Key Points
-
Innate lymphoid cells (ILCs) are newly identified members of the lymphoid lineage with emerging roles in mediating immune responses and in regulating tissue homeostasis and inflammation.
-
The existence of different ILC populations that can rapidly secrete immunoregulatory cytokines suggests that these cells may have evolved to provide immunity to infections. Indeed, it is notable that ILC subsets seem to be particularly prevalent at mucosal surfaces, which are constantly exposed to infectious agents in the external environment.
-
The group 1 ILC lineage comprises ILCs such as natural killer (NK) cells that produce type 1 cytokines, notably interferon-γ and tumour necrosis factor. Other group 1 ILCs have been reported, mainly in vitro, and their physiological roles remain to be defined.
-
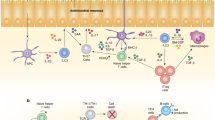
The group 2 ILC population comprises ILC2s, which express interleukin-5 (IL-5) and IL-13 and require GATA-binding protein 3 (GATA3) and retinoic acid receptor-related orphan receptor-α (RORα) for their development. They have crucial roles in protective type 2 immunity to helminth infection. Furthermore, although T helper 2 cells are a major source of type 2 cytokines during allergic asthma, ILC2s also contribute to disease pathology.
-
ILC3s were first defined as intestinal lymphoid cells that express the NK cell activating receptor NKp46, but otherwise bear little functional resemblance to conventional NK cells, and require RORγ for their development. They express IL-17A and IL-22.
-
Recent studies have also implicated ILC3s in the development of inflammatory bowel disease. Studies in Rag2−/− mice demonstrated that, in the early phase of Citrobacter rodentium infection, IL-22 is produced from an innate cell source.
-
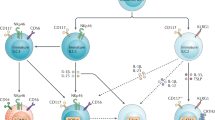
Lymphoid tissue-inducer (LTi) cells are an ILC subset that appears to be closely related to ILC3s, but their exact relationship remains controversial. Together, LTi cells and ILC3s have been classified as group 3 ILCs.
Abstract
Innate lymphoid cells (ILCs) are newly identified members of the lymphoid lineage that have emerging roles in mediating immune responses and in regulating tissue homeostasis and inflammation. Here, we review the developmental relationships between the various ILC lineages that have been identified to date and summarize their functions in protective immunity to infection and their pathological roles in allergic and autoimmune diseases.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Spits, H. et al. Innate lymphoid cells — a proposal for uniform nomenclature. Nature Rev. Immunol. 7 Jan 2013 (doi:10.1038/nri3365).
Kiessling, R. Klein, E., Pross, H. & Wigzell, H. “Natural” killer cells in the mouse. II. Cytotoxic cells with specificity for mouse Moloney leukemia cells. Characteristics of the killer cell. Eur. J. Immunol. 5, 117–121 (1975).
Herberman, R. B., Nunn, M. E., Holden, H. T. & Lavrin, D. H. Natural cytotoxic reactivity of mouse lymphoid cells against syngeneic and allogeneic tumors. II. Characterization of effector cells. Int. J. Cancer. 16, 230–239 (1975).
Vivier, E. et al. Innate or adaptive immunity? The example of natural killer cells. Science 331, 44–49 (2011).
Di Santo, J. P. & Vosshenrich, C. A. Bone marrow versus thymic pathways of natural killer cell development. Immunol. Rev. 214, 35–46 (2006).
Crellin, N. K., Trifari, S., Kaplan, C. D., Cupedo, T. & Spits, H. Human NKp44+IL-22+ cells and LTi-like cells constitute a stable RORC+ lineage distinct from conventional natural killer cells. J. Exp. Med. 207, 281–290 (2010).
Hurst, S. D. et al. New IL-17 family members promote Th1 or Th2 responses in the lung: in vivo function of the novel cytokine IL-25. J. Immunol. 169, 443–453 (2002).
Fort, M. M. et al. IL-25 induces IL-4, IL-5, and IL-13 and Th2-associated pathologies in vivo. Immunity 15, 985–995 (2001).
Fallon, P. G. et al. Identification of an interleukin (IL)-25-dependent cell population that provides IL-4, IL-5, and IL-13 at the onset of helminth expulsion. J. Exp. Med. 203, 1105–1116 (2006).
