Key Points
-
Parkinson's disease is a progressive neurological disorder characterized primarily by motor symptoms that include rigidity, hypokinesia and tremor. The most pronounced neuropathological feature is a loss of dopaminergic neurons in the substantia nigra pars compacta, which leads to a reduction in dopamine levels in the target region, the striatum. In the substantia nigra, some neurons have intracytoplasmic inclusions known as Lewy bodies.
-
In most patients, Parkinson's disease shows no clear inheritance and the cause of neurodegeneration is not known. Several disease mechanisms have been proposed, including oxidative stress and mitochondrial dysfunction. Some emphasis has been placed on the possibility that environmental toxins trigger these pathological changes.
-
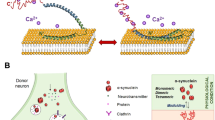
In the late 1990s, the discovery of the gene that causes a rare autosomal-dominant form of Parkinson's disease led to renewed interest in the search for pathogenic mechanisms. The mutated gene encodes α-synuclein, a synaptic protein of unknown function. It has been suggested that it plays a role in the recycling of vesicles that have released their neurotransmitter content into the synaptic cleft. Moreover, further rare forms of Parkinson's disease have been identified that result from mutations in parkin and ubiquitin carboxy-terminal hydrolase L1. These proteins participate in the ubiquitin–proteasome pathway, which is responsible for the degradation of unwanted proteins.
-
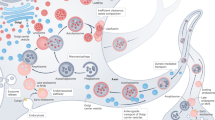
We speculate why changes in these diverse genes lead to a neurodegenerative process that is relatively focused on dopamine-containing neurons, and emphasize the role of dopamine-dependent oxidative stress in this process. We believe that there are multiple aetiological triggers, resulting from either genetic changes or environmental insults, which share the same final common pathway to cell death in dopaminergic neurons. Increased levels of cytoplasmic dopamine in nigral neurons in Parkinson's disease patients might result in dopamine oxidation and the generation of reactive oxygen species that can damage and eventually kill these neurons.
-
One pathway that might lead to these events involves impaired vesicular storage of dopamine. Recent experimental evidence shows that the expression of mutant α-synuclein in a human dopaminergic cell line increases cytoplasmic dopamine levels and raises the levels of superoxide radicals in the cytoplasm.
-
Dopamine-induced oxidative stress, impaired synaptic vesicle function and misfolding of α-synuclein, due to mutations or to oxidative damage to this protein, might be components in a self-perpetuating vicious cycle that eventually leads to the demise of dopaminergic neurons.
Abstract
Parkinson's disease is a devastating neurological condition that affects at least four million people. A striking feature of this disorder is the preferential loss of dopamine-producing neurons in the midbrain. Several aetiological triggers have been linked to Parkinson's disease, including genetic mutations and environmental toxins, but the pathway that leads to cell death is unknown. Recent developments have shed light on the pathogenic mechanisms that underlie the degeneration of these cells. We propose that defective sequestration of dopamine into vesicles, leading to the generation of reactive oxygen species in the cytoplasm, is a key event in the demise of dopaminergic neurons in Parkinson's disease, and might represent a common pathway that underlies both genetic and sporadic forms of the disorder.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$189.00 per year
only $15.75 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Kruger, R., Eberhardt, O., Riess, O., Schulz, J. B. & Riess, O. Parkinson's disease: one biochemical pathway to fit all genes? Trends Mol. Med. 8, 236–240 (2002).
Lansbury, P. T. & Brice, A. Genetics of Parkinson's disease and biochemical studies of implicated gene products. Curr. Opin. Genet. Dev. 12, 299–306 (2002).
Sherer, T. B., Betarbet, R. & Greenamyre, J. T. Pathogenesis of Parkinson's disease. Curr. Opin. Investig. Drugs 2, 657–662 (2001).
Duda, J. E., Giasson, B. I., Mabon, M. E., Lee, V. M. & Trojanowski, J. Q. Novel antibodies to synuclein show abundant striatal pathology in Lewy body diseases. Ann. Neurol. 52, 205–210 (2002).
Sauer, H. & Oertel, W. H. Progressive degeneration of nigrostriatal dopamine neurons following intrastriatal terminal lesions with 6-hydroxydopamine: a combined retrograde tracing and immunocytochemical study in the rat. Neuroscience 59, 401–415 (1994).
Lee, C. S., Sauer, H. & Bjorklund, A. Dopaminergic neuronal degeneration and motor impairments following axon terminal lesion by intrastriatal 6-hydroxydopamine in the rat. Neuroscience 72, 641–653 (1996).
Sohal, R. S. & Weindruch, R. Oxidative stress, caloric restriction, and aging. Science 273, 59–63 (1996).
Smith, C. D. et al. Excess brain protein oxidation and enzyme dysfunction in normal aging and in Alzheimer disease. Proc. Natl Acad. Sci. USA 88, 10540–10543 (1991).
