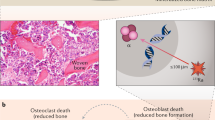
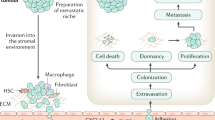
Abstract
Metastatic bone disease (MBD) in advanced-stage cancer increases the risk of intractable bone pain, pathological skeletal fracture, spinal-cord compression and decreased survival. The disease manifestation course during MBD is largely driven by homotypic and heterotypic cellular interactions between invading tumor cells, osteoblasts and osteoclasts. The outcome is a sustained vicious cycle of bone matrix remodeling. Osteoclast-mediated bone degradation and subsequent bone loss are the hallmarks of secondary bone metastases from most solid tumors. An additional complication in prostate cancer is the predominance of osteosclerotic lesions typified by inappropriate bone production. Successful therapeutic strategies for the treatment of osteolytic MBD include the administration of intravenous bisphosphonates or subcutaneous inhibitors of receptor activator of nuclear factor κB ligand (RANKL). Inhibitors of SRC and cABL kinases and cathepsin K are under clinical investigation as potential anti-osteolytics. In contrast to the rapid progress being made in the development of anti-osteolytic therapies, the treatment of osteosclerotic MBD remains restricted to palliative radiotherapy for symptomatic solitary lesions and systemic taxane-based chemotherapy for widespread multiple lesions. This Review discusses the complex pathology of bone lesions in metastatic castration-resistant prostate cancer and focuses on new therapeutic strategies and targets that are emerging in preclinical studies.
Key Points
-
Treatment of metastatic bone disease (MBD) in men with castration-resistant prostate cancer (CRPC) is complicated by osteolytic (bone-degrading), osteosclerotic (bone-forming) and mixed osteolytic and osteosclerotic lesions
-
It is essential to study the complex interactions between tumor cells, osteoblasts and osteoclasts in the bone metastatic niche using clinically relevant models to allow development of targeted treatments
-
Bisphosphonates are used as a palliative treatment to protect against the osteolytic effects of MBD; to date, clodronate has been shown to improve survival of CRPC patients with MBD
-
Denosumab, the RANKL inhibitor, has been approved for the treatment of MBD that originate from solid tumors; however, its efficacy in MBD associated with CRPC is unclear
-
Inhibition of Endothelin A receptor and systemic radionuclide therapy target osteoblast activity and are under investigation for their clinical impact in CRPC
-
Improved understanding of the molecular mechanisms of dysregulated type-I collagen deposition in MBD will open up new avenues for therapeutic exploitation
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Change history
05 August 2011
In the version of this article initially published online the title of Table 1 should have read "Completed and ongoing trials with bisphosphonates" and it should have stated that trial NCT00330759 excluded patients with prostate cancer. In Table 2, it should have been defined that patients enrolled in trial NCT00089674 did not present with any type of metastases and that the secondary end point was fractures. It should have also stated that trial NCT00321620 assessed denosumab versus zoledronic acid. The errors have been corrected for the HTML and PDF versions of the article.
References
Mundy, G. R. Metastasis to bone: causes, consequences and therapeutic opportunities. Nat. Rev. Cancer 2, 584–593 (2002).
Eisenberger, M. A. & Walsh, P. C. Early androgen deprivation for prostate cancer? N. Engl. J. Med. 341, 1837–1838 (1999).
Smith, M. R., Brown, G. A., Saad, F. New opportunities in the management of prostate cancer-related bone complications. Urologic Oncology: Seminars and Original Investigations 27 (Suppl. 1) S1–S20 (2009).
Janjan, N. et al. Therapeutic guidelines for the treatment of bone metastasis: a report from the American College of Radiology Appropriateness Criteria Expert Panel on Radiation Oncology. J. Palliat. Med. 12, 417–426 (2009).
Tannock, I. F. et al. Docetaxel plus prednisone or mitoxantrone plus prednisone for advanced prostate cancer. N. Engl. J. Med. 351, 1502–1512 (2004).
Berthold, D. R. et al. Docetaxel plus prednisone or mitoxantrone plus prednisone for advanced prostate cancer: updated survival in the TAX 327 study. J. Clin. Oncol. 26, 242–245 (2008).
Petrylak, D. P. et al. Docetaxel and estramustine compared with mitoxantrone and prednisone for advanced refractory prostate cancer. N. Engl. J. Med. 351, 1513–1520 (2004).
