Key Points
-
The three isoforms of nitric oxide synthase subserve distinct, but coordinated, functions through their subcellular confinement in cardiac and vascular cells
-
The redox environment dictates the fate of nitric oxide and pathophysiological effects
-
Multiple regulatory points of downstream effectors ensure signalling specificity and allow therapeutic modulation
-
New techniques for monitoring nitric oxide bioavailability will allow efficient tailoring of treatment
Abstract
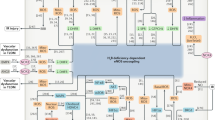
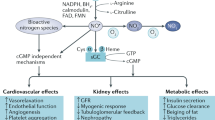
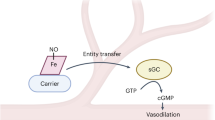
Nitric oxide (NO) signalling has pleiotropic roles in biology and a crucial function in cardiovascular homeostasis. Tremendous knowledge has been accumulated on the mechanisms of the nitric oxide synthase (NOS)–NO pathway, but how this highly reactive, free radical gas signals to specific targets for precise regulation of cardiovascular function remains the focus of much intense research. In this Review, we summarize the updated paradigms on NOS regulation, NO interaction with reactive oxidant species in specific subcellular compartments, and downstream effects of NO in target cardiovascular tissues, while emphasizing the latest developments of molecular tools and biomarkers to modulate and monitor NO production and bioavailability.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Kwon, N. S. et al. L-Citrulline production from L-arginine by macrophage nitric oxide synthase. The ureido oxygen derives from dioxygen. J. Biol. Chem. 265, 13442–13445 (1990).
Busse, R. & Mulsch, A. Calcium-dependent nitric oxide synthesis in endothelial cytosol is mediated by calmodulin. FEBS Lett. 265, 133–136 (1990).
Stuehr, D. J., Cho, H. J., Kwon, N. S., Weise, M. F. & Nathan, C. F. Purification and characterization of the cytokine-induced macrophage nitric oxide synthase: an FAD- and FMN-containing flavoprotein. Proc. Natl Acad. Sci. USA 88, 7773–7777 (1991).
Stuehr, D. J., Santolini, J., Wang, Z. Q., Wei, C. C. & Adak, S. Update on mechanism and catalytic regulation in the NO synthases. J. Biol. Chem. 279, 36167–36170 (2004).
Xia, Y., Tsai, A. L., Berka, V. & Zweier, J. L. Superoxide generation from endothelial nitric-oxide synthase. A Ca2+/calmodulin-dependent and tetrahydrobiopterin regulatory process. J. Biol. Chem. 273, 25804–25808 (1998).
Palmer, R. M., Ashton, D. S. & Moncada, S. Vascular endothelial cells synthesize nitric oxide from L-arginine. Nature 333, 664–666 (1988).
Balligand, J. L. et al. Nitric oxide-dependent parasympathetic signaling is due to activation of constitutive endothelial (type III) nitric oxide synthase in cardiac myocytes. J. Biol. Chem. 270, 14582–14586 (1995).
Petroff, M. G. et al. Endogenous nitric oxide mechanisms mediate the stretch dependence of Ca2+ release in cardiomyocytes. Nat. Cell Biol. 3, 867–873 (2001).
Wallerath, T. et al. Identification of the NO synthase isoforms expressed in human neutrophil granulocytes, megakaryocytes and platelets. Thromb. Haemost. 77, 163–167 (1997).
Kleinbongard, P. et al. Red blood cells express a functional endothelial nitric oxide synthase. Blood 107, 2943–2951 (2006).
Cortese-Krott, M. M. et al. Human red blood cells at work: identification and visualization of erythrocytic eNOS activity in health and disease. Blood 120, 4229–4237 (2012).
Balligand, J. L., Feron, O. & Dessy, C. eNOS activation by physical forces: from short-term regulation of contraction to chronic remodeling of cardiovascular tissues. Physiol. Rev. 89, 481–534 (2009).
Dimmeler, S. et al. Activation of nitric oxide synthase in endothelial cells by Akt-dependent phosphorylation. Nature 399, 601–605 (1999).
Fisslthaler, B., Loot, A. E., Mohamed, A., Busse, R. & Fleming, I. Inhibition of endothelial nitric oxide synthase activity by proline-rich tyrosine kinase 2 in response to fluid shear stress and insulin. Circ. Res. 102, 1520–1528 (2008).
Mattagajasingh, I. et al. SIRT1 promotes endothelium-dependent vascular relaxation by activating endothelial nitric oxide synthase. Proc. Natl Acad. Sci. USA 104, 14855–14860 (2007).
Feron, O., Michel, J. B., Sase, K. & Michel, T. Dynamic regulation of endothelial nitric oxide synthase: complementary roles of dual acylation and caveolin interactions. Biochemistry 37, 193–200 (1998).
Erwin, P. A., Lin, A. J., Golan, D. E. & Michel, T. Receptor-regulated dynamic S-nitrosylation of endothelial nitric-oxide synthase in vascular endothelial cells. J. Biol. Chem. 280, 19888–19894 (2005).
Chen, C. A. et al. S-Glutathionylation uncouples eNOS and regulates its cellular and vascular function. Nature 468, 1115–1118 (2010).
Yeh, D. C., Duncan, J. A., Yamashita, S. & Michel, T. Depalmitoylation of endothelial nitric-oxide synthase by acyl-protein thioesterase 1 is potentiated by Ca2+-calmodulin. J. Biol. Chem. 274, 33148–33154 (1999).
Feron, O. et al. Endothelial nitric oxide synthase targeting to caveolae. Specific interactions with caveolin isoforms in cardiac myocytes and endothelial cells. J. Biol. Chem. 271, 22810–22814 (1996).
Garcia-Cardena, G. et al. Dynamic activation of endothelial nitric oxide synthase by Hsp90. Nature 392, 821–824 (1998).
Fulton, D. et al. Regulation of endothelium-derived nitric oxide production by the protein kinase Akt. Nature 399, 597–601 (1999).
Fleming, I., Fisslthaler, B., Dimmeler, S., Kemp, B. E. & Busse, R. Phosphorylation of Thr(495) regulates Ca2+/calmodulin-dependent endothelial nitric oxide synthase activity. Circ. Res. 88, E68–E75 (2001).
Kupatt, C. et al. Heat shock protein 90 transfection reduces ischemia-reperfusion-induced myocardial dysfunction via reciprocal endothelial NO synthase serine 1177 phosphorylation and threonine 495 dephosphorylation. Arterioscler. Thromb. Vasc. Biol. 24, 1435–1441 (2004).
Chen, M. et al. Pim1 kinase promotes angiogenesis through phosphorylation of endothelial nitric oxide synthase at Ser-633. Cardiovasc. Res. 109, 141–150 (2016).
Bibli, S. I. et al. Tyrosine phosphorylation of eNOS regulates myocardial survival after an ischaemic insult: role of PYK2. Cardiovasc. Res. 113, 926–937 (2017).
Xu, K. Y., Huso, D. L., Dawson, T. M., Bredt, D. S. & Becker, L. C. Nitric oxide synthase in cardiac sarcoplasmic reticulum. Proc. Natl Acad. Sci. USA 96, 657–662 (1999).
Choate, J. K., Danson, E. J., Morris, J. F. & Paterson, D. J. Peripheral vagal control of heart rate is impaired in neuronal NOS knockout mice. Am. J. Physiol. Heart Circ. Physiol. 281, H2310–H2317 (2001).
Schwarz, P. M., Kleinert, H. & Forstermann, U. Potential functional significance of brain-type and muscle-type nitric oxide synthase I expressed in adventitia and media of rat aorta. Arterioscler. Thromb. Vasc. Biol. 19, 2584–2590 (1999).
Piech, A., Dessy, C., Havaux, X., Feron, O. & Balligand, J. L. Differential regulation of nitric oxide synthases and their allosteric regulators in heart and vessels of hypertensive rats. Cardiovasc. Res. 57, 456–467 (2003).
Brenman, J. E. et al. Interaction of nitric oxide synthase with the postsynaptic density protein PSD-95 and alpha1-syntrophin mediated by PDZ domains. Cell 84, 757–767 (1996).
Lai, Y. et al. Dystrophins carrying spectrin-like repeats 16 and 17 anchor nNOS to the sarcolemma and enhance exercise performance in a mouse model of muscular dystrophy. J. Clin. Invest. 119, 624–635 (2009).
Williams, J. C. et al. The sarcolemmal calcium pump, alpha-1 syntrophin, and neuronal nitric-oxide synthase are parts of a macromolecular protein complex. J. Biol. Chem. 281, 23341–23348 (2006).
Reilly, S. N. et al. Up-regulation of miR-31 in human atrial fibrillation begets the arrhythmia by depleting dystrophin and neuronal nitric oxide synthase. Sci. Transl Med. 8, 340ra74 (2016).
Eliasson, M. J., Blackshaw, S., Schell, M. J. & Snyder, S. H. Neuronal nitric oxide synthase alternatively spliced forms: prominent functional localizations in the brain. Proc. Natl Acad. Sci. USA 94, 3396–3401 (1997).
Fang, M. et al. Dexras1: a G protein specifically coupled to neuronal nitric oxide synthase via CAPON. Neuron 28, 183–193 (2000).
Kapoor, A. et al. An enhancer polymorphism at the cardiomyocyte intercalated disc protein NOS1AP locus is a major regulator of the QT interval. Am. J. Hum. Genet. 94, 854–869 (2014).
Chang, K. C. et al. CAPON modulates cardiac repolarization via neuronal nitric oxide synthase signaling in the heart. Proc. Natl Acad. Sci. USA 105, 4477–4482 (2008).
Arking, D. E. et al. A common genetic variant in the NOS1 regulator NOS1AP modulates cardiac repolarization. Nat. Genet. 38, 644–651 (2006).
Tobin, M. D. et al. Gender and effects of a common genetic variant in the NOS1 regulator NOS1AP on cardiac repolarization in 3761 individuals from two independent populations. Int. J. Epidemiol. 37, 1132–1141 (2008).
Tomas, M. et al. Polymorphisms in the NOS1AP gene modulate QT interval duration and risk of arrhythmias in the long QT syndrome. J. Am. Coll. Cardiol. 55, 2745–2752 (2010).
Kolder, I. et al. Analysis for genetic modifiers of disease severity in patients with long-QT syndrome type 2. Circ. Cardiovasc. Genet. 8, 447–456 (2015).
Earle, N. J. et al. Genetic markers of repolarization and arrhythmic events after acute coronary syndromes. Am. Heart J. 169, 579–586.e3 (2015).
Verweij, N. et al. Twenty-eight genetic loci associated with ST-T-wave amplitudes of the electrocardiogram. Hum. Mol. Genet. 25, 2093–2103 (2016).
Nunez, L. et al. Nitric oxide blocks hKv1.5 channels by S-nitrosylation and by a cyclic GMP-dependent mechanism. Cardiovasc. Res. 72, 80–89 (2006).
Gomez, R. et al. Nitric oxide inhibits Kv4.3 and human cardiac transient outward potassium current (Ito1). Cardiovasc. Res. 80, 375–384 (2008).
Lekontseva, O., Chakrabarti, S., Jiang, Y., Cheung, C. C. & Davidge, S. T. Role of neuronal nitric-oxide synthase in estrogen-induced relaxation in rat resistance arteries. J. Pharmacol. Exp. Ther. 339, 367–375 (2011).
Adak, S. et al. Neuronal nitric-oxide synthase mutant (Ser-1412 → Asp) demonstrates surprising connections between heme reduction, NO complex formation, and catalysis. J. Biol. Chem. 276, 1244–1252 (2001).
Trappanese, D. M. et al. Chronic beta1-adrenergic blockade enhances myocardial beta3-adrenergic coupling with nitric oxide-cGMP signaling in a canine model of chronic volume overload: new insight into mechanisms of cardiac benefit with selective beta1-blocker therapy. Bas. Res. Cardiol. 110, 456 (2015).
Kar, R., Kellogg, D. L. III & Roman, L. J. Oxidative stress induces phosphorylation of neuronal NOS in cardiomyocytes through AMP-activated protein kinase (AMPK). Biochem. Biophys. Res. Commun. 459, 393–397 (2015).
Jaffrey, S. R. & Snyder, S. H. PIN: an associated protein inhibitor of neuronal nitric oxide synthase. Science 274, 774–777 (1996).
Hemmens, B. et al. The protein inhibitor of neuronal nitric oxide synthase (PIN): characterization of its action on pure nitric oxide synthases. FEBS Lett. 430, 397–400 (1998).
