Abstract
Depression has often been associated with increased negative affect reactivity to stress (Stress-Sensitivity) and reduced capacity to experience pleasure or positive affect (Reward Experience). To date, no studies have prospectively examined changes in Stress-Sensitivity and Reward Experience following antidepressant treatment. The sample included 83 depressed patients and 22 healthy controls. A randomized controlled trial was carried out with patients receiving either imipramine or placebo for 6 weeks. At baseline and 6 weeks, patients and controls participated in an Experience Sampling procedure, prospectively measuring ecologically valid daily life appraisals of activities and mood states. The course of depression was assessed with the Hamilton Depression Rating Scale (HDRS). Multilevel linear regression analyses showed that patients had higher negative and lower positive appraisals of activities than controls. In addition, patients showed increased Stress-Sensitivity (negative affect reactivity to negatively appraised activities). Treatment with imipramine decreased Stress-Sensitivity and increased Reward Experience (positive affect reactivity to positively appraised activities). Changes in Stress-Sensitivity and Reward Experience were in part reducible to changes in the process of activity appraisal itself. However, increase in Reward Experience, but not decrease in Stress-Sensitivity, discriminated between patients who responded and those who did not, independent of changes in the process of activity appraisal itself. Response to treatment in depression may be conditional on restoration of hedonic capacity, the cerebral substrate of which requires further study in relation to antidepressant response. A search for (synergistic) antidepressant therapies specifically targeting ability to experience reward may be warranted.
Similar content being viewed by others
INTRODUCTION
Recent investigations into the factor structure of emotional experience have converged on two-factor models, often labeled positive affect (PA) and negative affect (NA) (Watson and Tellegen, 1985). Related theoretical perspectives have highlighted the functional significance of PA and NA by connecting these factors to broader affective systems governing approach and withdrawal motivation, respectively (Gray, 1973; Davidson, 1992; Depue and Collins, 1999; Watson et al, 1999). The PA system is associated with behavioral approach and is characterized by feelings such as enthusiasm, interest, and satisfaction. The NA system is associated with behavioral withdrawal and is characterized by feelings such as anxiety, nervousness, tension, and guilt (Watson et al, 1999). PA and NA reactions can thus be conceived as preparing individuals for adaptation to meaningful opportunities and threats in their environment (Watson et al, 1999).
In depression, emotional processing within both the NA and the PA dimension may be altered (Leppanen, 2006). First, depressed individuals and those at genetic risk for depression experience more NA (Clark et al, 1994) and respond with increased NA to small daily life stressors (Myin-Germeys et al, 2003; Wichers et al, 2007a, 2007b, 2007c). Second, anhedonia, or reduced capacity to experience pleasure or PA from events or activities that are normally rated as interesting or pleasant, is a core symptom of depression. There is experimental evidence showing lower levels of PA in depressed patients (Clark et al, 1994), decreased reward sensitivity toward positive stimuli (Sloan et al, 1997; Dunn et al, 2004; Shankman et al, 2007), and altered reward-related decision making (Forbes et al, 2007). Taken together, the findings suggest that depressed individuals show altered Stress-Sensitivity together with a diminished ability to make use of natural rewards generating positive emotions. Positive emotions, such as contentment, happiness and compassion, appear to be involved in stress resilience. They not only reduce Stress-Sensitivity in terms of altered mood response (Strand et al, 2006; Wichers et al, 2007a, 2007b, 2007c), but also in terms of stress-induced physical changes such as cardiovascular reactivity (Fredrickson and Levenson, 1998; Tugade and Fredrickson, 2004; Steptoe et al, 2007). In addition, they decrease the expression of genetic risk for depression and genetic risk for Stress-Sensitivity (Wichers et al, 2007a, 2007b, 2007c; Wichers et al, unpublished data). Thus, the decreased ability to generate positive emotions (decreased level of reward experience) in depressed individuals contributes to a loss of the normal protection or resilience against stress in daily life.
There has been little research on the effects of antidepressant treatment on emotional experiences in terms of alterations in Stress-Sensitivity (responding with NA to negative stimuli; hereafter: Stress-Sensitivity) and reward experience (responding with PA to pleasant stimuli; hereafter: Reward Experience). From animal studies, it is known that antidepressants reduce stress-induced brain alterations and activation of the hypothalamic-pituitary-adrenal axis, the most important brain system regulating stress responses (Connor et al, 2000; Basta-Kaim et al, 2005). In addition, antidepressant treatment in socially stressed rats restores anhedonia and motivational deficits (Von Frijtag et al, 2002; Rygula et al, 2006) and thus normalizes Reward Experience. However, there are very few studies evaluating the effects of antidepressant treatment on NA and PA reactivity in clinically depressed people. Two studies reported that both distress and anhedonia are affected by antidepressants (Tomarken et al, 2004; Dichter et al, 2005). Bhagwagar et al (2004) demonstrated that in individuals with a history of depression, antidepressant treatment normalized abnormal fear processing in the form of enhanced fear recognition. Other studies, sampling healthy volunteers, showed that (i) antidepressants increased the cortical response to pleasant and decreased the response to unpleasant stimuli (Kemp et al, 2004, ii) antidepressant medication biased perception to positive information (Harmer et al, 2003, 2004), and (iii) medication decreased recognition of fearful facial stimuli (Harmer et al, 2004, 2006). However, healthy subjects may exhibit different responses toward the above manipulations than depressed patients (Bhagwagar et al, 2004). An unanswered question is whether antidepressants primarily work by normalizing alterations in Stress-Sensitivity or by increasing Reward Experience, thus enhancing the individual's emotional resilience to stress.