Seruga, B., Ocana, A. & Tannock, I. F. Drug resistance in metastatic castration-resistant prostate cancer. Nat. Rev. Clin. Oncol. 8, 12–23 (2011).
Zaidi, M. Skeletal remodeling in health and disease. Nat. Med. 13, 791–801 (2007).
Ory, S., Brazier, H., Pawlak, G. & Blangy, A. Rho GTPases in osteoclasts: orchestrators of podosome arrangement. Eur. J. Cell Biol. 87, 469–477 (2008).
Heckel, T. et al. Src-dependent repression of ARF6 is required to maintain podosome-rich sealing zones in bone-digesting osteoclasts. Proc. Natl Acad. Sci. USA 106, 1451–1456 (2009).
Garnero, P. et al. The collagenolytic activity of cathepsin K is unique among mammalian proteinases. J. Biol. Chem. 273, 32347–32352 (1998).
Coxon, F. P. & Taylor, A. Vesicular trafficking in osteoclasts. Semin. Cell Dev. Biol. 19, 424–433 (2008).
Leblond, C. P. Synthesis and secretion of collagen by cells of connective tissue, bone, and dentin. Anat. Rec. 224, 123–138 (1989).
Rohde, M. & Mayer, H. Exocytotic process as a novel model for mineralization by osteoblasts in vitro and in vivo determined by electron microscopic analysis. Calcif. Tissue Int. 80, 323–336 (2007).
Lacey, D. L. et al. Osteoprotegerin ligand is a cytokine that regulates osteoclast differentiation and activation. Cell 93, 165–176 (1998).
Boyle, W. J., Simonet, W. S. & Lacey, D. L. Osteoclast differentiation and activation. Nature 423, 337–342 (2003).
Honore, P. et al. Osteoprotegerin blocks bone cancer-induced skeletal destruction, skeletal pain and pain-related neurochemical reorganization of the spinal cord. Nat. Med. 6, 521–528 (2000).
Clines, G. A. & Guise, T. A. Molecular mechanisms and treatment of bone metastasis. Expert Rev. Mol. Med. 10, e7 (2008).
Rose, A. A. & Siegel, P. M. Breast cancer-derived factors facilitate osteolytic bone metastasis. Bull. Cancer 93, 931–943 (2006).
Cereceda, L. E., Flechon, A. & Droz, J. P. Management of vertebral metastases in prostate cancer: a retrospective analysis in 119 patients. Clin. Prostate Cancer 2, 34–40 (2003).
Cheville, J. C. et al. Metastatic prostate carcinoma to bone: clinical and pathologic features associated with cancer-specific survival. Cancer 95, 1028–1036 (2002).
Brown, J. E. et al. Bone turnover markers as predictors of skeletal complications in prostate cancer, lung cancer, and other solid tumors. J. Natl Cancer Inst. 97, 59–69 (2005).
Coleman, R. E. et al. Predictive value of bone resorption and formation markers in cancer patients with bone metastases receiving the bisphosphonate zoledronic acid. J. Clin. Oncol. 23, 4925–4935 (2005).
Atley, L. M., Mort, J. S., Lalumiere, M. & Eyre, D. R. Proteolysis of human bone collagen by cathepsin K: characterization of the cleavage sites generating by cross-linked N.-telopeptide neoepitope. Bone 26, 241–247 (2000).
Brown, J. E. & Sim, S. Evolving role of bone biomarkers in castration-resistant prostate cancer. Neoplasia 12, 685–696 (2010).
Saad, F. & Sternberg, C. N. Multidisciplinary management of bone complications in prostate cancer and optimizing outcomes of bisphosphonate therapy. Nat. Clin. Pract. Urol. 4, S3–S13 (2007).
Drake, M. T., Clarke, B. L. & Khosla, S. Bisphosphonates: mechanism of action and role in clinical practice. Mayo Clin. Proc. 83, 1032–1045 (2008).
Bellido, T. & Plotkin, L. I. Novel actions of bisphosphonates in bone: Preservation of osteoblast and osteocyte viability. Bone, doi:10.1016/j.bone.2010.08.008 (2010).
Roelofs, A. J., Thompson, K., Gordon, S. & Rogers, M. J. Molecular mechanisms of action of bisphosphonates: current status. Clin. Cancer Res. 12, 6222s–6230s (2006).
