Abstract
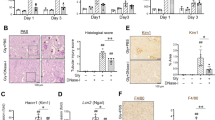
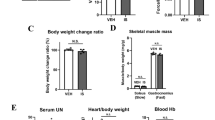
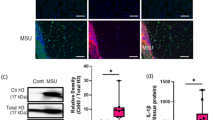
Rhabdomyolysis is a serious syndrome caused by skeletal muscle injury and the subsequent release of breakdown products from damaged muscle cells into systemic circulation1. The muscle damage most often results from strenuous exercise, muscle hypoxia, medications, or drug abuse and can lead to life-threatening complications, such as acute kidney injury (AKI)1. Rhabdomyolysis and the AKI complication can also occur during crush syndrome, an emergency condition that commonly occurs in victims of natural disasters, such as earthquakes, and man-made disasters, such as wars and terrorism2. Myoglobin released from damaged muscle is believed to trigger renal dysfunction in this form of AKI. Recently, macrophages were implicated in the disease pathogenesis of rhabdomyolysis-induced AKI3,4, but the precise molecular mechanism remains unclear. In the present study, we show that macrophages released extracellular traps (ETs) comprising DNA fibers and granule proteins in a mouse model of rhabdomyolysis. Heme-activated platelets released from necrotic muscle cells during rhabdomyolysis enhanced the production of macrophage extracellular traps (METs) through increasing intracellular reactive oxygen species generation and histone citrullination. Here we report, for the first time to our knowledge, this unanticipated role for METs and platelets as a sensor of myoglobin-derived heme in rhabdomyolysis-induced AKI. This previously unknown mechanism might be targeted for treatment of the disease. Finally, we found a new therapeutic tool for prevention of AKI after rhabdomyolysis, which might rescue some sufferers of this pathology.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Bosch, X., Poch, E. & Grau, J.M. Rhabdomyolysis and acute kidney injury. N. Engl. J. Med. 361, 62–72 (2009).
Sever, M.S., Vanholder, R. & Lameire, N. Management of crush-related injuries after disasters. N. Engl. J. Med. 354, 1052–1063 (2006).
Belliere, J. et al. Specific macrophage subtypes influence the progression of rhabdomyolysis-induced kidney injury. J. Am. Soc. Nephrol. 26, 1363–1377 (2015).
Sinniah, R. & Lye, W. Acute renal failure from myoglobinuria secondary to myositis from severe falciparum malaria. Am. J. Nephrol. 20, 339–343 (2000).
de Meijer, A.R., Fikkers, B.G., de Keijzer, M.H., van Engelen, B.G. & Drenth, J.P. Serum creatine kinase as predictor of clinical course in rhabdomyolysis: a 5-year intensive care survey. Intensive Care Med. 29, 1121–1125 (2003).
Boutaud, O. et al. Acetaminophen inhibits hemoprotein-catalyzed lipid peroxidation and attenuates rhabdomyolysis-induced renal failure. Proc. Natl. Acad. Sci. USA 107, 2699–2704 (2010).
Zager, R.A. Combined mannitol and deferoxamine therapy for myohemoglobinuric renal injury and oxidant tubular stress. Mechanistic and therapeutic implications. J. Clin. Invest. 90, 711–719 (1992).
Brinkmann, V. et al. Neutrophil extracellular traps kill bacteria. Science 303, 1532–1535 (2004).
Chow, O.A. et al. Statins enhance formation of phagocyte extracellular traps. Cell Host Microbe 8, 445–454 (2010).
Wang, Y. et al. Histone hypercitrullination mediates chromatin decondensation and neutrophil extracellular trap formation. J. Cell Biol. 184, 205–213 (2009).
Kessenbrock, K. et al. Netting neutrophils in autoimmune small-vessel vasculitis. Nat. Med. 15, 623–625 (2009).
Clark, S.R. et al. Platelet TLR4 activates neutrophil extracellular traps to ensnare bacteria in septic blood. Nat. Med. 13, 463–469 (2007).
von Brühl, M.L. et al. Monocytes, neutrophils, and platelets cooperate to initiate and propagate venous thrombosis in mice in vivo. J. Exp. Med. 209, 819–835 (2012).
Wong, S.L. et al. Diabetes primes neutrophils to undergo NETosis, which impairs wound healing. Nat. Med. 21, 815–819 (2015).
Xu, J. et al. Extracellular histones are major mediators of death in sepsis. Nat. Med. 15, 1318–1321 (2009).
Arnaout, M.A. Structure and function of the leukocyte adhesion molecules CD11/CD18. Blood 75, 1037–1050 (1990).
