Abstract
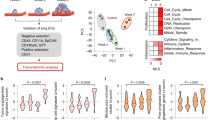
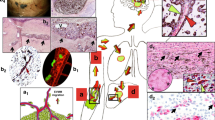
A deeper understanding of the metastatic process is required for the development of new therapies that improve patient survival. Metastatic tumor cell growth and survival in distant organs is facilitated by the formation of a pre-metastatic niche that is composed of hematopoietic cells, stromal cells and extracellular matrix (ECM). Perivascular cells, including vascular smooth muscle cells (vSMCs) and pericytes, are involved in new vessel formation and in promoting stem cell maintenance and proliferation. Given the well-described plasticity of perivascular cells, we hypothesized that perivascular cells similarly regulate tumor cell fate at metastatic sites. We used perivascular-cell-specific and pericyte-specific lineage-tracing models to trace the fate of perivascular cells in the pre-metastatic and metastatic microenvironments. We show that perivascular cells lose the expression of traditional vSMC and pericyte markers in response to tumor-secreted factors and exhibit increased proliferation, migration and ECM synthesis. Increased expression of the pluripotency gene Klf4 in these phenotypically switched perivascular cells promoted a less differentiated state, characterized by enhanced ECM production, that established a pro-metastatic fibronectin-rich environment. Genetic inactivation of Klf4 in perivascular cells decreased formation of a pre-metastatic niche and metastasis. Our data revealed a previously unidentified role for perivascular cells in pre-metastatic niche formation and uncovered novel strategies for limiting metastasis.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
Accession codes
References
Kaplan, R.N. et al. VEGFR1-positive hematopoietic bone marrow progenitors initiate the pre-metastatic niche. Nature 438, 820–827 (2005).
Giles, A.J. et al. Activation of hematopoietic stem–progenitor cells promotes immunosuppression within the pre-metastatic niche. Cancer Res. 76, 1335–1347 (2016).
Smith, H.A. & Kang, Y. The metastasis-promoting roles of tumor-associated immune cells. J. Mol. Med. (Berl.) 91, 411–429 (2013).
Sceneay, J., Parker, B.S., Smyth, M.J. & Möller, A. Hypoxia-driven immunosuppression contributes to the pre-metastatic niche. OncoImmunology 2, e22355 (2013).
McAllister, S.S. & Weinberg, R.A. The tumor-induced systemic environment as a critical regulator of cancer progression and metastasis. Nat. Cell Biol. 16, 717–727 (2014).
Ehling, M. & Mazzone, M. Vessel normalization in the spot-LIGHT of cancer treatment. Trends Mol. Med. 22, 85–87 (2016).
Gomez, D. & Owens, G.K. Smooth muscle cell phenotypic switching in atherosclerosis. Cardiovasc. Res. 95, 156–164 (2012).
Alexander, M.R. & Owens, G.K. Epigenetic control of smooth muscle cell differentiation and phenotypic switching in vascular development and disease. Annu. Rev. Physiol. 74, 13–40 (2012).
Armulik, A., Abramsson, A. & Betsholtz, C. Endothelial–pericyte interactions. Circ. Res. 97, 512–523 (2005).
Khan, J.A. et al. Fetal liver hematopoietic stem cell niches associate with portal vessels. Science 351, 176–180 (2016).
Kunisaki, Y. et al. Arteriolar niches maintain hematopoietic stem cell quiescence. Nature 502, 637–643 (2013).
Goel, S., Wong, A.H.-K. & Jain, R.K. Vascular normalization as a therapeutic strategy for malignant and nonmalignant disease. Cold Spring Harb. Perspect. Med. 2, a006486 (2012).
Hamzah, J. et al. Vascular normalization in Rgs5-deficient tumors promotes immune destruction. Nature 453, 410–414 (2008).
Bennett, M.R., Sinha, S. & Owens, G.K. Vascular smooth muscle cells in atherosclerosis. Circ. Res. 118, 692–702 (2016).