To date, no studies have prospectively examined changes in affective responses to negative and positive personal experiences (Stress-Sensitivity and Reward Experience, respectively) in response to antidepressant treatment. The current study investigated this issue with momentary assessment experience sampling methods (ESM), which yield data directly from the daily life of depressed patients, and thus takes into account the personal context of the individual within his or her daily life setting. Building on and extending the research reviewed above, it was hypothesized that antidepressants would alter NA responses to daily life activities appraised negatively (Stress-Sensitivity) and increase PA responses to daily life activities appraised positively (Reward Experience). In addition, it was examined to what degree changes in emotional experience in response to daily life activities coincided with clinical improvement, to elucidate the affective pathway underlying antidepressant action.
METHODS
Subjects
Eighty-three patients with a DSM-IV diagnosis of current major depressive disorder were recruited in eight primary care practices in the Netherlands (for full details concerning diagnosis and screening, see Barge-Schaapveld and Nicolson (2002)). Data were collected in the period between 1995 and 1996. Inclusion criteria were age between 18 and 65 years, a score at study entry of ⩾18 on the 17-item Hamilton Depression Rating Scale (HDRS) (Hamilton, 1960), and a score ⩾4 on the Clinical Global Impression (Guy, 1976). Exclusion criteria included major medical disorders and current use of psychotropic medications, except for the occasional use of temazepam.
A control group of 22 healthy individuals was recruited with sociodemographic characteristics similar to those of the patient group to provide normal reference values for ESM measures (for details, see Barge-Schaapveld et al (1999)).
All subjects gave written informed consent. The study was approved by the standing medical ethics committee.
Study Design
The study was conducted in a primary care setting in a sample of depressed outpatients. During an initial baseline week, participants received no treatment in any form. Thereafter, patients were randomly assigned to twice daily, double blind, 6-week treatment with either a tricyclic antidepressant (TCA) (imipramine: starting dose of 50 mg/day, increased to 200 mg/day over the first week of treatment) or placebo (starting with one capsule per day, increased to four capsules over the first week of treatment). In case of intolerance, the dose could be decreased to either 100 mg/day of imipramine or two placebo capsules per day. The healthy control subjects served as reference group and were not randomized to either antidepressant or placebo treatment. All subjects participated in the experience sampling procedure at baseline and at week 6. In addition, the depressed patients underwent semi-structured interviews at regular intervals to evaluate their level of depressive symptoms.
Experience Sampling Method
Experience sampling method is a structured diary technique to assess subjects in their daily living environment, which has been validated for the use of studying the immediate effects of stressors on mood (Csikszentmihalyi and Larson, 1987; DeVries, 1992; Delespaul, 1995; Myin-Germeys et al, 2003; Peeters et al, 2003). Subjects received a digital wristwatch and a set of ESM self-assessment forms collated in a booklet for each day. The wristwatch was programmed to emit a signal (‘beep’) at an unpredictable moment in each of ten 90-min time blocks between 0730 and 2230 hours, on 6 consecutive days. After each beep, subjects were asked to fill out the ESM self-assessment forms to record current thoughts, current context (activity, persons present, and location), appraisals of the current situation, and mood. All self-assessments were rated on 7-point Likert scales. Trained research nurses explained the ESM procedure to the participants during an initial briefing session. Subjects were instructed to complete their reports immediately after the beep, thus minimizing memory distortion, and to record the time at which they completed the form. To determine whether subjects completed the form on time, self-reported times were compared to the actual beep times. All reports not filled in within 15 min after the beep were excluded from the analysis, as previous study (Delespaul, 1995) has shown that reports completed after this interval are less reliable and consequently less valid. For the same reason, subjects with fewer than 20 valid reports (out of 60 maximum) were excluded from the analysis (Delespaul, 1995). ESM test-retest reliability was examined. Mean levels of PA, NA, and appraisal of activities were stable over a period of 6 weeks in the group of healthy individuals (Barge-Schaapveld, 2001).
Measurements
The 17-item HDRS was administered by the treating physician (general practitioner—GP) at screening, baseline, and week 6 to evaluate the level of depressive symptoms. All participating GPs had completed a standardized training for the HDRS procedure.
Daily life activity appraisal: stress and reward
To define stress and reward in relation to ecologically valid daily activities, ESM self-rated appraisals of ongoing activities were used, consistent with several previous studies of emotional reactivity to appraised daily activities and contexts (Myin-Germeys et al, 2001, 2003; Myin-Germeys and van Os, 2007). Self-report items on current activity were rated on a Likert scale (with 1=not at all and 7=very). Factor analysis supported inclusion of three items on activity appraisal, namely: ‘do you enjoy this activity,’ ‘does this activity require effort,’ and ‘are you skilled at doing this activity.’ On the basis of these ratings, a variable reflecting ‘activity-related stress’ and one reflecting ‘activity-related reward’ were created. For activity-related stress, the positive appraisals ‘do you enjoy the activity’ and ‘are you skilled at doing this activity’ were first recoded in reverse, so that higher scores represented more negative appraisals (low enjoyment and low skill, respectively). Then, low scores (⩽4) on all three scales were set to zero and the remaining values were recoded (5=1, 6=2, 7=3), so that only appraisals with a negative valence contributed to the summed activity-related stress score. Similarly, to create the variable activity-related reward, the item ‘does this activity require effort’ was first recoded in reverse so that high scores reflected lower appraised effort, low scores (⩽4) on this recoded item and the other two appraisal items were set to zero, and higher scores were recoded (5=1, 6=2, 7=3) before calculating a sum score for activity-related reward.
Mood states
At each beep, ESM mood adjectives were assessed, conform previous study (Barge-Schaapveld and Nicolson, 2002). Factor analysis, using principal component analysis with oblique rotation, was used to generate a factor representing PA and one representing NA. The mood adjectives ‘cheerful,’ ‘content,’ ‘energetic,’ ‘calm,’ ‘alert,’ ‘enthusiastic,’ ‘strong,’ and ‘happy’ loaded on the PA factor whereas ‘hostile,’ ‘depressed,’ ‘tensed,’ ‘insecure,’ ‘lonely,’ ‘anxious,’ ‘guilty,’ ‘hurried,’ and ‘irritable’ loaded on the NA factor. The item ‘I feel tired’ was left out of the constructed scales because its loading was not specific for either NA or PA.