Roelofs, A. J., Thompson, K., Ebetino, F. H., Rogers, M. J. & Coxon, F. P. Bisphosphonates: molecular mechanisms of action and effects on bone cells, monocytes and macrophages. Curr. Pharm. Des. 16, 2950–2960 (2010).
Corey, E. et al. Zoledronic acid exhibits inhibitory effects on osteoblastic and osteolytic metastases of prostate cancer. Clin. Cancer Res. 9, 295–306 (2003).
Berry, S., Waldron, T., Winquist, E. & Lukka, H. The use of bisphosphonates in men with hormone-refractory prostate cancer: a systematic review of randomized trials. Can. J. Urol. 13, 3180–3188 (2006).
Dearnaley, D. P., Mason, M. D., Parmar, M. K., Sanders, K. & Sydes, M. R. Adjuvant therapy with oral sodium clodronate in locally advanced and metastatic prostate cancer: long-term overall survival results from the MRC PR04 and PR05 randomised controlled trials. Lancet Oncol. 10, 872–876 (2009).
Saad, F. et al. Long-term efficacy of zoledronic acid for the prevention of skeletal complications in patients with metastatic hormone-refractory prostate cancer. J. Natl Cancer Inst. 96, 879–882 (2004).
Saad, F. et al. A randomized, placebo-controlled trial of zoledronic acid in patients with hormone-refractory metastatic prostate carcinoma. J. Natl Cancer Inst. 94, 1458–1468 (2002).
Sydes, M. R. et al. Issues in applying multi-arm multi-stage methodology to a clinical trial in prostate cancer: the MRC STAMPEDE trial. Trials 10, 39 (2009).
James, N. D. et al. STAMPEDE: Systemic Therapy for Advancing or Metastatic Prostate Cancer—a multi-arm multi-stage randomised controlled trial. Clin. Oncol. (R. Coll. Radiol) 20, 577–581 (2008).
James, N. D. et al. Systemic therapy for advancing or metastatic prostate cancer (STAMPEDE): a multi-arm, multistage randomized controlled trial. BJU Int. 103, 464–469 (2009).
Ishizaka, K. et al. Preventive effect of risedronate on bone loss in men receiving androgen-deprivation therapy for prostate cancer. Int. J. Urol. 14, 1071–1075 (2007).
Izumi, K. et al. Risedronate recovers bone loss in patients with prostate cancer undergoing androgen-deprivation therapy. Urology 73, 1342–1346 (2009).
Taxel, P. et al. Risedronate prevents early bone loss and increased bone turnover in the first 6 months of luteinizing hormone-releasing hormone-agonist therapy for prostate cancer. BJU Int. 106, 1473–1476 (2010).
Greenspan, S. L. et al. Skeletal health after continuation, withdrawal, or delay of alendronate in men with prostate cancer undergoing androgen-deprivation therapy. J. Clin. Oncol. 26, 4426–4434 (2008).
Stopeck, A. T. et al. Denosumab compared with zoledronic acid for the treatment of bone metastases in patients with advanced breast cancer: a randomized, double-blind study. J. Clin. Oncol. 28, 5132–5139 (2010).
Fizazi, K. et al. Randomized phase II trial of denosumab in patients with bone metastases from prostate cancer, breast cancer, or other neoplasms after intravenous bisphosphonates. J. Clin. Oncol. 27, 1564–1571 (2009).
Fizazi, K., Bosserman, L., Gao, G., Skacel, T. & Markus, R. Denosumab treatment of prostate cancer with bone metastases and increased urine N.-telopeptide levels after therapy with intravenous bisphosphonates: results of a randomized phase II trial. J. Urol. 182, 509–515; discussion 515–516 (2009).
Body, J. J. et al. Effects of denosumab in patients with bone metastases with and without previous bisphosphonate exposure. J. Bone Miner. Res. 25, 440–446 (2010).
Saftig, P. et al. Impaired osteoclastic bone resorption leads to osteopetrosis in cathepsin-K-deficient mice. Proc. Natl Acad. Sci. USA 95, 13453–13458 (1998).
Podgorski, I. et al. Bone marrow-derived cathepsin K cleaves SPARC in bone metastasis. Am. J. Pathol. 175, 1255–1269 (2009).