Behnen, M. et al. Immobilized immune complexes induce neutrophil extracellular trap release by human neutrophil granulocytes via FcγRIIIB and Mac-1. J. Immunol. 193, 1954–1965 (2014).
Rossaint, J. et al. Synchronized integrin engagement and chemokine activation is crucial in neutrophil extracellular trap–mediated sterile inflammation. Blood 123, 2573–2584 (2014).
Praticó, D. et al. Iron-dependent human platelet activation and hydroxyl radical formation: involvement of protein kinase C. Circulation 99, 3118–3124 (1999).
Chen, G. et al. Heme-induced neutrophil extracellular traps contribute to the pathogenesis of sickle cell disease. Blood 123, 3818–3827 (2014).
Hirahashi, J. et al. Mac-1 (CD11b/CD18) links inflammation and thrombosis after glomerular injury. Circulation 120, 1255–1265 (2009).
Sakatsume, M. et al. Rapid and sensitive electrophoresis of urinary protein clearly reveals the pathophysiological feature of renal diseases. Nephrology (Carlton) 12, 191–196 (2007).
Lande, R. et al. Neutrophils activate plasmacytoid dendritic cells by releasing self-DNA-peptide complexes in systemic lupus erythematosus. Sci. Transl. Med. 3, 73ra19 (2011).
Kim, J.H. et al. Macrophage depletion ameliorates glycerol-induced acute kidney injury in mice. Nephron. Exp. Nephrol. 128, 21–29 (2014).
Daley, J.M., Thomay, A.A., Connolly, M.D., Reichner, J.S. & Albina, J.E. Use of Ly6G-specific monoclonal antibody to deplete neutrophils in mice. J. Leukoc. Biol. 83, 64–70 (2008).
Bergmeier, W., Rackebrandt, K., Schröder, W., Zirngibl, H. & Nieswandt, B. Structural and functional characterization of the mouse von Willebrand factor receptor GPIb-IX with novel monoclonal antibodies. Blood 95, 886–893 (2000).
Rubio-Navarro, A. et al. CD163-macrophages are involved in rhabdomyolysis-induced kidney injury and may be detected by MRI with targeted gold-coated iron oxide nanoparticles. Theranostics 6, 896–914 (2016).
Mantovani, A. et al. The chemokine system in diverse forms of macrophage activation and polarization. Trends Immunol. 25, 677–686 (2004).
Lee, S. et al. Distinct macrophage phenotypes contribute to kidney injury and repair. J. Am. Soc. Nephrol. 22, 317–326 (2011).
Belcher, J.D. et al. Heme triggers TLR4 signaling leading to endothelial cell activation and vaso-occlusion in murine sickle cell disease. Blood 123, 377–390 (2014).
Thomas, G., Tacke, R., Hedrick, C.C. & Hanna, R.N. Nonclassical patrolling monocyte function in the vasculature. Arterioscler. Thromb. Vasc. Biol. 35, 1306–1316 (2015).
Finsterbusch, M. et al. Patrolling monocytes promote intravascular neutrophil activation and glomerular injury in the acutely inflamed glomerulus. Proc. Natl. Acad. Sci. USA 113, E5172–E5181 (2016).
Simon, D.I. et al. Platelet glycoprotein Ibα is a counterreceptor for the leukocyte integrin Mac-1 (CD11b/CD18). J. Exp. Med. 192, 193–204 (2000).
Kuijper, P.H. et al. Platelet associated fibrinogen and ICAM-2 induce firm adhesion of neutrophils under flow conditions. Thromb. Haemost. 80, 443–448 (1998).
Rosetti, F. & Mayadas, T.N. The many faces of Mac-1 in autoimmune disease. Immunol. Rev. 269, 175–193 (2016).
An, G. et al. P-selectin glycoprotein ligand-1 is highly expressed on Ly-6Chi monocytes and a major determinant for Ly-6Chi monocyte recruitment to sites of atherosclerosis in mice. Circulation 117, 3227–3237 (2008).
Jin, R. et al. Soluble CD40 ligand stimulates CD40-dependent activation of the β2 integrin Mac-1 and protein kinase C zeda (PKCζ) in neutrophils: implications for neutrophil–platelet interactions and neutrophil oxidative burst. PLoS One 8, e64631 (2013).
Hirahashi, J. et al. Mac-1 signaling via Src-family and Syk kinases results in elastase-dependent thrombohemorrhagic vasculopathy. Immunity 25, 271–283 (2006).
Okubo, K. et al. Lactoferrin suppresses neutrophil extracellular traps release in inflammation. EBioMedicine 10, 204–215 (2016).
Panizo, N., Rubio-Navarro, A., Amaro-Villalobos, J.M., Egido, J. & Moreno, J.A. Molecular mechanisms and novel therapeutic approaches to rhabdomyolysis-induced acute kidney injury. Kidney Blood Press. Res. 40, 520–532 (2015).