Statistical Analyses
Experience sampling method data have a hierarchical structure. Thus, multiple observations (level 1) were clustered within subjects (level 2). Multilevel analysis takes the variability associated with each level of nesting into account (Snijders and Bosker, 1999). Multilevel linear regression analyses, using the XTREG command in STATA 9.1 (StataCorp, 2005) were applied to the data.
‘Stress-Sensitivity’ was conceptualized in the analyses as the effect of stressful daily life activities on NA (ie the effect of the activity-related stress score on NA). Similarly, ‘Reward Experience’ was conceptualized as the effect of positively appraised daily life activities on PA (ie the effect of the activity-related reward score on PA). First, it was examined whether depressed patients differed at baseline from healthy controls in terms of daily life Stress-Sensitivity and Reward Experience by assessing the two-way interaction between group status (healthy or depressed) and appraisal in the models of NA and PA, respectively. In addition, a variable was created dividing all observations of appraisals into four categories (from low to high scores) with equal number of observations (quartile groups). This variable was used to examine a possible dose-response effect of valence of appraisal on differential mood response in depressed patients vs healthy controls. Effect sizes of the interactions between the four levels of appraisal on the one hand and group status on the other were calculated by applying and testing the appropriate linear combinations using the STATA LINCOM command. Main effects and interactions were assessed with the Wald test (Clayton and Hill, 1993).
Second, it was examined whether antidepressant treatment with imipramine decreased Stress-Sensitivity relative to the placebo group. To effectuate this, NA was regressed on the three-way interaction ‘time (6 weeks compared to baseline) × treatment group (placebo vs TCA) × activity-related stress appraisal.’ Similarly, the effect of treatment on increase in Reward Experience was examined. Again, effect sizes of treatment group on the changes (baseline—week 6) in Stress-Sensitivity and Reward Experience were calculated by applying and testing the appropriate linear combinations using the STATA LINCOM command. Main effects and interactions were assessed with the Wald test (Clayton and Hill, 1993). Given relatively low power, three-way interactions of p⩽0.1 were considered sufficiently suggestive for follow-up and calculation of stratified effect sizes.
Third, patients were categorized as responders or non-responders to treatment, to determine the degree to which a decrease in Stress-Sensitivity or an increase in Reward Experience over the 6 weeks of treatment was associated with clinical improvement, stratified by treatment group (placebo or TCA). To maximize statistical power, the sample was divided according to the median split on the percentage decrease in HDRS symptom score from baseline to 6 weeks: the responder group included patients in the upper half of the HDRS distribution of change and the non-responder group those in the lower half of the HDRS distribution of change. Associations between responder status and changes in Stress-Sensitivity and Reward experience were calculated by applying and testing the appropriate linear combinations, using LINCOM; significance was assessed using the Wald test (Clayton and Hill, 1993).
RESULTS
Patient Sample
Of 83 depressed patients, 11 were excluded on the basis of the described inclusion and exclusion criteria. Reasons were use of psychotropic medication, abnormal ECG, and HDRS lower than 18; one eligible subject was excluded due to an error in the randomization procedure. Five subjects were later excluded, because they failed to complete at least 20 valid ESM reports at baseline, (see ESM, above). One depressed subject had partially missing data for PA and NA, leaving 65 depressed patients (imipramine group: 33; placebo group: 32) for the baseline analyses. For the follow-up analyses, two additional subjects were excluded who completed fewer than 20 valid ESM reports at week 6. Of the 63 remaining patients, 49 (78%) completed the first 6 weeks of treatment. Analyses concerning changes over time in Stress-Sensitivity and Reward Experience were based solely on data of subjects who completed treatment. The dropouts showed a trend toward higher PA at baseline (B=0.31, p=0.09) compared to the completers. There were no other significant baseline differences in mood, stress appraisal, or emotional reactivity between these two groups.
Subject Characteristics
Patients ranged in age from 25 to 59 years (mean=42.7). The majority were women (72%) and married (68%). Most had a regular job (46%) or were housewives (25%).
Baseline average HDRS score was 23.9 (SD=3.1; range: 19–30). At week 6, average HDRS score was 10.6 (SD=6.5; range: 0–24). Mean HDRS scores at week 6 for the imipramine (8.5) and placebo (12.6) group differed significantly (B=−4.14, p=0.024). For responders as defined above, mean HDRS score at week 6 was 5.2 (SD=3.0; range: 0–9) and for non-responders 15.4 (SD=4.6; range: 8–24). According to the common definition of remission as an HDRS score <8 (Ballesteros et al, 2007), none of the non-responders had thus achieved remission. The mean percentage decline in HDRS score was 55% (SD=28.3; range: −10 to 100%). Only one subject increased in HDRS score (with 2 points) and one showed no change. For mean activity-related and mood appraisals see Table 1. Correlations between activity-related stress and reward (Table 2a) and between PA and NA (Table 2b) are depicted in Tables 2a and 2b. There were significant main effects of ‘time’ on both activity-related stress appraisal (B=−0.15, p<0.001) and activity-related reward appraisal (B=0.11, p<0.001). In addition, there were suggestive or significant associations between percentage decline in HDRS scores over time and activity appraisals (B=−0.01, p=0.086 for activity-related stress; B=0.02, p=0.004 for activity-related reward).