Moro, K. et al. Innate production of TH2 cytokines by adipose tissue-associated c-Kit+Sca-1+ lymphoid cells. Nature 463, 540–544 (2010).
Neill, D. R. et al. Nuocytes represent a new innate effector leukocyte that mediates type-2 immunity. Nature 464, 1367–1370 (2010).
Price, A. E. et al. Systemically dispersed innate IL-13-expressing cells in type 2 immunity. Proc. Natl Acad. Sci. USA 107, 11489–11494 (2010). References 10–12 comprehensively characterize the group 2 ILCs (referred to as nuocytes, NHCs and I H 2 cells) that were first identified in references 7–9.
Barlow, J. L. et al. Innate IL-13-producing nuocytes arise during allergic lung inflammation and contribute to airways hyperreactivity. J. Allergy Clin. Immunol. 129, 191–198 (2012).
Bartemes, K. R. et al. IL-33-responsive lineage−CD25+CD44hi lymphoid cells mediate innate type 2 immunity and allergic inflammation in the lungs. J. Immunol. 188, 1505–1513 (2011).
Chang, Y. J. et al. Innate lymphoid cells mediate influenza-induced airway hyper-reactivity independently of adaptive immunity. Nature Immunol. 12, 631–638 (2011).
Kim, H. Y. et al. Innate lymphoid cells responding to IL-33 mediate airway hyperreactivity independently of adaptive immunity. J. Allergy Clin. Immunol. 129, 216–227 (2012).
Monticelli, L. A. et al. Innate lymphoid cells promote lung-tissue homeostasis after infection with influenza virus. Nature Immunol. 12, 1045–1054 (2011).
Halim, T. Y. et al. Retinoic-acid-receptor-related orphan nuclear receptor α is required for natural helper cell development and allergic inflammation. Immunity 37, 463–474 (2012).
Wong, S. H. et al. Transcription factor RORα is critical for nuocyte development. Nature Immunol. 13, 229–236 (2012). References 18 and 19 illustrate the crucial role for the transcription factor RORα in the development of ILC2s.
Hoyler, T. et al. The transcription factor GATA-3 controls cell fate and maintenance of type 2 innate lymphoid cells. Immunity 37, 634–648 (2012).
Mjosberg, J. et al. The transcription factor GATA3 is essential for the function of human type 2 innate lymphoid cells. Immunity 37, 649–659 (2012). References 20 and 21 characterize the role of the transcription factor GATA3 in ILC2 development in mice and humans.
Barlow, J. L. & McKenzie, A. N. Nuocytes: expanding the innate cell repertoire in type-2 immunity. J. Leukoc. Biol. 90, 867–874 (2011).
Mjosberg, J. M. et al. Human IL-25- and IL-33-responsive type 2 innate lymphoid cells are defined by expression of CRTH2 and CD161. Nature Immunol. 12, 1055–1062 (2011). This paper is the first description of ILC2s in humans.
Luci, C. et al. Influence of the transcription factor RORγt on the development of NKp46+ cell populations in gut and skin. Nature Immunol. 10, 75–82 (2009).
Sanos, S. L. et al. RORγt and commensal microflora are required for the differentiation of mucosal interleukin 22-producing NKp46+ cells. Nature Immunol. 10, 83–91 (2009).
Satoh-Takayama, N. et al. Microbial flora drives interleukin 22 production in intestinal NKp46+ cells that provide innate mucosal immune defense. Immunity 29, 958–970 (2008). References 24–26 are the first reports of intestinal lymphoid cells that express NKp46 but are distinct from NK cells and require the transcription factor ROR? for their development.
Satoh-Takayama, N. et al. IL-7 and IL-15 independently program the differentiation of intestinal CD3−NKp46+ cell subsets from Id2-dependent precursors. J. Exp. Med. 207, 273–280 (2010).
Vonarbourg, C. et al. Regulated expression of nuclear receptor RORγt confers distinct functional fates to NK cell receptor-expressing RORγt+ innate lymphocytes. Immunity 33, 736–751 (2010).
