Abstract
Highly active antiretroviral therapy (HAART) can control HIV-1 replication1,2, but suboptimal treatment allows for the evolution of resistance and rebound viremia3,4,5,6,7,8. A comparative measure of antiviral activity under clinically relevant conditions would guide drug development and the selection of regimens that maximally suppress replication. Here we show that current measures of antiviral activity, including IC50 and inhibitory quotient, neglect a key dimension, the dose-response curve slope. Using infectivity assays with wide dynamic range, we show that this slope has noteworthy effects on antiviral activity. Slope values are class specific for antiviral drugs and define intrinsic limitations on antiviral activity for some classes. Nucleoside reverse transcriptase inhibitors and integrase inhibitors have slopes of ∼1, characteristic of noncooperative reactions, whereas non-nucleoside reverse transcriptase inhibitors, protease inhibitors and fusion inhibitors unexpectedly show slopes >1. Instantaneous inhibitory potential (IIP), the log reduction in single-round infectivity at clinical drug concentrations, is strongly influenced by slope and varies by >8 logs for anti-HIV drugs. IIP provides a more accurate measure of antiviral activity and in general correlates with clinical outcomes. Only agents with slopes >1 achieve high-level inhibition of single-round infectivity, a finding with profound implications for drug and vaccine development.
Similar content being viewed by others
Main
A classic description of dose-response relationships is the median effect model based on mass action9,10 (Equations 1 and 2 and Fig. 1):
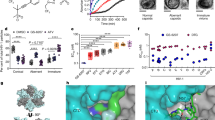
(a) Hypothetical linear-log plot of the fraction of viruses unaffected by a drug (fu) versus drug concentration, on the basis of the median-effect model for drugs with different m values. Concentrations are normalized by IC50. A typical clinical concentration range 10–100-fold above the IC50 is shaded. (b) A log-log plot of the same curves emphasizing the strong impact of slope on the suppression of infectivity. (c) A median effect plot [log (fa / fu) versus log(drug concentration)] (Equation 1) of the same curves. The m value is the slope of the line. (d) Each class of anti–HIV-1 drugs has a characteristic slope. The m value for each drug was calculated by linear-regression analysis using the median effect model. Each point is the average of more than three experiments. See Supplementary Table 1 for the mean values and s.d. PI, protease inhibitors; FI, fusion inhibitors; II, integrase inhibitors; 3TC, lamivudine; ABC, abacavir; AZT, zidovudine; d4T, stavudine; ddI, didanosine, FTC, emtricitabine; TDF, tenofovir disoproxil fumarate; EFV, efavirenz; NVP, nevirapine; DLV, delavirdine; APV, amprenavir; ATV, atazanavir; DRV, darunavir; IDV, indinavir; LPV, lopinavir; NFV, nelfinavir; SQV, saquinavir; TPV, tipranavir; T20, enfuvirtide; RAL, raltegravir. (e) Comparison of the antiviral activity of two hypothetical drugs with different m values. IIP is the number of logs of suppression of single-round infectivity at a clinically relevant drug concentration. At Cmax, the IIP of a drug with m = 3 is 10,000-fold greater than that of a drug with m = 1.

or,

For inhibition of HIV-1 infection, fa and fu (equal to 1 – fa) are the fractions of viruses affected and unaffected by the drug, D is drug concentration, IC50 is the drug concentration that causes 50% of the maximum inhibitory effect and m is a slope parameter mathematically analogous to the Hill coefficient11, a measure of cooperativity in the binding of multiple ligands to linked binding sites. In this model, drug activity is determined by three parameters: IC50, D and m. However, the widely used measures IC50 and inhibitory quotient (IQ, the ratio of plasma drug concentrations to IC50)12,13 both ignore slope. On traditional semi-log plots, dose-response curves with different slopes appear similar, approaching 100% inhibition at high drug concentrations (Fig. 1a). However, clinical outcome may depend on whether 99% or 99.99% inhibition is achieved14. Displaying the same data on a log-log plot reveals that drugs with the same IC50 or IQ values but higher slopes achieve much greater inhibition at clinically relevant concentrations (Fig. 1b). We therefore hypothesized that slope might have a substantial effect on antiviral activity.
