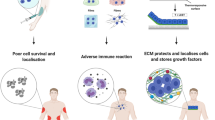
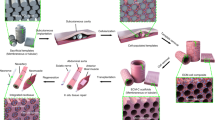
Abstract
A paradigm shift is taking place in medicine from using synthetic implants and tissue grafts to a tissue engineering approach that uses degradable porous material scaffolds integrated with biological cells or molecules to regenerate tissues. This new paradigm requires scaffolds that balance temporary mechanical function with mass transport to aid biological delivery and tissue regeneration. Little is known quantitatively about this balance as early scaffolds were not fabricated with precise porous architecture. Recent advances in both computational topology design (CTD) and solid free-form fabrication (SFF) have made it possible to create scaffolds with controlled architecture. This paper reviews the integration of CTD with SFF to build designer tissue-engineering scaffolds. It also details the mechanical properties and tissue regeneration achieved using designer scaffolds. Finally, future directions are suggested for using designer scaffolds with in vivo experimentation to optimize tissue-engineering treatments, and coupling designer scaffolds with cell printing to create designer material/biofactor hybrids.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
References
Sanan, A. & Haines, S. J. Repairing holes in the head: a history of cranioplasty. J. Neurosurg. 40, 588–603 (1997).
Langer, R. & Vacanti, J. P. Tissue engineering. Science 260, 920–926 (1993).
Audet, J. Stem cell bioengineering for regenerative medicine. Expert Opin. Biol. Ther. 4, 631–644 (2004).
Caplan, A. I., Reuben, D. & Haynesworth, S. E. Cell-based tissue engineering therapies: the influence of whole body physiology. Adv. Drug Deliv. Rev. 33, 3–14 (1998).
Bonadio, J. Tissue engineering via local gene delivery. J. Mol. Med. 78, 303–311 (2000).
Cutroneo, K. R. Gene therapy for tissue regeneration. J. Cell Biochem. 88 418–425 (2003).
Hashin, Z. & Shtrikman, S. A variational approach to the theory of the elastic behavior of multiphase materials. J. Mech. Phys. Solids 11, 127–140 (1962).
Torquato, S. Random Heterogenous Materials: Microstructure and Macroscopic Properties (Springer, New York, 2002).
Hollister, S. J., Levy R. A., Chu, T. M., Halloran, J. W. & Feinberg, S. E. An image-based approach for designing and manufacturing craniofacial scaffolds. Int. J. Oral Maxillofac. Surg. 29, 67–71 (2002).
Hollister, S. J., Maddox, R. D. & Taboas, J. M. Optimal design and fabrication of scaffolds to mimic tissue properties and satisfy biological constraints. Biomater. 23, 4095–4103 (2002).
Lin, C. Y., Kikuchi, N. & Hollister, S. J. A novel method for biomaterial scaffold internal architecture design to match bone elastic properties with desired porosity. J. Biomech. 37, 623–636 (2004).
Sun, W., Starly, B., Darling, A. & Gomez, C. Computer-aided tissue engineering: application to biomimetic modelling and design of tissue scaffolds. Biotechnol. Appl. Biochem. 39, 49–58 (2004).
Sun, W., Darling, A., Starly, B. & Nam, J. Computer-aided tissue engineering: overview, scope and challenges. Biotechnol. Appl. Biochem. 39, 29–47 (2004).
Fang, Z., Starly, B. & Sun, W. Computer-aided characterization for effective mechanical properties of porous tissue scaffolds. Comput. Aid. Design 37, 65–72 (2005).
Cheah, C. M., Chua, C. K., Leong, K. F., Cheong, C. H. & Naing, M. W. Automatic algorithm for generating complex polyhedral scaffold structures for tissue engineering. Tissue Eng. 10 595–610 (2004).
Van Cleyenbreugel, T., Van Oosterwyck, H., Vander Sloten J. & Schrooten J. Trabecular bone scaffolding using a biomimetic approach. J. Mater Sci. Mater. Med. 13, 1245–1249 (2002).
Yang, S., Leong, K. F., Du, Z. & Chua, C. K. The design of scaffolds for use in tissue engineering. Part II. Rapid prototyping techniques. Tissue Eng. 8, 1–11 (2002).
Sanchez-Palencia, E. & Zaoui, A. Homogenization Techniques for Composite Media (Springer, Berlin, 1987).