Cella, M. et al. A human natural killer cell subset provides an innate source of IL-22 for mucosal immunity. Nature 457, 722–725 (2009).
Cupedo, T. et al. Human fetal lymphoid tissue-inducer cells are interleukin 17-producing precursors to RORC+ CD127+ natural killer-like cells. Nature Immunol. 10, 66–74 (2009).
Hughes, T. et al. Stage 3 immature human natural killer cells found in secondary lymphoid tissue constitutively and selectively express the TH17 cytokine interleukin-22. Blood 113, 4008–4010 (2009).
Mebius, R. E., Rennert, P. & Weissman, I. L. Developing lymph nodes collect CD4+CD3− LTβ+ cells that can differentiate to APC, NK cells, and follicular cells but not T or B cells. Immunity 7, 493–504 (1997).
Mebius, R. E., Streeter, P. R., Michie, S., Butcher, E. C. & Weissman, I. L. A developmental switch in lymphocyte homing receptor and endothelial vascular addressin expression regulates lymphocyte homing and permits CD4+ CD3− cells to colonize lymph nodes. Proc. Natl Acad. Sci. USA 93, 11019–11024 (1996).
Yoshida, H. et al. IL-7 receptor α+ CD3− cells in the embryonic intestine induces the organizing center of Peyer's patches. Int. Immunol. 11, 643–655 (1999).
Eberl, G. et al. An essential function for the nuclear receptor RORγt in the generation of fetal lymphoid tissue inducer cells. Nature Immunol. 5, 64–73 (2004).
Eberl, G. & Littman, D. R. Thymic origin of intestinal αβ T cells revealed by fate mapping of RORγt+ cells. Science 305, 248–251 (2004).
Scandella, E. et al. Restoration of lymphoid organ integrity through the interaction of lymphoid tissue-inducer cells with stroma of the T cell zone. Nature Immunol. 9, 667–675 (2008).
Withers, D. R. et al. Cutting edge: lymphoid tissue inducer cells maintain memory CD4 T cells within secondary lymphoid tissue. J. Immunol. 189, 2094–2098 (2012).
Takatori, H. et al. Lymphoid tissue inducer-like cells are an innate source of IL-17 and IL-22. J. Exp. Med. 206, 35–41 (2009).
Sonnenberg, G. F., Monticelli, L. A., Elloso, M. M., Fouser, L. A. & Artis, D. CD4+ lymphoid tissue-inducer cells promote innate immunity in the gut. Immunity 34, 122–134 (2011).
O'Shea, J. J. & Paul, W. E. Mechanisms underlying lineage commitment and plasticity of helper CD4+ T cells. Science 327, 1098–1102 (2010).
Yoshida, H. et al. Expression of α4β7 integrin defines a distinct pathway of lymphoid progenitors committed to T cells, fetal intestinal lymphotoxin producer, NK, and dendritic cells. J. Immunol. 167, 2511–2521 (2001).
Mebius, R. E. et al. The fetal liver counterpart of adult common lymphoid progenitors gives rise to all lymphoid lineages, CD45+CD4+CD3− cells, as well as macrophages. J. Immunol. 166, 6593–6601 (2001).
Yang, Q., Saenz, S. A., Zlotoff, D. A., Artis, D. & Bhandoola, A. Cutting edge: natural helper cells derive from lymphoid progenitors. J. Immunol. 187, 5505–5509 (2011).
Sawa, S. et al. Lineage relationship analysis of RORγt+ innate lymphoid cells. Science 330, 665–669 (2010).
Cherrier, M., Sawa, S. & Eberl, G. Notch, Id2, and RORγt sequentially orchestrate the fetal development of lymphoid tissue inducer cells. J. Exp. Med. 209, 729–740 (2012).
Possot, C. et al. Notch signaling is necessary for adult, but not fetal, development of RORγt+ innate lymphoid cells. Nature Immunol. 12, 949–958 (2011).
Yokota, Y. et al. Development of peripheral lymphoid organs and natural killer cells depends on the helix-loop-helix inhibitor Id2. Nature 397, 702–706 (1999).