There were no large or significant initial differences between the two treatment groups with respect to sociodemographic characteristics, HDRS ratings, or activity appraisal. Patients randomized to the TCA group did not differ significantly at baseline in Reward Experience (ie effect of activity-related reward on PA) from the placebo group (B=−0.009, p=0.17). Similarly, there was no baseline difference in Stress-Sensitivity (ie the effect of the activity-related stress score on NA) (B=0.005, p=0.7). At week 6, patients in the TCA group complained more frequently about having ‘a dry mouth’ (B=0.9, p=0.032) than those in the placebo group, whereas ‘headache,’ ‘dizziness,’ ‘nausea,’ ‘drowsiness,’ and ‘other complaints’ were reported equally or less often in the imipramine group compared to placebo. As control subjects were frequency matched for demographic characteristics, there were no differences between patients and healthy controls in mean age, sex distribution, living situation (alone or not), or work status (see Barge-Schaapveld et al, 1999 for further information).
Daily Life Stress-Sensitivity and Reward Experience in Depressed Patients Vs Controls
At baseline, depressed patients showed significantly higher scores on activity-related stress (B=1.07, p<0.001) and lower scores on activity-related reward (B=−2.03, p<0.001) compared to healthy controls. With regard to emotional reactivity to daily life activities, depressed patients displayed an increased NA response to activity-related stress (Stress-Sensitivity) compared to controls (χ2 interaction=5.26; p=0.022; B=0.109 for depressed and B=0.068 for control subjects). The interaction effects showed a dose-response effect: the more negative the appraisal, the greater the difference in mood response between depressed and control subjects (Figure 1).
Difference in Stress-Sensitivity between depressed subjects and healthy controls stratified for degree of negative appraisal. *χ2=4.1, p=0.04. **χ2=12.5, p<0.001. §As the distribution of ‘activity-related stress’ was skewed, the first two (lowest 50% of scores) of the four categories are merged to one, representing the reference category ‘neutral.’
There was no significant difference in PA response to activity-related reward appraisals (Reward Experience) between depressed patients and healthy controls (χ2 interaction=1.01; p=0.3).
Effects of TCA Treatment on Stress-Sensitivity and Reward Experience in Depressed Patients
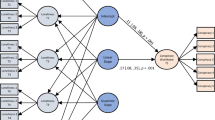
There was a significant three-way interaction between treatment group, time, and activity-related stress appraisal in the model of NA (χ2=7.2, B=−0.05, p=0.007), indicating that Stress-Sensitivity decreased more strongly in the TCA group (B=−0.073, p<0.001) than the placebo group (−0.023, p=0.04) (Figure 2a). Also, a significant three-way interaction between treatment, time, and positively appraised activities was found in the model of PA (χ2=5.2, B=0.027, p=0.02) (Figure 2b). Thus, Reward Experience was increased at week 6 compared to baseline, and this effect was stronger in the TCA (B=0.066, p<0.001) than the placebo group (B=0.038, p<0.001).
(a) Decrease in Stress-Sensitivity (effect of positive activities on NA) at baseline and at week 6, separated for those in the TCA and the placebo group. *χ2=7.2, B=−0.05, p=0.007. (b) Increase in Reward Experience (effect of positively appraised activities on PA) at baseline and at week 6, separated for those in the TCA and the placebo group. *χ2=5.2, B=0.027, p=0.02.
Both effects were independent of each other: when the first three-way interaction effect in the model of PA was controlled for change in Stress-Sensitivity, or vice versa (second interaction effect in the model of NA controlled for change in Reward Experience), interaction effects remained similar.
To investigate possible mediation by changes over the 6-week period in activity-related appraisals themselves, the analyses were repeated after adding an extra variable to the equation, reflecting the difference in (i) activity-related stress or (ii) activity-related reward appraisal between baseline and week 6. This analysis revealed that controlling for change in activity-related appraisals reduced both interaction effects by 50%: Stress-Sensitivity (χ2=3.0, B=−0.036, p=0.08) and Reward Experience (χ2=0.93, B=0.013, p=0.3).
Change in Stress-Sensitivity and Reward Experience in Relation to Treatment Response
There was no three-way interaction of responder group × time × negatively appraised activities in the model of NA (χ2=0.27, B=0.010, p=0.6). In both responders and non-responders, the NA response to activity-related stress decreased similarly after 6 weeks of active or placebo treatment (responders: B=−0.05, p=0.03; non-responders: B=−0.06, p<0.001) (Figure 3a). Also within the TCA group, being a responder was not associated with stronger decrease in Stress-Sensitivity, in fact, the effect was in the opposite direction (responders: B=−0.008, p=0.7; non-responders: B=−0.12, p<0.001). Controlling for change in activity-related stress appraisal yielded similar results.
The three-way interaction of responder group × time × positively appraised activities on PA response was statistically significant (χ2=10.1, B=0.036, p=0.001). Thus, responders (B=0.040, p<0.001) showed strong increases in Reward Experience from baseline to week 6, whereas non-responders did not (B=0.0035, p=0.7) (Figure 3b). Also within the TCA group only, the effect remained significant and was even stronger (χ2=15.9, B=0.059, p<0.001). After controlling for activity-related reward appraisal, the interactions remained significant for both the total group (χ2=6.1, B=0.032, p=0.01) and the TCA group only (χ2=10.5, B=0.054, p=0.001).
DISCUSSION
Findings
Depressed patients exhibited higher activity-related stress appraisals and lower activity-related reward appraisals than control subjects. However, in addition to differences in interpretation of the activity itself, the emotional reactivity differed as well. Depressed patients responded with more NA to similarly appraised activities than control subjects. Emotional reactivity associated with Reward Experience, however, did not differ between groups. In addition, antidepressant treatment with imipramine in the depressed patients decreased Stress-Sensitivity and increased Reward Experience compared to placebo treatment. These effects were brought about both by changes in emotional reactivity and by changes in appraisal of activities. Although stronger effects were found in the active treatment group, Stress-Sensitivity and Reward Experience also changed in the same direction in the placebo group. Increase in Reward Experience discriminated between treatment responders and non-responders—independently from changes in appraisal—and thus appeared to be a necessary condition for response to treatment, in contrast to changes in Stress-Sensitivity.