Xia, Y., Berlowitz, C. O. & Zweier, J. L. PIN inhibits nitric oxide and superoxide production from purified neuronal nitric oxide synthase. Biochim. Biophys. Acta 1760, 1445–1449 (2006).
Barouch, L. A. et al. Nitric oxide regulates the heart by spatial confinement of nitric oxide synthase isoforms. Nature 416, 337–339 (2002).
Zhang, Y. H. & Casadei, B. Sub-cellular targeting of constitutive NOS in health and disease. J. Mol. Cell. Cardiol. 52, 341–350 (2012).
Wilcox, J. N. et al. Expression of multiple isoforms of nitric oxide synthase in normal and atherosclerotic vessels. Arterioscler. Thromb. Vasc. Biol. 17, 2479–2488 (1997).
Balligand, J. L. et al. Cytokine-inducible nitric oxide synthase (iNOS) expression in cardiac myocytes. Characterization and regulation of iNOS expression and detection of iNOS activity in single cardiac myocytes in vitro. J. Biol. Chem. 269, 27580–27588 (1994).
de Vera, M. E. et al. Transcriptional regulation of human inducible nitric oxide synthase (NOS2) gene by cytokines: initial analysis of the human NOS2 promoter. Proc. Natl Acad. Sci. USA 93, 1054–1059 (1996).
Pautz, A. et al. Regulation of the expression of inducible nitric oxide synthase. Nitric Oxide 23, 75–93 (2010).
MacMicking, J., Xie, Q. W. & Nathan, C. Nitric oxide and macrophage function. Annu. Rev. Immunol. 15, 323–350 (1997).
Haywood, G. A. et al. Expression of inducible nitric oxide synthase in human heart failure. Circulation 93, 1087–1094 (1996).
Maron, B. A., Tang, S. S. & Loscalzo, J. S-Nitrosothiols and the S-nitrosoproteome of the cardiovascular system. Antioxid. Redox Signal. 18, 270–287 (2013).
Martinez-Ruiz, A. & Lamas, S. Detection and proteomic identification of S-nitrosylated proteins in endothelial cells. Arch. Biochem. Biophys. 423, 192–199 (2004).
Straub, A. C. et al. Endothelial cell expression of haemoglobin alpha regulates nitric oxide signalling. Nature 491, 473–477 (2012).
Kleschyov, A. L. The NO-heme signaling hypothesis. Free Radic. Biol. Med. 112, 544–552 (2017).
Montfort, W. R., Wales, J. A. & Weichsel, A. Structure and activation of soluble guanylyl cyclase, the nitric oxide sensor. Antioxid. Redox Signal. 26, 107–121 (2017).
Zaccolo, M. & Movsesian, M. A. cAMP and cGMP signaling cross-talk: role of phosphodiesterases and implications for cardiac pathophysiology. Circ. Res. 100, 1569–1578 (2007).
Weber, S. et al. PDE2 at the crossway between cAMP and cGMP signalling in the heart. Cell Signal. 38, 76–84 (2017).
Munzel, T. et al. Physiology and pathophysiology of vascular signaling controlled by guanosine 3′,5′-cyclic monophosphate-dependent protein kinase [corrected]. Circulation 108, 2172–2183 (2003).
Massion, P. B. & Balligand, J. L. Modulation of cardiac contraction, relaxation and rate by the endothelial nitric oxide synthase (eNOS): lessons from genetically modified mice. J. Physiol. 546, 63–75 (2003).
Surks, H. K. et al. Regulation of myosin phosphatase by a specific interaction with cGMP- dependent protein kinase Ialpha. Science 286, 1583–1587 (1999).
Klein, G., Drexler, H. & Schroder, F. Protein kinase G reverses all isoproterenol induced changes of cardiac single L-type calcium channel gating. Cardiovasc. Res. 48, 367–374 (2000).
Wollert, K. C. et al. Increased effects of C-type natriuretic peptide on contractility and calcium regulation in murine hearts overexpressing cyclic GMP-dependent protein kinase I. Br. J. Pharmacol. 140, 1227–1236 (2003).
Lee, D. I. et al. PDE5A suppression of acute beta-adrenergic activation requires modulation of myocyte beta-3 signaling coupled to PKG-mediated troponin I phosphorylation. Bas. Res. Cardiol. 105, 337–347 (2010).
Hamdani, N., Bishu, K. G., von Frieling-Salewsky, M., Redfield, M. M. & Linke, W. A. Deranged myofilament phosphorylation and function in experimental heart failure with preserved ejection fraction. Cardiovasc. Res. 97, 464–471 (2013).
Kruger, M. et al. Protein kinase G modulates human myocardial passive stiffness by phosphorylation of the titin springs. Circ. Res. 104, 87–94 (2009).
Burgoyne, J. R. et al. Cysteine redox sensor in PKGIa enables oxidant-induced activation. Science 317, 1393–1397 (2007).
Scotcher, J. et al. Disulfide-activated protein kinase G Ialpha regulates cardiac diastolic relaxation and fine-tunes the Frank-Starling response. Nat. Commun. 7, 13187 (2016).
Khavandi, K. et al. Pressure-induced oxidative activation of PKG enables vasoregulation by Ca2+ sparks and BK channels. Sci. Signal. 9, ra100 (2016).
Murphy, E. et al. Signaling by S-nitrosylation in the heart. J. Mol. Cell. Cardiol. 73, 18–25 (2014).
Lima, B., Forrester, M. T., Hess, D. T. & Stamler, J. S. S-Nitrosylation in cardiovascular signaling. Circ. Res. 106, 633–646 (2010).
Chouchani, E. T. et al. Cardioprotection by S-nitrosation of a cysteine switch on mitochondrial complex I. Nat. Med. 19, 753–759 (2013).
Zhang, R., Hess, D. T., Reynolds, J. D. & Stamler, J. S. Hemoglobin S-nitrosylation plays an essential role in cardioprotection. J. Clin. Invest. 126, 4654–4658 (2016).
Sun, J. et al. Ischaemic preconditioning preferentially increases protein S-nitrosylation in subsarcolemmal mitochondria. Cardiovasc. Res. 106, 227–236 (2015).
Gonzalez, D. R., Beigi, F., Treuer, A. V. & Hare, J. M. Deficient ryanodine receptor S-nitrosylation increases sarcoplasmic reticulum calcium leak and arrhythmogenesis in cardiomyocytes. Proc. Natl Acad. Sci. USA 104, 20612–20617 (2007).
Sun, J. et al. Hypercontractile female hearts exhibit increased S-nitrosylation of the L-type Ca2+ channel alpha1 subunit and reduced ischemia/reperfusion injury. Circ. Res. 98, 403–411 (2006).
Irie, T. et al. S-Nitrosylation of calcium-handling proteins in cardiac adrenergic signaling and hypertrophy. Circ. Res. 117, 793–803 (2015).
Figueiredo-Freitas, C. et al. S-Nitrosylation of sarcomeric proteins depresses myofilament Ca2+ sensitivity in intact cardiomyocytes. Antioxid. Redox Signal. 23, 1017–1034 (2015).
Jia, L., Bonaventura, C., Bonaventura, J. & Stamler, J. S. S-Nitrosohaemoglobin: a dynamic activity of blood involved in vascular control. Nature 380, 221–226 (1996).
Cai, Z. et al. Endothelial nitric oxide synthase-derived nitric oxide prevents dihydrofolate reductase degradation via promoting S-nitrosylation. Arterioscler. Thromb. Vasc. Biol. 35, 2366–2373 (2015).
Sayed, N., Baskaran, P., Ma, X., van den Akker, F. & Beuve, A. Desensitization of soluble guanylyl cyclase, the NO receptor, by S-nitrosylation. Proc. Natl Acad. Sci. USA 104, 12312–12317 (2007).
Liu, L. et al. A metabolic enzyme for S-nitrosothiol conserved from bacteria to humans. Nature 410, 490–494 (2001).
Hatzistergos, K. E. et al. S-Nitrosoglutathione reductase deficiency enhances the proliferative expansion of adult heart progenitors and myocytes post myocardial infarction. J. Am. Heart Assoc. 4, e001974 (2015).
Liu, L. et al. Essential roles of S-nitrosothiols in vascular homeostasis and endotoxic shock. Cell 116, 617–628 (2004).
Beigi, F. et al. Dynamic denitrosylation via S-nitrosoglutathione reductase regulates cardiovascular function. Proc. Natl Acad. Sci. USA 109, 4314–4319 (2012).
Yang, G. et al. H2S as a physiologic vasorelaxant: hypertension in mice with deletion of cystathionine gamma-lyase. Science 322, 587–590 (2008).
Coletta, C. et al. Hydrogen sulfide and nitric oxide are mutually dependent in the regulation of angiogenesis and endothelium-dependent vasorelaxation. Proc. Natl Acad. Sci. USA 109, 9161–9166 (2012).
Altaany, Z., Ju, Y., Yang, G. & Wang, R. The coordination of S-sulfhydration, S-nitrosylation, and phosphorylation of endothelial nitric oxide synthase by hydrogen sulfide. Sci. Signal. 7, ra87 (2014).
Kanagy, N. L., Szabo, C. & Papapetropoulos, A. Vascular biology of hydrogen sulfide. Am. J. Physiol. Cell Physiol. 312, C537–C549 (2017).
Zhou, Z. et al. Regulation of soluble guanylyl cyclase redox state by hydrogen sulfide. Pharmacol. Res. 111, 556–562 (2016).
Bucci, M. et al. Hydrogen sulfide is an endogenous inhibitor of phosphodiesterase activity. Arterioscler. Thromb. Vasc. Biol. 30, 1998–2004 (2010).
Stubbert, D. et al. Protein kinase G Ialpha oxidation paradoxically underlies blood pressure lowering by the reductant hydrogen sulfide. Hypertension 64, 1344–1351 (2014).
King, A. L. et al. Hydrogen sulfide cytoprotective signaling is endothelial nitric oxide synthase-nitric oxide dependent. Proc. Natl Acad. Sci. USA 111, 3182–3187 (2014).
Bibli, S. I. et al. Cardioprotection by H2S engages a cGMP-dependent protein kinase G/phospholamban pathway. Cardiovasc. Res. 106, 432–442 (2015).
Jian, Z. et al. Mechanochemotransduction during cardiomyocyte contraction is mediated by localized nitric oxide signaling. Sci. Signal. 7, ra27 (2014).
Ashley, E. A., Sears, C. E., Bryant, S. M., Watkins, H. C. & Casadei, B. Cardiac nitric oxide synthase 1 regulates basal and beta-adrenergic contractility in murine ventricular myocytes. Circulation 105, 3011–3016 (2002).
Wang, H., Kohr, M. J., Wheeler, D. G. & Ziolo, M. T. Endothelial nitric oxide synthase decreases beta-adrenergic responsiveness via inhibition of the L-type Ca2+ current. Am. J. Physiol. Heart Circ. Physiol. 294, H1473–H1480 (2008).
Sears, C. E. et al. Cardiac neuronal nitric oxide synthase isoform regulates myocardial contraction and calcium handling. Circ. Res. 92, e52–e59 (2003).
Brown, G. C. & Borutaite, V. Nitric oxide and mitochondrial respiration in the heart. Cardiovasc. Res. 75, 283–290 (2007).
Balligand, J. L., Kelly, R. A., Marsden, P. A., Smith, T. W. & Michel, T. Control of cardiac muscle cell function by an endogenous nitric oxide signaling system. Proc. Natl Acad. Sci. USA 90, 347–351 (1993).
Massion, P. B., Feron, O., Dessy, C. & Balligand, J. L. Nitric oxide and cardiac function: ten years after, and continuing. Circ. Res. 93, 388–398 (2003).
Martin, S. R., Emanuel, K., Sears, C. E., Zhang, Y. H. & Casadei, B. Are myocardial eNOS and nNOS involved in the beta-adrenergic and muscarinic regulation of inotropy? A systematic investigation. Cardiovasc. Res. 70, 97–106 (2006).
Gauthier, C. et al. The negative inotropic effect of beta3-adrenoceptor stimulation is mediated by activation of a nitric oxide synthase pathway in human ventricle. J. Clin. Invest. 102, 1377–1384 (1998).
Tavernier, G. et al. Beta3-adrenergic stimulation produces a decrease of cardiac contractility ex vivo in mice overexpressing the human beta3-adrenergic receptor. Cardiovasc. Res. 59, 288–296 (2003).
Varghese, P. et al. Beta3-adrenoceptor deficiency blocks nitric oxide-dependent inhibition of myocardial contractility. J. Clin. Invest. 106, 697–703 (2000).
Idigo, W. O. et al. Regulation of endothelial nitric-oxide synthase (NOS) S-glutathionylation by neuronal NOS: evidence of a functional interaction between myocardial constitutive NOS isoforms. J. Biol. Chem. 287, 43665–43673 (2012).