Le Gall, C. et al. A cathepsin K inhibitor reduces breast cancer induced osteolysis and skeletal tumor burden. Cancer Res. 67, 9894–9902 (2007).
Brubaker, K. D., Vessella, R. L., True, L. D., Thomas, R. & Corey, E. Cathepsin K mRNA and protein expression in prostate cancer progression. J. Bone Miner. Res. 18, 222–230 (2003).
Seals, D. F. et al. The adaptor protein Tks5/Fish is required for podosome formation and function, and for the protease-driven invasion of cancer cells. Cancer Cell 7, 155–165 (2005).
Berdeaux, R. L., Diaz, B., Kim, L. & Martin, G. S. Active Rho is localized to podosomes induced by oncogenic Src and is required for their assembly and function. J. Cell Biol. 166, 317–323 (2004).
Schramp, M., Ying, O., Kim, T. Y. & Martin, G. S. ERK5 promotes Src-induced podosome formation by limiting Rho activation. J. Cell Biol. 181, 1195–1210 (2008).
Mandal, S., Johnson, K. R. & Wheelock, M. J. TGF-β induces formation of F-actin cores and matrix degradation in human breast cancer cells via distinct signaling pathways. Exp. Cell Res. 314, 3478–3493 (2008).
Tu, C. et al. Lysosomal cathepsin B participates in the podosome-mediated extracellular matrix degradation and invasion via secreted lysosomes in v-Src fibroblasts. Cancer Res. 68, 9147–9156 (2008).
Peroni, A. et al. Drug-induced morphea: report of a case induced by balicatib and review of the literature. J. Am. Acad. Dermatol. 59, 125–129 (2008).
Bromme, D. & Lecaille, F. Cathepsin K inhibitors for osteoporosis and potential off-target effects. Expert Opin. Investig Drugs 18, 585–600 (2009).
Jensen, A. B. et al. The cathepsin K inhibitor odanacatib suppresses bone resorption in women with breast cancer and established bone metastases: results of a 4-week, double-blind, randomized, controlled trial. Clin. Breast Cancer 10, 452–458 (2010).
Migliaccio, A. et al. Steroid-induced androgen receptor-oestradiol receptor beta-Src complex triggers prostate cancer cell proliferation. EMBO J. 19, 5406–5417 (2000).
Slack, J. K. et al. Alterations in the focal adhesion kinase/Src signal transduction pathway correlate with increased migratory capacity of prostate carcinoma cells. Oncogene 20, 1152–1163 (2001).
Asim, M., Siddiqui, I. A., Hafeez, B. B., Baniahmad, A. & Mukhtar, H. Src kinase potentiates androgen receptor transactivation function and invasion of androgen-independent prostate cancer C4–2 cells. Oncogene 27, 3596–3604 (2008).
Xia, W., Unger, P., Miller, L., Nelson, J. & Gelman, I. H. The Src-suppressed C kinase substrate, SSeCKS, is a potential metastasis inhibitor in prostate cancer. Cancer Res. 61, 5644–5651 (2001).
Marzia, M. et al. Decreased c-Src expression enhances osteoblast differentiation and bone formation. J. Cell Biol. 151, 311–320 (2000).
Soriano, P., Montgomery, C., Geske, R. & Bradley, A. Targeted disruption of the c-src proto-oncogene leads to osteopetrosis in mice. Cell 64, 693–702 (1991).
Lee, Y. C. et al. Src family kinase/abl inhibitor dasatinib suppresses proliferation and enhances differentiation of osteoblasts. Oncogene 29, 3196–3207 (2010).
Id Boufker, H. et al. The Src inhibitor dasatinib accelerates the differentiation of human bone marrow-derived mesenchymal stromal cells into osteoblasts. BMC Cancer 10, 298 (2010).
Koreckij, T. et al. Dasatinib inhibits the growth of prostate cancer in bone and provides additional protection from osteolysis. Br. J. Cancer 101, 263–268 (2009).
Yang, J. C. et al. Effect of the specific Src family kinase inhibitor saracatinib on osteolytic lesions using the PC-3 bone model. Mol. Cancer Ther. 9, 1629–1637 (2010).
Rabbani, S. A., Valentino, M. L., Arakelian, A., Ali, S. & Boschelli, F. SKI-606 (Bosutinib) blocks prostate cancer invasion, growth, and metastasis in vitro and in vivo through regulation of genes involved in cancer growth and skeletal metastasis. Mol. Cancer Ther. 9, 1147–1157 (2010).