Hollister, S. J. & Kikuchi, N. Homogenization theory and digital imaging: a basis for studying the mechanics and design principles of bone tissue. Biotech. Bioeng. 43, 586–596 (1994).
Terada, K., Ito T. & Kikuchi, N. Characterization of the mechanical behaviors of solid-fluid mixture by the homogenization method. Comp. Meth. App. Mech. Eng. 153, 223–257 (1998).
Sigmund, O. Materials with prescribed constitutive parameters – an inverse homogenization problem. J. Solids Struct. 31, 2513–2529 (1994).
Lin, C. Y., Hsiao, C. C., Chen P. Q. & Hollister, S. J. Interbody fusion cage design using integrated global layout and local microstructure topology optimization. Spine 29, 1747–1754 (2004).
Hutmacher, D. W., Sittinger, M. & Risbud, M. V. Scaffold-based tissue engineering: rationale for computer-aided design and solid free-form fabrication systems. Trends Biotechnol. 22, 354–362 (2004).
Leong, K. F., Cheah, C. M. & Chua, C. K. Solid freeform fabrication of three-dimensional scaffolds for engineering replacement tissues and organs. Biomaterials 24, 2363–2378 (2003).
Sachlos, E. & Czernuszka, J. T. Making scaffolds work: a review on the application of solid freeform fabrication technology to the production of tissue engineering scaffolds. Eur. Cell Mater. 5, 29–40 (2003).
Tsang, V. L. & Bhatia, S. N. Three dimensional tissue fabrication. Adv. Drug Deliv. 56, 1635–1647 (2004).
Yeong, W. Y., Chua, C. K., Leong, K. F. & Chandrasekaran, M. Rapid prototyping in tissue engineering: challenges and potential. Trends Biotechnol. 22, 643–652 (2004).
Bose, S. et al. Processing and characterization of porous alumina scaffolds. J. Mater. Sci. Mater. Med. 13, 23–28 (2002).
Chu, T. M., Hollister, S. J., Halloran, J. W., Feinberg, S. E. & Orton, D. G. Manufacturing and characterization of 3-d hydroxyapatite bone tissue engineering scaffolds. Ann. NY Acad. Sci. 961, 114–117 (2002).
Chua, C. K., Leong, K. F., Tan, K. H., Wiria, F. E. & Cheah, C. M. Development of tissue scaffolds using selective laser sintering of polyvinyl alcohol/hydroxyapatite biocomposite for craniofacial and joint defects. J. Mater. Sci. Mater. Med. 15, 1113–1121 (2004).
Ciardelli, G. et al. Innovative tissue engineering structures through advanced manufacturing technologies. J. Mater. Sci. Mater. Med. 15, 305–310 (2004).
Cooke, M. N., Fisher, J. P., Dean, D., Rimnac, C. & Mikos, A. G. Use of stereolithography to manufacture critical-sized 3D biodegradable scaffolds for bone ingrowth. J. Biomed. Mater. Res. 64B, 65–69 (2003).
Dhariwala, B., Hunt, E. & Boland, T. Rapid prototyping of tissue-engineering constructs, using photopolymerizable hydrogels and stereolithography. Tissue Eng. 10, 1316–1322 (2004).
Fisher, J. P. et al. A. Soft and hard tissue response to photocrosslinked poly(propylene fumarate) scaffolds in a rabbit model. J. Biomed. Mater. Res. 59, 547–556 (2002).
Giordano, R. A. et al. Mechanical properties of dense polylactic acid structures fabricated by three dimensional printing. J. Biomater. Sci. Polym. Edn 8, 63–75 (1996).
Hutmacher, D. W. et al. Mechanical properties and cell cultural response of polycaprolactone scaffolds designed and fabricated via fused deposition modeling. J. Biomed. Mater. Res. 55, 203–216 (2001).
Khalil, S., Nam J. & Sun, W. Multi-nozzle deposition for construction of 3D biopolymer tissue scaffolds. Rapid Prototyp. J. 11, 9–17 (2005).
Landers, R., Hubner, U., Schmelzeisen, R. & Mulhaupt, R. Rapid prototyping of scaffolds derived from thermoreversible hydrogels and tailored for applications in tissue engineering. Biomaterials 23, 4437–4447 (2002).
Levy, R. A., Chu, T. M., Halloran, J. W., Feinberg, S. E. & Hollister, S. J. CT-generated porous hydroxyapatite orbital floor prosthesis as a prototype bioimplant. Am. J. Neuroradiol. 18, 1522–1525 (1997).
