Abstract
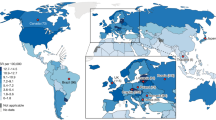
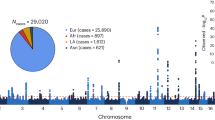
Several genetic alterations characteristic of leukemia and lymphoma have been detected in the blood of individuals without apparent hematological malignancies. The Cancer Genome Atlas (TCGA) provides a unique resource for comprehensive discovery of mutations and genes in blood that may contribute to the clonal expansion of hematopoietic stem/progenitor cells. Here, we analyzed blood-derived sequence data from 2,728 individuals from TCGA and discovered 77 blood-specific mutations in cancer-associated genes, the majority being associated with advanced age. Remarkably, 83% of these mutations were from 19 leukemia and/or lymphoma-associated genes, and nine were recurrently mutated (DNMT3A, TET2, JAK2, ASXL1, TP53, GNAS, PPM1D, BCORL1 and SF3B1). We identified 14 additional mutations in a very small fraction of blood cells, possibly representing the earliest stages of clonal expansion in hematopoietic stem cells. Comparison of these findings to mutations in hematological malignancies identified several recurrently mutated genes that may be disease initiators. Our analyses show that the blood cells of more than 2% of individuals (5–6% of people older than 70 years) contain mutations that may represent premalignant events that cause clonal hematopoietic expansion.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Welch, J.S. et al. The origin and evolution of mutations in acute myeloid leukemia. Cell 150, 264–278 (2012).
Limpens, J. et al. Lymphoma-associated translocation t(14;18) in blood B cells of normal individuals. Blood 85, 2528–2536 (1995).
Liu, Y., Hernandez, A.M., Shibata, D. & Cortopassi, G.A. BCL2 translocation frequency rises with age in humans. Proc. Natl. Acad. Sci. USA 91, 8910–8914 (1994).
Biernaux, C., Loos, M., Sels, A., Huez, G. & Stryckmans, P. Detection of major bcr-abl gene expression at a very low level in blood cells of some healthy individuals. Blood 86, 3118–3122 (1995).
Forsberg, L.A. et al. Age-related somatic structural changes in the nuclear genome of human blood cells. Am. J. Hum. Genet. 90, 217–228 (2012).
Jacobs, K.B. et al. Detectable clonal mosaicism and its relationship to aging and cancer. Nat. Genet. 44, 651–658 (2012).
Laurie, C.C. et al. Detectable clonal mosaicism from birth to old age and its relationship to cancer. Nat. Genet. 44, 642–650 (2012).
Busque, L. et al. Recurrent somatic TET2 mutations in normal elderly individuals with clonal hematopoiesis. Nat. Genet. 44, 1179–1181 (2012).
Shlush, L.I. et al. Identification of pre-leukaemic haematopoietic stem cells in acute leukaemia. Nature 506, 328–333 (2014).
Kanchi, K.L. et al. Integrated analysis of germline and somatic variants in ovarian cancer. Nat. Commun. 5, 3256 (2014).
Kandoth, C. et al. Mutational landscape and significance across 12 major cancer types. Nature 502, 333–339 (2013).
Vogelstein, B. et al. Cancer genome landscapes. Science 339, 1546–1558 (2013).
Lawrence, M.S. et al. Discovery and saturation analysis of cancer genes across 21 tumour types. Nature 505, 495–501 (2014).
Pritchard, C.C. et al. Validation and implementation of targeted capture and sequencing for the detection of actionable mutation, copy number variation, and gene rearrangement in clinical cancer specimens. J. Mol. Diagn. 16, 56–67 (2014).
Frampton, G.M. et al. Development and validation of a clinical cancer genomic profiling test based on massively parallel DNA sequencing. Nat. Biotechnol. 31, 1023–1031 (2013).
Ley, T.J. et al. DNMT3A mutations in acute myeloid leukemia. N. Engl. J. Med. 363, 2424–2433 (2010).
Delhommeau, F. et al. Mutation in TET2 in myeloid cancers. N. Engl. J. Med. 360, 2289–2301 (2009).
Kralovics, R. et al. A gain-of-function mutation of JAK2 in myeloproliferative disorders. N. Engl. J. Med. 352, 1779–1790 (2005).