Janssens, K., ten Dijke, P., Janssens, S. & Van Hul, W. Transforming growth factor-β1 to the bone. Endocr. Rev. 26, 743–774 (2005).
Blobe, G. C., Schiemann, W. P. & Lodish, H. F. Role of transforming growth factor-β in human disease. N. Engl. J. Med. 342, 1350–1358 (2000).
Gordon, K. J. & Blobe, G. C. Role of transforming growth factor-β superfamily signaling pathways in human disease. Biochim. Biophys. Acta 1782, 197–228 (2008).
Tang, Y. et al. TGF-β1-induced migration of bone mesenchymal stem cells couples bone resorption with formation. Nat. Med. 15, 757–765 (2009).
Mohammad, K. S. et al. Pharmacologic inhibition of the TGF-β type I receptor kinase has anabolic and anti-catabolic effects on bone. PLoS One 4, e5275 (2009).
Alliston, T., Choy, L., Ducy, P., Karsenty, G. & Derynck, R. TGF-β-induced repression of CBFA1 by Smad3 decreases cbfa1 and osteocalcin expression and inhibits osteoblast differentiation. EMBO J. 20, 2254–2272 (2001).
Qiu, T. et al. TGF-β type II receptor phosphorylates PTH receptor to integrate bone remodelling signalling. Nat. Cell Biol. 12, 224–234 (2010).
Kang, Y. et al. A multigenic program mediating breast cancer metastasis to bone. Cancer Cell 3, 537–549 (2003).
Kang, Y. et al. Breast cancer bone metastasis mediated by the Smad tumor suppressor pathway. Proc. Natl Acad. Sci. USA 102, 13909–13914 (2005).
Korpal, M. et al. Imaging transforming growth factor-β signaling dynamics and therapeutic response in breast cancer bone metastasis. Nat. Med. 15, 960–966 (2009).
Ganapathy, V. et al. Targeting the transforming growth factor-β pathway inhibits human basal-like breast cancer metastasis. Mol. Cancer 9, 122 (2010).
Nam, J. S. et al. An anti-transforming growth factor-β antibody suppresses metastasis via cooperative effects on multiple cell compartments. Cancer Res. 68, 3835–3843 (2008).
Mohammad, K. S. et al. TGF-β-RI kinase inhibitor SD-208 reduces the development and progression of melanoma bone metastases. Cancer Res. 71, 175–184 (2011).
Hu, Z., Zhang, Z., Guise, T. & Seth, P. Systemic delivery of an oncolytic adenovirus expressing soluble transforming growth factor-β receptor II-Fc fusion protein can inhibit breast cancer bone metastasis in a mouse model. Hum. Gene Ther. 21, 1623–1629 (2010).
Hu, Z. et al. A modified hTERT promoter-directed oncolytic adenovirus replication with concurrent inhibition of TGFβ signaling for breast cancer therapy. Cancer Gene Ther. 17, 235–243 (2010).
Criswell, T. L., Dumont, N., Barnett, J. V. & Arteaga, C. L. Knockdown of the transforming growth factor-beta type III receptor impairs motility and invasion of metastatic cancer cells. Cancer Res. 68, 7304–7312 (2008).
Ikushima, H. & Miyazono, K. TGFβ signalling: a complex web in cancer progression. Nat. Rev. Cancer 10, 415–424 (2010).
Jansen, D. R., Krijger, G. C., Kolar, Z. I., Zonnenberg, B. A. & Zeevaart, J. R. Targeted Radiotherapy of Bone Malignancies. Curr. Drug Discov. Technol. 7 233–246 (2010).
Bauman, G., Charette, M., Reid, R. & Sathya, J. Radiopharmaceuticals for the palliation of painful bone metastasis-a systemic review. Radiother Oncol. 75, 258–270 (2005).
Tu, S. M. et al. Bone-targeted therapy for advanced androgen-independent carcinoma of the prostate: a randomised phase II trial. Lancet 357, 336–341 (2001).
Collins, C. et al. Samarium-153-EDTMP in bone metastases of hormone refractory prostate carcinoma: a phase I/II trial. J. Nucl. Med. 34, 1839–1844 (1993).
