Abstract
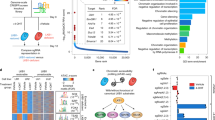
Lung cancer is the leading cause of cancer deaths worldwide, with the majority of mortality resulting from metastatic spread. However, the molecular mechanism by which cancer cells acquire the ability to disseminate from primary tumors, seed distant organs, and grow into tissue-destructive metastases remains incompletely understood. We combined tumor barcoding in a mouse model of human lung adenocarcinoma with unbiased genomic approaches to identify a transcriptional program that confers metastatic ability and predicts patient survival. Small-scale in vivo screening identified several genes, including Cd109, that encode novel pro-metastatic factors. We uncovered signaling mediated by Janus kinases (Jaks) and the transcription factor Stat3 as a critical, pharmacologically targetable effector of CD109-driven lung cancer metastasis. In summary, by coupling the systematic genomic analysis of purified cancer cells in distinct malignant states from mouse models with extensive human validation, we uncovered several key regulators of metastatic ability, including an actionable pro-metastatic CD109–Jak–Stat3 axis.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
References
Nguyen, D.X., Bos, P.D. & Massagué, J. Metastasis: from dissemination to organ-specific colonization. Nat. Rev. Cancer 9, 274–284 (2009).
Massagué, J. & Obenauf, A.C. Metastatic colonization by circulating tumor cells. Nature 529, 298–306 (2016).
Winslow, M.M. et al. Suppression of lung adenocarcinoma progression by Nkx2-1. Nature 473, 101–104 (2011).
Bos, P.D. et al. Genes that mediate breast cancer metastasis to the brain. Nature 459, 1005–1009 (2009).
Nguyen, D.X. et al. WNT–TCF signaling through LEF1 and HOXB9 mediates lung adenocarcinoma metastasis. Cell 138, 51–62 (2009).
Yang, J. et al. Twist, a master regulator of morphogenesis, plays an essential role in tumor metastasis. Cell 117, 927–939 (2004).
Clark, E.A., Golub, T.R., Lander, E.S. & Hynes, R.O. Genomic analysis of metastasis reveals an essential role for RhoC. Nature 406, 532–535 (2000).
Jackson, E.L. et al. The differential effects of mutant p53 alleles on advanced murine lung cancer. Cancer Res. 65, 10280–10288 (2005).
Kirsch, D.G. et al. A spatially and temporally restricted mouse model of soft-tissue sarcoma. Nat. Med. 13, 992–997 (2007).
Chiou, S.H. et al. Pancreatic cancer modeling using retrograde viral vector delivery and in vivo CRISPR–Cas9-mediated somatic genome editing. Genes Dev. 29, 1576–1585 (2015).
Meuwissen, R. et al. Induction of small-cell lung cancer by somatic inactivation of both Trp53 and Rb1 in a conditional mouse model. Cancer Cell 4, 181–189 (2003).
Kim, M. et al. Comparative oncogenomics identifies NEDD9 as a melanoma metastasis gene. Cell 125, 1269–1281 (2006).
Ding, L. et al. Somatic mutations affect key pathways in lung adenocarcinoma. Nature 455, 1069–1075 (2008).
Takahashi, T. et al. p53: a frequent target for genetic abnormalities in lung cancer. Science 246, 491–494 (1989).
Rodenhuis, S. et al. Mutational activation of the Kras oncogene. A possible pathogenetic factor in adenocarcinoma of the lung. N. Engl. J. Med. 317, 929–935 (1987).
Rodenhuis, S. et al. Incidence and possible clinical significance of Kras oncogene activation in adenocarcinoma of the human lung. Cancer Res. 48, 5738–5741 (1988).
Weir, B.A. et al. Characterizing the cancer genome in lung adenocarcinoma. Nature 450, 893–898 (2007).
Siegel, R.L., Miller, K.D. & Jemal, A. Cancer statistics, 2016. CA Cancer J. Clin. 66, 7–30 (2016).
Jackson, E.L. et al. Analysis of lung tumor initiation and progression using conditional expression of oncogenic Kras. Genes Dev. 15, 3243–3248 (2001).
Caswell, D.R. et al. Obligate progression precedes lung adenocarcinoma dissemination. Cancer Discov. 4, 781–789 (2014).
Cheung, W.K. et al. Control of alveolar differentiation by the lineage transcription factors GATA6 and HOPX inhibits lung adenocarcinoma metastasis. Cancer Cell 23, 725–738 (2013).