Coxon, A. et al. A novel role for the β2 integrin CD11b/CD18 in neutrophil apoptosis: a homeostatic mechanism in inflammation. Immunity 5, 653–666 (1996).
Tanikawa, C. et al. Regulation of histone modification and chromatin structure by the p53–PADI4 pathway. Nat. Commun. 3, 676 (2012).
Zanardo, R.C. et al. A down-regulatable -selecti E-selectin ligand is functionally important for PSGL-1-independent leukocyte–endothelial cell interactions. Blood 104, 3766–3773 (2004).
Golas, J.M. et al. SKI-606, a 4-anilino-3-quinolinecarbonitrile dual inhibitor of Src and Abl kinases, is a potent antiproliferative agent against chronic myelogenous leukemia cells in culture and causes regression of K562 xenografts in nude mice. Cancer Res. 63, 375–381 (2003).
Suljagic, M. et al. The Syk inhibitor fostamatinib disodium (R788) inhibits tumor growth in the Eμ– TCL1 transgenic mouse model of CLL by blocking antigen-dependent B-cell receptor signaling. Blood 116, 4894–4905 (2010).
Miller, R.E. et al. CCR2 chemokine receptor signaling mediates pain in experimental osteoarthritis. Proc. Natl. Acad. Sci. USA 109, 20602–20607 (2012).
Warnatsch, A., Ioannou, M., Wang, Q. & Papayannopoulos, V. Neutrophil extracellular traps license macrophages for cytokine production in atherosclerosis. Science 349, 316–320 (2015).
Acknowledgements
We thank the Collaborative Research Resources, School of Medicine, Keio University for technical assistance. We gratefully thank T. Shimosawa (University of Tokyo) for animal care assistance. This work was supported in part by a grant-in-aid from Ministry of Education, Culture, Sports, Science and Technology of Japan (15K09459 (J.H.) and 16K19497 (K.O.)). T.N.M. was supported by National Heart, Lung and Blood Institute (NLHBI), National Institutes of Health (HL065095). J.H. was also supported by grants from Research on Rare and Intractable Diseases, Ministry of Health, Labour and Welfare, Japan (nannti-ippann-004) and the study group for strategic exploration of drug seeds for antineutrophil cytoplasmic autoantibodies (ANCA)-associated vasculitis and construction of clinical evidence from Japan Agency for Medical Research and development, AMED under grant number JP17ek0109104.
Author information
Authors and Affiliations
Contributions
K.O. performed the majority of the experiments, analyzed the data, and wrote the manuscript. T.N.M. provided the Mac-1−/− mice and critical discussion of this work and revised the manuscript editorially. M. Kamiya and Y.U. contributed to the imaging of METs and the preparation of new reagents. M. Kurosawa contributed to mouse care and FACS analysis. A.S., K.Y., and K. Hase provided the Padi4−/− mice. K. Homma and J.S. contributed to clinical study of the subjects with rhabdomyolysis. H.M. conducted a part of the mouse experiments using some inhibitors. T.H. contributed the experiments using Lf. M.H. contributed to clinical concepts behind this study and laboratory management. J.H. designed the research, wrote the manuscript, and supervised the study. All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors applied for a new patent entitled “An inhibitor of leukocyte extracellular traps.” The application number is 14/783,295, and the patent was submitted to Meunier Carlin Curfman LLC.
Supplementary information
Supplementary Figures & Table
Supplementary Figures 1–15 & Supplementary Table (PDF 4633 kb)
Rights and permissions
About this article
Cite this article
Okubo, K., Kurosawa, M., Kamiya, M. et al. Macrophage extracellular trap formation promoted by platelet activation is a key mediator of rhabdomyolysis-induced acute kidney injury. Nat Med 24, 232–238 (2018). https://doi.org/10.1038/nm.4462
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nm.4462
This article is cited by
-
Phosphopeptides P140 cause oxidative burst responses of pulmonary macrophages in an imiquimod-induced lupus model
Molecular Biomedicine (2023)
-
Crosstalk between ferroptosis and macrophages: potential value for targeted treatment in diseases
Molecular and Cellular Biochemistry (2023)
-
Impact of endogenous and exogenous nitrogen species on macrophage extracellular trap (MET) formation by bone marrow–derived macrophages
Cell and Tissue Research (2023)
-
Inflammation, coagulation, and cellular injury in heat-induced shock
Inflammation Research (2023)
-
Bystander effect of SARS-CoV-2 spike protein on human monocytic THP-1 cell activation and initiation of prothrombogenic stimulus representing severe COVID-19
Journal of Inflammation (2022)