Gelsi-Boyer, V. et al. Mutations of polycomb-associated gene ASXL1 in myelodysplastic syndromes and chronic myelomonocytic leukaemia. Br. J. Haematol. 145, 788–800 (2009).
Abdel-Wahab, O. et al. Deletion of Asxl1 results in myelodysplasia and severe developmental defects in vivo. J. Exp. Med. 210, 2641–2659 (2013).
Cancer Genome Atlas Research Network. Genomic and epigenomic landscapes of adult de novo acute myeloid leukemia. N. Engl. J. Med. 368, 2059–2074 (2013).
Yoshida, K. et al. Frequent pathway mutations of splicing machinery in myelodysplasia. Nature 478, 64–69 (2011).
Li, M. et al. Somatic mutations in the transcriptional corepressor gene BCORL1 in adult acute myelogenous leukemia. Blood 118, 5914–5917 (2011).
Zhang, J. et al. The genetic basis of early T-cell precursor acute lymphoblastic leukaemia. Nature 481, 157–163 (2012).
Perez-Garcia, A. et al. Genetic loss of SH2B3 in acute lymphoblastic leukemia. Blood 122, 2425–2432 (2013).
Bejar, R. et al. Clinical effect of point mutations in myelodysplastic syndromes. N. Engl. J. Med. 364, 2496–2506 (2011).
Weinstein, L.S. Gsα mutations in fibrous dysplasia and McCune-Albright syndrome. J. Bone Miner. Res. 21 (suppl. 2), P120–P124 (2006).
Aldred, M.A. & Trembath, R.C. Activating and inactivating mutations in the human GNAS1 gene. Hum. Mutat. 16, 183–189 (2000).
Lumbroso, S., Paris, F. & Sultan, C. Activating Gsα mutations: analysis of 113 patients with signs of McCune-Albright syndrome—a European Collaborative Study. J. Clin. Endocrinol. Metab. 89, 2107–2113 (2004).
Ringel, M.D., Schwindinger, W.F. & Levine, M.A. Clinical implications of genetic defects in G proteins. The molecular basis of McCune-Albright syndrome and Albright hereditary osteodystrophy. Medicine 75, 171–184 (1996).
Ruark, E. et al. Mosaic PPM1D mutations are associated with predisposition to breast and ovarian cancer. Nature 493, 406–410 (2013).
Nangalia, J. et al. Somatic CALR mutations in myeloproliferative neoplasms with nonmutated JAK2. N. Engl. J. Med. 369, 2391–2405 (2013).
Walter, M.J. et al. Clonal diversity of recurrently mutated genes in myelodysplastic syndromes. Leukemia 27, 1275–1282 (2013).
Landau, D.A. et al. Evolution and impact of subclonal mutations in chronic lymphocytic leukemia. Cell 152, 714–726 (2013).
Akalin, A. et al. Base-pair resolution DNA methylation sequencing reveals profoundly divergent epigenetic landscapes in acute myeloid leukemia. PLoS Genet. 8, e1002781 (2012).
Lu, C. et al. Induction of sarcomas by mutant IDH2. Genes Dev. 27, 1986–1998 (2013).
Siegel, R., Naishadham, D. & Jemal, A. Cancer statistics, 2013. CA Cancer J. Clin. 63, 11–30 (2013).
Li, H. & Durbin, R. Fast and accurate short read alignment with Burrows-Wheeler transform. Bioinformatics 25, 1754–1760 (2009).
Koboldt, D.C. et al. VarScan 2: somatic mutation and copy number alteration discovery in cancer by exome sequencing. Genome Res. 22, 568–576 (2012).
McKenna, A. et al. The Genome Analysis Toolkit: a MapReduce framework for analyzing next-generation DNA sequencing data. Genome Res. 20, 1297–1303 (2010).
Ye, K., Schulz, M.H., Long, Q., Apweiler, R. & Ning, Z. Pindel: a pattern growth approach to detect break points of large deletions and medium sized insertions from paired-end short reads. Bioinformatics 25, 2865–2871 (2009).
Rehm, H.L. et al. ACMG clinical laboratory standards for next-generation sequencing. Genet. Med. 15, 733–747 (2013).