Gallo, M. P. et al. Modulation of guinea-pig cardiac L-type calcium current by nitric oxide synthase inhibitors. J. Physiol. 506, 639–651 (1998).
Poteser, M., Romanin, C., Schreibmayer, W., Mayer, B. & Groschner, K. S-Nitrosation controls gating and conductance of the alpha 1 subunit of class C L-type Ca(2+) channels. J. Biol. Chem. 276, 14797–14803 (2001).
Layland, J., Li, J. M. & Shah, A. M. Role of cyclic GMP-dependent protein kinase in the contractile response to exogenous nitric oxide in rat cardiac myocytes. J. Physiol. 540, 457–467 (2002).
Kohlhaas, M. et al. Endogenous nitric oxide formation in cardiac myocytes does not control respiration during beta-adrenergic stimulation. J. Physiol. 595, 3781–3798 (2017).
Cutler, M. J. et al. Aberrant S-nitrosylation mediates calcium-triggered ventricular arrhythmia in the intact heart. Proc. Natl Acad. Sci. USA 109, 18186–18191 (2012).
Fauconnier, J. et al. Leaky RyR2 trigger ventricular arrhythmias in Duchenne muscular dystrophy. Proc. Natl Acad. Sci. USA 107, 1559–1564 (2010).
Wang, H. et al. Regulation of myocyte contraction via neuronal nitric oxide synthase: role of ryanodine receptor S-nitrosylation. J. Physiol. 588, 2905–2917 (2010).
Zhang, Y. H. et al. Reduced phospholamban phosphorylation is associated with impaired relaxation in left ventricular myocytes from neuronal NO synthase-deficient mice. Circ. Res. 102, 242–249 (2008).
Khan, S. A. et al. Neuronal nitric oxide synthase negatively regulates xanthine oxidoreductase inhibition of cardiac excitation-contraction coupling. Proc. Natl Acad. Sci. USA 101, 15944–15948 (2004).
Carnicer, R. et al. The subcellular localisation of neuronal nitric oxide synthase determines the downstream effects of NO on myocardial function. Cardiovasc. Res. 113, 321–331 (2017).
Damy, T. et al. Increased neuronal nitric oxide synthase-derived NO production in the failing human heart. Lancet 363, 1365–1367 (2004).
Paulus, W. J., Vantrimpont, P. J. & Shah, A. M. Paracrine coronary endothelial control of left ventricular function in humans. Circulation 92, 2119–2126 (1995).
Godecke, A. et al. Inotropic response to beta-adrenergic receptor stimulation and anti-adrenergic effect of ACh in endothelial NO synthase-deficient mouse hearts. J. Physiol. 532, 195–204 (2001).
Liu, X. et al. Cytoglobin regulates blood pressure and vascular tone through nitric oxide metabolism in the vascular wall. Nat. Commun. 8, 14807 (2017).
Santizo, R., Baughman, V. L. & Pelligrino, D. A. Relative contributions from neuronal and endothelial nitric oxide synthases to regional cerebral blood flow changes during forebrain ischemia in rats. Neuroreport 11, 1549–1553 (2000).
Gotoh, J. et al. Regional differences in mechanisms of cerebral circulatory response to neuronal activation. Am. J. Physiol. Heart Circ. Physiol. 280, H821–H829 (2001).
Kurihara, N. et al. Role of nNOS in blood pressure regulation in eNOS null mutant mice. Hypertension 32, 856–861 (1998).
Toda, N. & Okamura, T. Modulation of renal blood flow and vascular tone by neuronal nitric oxide synthase-derived nitric oxide. J. Vasc. Res. 48, 1–10 (2011).
Huang, A. et al. Neuronal NOS-dependent dilation to flow in coronary arteries of male eNOS-KO mice. Am. J. Physiol. Heart Circ. Physiol. 282, H429–H436 (2002).
Seddon, M. D., Chowienczyk, P. J., Brett, S. E., Casadei, B. & Shah, A. M. Neuronal nitric oxide synthase regulates basal microvascular tone in humans in vivo. Circulation 117, 1991–1996 (2008).
Seddon, M. et al. Effects of neuronal nitric oxide synthase on human coronary artery diameter and blood flow in vivo. Circulation 119, 2656–2662 (2009).
Shabeeh, H. et al. Blood pressure in healthy humans is regulated by neuronal NO synthase. Hypertension 69, 970–976 (2017).
Thomas, G. D. et al. Impaired metabolic modulation of alpha-adrenergic vasoconstriction in dystrophin-deficient skeletal muscle. Proc. Natl Acad. Sci. USA 95, 15090–15095 (1998).
Thomas, G. D., Shaul, P. W., Yuhanna, I. S., Froehner, S. C. & Adams, M. E. Vasomodulation by skeletal muscle-derived nitric oxide requires alpha-syntrophin-mediated sarcolemmal localization of neuronal Nitric oxide synthase. Circ. Res. 92, 554–560 (2003).
Schwarz, P., Diem, R., Dun, N. J. & Forstermann, U. Endogenous and exogenous nitric oxide inhibits norepinephrine release from rat heart sympathetic nerves. Circ. Res. 77, 841–848 (1995).
Herring, N., Golding, S. & Paterson, D. J. Pre-synaptic NO-cGMP pathway modulates vagal control of heart rate in isolated adult guinea pig atria. J. Mol. Cell. Cardiol. 32, 1795–1804 (2000).
Massion, P. B. et al. Cardiomyocyte-restricted overexpression of endothelial nitric oxide synthase (NOS3) attenuates beta-adrenergic stimulation and reinforces vagal inhibition of cardiac contraction. Circulation 110, 2666–2672 (2004).
Packer, M. Neurohormonal interactions and adaptations in congestive heart failure. Circulation 77, 721–730 (1988).
Florea, V. G. & Cohn, J. N. The autonomic nervous system and heart failure. Circ. Res. 114, 1815–1826 (2014).
Soltis, E. E. & Cassis, L. A. Influence of perivascular adipose tissue on rat aortic smooth muscle responsiveness. Clin. Exp. Hypertens. A 13, 277–296 (1991).
Victorio, J. A., Fontes, M. T., Rossoni, L. V. & Davel, A. P. Different anti-contractile function and nitric oxide production of thoracic and abdominal perivascular adipose tissues. Front. Physiol. 7, 295 (2016).
Greenstein, A. S. et al. Local inflammation and hypoxia abolish the protective anticontractile properties of perivascular fat in obese patients. Circulation 119, 1661–1670 (2009).
Gil-Ortega, M. et al. Adaptative nitric oxide overproduction in perivascular adipose tissue during early diet-induced obesity. Endocrinology 151, 3299–3306 (2010).
Fang, L. et al. Hydrogen sulfide derived from periadventitial adipose tissue is a vasodilator. J. Hypertens. 27, 2174–2185 (2009).
Schleifenbaum, J. et al. Systemic peripheral artery relaxation by KCNQ channel openers and hydrogen sulfide. J. Hypertens. 28, 1875–1882 (2010).
Gao, Y. J., Lu, C., Su, L. Y., Sharma, A. M. & Lee, R. M. Modulation of vascular function by perivascular adipose tissue: the role of endothelium and hydrogen peroxide. Br. J. Pharmacol. 151, 323–331 (2007).
Lee, Y. C. et al. Role of perivascular adipose tissue-derived methyl palmitate in vascular tone regulation and pathogenesis of hypertension. Circulation 124, 1160–1171 (2011).
Lee, R. M., Lu, C., Su, L. Y. & Gao, Y. J. Endothelium-dependent relaxation factor released by perivascular adipose tissue. J. Hypertens. 27, 782–790 (2009).
Sampaio, W. O. et al. Angiotensin-(1–7) through receptor Mas mediates endothelial nitric oxide synthase activation via Akt-dependent pathways. Hypertension 49, 185–192 (2007).
Weston, A. H. et al. Stimulated release of a hyperpolarizing factor (ADHF) from mesenteric artery perivascular adipose tissue: involvement of myocyte BKCa channels and adiponectin. Br. J. Pharmacol. 169, 1500–1509 (2013).
Xi, W., Satoh, H., Kase, H., Suzuki, K. & Hattori, Y. Stimulated HSP90 binding to eNOS and activation of the PI3-Akt pathway contribute to globular adiponectin-induced NO production: vasorelaxation in response to globular adiponectin. Biochem. Biophys. Res. Commun. 332, 200–205 (2005).
Margaritis, M. et al. Interactions between vascular wall and perivascular adipose tissue reveal novel roles for adiponectin in the regulation of endothelial nitric oxide synthase function in human vessels. Circulation 127, 2209–2221 (2013).
Lundberg, J. O. et al. Nitrate and nitrite in biology, nutrition and therapeutics. Nat. Chem. Biol. 5, 865–869 (2009).
Cosby, K. et al. Nitrite reduction to nitric oxide by deoxyhemoglobin vasodilates the human circulation. Nat. Med. 9, 1498–1505 (2003).
Liu, C. et al. Mechanisms of human erythrocytic bioactivation of nitrite. J. Biol. Chem. 290, 1281–1294 (2015).
Pawloski, J. R., Hess, D. T. & Stamler, J. S. Export by red blood cells of nitric oxide bioactivity. Nature 409, 622–626 (2001).
Zhang, R. et al. Hemoglobin betaCys93 is essential for cardiovascular function and integrated response to hypoxia. Proc. Natl Acad. Sci. USA 112, 6425–6430 (2015).
Isbell, T. S. et al. SNO-hemoglobin is not essential for red blood cell-dependent hypoxic vasodilation. Nat. Med. 14, 773–777 (2008).
Lobysheva, I. I., Biller, P., Gallez, B., Beauloye, C. & Balligand, J. L. Nitrosylated hemoglobin levels in human venous erythrocytes correlate with vascular endothelial function measured by digital reactive hyperemia. PLoS ONE 8, e76457 (2013).
Lobysheva, I. I. et al. Heme-nitrosylated hemoglobin and oxidative stress in women consuming combined contraceptives. Clinical application of the EPR spectroscopy. Free Radic. Biol. Med. 108, 524–532 (2017).
Erkens, R. et al. Modulation of local and systemic heterocellular communication by mechanical forces: a role of endothelial nitric oxide synthase. Antioxid. Redox Signal. 26, 917–935 (2017).
Kuhn, V. et al. Red blood cell function and dysfunction: redox regulation, nitric oxide metabolism. Anemia. Antioxid. Redox Signal. 26, 718–742 (2017).
Zweier, J. L., Chen, C. A. & Druhan, L. J. S-Glutathionylation reshapes our understanding of endothelial nitric oxide synthase uncoupling and nitric oxide/reactive oxygen species-mediated signaling. Antioxid. Redox Signal. 14, 1769–1775 (2011).
Xia, Y., Dawson, V. L., Dawson, T. M., Snyder, S. H. & Zweier, J. L. Nitric oxide synthase generates superoxide and nitric oxide in arginine-depleted cells leading to peroxynitrite-mediated cellular injury. Proc. Natl Acad. Sci. USA 93, 6770–6774 (1996).
Xia, Y. & Zweier, J. L. Superoxide and peroxynitrite generation from inducible nitric oxide synthase in macrophages. Proc. Natl Acad. Sci. USA 94, 6954–6958 (1997).
Ramachandran, J. & Peluffo, R. D. Threshold levels of extracellular l-arginine that trigger NOS-mediated ROS/RNS production in cardiac ventricular myocytes. Am. J. Physiol. Cell Physiol. 312, C144–C154 (2017).
Antoniades, C. et al. Association of plasma asymmetrical dimethylarginine (ADMA) with elevated vascular superoxide production and endothelial nitric oxide synthase uncoupling: implications for endothelial function in human atherosclerosis. Eur. Heart J. 30, 1142–1150 (2009).
Cardounel, A. J., Xia, Y. & Zweier, J. L. Endogenous methylarginines modulate superoxide as well as nitric oxide generation from neuronal nitric-oxide synthase: differences in the effects of monomethyl- and dimethylarginines in the presence and absence of tetrahydrobiopterin. J. Biol. Chem. 280, 7540–7549 (2005).
Druhan, L. J. et al. Regulation of eNOS-derived superoxide by endogenous methylarginines. Biochemistry 47, 7256–7263 (2008).
Ryoo, S. et al. Oxidized low-density lipoprotein-dependent endothelial arginase II activation contributes to impaired nitric oxide signaling. Circ. Res. 99, 951–960 (2006).
Shemyakin, A. et al. Arginase inhibition improves endothelial function in patients with coronary artery disease and type 2 diabetes mellitus. Circulation 126, 2943–2950 (2012).
