Abstract
T cells must be tolerant of self antigens to avoid autoimmunity but responsive to foreign antigens to provide protection against infection. We found that in both naive T cells and effector T cells, the tyrosine phosphatase PTPN22 limited signaling via the T cell antigen receptor (TCR) by weak agonists and self antigens while not impeding responses to strong agonist antigens. T cells lacking PTPN22 showed enhanced formation of conjugates with antigen-presenting cells pulsed with weak peptides, which led to activation of the T cells and their production of inflammatory cytokines. This effect was exacerbated under conditions of lymphopenia, with the formation of potent memory T cells in the absence of PTPN22. Our data address how loss-of-function PTPN22 alleles can lead to the population expansion of effector and/or memory T cells and a predisposition to human autoimmunity.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout







Similar content being viewed by others
References
Polic, B., Kunkel, D., Scheffold, A. & Rajewsky, K. How αβ T cells deal with induced TCRα ablation. Proc. Natl. Acad. Sci. USA 98, 8744–8749 (2001).
Goldrath, A.W. & Bevan, M.J. Low-affinity ligands for the TCR drive proliferation of mature CD8+ T cells in lymphopenic hosts. Immunity 11, 183–190 (1999).
Kieper, W.C. & Jameson, S.C. Homeostatic expansion and phenotypic conversion of naive T cells in response to self peptide/MHC ligands. Proc. Natl. Acad. Sci. USA 96, 13306–13311 (1999).
Sprent, J. & Surh, C.D. Normal T cell homeostasis: the conversion of naive cells into memory-phenotype cells. Nat. Immunol. 12, 478–484 (2011).
Le Campion, A. et al. Lymphopenia-induced spontaneous T-cell proliferation as a cofactor for autoimmune disease development. Blood 114, 1784–1793 (2009).
Jones, J.L. et al. Human autoimmunity after lymphocyte depletion is caused by homeostatic T-cell proliferation. Proc. Natl. Acad. Sci. USA 110, 20200–20205 (2013).
King, C., Ilic, A., Koelsch, K. & Sarvetnick, N. Homeostatic expansion of T cells during immune insufficiency generates autoimmunity. Cell 117, 265–277 (2004).
Rhee, I. & Veillette, A. Protein tyrosine phosphatases in lymphocyte activation and autoimmunity. Nat. Immunol. 13, 439–447 (2012).
O'Shea, J.J., McVicar, D.W., Bailey, T.L., Burns, C. & Smyth, M.J. Activation of human peripheral blood T lymphocytes by pharmacological induction of protein-tyrosine phosphorylation. Proc. Natl. Acad. Sci. USA 89, 10306–10310 (1992).
Bottini, N. & Peterson, E.J. Tyrosine phosphatase PTPN22: multifunctional regulator of immune signaling, development, and disease. Annu. Rev. Immunol. 32, 83–119 (2014).
Brownlie, R.J. et al. Lack of the phosphatase PTPN22 increases adhesion of murine regulatory T cells to improve their immunosuppressive function. Sci. Signal. 5, ra87 (2012).
Hasegawa, K. et al. PEST domain-enriched tyrosine phosphatase (PEP) regulation of effector/memory T cells. Science 303, 685–689 (2004).
Dai, X. et al. A disease-associated PTPN22 variant promotes systemic autoimmunity in murine models. J. Clin. Invest. 123, 2024–2036 (2013).
Zhang, J. et al. The autoimmune disease-associated PTPN22 variant promotes calpain-mediated Lyp/Pep degradation associated with lymphocyte and dendritic cell hyperresponsiveness. Nat. Genet. 43, 902–907 (2011).
Wu, D.J. et al. Autoimmunity-associated LYP-W620 does not impair thymic negative selection of autoreactive T Cells. PLoS ONE 9, e86677 (2014).
Surh, C.D. & Sprent, J. Regulation of mature T cell homeostasis. Semin. Immunol. 17, 183–191 (2005).
Zhang, D.J. et al. Selective expression of the Cre recombinase in late-stage thymocytes using the distal promoter of the Lck gene. J. Immunol. 174, 6725–6731 (2005).
Kieper, W.C. et al. Recent immune status determines the source of antigens that drive homeostatic T cell expansion. J. Immunol. 174, 3158–3163 (2005).
Hogquist, K.A. et al. T cell receptor antagonist peptides induce positive selection. Cell 76, 17–27 (1994).
Yachi, P.P., Ampudia, J., Zal, T. & Gascoigne, N.R. Altered peptide ligands induce delayed CD8-T cell receptor interaction–a role for CD8 in distinguishing antigen quality. Immunity 25, 203–211 (2006).
