Abstract
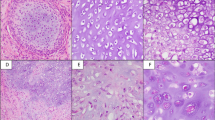
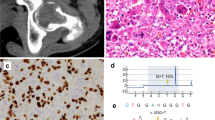
Ollier disease and Maffucci syndrome are non-hereditary skeletal disorders characterized by multiple enchondromas (Ollier disease) combined with spindle cell hemangiomas (Maffucci syndrome). We report somatic heterozygous mutations in IDH1 (c.394C>T encoding an R132C substitution and c.395G>A encoding an R132H substitution) or IDH2 (c.516G>C encoding R172S) in 87% of enchondromas (benign cartilage tumors) and in 70% of spindle cell hemangiomas (benign vascular lesions). In total, 35 of 43 (81%) subjects with Ollier disease and 10 of 13 (77%) with Maffucci syndrome carried IDH1 (98%) or IDH2 (2%) mutations in their tumors. Fourteen of 16 subjects had identical mutations in separate lesions. Immunohistochemistry to detect mutant IDH1 R132H protein suggested intraneoplastic and somatic mosaicism. IDH1 mutations in cartilage tumors were associated with hypermethylation and downregulated expression of several genes. Mutations were also found in 40% of solitary central cartilaginous tumors and in four chondrosarcoma cell lines, which will enable functional studies to assess the role of IDH1 and IDH2 mutations in tumor formation.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
Accession codes
References
Spranger, J., Kemperdieck, H., Bakowski, H. & Opitz, J.M. Two peculiar types of enchondromatosis. Pediatr. Radiol. 7, 215–219 (1978).
Lucas, D.R. & Bridge, J.A. Chondromas: enchondroma, periosteal chondroma, and enchondromatosis. In World Health Organization Classification of Tumours. Pathology and Genetics of Tumours of Soft Tissue and Bone (eds. Fletcher, C.D.M., Unni, K.K. & Mertens, F.) 237–240 (IARC Press, Lyon, France, 2002).
Pansuriya, T.C., Kroon, H.M. & Bovee, J.V.M.G. Enchondromatosis: insights on the different subtypes. Int. J. Clin. Exp. Pathol. 3, 557–569 (2010).
Verdegaal, S.H.M. et al. Incidence, predictive factors and prognosis of chondrosarcoma in patients with Ollier disease and Maffucci syndrome: an international multicenter study of 161 patients. Oncologist (in the press).
Hopyan, S. et al. A mutant PTH/PTHrP type I receptor in enchondromatosis. Nat. Genet. 30, 306–310 (2002).
Rozeman, L.B. et al. Enchondromatosis (Ollier disease, Maffucci syndrome) is not caused by the PTHR1 mutation p.R150C. Hum. Mutat. 24, 466–473 (2004).
Couvineau, A. et al. PTHR1 mutations associated with Ollier disease result in receptor loss of function. Hum. Mol. Genet. 17, 2766–2775 (2008).
Pansuriya, T.C. et al. Genome-wide analysis of Ollier disease: is it all in the genes? Orphanet J. Rare Dis. 6, 2 (2011).
Pansuriya, T.C. et al. Maffucci syndrome: a genome-wide analysis using high resolution single nucleotide polymorphism and expression arrays on four cases. Genes Chromosom. Cancer 50, 673–679 (2011).
Ranger, A. & Szymczak, A. Do intracranial neoplasms differ in Ollier disease and Maffucci syndrome? An in-depth analysis of the literature. Neurosurgery 65, 1106–1113 (2009).
Schwartz, H.S. et al. The malignant potential of enchondromatosis. J. Bone Joint Surg. Am. 69, 269–274 (1987).
Rietveld, L. et al. First case of juvenile granulosa cell tumor in an adult with Ollier disease. Int. J. Gynecol. Pathol. 28, 464–467 (2009).
Leyva-Carmona, M., Vazquez-Lopez, M.A. & Lendinez-Molinos, F. Ovarian juvenile granulosa cell tumors in infants. J. Pediatr. Hematol. Oncol. 31, 304–306 (2009).
