Abstract
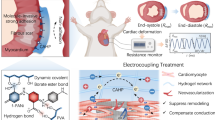
In cardiac tissue engineering approaches to treat myocardial infarction, cardiac cells are seeded within three-dimensional porous scaffolds to create functional cardiac patches. However, current cardiac patches do not allow for online monitoring and reporting of engineered-tissue performance, and do not interfere to deliver signals for patch activation or to enable its integration with the host. Here, we report an engineered cardiac patch that integrates cardiac cells with flexible, freestanding electronics and a 3D nanocomposite scaffold. The patch exhibited robust electronic properties, enabling the recording of cellular electrical activities and the on-demand provision of electrical stimulation for synchronizing cell contraction. We also show that electroactive polymers containing biological factors can be deposited on designated electrodes to release drugs in the patch microenvironment on demand. We expect that the integration of complex electronics within cardiac patches will eventually provide therapeutic control and regulation of cardiac function.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
References
Dvir, T., Timko, B. P., Kohane, D. S. & Langer, R. Nanotechnological strategies for engineering complex tissues. Nature Nanotech. 6, 13–22 (2011).
Fleischer, S. et al. Spring-like fibers for cardiac tissue engineering. Biomaterials 34, 8599–8606 (2013).
Chiu, L. L., Janic, K. & Radisic, M. Engineering of oriented myocardium on three-dimensional micropatterned collagen-chitosan hydrogel. Int. J. Artif. Organs 35, 237–250 (2012).
Engelmayr, G. C. Jr et al. Accordion-like honeycombs for tissue engineering of cardiac anisotropy. Nature Mater. 7, 1003–1010 (2008).
Kim, D. H. et al. Nanoscale cues regulate the structure and function of macroscopic cardiac tissue constructs. Proc. Natl Acad. Sci. USA 107, 565–570 (2010).
Radisic, M. et al. Biomimetic approach to cardiac tissue engineering: oxygen carriers and channeled scaffolds. Tissue Eng. 12, 2077–2091 (2006).
Eschenhagen, T. et al. Three-dimensional reconstitution of embryonic cardiomyocytes in a collagen matrix: a new heart muscle model system. FASEB J. 11, 683–694 (1997).
Shevach, M., Maoz, B. M., Feiner, R., Shapira, A. & Dvir, T. Nanoengineering gold particle composite fibers for cardiac tissue engineering. J. Mater. Chem. B 1, 5210–5217 (2013).
Fleischer, S. et al. Albumin fiber scaffolds for engineering functional cardiac tissues. Biotechnol. Bioeng. 111, 1246–1257 (2014).
Bian, W., Jackman, C. P. & Bursac, N. Controlling the structural and functional anisotropy of engineered cardiac tissues. Biofabrication 6, 024109 (2014).
Dvir, T. et al. Prevascularization of cardiac patch on the omentum improves its therapeutic outcome. Proc. Natl Acad. Sci. USA 106, 14990–14995 (2009).
Zimmermann, W. H. et al. Engineered heart tissue grafts improve systolic and diastolic function in infarcted rat hearts. Nature Med. 12, 452–458 (2006).
Radisic, M. et al. Functional assembly of engineered myocardium by electrical stimulation of cardiac myocytes cultured on scaffolds. Proc. Natl Acad. Sci. USA 101, 18129–18134 (2004).
Marsano, A. et al. The effect of controlled expression of VEGF by transduced myoblasts in a cardiac patch on vascularization in a mouse model of myocardial infarction. Biomaterials 34, 393–401 (2013).
Tian, B. et al. Macroporous nanowire nanoelectronic scaffolds for synthetic tissues. Nature Mater. 11, 986–994 (2012).
Tian, B. et al. Three-dimensional, flexible nanoscale field-effect transistors as localized bioprobes. Science 329, 830–834 (2010).
Duan, X., Fu, T. M., Liu, J. & Lieber, C. M. Nanoelectronics–biology frontier: from nanoscopic probes for action potential recording in live cells to three-dimensional cyborg tissues. Nano Today 8, 351–373 (2013).
