congenital hypospadias: is screening necessary? J. Urol. 135, 537–538 (1986).
Davenport, M. & MacKinnon, A. E. The value of ultrasound screening of the upper urinary tract in hypospadias. Br. J. Urol. 62, 595–596 (1988).
Friedman, T. et al. Detection and incidence of anomalies associated with hypospadias. Pediatr. Nephrol. 23, 1809–1816 (2008).
Gupta, L., Sharma, S. & Gupta, D. K. Is there a need to do routine sonological, urodynamic study and cystourethroscopic evaluation of patients with simple hypospadias? Pediatr. Surg. Int. 26, 971–976 (2010).
Faundez, T., Chariatte, V. & Cachat, F. Urinary tract anomalies in children with hypospadias. Pediatr. Surg. Int. 26, 1237–1238 (2010).
Ciftci, A. O., Senocak, M. E., Büyükpamukçu, N. & Hiçsönmez, A. Abnormal prostatic utricle configuration in hypospadias and intersex patients. Eur. J. Pediatr. Surg. 9, 167–172 (1999).
Kojima, Y., Hayashi, Y., Maruyama, T., Sasaki, S. & Kohri, K. Comparison between ultrasonography and retrograde urethrography for detection of prostatic utricle associated with hypospadias. Urology 57, 1151–1155 (2001).
Chertin, B., Koulikov, D., Hadas-Halpern, I. & Farkas, A. Masculinizing genitoplasty in intersex patients. J. Urol. 174, 1683–1686 (2005).
Lee, P. A., Houk, C. P., Ahmed, S. F. & Hughes, I. A. Consensus statement on management of intersex disorders. International Consensus Conference on Intersex. Pediatrics 118, e488–e500 (2006).
Kaefer, M. et al. The incidence of intersexuality in children with cryptorchidism and hypospadias: stratification based on gonadal palpability and meatal position. J. Urol. 162, 1003–1006 (1999).
McAleer, I. M. & Kaplan, G. W. Is routine karyotyping necessary in the evaluation of hypospadias and cryptorchidism? J. Urol. 165, 2029–2031 (2001).
Cox, M. J., Coplen, D. E. & Austin, P. F. The incidence of disorders of sexual differentiation and chromosomal abnormalities of cryptorchidism and hypospadias stratified by meatal location. J. Urol. 180, 2649–2652 (2008).
Sircili, M. H. et al. Long-term surgical outcome of masculinizing genitoplasty in large cohort of patients with disorders of sex development. J. Urol. 184, 1122–1127 (2010).
Gupta, D., Bhardwaj, M., Sharma, S., Ammini, A. C. & Gupta, D. K. Long-term psychosocial adjustments, satisfaction related to gender and the family equations in disorders of sexual differentiation with male sex assignment. Pediatr. Surg. Int. 26, 955–958 (2010).
Bhat, A. Extended urethral mobilization in incised plate urethroplasty for severe hypospadias: a variation in technique to improve chordee correction. J. Urol. 178, 1031–1035 (2007).
Moursy, E. E. Outcome of proximal hypospadias repair using three different techniques. J. Pediatr. Urol. 6, 45–53 (2010).
Arena, F. et al. Surgical correction of penoscrotal transposition associated with hypospadias and bifid scrotum: our experience of two-stage repair. J. Pediatr. Urol. 1, 289–294 (2005).
Djordjevic, M. L. et al. Combined buccal mucosa graft and dorsal penile skin flap for repair of severe hypospadias. Urology 71, 821–825 (2008).
Aoki, K., Fujimoto, K., Yoshida, K., Hirao, Y. & Ueoka, K. One-stage repair of severe hypospadias using modified tubularized transverse preputial island flap with V-incision suture. J. Pediatr. Urol. 4, 438–441 (2008).
Retik, A. B. et al. Management of severe hypospadias with a 2-stage repair. J. Urol. 152, 749–751 (1994).
Emir, H., Jayanthi, V. R., Nitahara, K. & Danismend, N. & Koff. S. A. Modification of the Koyanagi technique for the single stage repair of proximal hypospadias. J. Urol. 164, 973–975 (2000).
Barroso, U. Jr, Jednak, R., Spencer Barthold, J. & González, R. Further experience with the double onlay preputial flap for hypospadias repair. J. Urol. 164, 998–1001 (2000).
