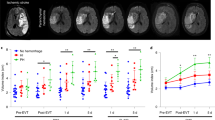
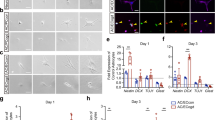
Abstract
The concept of the neurovascular unit as the key brain component affected by stroke is controversial, because current definitions of this entity neglect mechanisms that control perfusion and reperfusion of arteries and arterioles upstream of the cerebral microcirculation. Indeed, although definitions vary, many researchers consider the neurovascular unit to be restricted to endothelial cells, neurons and glia within millimetres of the cerebral capillary microcirculation. This Perspectives article highlights the roles of vascular smooth muscle, endothelial cells and perivascular innervation of cerebral arteries in the initiation and progression of, and recovery from, ischaemic stroke. The concept of the vascular neural network—which includes cerebral arteries, arterioles, and downstream neuronal and glial cell types and structures—is introduced as the fundamental component affected by stroke pathophysiology. The authors also propose that the vascular neural network should be considered the main target for future therapeutic intervention after cerebrovascular insult.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Lo, E. H., Dalkara, T. & Moskowitz, M. A. Mechanisms, challenges and opportunities in stroke. Nat. Rev. Neurosci. 4, 399–414 (2003).
Ginsberg, M. D. Neuroprotection for ischemic stroke: past, present and future. Neuropharmacology 55, 363–389 (2008).
del Zoppo, G. J. The neurovascular unit in the setting of stroke. J. Intern. Med. 267, 156–171 (2010).
Lo, E. H., Broderick, J. P. & Moskowitz, M. A. tPA and proteolysis in the neurovascular unit. Stroke 35, 354–356 (2004).
Iadecola, C. Neurovascular regulation in the normal brain and in Alzheimer's disease. Nat. Rev. Neurosci. 5, 347–360 (2004).
Cohen, Z., Bonvento, G., Lacombe, P. & Hamel, E. Serotonin in the regulation of brain microcirculation. Prog. Neurobiol. 50, 335–362 (1996).
Grotta, J. C. et al. Report of the Stroke Progress Review Group. National Institute of Neurological Disorders and Stroke [online], (2002).
Zlokovic, B. V. The blood–brain barrier in health and chronic neurodegenerative disorders. Neuron 57, 178–201 (2008).
Lee, R. M. Morphology of cerebral arteries. Pharmacol. Ther. 66, 149–173 (1995).
Alexander, M. R. & Owens, G. K. Epigenetic control of smooth muscle cell differentiation and phenotypic switchingin vascular development and disease. Annu. Rev. Physiol. 74, 13–40 (2012).
Croll, S. D. & Wiegand, S. J. Vascular growth factors in cerebral ischemia. Mol. Neurobiol. 23, 121–135 (2001).
Hamel, E. Perivascular nerves and the regulation of cerebrovascular tone. J. Appl. Physiol. 100, 1059–1064 (2006).
Alabadi, J. A. et al. Changes in the adrenergic mechanisms of cerebral arteries after subarachnoid hemorrhage in goats. Neurosurgery 34, 1027–1033; discussion 1033–1034 (1994).
Diansan, S., Shifen, Z., Zhen, G., Heming, W. & Xiangrui, W. Resection of the nerves bundle from the sphenopalatine ganglia tend to increase the infarction volume following middle cerebral artery occlusion. Neurol. Sci. 31, 431–435 (2010).
Bevan, R. D., Tsuru, H. & Bevan, J. A. Cerebral artery mass in the rabbit is reduced by chronic sympathetic denervation. Stroke 14, 393–396 (1983).
Mulligan-Kehoe, M. J. The vasa vasorum in diseased and nondiseased arteries. Am. J. Physiol. Heart Circ. Physiol. 298, H295–H305 (2010).
Zervas, N. T., Liszczak, T. M., Mayberg, M. R. & Black, P. M. Cerebrospinal fluid may nourish cerebral vessels through pathways in the adventitia that may be analogous to systemic vasa vasorum. J. Neurosurg. 56, 475–481 (1982).