Mecocci, P. et al. Oxidative damage to mitochondrial DNA shows marked age-dependent increases in human brain. Ann. Neurol. 34, 609–616 (1993).
Mecocci, P., MacGarvey, U. & Beal, M. F. Oxidative damage to mitochondrial DNA is increased in Alzheimer's disease. Ann. Neurol. 36, 747–751 (1994).
Lovell, M. A., Ehmann, W. D., Butler, S. M. & Markesbery, W. R. Elevated thiobarbituric acid-reactive substances and antioxidant enzyme activity in the brain in Alzheimer's disease. Neurology 45, 1594–1601 (1995).
Marcus, D. L. et al. Increased peroxidation and reduced antioxidant enzyme activity in Alzheimer's disease. Exp. Neurol. 150, 40–44 (1998).
Rosen, D. R. et al. Mutations in Cu/Zn superoxide dismutase gene are associated with familial amyotrophic lateral sclerosis. Nature 362, 59–62 (1993).
Ferrante, R. J. et al. Evidence of increased oxidative damage in both sporadic and familial amyotrophic lateral sclerosis. J. Neurochem. 69, 2064–2074 (1997).
Pedersen, W. A. et al. Protein modification by the lipid peroxidation product 4-hydroxynonenal in the spinal cords of amyotrophic lateral sclerosis patients. Ann. Neurol. 44, 819–824 (1998).
Graham, D. G. Oxidative pathways for catecholamines in the genesis of neuromelanin and cytotoxic quinones. Mol. Pharmacol. 14, 633–643 (1978).
Maker, H. S., Weiss, C., Silides, D. J. & Cohen, G. Coupling of dopamine oxidation (monoamine oxidase activity) to glutathione oxidation via the generation of hydrogen peroxide in rat brain homogenates. J. Neurochem. 36, 589–593 (1981).
Halliwell, B. Reactive oxygen species and the central nervous system. J. Neurochem. 59, 1609–1623 (1992).
Jenner, P. Oxidative mechanisms in nigral cell death in Parkinson's disease. Mov. Disord. 13 (Suppl. 1), 24–34 (1998).
Sofic, E. et al. Increased iron (III) and total iron content in post mortem substantia nigra of parkinsonian brain. J. Neural Transm. 74, 199–205 (1988).
Saggu, H. et al. A selective increase in particulate superoxide dismutase activity in parkinsonian substantia nigra. J. Neurochem. 53, 692–697 (1989).
Dexter, D. T. et al. Basal lipid peroxidation in substantia nigra is increased in Parkinson's disease. J. Neurochem. 52, 381–389 (1989).
Floor, E. & Wetzel, M. G. Increased protein oxidation in human substantia nigra pars compacta in comparison with basal ganglia and prefrontal cortex measured with an improved dinitrophenylhydrazine assay. J. Neurochem. 70, 268–275 (1998).
Alam, Z. I. et al. Oxidative DNA damage in the parkinsonian brain: an apparent selective increase in 8-hydroxyguanine levels in substantia nigra. J. Neurochem. 69, 1196–1203 (1997).
Dexter, D. T. et al. Increased nigral iron content and alterations in other metal ions occurring in brain in Parkinson's disease. J. Neurochem. 52, 1830–1836 (1989).
Yoritaka, A. et al. Immunohistochemical detection of 4-hydroxynonenal protein adducts in Parkinson disease. Proc. Natl Acad. Sci. USA 93, 2696–2701 (1996).
Zhang, J. et al. Parkinson's disease is associated with oxidative damage to cytoplasmic DNA and RNA in substantia nigra neurons. Am. J. Pathol. 154, 1423–1429 (1999).
Alam, Z. I. et al. A generalised increase in protein carbonyls in the brain in Parkinson's but not incidental Lewy body disease. J. Neurochem. 69, 1326–1329 (1997).
Schulz, J. B., Lindenau, J., Seyfried, J. & Dichgans, J. Glutathione, oxidative stress and neurodegeneration. Eur. J. Biochem. 267, 4904–4911 (2000).
Marttila, R. J., Lorentz, H. & Rinne, U. K. Oxygen toxicity protecting enzymes in Parkinson's disease. Increase of superoxide dismutase-like activity in the substantia nigra and basal nucleus. J. Neurol. Sci. 86, 321–331 (1988).
Ben-Shachar, D., Riederer, P. & Youdim, M. B. Iron–melanin interaction and lipid peroxidation: implications for Parkinson's disease. J. Neurochem. 57, 1609–1614 (1991).
Riederer, P. et al. Transition metals, ferritin, glutathione, and ascorbic acid in parkinsonian brains. J. Neurochem. 52, 515–520 (1989).
Jellinger, K. et al. Iron–melanin complex in substantia nigra of parkinsonian brains: an X-ray microanalysis. J. Neurochem. 59, 1168–1171 (1992).