Gershbaum, M. D., Stock, J. A. & Hanna, M. K. A case for 2-stage repair of perineoscrotal hypospadias with severe chordee. J. Urol. 168, 1727–1728 (2002).
Snodgrass, W. & Yucel S. Tubularized incised plate for mid shaft and proximal hypospadias repair. J. Urol. 177, 698–702 (2007).
Braga, L. H. et al. Comparative analysis of tubularized incised plate versus onlay island flap urethroplasty for penoscrotal hypospadias. J. Urol. 178, 1451–1456 (2007).
Hadidi, A. T. Lateral-based flap: a single stage urethral reconstruction for proximal hypospadias. J. Pediatr. Surg. 44, 797–801 (2009).
Snodgrass, W. & Prieto, J. Straightening ventral curvature while preserving the urethral plate in proximal hypospadias repair. J. Urol. 182, 1720–1725 (2009).
Catti, M., Lottmann, H., Babloyan, S., Lortat-Jacob, S. & Mouriquand, P. Original Koyanagi urethroplasty versus modified Hayashi technique: outcome in 57 patients. J. Pediatr. Urol. 5, 300–306 (2009).
Sakakibara, N., Nonomura, K., Koyanagi, T. & Imanaka, K. Use of testosterone ointment before hypospadias repair. Urol. Int. 47, 40–43 (1991).
Koff, S. A. & Jayanthi, V. R. Preoperative treatment with human chorionic gonadotropin in infancy decreases the severity of proximal hypospadias and chordee. J. Urol. 162, 1435–1439 (1999).
Luo, C. C., Lin, J. N., Chiu, C. H. & Lo, F. S. Use of parenteral testosterone prior to hypospadias surgery. Pediatr. Surg. Int. 19, 82–84 (2003).
Chalapathi, G. et al. Testosterone therapy in microphallic hypospadias: topical or parenteral? J. Pediatr. Surg. 38, 221–223 (2003).
Nerli, R. B., Koura, A., Prabha, V. & Reddy, M. Comparison of topical versus parenteral testosterone in children with microphallic hypospadias. Pediatr. Surg. Int. 25, 57–59 (2009).
Ishii, T., Hayashi, M., Suwanai, A., Amano, N. & Hasegawa, T. The effect of intramuscular testosterone enanthate treatment on stretched penile length in prepubertal boys with hypospadias. Urology 76, 97–100 (2010).
Gorduza, D. B. et al. Does androgen stimulation prior to hypospadias surgery increase the rate of healing complications? A preliminary report. J. Pediatr. Urol. doi: 10.1016/j.jpurol.2010.05.003.
Davits, R. J., van den Aker, E. S., Scholtmeijer, R. J., de Muinck Keizer-Schrama, S. M. & Nijman, R. J. Effect of parenteral testosterone therapy on penile development in boys with hypospadias. Br. J. Urol. 71, 593–595 (1993).
Kaya, C. et al. The efficacy of dihydrotestosterone transdermal gel before primary hypospadias surgery: a prospective, controlled, randomized study. J. Urol. 179, 684–688 (2008).
DeFoor, W. & Wacksman, J. Results of single staged hypospadias surgery to repair penoscrotal hypospadias with bifid scrotum or penoscrotal transposition. J. Urol. 170, 1585–1588 (2003).
Kuyumcuoglu, U., Eryildirim, B., Faydaci, G., Tarhan, F. & Ozgül, A. The comparison of belt-fuqua and “TIPU” techniques in proximal penile hypospadias cases: retrospective analysis of 65 cases. Int. Urol. Nephrol. 41, 755–759 (2009).
No authors listed. Timing of elective surgery on the genitalia of male children with particular reference to the risks, benefits, and psychological effects of surgery and anesthesia. American Academy of Pediatrics. Pediatrics 97, 590–594 (1996).
Alalami, A. A., Ayoub, C. M. & Baraka, A. S. Laryngospasm: review of different prevention and treatment modalities. Paediatr. Anaesth. 18, 281–288 (2008).
Hayashi, Y., Kojima, Y., Mizuno, K., Nakane, A. & Kohri, K. The modified Koyanagi repair for severe proximal hypospadias. BJU Int. 87, 235–238 (2001).
Hensle, T. W., Tennenbaum, S. Y., Reiley, E. A. & Pollard, J. Hypospadias repair in adults: adventures and misadventures. J. Urol. 165, 77–79 (2001).
