Abstract
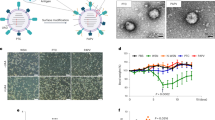
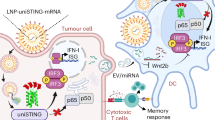
Nanotechnology has tremendous potential to contribute to cancer immunotherapy. The ‘in situ vaccination’ immunotherapy strategy directly manipulates identified tumours to overcome local tumour-mediated immunosuppression and subsequently stimulates systemic antitumour immunity to treat metastases. We show that inhalation of self-assembling virus-like nanoparticles from cowpea mosaic virus (CPMV) reduces established B16F10 lung melanoma and simultaneously generates potent systemic antitumour immunity against poorly immunogenic B16F10 in the skin. Full efficacy required Il-12, Ifn-γ, adaptive immunity and neutrophils. Inhaled CPMV nanoparticles were rapidly taken up by and activated neutrophils in the tumour microenvironment as an important part of the antitumour immune response. CPMV also exhibited clear treatment efficacy and systemic antitumour immunity in ovarian, colon, and breast tumour models in multiple anatomic locations. CPMV nanoparticles are stable, nontoxic, modifiable with drugs and antigens, and their nanomanufacture is highly scalable. These properties, combined with their inherent immunogenicity and demonstrated efficacy against a poorly immunogenic tumour, make CPMV an attractive and novel immunotherapy against metastatic cancer.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
References
Pardoll, D. M. The blockade of immune checkpoints in cancer immunotherapy. Nat. Rev. Cancer 12, 252–264 (2012).
Kershaw, M. H., Westwood, J. A. & Darcy, P. K. Gene-engineered T cells for cancer therapy. Nat. Rev. Cancer 13, 525–541 (2013).
Ali, O. A. et al. Identification of immune factors regulating antitumor immunity using polymeric vaccines with multiple adjuvants. Cancer Res. 74, 1670–1681 (2014).
Callahan, M. K., Postow, M. A. & Wolchok, J. D. CTLA-4 and PD-1 pathway blockade: combinations in the clinic. Front. Oncol. 4, ( 2015).
Winograd, R. et al. Induction of T cell immunity overcomes complete resistance to PD-1 and CTLA-4 blockade and improves survival in pancreatic carcinoma. Cancer Immunol. Res. 3, 399–411 (2015).
Robert, C. et al. Ipilimumab plus dacarbazine for previously untreated metastatic melanoma. N. Engl. J. Med. 364, 2517–2526 (2011).
Andtbacka, R. H. I. et al. Talimogene laherparepvec improves durable response rate in patients with advanced melanoma. J. Clin. Oncol. 33, 2780–2788 (2015).
Corrales, L. et al. Direct activation of STING in the tumor microenvironment leads to potent and systemic tumor regression and immunity. Cell Rep. 11, 1018–1030 (2015).
Sheen, M. R., Lizotte, P. H., Toraya-Brown, S. & Fiering, S. Stimulating antitumor immunity with nanoparticles. WIREs Nanomed. Nanobiotechnol. 6, 496–505 (2014).
Halperin, S. A. et al. Comparison of safety and immunogenicity of two doses of investigational hepatitis B virus surface antigen co-administered with an immunostimulatory phosphorothioate oligodeoxyribonucleotide and three doses of a licensed hepatitis B vaccine in healthy adults 18–55 years of age. Vaccine 30, 2556–2563 (2012).
Huber, B. et al. A chimeric 18L1-45RG1 virus-like particle vaccine cross-protects against oncogenic alpha-7 human papillomavirus types. PLoS ONE 10, e0120152 (2015).
Rynda-Apple, A., Patterson, D. P. & Douglas, T. Virus-like particles as antigenic nanomaterials for inducing protective immune responses in the lung. Nanomed. 9, 1857–1868 (2014).
Rynda-Apple, A. et al. Virus-like particle-induced protection against MRSA pneumonia is dependent on IL-13 and enhancement of phagocyte function. Am. J. Pathol. 181, 196–210 (2012).
Wiley, J. A. et al. Inducible bronchus-associated lymphoid tissue elicited by a protein cage nanoparticle enhances protection in mice against diverse respiratory viruses. PLoS ONE 4, e7142 (2009).
Patterson, D. P., Rynda-Apple, A., Harmsen, A. L., Harmsen, A. G. & Douglas, T. Biomimetic antigenic nanoparticles elicit controlled protective immune response to influenza. ACS Nano 7, 3036–3044 (2013).
Richert, L. E. et al. CD11c+ cells primed with unrelated antigens facilitate an accelerated immune response to influenza virus in mice. Eur. J. Immunol. 44, 397–408 (2014).