Yan, H. et al. IDH1 and IDH2 mutations in gliomas. N. Engl. J. Med. 360, 765–773 (2009).
Hartmann, C. et al. Type and frequency of IDH1 and IDH2 mutations are related to astrocytic and oligodendroglial differentiation and age: a study of 1,010 diffuse gliomas. Acta Neuropathol. 118, 469–474 (2009).
Dang, L., Jin, S. & Su, S.M. IDH mutations in glioma and acute myeloid leukemia. Trends Mol. Med. 16, 387–397 (2010).
Kalfa, N. et al. Activating mutations of the stimulatory G protein in juvenile ovarian granulosa cell tumors: a new prognostic factor? J. Clin. Endocrinol. Metab. 91, 1842–1847 (2006).
Amary, M.F. et al. IDH1 and IDH2 mutations are frequent events in central chondrosarcoma and central and periosteal chondromas but not in other mesenchymal tumours. J. Pathol. 224, 334–343 (2011).
van Krieken, J.H. et al. KRAS mutation testing for predicting response to anti-EGFR therapy for colorectal carcinoma: proposal for an European quality assurance program. Virchows Arch. 453, 417–431 (2008).
Wolff, J.N. & Gemmell, N.J. Combining allele-specific fluorescent probes and restriction assay in real-time PCR to achieve SNP scoring beyond allele ratios of 1:1000. Biotechniques 44, 193–194, 196, 199 (2008).
Sobreira, N.L. et al. Whole-genome sequencing of a single proband together with linkage analysis identifies a Mendelian disease gene. PLoS Genet. 6, e1000991 (2010).
Bowen, M.E. et al. Loss-of-function mutations in PTPN11 cause metachondromatosis, but not Ollier disease or Maffucci syndrome. PLoS Genet. 7, e1002050 (2011).
Lausch, E. et al. Genetic deficiency of tartrate-resistant acid phosphatase associated with skeletal dysplasia, cerebral calcifications and autoimmunity. Nat. Genet. 43, 132–137 (2011).
Briggs, T.A. et al. Tartrate-resistant acid phosphatase deficiency causes a bone dysplasia with autoimmunity and a type I interferon expression signature. Nat. Genet. 43, 127–131 (2011).
Collinson, M. et al. Symmetrical enchondromatosis is associated with duplication of 12p11.23 to 12p11.22 including PTHLH. Am. J. Med. Genet. A. 152A, 3124–3128 (2010).
Bianco, P. et al. Reproduction of human fibrous dysplasia of bone in immunocompromised mice by transplanted mosaics of normal and Gsalpha-mutated skeletal progenitor cells. J. Clin. Invest. 101, 1737–1744 (1998).
Jones, K.B. et al. A mouse model of osteochondromagenesis from clonal inactivation of Ext1 in chondrocytes. Proc. Natl. Acad. Sci. USA 107, 2054–2059 (2010).
de Andrea, C.E., Prins, F.A., Wiweger, M.I. & Hogendoorn, P.C.W. Growth plate regulation and osteochondroma formation: insights from tracing proteoglycans in zebrafish models and human cartilage. J. Pathol. 224, 160–168 (2011).
de Andrea, C.E. et al. Secondary peripheral chondrosarcoma evolving from osteochondroma as a result of the outgrowth of cells with functional EXT. Oncogene published online, doi:10.1038/onc.2011.311 (1 August 2011).
Reijnders, C.M. et al. No haploinsufficiency but loss of heterozygosity for EXT in multiple osteochondromas. Am. J. Pathol. 177, 1946–1957 (2010).
Bovée, J.V.M.G. EXTra hit for mouse osteochondroma. Proc. Natl. Acad. Sci. USA 107, 1813–1814 (2010).
Clément, A. et al. Regulation of zebrafish skeletogenesis by ext2/dackel and papst1/pinscher. PLoS Genet. 4, e1000136 (2008).
Cohen, M.M. Jr. Fibrous dysplasia is a neoplasm. Am. J. Med. Genet. 98, 290–293 (2001).