Jones, B. C., O'Brien, M., Chase, J., Southwell, B. R. & Hutson, J. M. Early hypospadias surgery may lead to a better long-term psychosexual outcome. J. Urol. 182, 1744–1749 (2009).
Weber, D. M., Schonbucher, V. B., Gobet, R., Gerber, A. & Landolt, M. A. Is there an ideal age for hypospadias repair? A pilot study. J. Pediatr. Urol. 5, 345–350 (2009).
Hayashi, Y. et al. Scrotal dartos flap for the prevention of the urethrocutaneous fistula on hypospadias urethroplasty. Int. J. Urol. 12, 280–283 (2005).
Telfer, J. R., Quaba, A. A., Kwai Ben, I. & Peddi, N. C. An investigation into the role of waterproofing in a two-stage hypospadias repair. Br. J. Plast. Surg. 51, 542–546 (1998).
Chuang, J. H. & Shieh, C. S. Two-layer versus one-layer closure in transverse island flap repair of posterior hypospadias. J. Pediatr. Surg. 30, 739–742 (1995).
Gopal, S. C. et al. Use of fibrin glue in preventing urethrocutaneous fistula after hypospadias repair. J. Pediatr. Surg. 43, 1869–1872 (2008).
Savanelli, A., Esposito, C. & Settimi, A. A prospective randomized comparative study on the use of ventral subcutaneous flap to prevent fistulas in the Snodgrass repair for distal hypospadias. World J. Urol. 25, 641–645 (2007).
Demirbilek, S., Kanmaz, T., Aydin, G. & Yücesan, S. Outcomes of one-stage techniques for proximal hypospadias repair. Urology 58, 267–270 (2001).
Sugita, Y., Tanikaze, S., Yoshino, K. & Yamamichi, F. Severe hypospadias repair with meatal based paracoronal skin flap: the modified Koyanagi repair. J. Urol. 166, 1051–1053 (2001).
Sugar, E. C. & Firlit, C. F. Urinary prophylaxis and postoperative care of children at home with an indwelling catheter after hypospadias repair. Urology 32, 418–420 (1988).
Montagnino, B. A., Gonzales, E. T. Jr & Roth, D. R. Open catheter drainage after urethral surgery. J. Urol. 140, 1250–1252 (1988).
Ben Meir, D. & Livne, P. M. Is prophylactic antimicrobial treatment necessary after hypospadias repair? J. Urol. 171, 2621–2622 (2004).
Demirbilek, S. & Atayurt, H. F. One-stage hypospadias repair with stent or suprapubic diversion: which is better? J. Pediatr. Surg. 32, 1711–1712 (1997).
Cilento, B. G. Jr, Stock, J. A. & Kaplan, G. W. Pantaloon spica cast: an effective method for postoperative immobilization after free graft hypospadias repair. J. Urol. 157, 1882–1883 (1997).
McLorie, G. et al. A prospective randomized clinical trial to evaluate methods of postoperative care of hypospadias. J. Urol. 165, 1669–1672 (2001).
Van Savage, J. G., Palanca, L. G. & Slaughenhoupt, B. L. A prospective randomized trial of dressings versus no dressings for hypospadias repair. J. Urol. 164, 981–983 (2000).
Author information
Authors and Affiliations
Contributions
M. Castagnetti and A. El-Ghoneimi contributed equally to the researching of data, discussion of content, writing the article and reviewing the manuscript before submission
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
About this article
Cite this article
Castagnetti, M., El-Ghoneimi, A. The influence of perioperative factors on primary severe hypospadias repair. Nat Rev Urol 8, 198–206 (2011). https://doi.org/10.1038/nrurol.2011.24
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrurol.2011.24
This article is cited by
-
Surgical management of primary severe hypospadias in children: an update focusing on penile curvature
Nature Reviews Urology (2022)
-
Double-face preputial island flap revisited: is it a reliable one-stage repair for severe hypospadias?
World Journal of Urology (2021)
-
Surgical management of hypospadias in cases with concomitant disorders of sex development
Pediatric Surgery International (2019)
-
Disorders of sex development in a developing country: perspectives and outcome of surgical management of 39 cases
Pediatric Surgery International (2015)
-
Génitoplastie masculinisante
Revue de médecine périnatale (2015)