Daniels, M.A. et al. Thymic selection threshold defined by compartmentalization of Ras/MAPK signalling. Nature 444, 724–729 (2006).
Enouz, S., Carrie, L., Merkler, D., Bevan, M.J. & Zehn, D. Autoreactive T cells bypass negative selection and respond to self-antigen stimulation during infection. J. Exp. Med. 209, 1769–1779 (2012).
D'Ambrosio, D., Cantrell, D.A., Frati, L., Santoni, A. & Testi, R. Involvement of p21ras activation in T cell CD69 expression. Eur. J. Immunol. 24, 616–620 (1994).
Kaech, S.M. & Cui, W. Transcriptional control of effector and memory CD8+ T cell differentiation. Nat. Rev. Immunol. 12, 749–761 (2012).
Sullivan, B.M., Juedes, A., Szabo, S.J., von Herrath, M. & Glimcher, L.H. Antigen-driven effector CD8 T cell function regulated by T-bet. Proc. Natl. Acad. Sci. USA 100, 15818–15823 (2003).
Wang, R. et al. The transcription factor Myc controls metabolic reprogramming upon T lymphocyte activation. Immunity 35, 871–882 (2011).
Intlekofer, A.M. et al. Effector and memory CD8+ T cell fate coupled by T-bet and eomesodermin. Nat. Immunol. 6, 1236–1244 (2005).
Man, K. et al. The transcription factor IRF4 is essential for TCR affinity-mediated metabolic programming and clonal expansion of T cells. Nat. Immunol. 14, 1155–1165 (2013).
Raczkowski, F. et al. The transcription factor interferon regulatory factor 4 is required for the generation of protective effector CD8+ T cells. Proc. Natl. Acad. Sci. USA 110, 15019–15024 (2013).
Yao, S. et al. Interferon regulatory factor 4 sustains CD8+ T cell expansion and effector differentiation. Immunity 39, 833–845 (2013).
Pearce, E.L. & Shen, H. Generation of CD8 T-cell memory is regulated by IL-12. J. Immunol. 179, 2074–2081 (2007).
Santori, F.R. et al. Rare, structurally homologous self-peptides promote thymocyte positive selection. Immunity 17, 131–142 (2002).
Wu, J. et al. Identification of substrates of human protein-tyrosine phosphatase PTPN22. J. Biol. Chem. 281, 11002–11010 (2006).
Sebzda, E., Bracke, M., Tugal, T., Hogg, N. & Cantrell, D.A. Rap1A positively regulates T cells via integrin activation rather than inhibiting lymphocyte signaling. Nat. Immunol. 3, 251–258 (2002).
Cohen, J.A. et al. Alemtuzumab versus interferon β1a as first-line treatment for patients with relapsing-remitting multiple sclerosis: a randomised controlled phase 3 trial. Lancet 380, 1819–1828 (2012).
Coles, A.J. et al. Alemtuzumab for patients with relapsing multiple sclerosis after disease-modifying therapy: a randomised controlled phase 3 trial. Lancet 380, 1829–1839 (2012).
Zhernakova, A., van Diemen, C.C. & Wijmenga, C. Detecting shared pathogenesis from the shared genetics of immune-related diseases. Nat. Rev. Genet. 10, 43–55 (2009).
Wiede, F., La Gruta, N.L. & Tiganis, T. PTPN2 attenuates T-cell lymphopenia-induced proliferation. Nat. Commun. 5, 3073 (2014).
Wiede, F. et al. T cell protein tyrosine phosphatase attenuates T cell signaling to maintain tolerance in mice. J. Clin. Invest. 121, 4758–4774 (2011).
Shields, B.J. et al. TCPTP regulates SFK and STAT3 signaling and is lost in triple-negative breast cancers. Mol. Cell. Biol. 33, 557–570 (2013).
Zikherman, J. & Weiss, A. Unraveling the functional implications of GWAS: how T cell protein tyrosine phosphatase drives autoimmune disease. J. Clin. Invest. 121, 4618–4621 (2011).
Grebe, K.M. & Potter, T.A. Enumeration, phenotyping, and identification of activation events in conjugates between T cells and antigen-presenting cells by flow cytometry. Sci. STKE 2002, pl14 (2002).
Matthews, S.A. et al. Protein kinase D isoforms are dispensable for integrin-mediated lymphocyte adhesion and homing to lymphoid tissues. Eur. J. Immunol. 42, 1316–1326 (2012).