Boos, M. D., Yokota, Y., Eberl, G. & Kee, B. L. Mature natural killer cell and lymphoid tissue-inducing cell development requires Id2-mediated suppression of E protein activity. J. Exp. Med. 204, 1119–1130 (2007).
Spits, H. & Di Santo, J. P. The expanding family of innate lymphoid cells: regulators and effectors of immunity and tissue remodeling. Nature Immunol. 12, 21–27 (2011).
Kiss, E. A. et al. Natural aryl hydrocarbon receptor ligands control organogenesis of intestinal lymphoid follicles. Science 334, 1561–1565 (2011).
Lee, J. S. et al. AHR drives the development of gut ILC22 cells and postnatal lymphoid tissues via pathways dependent on and independent of Notch. Nature Immunol. 13, 144–151 (2012).
Qiu, J. et al. The aryl hydrocarbon receptor regulates gut immunity through modulation of innate lymphoid cells. Immunity 36, 92–104 (2012).
Cella, M., Otero, K. & Colonna, M. Expansion of human NK-22 cells with IL-7, IL-2, and IL-1β reveals intrinsic functional plasticity. Proc. Natl Acad. Sci. USA 107, 10961–10966 (2010).
Hughes, T. et al. Interleukin-1β selectively expands and sustains interleukin-22+ immature human natural killer cells in secondary lymphoid tissue. Immunity 32, 803–814 (2010).
Buonocore, S. et al. Innate lymphoid cells drive interleukin-23-dependent innate intestinal pathology. Nature 464, 1371–1375 (2010). This paper is the first description of ILCs in inflammatory bowel disease models.
Vonarbourg, C. & Diefenbach, A. Multifaceted roles of interleukin-7 signaling for the development and function of innate lymphoid cells. Semin. Immunol. 24, 165–174 (2012).
Liang, H. E. et al. Divergent expression patterns of IL-4 and IL-13 define unique functions in allergic immunity. Nature Immunol. 13, 58–66 (2012).
Bajoghli, B. et al. Evolution of genetic networks underlying the emergence of thymopoiesis in vertebrates. Cell 138, 186–197 (2009).
Alder, M. N. et al. Diversity and function of adaptive immune receptors in a jawless vertebrate. Science 310, 1970–1973 (2005).
Pancer, Z. et al. Variable lymphocyte receptors in hagfish. Proc. Natl Acad. Sci. USA 102, 9224–9229 (2005).
Bajoghli, B. et al. A thymus candidate in lampreys. Nature 470, 90–94 (2011).
Saito, H. et al. Generation of intestinal T cells from progenitors residing in gut cryptopatches. Science 280, 275–278 (1998).
Wang, T., Martin, S. A. & Secombes, C. J. Two interleukin-17C-like genes exist in rainbow trout Oncorhynchus mykiss that are differentially expressed and modulated. Dev. Comp. Immunol. 34, 491–500 (2010).
Tsutsui, S., Nakamura, O. & Watanabe, T. Lamprey (Lethenteron japonicum) IL-17 upregulated by LPS-stimulation in the skin cells. Immunogenetics 59, 873–882 (2007).
Ohtani, M., Hayashi, N., Hashimoto, K., Nakanishi, T. & Dijkstra, J. M. Comprehensive clarification of two paralogous interleukin 4/13 loci in teleost fish. Immunogenetics 60, 383–397 (2008).
Lane, P. J., Gaspal, F. M., McConnell, F. M., Withers, D. R. & Anderson, G. Lymphoid tissue inducer cells: pivotal cells in the evolution of CD4 immunity and tolerance? Front. Immunol. 3, 24 (2012).
Flores, M. V., Hall, C., Jury, A., Crosier, K. & Crosier, P. The zebrafish retinoid-related orphan receptor (ror) gene family. Gene Expr. Patterns 7, 535–543 (2007).
Fallon, P. G. et al. IL-4 induces characteristic Th2 responses even in the combined absence of IL-5, IL-9, and IL-13. Immunity 17, 7–17 (2002).
Finkelman, F. D. et al. Interleukin-4- and interleukin-13-mediated host protection against intestinal nematode parasites. Immunol. Rev. 201, 139–155 (2004).