Kim, W.Y. et al. HIF-2α cooperates with RAS to promote lung tumorigenesis in mice. J. Clin. Invest. 119, 2160–2170 (2009).
Shedden, K. et al. Gene-expression-based survival prediction in lung adenocarcinoma: a multi-site, blinded validation study. Nat. Med. 14, 822–827 (2008).
Der, S.D. et al. Validation of a histology-independent prognostic gene signature for early-stage, non-small-cell lung cancer including stage IA patients. J. Thorac. Oncol. 9, 59–64 (2014).
Van Laar, R.K. Genomic signatures for predicting survival and adjuvant chemotherapy benefit in patients with non-small-cell lung cancer. BMC Med. Genomics 5, 30 (2012).
Gao, J. et al. Integrative analysis of complex cancer genomics and clinical profiles using the cBioPortal. Sci. Signal. 6, pl1 (2013).
Gyo˝rffy, B., Surowiak, P., Budczies, J. & Lánczky, A. Online survival analysis software to assess the prognostic value of biomarkers using transcriptomic data in non-small-cell lung cancer. PLoS One 8, e82241 (2013).
Brady, J.J. et al. An Arntl2-driven secretome enables lung adenocarcinoma metastatic self-sufficiency. Cancer Cell 29, 697–710 (2016).
Finnson, K.W. et al. Identification of CD109 as part of the TGF-β receptor system in human keratinocytes. FASEB J. 20, 1525–1527 (2006).
Bizet, A.A. et al. The TGF-β co-receptor, CD109, promotes internalization and degradation of TGF-β receptors. Biochim. Biophys. Acta 1813, 742–753 (2011).
Mii, S. et al. Epidermal hyperplasia and appendage abnormalities in mice lacking CD109. Am. J. Pathol. 181, 1180–1189 (2012).
Litvinov, I.V. et al. CD109 release from the cell surface in human keratinocytes regulates TGF-β receptor expression, TGF-β signaling and STAT3 activation: relevance to psoriasis. Exp. Dermatol. 20, 627–632 (2011).
Hagiwara, S. et al. Processing of CD109 by furin and its role in the regulation of TGF-β signaling. Oncogene 29, 2181–2191 (2010).
Govindan, R. et al. Genomic landscape of non-small-cell lung cancer in smokers and never-smokers. Cell 150, 1121–1134 (2012).
Lipson, D. et al. Identification of new ALK and RET gene fusions from colorectal and lung cancer biopsies. Nat. Med. 18, 382–384 (2012).
Xu, Y.H. & Lu, S. A meta-analysis of STAT3 and phospho-STAT3 expression and survival of patients with non-small-cell lung cancer. Eur. J. Surg. Oncol. 40, 311–317 (2014).
Jiang, R. et al. Correlation of activated STAT3 expression with clinicopathologic features in lung adenocarcinoma and squamous cell carcinoma. Mol. Diagn. Ther. 15, 347–352 (2011).
Bromberg, J.F. et al. Stat3 as an oncogene. Cell 98, 295–303 (1999).
Zhang, J.M. et al. CD109 attenuates TGF-β1 signaling and enhances EGF signaling in SK-MG-1 human glioblastoma cells. Biochem. Biophys. Res. Commun. 459, 252–258 (2015).
Ding, Z. et al. SMAD4-dependent barrier constrains prostate cancer growth and metastatic progression. Nature 470, 269–273 (2011).
David, C.J. et al. TGF-β tumor suppression through a lethal EMT. Cell 164, 1015–1030 (2016).
Zhong, Z., Wen, Z. & Darnell, J.E. Jr. Stat3: a STAT family member activated by tyrosine phosphorylation in response to epidermal growth factor and interleukin-6. Science 264, 95–98 (1994).
Parganas, E. et al. Jak2 is essential for signaling through a variety of cytokine receptors. Cell 93, 385–395 (1998).
Yu, C.L. et al. Enhanced DNA-binding activity of a Stat3-related protein in cells transformed by the Src oncoprotein. Science 269, 81–83 (1995).
Matsunaga, Y. et al. Effects of a Janus kinase inhibitor, pyridone 6, on airway responses in a murine model of asthma. Biochem. Biophys. Res. Commun. 404, 261–267 (2011).
Pedranzini, L. et al. Pyridone 6, a pan–Janus-activated kinase inhibitor, induces growth inhibition of multiple myeloma cells. Cancer Res. 66, 9714–9721 (2006).
Quintás-Cardama, A. et al. Preclinical characterization of the selective JAK1/2 inhibitor INCB018424: therapeutic implications for the treatment of myeloproliferative neoplasms. Blood 115, 3109–3117 (2010).
