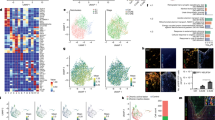
Abstract
At low levels, carbon monoxide (CO) has physiological roles as a second messenger and neuromodulator1,2. Here we assess the effects of CO in a mouse model of traumatic brain injury (TBI). Treatment with CO-releasing molecule (CORM)-3 reduced pericyte death and ameliorated the progression of neurological deficits. In contrast, although treatment with the radical scavenger N-tert-butyl-a-phenylnitrone (PBN) also reduced pericyte death, neurological outcomes were not rescued. As compared to vehicle-treated control and PBN-treated mice, CORM-3-treated mice showed higher levels of phosphorylated neural nitric oxide synthase within neural stem cells (NSCs). Inhibition of nitric oxide synthase diminished the CORM-3-mediated increase in the number of cells that stained positive for both the neuronal marker NeuN and 5-bromo-2′-deoxyuridine (BrdU; a marker for proliferating cells) in vivo, consequently interfering with neurological recovery after TBI. Because NSCs seemed to be in close proximity to pericytes, we asked whether cross-talk between pericytes and NSCs was induced by CORM-3, thereby promoting neurogenesis. In pericyte cultures that were undergoing oxygen and glucose deprivation, conditioned cell culture medium collected after CORM-3 treatment enhanced the in vitro differentiation of NSCs into mature neurons. Taken together, these findings suggest that CO treatment may provide a therapeutic approach for TBI by preventing pericyte death, rescuing cross-talk with NSCs and promoting neurogenesis.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Motterlini, R. & Otterbein, L.E. The therapeutic potential of carbon monoxide. Nat. Rev. Drug Discov. 9, 728–743 (2010).
Verma, A., Hirsch, D.J., Glatt, C.E., Ronnett, G.V. & Snyder, S.H. Carbon monoxide: a putative neural messenger. Science 259, 381–384 (1993).
Loane, D.J. & Faden, A.I. Neuroprotection for traumatic brain injury: translational challenges and emerging therapeutic strategies. Trends Pharmacol. Sci. 31, 596–604 (2010).
Xiong, Y., Mahmood, A. & Chopp, M. Animal models of traumatic brain injury. Nat. Rev. Neurosci. 14, 128–142 (2013).
Xiong, Y., Mahmood, A. & Chopp, M. Emerging treatments for traumatic brain injury. Expert Opin. Emerg. Drugs 14, 67–84 (2009).
Wang, G. et al. HDAC inhibition prevents white matter injury by modulating microglia–macrophage polarization through the GSK-3β–PTEN–Akt axis. Proc. Natl. Acad. Sci. USA 112, 2853–2858 (2015).
Hu, X. et al. Neurobiology of microglial action in CNS injuries: receptor-mediated signaling mechanisms and functional roles. Prog. Neurobiol. 119-120, 60–84 (2014).
Bell, R.D. et al. Pericytes control key neurovascular functions and neuronal phenotype in the adult brain and during brain aging. Neuron 68, 409–427 (2010).
Bell, R.D. et al. Apolipoprotein E controls cerebrovascular integrity via cyclophilin A. Nature 485, 512–516 (2012).
Goldman, S.A. & Chen, Z. Perivascular instruction of cell genesis and fate in the adult brain. Nat. Neurosci. 14, 1382–1389 (2011).
Chen, J. et al. The localization of neuronal nitric oxide synthase may influence its role in neuronal precursor proliferation and synaptic maintenance. Dev. Biol. 269, 165–182 (2004).
Yemisci, M. et al. Pericyte contraction induced by oxidative–nitrative stress impairs capillary reflow despite successful opening of an occluded cerebral artery. Nat. Med. 15, 1031–1037 (2009).
Winkler, E.A., Bell, R.D. & Zlokovic, B.V. Central nervous system pericytes in health and disease. Nat. Neurosci. 14, 1398–1405 (2011).
Lo, E.H., Lok, J., Ning, M. & Whalen, M. (eds.) Vascular Mechanisms in CNS Trauma (Springer, New York, 2014).
Xing, C. & Lo, E.H. Help-me signaling: non-cell-autonomous mechanisms of neuroprotection and neurorecovery. Prog. Neurobiol. S0301-0082(15)30024-1 (2016).
Fujita, T. et al. Paradoxical rescue from ischemic lung injury by inhaled carbon monoxide driven by de-repression of fibrinolysis. Nat. Med. 7, 598–604 (2001).
Lo, E.H. Degeneration and repair in central nervous system disease. Nat. Med. 16, 1205–1209 (2010).
National Research Council. Guide for the Care and Use of Laboratory Animals 8th edn. (The National Academies Press, 2011).
Acknowledgements
This work was supported in part by grants from the US National Institutes of Health (K.H., K.A., M.J.W., C.X., X.W. and E.H.L.), the Rappaport Foundation (E.H.L.), the Research Abroad grant from the National Research Foundation of Korea (Y.K.C., S.-H.K., Y.-M.K. and K.-W.K.) and the Global Research Laboratory Program of Korea (K.-W.K.). The vector expressing the HIF-1α double mutant was kindly provided by G.L. Semenza (Johns Hopkins University School of Medicine).
Author information
Authors and Affiliations
Contributions
Y.K.C. and E.H.L. designed experiments and wrote the manuscript; Y.K.C., T.M., E.T.M., C.X., S.-H.K., K.H. and X.W. performed experiments; K.A., Y.-M.K., M.J.W., X.W. and K.-W.K. analyzed and critically discussed the data; and E.H.L. supervised the project.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Supplementary Text and Figures
Supplementary Figures 1–8 (PDF 4214 kb)
Rights and permissions
About this article
Cite this article
Choi, Y., Maki, T., Mandeville, E. et al. Dual effects of carbon monoxide on pericytes and neurogenesis in traumatic brain injury. Nat Med 22, 1335–1341 (2016). https://doi.org/10.1038/nm.4188
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nm.4188
This article is cited by
-
Inhibition of the NLRP3 Inflammasome Activation/Assembly through the Activation of the PI3K Pathway by Naloxone Protects Neural Stem Cells from Ischemic Condition
Molecular Neurobiology (2023)
-
Chronic effects of blast injury on the microvasculature in a transgenic mouse model of Alzheimer’s disease related Aβ amyloidosis
Fluids and Barriers of the CNS (2022)
-
Endothelial cells regulate astrocyte to neural progenitor cell trans-differentiation in a mouse model of stroke
Nature Communications (2022)
-
Carbon Monoxide Protects Neural Stem Cells Against Iron Overload by Modulating the Crosstalk Between Nrf2 and NF-κB Signaling
Neurochemical Research (2022)
-
Neural correlates of beneficial effects of young plasma treatment in aged mice: PET-SPM analyses and neuro-behavioural/molecular biological studies
European Journal of Nuclear Medicine and Molecular Imaging (2022)