Dexter, D. T. et al. Nigral dopaminergic cell loss in vitamin E deficient rats. Neuroreport 5, 1773–1776 (1994).
Przedborski, S. & Jackson-Lewis, V. Mechanisms of MPTP toxicity. Mov. Disord. 13 (Suppl. 1), 35–38 (1998).
Del Zompo, M., Piccardi, M. P., Ruiu, S., Corsini, G. U. & Vaccari, A. High-affinity binding of [3H]1-methyl-4-phenyl-2,3-dihydropyridinium ion to mouse striatal membranes: putative vesicular location. Eur. J. Pharmacol. 202, 293–294 (1991).
Del Zompo, M., Piccardi, M. P., Ruiu, S., Corsini, G. U. & Vaccari, A. Characterization of a putatively vesicular binding site for [3H]MPP+ in mouse striatal membranes. Brain Res. 571, 354–357 (1992).
Peter, D., Jimenez, J., Liu, Y., Kim, J. & Edwards, R. H. The chromaffin granule and synaptic vesicle amine transporters differ in substrate recognition and sensitivity to inhibitors. J. Biol. Chem. 269, 7231–7237 (1994).
Nicklas, W. J., Vyas, I. & Heikkila, R. E. Inhibition of NADH-linked oxidation in brain mitochondria by 1-methyl-4-phenyl-pyridine, a metabolite of the neurotoxin, 1-methyl-4-phenyl-1,2,5,6-tetrahydropyridine. Life Sci. 36, 2503–2508 (1985).
Ramsay, R. R., Salach, J. I. & Singer, T. P. Uptake of the neurotoxin 1-methyl-4-phenylpyridine (MPP+) by mitochondria and its relation to the inhibition of the mitochondrial oxidation of NAD+-linked substrates by MPP+. Biochem. Biophys. Res. Commun. 134, 743–748 (1986).
Ramsay, R. R. et al. Interaction of 1-methyl-4-phenylpyridinium ion (MPP+) and its analogs with the rotenone/piericidin binding site of NADH dehydrogenase. J. Neurochem. 56, 1184–1190 (1991).
Denton, T. & Howard, B. D. A dopaminergic cell line variant resistant to the neurotoxin 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine. J. Neurochem. 49, 622–630 (1987).
Krueger, M. J., Singer, T. P., Casida, J. E. & Ramsay, R. R. Evidence that the blockade of mitochondrial respiration by the neurotoxin 1-methyl-4-phenylpyridinium (MPP+) involves binding at the same site as the respiratory inhibitor, rotenone. Biochem. Biophys. Res. Commun. 169, 123–128 (1990).
Lotharius, J. & O'Malley, K. L. The parkinsonism-inducing drug 1-methyl-4-phenylpyridinium triggers intracellular dopamine oxidation. A novel mechanism of toxicity. J. Biol. Chem. 275, 38581–38588 (2000).The first study to show that dopamine-dependent oxidative stress contributes to the toxicity of the parkinsonism-inducing drug MPTP.
Jones, S. R., Gainetdinov, R. R., Wightman, R. M. & Caron, M. G. Mechanisms of amphetamine action revealed in mice lacking the dopamine transporter. J. Neurosci. 18, 1979–1986 (1998).
Sulzer, D. & Rayport, S. Amphetamine and other psychostimulants reduce pH gradients in midbrain dopaminergic neurons and chromaffin granules: a mechanism of action. Neuron 5, 797–808 (1990).The first study to show that amphetamine leads to the cytoplasmic accumulation of dopamine by disrupting the pH gradient across vesicular membranes, which provides the proton-motive force required by the vesicular monoamine transporter.
Sulzer, D. et al. Amphetamine redistributes dopamine from synaptic vesicles to the cytosol and promotes reverse transport. J. Neurosci. 15, 4102–4108 (1995).The first report to show that amphetamine promotes reverse transport of dopamine through the plasma-membrane dopamine transporter after its redistribution from vesicles to the cytosol.
Seiden, L. S., Commins, D. L., Vosmer, G., Axt, K. & Marek, G. Neurotoxicity in dopamine and 5-hydroxytryptamine terminal fields: a regional analysis in nigrostriatal and mesolimbic projections. Ann. NY Acad. Sci. 537, 161–172 (1988).
Sonsalla, P. K., Jochnowitz, N. D., Zeevalk, G. D., Oostveen, J. A. & Hall, E. D. Treatment of mice with methamphetamine produces cell loss in the substantia nigra. Brain Res. 738, 172–175 (1996).
Schmidt, C. J., Ritter, J. K., Sonsalla, P. K., Hanson, G. R. & Gibb, J. W. Role of dopamine in the neurotoxic effects of methamphetamine. J. Pharmacol. Exp. Ther. 233, 539–544 (1985).By showing that rats pretreated with a dopamine-synthesis inhibitor show less toxicity in response to methamphetamine than non-treated rats, this study was one of the first to suggest that dopamine is involved in the neurotoxic actions of this psychostimulant.