Cogan, S. F. Neural stimulation and recording electrodes. Annu. Rev. Biomed. Eng. 10, 275–309 (2008).
Lampin, M., Warocquier, C., Legris, C., Degrange, M. & Sigot-Luizard, M. F. Correlation between substratum roughness and wettability, cell adhesion, and cell migration. J. Biomed. Mater. Res. 36, 99–108 (1997).
Jensen, M., Hansen, P. B., Murdan, S., Frokjaer, S. & Florence, A. T. Loading into and electro-stimulated release of peptides and proteins from chondroitin 4-sulphate hydrogels. Eur. J. Pharm. Sci. 15, 139–148 (2002).
Pillay, V. et al. A review of integrating electroactive polymers as responsive systems for specialized drug delivery applications. J. Biomed. Mater. Res. A 102, 2039–2054 (2014).
Levesque, J. P., Hendy, J., Takamatsu, Y., Simmons, P. J. & Bendall, L. J. Disruption of the CXCR4/CXCL12 chemotactic interaction during hematopoietic stem cell mobilization induced by GCSF or cyclophosphamide. J. Clin. Invest. 111, 187–196 (2003).
Aiuti, A., Webb, I. J., Bleul, C., Springer, T. & Gutierrez-Ramos, J. C. The chemokine SDF-1 is a chemoattractant for human CD34 + hematopoietic progenitor cells and provides a new mechanism to explain the mobilization of CD34 + progenitors to peripheral blood. J. Exp. Med. 185, 111–120 (1997).
Leor, J., Amsalem, Y. & Cohen, S. Cells, scaffolds, and molecules for myocardial tissue engineering. Pharmacol. Ther. 105, 151–163 (2005).
Wadhwa, R., Lagenaur, C. F. & Cui, X. T. Electrochemically controlled release of dexamethasone from conducting polymer polypyrrole coated electrode. J. Control. Release 110, 531–541 (2006).
Tsurufuji, S., Sugio, K. & Takemasa, F. The role of glucocorticoid receptor and gene expression in the anti-inflammatory action of dexamethasone. Nature 280, 408–410 (1979).
Patil, S. D., Papadmitrakopoulos, F. & Burgess, D. J. Concurrent delivery of dexamethasone and VEGF for localized inflammation control and angiogenesis. J. Control. Release 117, 68–79 (2007).
Mond, H. G., Helland, J. R., Stokes, K., Bornzin, G. A. & McVenes, R. The electrode–tissue interface: the revolutionary role of steroid-elution. Pacing Clin. Electrophysiol. 37, 1232–1249 (2014).
Kim, J. H. et al. Sulfated chitosan oligosaccharides suppress LPS-induced NO production via JNK and NF-κB inactivation. Molecules 19, 18232–18247 (2014).
Zinger, B. & Miller, L. L. Timed release of chemicals from polypyrrole films. J. Am. Chem. Soc. 106, 6861–6863 (1984).
Sivakumar, R., Anandh Babu, P. V. & Shyamaladevi, C. S. Protective effect of aspartate and glutamate on cardiac mitochondrial function during myocardial infarction in experimental rats. Chem. Biol. Interact. 176, 227–233 (2008).
Fleischer, S. & Dvir, T. Tissue engineering on the nanoscale: lessons from the heart. Curr. Opin. Biotechnol. 24, 664–671 (2013).
Pope, A. J., Sands, G. B., Smaill, B. H. & LeGrice, I. J. Three-dimensional transmural organization of perimysial collagen in the heart. Am. J. Physiol. Heart Circ. Physiol. 295, H1243–H1252 (2008).
Zimmermann, W. H. et al. Tissue engineering of a differentiated cardiac muscle construct. Circ. Res. 90, 223–230 (2002).
Nunes, S. S. et al. Biowire: a platform for maturation of human pluripotent stem cell-derived cardiomyocytes. Nature Methods 10, 781–787 (2013).