Armulik, A., Genové, G. & Betsholtz, C. Pericytes: developmental, physiological and pathological perspectives, problems and promises. Dev. Cell 21, 193–215 (2011).
Salmon, M. et al. KLF4 regulates abdominal aortic aneurysm morphology, and deletion attenuates aneurysm formation. Circulation 128 (Suppl. 1), S163–S174 (2013).
Shankman, L.S. et al. KLF4-dependent phenotypic modulation of smooth muscle cells has a key role in atherosclerotic plaque pathogenesis. Nat. Med. 21, 628–637 (2015).
Cherepanova, O.A. et al. Activation of the pluripotency factor OCT4 in smooth muscle cells is atheroprotective. Nat. Med. 22, 657–665 (2016).
Gomez, D., Shankman, L.S., Nguyen, A.T. & Owens, G.K. Detection of histone modifications at specific gene loci in single cells in histological sections. Nat. Methods 10, 171–177 (2013).
Kim, K.H. & Sederstrom, J.M. Assaying cell cycle status using flow cytometry. Curr. Protoc. Mol. Biol. 111, 28.6.1–28.6.11 (2015).
Rock, J.R. et al. Multiple stromal populations contribute to pulmonary fibrosis without evidence for epithelial to mesenchymal transition. Proc. Natl. Acad. Sci. USA 108, E1475–E1483 (2011).
Salmon, M., Gomez, D., Greene, E., Shankman, L. & Owens, G.K. Cooperative binding of KLF4, pELK-1 and HDAC2 to a G/C repressor element in the SM22-α promoter mediates transcriptional silencing during SMC phenotypic switching in vivo. Circ. Res. 111, 685–696 (2012).
Yoshida, T., Gan, Q. & Owens, G.K. Kruppel-like factor 4, Elk-1 and histone deacetylases cooperatively suppress smooth muscle cell differentiation markers in response to oxidized phospholipids. Am. J. Physiol. Cell Physiol. 295, C1175–C1182 (2008).
Hoshino, A. et al. Tumor exosome integrins determine organotropic metastasis. Nature 527, 329–335 (2015).
Gajos-Michniewicz, A., Duechler, M. & Czyz, M. miRNA in melanoma-derived exosomes. Cancer Lett. 347, 29–37 (2014).
Rafii, S. & Lyden, D. S100 chemokines mediate bookmarking of pre-metastatic niches. Nat. Cell Biol. 8, 1321–1323 (2006).
Deaton, R.A., Gan, Q. & Owens, G.K. Sp1-dependent activation of KLF4 is required for PDGF-BB-induced phenotypic modulation of smooth muscle. Am. J. Physiol. Heart Circ. Physiol. 296, H1027–H1037 (2009).
Yang, M., Du, Y., Xu, Z. & Jiang, Y. Functional effects of WNT1-inducible signaling pathway protein 1 on bronchial smooth muscle cell migration and proliferation in OVA-induced airway remodeling. Inflammation 39, 16–29 (2016).
Reddy, V.S., Valente, A.J., Delafontaine, P. & Chandrasekar, B. Interleukin-18–WNT1-inducible signaling pathway protein 1 signaling mediates human saphenous vein smooth muscle cell proliferation. J. Cell. Physiol. 226, 3303–3315 (2011).
Le, C.T.K. et al. Synergistic actions of blocking angiopoietin-2 and tumor necrosis factor–α in suppressing remodeling of blood vessels and lymphatics in airway inflammation. Am. J. Pathol. 185, 2949–2968 (2015).
Keskin, D. et al. Targeting vascular pericytes in hypoxic tumors increases lung metastasis via angiopoietin-2. Cell Rep. 10, 1066–1081 (2015).