De Vito, M. J. & Wagner, G. C. Methamphetamine-induced neuronal damage: a possible role for free radicals. Neuropharmacology 28, 1145–1150 (1989).
Cadet, J. L., Ladenheim, B., Baum, I., Carlson, E. & Epstein, C. CuZn-superoxide dismutase (CuZnSOD) transgenic mice show resistance to the lethal effects of methylenedioxyamphetamine (MDA) and of methylenedioxymethamphetamine (MDMA). Brain Res. 655, 259–262 (1994).
Betarbet, R. et al. Chronic systemic pesticide exposure reproduces features of Parkinson's disease. Nature Neurosci. 3, 1301–1306 (2000).
McCormack, A. L. et al. Environmental risk factors and Parkinson's disease: selective degeneration of nigral dopaminergic neurons caused by the herbicide paraquat. Neurobiol. Dis. 10, 119–127 (2002).
Le Couteur, D. G., McLean, A. J., Taylor, M. C., Woodham, B. L. & Board, P. G. Pesticides and Parkinson's disease. Biomed. Pharmacother. 53, 122–130 (1999).
Liou, H. H. et al. Environmental risk factors and Parkinson's disease: a case-control study in Taiwan. Neurology 48, 1583–1588 (1997).
Fukushima, T., Yamada, K., Isobe, A., Shiwaku, K. & Yamane, Y. Mechanism of cytotoxicity of paraquat. I. NADH oxidation and paraquat radical formation via complex I. Exp. Toxicol. Pathol. 45, 345–349 (1993).
Lewy, F. in Handbuch der Neurologie Vol. 3 (eds Lewandowski, M. & Abelsdorff, G.) 920–933 (Springer, Berlin, 1912).
Goedert, M. α-Synuclein and neurodegenerative diseases. Nature Rev. Neurosci. 2, 492–501 (2001).
Spillantini, M. G. et al. α-Synuclein in Lewy bodies. Nature 388, 839–840 (1997).
George, J. M. The synucleins. Genome Biol. 3, reviews3002.1–3002.6 (2002). | PubMed |
Polymeropoulos, M. H. et al. Mutation in the α-synuclein gene identified in families with Parkinson's disease. Science 276, 2045–2047 (1997).The first study to link mutations in the α-synuclein gene to familial Parkinson's disease.
Krüger, R. et al. Ala30Pro mutation in the gene encoding α-synuclein in Parkinson's disease. Nature Genet. 18, 106–108 (1998).
Kitada, T. et al. Mutations in the parkin gene cause autosomal recessive juvenile parkinsonism. Nature 392, 605–608 (1998).
Giasson, B. I. & Lee, V. M. Parkin and the molecular pathways of Parkinson's disease. Neuron 31, 885–888 (2001).
Leroy, E. et al. The ubiquitin pathway in Parkinson's disease. Nature 395, 451–452 (1998).
Liu, Y., Fallon, L., Lashuel, H. A., Liu, Z. & Lansbury, P. T. Jr. The UCH-L1 gene encodes two opposing enzymatic activities that affect α-synuclein degradation and parkinson's disease susceptibility. Cell 111, 209–218 (2002).
Kuzuhara, S., Mori, H., Izumiyama, N., Yoshimura, M. & Ihara, Y. Lewy bodies are ubiquitinated. A light and electron microscopic immunocytochemical study. Acta Neuropathol. (Berl.) 75, 345–353 (1988).
Ii, K., Ito, H., Tanaka, K. & Hirano, A. Immunocytochemical co-localization of the proteasome in ubiquitinated structures in neurodegenerative diseases and the elderly. J. Neuropathol. Exp. Neurol. 56, 125–131 (1997).
Auluck, P. K., Chan, H. Y., Trojanowski, J. Q., Lee, V. M. & Bonini, N. M. Chaperone suppression of α-synuclein toxicity in a Drosophila model for Parkinson's disease. Science 295, 865–868 (2002).
Galvin, J. E. et al. Monoclonal antibodies to purified cortical Lewy bodies recognize the mid-size neurofilament subunit. Ann. Neurol. 42, 595–603 (1997).
Conway, K. A., Harper, J. D. & Lansbury, P. T. Fibrils formed in vitro from α-synuclein and two mutant forms linked to Parkinson's disease are typical amyloid. Biochemistry 39, 2552–2563 (2000).
Conway, K. A. et al. Acceleration of oligomerization, not fibrillization, is a shared property of both α-synuclein mutations linked to early-onset Parkinson's disease: implications for pathogenesis and therapy. Proc. Natl Acad. Sci. USA 97, 571–576 (2000).The first study to show that both α-synuclein mutations increase the protein's ability to form oligomers, key intermediates in the aggregation process.