Van Rompaey, L. et al. Preclinical characterization of GLPG0634, a selective inhibitor of JAK1, for the treatment of inflammatory diseases. J. Immunol. 191, 3568–3577 (2013).
Tao, J., Li, H., Li, Q. & Yang, Y. CD109 is a potential target for triple-negative breast cancer. Tumour Biol. 35, 12083–12090 (2014).
Zhang, F. et al. SWATH- and iTRAQ-based quantitative proteomic analyses reveal an overexpression and biological relevance of CD109 in advanced NSCLC. J. Proteomics 102, 125–136 (2014).
Greenleaf, W.J. Assaying the epigenome in limited numbers of cells. Methods 72, 51–56 (2015).
Denny, S.K. et al. Nfib promotes metastasis through a widespread increase in chromatin accessibility. Cell 166, 328–342 (2016).
Takeda, K. et al. Targeted disruption of the mouse Stat3 gene leads to early embryonic lethality. Proc. Natl. Acad. Sci. USA 94, 3801–3804 (1997).
Steeg, P.S. Targeting metastasis. Nat. Rev. Cancer 16, 201–218 (2016).
Tuveson, D.A. et al. Endogenous oncogenic K-rasG12D stimulates proliferation and widespread neoplastic and developmental defects. Cancer Cell 5, 375–387 (2004).
DuPage, M., Dooley, A.L. & Jacks, T. Conditional mouse lung cancer models using adenoviral or lentiviral delivery of Cre recombinase. Nat. Protoc. 4, 1064–1072 (2009).
Li, H. et al. The Sequence Alignment/Map format and SAMtools. Bioinformatics 25, 2078–2079 (2009).
Piskol, R., Ramaswami, G. & Li, J.B. Reliable identification of genomic variants from RNA–seq data. Am. J. Hum. Genet. 93, 641–651 (2013).
Li, H. & Durbin, R. Fast and accurate short read alignment with Burrows–Wheeler transform. Bioinformatics 25, 1754–1760 (2009).
McKenna, A. et al. The Genome Analysis Toolkit: a MapReduce framework for analyzing next-generation DNA sequencing data. Genome Res. 20, 1297–1303 (2010).
Patro, R., Mount, S.M. & Kingsford, C. Sailfish enables alignment-free isoform quantification from RNA–seq reads using lightweight algorithms. Nat. Biotechnol. 32, 462–464 (2014).
Leek, J.T. & Storey, J.D. Capturing heterogeneity in gene expression studies by surrogate variable analysis. PLoS Genet. 3, 1724–1735 (2007).
Smyth, G.K. Linear models and empirical Bayes methods for assessing differential expression in microarray experiments. Stat. Appl. Genet. Mol. Biol. 3, Article3 (2004).
Durinck, S., Spellman, P.T., Birney, E. & Huber, W. Mapping identifiers for the integration of genomic datasets with the R/Bioconductor package biomaRt. Nat. Protoc. 4, 1184–1191 (2009).
Subramanian, A. et al. Gene set enrichment analysis: a knowledge-based approach for interpreting genome-wide expression profiles. Proc. Natl. Acad. Sci. USA 102, 15545–15550 (2005).
Cancer Genome Atlas Research Network. Comprehensive molecular profiling of lung adenocarcinoma. Nature 511, 543–550 (2014).
Ishwaran, H. & Kogalur, U.B. Random survival forests for R. R News 7, 25–31 (2007).
Ishwaran, H., Kogalur, U.B., Blackstone, E.H. & Lauer, M.S. Random survival forests. Ann. Appl. Stat. 2, 841–860 (2008).
Trapnell, C. et al. Differential gene and transcript expression analysis of RNA–seq experiments with TopHat and Cufflinks. Nat. Protoc. 7, 562–578 (2012).
Doench, J.G. et al. Rational design of highly active sgRNAs for CRISPR-Cas9-mediated gene inactivation. Nat. Biotechnol. 32, 1262–1267 (2014).
Sanjana, N.E., Shalem, O. & Zhang, F. Improved vectors and genome-wide libraries for CRISPR screening. Nat. Methods 11, 783–784 (2014).
Morimoto-Tomita, M., Ohashi, Y., Matsubara, A., Tsuiji, M. & Irimura, T. Mouse colon carcinoma cells established for high incidence of experimental hepatic metastasis exhibit accelerated and anchorage-independent growth. Clin. Exp. Metastasis 22, 513–521 (2005).