Nilsson, S. et al. Radium-223 chloride, a first-in-class alpha-pharmaceutical with a benign safety profile for patients with castration-resistant prostate cancer (CRPC) and bone metastases: Combined analysis of phase I and II clinical trials. ASCO Meeting Abstracts 28, 4678 (2010).
Morris, M. J. et al. Phase I study of samarium-153 lexidronam with docetaxel in castration-resistant metastatic prostate cancer. J. Clin. Oncol. 27, 2436–2442 (2009).
Fizazi, K. et al. Phase II trial of consolidation docetaxel and samarium-153 in patients with bone metastases from castration-resistant prostate cancer. J. Clin. Oncol. 27, 2429–2435 (2009).
Tu, S. M. et al. Phase I study of concurrent weekly docetaxel and repeated samarium-153 lexidronam in patients with castration-resistant metastatic prostate cancer. J. Clin. Oncol. 27, 3319–3324 (2009).
Lam, M. G. et al. Combined use of zoledronic acid and 153Sm-EDTMP in hormone-refractory prostate cancer patients with bone metastases. Eur. J. Nucl. Med. Mol. Imaging 35, 756–65 (2008).
Lam, M. G., de Klerk, J. M. & Zonnenberg, B. A. Treatment of painful bone metastases in hormone-refractory prostate cancer with zoledronic acid and samarium-153-ethylenediaminetetramethylphosphonic acid combined. J. Palliat. Med. 12, 649–651 (2009).
Nelson, J. B. et al. Identification of endothelin-1 in the pathophysiology of metastatic adenocarcinoma of the prostate. Nat. Med. 1, 944–949 (1995).
Yin, J. J. et al. A causal role for endothelin-1 in the pathogenesis of osteoblastic bone metastases. Proc. Natl Acad. Sci. USA 100, 10954–10959 (2003).
Drake, J. M., Danke, J. R. & Henry, M. D. Bone-specific growth inhibition of prostate cancer metastasis by atrasentan. Cancer Biol. Ther. 9, 607–614 (2010).
Guise, T. A., Yin, J. J. & Mohammad, K. S. Role of endothelin-1 in osteoblastic bone metastases. Cancer 97, 779–784 (2003).
Carducci, M. A. et al. Effect of endothelin-A receptor blockade with atrasentan on tumor progression in men with hormone-refractory prostate cancer: a randomized, phase II, placebo-controlled trial. J. Clin. Oncol. 21, 679–689 (2003).
Cella, D. et al. Role of quality of life in men with metastatic hormone-refractory prostate cancer: how does atrasentan influence quality of life? Eur. Urol. 49, 781–789 (2006).
Nelson, J. B. et al. Suppression of prostate cancer induced bone remodeling by the endothelin receptor A antagonist atrasentan. J. Urol. 169, 1143–1149 (2003).
Carducci, M. A. et al. A phase 3 randomized controlled trial of the efficacy and safety of atrasentan in men with metastatic hormone-refractory prostate cancer. Cancer 110, 1959–1966 (2007).
Vogelzang, N. J. et al. Meta-analysis of clinical trials of atrasentan 10 mg in metastatic hormone-refractory prostate cancer. J. Clin. Oncol. (Meeting Abstracts) 23, Suppl. 4563 (2005).
Michaelson, M. D., Kaufman, D. S., Kantoff, P., Oh, W. K. & Smith, M. R. Randomized phase II study of atrasentan alone or in combination with zoledronic acid in men with metastatic prostate cancer. Cancer 107, 530–535 (2006).
Nelson, J. B. Phase III study of the efficacy and safety of zibotentan (ZD4054) in patients with bone metastatic castration-resistant prostate cancer (CRPC) [abstract]. J. Clin. Oncol. 29 (Suppl. 7), a117 (2011).
James, N. D. et al. Final safety and efficacy analysis of the specific endothelin A receptor antagonist zibotentan (ZD4054) in patients with metastatic castration-resistant prostate cancer and bone metastases who were pain-free or mildly symptomatic for pain: a double-blind, placebo-controlled, randomized phase II trial. BJU Int. 106, 966–973 (2010).
Day, T. F., Guo, X., Garrett-Beal, L. & Yang, Y. Wnt/beta-catenin signaling in mesenchymal progenitors controls osteoblast and chondrocyte differentiation during vertebrate skeletogenesis. Dev. Cell 8, 739–750 (2005).