Saunders, K., Sainsbury, F. & Lomonossoff, G. P. Efficient generation of cowpea mosaicvirus empty virus-like particles by the proteolytic processing of precursors in insect cells and plants. Virology 393, 329–337 (2009).
Aljabali, A. A. A., Shukla, S., Lomonossoff, G. P., Steinmetz, N. F. & Evans, D. J. CPMV-DOX delivers. Mol. Pharm. 10, 3–10 (2013).
Yildiz, I., Lee, K. L., Chen, K., Shukla, S. & Steinmetz, N. F. Infusion of imaging and therapeutic molecules into the plant virus-based carrier cowpea mosaic virus: Cargo-loading and delivery. J. Controlled Release 172, 568–578 (2013).
Costantini, C. et al. Neutrophil activation and survival are modulated by interaction with NK cells. Int. Immunol. 22, 827-838 (2010).
Gabrilovich, D. I., Ostrand-Rosenberg, S. & Bronte, V. Coordinated regulation of myeloid cells by tumours. Nat. Rev. Immunol. 12, 253–268 (2012).
Fridlender, Z. G. et al. Polarization of tumor-associated neutrophil (TAN) phenotype by TGF-β: ‘N1’ versus ‘N2’ TAN. Cancer Cell 16, 183–194 (2009).
Mantovani, A., Cassatella, M. A., Costantini, C. & Jaillon, S. Neutrophils in the activation and regulation of innate and adaptive immunity. Nat. Rev. Immunol. 11, 519–531 (2011).
Zhu, M.-L., Nagavalli, A. & Su, M. A. Aire deficiency promotes TRP-1–specific immune rejection of melanoma. Cancer Res. 73, 2104–2116 (2013).
Conejo-Garcia, J. R. et al. Tumor-infiltrating dendritic cell precursors recruited by a β-defensin contribute to vasculogenesis under the influence of Vegf-A. Nature Med. 10, 950–958 (2004).
Lebel, M.-È. et al. Nanoparticle adjuvant sensing by TLR7 enhances CD8+ T cell–mediated protection from listeria monocytogenes infection. J. Immunol. 192, 1071–1078 (2014).
Link, A. et al. Innate immunity mediates follicular transport of particulate but not soluble protein antigen. J. Immunol. 188, 3724–3733 (2012).
Wu, G. J. & Bruening, G. Two proteins from cowpea mosaic virus. Virology 46, 596–612 (1971).
Steinmetz, N. F., Cho, C.-F., Ablack, A., Lewis, J. D. & Manchester, M. Cowpea mosaic virus nanoparticles target surface vimentin on cancer cells. Nanomed. 6, 351–364 (2011).
Satelli, A. & Li, S. Vimentin in cancer and its potential as a molecular target for cancer therapy. Cell. Mol. Life Sci. 68, 3033–3046 (2011).
Gonzalez, M. J., Plummer, E. M., Rae, C. S. & Manchester, M. Interaction of cowpea mosaic virus (CPMV) nanoparticles with antigen presenting cells in vitro and in vivo. PLoS ONE 4, e7981 (2009).
Jablonska, J., Leschner, S., Westphal, K., Lienenklaus, S. & Weiss, S. Neutrophils responsive to endogenous IFN-β regulate tumor angiogenesis and growth in a mouse tumor model. J. Clin. Invest. 120, 1151–1164 (2010).
Kuang, D.-M. et al. Peritumoral neutrophils link inflammatory response to disease progression by fostering angiogenesis in hepatocellular carcinoma. J. Hepatol. 54, 948–955 (2011).
Pekarek, L. A., Starr, B. A., Toledano, A. Y. & Schreiber, H. Inhibition of tumor growth by elimination of granulocytes. J. Exp. Med. 181, 435–440 (1995).
Wislez, M. et al. Hepatocyte growth factor production by neutrophils infiltrating bronchioloalveolar subtype pulmonary adenocarcinoma role in tumor progression and death. Cancer Res. 63, 1405–1412 (2003).
Abdallah, D. S. A., Egan, C. E., Butcher, B. A. & Denkers, E. Y. Mouse neutrophils are professional antigen-presenting cells programmed to instruct Th1 and Th17 T-cell differentiation. Int. Immunol. 23, 317–326 (2011).
van Gisbergen, K. P. J. M., Sanchez-Hernandez, M., Geijtenbeek, T. B. H. & van Kooyk, Y. Neutrophils mediate immune modulation of dendritic cells through glycosylation-dependent interactions between Mac-1 and DC-SIGN. J. Exp. Med. 201, 1281–1292 (2005).
Beauvillain, C. et al. Neutrophils efficiently cross-prime naive T cells in vivo. Blood 110, 2965–2973 (2007).
Pelletier, M. et al. Evidence for a cross-talk between human neutrophils and Th17 cells. Blood 115, 335–343 (2010).