Shuaib, A., Butcher, K., Mohammad, A. A., Saqqur, M. & Liebeskind, D. S. Collateral blood vessels in acute ischaemic stroke: a potential therapeutic target. Lancet Neurol. 10, 909–921 (2011).
Kampoli, A. M. et al. Potential pathogenic inflammatory mechanisms of endothelial dysfunction induced by type 2 diabetes mellitus. Curr. Pharm. Des 17, 4147–4158 (2011).
Manolio, T. A., Olson, J. & Longstreth, W. T. Hypertension and cognitive function: pathophysiologic effects of hypertension on the brain. Curr. Hypertens. Rep. 5, 255–261 (2003).
Manjila, S. et al. Evidence-based review of primary and secondary ischemic stroke prevention in adults: a neurosurgical perspective. Neurosurg. Focus 30, E1 (2011).
Behrouz, R., Malek, A. R. & Torbey, M. T. Small vessel cerebrovascular disease: the past, present, and future. Stroke Res. Treat. 2012, 839151 (2012).
Balami, J. S. & Buchan, A. M. Complications of intracerebral haemorrhage. Lancet Neurol. 11, 101–118 (2012).
Ayata, C. CADASIL: experimental insights from animal models. Stroke 41, S129–S134 (2010).
Lee, J. et al. Glioma-induced remodeling of the neurovascular unit. Brain Res. 1288, 125–134 (2009).
Kuklina, E. V., Tong, X., George, M. G. & Bansil, P. Epidemiology and prevention of stroke: a worldwide perspective. Expert Rev. Neurother. 12, 199–208 (2012).
Rajamani, K. & Chaturvedi, S. Stroke prevention—surgical and interventional approaches to carotid stenosis. Neurotherapeutics 8, 503–514 (2011).
O'Dell, K. M., Igawa, D. & Hsin, J. New oral anticoagulants for atrial fibrillation: a review of clinical trials. Clin. Ther. 34, 894–901 (2012).
Rose, M. J. Aneurysmal subarachnoid hemorrhage: an update on the medical complications and treatments strategies seen in these patients. Curr. Opin. Anaesthesiol. 24, 500–507 (2011).
Hussain, M. S. et al. Mechanical thrombectomy for acute stroke with the alligator retrieval device. Stroke 40, 3784–3788 (2009).
Acknowledgements
The authors' research is supported by grants to J. H. Zhang (NIH NS43338), J. Badaut (NIH HD061946), J. Tang (NIH NS060936) and W. J. Pearce (NIH NS076945 and HD031226).
Author information
Authors and Affiliations
Contributions
J. H. Zhang, J. Badaut and W. J. Pearce wrote the article. J. H. Zhang, J. Badaut, J. Tang and W. J. Pearce researched the data for the article. J. H. Zhang, J. Badaut, J. Tang, A. Obenaus, R. Hartman and W. J. Pearce provided substantial contributions to discussion of the content and reviewing and/or editing of the manuscript before submission.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
About this article
Cite this article
Zhang, J., Badaut, J., Tang, J. et al. The vascular neural network—a new paradigm in stroke pathophysiology. Nat Rev Neurol 8, 711–716 (2012). https://doi.org/10.1038/nrneurol.2012.210
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrneurol.2012.210
This article is cited by
-
Non-genomic Effect of Estradiol on the Neurovascular Unit and Possible Involvement in the Cerebral Vascular Accident
Molecular Neurobiology (2023)
-
Longitudinal dynamics of microvascular recovery after acquired cortical injury
Acta Neuropathologica Communications (2022)
-
Profiling the neurovascular unit unveils detrimental effects of osteopontin on the blood–brain barrier in acute ischemic stroke
Acta Neuropathologica (2022)
-
Cyclophilin a signaling induces pericyte-associated blood-brain barrier disruption after subarachnoid hemorrhage
Journal of Neuroinflammation (2020)
-
Activation of the Hedgehog Pathway Promotes Recovery of Neurological Function After Traumatic Brain Injury by Protecting the Neurovascular Unit
Translational Stroke Research (2020)