Bucciantini, M. et al. Inherent toxicity of aggregates implies a common mechanism for protein misfolding diseases. Nature 416, 507–511 (2002).The first paper to show that prefibrillar, aggregated forms of non-disease-associated proteins are highly toxic to cells.
Goldberg, M. S. & Lansbury, P. T. Jr. Is there a cause-and-effect relationship between α-synuclein fibrillization and Parkinson's disease? Nature Cell Biol. 2, E115–E119 (2002).
Lee, H. J. & Lee, S. J. Characterization of cytoplasmic α-synuclein aggregates: fibril formation is tightly linked to the inclusion forming process in cells. J. Biol. Chem. 25 September 2002 (doi:10.1074/jbc.M208192200). | PubMed |
Gosavi, N., Lee, H. J., Lee, J. S., Patel, S. & Lee, S. J. Golgi fragmentation occurs in the cells with prefibrillar α-synuclein aggregates and precedes the formation of fibrillar inclusion. J. Biol. Chem. 25 September 2002 (doi:10.1074/jbc.M208194200).
Tompkins, M. M. & Hill, W. D. Contribution of somal Lewy bodies to neuronal death. Brain Res. 775, 24–29 (1997).
Hurtig, H. I. et al. α-synuclein cortical Lewy bodies correlate with dementia in Parkinson's disease. Neurology 54, 1916–1921 (2000).
Mattila, P. M., Rinne, J. O., Helenius, H., Dickson, D. W. & Roytta, M. α-synuclein-immunoreactive cortical Lewy bodies are associated with cognitive impairment in Parkinson's disease. Acta Neuropathol. (Berl.) 100, 285–290 (2000).
Shtilerman, M. D., Ding, T. T. & Lansbury, P. T. Jr. Molecular crowding accelerates fibrillization of α-synuclein: could an increase in the cytoplasmic protein concentration induce Parkinson's disease? Biochemistry 41, 3855–3860 (2002).
Conway, K. A., Rochet, J. C., Bieganski, R. M. & Lansbury, P. T. Jr. Kinetic stabilization of the α-synuclein protofibril by a dopamine–α-synuclein adduct. Science 294, 1346–1349 (2001).
Volles, M. J. et al. Vesicle permeabilization by protofibrillar α-synuclein: implications for the pathogenesis and treatment of Parkinson's disease. Biochemistry 40, 7812–7819 (2001).This study shows that protofibrillar α-synuclein can permeabilize vesicles, allowing the leakage of small molecules, such as dopamine, which could potentially lead to an increase in cytoplasmic dopamine levels.
Volles, M. J. & Lansbury, P. T. Jr. Vesicle permeabilization by protofibrillar α-synuclein is sensitive to Parkinson's disease-linked mutations and occurs by a pore-like mechanism. Biochemistry 41, 4595–4602 (2002).
Lashuel, H. A., Hartley, D., Petre, B. M., Walz, T. & Lansbury, P. T. Neurodegenerative disease: amyloid pores from pathogenic mutations. Nature 418, 291 (2002).
Lashuel, H. et al. α-synuclein, especially the Parkinson's disease-associated mutants, forms pore-like annular and tubular protofibrils. J. Mol. Biol. 322, 1089 (2002).
Hashimoto, M. et al. Oxidative stress induces amyloid-like aggregate formation of NACP/α-synuclein in vitro. Neuroreport 10, 717–721 (1999).
Kim, K. S. et al. Aggregation of α-synuclein induced by the Cu,Zn-superoxide dismutase and hydrogen peroxide system. Free Radic. Biol. Med. 32, 544–550 (2002).
Sherman, M. Y. & Goldberg, A. L. Involvement of molecular chaperones in intracellular protein breakdown. EXS 77, 57–78 (1996).
Zhang, Y. et al. Parkin functions as an E2-dependent ubiquitin–protein ligase and promotes the degradation of the synaptic vesicle-associated protein, CDCrel-1. Proc. Natl Acad. Sci USA 97, 13354–13359 (2000).
Shimura, H. et al. Parkinson disease gene product, parkin, is a ubiquitin–protein ligase. Nature Genet. 25, 302–305 (2000).References 90 and 91 show that parkin is a key enzyme in the ubiquitin–proteasome system, and is essential for the degradation of cellular proteins.
West, A. B. et al. Functional association of the parkin gene promoter with idiopathic Parkinson's disease. Hum. Mol. Genet. 11, 2787–2792 (2002).
Farrer, M. et al. Lewy bodies and parkinsonism in families with parkin mutations. Ann. Neurol. 50, 293–300 (2001).
Chung, K. K. et al. Parkin ubiquitinates the α-synuclein-interacting protein, synphilin-1: implications for Lewy-body formation in Parkinson disease. Nature Med. 7, 1144–1150 (2001).
