Key Points
-
Prodrugs are bioreversible derivatives of drug molecules that must undergo an enzymatic and/or chemical transformation in vivo to release the active parent drug, which can then exert its desired pharmacological effect.
-
The development of prodrugs is presently well established as a strategy for improving the physicochemical, biopharmaceutical or pharmacokinetic properties of pharmacologically potent compounds and thereby overcoming barriers to a drug's developability and usefulness.
-
About 5–7% of the drugs approved worldwide can be classified as prodrugs, and the implementation of a prodrug approach in the early stages of drug discovery is a growing trend.
-
Clinically, the majority of prodrugs are used with the aim of enhancing drug permeation by increasing drug lipophilicity and more recently to improve drug water solubility.
-
Site-selective drug delivery with reduced side effects, prevention of pre-systemic drug metabolism and the circumvention of efflux-limited drug absorption/distribution have not yet received enough attention in prodrug research, despite great possibilities.
-
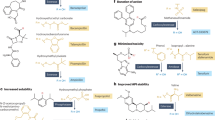
This Review provides an overview of functional groups that are amenable to prodrug design, and highlights major applications of the prodrug strategy, including improving oral absorption, improving aqueous solubility, enhancing lipophilicity, enhancing active transport as well as achieving site-selective delivery.
Abstract
Prodrugs are bioreversible derivatives of drug molecules that undergo an enzymatic and/or chemical transformation in vivo to release the active parent drug, which can then exert the desired pharmacological effect. In both drug discovery and development, prodrugs have become an established tool for improving physicochemical, biopharmaceutical or pharmacokinetic properties of pharmacologically active agents. About 5–7% of drugs approved worldwide can be classified as prodrugs, and the implementation of a prodrug approach in the early stages of drug discovery is a growing trend. To illustrate the applicability of the prodrug strategy, this article describes the most common functional groups that are amenable to prodrug design, and highlights examples of prodrugs that are either launched or are undergoing human trials.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Venkatesh, S. & Lipper, R. A. Role of the development scientist in compound lead selection and optimization. J. Pharm. Sci. 89, 145–154 (2000).
Stella, V. in Optimizing the “Drug-Like” Properties of Leads in Drug Discovery (eds Borchardt, R., Hageman, M., Stevens, J., Kerns, E. & Thakker, D.) 221–242 (Springer, New York, 2006).
Beaumont, K., Webster, R., Gardner, I. & Dack, K. Design of ester prodrugs to enhance oral absorption of poorly permeable compounds: challenges to the discovery scientist. Curr. Drug Metab. 4, 461–485 (2003). A comprehensive review on ester prodrugs for improved oral absorption.
Ettmayer, P., Amidon, G. L., Clement, B. & Testa, B. Lessons learned from marketed and investigational prodrugs. J. Med. Chem. 47, 2393–2404 (2004).
Jarvinen, T., Rautio, J., Masson, M. & Loftsson, T. in Drug Discovery Handbook (ed. Gad, S.) 733–796 (John Wiley & Sons, Hoboken, 2005).
Stella, V. J. Prodrugs as therapeutics. Expert Opin. Ther. Pat. 14, 277–280 (2004). An evaluation of prodrug patents and research through 2004.
Testa, B. Prodrug research: futile or fertile? Biochem. Pharmacol. 68, 2097–2106 (2004).
Stella, V. et al. Prodrugs: Challenges and Rewards (AAPS Press/Springer, New York, 2007). An excellent book of all aspects of prodrugs.
Stella, V. J. & Nti-Addae, K. W. Prodrug strategies to overcome poor water solubility. Adv. Drug Deliv. Rev. 59, 677–694 (2007). A recent review on water-soluble prodrugs.
Kiptoo, P. K., Hamad, M. O., Crooks, P. A. & Stinchcomb, A. L. Enhancement of transdermal delivery of 6-b-naltrexol via a codrug linked to hydroxybupropion. J. Control. Release 113, 137–145 (2006).
Leppanen, J. et al. Design and synthesis of a novel L-DOPA-entacapone codrug. J. Med. Chem. 45, 1379–1382 (2002).
Notari, R. E. Prodrug design. Pharmacol. Ther. 14, 25–53 (1981).
Sinkula, A. A. & Yalkowsky, S. H. Rationale for design of biologically reversible drug derivatives: prodrugs. J. Pharm. Sci. 64, 181–210 (1975).
Stella, V. J., Charman, W. N. & Naringrekar, V. H. Prodrugs. Do they have advantages in clinical practice? Drugs 29, 455–473 (1985).
Bodor, N. & Buchwald, P. Drug targeting via retrometabolic approaches. Pharmacol. Ther. 76, 1–27 (1997).
Bodor, N. & Buchwald, P. Soft drug design: general principles and recent applications. Med. Res. Rev. 20, 58–101 (2000).
Thorsteinsson, T., Loftsson, T. & Masson, M. Soft antibacterial agents. Curr. Med. Chem. 10, 1129–1136 (2003).
Majumdar, S. & Sloan, K. B. Synthesis, hydrolyses and dermal delivery of N-alkyl-N-alkyloxycarbonylaminomethyl (NANAOCAM) derivatives of phenol, imide and thiol containing drugs. Bioorg. Med. Chem. Lett. 16, 3590–3594 (2006).
Peyrottes, S. et al. SATE pronucleotide approaches: an overview. Mini Rev. Med. Chem. 4, 395–408 (2004).