To test this hypothesis, we obtained dose-response curves for anti–HIV-1 drugs using a single-round infectivity assay with a sensitivity able to detect infection of individual cells15,16. CXCR4-pseudotyped wild-type viruses carrying GFP in the env gene were used to infect primary CD4+ T lymphoblasts, the principal target cells for HIV-1 in vivo. Infectivity was quantified by flow cytometry, and fu was calculated as the percentage of GFP+ cells in the presence of drug normalized by the percentage of GFP+ cells without drug. Using the median effect model (Equation 1), dose-response curves can be linearized (Fig. 1c) and IC50 and slope can be determined (Supplementary Table 1 online). We chose a single-round assay because it is not complicated by virus growth and evolution over a prolonged culture period, reflects the degree of instantaneous inhibition caused by the drugs and correlates more closely with mechanisms of drug action17.
Analysis of dose-response curves for anti–HIV-1 drugs gave a noteworthy result. Each drug class had a characteristic slope (Fig. 1d and Supplementary Table 1). The slopes of all nucleoside reverse transcriptase inhibitors (NRTIs) were ∼1, characteristic of noncooperative reactions (Fig. 1d). Five structurally diverse integrase inhibitors also showed slopes close to 1 (Fig. 1d). In contrast, the slopes for non-nucleoside reverse transcriptase inhibitors (NNRTIs) and fusion inhibitors were ∼1.7, whereas the slopes for protease inhibitors ranged from 1.8 to 4.5 (Fig. 1d). Thus, antiretroviral drugs acting through different mechanisms show distinct slope values.
To include the influence of slope in a quantitative measure of antiviral activity, we developed a new index termed instantaneous inhibitory potential (IIP), which equals the log reduction in single-round infectivity at clinically relevant concentrations (Fig. 1e). IIP is equivalent to log(1 / fu) and can be calculated from Equations 3–5.



Here Cmin, Cave and Cmax represent steady-state minimum, average (area under the curve during dose interval/dose interval), and maximum plasma drug concentrations for the commonly recommended dose of each drug18. IIP incorporates all three parameters in the median effect model—IC50, D and m—into a single value with an intuitive meaning, the log reduction in infectivity.
Initial studies showed that the IIP of different drugs varied substantially (>8 logs) owing to the influence of slope (Fig. 1e). For NRTIs, IIP values were ≤3.5 and within the dynamic range of the standard assay (Fig. 2a–c). For example, clinical concentrations of zidovudine produce inhibition that is readily measured by collecting ∼50,000 live cell events (Fig. 2a). For NNRTIs and protease inhibitors, the IIP values ranged from 2 to 10. Clinical concentrations of efavirenz produce inhibition that can only be measured with assays having a dynamic range of >5 logs. IIP values beyond the assay's normal dynamic range were determined by extrapolation (Fig. 2d–f). To verify the extrapolated values, we carried out larger scale assays with 2 × 106 live cell events. Our results confirm that drugs like efavirenz at clinically relevant concentrations can decrease single-round infection by >5 logs, as evidenced by the marked absence of GFP+ cells (Fig. 2f).
(a) Log-log dose-response curve for AZT. Each point represents the mean ± s.d. from more than three experiments. The clinical concentration range for AZT is shaded. Because of the short plasma half-life of the AZT prodrug, the range between Cave and Cmax is shown. (b) Linearized dose-response curve for AZT based on median effect model. (c) Flow cytometric data showing detection of cells that were infected in the presence of 10 μM AZT. (d) Log-log dose-response curve for EFV. (e) Linearized dose-response curve for EFV based on median effect model. IIP values at Cmin, Cave or Cmax were calculated with Equations 3–5. This is graphically equivalent to extrapolation of the median effect plot to higher concentrations (dashed line). To verify values obtained by extrapolation, large-scale infections were carried out (open symbol). (f) Verifying the IIP of EFV in large-scale infections (∼2 × 106 events). In cultures with 10 μM EFV, less than three GFP+ cells were detected. This represents >5 logs of inhibition, consistent with the values predicted by extrapolation. FL2 measures red fluorescence.