Zhou, S. et al. Asymmetric dimethylarginine and all-cause mortality: a systematic review and meta-analysis. Sci. Rep. 7, 44692 (2017).
Bendall, J. K. et al. Stoichiometric relationships between endothelial tetrahydrobiopterin, endothelial NO synthase (eNOS) activity, and eNOS coupling in vivo: insights from transgenic mice with endothelial-targeted GTP cyclohydrolase 1 and eNOS overexpression. Circ. Res. 97, 864–871 (2005).
Dumitrescu, C. et al. Myocardial ischemia results in tetrahydrobiopterin (BH4) oxidation with impaired endothelial function ameliorated by BH4. Proc. Natl Acad. Sci. USA 104, 15081–15086 (2007).
Crabtree, M. J., Tatham, A. L., Hale, A. B., Alp, N. J. & Channon, K. M. Critical role for tetrahydrobiopterin recycling by dihydrofolate reductase in regulation of endothelial nitric-oxide synthase coupling: relative importance of the de novo biopterin synthesis versus salvage pathways. J. Biol. Chem. 284, 28128–28136 (2009).
Moens, A. L. et al. Bi-modal dose-dependent cardiac response to tetrahydrobiopterin in pressure-overload induced hypertrophy and heart failure. J. Mol. Cell. Cardiol. 51, 564–569 (2011).
Reilly, S. N. et al. Atrial sources of reactive oxygen species vary with the duration and substrate of atrial fibrillation: implications for the antiarrhythmic effect of statins. Circulation 124, 1107–1117 (2011).
Schmidt, T. S. & Alp, N. J. Mechanisms for the role of tetrahydrobiopterin in endothelial function and vascular disease. Clin. Sci. 113, 47–63 (2007).
Moens, A. L. et al. Reversal of cardiac hypertrophy and fibrosis from pressure overload by tetrahydrobiopterin: efficacy of recoupling nitric oxide synthase as a therapeutic strategy. Circulation 117, 2626–2636 (2008).
Nishijima, Y. et al. Tetrahydrobiopterin depletion and NOS2 uncoupling contribute to heart failure-induced alterations in atrial electrophysiology. Cardiovasc. Res. 91, 71–79 (2011).
Tiefenbacher, C. P. et al. Endothelial dysfunction of coronary resistance arteries is improved by tetrahydrobiopterin in atherosclerosis. Circulation 102, 2172–2179 (2000).
Alp, N. J. et al. Tetrahydrobiopterin-dependent preservation of nitric oxide-mediated endothelial function in diabetes by targeted transgenic GTP-cyclohydrolase I overexpression. J. Clin. Invest. 112, 725–735 (2003).
Chen, W. et al. Peroxynitrite induces destruction of the tetrahydrobiopterin and heme in endothelial nitric oxide synthase: transition from reversible to irreversible enzyme inhibition. Biochemistry 49, 3129–3137 (2010).
Reyes, L. A. et al. Depletion of NADP(H) due to CD38 activation triggers endothelial dysfunction in the postischemic heart. Proc. Natl Acad. Sci. USA 112, 11648–11653 (2015).
Kojima, S. et al. Antioxidative activity of 5,6,7,8-tetrahydrobiopterin and its inhibitory effect on paraquat-induced cell toxicity in cultured rat hepatocytes. Free Radic. Res. 23, 419–430 (1995).
Bailey, J. et al. A novel role for endothelial tetrahydrobiopterin in mitochondrial redox balance. Free Radic. Biol. Med. 104, 214–225 (2017).
Antoniades, C. et al. Induction of vascular GTP-cyclohydrolase I and endogenous tetrahydrobiopterin synthesis protect against inflammation-induced endothelial dysfunction in human atherosclerosis. Circulation 124, 1860–1870 (2011).
Hashimoto, T. et al. Tetrahydrobiopterin protects against hypertrophic heart disease independent of myocardial nitric oxide synthase coupling. J. Am. Heart Assoc. 5, e003208 (2016).
Chen, Z. et al. Shear stress, SIRT1, and vascular homeostasis. Proc. Natl Acad. Sci. USA 107, 10268–10273 (2010).
Maizel, J. et al. Sirtuin 1 ablation in endothelial cells is associated with impaired angiogenesis and diastolic dysfunction. Am. J. Physiol. Heart Circ. Physiol. 307, H1691–H1704 (2014).
Nagar, H. et al. CR6-interacting factor 1 deficiency impairs vascular function by inhibiting the Sirt1-endothelial nitric oxide synthase pathway. Antioxid. Redox Signal. 27, 234–249 (2017).
Charles, S., Raj, V., Arokiaraj, J. & Mala, K. Caveolin1/protein arginine methyltransferase1/sirtuin1 axis as a potential target against endothelial dysfunction. Pharmacol. Res. 119, 1–11 (2017).
Sharina, I. G. & Martin, E. The role of reactive oxygen and nitrogen species in the expression and splicing of nitric oxide receptor. Antioxid. Redox Signal. 26, 122–136 (2017).
Stasch, J. P. et al. Targeting the heme-oxidized nitric oxide receptor for selective vasodilatation of diseased blood vessels. J. Clin. Invest. 116, 2552–2561 (2006).
Ghosh, A. et al. Soluble guanylate cyclase as an alternative target for bronchodilator therapy in asthma. Proc. Natl Acad. Sci. USA 113, E2355–2362 (2016).
Rahaman, M. M. et al. Cytochrome b5 reductase 3 modulates soluble guanylate cyclase redox state and cGMP signaling. Circ. Res. 121, 137–148 (2017).
Thoonen, R. et al. Cardiovascular and pharmacological implications of haem-deficient NO-unresponsive soluble guanylate cyclase knock-in mice. Nat. Commun. 6, 8482 (2015).
Fernhoff, N. B., Derbyshire, E. R., Underbakke, E. S. & Marletta, M. A. Heme-assisted S-nitrosation desensitizes ferric soluble guanylate cyclase to nitric oxide. J. Biol. Chem. 287, 43053–43062 (2012).
Sayed, N. et al. Nitroglycerin-induced S-nitrosylation and desensitization of soluble guanylyl cyclase contribute to nitrate tolerance. Circ. Res. 103, 606–614 (2008).
Huang, C. et al. Guanylyl cyclase sensitivity to nitric oxide is protected by a thiol oxidation-driven interaction with thioredoxin-1. J. Biol. Chem. 292, 14362–14370 (2017).
Yasmin, W., Strynadka, K. D. & Schulz, R. Generation of peroxynitrite contributes to ischemia-reperfusion injury in isolated rat hearts. Cardiovasc. Res. 33, 422–432 (1997).
Saraiva, R. M. et al. Deficiency of neuronal nitric oxide synthase increases mortality and cardiac remodeling after myocardial infarction: role of nitroso-redox equilibrium. Circulation 112, 3415–3422 (2005).
Dawson, D. et al. nNOS gene deletion exacerbates pathological left ventricular remodeling and functional deterioration after myocardial infarction. Circulation 112, 3729–3737 (2005).
Burger, D. E. et al. Neuronal nitric oxide synthase protects against myocardial infarction-induced ventricular arrhythmia and mortality in mice. Circulation 120, 1345–1354 (2009).
Brunner, F. et al. Attenuation of myocardial ischemia/reperfusion injury in mice with myocyte-specific overexpression of endothelial nitric oxide synthase. Cardiovasc. Res. 57, 55–62 (2003).
Elrod, J. W. et al. Cardiomyocyte-specific overexpression of NO synthase-3 protects against myocardial ischemia-reperfusion injury. Arterioscler. Thromb. Vasc. Biol. 26, 1517–1523 (2006).
Szelid, Z. et al. Cardioselective nitric oxide synthase 3 gene transfer protects against myocardial reperfusion injury. Bas. Res. Cardiol. 105, 169–179 (2010).
Janssens, S. et al. Cardiomyocyte-specific overexpression of nitric oxide synthase 3 improves left ventricular performance and reduces compensatory hypertrophy after myocardial infarction. Circ. Res. 94, 1256–1262 (2004).
Burkard, N. et al. Conditional overexpression of neuronal nitric oxide synthase is cardioprotective in ischemia/reperfusion. Circulation 122, 1588–1603 (2010).
Korge, P., Ping, P. & Weiss, J. N. Reactive oxygen species production in energized cardiac mitochondria during hypoxia/reoxygenation: modulation by nitric oxide. Circ. Res. 103, 873–880 (2008).
Heusch, G., Boengler, K. & Schulz, R. Cardioprotection: nitric oxide, protein kinases, and mitochondria. Circulation 118, 1915–1919 (2008).
Wang, P. & Zweier, J. L. Measurement of nitric oxide and peroxynitrite generation in the postischemic heart. Evidence for peroxynitrite-mediated reperfusion injury. J. Biol. Chem. 271, 29223–29230 (1996).
Flogel, U., Decking, U. K., Godecke, A. & Schrader, J. Contribution of NO to ischemia-reperfusion injury in the saline-perfused heart: a study in endothelial NO synthase knockout mice. J. Mol. Cell. Cardiol. 31, 827–836 (1999).
Csonka, C. et al. Classic preconditioning decreases the harmful accumulation of nitric oxide during ischemia and reperfusion in rat hearts. Circulation 100, 2260–2266 (1999).
de Waard, M. C. et al. Detrimental effect of combined exercise training and eNOS overexpression on cardiac function after myocardial infarction. Am. J. Physiol. Heart Circ. Physiol. 296, H1513–H1523 (2009).
Wajima, T., Shimizu, S., Hiroi, T., Ishii, M. & Kiuchi, Y. Reduction of myocardial infarct size by tetrahydrobiopterin: possible involvement of mitochondrial KATP channels activation through nitric oxide production. J. Cardiovasc. Pharmacol. 47, 243–249 (2006).
Xie, L., Talukder, M. A., Sun, J., Varadharaj, S. & Zweier, J. L. Liposomal tetrahydrobiopterin preserves eNOS coupling in the post-ischemic heart conferring in vivo cardioprotection. J. Mol. Cell. Cardiol. 86, 14–22 (2015).
Zhang, P. et al. Inducible nitric oxide synthase deficiency protects the heart from systolic overload-induced ventricular hypertrophy and congestive heart failure. Circ. Res. 100, 1089–1098 (2007).
Sam, F. et al. Mice lacking inducible nitric oxide synthase have improved left ventricular contractile function and reduced apoptotic cell death late after myocardial infarction. Circ. Res. 89, 351–356 (2001).
Feng, Q., Lu, X., Jones, D. L., Shen, J. & Arnold, J. M. Increased inducible nitric oxide synthase expression contributes to myocardial dysfunction and higher mortality after myocardial infarction in mice. Circulation 104, 700–704 (2001).
West, M. B. et al. Cardiac myocyte-specific expression of inducible nitric oxide synthase protects against ischemia/reperfusion injury by preventing mitochondrial permeability transition. Circulation 118, 1970–1978 (2008).
Guo, Y. et al. The late phase of ischemic preconditioning is abrogated by targeted disruption of the inducible NO synthase gene. Proc. Natl Acad. Sci. USA 96, 11507–11512 (1999).
Bolli, R. Cardioprotective function of inducible nitric oxide synthase and role of nitric oxide in myocardial ischemia and preconditioning: an overview of a decade of research. J. Mol. Cell. Cardiol. 33, 1897–1918 (2001).
Yang, C., Talukder, M. A., Varadharaj, S., Velayutham, M. & Zweier, J. L. Early ischaemic preconditioning requires Akt- and PKA-mediated activation of eNOS via serine1176 phosphorylation. Cardiovasc. Res. 97, 33–43 (2013).
Wang, Y., Kudo, M., Xu, M., Ayub, A. & Ashraf, M. Mitochondrial K(ATP) channel as an end effector of cardioprotection during late preconditioning: triggering role of nitric oxide. J. Mol. Cell. Cardiol. 33, 2037–2046 (2001).
Sun, J., Morgan, M., Shen, R. F., Steenbergen, C. & Murphy, E. Preconditioning results in S-nitrosylation of proteins involved in regulation of mitochondrial energetics and calcium transport. Circ. Res. 101, 1155–1163 (2007).
Chouchani, E. T. et al. Identification and quantification of protein S-nitrosation by nitrite in the mouse heart during ischemia. J. Biol. Chem. 292, 14486–14495 (2017).
Takimoto, E. et al. Oxidant stress from nitric oxide synthase-3 uncoupling stimulates cardiac pathologic remodeling from chronic pressure load. J. Clin. Invest. 115, 1221–1231 (2005).
van Deel, E. D. et al. Normal and high eNOS levels are detrimental in both mild and severe cardiac pressure-overload. J. Mol. Cell. Cardiol. 88, 145–154 (2015).