Fozard, J. R. BP-294 Ste Civile Bioprojet. Curr. Opin. Investig. Drugs 1, 86–89 (2000).
Rouleau, A. et al. Bioavailability, antinociceptive and antiinflammatory properties of BP 2-94, a histamine H3 receptor agonist prodrug. J. Pharmacol. Exp. Ther. 281, 1085–1094 (1997).
Simplicio, A. L., Clancy, J. M. & Gilmer, J. F. β-Aminoketones as prodrugs with pH-controlled activation. Int. J. Pharm. 208–214 (2006).
Taylor, M. D. Improved passive oral drug delivery via prodrugs. Adv. Drug Deliv. Rev. 19, 131–148 (1996).
Liederer, B. M. & Borchardt, R. T. Enzymes involved in the bioconversion of ester-based prodrugs. J. Pharm. Sci. 95, 1177–1195 (2006).
Ecobichon, D. Relative amounts of hepatic and renal carboxylesterase in mammalian species. Res. Commun. Chem. Pathol. Pharmacol. 3, 629–636 (1972).
Pao, L. H., Hsiong, C. H., Hu, O. Y., Wang, J. J. & Ho, S. T. In vitro and in vivo evaluation of the metabolism and pharmacokinetics of sebacoyl dinalbuphine. Drug Metab. Dispos. 33, 395–402 (2005).
Heimbach, T. et al. Enzyme-mediated precipitation of parent drugs from their phosphate prodrugs. Int. J. Pharm. 261, 81–92 (2003).
Heimbach, T., Fleisher, D. & Kaddoumi, A. in Prodrugs: Challenges and Rewards. Part 1 (eds. Stella, V. et al.) 155–212 (AAPS Press/Springer, New York, 2007).
McComb, R., Bowers, G. & Posen, S. Alkaline Phosphatase (Plenum Press, New York and London, 1979).
Potter, P. M. & Wadkins, R. M. Carboxylesterases — detoxifying enzymes and targets for drug therapy. Curr. Med. Chem. 13, 1045–1054 (2006).
Yang, C. Y., Dantzig, A. H. & Pidgeon, C. Intestinal peptide transport systems and oral drug availability. Pharm. Res. 16, 1331–1343 (1999).
Steffansen, B. et al. Intestinal solute carriers: an overview of trends and strategies for improving oral drug absorption. Eur. J. Pharm. Sci. 21, 3–16 (2004).
Jousserandot, A. et al. Microsomal cytochrome P450 dependent oxidation of N-hydroxyguanidines, amidoximes, and ketoximes: mechanism of the oxidative cleavage of their C=N (OH) bond with formation of nitrogen oxides. Biochemistry 37, 17179–17191 (1998).
Kumpulainen, H. et al. Evaluation of hydroxyimine as cytochrome P450-selective prodrug structure. J. Med. Chem. 49, 1207–1211 (2006).
Guengerich, F. P. Common and uncommon cytochrome P450 reactions related to metabolism and chemical toxicity. Chem. Res. Toxicol. 14, 611–650 (2001).
Meunier, B., de Visser, S. P. & Shaik, S. Mechanism of oxidation reactions catalyzed by cytochrome P450 enzymes. Chem. Rev. 104, 3947–3980 (2004).
Clement, B. Reduction of N-hydroxylated compounds: amidoximes (N-hydroxyamidines) as pro-drugs of amidines. Drug Metab. Rev. 34, 565–579 (2002).
Amidon, G. L., Lennernas, H., Shah, V. P. & Crison, J. R. A theoretical basis for a biopharmaceutic drug classification: the correlation of in vitro drug product dissolution and in vivo bioavailability. Pharm. Res. 12, 413–420 (1995). An introduction to the BCS.
Aungst, B. & Matz, N. in Prodrugs: Challenges and Rewards. Part 1 (eds. Stella, V. J. et al.) 339–355 (AAPS Press/Springer, New York, 2007).
Harnden, M. R., Jarvest, R. L., Boyd, M. R., Sutton, D. & Vere Hodge, R. A. Prodrugs of the selective antiherpesvirus agent 9-[4-hydroxy-3-(hydroxymethyl)but-1-yl]guanine (BRL 39123) with improved gastrointestinal absorption properties. J. Med. Chem. 32, 1738–1743 (1989).
Nakamura, M. et al. In vitro and in vivo evaluation of the metabolism and bioavailability of ester prodrugs of MGS0039 (3-(3,4-dichlorobenzyloxy)-2-amino-6-fluorobicyclo[3.1.0]hexane-2,6-dicarb oxylic acid), a potent metabotropic glutamate receptor antagonist. Drug Metab. Dispos. 34, 369–374 (2006).
Eisenberg, E. J., He, G.-X. & Lee, W. A. Metabolism of GS-7340, a novel phenyl monophosphoramidate intracellular prodrug of PMPA, in blood. Nucleosides Nucleotides Nucleic Acids 20, 1091–1098 (2001).
Hwang, J.-T. & Choi, J.-R. Novel phosphonate nucleosides as antiviral agents. Drugs Future 29, 163–177 (2004).
Naesens, L., Balzarini, J. & De Clercq, E. Pharmacokinetics in mice of the anti-retrovirus agent 9-(2-phosphonylmethoxyethyl)adenine. Drug Metab. Dispos. 20, 747–752 (1992).