Barner, M., Mohrs, M., Brombacher, F. & Kopf, M. Differences between IL-4R α-deficient and IL-4-deficient mice reveal a role for IL-13 in the regulation of Th2 responses. Curr. Biol. 8, 669–672 (1998).
McKenzie, G. J., Bancroft, A., Grencis, R. K. & McKenzie, A. N. A distinct role for interleukin-13 in Th2-cell-mediated immune responses. Curr. Biol. 8, 339–342 (1998).
Voehringer, D., Reese, T. A., Huang, X., Shinkai, K. & Locksley, R. M. Type 2 immunity is controlled by IL-4/IL-13 expression in hematopoietic non-eosinophil cells of the innate immune system. J. Exp. Med. 203, 1435–1446 (2006).
Kang, Z. et al. Epithelial cell-specific Act1 adaptor mediates interleukin-25-dependent helminth expulsion through expansion of Lin−c-Kit+ innate cell population. Immunity 36, 821–833 (2012).
Zheng, Y. et al. Interleukin-22 mediates early host defense against attaching and effacing bacterial pathogens. Nature Med. 14, 282–289 (2008).
Zenewicz, L. A. & Flavell, R. A. Recent advances in IL-22 biology. Int. Immunol. 23, 159–163 (2011).
Vallance, B. A., Deng, W., Knodler, L. A. & Finlay, B. B. Mice lacking T and B lymphocytes develop transient colitis and crypt hyperplasia yet suffer impaired bacterial clearance during Citrobacter rodentium infection. Infect. Immun. 70, 2070–2081 (2002).
De Luca, A. et al. IL-22 defines a novel immune pathway of antifungal resistance. Mucosal Immunol. 3, 361–373 (2010).
Sonnenberg, G. F. et al. Innate lymphoid cells promote anatomical containment of lymphoid-resident commensal bacteria. Science 336, 1321–1325 (2012).
Wolterink, R. G. et al. Pulmonary innate lymphoid cells are major producers of IL-5 and IL-13 in murine models of allergic asthma. Eur. J. Immunol. 42, 1106–1116 (2012).
Halim, T. Y., Krauss, R. H., Sun, A. C. & Takei, F. Lung natural helper cells are a critical source of Th2 cell-type cytokines in protease allergen-induced airway inflammation. Immunity 36, 451–463 (2012).
Ikutani, M. et al. Identification of innate IL-5-producing cells and their role in lung eosinophil regulation and antitumor immunity. J. Immunol. 188, 703–713 (2012).
Jackson, D. J., Sykes, A., Mallia, P. & Johnston, S. L. Asthma exacerbations: origin, effect, and prevention. J. Allergy Clin. Immunol. 128, 1165–1174 (2011).
Maloy, K. J. & Powrie, F. Intestinal homeostasis and its breakdown in inflammatory bowel disease. Nature 474, 298–306 (2011).
Fuss, I. J. et al. Nonclassical CD1d-restricted NK T cells that produce IL-13 characterize an atypical Th2 response in ulcerative colitis. J. Clin. Invest. 113, 1490–1497 (2004).
Heller, F., Fuss, I. J., Nieuwenhuis, E. E., Blumberg, R. S. & Strober, W. Oxazolone colitis, a Th2 colitis model resembling ulcerative colitis, is mediated by IL-13-producing NK-T cells. Immunity 17, 629–638 (2002).
Powell, N. et al. The transcription factor T-bet regulates intestinal inflammation mediated by interleukin-7 receptor+ innate lymphoid cells. Immunity 37, 674–684 (2012).
Lochner, M. et al. Microbiota-induced tertiary lymphoid tissues aggravate inflammatory disease in the absence of RORγt and LTi cells. J. Exp. Med. 208, 125–134 (2011).
Geremia, A. et al. IL-23-responsive innate lymphoid cells are increased in inflammatory bowel disease. J. Exp. Med. 208, 1127–1133 (2011).
Takayama, T. et al. Imbalance of NKp44+NKp46− and NKp44−NKp46+ natural killer cells in the intestinal mucosa of patients with Crohn's disease. Gastroenterology 139, 882–892 (2010).