Loyer, X. et al. Cardiomyocyte overexpression of neuronal nitric oxide synthase delays transition toward heart failure in response to pressure overload by preserving calcium cycling. Circulation 117, 3187–3198 (2008).
Hermida, N. et al. Cardiac myocyte b3-adrenergic receptors prevent myocardial fibrosis by modulating oxidant stress-dependent paracrine signaling. Eur. Heart J. http://dx.doi.org/10.1093/eurheartj/ehx366 (2017).
Niu, X. et al. Cardioprotective effect of beta-3 adrenergic receptor agonism: role of neuronal nitric oxide synthase. J. Am. Coll. Cardiol. 59, 1979–1987 (2012).
Belge, C. et al. Enhanced expression of beta3-adrenoceptors in cardiac myocytes attenuates neurohormone-induced hypertrophic remodeling through nitric oxide synthase. Circulation 129, 451–462 (2014).
Davignon, J. & Ganz, P. Role of endothelial dysfunction in atherosclerosis. Circulation 109, III-27–III-32 (2004).
Forstermann, U., Xia, N. & Li, H. Roles of vascular oxidative stress and nitric oxide in the pathogenesis of atherosclerosis. Circ. Res. 120, 713–735 (2017).
Panza, J. A., Quyyumi, A. A., Brush, J. E. Jr & Epstein, S. E. Abnormal endothelium-dependent vascular relaxation in patients with essential hypertension. N. Engl. J. Med. 323, 22–27 (1990).
Panza, J. A., Casino, P. R., Kilcoyne, C. M. & Quyyumi, A. A. Role of endothelium-derived nitric oxide in the abnormal endothelium-dependent vascular relaxation of patients with essential hypertension. Circulation 87, 1468–1474 (1993).
Huang, P. L. et al. Hypertension in mice lacking the gene for endothelial nitric oxide synthase. Nature 377, 239–242 (1995).
Paolocci, N. et al. Oxygen radical-mediated reduction in basal and agonist-evoked NO release in isolated rat heart. J. Mol. Cell. Cardiol. 33, 671–679 (2001).
Li, H. et al. Reversal of endothelial nitric oxide synthase uncoupling and up-regulation of endothelial nitric oxide synthase expression lowers blood pressure in hypertensive rats. J. Am. Coll. Cardiol. 47, 2536–2544 (2006).
Alp, N. J., McAteer, M. A., Khoo, J., Choudhury, R. P. & Channon, K. M. Increased endothelial tetrahydrobiopterin synthesis by targeted transgenic GTP-cyclohydrolase I overexpression reduces endothelial dysfunction and atherosclerosis in ApoE-knockout mice. Arterioscler. Thromb. Vasc. Biol. 24, 445–450 (2004).
Antoniades, C. et al. Altered plasma versus vascular biopterins in human atherosclerosis reveal relationships between endothelial nitric oxide synthase coupling, endothelial function, and inflammation. Circulation 116, 2851–2859 (2007).
Lobysheva, I. et al. Moderate caveolin-1 downregulation prevents NADPH oxidase-dependent endothelial nitric oxide synthase uncoupling by angiotensin II in endothelial cells. Arterioscler. Thromb. Vasc. Biol. 31, 2098–2105 (2011).
Zhang, Q. J. et al. Endothelium-specific overexpression of class III deacetylase SIRT1 decreases atherosclerosis in apolipoprotein E-deficient mice. Cardiovasc. Res. 80, 191–199 (2008).
Kadlec, A. O. et al. PGC-1alpha (peroxisome proliferator-activated receptor gamma coactivator 1-alpha) overexpression in coronary artery disease recruits NO and hydrogen peroxide during flow-mediated dilation and protects against increased intraluminal pressure. Hypertension 70, 166–173 (2017).
Kuhlencordt, P. J. et al. Atheroprotective effects of neuronal nitric oxide synthase in apolipoprotein e knockout mice. Arterioscler. Thromb. Vasc. Biol. 26, 1539–1544 (2006).
Campos-Mota, G. P., Navia-Pelaez, J. M., Araujo-Souza, J. C., Stergiopulos, N. & Capettini, L. S. A. Role of ERK1/2 activation and nNOS uncoupling on endothelial dysfunction induced by lysophosphatidylcholine. Atherosclerosis 258, 108–118 (2017).
Kuhlencordt, P. J., Chen, J., Han, F., Astern, J. & Huang, P. L. Genetic deficiency of inducible nitric oxide synthase reduces atherosclerosis and lowers plasma lipid peroxides in apolipoprotein E-knockout mice. Circulation 103, 3099–3104 (2001).
Reventun, P. et al. iNOS-derived nitric oxide induces integrin-linked kinase endocytic lysosome-mediated degradation in the vascular endothelium. Arterioscler. Thromb. Vasc. Biol. 37, 1272–1281 (2017).
Herranz, B. et al. Integrin-linked kinase regulates vasomotor function by preventing endothelial nitric oxide synthase uncoupling: role in atherosclerosis. Circ. Res. 110, 439–449 (2012).
Cannon, B. & Nedergaard, J. Brown adipose tissue: function and physiological significance. Physiol. Rev. 84, 277–359 (2004).
Vegiopoulos, A. et al. Cyclooxygenase-2 controls energy homeostasis in mice by de novo recruitment of brown adipocytes. Science 328, 1158–1161 (2010).
Takx, R. A. et al. Supraclavicular brown adipose tissue 18F-FDG uptake and cardiovascular disease. J. Nuclear Med. 57, 1221–1225 (2016).
Franssens, B. T., Hoogduin, H., Leiner, T., van der Graaf, Y. & Visseren, F. L. J. Relation between brown adipose tissue and measures of obesity and metabolic dysfunction in patients with cardiovascular disease. J. Magn. Reson. Imag. 46, 497–504 (2017).
Chondronikola, M. et al. Brown adipose tissue improves whole-body glucose homeostasis and insulin sensitivity in humans. Diabetes 63, 4089–4099 (2014).
Lee, P. et al. Temperature-acclimated brown adipose tissue modulates insulin sensitivity in humans. Diabetes 63, 3686–3698 (2014).
Valerio, A. et al. TNF-alpha downregulates eNOS expression and mitochondrial biogenesis in fat and muscle of obese rodents. J. Clin. Invest. 116, 2791–2798 (2006).
Wisloff, U. et al. Cardiovascular risk factors emerge after artificial selection for low aerobic capacity. Science 307, 418–420 (2005).
Nisoli, E. et al. Mitochondrial biogenesis in mammals: the role of endogenous nitric oxide. Science 299, 896–899 (2003).
Haas, B. et al. Protein kinase G controls brown fat cell differentiation and mitochondrial biogenesis. Sci. Signal. 2, ra78 (2009).
Kikuchi-Utsumi, K. et al. Enhanced gene expression of endothelial nitric oxide synthase in brown adipose tissue during cold exposure. Am. J. Physiol. Regul. Integr. Comp. Physiol. 282, R623–R626 (2002).
Oguri, Y. et al. Tetrahydrobiopterin activates brown adipose tissue and regulates systemic energy metabolism. JCI Insight http://dx.doi.org/10.1172/jci.insight.91981 (2017).
Nisoli, E. et al. Effects of nitric oxide on proliferation and differentiation of rat brown adipocytes in primary cultures. Br. J. Pharmacol. 125, 888–894 (1998).
Roberts, L. D. et al. Inorganic nitrate promotes the browning of white adipose tissue through the nitrate-nitrite-nitric oxide pathway. Diabetes 64, 471–484 (2015).
Miller, M. W. et al. Nitric oxide regulates vascular adaptive mitochondrial dynamics. Am. J. Physiol. Heart Circ. Physiol. 304, H1624–1633 (2013).
Nisoli, E. et al. Mitochondrial biogenesis by NO yields functionally active mitochondria in mammals. Proc. Natl Acad. Sci. USA 101, 16507–16512 (2004).
Wu, Z. et al. Mechanisms controlling mitochondrial biogenesis and respiration through the thermogenic coactivator PGC-1. Cell 98, 115–124 (1999).
Lehman, J. J. et al. Peroxisome proliferator-activated receptor gamma coactivator-1 promotes cardiac mitochondrial biogenesis. J. Clin. Invest. 106, 847–856 (2000).
Nisoli, E. et al. Calorie restriction promotes mitochondrial biogenesis by inducing the expression of eNOS. Science 310, 314–317 (2005).
Vettor, R. et al. Exercise training boosts eNOS-dependent mitochondrial biogenesis in mouse heart: role in adaptation of glucose metabolism. Am. J. Physiol. Endocrinol. Metab. 306, E519–E528 (2014).
D'Antona, G. et al. Branched-chain amino acid supplementation promotes survival and supports cardiac and skeletal muscle mitochondrial biogenesis in middle-aged mice. Cell. Metab. 12, 362–372 (2010).
Xia, N. et al. Uncoupling of endothelial nitric oxide synthase in perivascular adipose tissue of diet-induced obese mice. Arterioscler. Thromb. Vasc. Biol. 36, 78–85 (2016).
Xia, N. et al. Restoration of perivascular adipose tissue function in diet-induced obese mice without changing bodyweight. Br. J. Pharmacol. 174, 3443–3453 (2017).
Aghamohammadzadeh, R. et al. Effects of bariatric surgery on human small artery function: evidence for reduction in perivascular adipocyte inflammation, and the restoration of normal anticontractile activity despite persistent obesity. J. Am. Coll. Cardiol. 62, 128–135 (2013).
Virdis, A. et al. Tumour necrosis factor-alpha participates on the endothelin-1/nitric oxide imbalance in small arteries from obese patients: role of perivascular adipose tissue. Eur. Heart J. 36, 784–794 (2015).
Zweier, J. L., Wang, P., Samouilov, A. & Kuppusamy, P. Enzyme-independent formation of nitric oxide in biological tissues. Nat. Med. 1, 804–809 (1995).
Duncan, C. et al. Chemical generation of nitric oxide in the mouth from the enterosalivary circulation of dietary nitrate. Nat. Med. 1, 546–551 (1995).
Benjamin, N. et al. Stomach NO synthesis. Nature 368, 502 (1994).
Lundberg, J. O., Weitzberg, E., Lundberg, J. M. & Alving, K. Intragastric nitric oxide production in humans: measurements in expelled air. Gut 35, 1543–1546 (1994).
Gladwin, M. T. et al. Role of circulating nitrite and S-nitrosohemoglobin in the regulation of regional blood flow in humans. Proc. Natl Acad. Sci. USA 97, 11482–11487 (2000).
Huang, Z. et al. Enzymatic function of hemoglobin as a nitrite reductase that produces NO under allosteric control. J. Clin. Invest. 115, 2099–2107 (2005).
Shiva, S. et al. Deoxymyoglobin is a nitrite reductase that generates nitric oxide and regulates mitochondrial respiration. Circ. Res. 100, 654–661 (2007).
Ormerod, J. O. et al. The role of vascular myoglobin in nitrite-mediated blood vessel relaxation. Cardiovasc. Res. 89, 560–565 (2011).
Rassaf, T. et al. Nitrite reductase function of deoxymyoglobin: oxygen sensor and regulator of cardiac energetics and function. Circ. Res. 100, 1749–1754 (2007).
Li, H., Samouilov, A., Liu, X. & Zweier, J. L. Characterization of the magnitude and kinetics of xanthine oxidase-catalyzed nitrite reduction. Evaluation of its role in nitric oxide generation in anoxic tissues. J. Biol. Chem. 276, 24482–24489 (2001).
Webb, A. J. et al. Mechanisms underlying erythrocyte and endothelial nitrite reduction to nitric oxide in hypoxia: role for xanthine oxidoreductase and endothelial nitric oxide synthase. Circ. Res. 103, 957–964 (2008).
Li, H., Kundu, T. K. & Zweier, J. L. Characterization of the magnitude and mechanism of aldehyde oxidase-mediated nitric oxide production from nitrite. J. Biol. Chem. 284, 33850–33858 (2009).
Castello, P. R., David, P. S., McClure, T., Crook, Z. & Poyton, R. O. Mitochondrial cytochrome oxidase produces nitric oxide under hypoxic conditions: implications for oxygen sensing and hypoxic signaling in eukaryotes. Cell. Metab. 3, 277–287 (2006).
Vanin, A. F., Bevers, L. M., Slama-Schwok, A. & van Faassen, E. E. Nitric oxide synthase reduces nitrite to NO under anoxia. Cell. Mol. Life Sci. 64, 96–103 (2007).