Russell, J. W., Marrero, D., Whiterock, V. J., Klunk, L. J. & Starrett, J. E. Determination of 9-[(2-phosphonylmethoxy)ethyl]adenine in rat urine by high-performance liquid chromatography with fluorescence detection. J. Chromatogr. 572, 321–326 (1991).
Starrett, J. E. Jr, Mansuri, M. M., Martin, J. C., Tortolani, D. R. & Bronson, J. J. Prodrugs of phosphonates. CA2051239 (1992).
Deconinck, E. et al. Prediction of gastro-intestinal absorption using multivariate adaptive regression splines. J. Pharm. Biomed. Anal. 39, 1021–1030 (2005).
Starrett, J. E. Jr, Tortolani, D. R., Hitchcock, M. J., Martin, J. C. & Mansuri, M. M. Synthesis and in vitro evaluation of a phosphonate prodrug: bis(pivaloyloxymethyl) 9-(2-phosphonylmethoxyethyl)adenine. Antiviral Res. 19, 267–273 (1992).
Shaw, J.-P. et al. Pharmacokinetics and metabolism of selected prodrugs of PMEA in rats. Drug Metab. Dispos. 25, 362–366 (1997).
Yasuhara, A. et al. Prodrugs of 3-(3,4-dichlorobenzyloxy)-2-amino-6-fluorobicyclo[3.1.0]hexane-2,6-dicarboxylic acid (MGS0039): a potent and orally active group II mGluR antagonist with antidepressant-like potential. Bioorg. Med. Chem. 14, 4193–4207 (2006).
van De Waterbeemd, H. & Smith, D. A. in Pharmacokinetic Optimization in Drug Research (eds Testa, B., Van De Waterbeemd, H., Folkers, G. & Guy, R.) 51–116 (Verlag Helvetica Chimica Acta and Wiley-VCH, Ochsenfurt-Hohenstad, 2001).
Lennernas, H. Intestinal drug absorption and bioavailability: beyond involvement of single transport function. J. Pharm. Pharmacol. 55, 429–433 (2003).
van De Waterbeemd, H., Smith, D. A., Beaumont, K. & Walker, D. K. Property-based design: optimization of drug absorption and pharmacokinetics. J. Med. Chem. 44, 1313–1333 (2001).
Cascorbi, I. Role of pharmacogenetics of ATP-binding cassette transporters in the pharmacokinetics of drugs. Pharmacol. Ther. 112, 457–473 (2006).
Choudhuri, S. & Klaassen, C. D. Structure, function, expression, genomic organization, and single nucleotide polymorphisms of human ABCB1 (MDR1), ABCC (MRP), and ABCG2 (BCRP) efflux transporters. Int. J. Toxicol. 25, 231–259 (2006).
Katragadda, S., Budda, B., Anand, B. S. & Mitra, A. K. Role of efflux pumps and metabolising enzymes in drug delivery. Expert Opin. Drug Deliv. 2, 683–705 (2005).
Jain, R. et al. Evasion of P-gp mediated cellular efflux and permeability enhancement of HIV-protease inhibitor saquinavir by prodrug modification. Int. J. Pharm. 303, 8–19 (2005).
Jain, R., Majumdar, S., Nashed, Y., Pal, D. & Mitra, A. K. Circumventing P-glycoprotein-mediated cellular efflux of quinidine by prodrug derivatization. Mol. Pharm. 1, 290–299 (2004).
Tanino, T. et al. Paclitaxel-2′-ethylcarbonate prodrug can circumvent P-glycoprotein-mediated cellular efflux to increase drug cytotoxicity. Pharm. Res. 24, 555–565 (2007).
Lipinski, C. Poor solubility — an industry wide problem in drug discovery. Am. Pharm. Rev. 5, 82–85 (2002).
Lipinski, C. in Biotechnology: Pharmaceutical Aspects (Pharmaceutical Profiling in Drug Discovery for Lead Selection) (eds Borchardt, R. T. et al.) 93–125 (AAPS, Virgina, 2004).
Duggan, D. E., Hare, L. E., Ditzler, C. A., Lei, B. W. & Kwan, K. C. The disposition of sulindac. Clin. Pharmacol. Ther. 21, 326–335 (1977).
Duggan, D. E., Hooke, K. F., Noll, R. M., Hucker, H. B. & Van Arman, C. G. Comparative disposition of sulindac and metabolites in five species. Biochem. Pharmacol. 27, 2311–2320 (1978).
Shen, T. & Winter, C. Chemical and biological studies on indomethacin, sulindac and their analogs. Adv. Drug Res. 12, 90–295 (1977).
Davies, N. M. & Watson, M. S. Clinical pharmacokinetics of sulindac. A dynamic old drug. Clin. Pharmacokinet. 32, 437–459 (1997).
Masuda, H., Ikeda, K., Nagamachi, N., Nagayama, S. & Kawaguchi, Y. Metabolic fate of TAT-59. (4th report): species difference, dose response and protein binding. Yakuri to Chiryo 26, 809–828 (1998) (in Japanese).
Gunnarsson, P. O., Andersson, S. B., Johansson, S. A., Nilsson, T. & Plym-Forshell, G. Pharmacokinetics of estramustine phosphate (Estracyt) in prostatic cancer patients. Eur. J. Clin. Pharmacol. 26, 113–119 (1984).