We next compared three indices of antiviral activity, IC50, IQ and IIP, for different classes of anti–HIV-1 drugs (Fig. 3). There was no general difference in the range of IC50 values for different classes (Fig. 3a). For IQ, the NNRTI efavirenz had the highest value, but the IQ values for the protease inhibitor and NRTI classes overlapped (Fig. 3b). However, when IIP was used for comparison, NNRTIs and most protease inhibitors gave much higher values than NRTIs (Fig. 3c). This finding partially explains why the most effective initial HAART regimens include an NNRTI or protease inhibitor14. Particularly noteworthy was the finding that efavirenz and a subset of protease inhibitors produced >5 logs of inhibition at Cave, which is substantially greater than the inhibition produced by NRTIs, fusion inhibitors or integrase inhibitors. Most impressively, the protease inhibitors darunavir, indinavir and saquinavir produced >9 logs of inhibition at Cmax, largely as a result of high m values (Fig. 3c,d). These drugs had slopes >3.5 (Fig. 1d). The steepness of the dose-response curve, as captured in the m value, is a major factor leading to high IIP, as illustrated in contour plots of IIP as a function of m and IQ (Fig. 3d). Thus, the slope parameter is a crucial missing dimension in the analysis of antiviral activity.
(a) IC50 determined in the single-round infectivity assay. IC50 was determined by least-squares regression analysis of median effect plots. (b) IQ values (concentration/IC50) at Cmin, Cave and Cmax. (c) IIP values at Cmin, Cave and Cmax. IIP values were determined with Equations 3–5 from measured IC50 and m values as described in Figure 2. See Supplementary Table 1 for details. (d) Contour plots of m versus IQ. Colored lines are theoretical IIP values representing 1–6 logs of inhibition of a single round of infection based on the median effect model. All the data points are the average of more than three experiments. Mean values and s.d. are shown in Supplementary Table 1. NRTI data points with IQ values below the scale range were placed at the left edge of the x axis in d.
Although a high slope endows a drug with a high IIP, it also indicates extreme sensitivity to the changes in plasma drug concentration. For drugs with a high slope and a short half-life (t1/2), such as indinavir and saquinavir, IIP drops quickly during the dosing interval and with missed doses (Fig. 4a and Supplementary Notes online). In contrast, for drugs with a long t1/2, such as efavirenz and darunavir, IIP is maintained at a high level even if doses are missed. This result, together with issues of bioavailability, toxicity and convenience, may explain why indinavir and saquinavir are used less commonly despite their high IIP values. The two drugs that maintain IIP values above 5 logs at 24 h after the last dose (IIP24), efavirenz and darunavir (Fig. 4a), consistently excel in clinical trials14,19,20,21,22.
(a) Predicted decay of IIP if subsequent doses are missed. IIP is plotted as a function of time after Cmax from the last dose. We calculated IIP using measured m and IC50 values (Supplementary Table 1) and published t1/2 values. For NRTIs, we used t1/2 values for the active intracellular triphosphate forms18. Drug levels are assumed to decay exponentially. (b) Relationship between IIP24 values and recommended 'Column A' drugs. The IIP24 values for the preferred Column A drugs (dark shading) tend to be higher than those of the alternate Column A drugs (light shading) or non–Column A drugs. Data for unboosted protease inhibitors are indicated by symbols with a black border. (c) Relationship between IIP24 values and virologic outcomes in major clinical trials (Supplementary Notes) cited in the treatment guidelines14,19, with trial titles given beside each arrow. Solid arrows point toward drugs with superior virologic activity in head-to-head comparisons with the same background regimens. Broken arrows indicate a trend toward superiority not reaching statistical significance. Double-headed arrows indicate equivalent virologic outcomes.