Gautier, C., van Faassen, E., Mikula, I., Martasek, P. & Slama-Schwok, A. Endothelial nitric oxide synthase reduces nitrite anions to NO under anoxia. Biochem. Biophys. Res. Commun. 341, 816–821 (2006).
Modin, A. et al. Nitrite-derived nitric oxide: a possible mediator of 'acidic-metabolic' vasodilation. Acta Physiol. Scand. 171, 9–16 (2001).
Larsen, F. J., Ekblom, B., Sahlin, K., Lundberg, J. O. & Weitzberg, E. Effects of dietary nitrate on blood pressure in healthy volunteers. N. Engl. J. Med. 355, 2792–2793 (2006).
Kapil, V., Khambata, R. S., Robertson, A., Caulfield, M. J. & Ahluwalia, A. Dietary nitrate provides sustained blood pressure lowering in hypertensive patients: a randomized, phase 2, double-blind, placebo-controlled study. Hypertension 65, 320–327 (2015).
Velmurugan, S. et al. Antiplatelet effects of dietary nitrate in healthy volunteers: involvement of cGMP and influence of sex. Free Radic. Biol. Med. 65, 1521–1532 (2013).
Webb, A. J. et al. Acute blood pressure lowering, vasoprotective, and antiplatelet properties of dietary nitrate via bioconversion to nitrite. Hypertension 51, 784–790 (2008).
Bhushan, S. et al. Nitrite therapy improves left ventricular function during heart failure via restoration of nitric oxide-mediated cytoprotective signaling. Circ. Res. 114, 1281–1291 (2014).
Duranski, M. R. et al. Cytoprotective effects of nitrite during in vivo ischemia-reperfusion of the heart and liver. J. Clin. Invest. 115, 1232–1240 (2005).
Baker, J. E. et al. Nitrite confers protection against myocardial infarction: role of xanthine oxidoreductase, NADPH oxidase and K(ATP) channels. J. Mol. Cell. Cardiol. 43, 437–444 (2007).
Webb, A. et al. Reduction of nitrite to nitric oxide during ischemia protects against myocardial ischemia-reperfusion damage. Proc. Natl Acad. Sci. USA 101, 13683–13688 (2004).
Rassaf, T. et al. Circulating nitrite contributes to cardioprotection by remote ischemic preconditioning. Circ. Res. 114, 1601–1610 (2014).
Ingram, T. E. et al. Low-dose sodium nitrite attenuates myocardial ischemia and vascular ischemia-reperfusion injury in human models. J. Am. Coll. Cardiol. 61, 2534–2541 (2013).
Hendgen-Cotta, U. B. et al. Nitrite reductase activity of myoglobin regulates respiration and cellular viability in myocardial ischemia-reperfusion injury. Proc. Natl Acad. Sci. USA 105, 10256–10261 (2008).
Hendgen-Cotta, U. B. et al. Dietary nitrate supplementation improves revascularization in chronic ischemia. Circulation 126, 1983–1992 (2012).
Borlaug, B. A. et al. Global cardiovascular reserve dysfunction in heart failure with preserved ejection fraction. J. Am. Coll. Cardiol. 56, 845–854 (2010).
van Heerebeek, L. et al. Low myocardial protein kinase G activity in heart failure with preserved ejection fraction. Circulation 126, 830–839 (2012).
Borlaug, B. A., Koepp, K. E. & Melenovsky, V. Sodium nitrite improves exercise hemodynamics and ventricular performance in heart failure with preserved ejection fraction. J. Am. Coll. Cardiol. 66, 1672–1682 (2015).
Zamani, P. et al. Effect of inorganic nitrate on exercise capacity in heart failure with preserved ejection fraction. Circulation 131, 371–380 (2015).
Catry, E. et al. Targeting the gut microbiota with inulin-type fructans: preclinical demonstration of a novel approach in the management of endothelial dysfunction. Gut http://dx.doi.org/10.1136/gutjnl-2016-313316 (2017).
Oller, J. et al. Nitric oxide mediates aortic disease in mice deficient in the metalloprotease Adamts1 and in a mouse model of Marfan syndrome. Nat. Med. 23, 200–212 (2017).
Shen, J. S. et al. Tetrahydrobiopterin deficiency in the pathogenesis of Fabry disease. Hum. Mol. Genet. 26, 1182–1192 (2017).
Galie, N. et al. Sildenafil citrate therapy for pulmonary arterial hypertension. N. Engl. J. Med. 353, 2148–2157 (2005).
Galie, N. et al. Tadalafil therapy for pulmonary arterial hypertension. Circulation 119, 2894–2903 (2009).
Shan, X. et al. Differential expression of PDE5 in failing and nonfailing human myocardium. Circ. Heart Fail. 5, 79–86 (2012).
Lu, Z. et al. Oxidative stress regulates left ventricular PDE5 expression in the failing heart. Circulation 121, 1474–1483 (2010).
Salloum, F. N. et al. Phosphodiesterase-5 inhibitor, tadalafil, protects against myocardial ischemia/reperfusion through protein-kinase G-dependent generation of hydrogen sulfide. Circulation 120, S31–36 (2009).
Ahmad, N., Wang, Y., Ali, A. K. & Ashraf, M. Long-acting phosphodiesterase-5 inhibitor, tadalafil, induces sustained cardioprotection against lethal ischemic injury. Am. J. Physiol. Heart Circ. Physiol. 297, H387–H391 (2009).
Andersen, M. J. et al. Sildenafil and diastolic dysfunction after acute myocardial infarction in patients with preserved ejection fraction: the Sildenafil and Diastolic Dysfunction After Acute Myocardial Infarction (SIDAMI) trial. Circulation 127, 1200–1208 (2013).
Takimoto, E. et al. Chronic inhibition of cyclic GMP phosphodiesterase 5A prevents and reverses cardiac hypertrophy. Nat. Med. 11, 214–222 (2005).
Takimoto, E. et al. Regulator of G protein signaling 2 mediates cardiac compensation to pressure overload and antihypertrophic effects of PDE5 inhibition in mice. J. Clin. Invest. 119, 408–420 (2009).
Guazzi, M., Vicenzi, M., Arena, R. & Guazzi, M. D. PDE5 inhibition with sildenafil improves left ventricular diastolic function, cardiac geometry, and clinical status in patients with stable systolic heart failure: results of a 1-year, prospective, randomized, placebo-controlled study. Circ. Heart Fail. 4, 8–17 (2011).
Lewis, G. D. et al. Sildenafil improves exercise capacity and quality of life in patients with systolic heart failure and secondary pulmonary hypertension. Circulation 116, 1555–1562 (2007).
Guazzi, M., Tumminello, G., Di Marco, F., Fiorentini, C. & Guazzi, M. D. The effects of phosphodiesterase-5 inhibition with sildenafil on pulmonary hemodynamics and diffusion capacity, exercise ventilatory efficiency, and oxygen uptake kinetics in chronic heart failure. J. Am. Coll. Cardiol. 44, 2339–2348 (2004).
Giannetta, E. et al. Is chronic inhibition of phosphodiesterase type 5 cardioprotective and safe? A meta-analysis of randomized controlled trials. BMC Med. 12, 185 (2014).
Guazzi, M., Vicenzi, M., Arena, R. & Guazzi, M. D. Pulmonary hypertension in heart failure with preserved ejection fraction: a target of phosphodiesterase-5 inhibition in a 1-year study. Circulation 124, 164–174 (2011).
Melenovsky, V., Hwang, S. J., Lin, G., Redfield, M. M. & Borlaug, B. A. Right heart dysfunction in heart failure with preserved ejection fraction. Eur. Heart J. 35, 3452–3462 (2014).
Redfield, M. M. et al. Effect of phosphodiesterase-5 inhibition on exercise capacity and clinical status in heart failure with preserved ejection fraction: a randomized clinical trial. JAMA 309, 1268–1277 (2013).
Hoendermis, E. S. et al. Effects of sildenafil on invasive haemodynamics and exercise capacity in heart failure patients with preserved ejection fraction and pulmonary hypertension: a randomized controlled trial. Eur. Heart J. 36, 2565–2573 (2015).
Borlaug, B. A. et al. Effects of sildenafil on ventricular and vascular function in heart failure with preserved ejection fraction. Circ. Heart Fail. 8, 533–541 (2015).
Brutsaert, D. L. & De Keulenaer, G. W. Letter by Brutsaert and De Keulenaer regarding article, “Effects of sildenafil on ventricular and vascular function in heart failure with preserved ejection fraction”. Circ. Heart Fail. 8, 839 (2015).
Balligand, J. L. & Hammond, J. Protein kinase G type I in cardiac myocytes: unmasked at last? Eur. Heart J. 34, 1181–1185 (2013).
Tobler, D. et al. Effect of phosphodiesterase-5 inhibition with Tadalafil on SystEmic Right VEntricular size and function - A multi-center, double-blind, randomized, placebo-controlled clinical trial — SERVE trial — Rational and design. Int. J. Cardiol. 243, 354–359 (2017).
Ko, F. N., Wu, C. C., Kuo, S. C., Lee, F. Y. & Teng, C. M. YC-1, a novel activator of platelet guanylate cyclase. Blood 84, 4226–4233 (1994).
Stasch, J. P. et al. NO- and haem-independent activation of soluble guanylyl cyclase: molecular basis and cardiovascular implications of a new pharmacological principle. Br. J. Pharmacol. 136, 773–783 (2002).
Gheorghiade, M. et al. Cinaciguat, a soluble guanylate cyclase activator: results from the randomized, controlled, phase IIb COMPOSE programme in acute heart failure syndromes. Eur. J. Heart Fail. 14, 1056–1066 (2012).
Erdmann, E. et al. Cinaciguat, a soluble guanylate cyclase activator, unloads the heart but also causes hypotension in acute decompensated heart failure. Eur. Heart J. 34, 57–67 (2013).
Ghofrani, H. A. et al. Riociguat for the treatment of chronic thromboembolic pulmonary hypertension. N. Engl. J. Med. 369, 319–329 (2013).
Rubin, L. J. et al. Riociguat for the treatment of pulmonary arterial hypertension: a long-term extension study (PATENT-2). Eur. Respir. J. 45, 1303–1313 (2015).
Simonneau, G. et al. Incident and prevalent cohorts with pulmonary arterial hypertension: insight from SERAPHIN. Eur. Respir. J. 46, 1711–1720 (2015).
Bonderman, D. et al. Acute hemodynamic effects of riociguat in patients with pulmonary hypertension associated with diastolic heart failure (DILATE-1): a randomized, double-blind, placebo-controlled, single-dose study. Chest 146, 1274–1285 (2014).
Bonderman, D. et al. Riociguat for patients with pulmonary hypertension caused by systolic left ventricular dysfunction: a phase IIb double-blind, randomized, placebo-controlled, dose-ranging hemodynamic study. Circulation 128, 502–511 (2013).
Gheorghiade, M. et al. Effect of vericiguat, a soluble guanylate cyclase stimulator, on natriuretic peptide levels in patients with worsening chronic heart failure and reduced ejection fraction: the SOCRATES-REDUCED randomized trial. JAMA 314, 2251–2262 (2015).
Pieske, B. et al. Rationale and design of the SOluble guanylate Cyclase stimulatoR in heArT failurE Studies (SOCRATES). Eur. J. Heart Fail. 16, 1026–1038 (2014).
Pieske, B. et al. Vericiguat in patients with worsening chronic heart failure and preserved ejection fraction: results of the SOluble guanylate Cyclase stimulatoR in heArT failurE patientS with PRESERVED EF (SOCRATES-PRESERVED) study. Eur. Heart J. 38, 1119–1127 (2017).
Heitzer, T., Krohn, K., Albers, S. & Meinertz, T. Tetrahydrobiopterin improves endothelium-dependent vasodilation by increasing nitric oxide activity in patients with type II diabetes mellitus. Diabetologia 43, 1435–1438 (2000).
Porkert, M. et al. Tetrahydrobiopterin: a novel antihypertensive therapy. J. Hum. Hypertens. 22, 401–407 (2008).
Cunnington, C. et al. Systemic and vascular oxidation limits the efficacy of oral tetrahydrobiopterin treatment in patients with coronary artery disease. Circulation 125, 1356–1366 (2012).
Hao, L. et al. Folate status and homocysteine response to folic acid doses and withdrawal among young Chinese women in a large-scale randomized double-blind trial. Am. J. Clin. Nutr. 88, 448–457 (2008).
Gao, L., Chalupsky, K., Stefani, E. & Cai, H. Mechanistic insights into folic acid-dependent vascular protection: dihydrofolate reductase (DHFR)-mediated reduction in oxidant stress in endothelial cells and angiotensin II-infused mice: a novel HPLC-based fluorescent assay for DHFR activity. J. Mol. Cell. Cardiol. 47, 752–760 (2009).