Heimbach, T. et al. Absorption rate limit considerations for oral phosphate prodrugs. Pharm. Res. 20, 848–856 (2003). A guidance for parent-drug selection when employing the phosphate prodrug approach for oral delivery.
Nomura, Y. et al. Phase I study of TAT-59 (a new antiestrogen) in breast cancer. Gan To Kagaku Ryoho 25, 553–561 (1998) (in Japanese).
Wire, M. B., Shelton, M. J. & Studenberg, S. Fosamprenavir: clinical pharmacokinetics and drug interactions of the amprenavir prodrug. Clin. Pharmacokinet. 45, 137–168 (2006).
Chapman, T. M., Plosker, G. L. & Perry, C. M. Fosamprenavir: a review of its use in the management of antiretroviral therapy-naive patients with HIV infection. Drugs 64, 2101–2124 (2004).
Furfine, E. S. et al. Preclinical pharmacology and pharmacokinetics of GW433908, a water-soluble prodrug of the human immunodeficiency virus protease inhibitor amprenavir. Antimicrob. Agents Chemother. 48, 791–798 (2004).
Stella, V. J. in Prodrugs: Challenges and Rewards. Part 1 (eds Stella, V. J. et al.) 3–33 (AAPS Press/Springer, New York, 2007).
Shaw, J. P. et al. Metabolism and pharmacokinetics of novel oral prodrugs of 9-[(R)-2-(phosphonomethoxy)propyl]adenine (PMPA) in dogs. Pharm. Res. 14, 1824–1829 (1997).
Fardis, M. & Oliyai, R. in Prodrugs: Challenges and Rewards. Part 2 (eds Stella, V. J. et al.) 647–657 (AAPS Press/Springer, New York, 2007).
Gallant, J. E. & Deresinski, S. Tenofovir disoproxil fumarate. Clin. Infect. Dis. 37, 944–950 (2003).
Chapman, T., McGavin, J. & Noble, S. Tenofovir disoproxil fumarate. Drugs 63, 1597–1608 (2003).
Dando, T. & Plosker, G. Adefovir dipivoxil: a review of its use in chronic hepatitis B. Drugs 63, 2215–2234 (2003).
Noble, S. & Goa, K. L. Adefovir dipivoxil. Drugs 58, 479–487 (1999).
Bardsley-Elliot, A. & Noble, S. Oseltamivir. Drugs 58, 851–860 (1999).
Doucette, K. E. & Aoki, F. Y. Oseltamivir: a clinical and pharmacological perspective. Expert Opin. Pharmacother. 2, 1671–1683 (2001).
McClellan, K. & Perry, C. M. Oseltamivir: a review of its use in influenza. Drugs 61, 263–283 (2001).
Shi, D. et al. Anti-influenza prodrug oseltamivir is activated by carboxylesterase human carboxylesterase 1, and the activation is inhibited by antiplatelet agent clopidogrel. J. Pharmacol. Exp. Ther. 319, 1477–1484 (2006).
Eriksson, U. G. et al. Absorption, distribution, metabolism, and excretion of ximelagatran, an oral direct thrombin inhibitor, in rats, dogs, and humans. Drug Metab. Dispos. 31, 294–305 (2003).
Clement, B. & Lopian, K. Characterization of in vitro biotransformation of new, orally active, direct thrombin inhibitor ximelagatran, an amidoxime and ester prodrug. Drug Metab. Dispos. 31, 645–651 (2003).
Gustafsson, D. et al. The direct thrombin inhibitor melagatran and its oral prodrug H 376/95: intestinal absorption properties, biochemical and pharmacodynamic effects. Thromb. Res. 101, 171–181 (2001).
Frantz, S. Pharma faces major challenges after a year of failures and heated battles. Nature Rev. Drug Discov. 6, 5–7 (2007).
Han, H. K. & Amidon, G. L. Targeted prodrug design to optimize drug delivery. AAPS PharmSci 2, e6 (2000).
Yang, C., Tirucherai, G. S. & Mitra, A. K. Prodrug based optimal drug delivery via membrane transporter/receptor. Expert Opin. Biol. Ther. 1, 159–175 (2001).
Balimane, P. V. et al. Direct evidence for peptide transporter (PepT1)-mediated uptake of a nonpeptide prodrug, valacyclovir. Biochem. Biophys. Res. Commun. 250, 246–251 (1998).
de Vrueh, R. L., Smith, P. L. & Lee, C. P. Transport of L-valine-acyclovir via the oligopeptide transporter in the human intestinal cell line, Caco-2. J. Pharmacol. Exp. Ther. 286, 1166–1170 (1998).
Guo, A., Hu, P., Balimane, P. V., Leibach, F. H. & Sinko, P. J. Interactions of a nonpeptidic drug, valacyclovir, with the human intestinal peptide transporter (hPEPT1) expressed in a mammalian cell line. J. Pharmacol. Exp. Ther. 289, 448–454 (1999).
Sugawara, M. et al. Transport of valganciclovir, a ganciclovir prodrug, via peptide transporters PEPT1 and PEPT2. J. Pharm. Sci. 89, 781–789 (2000).
Tsuda, M. et al. Transport characteristics of a novel peptide transporter 1 substrate, antihypotensive drug midodrine, and its amino acid derivatives. J. Pharmacol. Exp. Ther. 318, 455–460 (2006).
Han, H. et al. 5′-Amino acid esters of antiviral nucleosides, acyclovir, and AZT are absorbed by the intestinal PEPT1 peptide transporter. Pharm. Res. 15, 1154–1159 (1998).