Engelender, S. et al. Synphilin-1 associates with α-synuclein and promotes the formation of cytosolic inclusions. Nature Genet. 22, 110–114 (1999).
Ribeiro, C. S., Carneiro, K., Ross, C. A., Menezes, J. R. & Engelender, S. Synphilin-1 is developmentally localized to synaptic terminals, and its association with synaptic vesicles is modulated by α-synuclein. J. Biol. Chem. 277, 23927–23933 (2002).
Bence, N. F., Sampat, R. M. & Kopito, R. R. Impairment of the ubiquitin–proteasome system by protein aggregation. Science 292, 1552–1555 (2001).
McNaught, K. St P. & Jenner, P. Proteasomal function is impaired in substantia nigra in Parkinson's disease. Neurosci. Lett. 297, 191–194 (2001).
Furukawa, Y. et al. Brain proteasomal function in sporadic Parkinson's disease and related disorders. Ann. Neurol. 51, 779–782 (2002).
McNaught, K. S., Belizaire, R., Jenner, P., Olanow, C. W. & Isacson, O. Selective loss of 20S proteasome α-subunits in the substantia nigra pars compacta in Parkinson's disease Neurosci. Lett. 326, 155–158 (2002).
Rideout, H. J., Larsen, K. E., Sulzer, D. & Stefanis, L. Proteasomal inhibition leads to formation of ubiquitin/α-synuclein-immunoreactive inclusions in PC12 cells. J. Neurochem. 78, 899–908 (2001).
McNaught, K. S. et al. Proteasome inhibition causes nigral degeneration with inclusion bodies in rats. Neuroreport 13, 1437–1441 (2002).
McNaught, K. S. et al. Impairment of the ubiquitin–proteasome system causes dopaminergic cell death and inclusion body formation in ventral mesencephalic cultures. J. Neurochem. 81, 301–306 (2002).
Abeliovich, A. et al. Mice lacking α-synuclein display functional deficits in the nigrostriatal dopamine system. Neuron 25, 239–252 (2000).The first group to delete the α-synuclein gene in mice report subtle defects in synaptic transmission but not in overt phenotype.
Cabin, D. E. et al. Synaptic vesicle depletion in mice lacking α-synuclein. J. Neurosci. 22, 8797–8807 (2002).
Dauer, W. et al. Resistance of α-synuclein null mice to the parkinsonism-inducing neurotoxin MPTP. Proc. Natl Acad. Sci. USA 99, 14524–14529 (2002).
Lotharius, J. et al. Effect of mutant α-synuclein on dopamine homeostasis in a new human mesencephalic cell line. J. Biol. Chem. 277, 38884–38894 (2002).This paper shows that mutant α-synuclein might increase cytoplasmic levels of dopamine in human mesencephalic cells.
Hansson, O. et al. Transgenic mice expressing a Huntington's disease mutation are resistant to quinolinic acid-induced striatal excitotoxicity. Proc. Natl Acad. Sci. USA 96, 8727–8732 (1999).
Hansson, O. et al. Resistance to NMDA toxicity correlates with appearance of nuclear inclusions, behavioural deficits and changes in calcium homeostasis in mice transgenic for exon 1 of the huntington gene. Eur. J. Neurosci. 14, 1492–1504 (2001).
Tyagi, P. & Tayal, G. Ischemic preconditioning of myocardium. Acta Pharmacol. Sin. 23, 865–870 (2002).
Masliah, E. et al. Dopaminergic loss and inclusion body formation in α-synuclein mice: implications for neurodegenerative disorders. Science 287, 1265–1269 (2000).This was the first α-synuclein transgenic mouse to be created; it overexpresses human wild-type α-synuclein under the control of the platelet-derived growth factor-β promoter. This is the only paper so far to report a nigrostriatal defect in mice that overexpress any form of α-synuclein.
Putten, H. et al. Neuropathology in mice expressing human α-synuclein. J. Neurosci. 20, 6021–6029 (2000).
Giasson, B. I. et al. Neuronal α-synucleinopathy with severe movement disorder in mice expressing A53T human α-synuclein. Neuron 34, 521–533 (2002).
Lee, M. K. et al. Human α-synuclein harboring familial Parkinson's disease-linked Ala-53 → Thr mutation causes neurodegenerative disease with α-synuclein aggregation in transgenic mice. Proc. Natl Acad. Sci. USA 99, 8968–8973 (2002).
Feany, M. B. & Bender, W. W. A Drosophila model of Parkinson's disease. Nature 404, 394–398 (2000).
Stein, T. D. & Johnson, J. A. Lack of neurodegeneration in transgenic mice overexpressing mutant amyloid precursor protein is associated with increased levels of transthyretin and the activation of cell survival pathways. J. Neurosci. 22, 7380–7388 (2002).
Zhou, W., Schaack, J., Zawada, W. M. & Freed, C. R. Overexpression of human α-synuclein causes dopamine neuron death in primary human mesencephalic culture. Brain Res. 926, 42–50 (2002).