Emotional Processes and Biological Systems
As the two dimensions of emotional experience, NA and PA, are relatively independent, there is face validity to the hypothesis that different biological systems may be involved. There is much evidence for a role of the amygdala in stress-induced negative emotions as fear and anxiety (Vyas et al, 2006; Sajdyk et al, 2008; Yang et al, 2008). In addition, serotonin function has been hypothesized to regulate emotional processes related to Stress-Sensitivity (Hariri and Holmes, 2006). Animal (Lira et al, 2003; Wellman et al, 2007) and human research (Hariri et al, 2002; Caspi et al, 2003) suggest that variation in serotonin transporter (5-HTT) gene function influences depression-related behavior in response to stress and affects amygdala function. Moreover, serotonergic antidepressants seem to be more effective in treating symptoms associated with negative affectivity (fear, anxiety, and irritability) than those related to diminished PA (Nutt et al, 2007).
In contrast, mesolimbic brain structures are involved in mediating reward. Reduced dopaminergic activity has been associated with decreased motivation and anhedonia (Salamone et al, 2003; Bressan and Crippa, 2005). Dopaminergic transmission between the ventral tegmental area and the nucleus accumbens (NAc), in interaction with frontal lobe connections, mediates the affective and behavioral response to rewarding stimuli (Chau et al, 2004; Nestler and Carlezon, 2006). Also, equally high levels of noradrenaline and dopamine are found in the NAc (Tong et al, 2006), suggesting that noradrenaline is implicated in mediating reward and motivation as well. In addition, another study provided support for the supposition that noradrenergic transmission is necessary for motivated behaviors (Jasmin et al, 2006). Imipramine has been shown in animal studies to affect both the dopaminergic (De Montis et al, 1990) and noradrenergic system (Linner et al, 1999).
Complex interactions between neurotransmitter systems take place. Dremencov et al (2004, 2005) showed that the increased inhibition of dopamine release in the NAc, mediated by 5-HT2C receptors in rats with depressive-like behavior, is normalized by antidepressants and that restoration of the 5-HT–dopamine interaction correlated directly with improvement of behavior (Dremencov et al, 2004, 2005). Although it may be speculated that this interaction at the biological level reflects the interdependence between experience of stress-sensitivity and reward experience at the behavioral level, there are no data to support this hypothesis at present. Future research may address this issue. Given the current finding that reward experience mediates recovery of depression, this study supports the suggestion made by Nutt et al (2007) that the use of antidepressants specifically targeting reward-associated biological mediators should be explored further.
Stress-Sensitivity, Reward Experience and Depression
Interactions take place at the affective level as well. Although the two core processes of Stress-Sensitivity and Reward Experience described in this paper may fluctuate relatively independently, they may also moderate each other. For example, it has been shown that the experience of positive emotions decreases momentary Stress-Sensitivity (Wichers et al, 2007a, 2007b, 2007c). It can also be hypothesized that a decrease in emotional Stress-Sensitivity facilitates the engaging in and enjoying of activities, thus aiding in the restoration of Reward Experience (Fredrickson, 2004). In this study, patients receiving imipramine displayed strong reductions in daily life Stress-Sensitivity, albeit mediated in part by changes in appraisal. However, reduction in daily life Stress-Sensitivity was only associated with a substantial reduction in clinical symptoms (HDRS) if there was a concurrent increase in Reward Experience. An attractive speculation for further investigation is that genetic variation is involved in differential changes in Reward Experience following changes in Stress-Sensitivity. For example, recent study suggests that catechol- O -methyltransferase Val158Met polymorphism genotypes, involved in the regulation of cerebral dopamine catabolism, are differentially associated with the capacity to make use of natural rewards in daily life (Wichers et al, 2007a, 2007b, 2007c). More knowledge in the field of individual genetic and biological variation in association with the above emotional processes may add to the process of prediction and improvement of treatment response to antidepressant medication.
Methodological Issues
Imipramine has a somewhat stronger impact on noradrenergic than serotonergic activity and also enhances dopaminergic activity. This represents a contrast with other antidepressant medication such as selective serotonin reuptake inhibitors. Therefore, the current results may not be generalizable to antidepressant drugs that selectively target other neurotransmitter systems.
The complaint of having a dry mouth was more often reported in the TCA group than the placebo group. Post hoc analyses showed that this complaint was associated with increased Stress-Sensitivity, but not with change in Reward Experience. Thus, this suggests that in reality effect sizes of treatment on decrease in stress-sensitivity might have been even larger than those reported in the study.
Although the baseline difference between groups in Reward Experience was not statistically significant, the TCA group had slightly lower initial Reward Experience than the placebo group. This meant that, although Reward Experience increased more in the TCA group, scores on this measure at 6 weeks were similar to those in the placebo group. Theoretically, it may be hypothesized that imipramine treatment would have resulted in a different effect size if baseline values had been equal. This is unlikely, however, as the effect of being a responder (for which no baseline difference in Reward Experience existed) on increase in Reward Experience was even more apparent in the TCA-only analyses than in those combining TCA and placebo (see Figure 3b). Nevertheless, replication of antidepressant treatment effects on Reward Experience is needed.
There was a suggestive baseline difference in PA between those who dropped out and those who completed the study. In addition, dropout was higher in the treatment than the placebo group. Thus, influence of differential dropout on the data may explain the low mean PA score of subjects in the TCA group at week 6 (Table 1).