Kim, I. et al. Identification of a human valacyclovirase: biphenyl hydrolase-like protein as valacyclovir hydrolase. J. Biol. Chem. 278, 25348–25356 (2003).
Cruz, D. N. Midodrine: a selective α-adrenergic agonist for orthostatic hypotension and dialysis hypotension. Expert Opin. Pharmacother. 1, 835–840 (2000).
Cundy, K. C. et al. XP13512 [(+/-)-1-([(α-isobutanoyloxyethoxy)carbonyl] aminomethyl)-1-cyclohexane acetic acid], a novel gabapentin prodrug: II. Improved oral bioavailability, dose proportionality, and colonic absorption compared with gabapentin in rats and monkeys. J. Pharmacol. Exp. Ther. 311, 324–333 (2004).
Cundy, K. C. et al. XP13512 [(+/-)-1-([(α-isobutanoyloxyethoxy)carbonyl] aminomethyl)-1-cyclohexane acetic acid], a novel gabapentin prodrug: I. Design, synthesis, enzymatic conversion to gabapentin, and transport by intestinal solute transporters. J. Pharmacol. Exp. Ther. 311, 315–323 (2004).
Boucher, B. A. Fosphenytoin: a novel phenytoin prodrug. Pharmacotherapy 16, 777–791 (1996).
Browne, T. R., Kugler, A. R. & Eldon, M. A. Pharmacology and pharmacokinetics of fosphenytoin. Neurology 46, S3–S7 (1996).
Varia, S. A., Schuller, S., Sloan, K. B. & Stella, V. J. Phenytoin prodrugs III: water-soluble prodrugs for oral and/or parenteral use. J. Pharm. Sci. 73, 1068–1073 (1984).
Heck, H. D., Casanova, M. & Starr, T. B. Formaldehyde toxicity — new understanding. Crit. Rev. Toxicol. 20, 397–426 (1990).
Bentley, A. et al. The discovery and process. Development of a commercial route to the water soluble prodrug, Fosfluconazole. Org. Proc. Res. Develop. 6, 109–112 (2002).
Sobue, S., Sekiguchi, K., Shimatani, K. & Tan, K. Pharmacokinetics and safety of Fosfluconazole after single intravenous bolus injection in healthy male Japanese volunteers. J. Clin. Pharmacol. 44, 284–292 (2004).
Schywalsky, M. et al. Pharmacokinetics and pharmacodynamics of the new propofol prodrug GPI 15715 in rats. Eur. J. Anaesthesiol. 20, 182–190 (2003).
Banaszczyk, M. G. et al. Propofol phosphate, a water-soluble propofol prodrug: in vivo evaluation. Anesth. Analg. 95, 1285–1292 (2002).
Safadi, M., Oliyai, R. & Stella, V. J. Phosphoryloxymethyl carbamates and carbonates — novel water-soluble prodrugs for amines and hindered alcohols. Pharm. Res. 10, 1350–1355 (1993).
Bencharit, S. et al. Structural insights into CPT-11 activation by mammalian carboxylesterases. Nature Struct. Biol. 9, 337–342 (2002).
Sanghani, S. P. et al. Hydrolysis of irinotecan and its oxidative metabolites, 7-ethyl-10-[4-N-(5-aminopentanoic acid)-1-piperidino] carbonyloxycamptothecin and 7-ethyl-10-[4-(1-piperidino)-1-amino]-carbonyloxycamptothecin, by human carboxylesterases CES1A1, CES2, and a newly expressed carboxylesterase isoenzyme, CES3. Drug Metab. Dispos. 32, 505–511 (2004).
Slatter, J. G., Su, P., Sams, J. P., Schaaf, L. J. & Wienkers, L. C. Bioactivation of the anticancer agent CPT-11 to SN-38 by human hepatic microsomal carboxylesterases and the in vitro assessment of potential drug interactions. Drug Metab. Dispos. 25, 1157–1164 (1997).
Rothenberg, M. L. Irinotecan (CPT-11): recent developments and future directions — colorectal cancer and beyond. Oncologist 6, 66–80 (2001).
Guichard, S. et al. CPT-11 converting carboxylesterase and topoisomerase activities in tumour and normal colon and liver tissues. Br. J. Cancer 80, 364–370 (1999).
Slatter, J. G. et al. Pharmacokinetics, metabolism, and excretion of irinotecan (CPT-11) following I.V. infusion of [(14)C]CPT-11 in cancer patients. Drug Metab. Dispos. 28, 423–433 (2000).
Hageman, M. & Morozowich, W. in Prodrugs: Challenges and Rewards. Part 2 (eds Stella, V. J., Hageman, M., Oliyai, R., Tilley, J. & Maag, H.) 571–579 (AAPS Press/Springer, Arlington, Virginia, 2007).
Järvinen, T. & Järvinen, K. Prodrugs for improved ocular drug delivery. Adv. Drug Deliv. Rev. 19, 203–224 (1996).
Hussain, A. & Truelove, J. E. Prodrug approaches to enhancement of physicochemical properties of drugs IV: novel epinephrine prodrug. J. Pharm. Sci. 65, 1510–1512 (1976).
Anderson, J. A. Systemic absorption of topical ocularly applied epinephrine and dipivefrin. Arch. Ophthalmol. 98, 350–353 (1980).