Clancy-Thompson, E. et al. Peptide vaccination in montanide adjuvant induces and GM-CSF increases CXCR3 and cutaneous lymphocyte antigen expression by tumor antigen–specific CD8 T cells. Cancer Immunol. Res. 1, 332–339 (2013).
Baird, J. R. et al. Immune-mediated regression of established B16F10 melanoma by intratumoral injection of attenuated toxoplasma gondii protects against rechallenge. J. Immunol. 190, 469–478 (2013).
Caramori, G., Adcock, I. M., Di Stefano, A. & Chung, K. F. Cytokine inhibition in the treatment of COPD. Int. J. Chron. Obstruct. Pulmon. Dis. 9, 397–412 (2014).
Lizotte, P. H. et al. Attenuated Listeria monocytogenes reprograms M2-polarized tumor-associated macrophages in ovarian cancer leading to iNOS-mediated tumor cell lysis. Oncoimmunology 3, ( 2014).
Baird, J. R. et al. Avirulent toxoplasma gondii generates therapeutic antitumor immunity by reversing immunosuppression in the ovarian cancer microenvironment. Cancer Res. 73, 3842–3851 (2013).
Scarlett, U. K. et al. In situ stimulation of CD40 and toll-like receptor 3 transforms ovarian cancer–infiltrating dendritic cells from immunosuppressive to immunostimulatory cells. Cancer Res. 69, 7329–7337 (2009).
Hart, K., Byrne, K., Molloy, M., Usherwood, E. & Berwin, B. IL-10 immunomodulation of myeloid cells regulates a murine model of ovarian cancer. T Cell Biol. 2, 29 (2011).
Sainsbury, F. et al. Genetic engineering and characterisation of Cowpea mosaic virus empty virus-like particles. Methods Mol Biol Clifton NJ. 1108, 139–153 (2014).
Lizotte, P. H., et al. Attenuated Listeria monocytogenes reprograms M2-polarized tumour-associated macrophages in ovarian cancer leading to iNOS-mediated tumour cell lysis. Oncoimmunology 3, e28926 (2014)
Pulaski, B. A. & Ostrand-Rosenberg, S. in Current Protocols in Immunology (eds Cooligan, J. E. et al.) 39:20.2:20.2.1–20.2.16 (John Wiley & Sons, 2001); http://onlinelibrary.wiley.com/doi/10.1002/0471142735.im2002s39/abstract.
Acknowledgements
George P. Lomonossoff (John Innes Centre, UK) is thanked for providing the pEAQexpress-VP60-24K plasmid. We thank the following for their assistance: Zachary Parker; the lab of David Mullins; the lab of Brent Berwin; the Immune Monitoring Lab and DartLab at the Geisel School of Medicine at Dartmouth, particularly Gary Ward and John DeLong; the Dartmouth Transgenic and Genetic shared resource; the Dartmouth Hitchcock Medical Center pathology department; the Irradiation, Pre-clinical Imaging, and Microscopy (IPIM) and Genomics/Molecular Biology (GMB) shared resources at the Norris Cotton Cancer Center. Shared resources at Dartmouth are made possible through generous Centers of Biomedical Research Excellence support. Work was supported by Dartmouth Immunobiology of Myeloid and Lymphoid Cells National Institutes of Health Training Grant 5T32AI007363–22 (P.H.L.), Case Western Reserve University Cardiovascular Research National Institutes of Health Training Grant T32 HL105338 (A.M.W.), National Science Foundation CMMI 1333651 (N.F.S.), Dartmouth Center of Nanotechnology Excellence NIH 1 U54 CA151662 (S.F.), Center for Molecular, Cellular, and Translational Immunological Research NIGMS 1P30RR032136–01 (S.F.), and Norris Cotton Cancer Center P30 CA023108-27 (S.F.).
Author information
Authors and Affiliations
Contributions
P.H.L., N.F.S., and S.F. conceived and designed the experiments, and wrote the manuscript. P.H.L., A.M.W., P.R., M.R.S., and J.F. performed the experiments. M.R.S. was responsible for Supplementary Fig. 4. P.R. was responsible for Supplementary Fig. 6. A.M.W. was responsible for Supplementary Fig. 8. P.H.L. performed all other experiments and analysed the data. J.F. assisted with in vivo work. All authors commented on the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors have a patent pending for the immunotherapeutic use of the eCPMV nanoparticle.
Supplementary information
Supplementary information
Supplementary information (PDF 757 kb)
Rights and permissions
About this article
Cite this article
Lizotte, P., Wen, A., Sheen, M. et al. In situ vaccination with cowpea mosaic virus nanoparticles suppresses metastatic cancer. Nature Nanotech 11, 295–303 (2016). https://doi.org/10.1038/nnano.2015.292
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nnano.2015.292