Fuss, I. J. et al. Disparate CD4+ lamina propria (LP) lymphokine secretion profiles in inflammatory bowel disease. Crohn's disease LP cells manifest increased secretion of IFN-γ, whereas ulcerative colitis LP cells manifest increased secretion of IL-5. J. Immunol. 157, 1261–1270 (1996).
Sawa, S. et al. RORγt+ innate lymphoid cells regulate intestinal homeostasis by integrating negative signals from the symbiotic microbiota. Nature Immunol. 12, 320–326 (2011).
Besnard, A. G. et al. Dual role of IL-22 in allergic airway inflammation and its cross-talk with IL-17A. Am. J. Respir. Crit. Care Med. 183, 1153–1163 (2011).
Schnyder, B., Lima, C. & Schnyder-Candrian, S. Interleukin-22 is a negative regulator of the allergic response. Cytokine 50, 220–227 (2010).
Taube, C. et al. IL-22 is produced by innate lymphoid cells and limits inflammation in allergic airway disease. PLoS ONE 6, e21799 (2011).
Takahashi, K. et al. IL-22 attenuates IL-25 production by lung epithelial cells and inhibits antigen-induced eosinophilic airway inflammation. J. Allergy Clin. Immunol. 128, 1067–1076 (2011).
Barlow, J. L., Flynn, R. J., Ballantyne, S. J. & McKenzie, A. N. Reciprocal expression of IL-25 and IL-17A is important for allergic airways hyperreactivity. Clin. Exp. Allergy 41, 1447–1455 (2011).
Wilhelm, C. et al. An IL-9 fate reporter demonstrates the induction of an innate IL-9 response in lung inflammation. Nature Immunol. 12, 1071–1077 (2011).
Huntington, N. D., Vosshenrich, C. A. & Di Santo, J. P. Developmental pathways that generate natural-killer-cell diversity in mice and humans. Nature Rev. Immunol. 7, 703–714 (2007).
Jackson, J. T. et al. Id2 expression delineates differential checkpoints in the genetic program of CD8α+ and CD103+ dendritic cell lineages. EMBO J. 30, 2690–2704 (2011).
Gascoyne, D. M. et al. The basic leucine zipper transcription factor E4BP4 is essential for natural killer cell development. Nature Immunol. 10, 1118–1124 (2009).
Kamizono, S. et al. Nfil3/E4bp4 is required for the development and maturation of NK cells in vivo. J. Exp. Med. 206, 2977–2986 (2009).
Yang, X. O. et al. T helper 17 lineage differentiation is programmed by orphan nuclear receptors ROR α and RORγ. Immunity 28, 29–39 (2008).
Samson, S. I. et al. GATA-3 promotes maturation, IFN-γ production, and liver-specific homing of NK cells. Immunity 19, 701–711 (2003).
Veldhoen, M. et al. The aryl hydrocarbon receptor links TH17-cell-mediated autoimmunity to environmental toxins. Nature 453, 106–109 (2008).
Aliahmad, P., de la Torre, B. & Kaye, J. Shared dependence on the DNA-binding factor TOX for the development of lymphoid tissue-inducer cell and NK cell lineages. Nature Immunol. 11, 945–952 (2010).
Ohno, S. et al. Runx proteins are involved in regulation of CD122, Ly49 family and IFN-γ expression during NK cell differentiation. Int. Immunol. 20, 71–79 (2008).
Tachibana, M. et al. Runx1/Cbfβ2 complexes are required for lymphoid tissue inducer cell differentiation at two developmental stages. J. Immunol. 186, 1450–1457 (2011).
Sciumé, G. et al. Distinct requirements for T-bet in gut innate lymphoid cells. J. Exp. Med. 3 Dec 2012 (doi:10.1084/jem.20122097).
Acknowledgements
The authors would like to thank S. Bell, C. Oliphant and S. Scanlon for critical appraisal of the manuscript. J.A.W. and A.N.J.M. are supported by the American Asthma Foundation.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Related links
Glossary
- Type 1 immune responses
-
Type 1 immune responses are characterized by the production of cytokines such as interferon-γ interleukin-2, tumour necrosis factor and lymphotoxin-α by various immune cells, including T helper 1 cells, neutrophils, macrophages and NK cells. Such responses protect against intracellular pathogens and are also implicated in several autoimmune diseases.