Hill, T. P., Später, D., Taketo, M. M., Birchmeier, W. & Hartmann, C. Canonical Wnt/β-catenin signaling prevents osteoblasts from differentiating into chondrocytes. Dev. Cell 8, 727–738 (2005).
Bennett, C. N. et al. Wnt10b increases postnatal bone formation by enhancing osteoblast differentiation. J. Bone Miner. Res. 22, 1924–1932 (2007).
Morvan, F. et al. Deletion of a single allele of the Dkk1 gene leads to an increase in bone formation and bone mass. J. Bone Miner. Res. 21, 934–945 (2006).
ten Dijke, P., Krause, C., de Gorter, D. J., Löwik, C. W. & van Bezooijen, R. L. Osteocyte-derived sclerostin inhibits bone formation: its role in bone morphogenetic protein and Wnt signaling. J. Bone Joint Surg. Am. 90 (Suppl. 1), 31–35 (2008).
Hall, C. L., Bafico, A., Dai, J., Aaronson, S. A. & Keller, E. T. Prostate cancer cells promote osteoblastic bone metastases through Wnts. Cancer Res. 65, 7554–7560 (2005).
Dai, J. et al. Prostate cancer induces bone metastasis through Wnt-induced bone morphogenetic protein-dependent and independent mechanisms. Cancer Res. 68, 5785–5794 (2008).
Schwaninger, R. et al. Lack of noggin expression by cancer cells is a determinant of the osteoblast response in bone metastases. Am. J. Pathol. 170, 160–175 (2007).
Rentsch, C. A., Cecchini, M. G. & Thalmann, G. N. Loss of inhibition over master pathways of bone mass regulation results in osteosclerotic bone metastases in prostate cancer. Swiss Med. Wkly 139, 220–225 (2009).
Hall, C. L. & Keller, E. T. The role of Wnts in bone metastases. Cancer Metastasis Rev. 25, 551–558 (2006).
Smith, H. W. & Marshall, C. J. Regulation of cell signalling by uPAR. Nat. Rev. Mol. Cell Biol. 11, 23–36 (2010).
Shariat, S. F. et al. Association of the circulating levels of the urokinase system of plasminogen activation with the presence of prostate cancer and invasion, progression, and metastasis. J. Clin. Oncol. 25, 349–355 (2007).
Thomas, C. et al. Urokinase-plasminogen-activator receptor expression in disseminated tumour cells in the bone marrow and peripheral blood of patients with clinically localized prostate cancer. BJU Int. 104, 29–34 (2009).
Rabbani, S. A. et al. An amino-terminal fragment of urokinase isolated from a prostate cancer cell line (PC-3) is mitogenic for osteoblast-like cells. Biochem. Biophys. Res. Commun. 173, 1058–1064 (1990).
Rabbani, S. A., Gladu, J., Mazar, A. P., Henkin, J. & Goltzman, D. Induction in human osteoblastic cells (SaOS2) of the early response genes fos, jun, and myc by the amino terminal fragment (ATF) of urokinase. J. Cell Physiol. 172, 137–145 (1997).
Koutsilieris, M., Sourla, A., Pelletier, G. & Doillon, C. J. Three-dimensional type I collagen gel system for the study of osteoblastic metastases produced by metastatic prostate cancer. J. Bone Miner. Res. 9, 1823–1832 (1994).
Mitsiades, C., Sourla, A., Doillon, C., Lembessis, P. & Koutsilieris, M. Three-dimensional type I collagen co-culture systems for the study of cell-cell interactions and treatment response in bone metastases. J. Musculoskelet. Neuronal Interact. 1, 153–155 (2000).
Achbarou, A. et al. Urokinase overproduction results in increased skeletal metastasis by prostate cancer cells in vivo. Cancer Res. 54, 2372–2377 (1994).
Fritz, V. et al. Antitumoral activity and osteogenic potential of mesenchymal stem cells expressing the urokinase-type plasminogen antagonist amino-terminal fragment in a murine model of osteolytic tumor. Stem Cells 26, 2981–2990 (2008).
Sturge, J., Wienke, D., East, L., Jones, G. E. & Isacke, C. M. GPI-anchored uPAR requires Endo180 for rapid directional sensing during chemotaxis. J. Cell Biol. 162, 789–794 (2003).
Thomas, E. K. et al. Endo180 binds to the C-terminal region of type I collagen. J. Biol. Chem. 280, 22596–22605 (2005).