Because antiviral activity is likely to be a major determinant of clinical outcome, we compared IIP values with clinical trial results (Fig. 4b,c). We used IIP24 as a measure of sustained antiviral activity and the HIV-1 treatment guidelines as a source of clinical outcomes14,19. The guidelines recommend that initial HAART regimens consist of one drug from a select group of NNRTIs and protease inhibitors, the so-called 'column A' drugs, plus two NRTIs. Our analysis showed that the preferred column A drugs tended to have high sustained IIP (Fig. 4b). In addition, drugs with high sustained IIP tended to show superiority over drugs with lower IIP in high-quality randomized clinical trials (Fig. 4c and Supplementary Notes). Furthermore, our results indicate that darunavir is superior to all available antiretroviral drugs on the basis of IIP, suggesting that darunavir-based initial HAART regimens may be uniquely effective. Preliminary results from the Artemis trial in treatment-naive subjects confirm this prediction22.
Our results demonstrate that IIP provides a more accurate in vitro pharmacodynamic measure of antiviral activity than the traditional measures because it takes into account the slope parameter. Nevertheless, IIP is only one factor in clinical outcome. It cannot be directly related to the initial decay rate of viremia, which depends on where in the viral life cycle the drugs act23, or the magnitude and durability of viral load suppression, which are influenced by multiple factors including pharmacokinetics, distribution, toxicity, adherence, drug interactions and barriers to resistance (Supplementary Notes). Although no in vitro assay can predict clinical outcomes, our results suggest that IIP may identify drugs with high antiviral activity in vivo.
Our data show that slope is characteristic of drug class. A mechanistic explanation can be found by reconsidering the concept of cooperativity in drug action. Although m >1 classically represents positive cooperativity between ligand binding sites on a multivalent receptor11, multiple equilibria models based on mass action24 and statistical models incorporating heterogeneity25 can be applied to antiviral drugs and predict steep dose-response curves without the need to postulate interactions between binding sites (L.S. and R.F.S., unpublished data). For all forms of cooperativity leading to steep dose-response curves, the crucial requirement is participation of multiple copies of a drug target in the relevant step in the life cycle. Drugs like NRTIs and integrase inhibitors with m = 1 (no cooperativity) target reactions in which a single molecular complex of enzyme with viral nucleic acid mediates a key step—nucleotide addition leading to chain termination or strand transfer26,27,28. Other reverse transcriptase or integrase molecules present are irrelevant. In contrast, NNRTIs and protease inhibitors target the enzymes themselves. Multiple copies of reverse transcriptase and protease participate in the processes of reverse transcription and virion maturation, respectively, allowing for a form of intermolecular cooperativity within the preintegration complex or the maturing virion. The lack of this form of cooperativity for NRTIs and integrase inhibitors results in m values of 1, thus imposing intrinsic limitations on IIP.
Although there may be different mechanistic explanations for high slope values, our demonstration that the slope is a crucial determinant of drug activity is a general result that is an inevitable consequence of the dose-response relationship. This result may apply to all viral infections, as evidenced by the role of slope in the effectiveness of interferon-α treatment of hepatitis C virus infection29. Notably, these principles apply not only to antiviral drugs, but also to vaccine-induced effector mechanisms, including neutralizing antibodies, and any other drugs that target exponential processes, such as the growth of microorganisms or cancer cells.
Methods
Drug preparation.
We obtained raltegravir, L870812, L240, L525, GS9137, TMC125 and TMC278 from Merck. We obtained all other anti–HIV-1 drugs through the AIDS Research and Reference Reagent Program, Division of AIDS, National Institute of Allergy and Infections Diseases, US National Institutes of Health. Zidovudine, lamivudine, abacavir, didanosine, efavirenz, nevirapine, atazanavir, lopinavir, nelfinavir, tipranavir, darunavir, saquinavir, amprenavir, T1249, L240, L525, GS9137, TMC125 and TMC278 were dissolved in DMSO at 50 mM, aliquoted and stored at −20 °C. Raltegravir and L870812 were dissolved in DMSO at 6 mM, aliquoted and stored at −20 °C. Tenofovir, emtricitabine, stavudine and indinavir were dissolved in ddH2O at 50 mM, aliquoted and stored at −20 °C. Enfuvirtide (Roche) was dissolved in 0.1 M NaHCO3 at 1 mM, aliquoted and stored at −80 °C. We serially diluted drugs in their corresponding solvents and kept their final solvent concentration in cell culture constant at 0.5%.