Crabtree, M. J. & Channon, K. M. Synthesis and recycling of tetrahydrobiopterin in endothelial function and vascular disease. Nitric Oxide 25, 81–88 (2011).
Joshi, R., Adhikari, S., Patro, B. S., Chattopadhyay, S. & Mukherjee, T. Free radical scavenging behavior of folic acid: evidence for possible antioxidant activity. Free Radic. Biol. Med. 30, 1390–1399 (2001).
Antoniades, C. et al. 5-Methyltetrahydrofolate rapidly improves endothelial function and decreases superoxide production in human vessels: effects on vascular tetrahydrobiopterin availability and endothelial nitric oxide synthase coupling. Circulation 114, 1193–1201 (2006).
Chalupsky, K., Kracun, D., Kanchev, I., Bertram, K. & Gorlach, A. Folic acid promotes recycling of tetrahydrobiopterin and protects against hypoxia-induced pulmonary hypertension by recoupling endothelial nitric oxide synthase. Antioxid. Redox Signal. 23, 1076–1091 (2015).
Shirodaria, C. et al. Global improvement of vascular function and redox state with low-dose folic acid: implications for folate therapy in patients with coronary artery disease. Circulation 115, 2262–2270 (2007).
Doshi, S. N. et al. Folic acid improves endothelial function in coronary artery disease via mechanisms largely independent of homocysteine lowering. Circulation 105, 22–26 (2002).
Tucker, K. L., Mahnken, B., Wilson, P. W., Jacques, P. & Selhub, J. Folic acid fortification of the food supply. Potential benefits and risks for the elderly population. JAMA 276, 1879–1885 (1996).
Gori, T. et al. Folic acid prevents nitroglycerin-induced nitric oxide synthase dysfunction and nitrate tolerance: a human in vivo study. Circulation 104, 1119–1123 (2001).
Title, L. M., Cummings, P. M., Giddens, K., Genest, J. J. Jr & Nassar, B. A. Effect of folic acid and antioxidant vitamins on endothelial dysfunction in patients with coronary artery disease. J. Am. Coll. Cardiol. 36, 758–765 (2000).
Bonaa, K. H. et al. Homocysteine lowering and cardiovascular events after acute myocardial infarction. N. Engl. J. Med. 354, 1578–1588 (2006).
Albert, C. M. et al. Effect of folic acid and B vitamins on risk of cardiovascular events and total mortality among women at high risk for cardiovascular disease: a randomized trial. JAMA 299, 2027–2036 (2008).
Li, Y. et al. Folic acid supplementation and the risk of cardiovascular diseases: a meta-analysis of randomized controlled trials. J. Am. Heart Assoc. 5, e003768 (2016).
Mason, J. B. et al. A temporal association between folic acid fortification and an increase in colorectal cancer rates may be illuminating important biological principles: a hypothesis. Cancer Epidemiol. Biomarkers Prev. 16, 1325–1329 (2007).
Qin, X. et al. Effect of folic acid supplementation on cancer risk among adults with hypertension in China: a randomized clinical trial. Int. J. Cancer 141, 837–847 (2017).
Hubner, R. A., Houlston, R. D. & Muir, K. R. Should folic acid fortification be mandatory? No. BMJ 334, 1253 (2007).
Boslett, J., Hemann, C., Zhao, Y. J., Lee, H. C. & Zweier, J. L. Luteolinidin protects the postischemic heart through CD38 inhibition with preservation of NAD(P)(H). J. Pharmacol. Exp. Ther. 361, 99–108 (2017).
Moccia, F. et al. Hydrogen sulfide regulates intracellular Ca2+ concentration in endothelial cells from excised rat aorta. Curr. Pharm. Biotechnol. 12, 1416–1426 (2011).
Altaany, Z., Yang, G. & Wang, R. Crosstalk between hydrogen sulfide and nitric oxide in endothelial cells. J. Cell. Mol. Med. 17, 879–888 (2013).
Bir, S. C. et al. Hydrogen sulfide stimulates ischemic vascular remodeling through nitric oxide synthase and nitrite reduction activity regulating hypoxia-inducible factor-1alpha and vascular endothelial growth factor-dependent angiogenesis. J. Am. Heart Assoc. 1, e004093 (2012).
Nishida, M. et al. Hydrogen sulfide anion regulates redox signaling via electrophile sulfhydration. Nat. Chem. Biol. 8, 714–724 (2012).
Predmore, B. L. et al. The polysulfide diallyl trisulfide protects the ischemic myocardium by preservation of endogenous hydrogen sulfide and increasing nitric oxide bioavailability. Am. J. Physiol. Heart Circ. Physiol. 302, H2410–H2418 (2012).
Polhemus, D. et al. Hydrogen sulfide attenuates cardiac dysfunction after heart failure via induction of angiogenesis. Circ. Heart Fail. 6, 1077–1086 (2013).
Elrod, J. W. et al. Hydrogen sulfide attenuates myocardial ischemia-reperfusion injury by preservation of mitochondrial function. Proc. Natl Acad. Sci. USA 104, 15560–15565 (2007).
Hayashida, R. et al. Diallyl trisulfide augments ischemia-induced angiogenesis via an endothelial nitric oxide synthase-dependent mechanism. Circ. J. 81, 870–878 (2017).
Kang, J. et al. pH-controlled hydrogen sulfide release for myocardial ischemia-reperfusion injury. J. Am. Chem. Soc. 138, 6336–6339 (2016).
Polhemus, D. J. et al. A novel hydrogen sulfide prodrug, SG1002, promotes hydrogen sulfide and nitric oxide bioavailability in heart failure patients. Cardiovasc. Ther. 33, 216–226 (2015).
Hu, Q. et al. Novel angiogenic activity and molecular mechanisms of ZYZ-803, a slow-releasing hydrogen sulfide-nitric oxide hybrid molecule. Antioxid. Redox Signal. 25, 498–514 (2016).
Pufahl, R. A., Wishnok, J. S. & Marletta, M. A. Hydrogen peroxide-supported oxidation of NG-hydroxy-L-arginine by nitric oxide synthase. Biochemistry 34, 1930–1941 (1995).
Adak, S., Wang, Q. & Stuehr, D. J. Arginine conversion to nitroxide by tetrahydrobiopterin-free neuronal nitric-oxide synthase. Implications for mechanism. J. Biol. Chem. 275, 33554–33561 (2000).
Woodward, J. J., Nejatyjahromy, Y., Britt, R. D. & Marletta, M. A. Pterin-centered radical as a mechanistic probe of the second step of nitric oxide synthase. J. Am. Chem. Soc. 132, 5105–5113 (2010).
Katori, T. et al. Peroxynitrite and myocardial contractility: in vivo versus in vitro effects. Free Radic. Biol. Med. 41, 1606–1618 (2006).
Paolocci, N. et al. Positive inotropic and lusitropic effects of HNO/NO- in failing hearts: independence from beta-adrenergic signaling. Proc. Natl Acad. Sci. USA 100, 5537–5542 (2003).
Tocchetti, C. G. et al. Nitroxyl improves cellular heart function by directly enhancing cardiac sarcoplasmic reticulum Ca2+ cycling. Circ. Res. 100, 96–104 (2007).
Ding, W. et al. Reversal of isoflurane-induced depression of myocardial contraction by nitroxyl via myofilament sensitization to Ca2+. J. Pharmacol. Exp. Ther. 339, 825–831 (2011).
Gao, W. D. et al. Nitroxyl-mediated disulfide bond formation between cardiac myofilament cysteines enhances contractile function. Circ. Res. 111, 1002–1011 (2012).
Froehlich, J. P. et al. Phospholamban thiols play a central role in activation of the cardiac muscle sarcoplasmic reticulum calcium pump by nitroxyl. Biochemistry 47, 13150–13152 (2008).
Sivakumaran, V. et al. HNO enhances SERCA2a activity and cardiomyocyte function by promoting redox-dependent phospholamban oligomerization. Antioxid. Redox Signal. 19, 1185–1197 (2013).
Tocchetti, C. G. et al. Playing with cardiac “redox switches”: the “HNO way” to modulate cardiac function. Antioxid. Redox Signal. 14, 1687–1698 (2011).
Sabbah, H. N. et al. Nitroxyl (HNO): a novel approach for the acute treatment of heart failure. Circ. Heart Fail. 6, 1250–1258 (2013).
Zhu, G. et al. Soluble guanylate cyclase is required for systemic vasodilation but not positive inotropy induced by nitroxyl in the mouse. Hypertension 65, 385–392 (2015).
Tita, C. et al. A phase 2a dose-escalation study of the safety, tolerability, pharmacokinetics and haemodynamic effects of BMS-986231 in hospitalized patients with heart failure with reduced ejection fraction. Eur. J. Heart Fail. 19, 1321–1332 (2017).
Siddiqi, N. et al. Intravenous sodium nitrite in acute ST-elevation myocardial infarction: a randomized controlled trial (NIAMI). Eur. Heart J. 35, 1255–1262 (2014).
Jones, D. A. et al. Randomized phase 2 trial of intracoronary nitrite during acute myocardial infarction. Circ. Res. 116, 437–447 (2015).
Borlaug, B. A., Melenovsky, V. & Koepp, K. E. Inhaled sodium nitrite improves rest and exercise hemodynamics in heart failure with preserved ejection fraction. Circ. Res. 119, 880–886 (2016).
Eggebeen, J. et al. One week of daily dosing with beetroot juice improves submaximal endurance and blood pressure in older patients with heart failure and preserved ejection fraction. JACC Heart Fail. 4, 428–437 (2016).
Reddy, Y. N. V. et al. INDIE-HFpEF (Inorganic Nitrite Delivery to Improve Exercise Capacity in Heart Failure With Preserved Ejection Fraction): rationale and design. Circ. Heart Fail. 10, e003862 (2017).
Simon, M. A. et al. Acute hemodynamic effects of inhaled sodium nitrite in pulmonary hypertension associated with heart failure with preserved ejection fraction. JCI Insight 1, e89620 (2016).
Montenegro, M. F. et al. Blood pressure-lowering effect of orally ingested nitrite is abolished by a proton pump inhibitor. Hypertension 69, 23–31 (2017).
Hughan, K. S. et al. Conjugated linoleic acid modulates clinical responses to oral nitrite and nitrate. Hypertension 70, 634–644 (2017).
Nantel, F. et al. The human beta 3-adrenergic receptor is resistant to short term agonist-promoted desensitization. Mol. Pharmacol. 43, 548–555 (1993).
Moniotte, S. et al. Upregulation of beta(3)-adrenoceptors and altered contractile response to inotropic amines in human failing myocardium. Circulation 103, 1649–1655 (2001).
Dessy, C. et al. Endothelial beta3-adrenoceptors mediate vasorelaxation of human coronary microarteries through nitric oxide and endothelium-dependent hyperpolarization. Circulation 110, 948–954 (2004).
Vij, M. & Drake, M. J. Clinical use of the beta3 adrenoceptor agonist mirabegron in patients with overactive bladder syndrome. Ther. Adv. Urol. 7, 241–248 (2015).
Bundgaard, H. et al. The-first-in-man randomized trial of a beta3 adrenoceptor agonist in chronic heart failure: the BEAT-HF trial. Eur. J. Heart Fail. 19, 566–575 (2017).
Balligand, J. L. Cardiac beta3-adrenergic receptors in the clinical arena: the end of the beginning. Eur. J. Heart Fail. 19, 576–578 (2017).
Garcia-Alvarez, A. et al. Beta-3 adrenergic agonists reduce pulmonary vascular resistance and improve right ventricular performance in a porcine model of chronic pulmonary hypertension. Bas. Res. Cardiol. 111, 49 (2016).
Karimi Galougahi, K. et al. Beta3 adrenergic stimulation restores nitric oxide/redox balance and enhances endothelial function in hyperglycemia. J. Am. Heart Assoc. 5, e002824 (2016).
Garlichs, C. D. et al. Decreased plasma concentrations of L-hydroxy-arginine as a marker of reduced NO formation in patients with combined cardiovascular risk factors. J. Lab. Clin. Med. 135, 419–425 (2000).
Henry, Y. & Banerjee, R. Electron paramagnetic studies of nitric oxide haemoglobin derivatives: isolated subunits and nitric oxide hybrids. J. Mol. Biol. 73, 469–482 (1973).
Hamburg, N. M. et al. Cross-sectional relations of digital vascular function to cardiovascular risk factors in the Framingham Heart Study. Circulation 117, 2467–2474 (2008).
Nakayama, M. et al. T-786→C mutation in the 5′-flanking region of the endothelial nitric oxide synthase gene is associated with coronary spasm. Circulation 99, 2864–2870 (1999).