Acknowledgements
We thank H. Shen (University of Pennsylvania) for the attenuated OVA-expressing L. monocytogenes strain with deletion of the actin assembly–inducing protein; D. Wright and C. Garcia for technical assistance, and P. Travers for reading the manuscript. Supported by the Wellcome Trust (096669 to R.Z., and 095831 for the Centre for Immunity, Infection and Evolution of the University of Edinburgh) and the Biotechnology and Biological Sciences Research Council (801148 to V.L.M.).
Author information
Authors and Affiliations
Contributions
R.J.S. designed and did most in vitro experiments; R.J.B. designed and did most in vivo experiments and in vitro analyses of the formation of T cell conjugates; V.L.M. designed and did analyses of adhesion under shear flow; R.Z. designed experiments and led the overall project; and R.J.S. and R.Z. wrote the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Integrated supplementary information
Supplementary Figure 1 Basal phenotype of OT-I thymus and lymph node T cells.
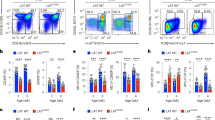
(a) Total cell numbers in wildtype (WT) and Ptpn22-/- (KO) thymi. (b) FACS dotplots showing distribution of thymocyte populations in 7 wk old WT and Ptpn22-/- OT-1 Rag1-/- mice. (c) Proportions of gated CD4+CD8+ double-positive (DP), and CD4+ and CD8+ single-positive (SP) thymocytes. (d) Absolute cell numbers of gated DP and SP thymocytes. (e) FACS histograms showing levels of expression of surface markers by gated CD8+ LN OT-1 T cells, as indicated. Data are representative of 8 mice of each genotype. In graphs, lines represent means and dots values from individual mice. NS - not significant, * p<0.001 by Student’s t-test.
Supplementary Figure 2 PTPN22 regulates early activation of T cells.
Wildtype (WT) and Ptpn22-/- (KO) OT-1 T cells were left unstimulated (US) or stimulated (stim) for 24h with 1 μM peptide (as indicated) and stained for cell surface and intracellular markers. Histograms showing the mean fluorescence intensities following intracellular staining for T-bet (a), c-Myc (b), eomesodermin (Eomes) (c) and IRF4 (d). (e) Cell size was assessed by analysis of forward scatter area (FSC-A) and levels of NB-d-glucose uptake (f) and surface expression of CD71 (g) and CD98 (h) measured. Data are representative of triplicate samples within 1 of at least 4 repeated experiments.
Supplementary Figure 3 Flow cytometry of CTLs generated in vitro.
(a) Comparable expansion of day 2 N4-stimulated wildtype (WT) and Ptpn22-/- OT-1 T cells in IL-2. Values represent means (n=3 replicate samples) and error bars SD. (b) Histograms show cell size (FSC-A) and expression of cell surface receptors, as indicated, by d6 IL-2-generated WT and Ptpn22-/- CTLs. (c) Intracellular expression of transcription factors and effector proteins by d6 IL-2-generated WT and Ptpn22-/- CTLs.
Supplementary Figure 4 Elevated inflammatory cytokine production by Ptpn22–/– (KO) CTLs.
(a) Histograms show levels of intracellular TNF and GM-CSF expressed by d6 WT and Ptpn22-/- CTLs following 4 h cultures unstimulated (US) or re-stimulation with 1 μM G4 peptide (stim). Data are representative of >3 repeated experiments. (b) Levels of MIP1α protein in culture supernatants following 24 h of G4 restimulation of d6 WT and Ptpn22-/- CTLs. Values represent means ± SD (n=3) from 1 of 2 repeated experiments.
Supplementary information
Supplementary Text and Figures
Supplementary Figures 1–4 (PDF 1178 kb)
Rights and permissions
About this article
Cite this article
Salmond, R., Brownlie, R., Morrison, V. et al. The tyrosine phosphatase PTPN22 discriminates weak self peptides from strong agonist TCR signals. Nat Immunol 15, 875–883 (2014). https://doi.org/10.1038/ni.2958
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ni.2958
This article is cited by
-
Insights from a 30-year journey: function, regulation and therapeutic modulation of PD1
Nature Reviews Immunology (2023)
-
Robust and tunable signal processing in mammalian cells via engineered covalent modification cycles
Nature Communications (2022)
-
Regulation of activated T cell survival in rheumatic autoimmune diseases
Nature Reviews Rheumatology (2022)
-
Autoimmunity and organ damage in systemic lupus erythematosus
Nature Immunology (2020)
-
Activation of naïve CD4+ T cells re-tunes STAT1 signaling to deliver unique cytokine responses in memory CD4+ T cells
Nature Immunology (2019)