Virus stocks.
We generated pseudotyped virus capable of single-round infection as described previously15. Briefly, we transfected HEK293T cells with a GFP-tagged, envelope-defective HIV-1 vector (pNL43-ΔE-EGFP) along with an HIV-1 CXCR4 envelope expression vector using Lipofectamine 2000 (Invitrogen) according to the manufacture's protocol. For experiments testing protease inhibitors, we replaced medium with RPMI1640 (Invitrogen) supplemented with 50% human serum (Gemini) and 10% FBS (Gemini) 6–7 h after transfection and then added drugs at this step. We chose to use 50% human serum to account for the protein binding of the drugs without compromising cell viability. At 48 h after transfection, we spun virus-containing supernatants at 335g for 10 min, filtered them through a 0.22-μm membrane to remove cell debris and used them for infection or stored them at −80 °C. For experiments testing other drugs, we replaced medium by RPMI1640 supplemented with 10% FBS only. At 48 h after transfection, we cleared cell debris as described above and harvested virus particles by ultracentrifugation at 100,000g at 4 °C for 2 h, aliquoted them and stored them at −80 °C. We standardized the amount of virus used for each experiment by p24 using an ELISA (Perkin-Elmer).
Single-round infectivity assay.
We used a modified single-round infectivity assay to evaluate anti–HIV-1 drug activity15,16. Briefly, we obtained peripheral blood mononuclear cells from healthy blood donors by Hypaque-Ficoll gradient centrifugation and activated the cells with phytohemagglutinin (0.5 μg/ml) and interleukin-2 (100 U/ml) for 3 d. We selected CD4+ T cells by magnetic beads (Miltenyi) and seeded them in a 96-well plate at 1 × 105 cells per well in RPMI1640 supplemented with 50% human serum, 10% FBS, interleukin-2 (100 U/ml) and cytokine-rich supernatant. We added drugs other than protease inhibitors at this step and maintained them throughout the culture. We added standardized amounts of virus 16–18 h after the addition of drugs. This period was shown to be sufficient to allow optimal intracellular phosphorylation of NRTIs15. We carried out infection by 'spinoculation' at 1,200g, 30 °C for 2 h. We incubated infected cells at 37 °C for 3 d. We then washed cells and fixed them with 2% formaldehyde. We quantified infectivity as the percentage of GFP+ cells by FACS analysis (BD Bioscience). We did all of the experiments in triplicate with cells from at least three different donors. All healthy blood donors gave their informed consent, and the study was approved by the Institutional Review Board of Johns Hopkins University.
Analysis of dose-response curves.
We obtained dose-response curves by normalizing the percentage of GFP+ cells without drug treatment to 100%. We obtained the IC50 and the slope (m value) from each dose-response curve by fitting data to the median effect model (Equation 1) through least-square regression analysis. We calculated IIP with Equations 3–5. We checked the consistency of slope and considered it constant with r2 > 0.96. For some protease inhibitors such as lopinavir, the slopes of dose-response curves increase at higher concentration (Supplementary Fig. 1 online). In this case, we used the lowest slope for estimation of IIP. For raltegravir and L240, a low-level GFP expression from a small number of cells with unintegrated virus was apparent at high concentrations of the drug. To correct for this effect, we fitted the data to the following equation to obtain mact and x:

where is the observed fu, , IC50act, mact are the actual fu, IC50, m values, and x is the percentage of GFP expression from unintegrated virus. We assumed that IC50act is approximately equal to IC50 obs calculated from , as x is very small. The resulting estimate for x was less than 1.5% in all experiments, and the m values reported for raltegravir and L240 were the adjusted m values (mact; Supplementary Fig. 2 online).
Statistical analyses.
We performed least-square regression analysis and calculated mean values and standard deviation for IC50 and slope with Microsoft Office Excel 2003 software.
Note: Supplementary information is available on the Nature Medicine website.
References
Gulick, R.M. et al. Treatment with indinavir, zidovudine and lamivudine in adults with human immunodeficiency virus infection and prior antiretroviral therapy. N. Engl. J. Med. 337, 734–739 (1997).