Mandell, A. I., Stentz, F. & Kitabchi, A. E. Dipivalyl epinephrine: a new pro-drug in the treatment of glaucoma. Ophthalmology 85, 268–275 (1978).
Wei, C. P., Anderson, J. A. & Leopold, I. Ocular absorption and metabolism of topically applied epinephrine and a dipivalyl ester of epinephrine. Invest. Ophthalmol. Vis. Sci. 17, 315–321 (1978).
Kaback, M. B., Podos, S. M., Harbin, T. S. Jr, Mandell, A. & Becker, B. The effects of dipivalyl epinephrine on the eye. Am. J. Ophthalmol. 81, 768–772 (1976).
Kohn, A. N. et al. Clinical comparison of dipivalyl epinephrine and epinephrine in the treatment of glaucoma. Am. J. Ophthalmol. 87, 196–201 (1979).
Hellberg, M. R. et al. The hydrolysis of the prostaglandin analog prodrug bimatoprost to 17-phenyl-trinor PGF2α by human and rabbit ocular tissue. J. Ocul. Pharmacol. Ther. 19, 97–103 (2003).
Netland, P. A. et al. Travoprost compared with latanoprost and timolol in patients with open-angle glaucoma or ocular hypertension. Am. J. Ophthalmol. 132, 472–484 (2001).
Sharif, N. A., Kelly, C. R., Crider, J. Y., Williams, G. W. & Xu, S. X. Ocular hypotensive FP prostaglandin (PG) analogs: PG receptor subtype binding affinities and selectivities, and agonist potencies at FP and other PG receptors in cultured cells. J. Ocul. Pharmacol. Ther. 19, 501–515 (2003).
Susanna, R., Jr., Chew, P. & Kitazawa, Y. Current status of prostaglandin therapy: latanoprost and unoprostone. Surv. Ophthalmol. 47 (Suppl. 1), 97–104 (2002).
Sloan, K. B. & Wasdo, S. Designing for topical delivery: prodrugs can make the difference. Med. Res. Rev. 23, 763–793 (2003).
Sloan, K. B., Wasdo, S. C. & Rautio, J. Design for optimized topical delivery: Prodrugs and a paradigm change. Pharm. Res. 23, 2729–2747 (2006). Offers useful directives for the design of drugs or prodrugs for optimized topical delivery.
Rautio, J. et al. Piperazinylalkyl prodrugs of naproxen improve in vitro skin permeation. Eur. J. Pharm. Sci. 11, 157–163 (2000).
Rautio, J. et al. Synthesis and in vitro evaluation of novel morpholinyl- and methylpiperazinylacyloxyalkyl prodrugs of 2-(6-methoxy-2-naphthyl)propionic acid (Naproxen) for topical drug delivery. J. Med. Chem. 43, 1489–1494 (2000).
Chandraratna, R. A. Tazarotene — first of a new generation of receptor-selective retinoids. Br. J. Dermatol. 135 (Suppl. 49), 18–25 (1996).
Dando, T. M. & Wellington, K. Topical tazarotene: a review of its use in the treatment of plaque psoriasis. Am. J. Clin. Dermatol. 6, 255–272 (2005).
Foster, R. H., Brogden, R. N. & Benfield, P. Tazarotene. Drugs 55, 705–711 (1998).
Marks, R. Clinical safety of tazarotene in the treatment of plaque psoriasis. J. Am. Acad. Dermatol. 37, S25–S32 (1997).
Tang-Liu, D. D., Matsumoto, R. M. & Usansky, J. I. Clinical pharmacokinetics and drug metabolism of tazarotene: a novel topical treatment for acne and psoriasis. Clin. Pharmacokinet. 37, 273–287 (1999).
Nutt, J. G. & Woodward, W. R. Levodopa pharmacokinetics and pharmacodynamics in fluctuating parkinsonian patients. Neurology 36, 739–744 (1986).
Nutt, J. G., Woodward, W. R., Hammerstad, J. P., Carter, J. H. & Anderson, J. L. The "on-off" phenomenon in Parkinson's disease. Relation to levodopa absorption and transport. N. Engl. J. Med. 310, 483–488 (1984).
Anderson, B. D. Prodrugs for improved CNS delivery. Adv. Drug Deliv. Rev. 19, 171–202 (1996).
Damen, E. W., Groot, F. M. & Scheeren, H. W. Novel anthracyclin prodrugs. Exp. Opin. Ther. Pat. 11, 651–666 (2001).
de Groot, F. M., Damen, E. W. & Scheeren, H. W. Anticancer prodrugs for application in monotherapy: targeting hypoxia, tumor-associated enzymes, and receptors. Curr. Med. Chem. 8, 1093–1122 (2001).
Shinhababu, A. & Thakker, D. Prodrug of anticancer agents. Adv. Drug Deliv. Rev. 19, 241–273 (1996).
Quinney, S. K. et al. Hydrolysis of capecitabine to 5′-deoxy-5-fluorocytidine by human carboxylesterases and inhibition by loperamide. J. Pharmacol. Exp. Ther. 313, 1011–1016 (2005).
Walko, C. M. & Lindley, C. Capecitabine: a review. Clin. Ther. 27, 23–44 (2005).
Miwa, M. et al. Design of a novel oral fluoropyrimidine carbamate, capecitabine, which generates 5-fluorouracil selectively in tumours by enzymes concentrated in human liver and cancer tissue. Eur. J. Cancer 34, 1274–1281 (1998).