- Type 2 immune responses
-
Type 2 immune responses are characterized by the secretion of cytokines such as interleukin-4 (IL-4), IL-5, IL-9 and IL-13 by various immune cells, including T helper 2 cells, eosinophils, basophils, mast cells and ILC2s. Such responses are required for controlling extracellular parasite infections, but they are also responsible for the immunopathology that develops in patients with allergy and asthma.
- TH17 cells
-
A subset of CD4+ T helper cells that secrete predominantly the pro-inflammatory cytokine interleukin-17A and have been implicated in the pathogenesis of many chronic inflammatory disorders.
- T follicular helper cells
-
(TFH cells). A subset of CD4+ helper T cells that interact with B cells within germinal centres to provide co-stimulatory signals and regulate the development of antigen-specific B cell immune responses.
- OP9 cells
-
A bone marrow-derived stromal cell line used to support haematopoietic stem cells and common lymphoid progenitor cells during in vitro culture. The OP9–DL1 variation of this cell line ectopically expresses the Notch ligand Delta-like 1, which promotes the differentiation of T cells.
- Common lymphoid progenitor
-
(CLP). CLPs are the earliest progenitors of the lymphoid cell lineages, which include B cells, T cells, NK cells and the newly described innate lymphoid cells. Bone marrow CLPs are defined by their expression of the IL-7 receptor, FMS-related tyrosine kinase 3 (FLT3) and KIT, and the absence of all conventional lineage markers.
- Notch signalling
-
The Notch signalling pathway regulates cellular differentiation in various tissues and at various stages of development. During lymphopoiesis, signals through the Notch receptor modify gene expression patterns and have crucial roles in the development of T cells and the inhibition of B cell differentiation. In mammals, there are four Notch receptors, which bind to ligands of the Delta family (Delta-like 1, Delta-like 3 and Delta-like 4) and the jagged family (jagged 1 and jagged 2), which are typically expressed on stromal cells.
- Aryl hydrocarbon receptor
-
(AHR). AHR is a cytosolic, ligand-dependent transcription factor that translocates to the nucleus following the binding of specific ligands, which include dietary and microbial metabolites. AHR participates in the differentiation of regulatory T cells, TH17 cells and intraepithelial intestinal γδ T cells, and it is required for the secretion of IL-22 by TH17 cells. More recently, AHR has been shown to have crucial roles in the development and function of LTi cells and ILC3s.
- Forkhead box N1
-
(FOXN1). A winged-helix transcription factor that is thought to regulate keratin gene expression. Mutations in the Foxn1 gene result in a hairless ('nude') phenotype and athymia.
- REG family of C-type lectins
-
Members of the REG3 subgroup of the C-type lectin family are antimicrobial peptides that interact with the peptidoglycans present on the surface of Gram-positive bacteria. They can be released into the intestinal lumen from multiple epithelial cell lineages.
- Amphiregulin
-
A member of the epidermal growth factor family that drives the proliferation of epithelial cells and fibroblasts to promote tissue repair and remodelling in response to epithelial injury.
Rights and permissions
About this article
Cite this article
Walker, J., Barlow, J. & McKenzie, A. Innate lymphoid cells — how did we miss them?. Nat Rev Immunol 13, 75–87 (2013). https://doi.org/10.1038/nri3349
Published:
Issue Date:
DOI: https://doi.org/10.1038/nri3349
This article is cited by
-
A diversity of novel type-2 innate lymphoid cell subpopulations revealed during tumour expansion
Communications Biology (2024)
-
Phenotypic heterogeneity in psoriatic arthritis: towards tissue pathology-based therapy
Nature Reviews Rheumatology (2023)
-
Steady-state memory-phenotype conventional CD4+ T cells exacerbate autoimmune neuroinflammation in a bystander manner via the Bhlhe40/GM-CSF axis
Experimental & Molecular Medicine (2023)
-
Advances in the modulation of ROS and transdermal administration for anti-psoriatic nanotherapies
Journal of Nanobiotechnology (2022)
-
A cardioimmunologist’s toolkit: genetic tools to dissect immune cells in cardiac disease
Nature Reviews Cardiology (2022)