Hammer, S.M. et al. A controlled trial of two nucleoside analogues plus indinavir in persons with human immunodeficiency virus infection and CD4 cell counts of 200 per cubic millimeter or less. AIDS Clinical Trials Group 320 Study Team. N. Engl. J. Med. 337, 725–733 (1997).
Ho, D.D. et al. Rapid turnover of plasma virions and CD4 lymphocytes in HIV-1 infection. Nature 373, 123–126 (1995).
Wei, X. et al. Viral dynamics in human immunodeficiency virus type 1 infection. Nature 373, 117–122 (1995).
Preston, B.D., Poiesz, B.J. & Loeb, L.A. Fidelity of HIV-1 reverse transcriptase. Science 242, 1168–1171 (1988).
Roberts, J.D., Bebenek, K. & Kunkel, T.A. The accuracy of reverse transcriptase from HIV-1. Science 242, 1171–1173 (1988).
Larder, B.A., Darby, G. & Richman, D.D. HIV with reduced sensitivity to zidovudine (AZT) isolated during prolonged therapy. Science 243, 1731–1734 (1989).
Coffin, J.M. HIV population dynamics in vivo: implications for genetic variation, pathogenesis, and therapy. Science 267, 483–489 (1995).
Chou, T.C. Derivation and properties of Michaelis-Menten type and Hill type equations for reference ligands. J. Theor. Biol. 59, 253–276 (1976).
Chou, T.C. & Talalay, P. Quantitative analysis of dose-effect relationships: the combined effects of multiple drugs or enzyme inhibitors. Adv. Enzyme Regul. 22, 27–55 (1984).
Hill, A.V. The possible effects of the aggregation of the molecules of haemoglobin on its dissociation curves. J. Physiol. (Lond.) 40, iv–vii (1910).
Hoefnagel, J.G., Koopmans, P.P., Burger, D.M., Schuurman, R. & Galama, J.M. Role of the inhibitory quotient in HIV therapy. Antivir. Ther. 10, 879–892 (2005).
Morse, G.D., Catanzaro, L.M. & Acosta, E.P. Clinical pharmacodynamics of HIV-1 protease inhibitors: use of inhibitory quotients to optimise pharmacotherapy. Lancet Infect. Dis. 6, 215–225 (2006).
Panel on Antiretroviral Guidelines for Adult and Adolescents. Guidelines for the use of antiretroviral agents in HIV-1-infected adults and adolescents. AIDSinfo http://aidsinfo.nih.gov/contentfiles/AdultandAdolescentGL.pdf (2008).
Zhang, H. et al. Novel single-cell–level phenotypic assay for residual drug susceptibility and reduced replication capacity of drug-resistant human immunodeficiency virus type 1. J. Virol. 78, 1718–1729 (2004).
McMahon, M.A. et al. The HBV drug entecavir—effects on HIV-1 replication and resistance. N. Engl. J. Med. 356, 2614–2621 (2007).
Ferguson, N.M., Fraser, C. & Anderson, R.M. Viral dynamics and anti-viral pharmacodynamics: rethinking in vitro measures of drug potency. Trends Pharmacol. Sci. 22, 97–100 (2001).
Acosta, E.P., Gerber, J.G. & Kuritzkes, D.R. in Antiretroviral Pharmacokinetics, Resistance Testing and Therapeutic Drug Monitoring (eds. Libman, H. & Makadon, H.J.) 115–136 (American College of Physicians Therapy Series: HIV, Philadelphia, 2007).
Bartlett, J.G. & Gallant, J.E. in 2007 Medical Management of HIV Infection 510 (Johns Hopkins Medicine Health Publishing Business Group, Baltimore, MD, 2007).
Madruga, J.V. et al. Efficacy and safety of darunavir-ritonavir compared with that of lopinavir-ritonavir at 48 weeks in treatment-experienced, HIV-infected patients in TITAN: a randomised controlled phase 3 trial. Lancet 370, 49–58 (2007).
Clotet, B. et al. Efficacy and safety of darunavir-ritonavir at week 48 in treatment-experienced patients with HIV-1 infection in POWER 1 and 2: a pooled subgroup analysis of data from two randomised trials. Lancet 369, 1169–1178 (2007).