Alexander, M.R., Murgai, M., Moehle, C.W. & Owens, G.K. Interleukin-1β modulates smooth muscle cell phenotype to a distinct inflammatory state relative to PDGF-DD via NF-κB-dependent mechanisms. Physiol. Genomics 44, 417–429 (2012).
Alexander, M.R. et al. Genetic inactivation of IL-1 signaling enhances atherosclerotic plaque instability and reduces outward vessel remodeling in advanced atherosclerosis in mice. J. Clin. Invest. 122, 70–79 (2012).
Dulauroy, S., Di Carlo, S.E., Langa, F., Eberl, G. & Peduto, L. Lineage tracing and genetic ablation of ADAM12+ perivascular cells identify a major source of profibrotic cells during acute tissue injury. Nat. Med. 18, 1262–1270 (2012).
Laklai, H. et al. Genotype tunes pancreatic ductal adenocarcinoma tissue tension to induce matricellular fibrosis and tumor progression. Nat. Med. 22, 497–505 (2016).
Bissell, M.J. & Radisky, D. Putting tumors in context. Nat. Rev. Cancer 1, 46–54 (2001).
Kessenbrock, K., Plaks, V. & Werb, Z. Matrix metalloproteinases: regulators of the tumor microenvironment. Cell 141, 52–67 (2010).
Cox, T.R. et al. LOX-mediated collagen cross-linking is responsible for fibrosis-enhanced metastasis. Cancer Res. 73, 1721–1732 (2013).
Del Pozo Martin, Y. et al. Mesenchymal cancer cell–stroma cross-talk promotes niche activation, epithelial reversion and metastatic colonization. Cell Rep. 13, 2456–2469 (2015).
Oskarsson, T., Batlle, E. & Massagué, J. Metastatic stem cells: sources, niches and vital pathways. Cell Stem Cell 14, 306–321 (2014).
LeBleu, V.S. et al. Origin and function of myofibroblasts in kidney fibrosis. Nat. Med. 19, 1047–1053 (2013).
Baluk, P., Falcón, B.L., Hashizume, H., Sennino, B. & McDonald, D.M. in Tumor Angiogenesis 557–576 (Springer, 2008).
Hanahan, D. & Folkman, J. Patterns and emerging mechanisms of the angiogenic switch during tumorigenesis. Cell 86, 353–364 (1996).
Bergers, G., Song, S., Meyer-Morse, N., Bergsland, E. & Hanahan, D. Benefits of targeting both pericytes and endothelial cells in the tumor vasculature with kinase inhibitors. J. Clin. Invest. 111, 1287–1295 (2003).
Morikawa, S. et al. Abnormalities in pericytes on blood vessels and endothelial sprouts in tumors. Am. J. Pathol. 160, 985–1000 (2002).
Fukumura, D. & Jain, R.K. Tumor microvasculature and microenvironment: targets for anti-angiogenesis and normalization. Microvasc. Res. 74, 72–84 (2007).
Chambers, A.F., Groom, A.C. & MacDonald, I.C. Dissemination and growth of cancer cells in metastatic sites. Nat. Rev. Cancer 2, 563–572 (2002).
Özdemir, B.C. et al. Depletion of carcinoma-associated fibroblasts and fibrosis induces immunosuppression and accelerates pancreas cancer with reduced survival. Cancer Cell 25, 719–734 (2014).
Murgai, M., Giles, A. & Kaplan, R. Physiological, tumor and metastatic niches: opportunities and challenges for targeting the tumor microenvironment. Crit. Rev. Oncog. 20, 301–314 (2015).
Hanoun, M. et al. Acute myelogenous leukemia–induced sympathetic neuropathy promotes malignancy in an altered hematopoietic stem cell niche. Cell Stem Cell 15, 365–375 (2014).
Butler, J.M., Kobayashi, H. & Rafii, S. Instructive role of the vascular niche in promoting tumor growth and tissue repair by angiocrine factors. Nat. Rev. Cancer 10, 138–146 (2010).