Venturini, M. Rational development of capecitabine. Eur. J. Cancer 38 (Suppl. 2), 3–9 (2002).
Bagshawe, K. D., Sharma, S. K. & Begent, R. H. Antibody-directed enzyme prodrug therapy (ADEPT) for cancer. Expert Opin. Biol. Ther. 4, 1777–1789 (2004).
Sharma, S. K., Bagshawe, K. D. & Begent, R. H. Advances in antibody-directed enzyme prodrug therapy. Curr. Opin. Investig. Drugs 6, 611–615 (2005). This review summarizes the recent progress of ADEPT for cancer treatment.
Niculescu-Duvaz, I., Spooner, R., Marais, R. & Springer, C. J. Gene-directed enzyme prodrug therapy. Bioconjug. Chem. 9, 4–22 (1998).
Dachs, G. U., Tupper, J. & Tozer, G. M. From bench to bedside for gene-directed enzyme prodrug therapy of cancer. Anticancer Drugs 16, 349–359 (2005). This review describes seven of the most utilized GDEPT systems in vitro and in vivo.
Chester, K. et al. Engineering antibodies for clinical applications in cancer. Tumour Biol. 25, 91–98 (2004).
Francis, R. J. et al. A phase I trial of antibody directed enzyme prodrug therapy (ADEPT) in patients with advanced colorectal carcinoma or other CEA producing tumours. Br. J. Cancer 87, 600–607 (2002).
Napier, M. P. et al. Antibody-directed enzyme prodrug therapy: efficacy and mechanism of action in colorectal carcinoma. Clin. Cancer Res. 6, 765–772 (2000).
van Montfoort, J. E. et al. Drug uptake systems in liver and kidney. Curr. Drug Metab. 4, 185–211 (2003).
Erion, M. D., Bullough, D. A., Lin, C. C. & Hong, Z. HepDirect prodrugs for targeting nucleotide-based antiviral drugs to the liver. Curr. Opin. Investig. Drugs 7, 109–117 (2006).
Erion, M. D. et al. Design, synthesis, and characterization of a series of cytochrome P(450) 3A-activated prodrugs (HepDirect prodrugs) useful for targeting phosph(on)ate-based drugs to the liver. J. Am. Chem. Soc. 126, 5154–5163 (2004).
Mauro, V. F. Clinical pharmacokinetics and practical applications of simvastatin. Clin. Pharmacokinet. 24, 195–202 (1993).
Shitara, Y. & Sugiyama, Y. Pharmacokinetic and pharmacodynamic alterations of 3-hydroxy-3-methylglutaryl coenzyme A (HMG-CoA) reductase inhibitors: drug-drug interactions and interindividual differences in transporter and metabolic enzyme functions. Pharmacol. Ther. 112, 71–105 (2006).
Sirtori, C. R. Tissue selectivity of hydroxymethylglutaryl coenzyme A (HMG CoA) reductase inhibitors. Pharmacol. Ther. 60, 431–459 (1993).
Neuvonen, P. J., Niemi, M. & Backman, J. T. Drug interactions with lipid-lowering drugs: mechanisms and clinical relevance. Clin. Pharmacol. Ther. 80, 565–581 (2006).
Altamura, A. C. et al. Intramuscular preparations of antipsychotics: uses and relevance in clinical practice. Drugs 63, 493–512 (2003).
Minto, C. F., Howe, C., Wishart, S., Conway, A. J. & Handelsman, D. J. Pharmacokinetics and pharmacodynamics of nandrolone esters in oil vehicle: effects of ester, injection site and injection volume. J. Pharmacol. Exp. Ther. 281, 93–102 (1997).
Marder, S. R. et al. Fluphenazine plasma level monitoring for patients receiving fluphenazine decanoate. Schizophr. Res. 53, 25–30 (2002).
Svensson, L. & Tunek, A. The design and bioactivation of presystemically stable prodrugs. Drug Metab. Rev. 19, 165–194 (1988).
Tunek, A., Levin, E. & Svensson, L. Hydrolysis of 3H-bambuterol, a carbamate prodrug of terbutaline, in blood from humans and laboratory animals in vitro. Biochem. Pharmacol. 37, 3867–3876 (1988).
Persson, G., Pahlm, O. & Gnosspelius, Y. Oral bambuterol versus terbutaline in patients with asthma. Curr. Therap. Res. 56, 457–465 (1995).
Grossman, S. in Prodrugs: Challenges and Rewards. Part 2 (eds. Stella, V. J. et al.) 411–424 (AAPS/Springer, New York, 2007).
Brass, E. P. Pivalate-generating prodrugs and carnitine homeostasis in man. Pharmacol. Rev. 54, 589–598 (2002).
Kwan, K. C. Oral bioavailability and first-pass effects. Drug Metab. Dispos. 25, 1329–1336 (1997).
Thomas, V. H. et al. The road map to oral bioavailability: an industrial perspective. Expert Opin. Drug Metab. Toxicol. 2, 591–608 (2006).
Kwon, Y. Handbook of Essential Pharmacokinetics, Pharmacokinetics, and Drug Metabolism for Industrial Scientists (Springer-Verlag, New York, 2001).
Boxenbaum, H. Interspecies variation in liver weight, hepatic blood flow, and antipyrine intrinsic clearance: extrapolation of data to benzodiazepines and phenytoin. J. Pharmacokinet. Biopharm. 8, 165–176 (1980).