Pfister, A. et al. Biofunctional rapid prototyping for tissue-engineering applications: 3D bioplotting versus 3D printing. J. Polym. Sci. 42, 624–638 (2004).
Sodian, R. et al. Application of stereolithography for scaffold fabrication for tissue engineered heart valves. Am. Soc. Artificial Internal Organs J. 48, 12–16 (2002).
Tan, K. H. et al. Selective laser sintering of biocompatible polymers for applications in tissue engineering. Biomed. Mater. Eng. 15, 113–124 (2005).
Vozzi, G., Flaim, C., Ahluwalia, A. & Bhatia, S. Fabrication of PLGA scaffolds using soft lithography and microsyringe deposition. Biomaterials 24, 2533–2540 (2003).
Wang, F. et al. Precision extruding deposition and characterization of poly-e-caprolactone tissue scaffolds. Rapid Prototype J. 10, 42–49 (2004).
Wilson, C. E., de Bruijn, J. D., van Blitterswijk, C. A., Verbout, A. J. & Dhert, W. J. Design and fabrication of standardized hydroxyapatite scaffolds with a defined macro-architecture by rapid prototyping for bone-tissue-engineering research. J. Biomed. Mate.r Res. A 68, 123–132 (2004).
Zein, I., Hutmacher, D. W., Tan, K. C. & Teoh, S. H. Fused deposition modeling of novel scaffold architectures for tissue engineering applications. Biomaterials 23, 1169–1185 (2002).
Koegler, W. S. & Griffith, L. G. Osteoblast response to PLGA tissue engineering scaffolds with PEO modified surface chemistries and demonstration of patterned cell response. Biomaterials 25, 2819–2830 (2004).
Taboas, J. M., Maddox, R. D., Krebsbach, P. H. & Hollister, S. J. Indirect solid free form fabrication of local and global porous, biomimetic and composite 3D polymer-ceramic scaffolds. Biomaterials 24, 181–194 (2003).
Park, A., Wu, B. & Griffith, L. G. Integration of surface modification and 3D fabrication techniques to prepare patterned poly(L-lactide) substrates allowing regionally selective cell adhesion. J. Biomater. Sci. Polym. Edn 9, 89–110 (1998).
Goulet, R. W. et al. The relationship between the structural and orthogonal compressive properties of trabecular bone, J. Biomech. 27m 375–389 (1994).
Hayashi, K. in Biomechanics of soft tissue in cardiovascular systems (eds Holzapfel, G. & Ogden, R. W.) 15–64 (Springer, New York, 2003).
Ma, P. X. & Choi, J. W. Biodegradable polymer scaffolds with well-defined interconnected spherical pore network. Tissue Eng. 7, 23–33 (2001).
Murphy, W. L., Dennis, R. G., Kileny, J. L. & Mooney, D. J. Salt fusion: an approach to improve pore interconnectivity within tissue engineering scaffolds. Tissue Eng. 8, 43–52 (2002).
Sherwood, J. K. et al. A three-dimensional osteochondral composite scaffold for articular cartilage repair. Biomaterials 23, 4739–4751 (2002).
Hutmacher, D. W. et al. Mechanical properties and cell cultural response of polycaprolactone scaffolds designed and fabricated via fused deposition modeling. J. Biomed. Mater. Res. 55, 203–216 (2001).
Williams, J. L. et al. Bone tissue engineering using polycaprolactone scaffolds fabricated via selective laser sintering. Biomaterials 26, 4817–4827 (2005).
Chu, T. M., Orton, D. G., Hollister, S. J., Feinberg, S. E. & Halloran, J. W. Mechanical and in vivo performance of hydroxyapatite implants with controlled architectures. Biomaterials 23, 1283–1293 (2002).
Woodfield, T. B. et al. Design of porous scaffolds for cartilage tissue engineering using a three-dimensional fiber-deposition technique. Biomaterials 25, 4149–4161 (2004).
Malda, J. et al. The effect of PEGT/PBT scaffold architecture on oxygen gradients in tissue engineered cartilaginous constructs. Biomaterials 25, 5773–5780 (2004).
Malda, J. et al. The effect of PEGT/PBT scaffold architecture on the composition of tissue engineered cartilage. Biomaterials 26, 63–72 (2005).