Kusumbe, A.P. et al. Age-dependent modulation of vascular niches for hematopoietic stem cells. Nature 532, 380–384 (2016).
Calabrese, C. et al. A perivascular niche for brain tumor stem cells. Cancer Cell 11, 69–82 (2007).
Wculek, S.K. & Malanchi, I. Neutrophils support lung colonization of metastasis-initiating breast cancer cells. Nature 528, 413–417 (2015).
Yu, F. et al. Kruppel-like factor 4 (KLF4) is required for maintenance of breast cancer stem cells and for cell migration and invasion. Oncogene 30, 2161–2172 (2011).
Wei, D., Kanai, M., Huang, S. & Xie, K. Emerging role of KLF4 in human gastrointestinal cancer. Carcinogenesis 27, 23–31 (2006).
Pandya, A.Y. et al. Nuclear localization of KLF4 is associated with an aggressive phenotype in early-stage breast cancer. Clin. Cancer Res. 10, 2709–2719 (2004).
Meadors, J.L. et al. Murine rhabdomyosarcoma is immunogenic and responsive to T cell–based immunotherapy. Pediatr. Blood Cancer 57, 921–929 (2011).
Carpenter, A.E. et al. CellProfiler: image analysis software for identifying and quantifying cell phenotypes. Genome Biol. 7, R100 (2006).
Faul, F., Erdfelder, E., Buchner, A. & Lang, A.-G. Statistical power analyses using G*Power 3.1: tests for correlation and regression analyses. Behav. Res. Methods 41, 1149–1160 (2009).
Acknowledgements
We thank K. McKinnon and C. Thiele for their advice, and Z. Liu, M. Kasai, J. Zhu and K. Bhatt for their technical assistance. This work was supported by the US National Institutes of Health (grants 1ZIABC011332-07, 1ZIABC011334-07, NIH HL057353 and NIH HL135018).
Author information
Authors and Affiliations
Contributions
M.M. conducted most of the experiments, performed data analysis, generated most of the experimental mice and was the primary writer of the manuscript; W.J. conducted in vivo metastasis studies and in vitro matrix experiments, generated RNA for sequencing and analyzed exosomal content by western blot; M.E. conducted in vitro immunostaining and western blot experiments; J.K. assisted with the generation of experimental mice and conducted image analysis; D.W.B. and S.K. assisted with mouse experiments, and generated and analyzed flow cytometry data; M.M.M. analyzed pathological tissue specimens; M.K. assisted with confocal image acquisition, analysis and figure preparation; H.L. and J.F.S. analyzed RNA-seq data and assisted with figure preparation; O.A.C. and G.K.O. generated preliminary data, provided initial experimental mice and provided advice throughout; R.N.K. supervised the project and provided guidance on experimental design, data interpretation and writing of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Supplementary Text and Figures
Supplementary Figures 1–12 & Supplementary Table 1. (PDF 6364 kb)
Rights and permissions
About this article
Cite this article
Murgai, M., Ju, W., Eason, M. et al. KLF4-dependent perivascular cell plasticity mediates pre-metastatic niche formation and metastasis. Nat Med 23, 1176–1190 (2017). https://doi.org/10.1038/nm.4400
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nm.4400
This article is cited by
-
Informing immunotherapy with multi-omics driven machine learning
npj Digital Medicine (2024)
-
Regulation and signaling pathways in cancer stem cells: implications for targeted therapy for cancer
Molecular Cancer (2023)
-
Gastric cancer-derived LBP promotes liver metastasis by driving intrahepatic fibrotic pre-metastatic niche formation
Journal of Experimental & Clinical Cancer Research (2023)
-
The evolution and heterogeneity of neutrophils in cancers: origins, subsets, functions, orchestrations and clinical applications
Molecular Cancer (2023)
-
Pan-cancer spatially resolved single-cell analysis reveals the crosstalk between cancer-associated fibroblasts and tumor microenvironment
Molecular Cancer (2023)