It has been suggested that the ESM procedure is vulnerable to effects of poor participant compliance with the timing of self-reports (Kudielka et al, 2003; Broderick et al, 2004). In particular, fixed time sampling protocols may be problematic and can bias results. However, this study did not have a fixed time sampling frame, and the ESM procedure we used has been validated with electronic monitoring data in a different study; there, over 90% of the samples were accurately timed, and inclusion of the inaccurately timed samples did not distort the results (Jacobs et al, 2005).
Future Research
These findings indicate that imipramine treatment, relative to placebo treatment, decreases Stress-Sensitivity and also increases Reward Experience, although to a lesser extent. However, as an increase in daily life Reward Experience, but not a decrease in Stress-Sensitivity, was associated with treatment response, it may be beneficial to search for therapies that specifically aim at increasing the ability to experience reward (Nutt et al, 2006). In addition, individual factors, genetic variation, or environmental factors that impact on this ability should become the target of future investigation, so as to improve prediction of treatment response.
References
Ballesteros J, Bobes J, Bulbena A, Luque A, Dal-Re R, Ibarra N et al (2007). Sensitivity to change, discriminative performance, and cutoff criteria to define remission for embedded short scales of the Hamilton depression rating scale (HAMD). J Affect Disord 102: 93–99.
Barge-Schaapveld DQ (2001). Impact of Depression and Antidepressant Treatment in Daily Life: An Experience Sampling Approach. Maastricht University: Maastricht. 173.
Barge-Schaapveld DQ, Nicolson NA (2002). Effects of antidepressant treatment on the quality of daily life: an experience sampling study. J Clin Psychiatry 63: 477–485.
Barge-Schaapveld DQ, Nicolson NA, Berkhof J, deVries MW (1999). Quality of life in depression: daily life determinants and variability. Psychiatry Res 88: 173–189.
Basta-Kaim A, Budziszewska B, Jaworska-Feil L, Tetich M, Kubera M, Leskiewicz M et al (2005). Inhibitory effect of imipramine on the human corticotropin-releasing-hormone gene promoter activity operates through a PI3-K/AKT mediated pathway. Neuropharmacology 49: 156–164.
Bhagwagar Z, Cowen PJ, Goodwin GM, Harmer CJ (2004). Normalization of enhanced fear recognition by acute SSRI treatment in subjects with a previous history of depression. Am J Psychiatry 161: 166–168.
Bressan RA, Crippa JA (2005). The role of dopamine in reward and pleasure behaviour—review of data from preclinical research. Acta Psychiatr Scand Suppl 427: 14–21.
Broderick JE, Arnold D, Kudielka BM, Kirschbaum C (2004). Salivary cortisol sampling compliance: comparison of patients and healthy volunteers. Psychoneuroendocrinology 29: 636–650.
Caspi A, Sugden K, Moffitt TE, Taylor A, Craig IW, Harrington H et al (2003). Influence of life stress on depression: moderation by a polymorphism in the 5-HTT gene. Science 301: 386–389.
Chau DT, Roth RM, Green AI (2004). The neural circuitry of reward and its relevance to psychiatric disorders. Curr Psychiatry Rep 6: 391–399.
Clark LA, Watson D, Mineka S (1994). Temperament, personality, and the mood and anxiety disorders. J Abnorm Psychol 103: 103–116.
Clayton D, Hill M (1993). Wald tests. In: Clayton D, Hills M (eds). Statistical Models in Epidemiology. Oxford Science Publications: Oxford. pp 101–102.
Connor TJ, Kelliher P, Shen Y, Harkin A, Kelly JP, Leonard BE (2000). Effect of subchronic antidepressant treatments on behavioral, neurochemical, and endocrine changes in the forced-swim test. Pharmacol Biochem Behav 65: 591–597.
Csikszentmihalyi M, Larson R (1987). Validity and reliability of the Experience-Sampling Method. J Nerv Ment Dis 175: 526–536.
Davidson JR (1992). Emotion and affective style: hemispheric substrates. Psychol Sci 3: 39–43.
De Montis GM, Devoto P, Gessa GL, Meloni D, Porcella A, Saba P et al (1990). Central dopaminergic transmission is selectively increased in the limbic system of rats chronically exposed to antidepressants. Eur J Pharmacol 180: 31–35.
Delespaul P (1995). Assessing Schizophrenia in Daily Life: The Experience Sampling Method. University of Limburg: Maastricht.
Depue RA, Collins PF (1999). Neurobiology of the structure of personality: dopamine, facilitation of incentive motivation, and extraversion. Behav Brain Sci 22: 491–517; discussion 518–69.
DeVries MW (ed.) (1992). The Experience of Psychopathology: Investigating Mental Disorders in their Natural Settings. Cambridge University Press: Cambridge.
Dichter GS, Tomarken AJ, Freid CM, Addington S, Shelton RC (2005). Do venlafaxine XR and paroxetine equally influence negative and positive affect? J Affect Disord 85: 333–339.
Dremencov E, Gispan-Herman I, Rosenstein M, Mendelman A, Overstreet DH, Zohar J et al (2004). The serotonin–dopamine interaction is critical for fast-onset action of antidepressant treatment: in vivo studies in an animal model of depression. Prog Neuropsychopharmacol Biol Psychiatry 28: 141–147.
Dremencov E, Newman ME, Kinor N, Blatman-Jan G, Schindler CJ, Overstreet DH et al (2005). Hyperfunctionality of serotonin-2C receptor-mediated inhibition of accumbal dopamine release in an animal model of depression is reversed by antidepressant treatment. Neuropharmacology 48: 34–42.
Dunn BD, Dalgleish T, Lawrence AD, Cusack R, Ogilvie AD (2004). Categorical and dimensional reports of experienced affect to emotion-inducing pictures in depression. J Abnorm Psychol 113: 654–660.
Forbes EE, Shaw DS, Dahl RE (2007). Alterations in reward-related decision making in boys with recent and future depression. Biol Psychiatry 61: 633–639.