Acknowledgements
This work was supported by US National Cancer Institute grants R01CA180006 to L.D. and PO1CA101937 to T.J.L. and US National Human Genome Research Institute grants U54HG003079 to R.K.W. and U01HG006517 to L.D. M.J.W. is supported by a Leukemia and Lymphoma Society Scholar Award (1230-14), and J.S.W. is supported by R00HL103975. We thank M. Wyczalkowski for suggestions on figures and C. Kandoth on somatic mutation analysis. We also acknowledge The Cancer Genome Atlas as the source of primary data.
Author information
Authors and Affiliations
Contributions
L.D. designed and supervised research. M.X., C.L., J.W., M.D.M., M.C.W., H.K.S., V.Y., C.A.M., J.S.W., D.C.L., M.J.W., T.J.L., F.C. K.J.J. and L.D. analyzed the data. T.J.L., J.S.W., D.C.L., M.J.W. and J.F.D. provided disease-specific analysis. M.C.W. performed statistical analysis. E.R.M. and R.K.W. directed sequencing experiments. M.X., M.D.M., C.L., M.C.W. and J.F.M. prepared figures and tables. L.D. and F.C. wrote the manuscript. L.D., T.J.L., B.A.O. and M.C.W. revised the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Supplementary Text and Figures
Supplementary Figures 1 and 2 (PDF 538 kb)
Supplementary Table 1
Sample IDs for the 2,728 TCGA cases included in this study. (XLSX 90 kb)
Supplementary Table 2
Samples included in the study and their clinical characteristics. (XLSX 12 kb)
Supplementary Table 3
The distribution of germline variants across 2,728 TCGA samples. TCGA ovarian counts were collected from the previous report (XLSX 10 kb)
Supplementary Table 4
Somatic mutations in 2,241 TCGA tumor samples included in the study. Somatic mutation data are unavailable for a subset of samples. (XLSX 23405 kb)
Supplementary Table 5
Somatic mutations in 3,355 TCGA tumor samples from 12 cancer types used for identifying recurrent mutations. (XLSX 24682 kb)
Supplementary Table 6
Recurrent somatic mutations from 12 TCGA cancer types used for hotspot analysis. (XLSX 859 kb)
Supplementary Table 7
556 cancer-associated genes used in this study. (XLSX 15 kb)
Supplementary Table 8
77 blood-specific events detected in 2,728 cases using our standard discovery pipeline. (XLSX 53 kb)
Supplementary Table 9
Low-level blood-specific events detected in DNMT3A, JAK2, SF3B1, GNAS and IDH2 in TCGA samples. (XLSX 9 kb)
Supplementary Table 10
Deep-sequencing based validation of low-level blood-specific events detected in DNMT3A, JAK2 and SF3B1 in TCGA samples. (XLSX 13 kb)
Supplementary Table 11
Truncation and hotspot variants in four prominent genes (DNMT3A, TET2, JAK2 and ASXL1) involved in HSPC clonal expansion in 6,503 ESP samples. (XLSX 13 kb)
Supplementary Table 12
Rare truncation variants and known hotspot variants detected in DNMT3A, TET2, ASXL1, GNAS, JAK2, SF3B1, IDH1 and IDH2 in 557 WHISP samples. (XLSX 10 kb)
Supplementary Table 13
Exome capture sequencing coverage for 11 TCGA cancer types analyzed. (XLSX 9 kb)
Rights and permissions
About this article
Cite this article
Xie, M., Lu, C., Wang, J. et al. Age-related mutations associated with clonal hematopoietic expansion and malignancies. Nat Med 20, 1472–1478 (2014). https://doi.org/10.1038/nm.3733
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nm.3733
This article is cited by
-
Dynamics of clonal hematopoiesis under DNA-damaging treatment in patients with ovarian cancer
Leukemia (2024)
-
Driver mutation zygosity is a critical factor in predicting clonal hematopoiesis transformation risk
Blood Cancer Journal (2024)
-
Extended genetic analysis and tumor characteristics in over 4600 women with suspected hereditary breast and ovarian cancer
BMC Cancer (2023)
-
Multiparameter prediction of myeloid neoplasia risk
Nature Genetics (2023)
-
Potential utility of risk stratification for multicancer screening with liquid biopsy tests
npj Precision Oncology (2023)