Todd, P. A. & Heel, R. C. Enalapril. A review of its pharmacodynamic and pharmacokinetic properties, and therapeutic use in hypertension and congestive heart failure. Drugs 31, 198–248 (1986).
Ehrnebo, M., Nilsson, S. O. & Boreus, L. O. Pharmacokinetics of ampicillin and its prodrugs bacampicillin and pivampicillin in man. J. Pharmacokinet. Biopharm. 7, 429–451 (1979).
Jusko, W. J. & Lewis, G. P. Comparison of ampicillin and hetacillin pharmacokinetics in man. J. Pharm. Sci. 62, 69–76 (1973).
Hodge, R. A. V., Sutton, D., Boyd, M. R., Harnden, M. R. & Jarvest, R. L. Selection of an oral prodrug (BRL 42810; famciclovir) for the antiherpesvirus agent BRL 39123 [9-(4-hydroxy-3-hydroxymethylbut-1-yl)guanine; penciclovir]. Antimicrob. Agents Chemother. 33, 1765–1773 (1989).
Simpson, D. & Lyseng-Williamson, K. A. Famciclovir: a review of its use in herpes zoster and genital and orolabial herpes. Drugs 66, 2397–2416 (2006).
Gudmundsson, O. S. & Antman, M. in Prodrugs: Challenges and Rewards. Part 2 (eds Stella, V. J. et al.) 531–539 (AAPS Press/Springer, New York, 2007).
Bergenheim, A. T. & Henriksson, R. Pharmacokinetics and pharmacodynamics of estramustine phosphate. Clin. Pharmacokinet. 34, 163–172 (1998).
Perry, C. M. & McTavish, D. Estramustine phosphate sodium. A review of its pharmacodynamic and pharmacokinetic properties, and therapeutic efficacy in prostate cancer. Drugs Aging 7, 49–74 (1995).
Sousa, F. The bioavailability and therapeutic effectiveness of prednisolone acetate vs. prednisolone sodium phosphate: a 20-year review. CLAO J. 17, 282–284 (1991).
Boogaerts, M. A. et al. Activity of oral fludarabine phosphate in previously treated chronic lymphocytic leukemia. J. Clin. Oncol. 19, 4252–4258 (2001).
Perry, C. M. & Faulds, D. Valaciclovir. A review of its antiviral activity, pharmacokinetic properties and therapeutic efficacy in herpesvirus infections. Drugs 52, 754–772 (1996).
Cocohoba, J. M. & McNicholl, I. R. Valganciclovir: an advance in cytomegalovirus therapeutics. Ann. Pharmacother. 36, 1075–1079 (2002).
Reusser, P. Oral valganciclovir: a new option for treatment of cytomegalovirus infection and disease in immunocompromised hosts. Expert Opin. Investig. Drugs 10, 1745–1753 (2001).
Stella, V. J., Zygmunt, J. J, Georg, I. G. & Muhammed, S. Water soluble prodrugs of hindered alcohols or phenols. US19980131385 (2005).
Jarvinen, T. & Niemi, R. in Prodrugs: Challenges and Rewards. Part 1 (eds Stella, V. J. et al.) 125–155 (AAPS Press/Springer, New York, 2007).
Erion, M. D. et al. Liver-targeted drug delivery using HepDirect prodrugs. J. Pharmacol. Exp. Ther. 312, 554–560 (2005).
Mauro, V. F. & MacDonald, J. L. Simvastatin: a review of its pharmacology and clinical use. Ann. Pharmacother. 25, 257–264 (1991).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Related links
Glossary
- Combinatorial chemistry
-
The rapid synthesis or the computer simulation of a large number of different but structurally related molecules.
- Promoiety
-
A functional group used to modify the structure of pharmacologically active agents to improve physicochemical, biopharmaceutical or pharmacokinetic properties.
- Co-drug
-
A chemical structure that undergoes conversion to two or more active drugs within a biological system, such conversion usually involves the metabolism of the co-drug.
- Bioprecursor prodrug
-
A prodrug that does not contain a carrier or promoiety, but is metabolically or chemically transformed into an active drug.
- Soft drug
-
Soft drugs are the opposite of prodrugs. They are active drugs that are designed to undergo a predictable and controllable deactivation or metabolism in vivo after achieving their therapeutic effect.
- Bioconversion
-
A process in which the pharmacologically active drug is released or formed.
Rights and permissions
About this article
Cite this article
Rautio, J., Kumpulainen, H., Heimbach, T. et al. Prodrugs: design and clinical applications. Nat Rev Drug Discov 7, 255–270 (2008). https://doi.org/10.1038/nrd2468
Issue Date:
DOI: https://doi.org/10.1038/nrd2468
This article is cited by
-
Exploring the next generation of antibody–drug conjugates
Nature Reviews Clinical Oncology (2024)
-
Cholesterol-modified sphingomyelin chimeric lipid bilayer for improved therapeutic delivery
Nature Communications (2024)
-
Conversion of Olmesartan to Olmesartan Medoxomil, A Prodrug that Improves Intestinal Absorption, Confers Substrate Recognition by OATP2B1
Pharmaceutical Research (2024)
-
Self-assembled lipid–prodrug nanoparticles
Nature Reviews Bioengineering (2023)
-
Direct nucleophilic and electrophilic activation of alcohols using a unified boron-based organocatalyst scaffold
Nature Communications (2023)