Ortiz, R. et al. Efficacy and safety of once-daily darunavir-ritonavir versus lopinavir-ritonavir in treatment-naive HIV-1–infected patients at week 48. AIDS (in the press).
Sedaghat, A.R., Dinoso, J.B., Shen, L., Wilke, C.O. & Siliciano, R.F. Decay dynamics of HIV-1 depend on the inhibited stages of the viral life cycle. Proc. Natl. Acad. Sci. USA 105, 4832–4837 (2008).
Weiss, J.N. The Hill equation revisited: uses and misuses. FASEB J. 11, 835–841 (1997).
Hoffman, A. & Goldberg, A. The relationship between receptor-effector unit heterogeneity and the shape of the concentration-effect profile: pharmacodynamic implications. J. Pharmacokinet. Biopharm. 22, 449–468 (1994).
Ambrose, Z., Julias, J.G., Boyer, P.L., Kewalramani, V.N. & Hughes, S.H. The level of reverse transcriptase (RT) in human immunodeficiency virus type 1 particles affects susceptibility to nonnucleoside RT inhibitors but not to lamivudine. J. Virol. 80, 2578–2581 (2006).
Pommier, Y., Johnson, A.A. & Marchand, C. Integrase inhibitors to treat HIV/AIDS. Nat. Rev. Drug Discov. 4, 236–248 (2005).
Pandey, K.K. et al. Inhibition of human immunodeficiency virus type 1 concerted integration by strand transfer inhibitors which recognize a transient structural intermediate. J. Virol. 81, 12189–12199 (2007).
Talal, A.H. et al. Pharmacodynamics of PEG-IFN-α differentiate HIV/HCV coinfected sustained virological responders from nonresponders. Hepatology 43, 943–953 (2006).
Acknowledgements
We thank healthy blood donors for their participation. We thank the AIDS Research and Reference Reagent Program of the US National Institutes of Health and Merck for providing anti–HIV-1 drugs. We thank C. Flexner, A. Mildvan, J. Gallant, G. Lucas, J. Cofrancesco, J. Bartlett, D. Hazuda and R. Moore for helpful discussions and critical review of the manuscript. This work was supported by the US National Institutes of Health grants AI43222 and AI51178, by the Doris Duke Charitable Foundation and by the Howard Hughes Medical Institute.
Author information
Authors and Affiliations
Contributions
L.S. and R.F.S. designed the experiments. L.S. conducted the experiments. S.P., M.A.M., M.C., H.Z., Y.Z. and E.P. contributed to the development of the single-round infectivity assay. L.S., A.R.S. and R.F.S. conducted the data analysis. E.P.A. provided pharmacokinetic data used in the analysis. K.S.A. provided reagents used in the experiments. All of the authors contributed to the manuscript preparation. R.F.S. supervised the project.
Corresponding author
Supplementary information
Supplementary Text and Figures
Supplementary Figs.1 and 2, Supplementary Table 1 and Supplementary Notes (PDF 199 kb)
Rights and permissions
About this article
Cite this article
Shen, L., Peterson, S., Sedaghat, A. et al. Dose-response curve slope sets class-specific limits on inhibitory potential of anti-HIV drugs. Nat Med 14, 762–766 (2008). https://doi.org/10.1038/nm1777
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nm1777
This article is cited by
-
Coupling the Within-Host Process and Between-Host Transmission of COVID-19 Suggests Vaccination and School Closures are Critical
Bulletin of Mathematical Biology (2023)
-
Modeling Antiretrovial Treatment to Mitigate HIV in the Brain: Impact of the Blood-Brain Barrier
Bulletin of Mathematical Biology (2023)
-
Required concentration index quantifies effective drug combinations against hepatitis C virus infection
Theoretical Biology and Medical Modelling (2021)
-
Escape of SARS-CoV-2 501Y.V2 from neutralization by convalescent plasma
Nature (2021)
-
Resonance of Periodic Combination Antiviral Therapy and Intracellular Delays in Virus Model
Bulletin of Mathematical Biology (2020)