Lietman, S.A., Ding, C. & Levine, M.A. A highly sensitive polymerase chain reaction method detects activating mutations of the GNAS gene in peripheral blood cells in McCune-Albright syndrome or isolated fibrous dysplasia. J. Bone Joint Surg. Am. 87, 2489–2494 (2005).
Ikota, H., Nobusawa, S., Tanaka, Y., Yokoo, H. & Nakazato, Y. High-throughput immunohistochemical profiling of primary brain tumors and non-neoplastic systemic organs with a specific antibody against the mutant isocitrate dehydrogenase 1 R132H protein. Brain Tumor Pathol. 28, 107–114 (2011).
Figueroa, M.E. et al. Leukemic IDH1 and IDH2 mutations result in a hypermethylation phenotype, disrupt TET2 function, and impair hematopoietic differentiation. Cancer Cell 18, 553–567 (2010).
Thomas, D.M. Lessons from the deep study of rare tumours. J. Pathol. 224, 306–308 (2011).
Parsons, D.W. et al. An integrated genomic analysis of human glioblastoma multiforme. Science 321, 1807–1812 (2008).
Mardis, E.R. et al. Recurring mutations found by sequencing an acute myeloid leukemia genome. N. Engl. J. Med. 361, 1058–1066 (2009).
Yen, K.E., Bittinger, M.A., Su, S.M. & Fantin, V.R. Cancer-associated IDH mutations: biomarker and therapeutic opportunities. Oncogene 29, 6409–6417 (2010).
Kang, M.R. et al. Mutational analysis of IDH1 codon 132 in glioblastomas and other common cancers. Int. J. Cancer 125, 353–355 (2009).
Gaal, J. et al. Isocitrate dehydrogenase mutations are rare in pheochromocytomas and paragangliomas. J. Clin. Endocrinol. Metab. 95, 1274–1278 (2010).
Hemerly, J.P., Bastos, A.U. & Cerutti, J.M. Identification of several novel non-p.R132 IDH1 variants in thyroid carcinomas. Eur. J. Endocrinol. 163, 747–755 (2010).
Dang, L. et al. Cancer-associated IDH1 mutations produce 2-hydroxyglutarate. Nature 462, 739–744 (2009).
Noushmehr, H. et al. Identification of a CpG island methylator phenotype that defines a distinct subgroup of glioma. Cancer Cell 17, 510–522 (2010).
Toyota, M. et al. CpG island methylator phenotype in colorectal cancer. Proc. Natl. Acad. Sci. USA 96, 8681–8686 (1999).
Chin, H.J. et al. Studies on the role of Dlx5 in regulation of chondrocyte differentiation during endochondral ossification in the developing mouse limb. Dev. Growth Differ. 49, 515–521 (2007).
Zhu, H. & Bendall, A.J. Dlx5 is a cell autonomous regulator of chondrocyte hypertrophy in mice and functionally substitutes for Dlx6 during endochondral ossification. PLoS ONE 4, e8097 (2009).
Lee, M.H., Kwon, T.G., Park, H.S., Wozney, J.M. & Ryoo, H.M. BMP-2-induced Osterix expression is mediated by Dlx5 but is independent of Runx2. Biochem. Biophys. Res. Commun. 309, 689–694 (2003).
Ulsamer, A. et al. BMP-2 induces Osterix expression through up-regulation of Dlx5 and its phosphorylation by p38. J. Biol. Chem. 283, 3816–3826 (2008).
Scully, S.P. et al. Marshall Urist Award. Interstitial collagenase gene expression correlates with in vitro invasion in human chondrosarcoma. Clin. Orthop. Relat. Res. 291–303 (2000).
Gil-Benso, R. et al. Establishment and characterization of a continuous human chondrosarcoma cell line, ch-2879: comparative histologic and genetic studies with its tumor of origin. Lab. Invest. 83, 877–887 (2003).
Kunisada, T. et al. A new human chondrosarcoma cell line (OUMS-27) that maintains chondrocytic differentiation. Int. J. Cancer 77, 854–859 (1998).