Fredrickson BL (2004). The broaden-and-build theory of positive emotions. Philos Trans R Soc Lond B Biol Sci 359: 1367–1378.
Fredrickson BL, Levenson RW (1998). Positive emotions speed recovery from the cardiovascular sequelae of negative emotions. Cognition and Emotion 12: 191–220.
Gray J (1973). Causal Theories of Personality and How to Test Them. Multivariate Analysis and Psychological Theory J. Royce. Academic Press: New York. 409–463.
Guy W (1976). ECDEU Assessment Manual for Psychopharmacology. US Department of Health, Education and Welfare: Rockville, MD. 59–70.
Hamilton M (1960). A rating scale for depression. J Neurol Neurosurg Psychiatry 23: 56–62.
Hariri AR, Holmes A (2006). Genetics of emotional regulation: the role of the serotonin transporter in neural function. Trends Cogn Sci 10: 182–191.
Hariri AR, Mattay VS, Tessitore A, Kolachana B, Fera F, Goldman D et al (2002). Serotonin transporter genetic variation and the response of the human amygdala. Science 297: 400–403.
Harmer CJ, Hill SA, Taylor MJ, Cowen PJ, Goodwin GM (2003). Toward a neuropsychological theory of antidepressant drug action: increase in positive emotional bias after potentiation of norepinephrine activity. Am J Psychiatry 160: 990–992.
Harmer CJ, Mackay CE, Reid CB, Cowen PJ, Goodwin GM (2006). Antidepressant drug treatment modifies the neural processing of nonconscious threat cues. Biol Psychiatry 59: 816–820.
Harmer CJ, Shelley NC, Cowen PJ, Goodwin GM (2004). Increased positive versus negative affective perception and memory in healthy volunteers following selective serotonin and norepinephrine reuptake inhibition. Am J Psychiatry 161: 1256–1263.
Jacobs N, Nicolson NA, Derom C, Delespaul P, van Os J, Myin-Germeys I (2005). Electronic monitoring of salivary cortisol sampling compliance in daily life. Life Sci 76: 2431–2443.
Jasmin L, Narasaiah M, Tien D (2006). Noradrenaline is necessary for the hedonic properties of addictive drugs. Vascul Pharmacol 45: 243–250.
Kemp AH, Gray MA, Silberstein RB, Armstrong SM, Nathan PJ (2004). Augmentation of serotonin enhances pleasant and suppresses unpleasant cortical electrophysiological responses to visual emotional stimuli in humans. Neuroimage 22: 1084–1096.
Kudielka BM, Broderick JE, Kirschbaum C (2003). Compliance with saliva sampling protocols: electronic monitoring reveals invalid cortisol daytime profiles in noncompliant subjects. Psychosom Med 65: 313–319.
Leppanen JM (2006). Emotional information processing in mood disorders: a review of behavioral and neuroimaging findings. Curr Opin Psychiatry 19: 34–39.
Linner L, Arborelius L, Nomikos GG, Bertilsson L, Svensson TH (1999). Locus coeruleus neuronal activity and noradrenaline availability in the frontal cortex of rats chronically treated with imipramine: effect of alpha 2-adrenoceptor blockade. Biol Psychiatry 46: 766–774.
Lira A, Zhou M, Castanon N, Ansorge MS, Gordon JA, Francis JH et al (2003). Altered depression-related behaviors and functional changes in the dorsal raphe nucleus of serotonin transporter-deficient mice. Biol Psychiatry 54: 960–971.
Myin-Germeys I, Peeters F, Havermans R, Nicolson NA, DeVries MW, Delespaul P et al (2003). Emotional reactivity to daily life stress in psychosis and affective disorder: an experience sampling study. Acta Psychiatr Scand 107: 124–131.
Myin-Germeys I, van Os J (2007). Stress-reactivity in psychosis: evidence for an affective pathway to psychosis. Clin Psychol Rev 27: 409–424.
Myin-Germeys I, van Os J, Schwartz JE, Stone AA, Delespaul PA (2001). Emotional reactivity to daily life stress in psychosis. Arch Gen Psychiatry 58: 1137–1144.
Nestler EJ, Carlezon Jr WA (2006). The mesolimbic dopamine reward circuit in depression. Biol Psychiatry 59: 1151–1159.
Nutt D, Demyttenaere K, Janka Z, Aarre T, Bourin M, Canonico PL et al (2007). The other face of depression, reduced positive affect: the role of catecholamines in causation and cure. J Psychopharmacol 21: 461–471.
Peeters F, Nicolson NA, Berkhof J, Delespaul P, deVries M (2003). Effects of daily events on mood states in major depressive disorder. J Abnorm Psychol 112: 203–211.
Rygula R, Abumaria N, Flugge G, Hiemke C, Fuchs E, Ruther E et al (2006). Citalopram counteracts depressive-like symptoms evoked by chronic social stress in rats. Behav Pharmacol 17: 19–29.
Sajdyk TJ, Johnson PL, Leitermann RJ, Fitz SD, Dietrich A, Morin M et al (2008). Neuropeptide Y in the amygdala induces long-term resilience to stress-induced reductions in social responses but not hypothalamic-adrenal-pituitary axis activity or hyperthermia. J Neurosci 28: 893–903.
Salamone JD, Correa M, Mingote S, Weber SM (2003). Nucleus accumbens dopamine and the regulation of effort in food-seeking behavior: implications for studies of natural motivation, psychiatry, and drug abuse. J Pharmacol Exp Ther 305: 1–8.
Shankman SA, Klein DN, Tenke CE, Bruder GE (2007). Reward sensitivity in depression: a biobehavioral study. J Abnorm Psychol 116: 95–104.
Sloan DM, Strauss ME, Quirk SW, Sajatovic M (1997). Subjective and expressive emotional responses in depression. J Affect Disord 46: 135–141.