Saito, E., Partee, B., Das, S. & Hollister, S. J. Engineered wavy fibered polycaprolactone soft tissue scaffolds: design, fabrication and mechanical testing. Trans. 51st Orthopaedic Research Society Meeting 51, 1794 (2005).
Fisher, J. P. et al. Soft and hard tissue response to photocrosslinked poly(propylene fumarate) scaffolds in a rabbit model. J. Biomed. Mater. Res. 59, 547–556 (2002).
Rohner, D., Hutmacher, D. W., Cheng, T. K., Oberholzer, M. & Hammer, B. In vivo efficacy of bone marrow-coated polycaprolactone scaffolds for the reconstruction of orbital defects in the pig. J. Biomed. Mater. Res. 66B, 574–580 (2003).
Roy, T. D. et al. Performance of degradable composite bone repair products made via three-dimensional fabrication techniques. J. Biomed. Mater. Res. 66A, 283–291 (2003).
Simon, J. L. et al. Engineered cellular response to scaffold architecture in a rabbit trephine defect. J. Biomed. Mater. Res. 66A, 275–282 (2003).
Hollister, S. J. et al. Engineering craniofacial scaffolds. Orthod. Craniofac. Res. (in the press).
Lin, C. Y. et al. Functional bone tissue engineering using ex vivo gene therapy and topology optimized, biodegradable polymer composite scaffolds. Tissue Eng. (in the press).
Schek, R. M., Taboas, J.M., Segvich, S.J., Hollister, S. J. & Krebsbach, P. H. Engineered osteochondral grafts using biphasic composite solid free-form fabricated scaffolds. Tissue Eng. 10, 1376–1385 (2004).
Wilson, W. C. Jr & Boland, T. Cell and organ printing 1: protein and cell printers. Anat. Rec. 272A, 491–496 (2003).
Roth, E. A. et al. Inkjet printing for high throughput cell patterning. Biomaterials 25, 3707–3715 (2004).
Xu, T., Jin, J., Gregory, C., Hickman, J. J. & Boland, T. Inkjet printing of viable mammalian cells. Biomaterials 26, 93–99 (2005).
Hollister, S. J. & Bergman, T. L. in Addititve/Subtractive Manufacturing Research and Development in Europe (WTEC, www.wtec.org) (in the press).
Cohen, D. L., Maher, S., Rawlinson, J., Lipson, H. & Bonassar, L. J. Direct freeform fabrication of living cell-seeded alginate hydrogel implants in anatomic shapes. Trans. Orthopaedic Res. Soc. 51, 1781 (2005).
Friedman, J. A. et al. Biodegradable polymer grafts for surgical repair of the injured spinal cord. Neurosurgery 51, 742–751 (2002).
Acknowledgements
The author has been funded by the National Institutes of Health R01 DE 13608 (Bioengineering Research Partnership) and R01 DE 13416. He also acknowledges the contributions from his students, former students and laboratory staff including Alisha Diggs, Colleen Flanagan, Elly Liao, Cheng Yu Lin, Chia-Ying Lin, Sara Mantila, Eiji Saito, Rachel Schek, Juan Taboas, Jessica Williams and Darice Wong. Finally, he would like to thank his collaborators including Paul Krebsbach, Stephen Feinberg, Suman Das, Noboru Kikuchi, Michael Yaszemski and Antonios Mikos for many fruitful and stimulating research interactions.
Author information
Authors and Affiliations
Ethics declarations
Competing interests
The author declares no competing financial interests.
Rights and permissions
About this article
Cite this article
Hollister, S. Porous scaffold design for tissue engineering. Nature Mater 4, 518–524 (2005). https://doi.org/10.1038/nmat1421
Issue Date:
DOI: https://doi.org/10.1038/nmat1421
This article is cited by
-
Adaptable test bench for ASTM-compliant permeability measurement of porous scaffolds for tissue engineering
Scientific Reports (2024)
-
Design and Analysis of Three-Dimensional Foams: A Review
Archives of Computational Methods in Engineering (2024)
-
Three dimensional scaffolds of hybrid PLA/PCL/HA/silica nanocomposites for bone tissue engineering
Polymer Bulletin (2024)
-
Hybrid composite cellulose nanocrystal, hydroxyapatite, and chitosan material with controlled hydrophilic/hydrophobic properties as a remineralizable dental material
Cellulose (2024)
-
Extraction and Characterization of Human Adipose Tissue-Derived Collagen: Toward Xeno-Free Tissue Engineering
Tissue Engineering and Regenerative Medicine (2024)