Sturge, J., Wienke, D. & Isacke, C. M. Endosomes generate localized Rho-ROCK-MLC2-based contractile signals via Endo180 to promote adhesion disassembly. J. Cell Biol. 175, 337–347 (2006).
Wu, K., Yuan, J. & Lasky, L. A. Characterization of a novel member of the macrophage mannose receptor type C lectin family. J. Biol. Chem. 271, 21323–21330 (1996).
Fasquelle, C. et al. Balancing selection of a frame-shift mutation in the MRC2 gene accounts for the outbreak of the Crooked Tail Syndrome in Belgian Blue Cattle. PLoS Genet. 5, e1000666 (2009).
Wagenaar-Miller, R. A. et al. Complementary roles of intracellular and pericellular collagen degradation pathways in vivo. Mol. Cell Biol. 27, 6309–6322 (2007).
Huijbers, I. J. et al. A role for fibrillar collagen deposition and the collagen internalization receptor Endo180 in glioma invasion. PLoS One 5, e9808 (2010).
Wienke, D. et al. The collagen receptor Endo180 (CD280) is expressed on basal-like breast tumor cells and promotes tumor growth in vivo. Cancer Res. 67, 10230–10240 (2007).
Caley, M. et al. Osteoblasts orchestrate collagen remodelling via tumour cell-dependent regulation of Endo180 in metastatic bone disease. 2010 Nature - CNIO Cancer Symposium: Frontiers in Tumour Progression, http://www.nature.com/natureconferences/fitp2010/index.html.
Kogianni, G., Walker, M. M., Waxman, J. & Sturge, J. Endo180 expression with cofunctional partners MT1-MMP and uPAR-uPA is correlated with prostate cancer progression. Eur. J. Cancer 45, 685–693 (2009).
Wang, G. et al. Osteoblast-derived factors induce an expression signature that identifies prostate cancer metastasis and hormonal progression. Cancer Res. 69, 3433–3442 (2009).
Hikita, A. et al. Identification of an alternatively spliced variant of Ca2+-promoted Ras inactivator as a possible regulator of RANKL shedding. J. Biol. Chem. 280, 41700–41706 (2005).
Hikita, A. et al. Negative regulation of osteoclastogenesis by ectodomain shedding of receptor activator of NFκB ligand. J. Biol. Chem. 281, 36846–36855 (2006).
Lynch, C. C. et al. MMP-7 promotes prostate cancer-induced osteolysis via the solubilization of RANKL. Cancer Cell 7, 485–496 (2005).
Acknowledgements
The authors would like to acknowledge funding support from The Prostate Cancer Charity (Grant 110632), The Prostate Cancer Charity and the Milly Apthorp Charitable Trust (Grant 110854), The Association of International Cancer Research (Grant 08-0803), The Rosetrees Trust (Grant JS16/M59), Tony & Rita Gallagher, Imperial College NHS Healthcare Trust Special Trustees and The Fundação para a Ciência e Tecnologia. We thank A. V. Fonseca for her help in the schematic design.
Author information
Authors and Affiliations
Contributions
J. Sturge and M. P. Caley contributed to researching the data for the article. J. Sturge made a substantial contribution to the discussion and writing of the content. All authors contributed to reviewing and editing of the manuscript before submission.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
About this article
Cite this article
Sturge, J., Caley, M. & Waxman, J. Bone metastasis in prostate cancer: emerging therapeutic strategies. Nat Rev Clin Oncol 8, 357–368 (2011). https://doi.org/10.1038/nrclinonc.2011.67
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrclinonc.2011.67
This article is cited by
-
Targeting SphK1/2 by SKI-178 inhibits prostate cancer cell growth
Cell Death & Disease (2023)
-
Quantitative assessment of 99mTc-methylene diphosphonate bone SPECT/CT for assessing bone metastatic burden and its prognostic value in patients with castration-resistant prostate cancers: initial results in a single-center retrospective study
Annals of Nuclear Medicine (2023)
-
Osteoblasts and osteoclasts: an important switch of tumour cell dormancy during bone metastasis
Journal of Experimental & Clinical Cancer Research (2022)
-
Construction and validation of web-based nomograms for detecting and prognosticating in prostate adenocarcinoma with bone metastasis
Scientific Reports (2022)
-
Evolving cancer–niche interactions and therapeutic targets during bone metastasis
Nature Reviews Cancer (2022)