Snijders T, Bosker R (1999). Multilevel Analysis: An Introduction to Basis and Advanced Multilevel Modeling. SAGE publications Ltd: London.
Steptoe A, Gibson EL, Hamer M, Wardle J (2007). Neuroendocrine and cardiovascular correlates of positive affect measured by ecological momentary assessment and by questionnaire. Psychoneuroendocrinology 32: 56–64.
Strand EB, Zautra AJ, Thoresen M, Odegard S, Uhlig T, Finset A (2006). Positive affect as a factor of resilience in the pain-negative affect relationship in patients with rheumatoid arthritis. J Psychosom Res 60: 477–484.
Tomarken AJ, Dichter GS, Freid C, Addington S, Shelton RC (2004). Assessing the effects of bupropion SR on mood dimensions of depression. J Affect Disord 78: 235–241.
Tong J, Hornykiewicz O, Kish SJ (2006). Identification of a noradrenaline-rich subdivision of the human nucleus accumbens. J Neurochem 96: 349–354.
Tugade MM, Fredrickson BL (2004). Resilient individuals use positive emotions to bounce back from negative emotional experiences. J Pers Soc Psychol 86: 320–333.
Von Frijtag JC, Van den Bos R, Spruijt BM (2002). Imipramine restores the long-term impairment of appetitive behavior in socially stressed rats. Psychopharmacology (Berl) 162: 232–238.
Vyas A, Jadhav S, Chattarji S (2006). Prolonged behavioral stress enhances synaptic connectivity in the basolateral amygdala. Neuroscience 143: 387–393.
Watson D, Tellegen A (1985). Toward a consensual structure of mood. Psychol Bull 98: 219–235.
Watson D, Wiese D, Vaidya J, Tellegen A (1999). The two general activation systems of affect: structural findings, evolutionary considerations, and psychobiological evidence. J Pers Soc Psychol 76: 820–838.
Wellman CL, Izquierdo A, Garrett JE, Martin KP, Carroll J, Millstein R et al (2007). Impaired stress-coping and fear extinction and abnormal corticolimbic morphology in serotonin transporter knock-out mice. J Neurosci 27: 684–691.
Wichers M, Aguilera M, Kenis G, Krabbendam L, Myin-Germeys I, Jacobs N et al (2007a). The Catechol-O-methyl transferase Val(158)Met polymorphism and experience of reward in the flow of daily life. Neuropsychopharmacology [E-pub ahead of print 8 August 2007].
Wichers MC, Kenis G, Jacobs N, Myin-Germeys I, Derom C, Vlietinck R et al (submitted manuscript). Genetic sensitivity for social stress associated with BDNF Val/Met is neutralised by positive emotional experiences.
Wichers MC, Myin-Germeys I, Jacobs N, Peeters F, Kenis G, Derom C et al (2007b). Evidence that moment-to-moment variation in positive emotions buffer genetic risk for depression: a momentary assessment twin study. Acta Psychiatr Scand 115: 451–457.
Wichers MC, Myin-Germeys I, Jacobs N, Peeters F, Kenis G, Derom C et al (2007c). Genetic risk of depression and stress-induced negative affect in the flow of daily life. Br J Psychiatry 191: 218–223.
Yang RJ, Mozhui K, Karlsson RM, Cameron HA, Williams RW, Holmes A (2008). Variation in mouse basolateral amygdala volume is associated with differences in stress reactivity and fear learning. Neuropsychopharmacology [E-pub ahead of print].
Acknowledgements
This study was supported by a research grant from Solvay Pharmaceuticals BV. We gratefully acknowledge the assistance of PMLF, Verburg-Noteborn, CJM van der Voort-Duindam, GHM Driesen, and FJ Delespaul-van Goethem in the data collection and processing and thank PAEG Delespaul for advice on the use of ESM. We are also indebted to MFJ Bemelmans, RHJ Brouwers, G Costongs, ACJ Schlösser, JJM Theunissen, PGJ van Aubel, DJM van der Voort, and M Weijts for subject recruitment and clinical assessments and, of course, to the participants themselves. Dr MC Wichers was supported by the Dutch Medical Council (VENI Grant no. 916.76.147).
Author information
Authors and Affiliations
Corresponding author
Additional information
DISCLOSURE
Over the past 3 years, Jim van Os has been a research grant holder, or has received financial compensation as a speaker or advisory board member with Eli Lilly, BMS, Lundbeck, Organon, Janssen-Cilag, GSK, Otsuka, and AstraZeneca. Frenk Peeters has received financial compensation as a speaker from Wyeth, Glaxo-SmithKlineBeecham, Lundbeck, and Astra Zeneca.
Rights and permissions
About this article
Cite this article
Wichers, M., Barge-Schaapveld, D., Nicolson, N. et al. Reduced Stress-Sensitivity or Increased Reward Experience: The Psychological Mechanism of Response to Antidepressant Medication. Neuropsychopharmacol 34, 923–931 (2009). https://doi.org/10.1038/npp.2008.66
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/npp.2008.66
Keywords
This article is cited by
-
Increases in External Sensory Observing Cross-Sectionally Mediate the Repair of Positive Affect Following Mindfulness-Based Cognitive Therapy in Individuals with Residual Depression Symptoms
Mindfulness (2023)
-
Bio-Behavioral Indices of Emotion Regulation: Potential Targets for Treatment in Addiction
Current Addiction Reports (2020)
-
Daily Interpersonal and Noninterpersonal Stress Reactivity in Current and Remitted Depression
Cognitive Therapy and Research (2020)
-
Economic evaluation of an experience sampling method intervention in depression compared with treatment as usual using data from a randomized controlled trial
BMC Psychiatry (2017)
-
The Effects of Psychotherapy for Major Depressive Disorder on Daily Mood and Functioning: A Longitudinal Experience Sampling Study
Cognitive Therapy and Research (2017)