Bursac, N. et al. Cardiac muscle tissue engineering: toward an in vitro model for electrophysiological studies. Am. J. Physiol. 277, H433–H444 (1999).
Iyer, R. K., Chiu, L. L., Reis, L. A. & Radisic, M. Engineered cardiac tissues. Curr. Opin. Biotechnol. 22, 706–714 (2011).
Tandon, N. et al. Electrical stimulation systems for cardiac tissue engineering. Nature Protocols 4, 155–173 (2009).
Kim, D. H., Ghaffari, R., Lu, N. & Rogers, J. A. Flexible and stretchable electronics for biointegrated devices. Annu. Rev. Biomed. Eng. 14, 113–128 (2012).
Kim, D. H. & Rogers, J. A. Stretchable electronics: materials strategies and devices. Adv. Mater. 20, 4887–4892 (2008).
Rogers, J. A., Someya, T. & Huang, Y. Materials and mechanics for stretchable electronics. Science 327, 1603–1607 (2010).
Xu, L. et al. Materials and fractal designs for 3D multifunctional integumentary membranes with capabilities in cardiac electrotherapy. Adv. Mater. 27, 1731–1737 (2015).
Zhang, Y., Ouyang, H., Lim, C. T., Ramakrishna, S. & Huang, Z. M. Electrospinning of gelatin fibers and gelatin/PCL composite fibrous scaffolds. J. Biomed. Mater. Res. 72, 156–165 (2005).
Shevach, M., Fleischer, S., Shapira, A. & Dvir, T. Gold nanoparticle-decellularized matrix hybrids for cardiac tissue engineering. Nano Lett. 14, 5792–5796 (2014).
Acknowledgements
T.D. acknowledges support from European Research Council (ERC) Starting Grant 637943, the European Union FP7 programme (Marie Curie, CIG), an Alon Fellowship, the Slezak Foundation, and the Israeli Science Foundation (700/13). R.F. thanks the Marian Gertner Institute for Medical Nanosystems Fellowship. The work is part of the doctoral thesis of R.F. at Tel Aviv University. We would like to thank T. Yoetz and N. Noor for technical assistance.
Author information
Authors and Affiliations
Contributions
R.F. and T.D. conceived the idea and designed the experiments. R.F. performed all experiments. L.E. assisted in microfabrication and characterization of the electronics. S.F. and A.S. performed cell culture work. M.M. and I.G. assisted in drug release experiments. Y.S.-D. analysed data. R.F. and T.D. wrote the manuscript. The study was directed by T.D.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Supplementary Information
Supplementary Information (PDF 3141 kb)
Supplementary Movie 1
Supplementary Movie 1 (AVI 1048 kb)
Supplementary Movie 2
Supplementary Movie 2 (AVI 1085 kb)
Supplementary Movie 3
Supplementary Movie 3 (AVI 1100 kb)
Supplementary Movie 4
Supplementary Movie 4 (AVI 4041 kb)
Supplementary Movie 5
Supplementary Movie 5 (AVI 4588 kb)
Rights and permissions
About this article
Cite this article
Feiner, R., Engel, L., Fleischer, S. et al. Engineered hybrid cardiac patches with multifunctional electronics for online monitoring and regulation of tissue function. Nature Mater 15, 679–685 (2016). https://doi.org/10.1038/nmat4590
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nmat4590
This article is cited by
-
Graphene-integrated mesh electronics with converged multifunctionality for tracking multimodal excitation-contraction dynamics in cardiac microtissues
Nature Communications (2024)
-
Optimizing the fabrication of a 3D high-resolution implant for neural stimulation
Journal of Biological Engineering (2023)
-
Chronological adhesive cardiac patch for synchronous mechanophysiological monitoring and electrocoupling therapy
Nature Communications (2023)
-
Electro-metabolic coupling in multi-chambered vascularized human cardiac organoids
Nature Biomedical Engineering (2023)
-
Nanomedicines for cardiovascular disease
Nature Cardiovascular Research (2023)