Xu, J. et al. Dopamine-dependent neurotoxicity of α-synuclein: a mechanism for selective neurodegeneration in Parkinson's disease. Nature Med. 8, 600–606 (2002).This is the first study to show that dopamine contributes to the toxicity of mutant α-synuclein using primary human mesencephalic cultures.
Hartmann, A. & Hirsch, E. C. Parkinson's disease. The apoptosis hypothesis revisited. Adv. Neurol. 86, 143–153 (2001).
Lee, C. S. et al. In vivo positron emission tomographic evidence for compensatory changes in presynaptic dopaminergic nerve terminals in Parkinson's disease. Ann. Neurol. 47, 493–503 (2000).
da Costa, C. A., Ancolio, K. & Checler, F. Wild-type but not Parkinson's disease-related Ala-53 → Thr mutant α-synuclein protects neuronal cells from apoptotic stimuli. J. Biol. Chem. 275, 24065–24069 (2000).
Hashimoto, M. et al. α-synuclein protects against oxidative stress via inactivation of the c-Jun N-terminal kinase stress-signaling pathway in neuronal cells. J. Biol. Chem. 277, 11465–11472 (2002).
Seo, J. H. et al. α-synuclein regulates neuronal survival via Bcl-2 family expression and PI3/Akt kinase pathway. FASEB J. 5 September 2002 (doi:10.1096/fj.02–0041fje).
Davidson, W. S., Jonas, A., Clayton, D. F. & George, J. M. Stabilization of α-synuclein secondary structure upon binding to synthetic membranes. J. Biol. Chem. 273, 9443–9449 (1998).
Jensen, P. H., Nielsen, M. H., Jakes, R., Dotti, C. G. & Goedert, M. Binding of α-synuclein to rat brain vesicles is abolished by familial Parkinson's disease mutation. J. Biol. Chem. 273, 26292–26294 (1998).
Jo, E., Fuller, N., Rand, R. P., St George-Hyslop, P. & Fraser, P. E. Defective membrane interactions of familial Parkinson's disease mutant A30P α-synuclein. J. Mol. Biol. 315, 799–807 (2002).
Jo, E., McLaurin, J. A., Yip, C. M., St George-Hyslop, P. H. & Fraser, P. α-synuclein membrane interactions and lipid specificity. J. Biol. Chem. 275, 34328–34334 (2000).
Jenco, J. M., Rawlingson, A., Daniels, B. & Morris, A. J. Regulation of phospholipase D2: selective inhibition of mammalian phospholipase D isoenzymes by α- and β-synuclein. Biochemistry 37, 4901–4909 (1998).A seminal study indicating that an important housekeeping function of the synucleins might be to modulate PLD2 activity.
Ahn, B. H. et al. α-synuclein interacts with phospholipase D isozymes and inhibits pervanadate-induced phospholipase D activation in human embryonic kidney-293 cells. J. Biol. Chem. 277, 12334–12342 (2002).
Cockcroft, S. Signalling roles of mammalian phospholipase D1 and D2. Cell. Mol. Life Sci. 58, 1674–1687 (2001).
Liscovitch, M., Czarny, M., Fiucci, G. & Tang, X. Phospholipase D: molecular and cell biology of a novel gene family. Biochem. J. 345, 401–415 (2000).
Lotharius, J. & Brundin, P. Impaired dopamine storage resulting from α-synuclein mutations may contribute to the pathogenesis of Parkinson's disease. Hum. Mol. Genet. 11, 2395–2407 (2002).
Murphy, D. D., Rueter, S. M., Trojanowski, J. Q. & Lee, V. M. Synucleins are developmentally expressed, and α-synuclein regulates the size of the presynaptic vesicular pool in primary hippocampal neurons. J. Neurosci. 20, 3214–2310 (2000).A study showing that deletion of wild-type α-synuclein using antisense oligonucleotide technology reduces the number of vesicles in the reserve pool, indicating that α-synuclein might regulate vesicle biogenesis.
Kahle, P. J. et al. Subcellular localization of wild-type and Parkinson's disease-associated mutant α-synuclein in human and transgenic mouse brain. J. Neurosci. 20, 6365–6373 (2000).
Rathke-Hartlieb, S. et al. Sensitivity to MPTP is not increased in Parkinson's disease-associated mutant α-synuclein transgenic mice. J. Neurochem. 77, 1181–1184 (2001).
Matsuoka, Y. & Vila, M. et al. Lack of nigral pathology in transgenic mice expressing human α-synuclein driven by the tyrosine hydroxylase promoter. Neurobiol. Dis. 8, 535–539 (2001).
Richfield, E. K. et al. Behavioral and neurochemical effects of wild-type and mutated human α-synuclein in transgenic mice. Exp. Neurol. 175, 35–48 (2002).