Miyamoto, Y. et al. Replication protein A1 reduces transcription of the endothelial nitric oxide synthase gene containing a -786T→C mutation associated with coronary spastic angina. Hum. Mol. Genet. 9, 2629–2637 (2000).
Rai, H., Parveen, F., Kumar, S., Kapoor, A. & Sinha, N. Association of endothelial nitric oxide synthase gene polymorphisms with coronary artery disease: an updated meta-analysis and systematic review. PLoS ONE 9, e113363 (2014).
Sandrim, V. C. et al. Susceptible and protective eNOS haplotypes in hypertensive black and white subjects. Atherosclerosis 186, 428–432 (2006).
Serrano, N. C. et al. Endothelial NO synthase genotype and risk of preeclampsia: a multicenter case-control study. Hypertension 44, 702–707 (2004).
Safarinejad, M. R., Khoshdel, A., Shekarchi, B., Taghva, A. & Safarinejad, S. Association of the T-786C, G894T and 4a/4b polymorphisms of the endothelial nitric oxide synthase gene with vasculogenic erectile dysfunction in Iranian subjects. BJU Int. 107, 1994–2001 (2011).
Salvi, E. et al. Target sequencing, cell experiments, and a population study establish endothelial nitric oxide synthase (eNOS) gene as hypertension susceptibility gene. Hypertension 62, 844–852 (2013).
Nelson, C. P. et al. Association analyses based on false discovery rate implicate new loci for coronary artery disease. Nat. Genet. 49, 1385–1391 (2017).
Nikpay, M. et al. A comprehensive 1,000 Genomes-based genome-wide association meta-analysis of coronary artery disease. Nat. Genet. 47, 1121–1130 (2015).
Johnson, T. et al. Blood pressure loci identified with a gene-centric array. Am. J. Hum. Genet. 89, 688–700 (2011).
Zhang, M. X. et al. Regulation of endothelial nitric oxide synthase by small RNA. Proc. Natl Acad. Sci. USA 102, 16967–16972 (2005).
Zhang, M. X. et al. Effect of 27nt small RNA on endothelial nitric-oxide synthase expression. Mol. Biol. Cell 19, 3997–4005 E07-11-1186 (2008).
Casas, J. P., Bautista, L. E., Humphries, S. E. & Hingorani, A. D. Endothelial nitric oxide synthase genotype and ischemic heart disease: meta-analysis of 26 studies involving 23028 subjects. Circulation 109, 1359–1365 (2004).
Galanakis, E. et al. Intron 4 a/b polymorphism of the endothelial nitric oxide synthase gene is associated with both type 1 and type 2 diabetes in a genetically homogeneous population. Hum. Immunol. 69, 279–283 (2008).
Mehrab-Mohseni, M. et al. Endothelial nitric oxide synthase VNTR (intron 4 a/b) polymorphism association with type 2 diabetes and its chronic complications. Diabetes Res. Clin. Practice 91, 348–352 (2011).
Joshi, M. S., Mineo, C., Shaul, P. W. & Bauer, J. A. Biochemical consequences of the NOS3 Glu298Asp variation in human endothelium: altered caveolar localization and impaired response to shear. FASEB J. 21, 2655–2663 (2007).
Antoniades, C. et al. Genetic polymorphism on endothelial nitric oxide synthase affects endothelial activation and inflammatory response during the acute phase of myocardial infarction. J. Am. Coll. Cardiol. 46, 1101–1109 (2005).
Shimasaki, Y. et al. Association of the missense Glu298Asp variant of the endothelial nitric oxide synthase gene with myocardial infarction. J. Am. Coll. Cardiol. 31, 1506–1510 (1998).
Colombo, M. G. et al. Evidence for association of a common variant of the endothelial nitric oxide synthase gene (Glu298→Asp polymorphism) to the presence, extent, and severity of coronary artery disease. Heart 87, 525–528 (2002).
Lee, Y. C. et al. The associations among eNOS G894T gene polymorphism, erectile dysfunction, and benign prostate hyperplasia-related lower urinary tract symptoms. J. Sexual Med. 6, 3158–3165 (2009).
Kessler, T. et al. Functional characterization of the GUCY1A3 coronary artery disease risk locus. Circulation 136, 476–489 (2017).
Erdmann, J. et al. Dysfunctional nitric oxide signalling increases risk of myocardial infarction. Nature 504, 432–436 (2013).
Ding, H. et al. A novel loss-of-function DDAH1 promoter polymorphism is associated with increased susceptibility to thrombosis stroke and coronary heart disease. Circ. Res. 106, 1145–1152 (2010).
Yang, Z. et al. Identification of a novel polymorphism in the 3′UTR of the L-arginine transporter gene SLC7A1: contribution to hypertension and endothelial dysfunction. Circulation 115, 1269–1274 (2007).
Guo, D. C. et al. Recurrent gain-of-function mutation in PRKG1 causes thoracic aortic aneurysms and acute aortic dissections. Am. J. Hum. Genet. 93, 398–404 (2013).
Ganesh, S. K. et al. Loci influencing blood pressure identified using a cardiovascular gene-centric array. Hum. Mol. Genet. 22, 1663–1678 (2013).
The International Consortium for Blood Pressure Genome-Wide Association Studies. Genetic variants in novel pathways influence blood pressure and cardiovascular disease risk. Nature 478, 103–109 (2011).
Ehret, G. B. et al. The genetics of blood pressure regulation and its target organs from association studies in 342,415 individuals. Nat. Genet. 48, 1171–1184 (2016).
Liu, C. et al. Meta-analysis identifies common and rare variants influencing blood pressure and overlapping with metabolic trait loci. Nat. Genet. 48, 1162–1170 (2016).
Kato, N. et al. Trans-ancestry genome-wide association study identifies 12 genetic loci influencing blood pressure and implicates a role for DNA methylation. Nat. Genet. 47, 1282–1293 (2015).
Warren, H. R. et al. Genome-wide association analysis identifies novel blood pressure loci and offers biological insights into cardiovascular risk. Nat. Genet. 49, 403–415 (2017).
Wild, P. S. et al. Large-scale genome-wide analysis identifies genetic variants associated with cardiac structure and function. J. Clin. Invest. 127, 1798–1812 (2017).
Vasan, R. S. et al. Genetic variants associated with cardiac structure and function: a meta-analysis and replication of genome-wide association data. JAMA 302, 168–178 (2009).
Newton-Cheh, C. et al. Common variants at ten loci influence QT interval duration in the QTGEN Study. Nat. Genet. 41, 399–406 (2009).
Pfeufer, A. et al. Common variants at ten loci modulate the QT interval duration in the QTSCD Study. Nat. Genet. 41, 407–414 (2009).
Jamshidi, Y. et al. Common variation in the NOS1AP gene is associated with drug-induced QT prolongation and ventricular arrhythmia. J. Am. Coll. Cardiol. 60, 841–850 (2012).
Kao, W. H. et al. Genetic variations in nitric oxide synthase 1 adaptor protein are associated with sudden cardiac death in US white community-based populations. Circulation 119, 940–951 (2009).
Eijgelsheim, M. et al. Genetic variation in NOS1AP is associated with sudden cardiac death: evidence from the Rotterdam Study. Hum. Mol. Genet. 18, 4213–4218 (2009).
Yin, C., Salloum, F. N. & Kukreja, R. C. A novel role of microRNA in late preconditioning: upregulation of endothelial nitric oxide synthase and heat shock protein 70. Circ. Res. 104, 572–575 (2009).
Meloni, M. et al. Local inhibition of microRNA-24 improves reparative angiogenesis and left ventricle remodeling and function in mice with myocardial infarction. Mol. Ther. 21, 1390–1402 (2013).
Sun, H. X. et al. Essential role of microRNA-155 in regulating endothelium-dependent vasorelaxation by targeting endothelial nitric oxide synthase. Hypertension 60, 1407–1414 (2012).
Zhang, J., Zhao, F., Yu, X., Lu, X. & Zheng, G. MicroRNA-155 modulates the proliferation of vascular smooth muscle cells by targeting endothelial nitric oxide synthase. Int. J. Mol. Med. 35, 1708–1714 (2015).
Fichtlscherer, S. et al. Circulating microRNAs in patients with coronary artery disease. Circ. Res. 107, 677–684 (2010).
Magenta, A. et al. miR-200c is upregulated by oxidative stress and induces endothelial cell apoptosis and senescence via ZEB1 inhibition. Cell Death Differ. 18, 1628–1639 (2011).
Carlomosti, F. et al. Oxidative stress-induced miR-200c disrupts the regulatory loop among SIRT1, FOXO1, and eNOS. Antioxid. Redox Signal. 27, 328–344 (2017).
Ho, J. J. et al. Active stabilization of human endothelial nitric oxide synthase mRNA by hnRNP E1 protects against antisense RNA and microRNAs. Mol. Cell. Biol. 33, 2029–2046 (2013).
Fish, J. E. et al. Hypoxia-inducible expression of a natural cis-antisense transcript inhibits endothelial nitric-oxide synthase. J. Biol. Chem. 282, 15652–15666 (2007).
Meng, F. et al. MicroRNA-21 regulates expression of the PTEN tumor suppressor gene in human hepatocellular cancer. Gastroenterology 133, 647–658 (2007).
Weber, M., Baker, M. B., Moore, J. P. & Searles, C. D. MiR-21 is induced in endothelial cells by shear stress and modulates apoptosis and eNOS activity. Biochem. Biophys. Res. Commun. 393, 643–648 (2010).
Zhou, J. et al. MicroRNA-21 targets peroxisome proliferators-activated receptor-alpha in an autoregulatory loop to modulate flow-induced endothelial inflammation. Proc. Natl Acad. Sci. USA 108, 10355–10360 (2011).
Cengiz, M. et al. Circulating miR-21 and eNOS in subclinical atherosclerosis in patients with hypertension. Clin. Exp. Hypertens. 37, 643–649 (2015).
Fang, Y. & Davies, P. F. Site-specific microRNA-92a regulation of Kruppel-like factors 4 and 2 in atherosusceptible endothelium. Arterioscler. Thromb. Vasc. Biol. 32, 979–987 (2012).
Chiplunkar, A. R. et al. The Kruppel-like factor 2 and Kruppel-like factor 4 genes interact to maintain endothelial integrity in mouse embryonic vasculogenesis. BMC Dev. Biol. 13, 40 (2013).
Wu, W. et al. Flow-dependent regulation of Kruppel-like factor 2 is mediated by microRNA-92a. Circulation 124, 633–641 (2011).
Loyer, X. et al. Inhibition of microRNA-92a prevents endothelial dysfunction and atherosclerosis in mice. Circ. Res. 114, 434–443 (2014).
Chen, Z. et al. Oxidative stress activates endothelial innate immunity via sterol regulatory element binding protein 2 (SREBP2) transactivation of microRNA-92a. Circulation 131, 805–814 (2015).
Bonauer, A. et al. MicroRNA-92a controls angiogenesis and functional recovery of ischemic tissues in mice. Science 324, 1710–1713 (2009).
Li, P. et al. Inhibition of aberrant microRNA-133a expression in endothelial cells by statin prevents endothelial dysfunction by targeting GTP cyclohydrolase 1 in vivo. Circulation 134, 1752–1765 (2016).
Vikram, A. et al. Vascular microRNA-204 is remotely governed by the microbiome and impairs endothelium-dependent vasorelaxation by downregulating sirtuin1. Nat. Commun. 7, 12565 (2016).
Author information
Authors and Affiliations
Contributions
All authors researched data for the article, discussed its content, wrote the manuscript, and reviewed and edited it before submission.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Supplementary information S1 (table)
Current clinical trials targeting the NOS–NO signalling pathway in cardiovascular diseases (PDF 189 kb)
Rights and permissions
About this article
Cite this article
Farah, C., Michel, L. & Balligand, JL. Nitric oxide signalling in cardiovascular health and disease. Nat Rev Cardiol 15, 292–316 (2018). https://doi.org/10.1038/nrcardio.2017.224
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrcardio.2017.224
This article is cited by
-
Protein–protein interaction network-based integration of GWAS and functional data for blood pressure regulation analysis
Human Genomics (2024)
-
Red blood cell-derived arginase release in hemolytic uremic syndrome
Journal of Translational Medicine (2024)
-
Amino acid profile alteration in age-related atrial fibrillation
Journal of Translational Medicine (2024)
-
Dietary nitrate intake and association with markers of cardiometabolic risk in Iranian female adolescents
European Journal of Clinical Nutrition (2024)
-
Genetics of ischemic stroke functional outcome
Journal of Neurology (2024)