Gebäck, T., Schulz, M.M., Koumoutsakos, P. & Detmar, M. TScratch: a novel and simple software tool for automated analysis of monolayer wound healing assays. Biotechniques 46, 265–274 (2009).
Acknowledgements
We thank P. Chu and S. Cheemalavagu for technical assistance, the Stanford Shared FACS Facility and Protein and Nucleic Acid Facility for expert assistance, J. Pollack and X. Gong for reagents, S. Dolan and A. Orantes for administrative support, and D. Feldser, C. Murray, and members of the Winslow lab for helpful comments. This work was supported by an American Lung Association Fellowship (C.-H.C.), the US National Institutes of Health (NIH) (grant no. F32-CA189659 (J.J.B.), T32-CA009302 (A.L.S.), R01-GM102484 (J.B.L.), R01-CA157510 (E.A.S.-C.), R01-CA175336 (M.M.W.), and R01-CA204620 (M.M.W.)), the Stanford Biomedical Informatics Training Grant from the National Library of Medicine (LM-07033; P.G.G.), a Bio-X Stanford Interdisciplinary Graduate Fellowship (P.G.G.), Stanford Graduate Fellowships (Z.N.R. and G.R.), National Science Foundation Graduate Research Fellowships (D.R.C. and Z.N.R.), the Spider Internship Funds (A.F.W.), an Alfred Sloan Fellowship (A.K.), a V Foundation for Cancer Research Martin D. Abeloff, M.D. V Scholar Award (M.M.W.), and, in part, by a Stanford Cancer Institute support grant (NIH P30-CA124435).
Author information
Authors and Affiliations
Contributions
C.-H.C. and M.M.W. conceived the study; C.-H.C. designed, conducted, and analyzed the majority of experiments; P.G.G. conducted the majority of bioinformatics analyses; Z.N.R., J.J.B., D.Y., R.K.M., D.R.C., S.-H.C., A.F.W., B.M.G., A.L.S., and K.E.K. conducted experiments, analyzed data and contributed to the Discussion; G.R. and J.B.L. (SNPiR), L.C.S. and E.A.S.-C. (pLKO library and human lung cell lines), and A.K. (bioinformatics) provided crucial reagents and discussion; and M.M.W. and C.-H.C. wrote the manuscript with comments from all authors.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Supplementary Figures
Supplementary Figures 1–22 (PDF 15113 kb)
Supplementary Table 1
Gene expression profiles for all ex vivo samples. (XLS 27399 kb)
Supplementary Tables 2–8
Supplementary Table 2: Gene sets that are higher in late stage primary tumours(TnonMet and TMet) relative to KPT-Early/KT samples. Supplementary Table 3: Gene sets that are lower in late stage primary tumours(TnonMet and TMet) relative to KPT-Early/KT samples. Supplementary Table 4: Gene sets that are higher in metastases (Met) relative to nonmetastatic primary tumours (TnonMet). Supplementary Table 5: Gene sets that are lower in metastases (Met) relative to nonmetastatic primary tumours (TnonMet). Supplementary Table 6: Gene expression changes elicited by Cd109 knockdown. Supplementary Table 7: Gene sets that are higher in cells with Cd109 knocked down relative to control cells. Supplementary Table 8: Gene sets that are lower in cells with Cd109 knocked down relative to control cells. (XLS 3803 kb)
Supplementary Table 9
List of pLKO plasmids (XLSX 30 kb)
Supplementary Table10
List of qPCR Primers (XLSX 25 kb)
Rights and permissions
About this article
Cite this article
Chuang, CH., Greenside, P., Rogers, Z. et al. Molecular definition of a metastatic lung cancer state reveals a targetable CD109–Janus kinase–Stat axis. Nat Med 23, 291–300 (2017). https://doi.org/10.1038/nm.4285
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nm.4285
This article is cited by
-
Ubiquitin ligase subunit FBXO9 inhibits V-ATPase assembly and impedes lung cancer metastasis
Experimental Hematology & Oncology (2024)
-
Protein lipidation in health and disease: molecular basis, physiological function and pathological implication
Signal Transduction and Targeted Therapy (2024)
-
STAT3 potentiates RNA polymerase I-directed transcription and tumor growth by activating RPA34 expression
British Journal of Cancer (2023)
-
Drug-tolerant persister cells in cancer: the cutting edges and future directions
Nature Reviews Clinical Oncology (2023)
-
Multiplexed screens identify RAS paralogues HRAS and NRAS as suppressors of KRAS-driven lung cancer growth
Nature Cell Biology (2023)