Acknowledgements
Our work described in this article was supported by grants from the US Parkinson's Disease Foundation, the Swedish Parkinson's Disease Foundation and the Swedish Research Council, and by awards from the Swedish Society for the Neurologically Handicapped and the Åke Wiberg Foundation. We thank members of the EU-funded concerted action on Early Pathogenetic Markers of Slow Neurodegenerative Diseases for fruitful discussions, M.-F. Chesselet, S. Lund, G. Paul and R. Smith for critical reading of the manuscript, and B. Mattsson for invaluable help with figures.
Author information
Authors and Affiliations
Related links
Related links
DATABASES
Locuslink
OMIM
FURTHER INFORMATION
Section for Neuronal Survival, Lund University
Encyclopedia of Life Sciences
Glossary
- CATECHOLAMINE
-
A neurotransmitter that is characterized by a catechol ring and an alkylamine side chain; examples are dopamine, adrenaline and noradrenaline.
- OXIDATIVE STRESS
-
A state of imbalance between the production of reactive oxygen species and their clearance by cellular antioxidant systems.
- LEWY BODY
-
An electron-dense, intracytoplasmic neuronal inclusion composed of granular and filamentous material that is particularly prevalent in the brains of patients with Parkinson's disease, dementia with Lewy bodies and Lewy body disease.
- GLIOSIS
-
The process of producing of a dense fibrous network of neuroglia; includes astrocytosis — the proliferation of astrocytes in the area of a degenerative lesion.
- PROTEIN CARBONYL
-
The characteristic −C=O group of aldehydes and ketones, which are derived from the direct oxidation of amino-acid side chains by reactive oxygen species. They are indicative of oxidative damage to proteins.
- DOPAMINE–QUINONE
-
A reactive molecule that is formed by the spontaneous oxidation of dopamine; it can react with and covalently modify cysteinyl residues in proteins.
- LOCUS COERULEUS
-
A nucleus of the brainstem that is the main supplier of noradrenaline to the brain.
- RAPHE NUCLEI
-
A series of neuronal groups located along the midline of the brainstem. They constitute the main supply of 5-hydroxytryptamine to the rest of the brain.
- UBIQUITIN–PROTEASOME PATHWAY
-
A cellular system that is responsible for degrading damaged or misfolded proteins; attachment of ubiquitin molecules to lysine residues in a given protein targets it for destruction by a multi-enzyme complex known as the proteasome.
- PROTOFIBRIL
-
An intermediate species resembling an elongated filament that is formed in the fibrillization process from monomer to fibril.
- RESERVE POOL
-
A population of vesicles distal to the active zone that is recruited during periods of high-frequency stimulation.
- ISCHAEMIC PRECONDITIONING
-
A phenomenon whereby a brief interruption of blood supply to the brain protects the tissue from a subsequent ischaemic episode.
- PC12 CELLS
-
Neuron-like cells that are derived from a malignant neural crest tumour (a phaeochromocytoma).
- ADAPTOR MOLECULE
-
A protein that contributes to cellular function by recruiting other proteins to a complex. Such molecules often contain several protein–protein interaction domains.
- ANTISENSE OLIGONUCLEOTIDE
-
An RNA sequence complementary to the messenger RNA of a given gene that can hybridize to this piece of RNA, thereby blocking its translation into protein.
- ACTIVE ZONE
-
A portion of the presynaptic membrane that faces the postsynaptic density across the synaptic cleft. It constitutes the site of synaptic vesicle clustering, docking and transmitter release.
- READILY RELAEASABLE POOL
-
The pool of synaptic vesicles that is available for rapid fusion with the presynaptic membrane in response to the arrival of a nerve impulse. These vesicles are docked to the membrane and have been biochemically primed for release.
Rights and permissions
About this article
Cite this article
Lotharius, J., Brundin, P. Pathogenesis of parkinson's disease: dopamine, vesicles and α-synuclein. Nat Rev Neurosci 3, 932–942 (2002). https://doi.org/10.1038/nrn983
Issue Date:
DOI: https://doi.org/10.1038/nrn983
This article is cited by
-
PLCγ1 in dopamine neurons critically regulates striatal dopamine release via VMAT2 and synapsin III
Experimental & Molecular Medicine (2023)
-
Transcriptional mutagenesis of α-synuclein caused by DNA oxidation in Parkinson’s disease pathogenesis
Acta Neuropathologica (2023)
-
Effects of acupuncture and moxibustion on PINK1/Parkin signaling pathway in substantia nigra of Thy1-αSyn transgenic mice with Parkinson disease
Journal of Acupuncture and Tuina Science (2023)
-
A core-satellite-like nanoassembly reverses a decisive tyrosine hydroxylase loss in degenerative dopaminergic neurons
Nano Research (2023)
-
Early diagnosis and clinical score prediction of Parkinson's disease based on longitudinal neuroimaging data
Neural Computing and Applications (2023)