Kalinski, T. et al. Establishment and characterization of the permanent human cell line C3842 derived from a secondary chondrosarcoma in Ollier's disease. Virchows Arch. 446, 287–299 (2005).
Kudo, N. et al. Establishment of novel human dedifferentiated chondrosarcoma cell line with osteoblastic differentiation. Virchows Arch. 451, 691–699 (2007).
Evans, H.L., Ayala, A.G. & Romsdahl, M.M. Prognostic factors in chondrosarcoma of bone. A clinicopathologic analysis with emphasis on histologic grading. Cancer 40, 818–831 (1977).
van Eijk, R. et al. Rapid KRAS, EGFR, BRAF and PIK3CA mutation analysis of fine needle aspirates from non-small-cell lung cancer using allele-specific qPCR. PLoS ONE 6, e17791 (2011).
Szuhai, K. et al. Tiling resolution array-CGH shows that somatic mosaic deletion of the EXT gene is causative in EXT gene mutation negative multiple osteochondromas patients. Hum. Mutat. 32, E2036–E2049 (2011).
Verbeke, S.L. et al. Distinct histological features characterize primary angiosarcoma of bone. Histopathology 58, 254–264 (2011).
Meijer, D. et al. Expression of aromatase and estrogen receptor alpha in chondrosarcoma, but no beneficial effect of inhibiting estrogen signaling both in vitro and. in vivo. Clin. Sarcoma Res. 1, 5 (2011).
Rozeman, L.B. et al. Dedifferentiated peripheral chondrosarcomas: regulation of EXT-downstream molecules and differentiation-related genes. Mod. Pathol. 22, 1489–1498 (2009).
Hallor, K.H. et al. Genomic profiling of chondrosarcoma: chromosomal patterns in central and peripheral tumors. Clin. Cancer Res. 15, 2685–2694 (2009).
Buddingh, E.P. et al. Tumor-infiltrating macrophages are associated with metastasis suppression in high-grade osteosarcoma: a rationale for treatment with macrophage-activating agents. Clin. Cancer Res. 17, 2110–2119 (2011).
Smyth, G.K. Linear models and empirical bayes methods for assessing differential expression in microarray experiments. Stat. Appl. Genet. Mol. Biol. 3, Article3 (2004).
Acknowledgements
We are grateful to all of the participants and their families for taking part in this study. We would like to thank S. Romeo and C.M.A. Reijnders for providing DNA from cartilage tumors. We are grateful to A.B. Mohseny for help with statistics, to D. van der Geest and T. Krenács for constructing TMAs and to P. Wijers-Koster, D. de Jong, B. van den Akker, R. Duim, M. Winter, I.H. Briaire-de Bruijn and M.E. Bowen for expert technical assistance. C.J.F. Waaijer, P.C.W. Hogendoorn and C.E. de Andrea are acknowledged for fruitful discussion. We would like to acknowledge F. Bertoni, E.L. Staals and P. Bacchini for kindly providing peripheral dedifferentiated chondrosarcomas and vascular tumors, T. Kalinski for the C3842 cell line, M. Namba for the OUMS27 cell line, T. Ariizumi for the NDCS1 cell line and A. Llombart Bosch for the CH2879 cell line. J. Mulliken, J. Upton and S. Fishman kindly provided spindle cell hemangiomas. S.H.M. Verdegaal, A.H.M. Taminiau and M.A.J. van de Sande are acknowledged for contributing patient data. We are thankful to S. Boeuf, R. Forsyth and P.P. Mainil-Varlet for providing single Ollier disease cases and to W. Wutys for providing a single metachondromatosis case. The continuous support of the Netherlands Committee on Bone Tumors is highly acknowledged. The study was funded by The Netherlands Organization for Scientific Research (917-76-315 to J.V.M.G.B. and T.C.P.), the Liddy Shriver Sarcoma Initiative (to J.V.M.G.B. and J.O.), the Interuniversity Attraction Poles initiated by the Belgian Federal Science Policy, network 6/05, the US National Institutes of Health (AR048564) and the FNRS–Fonds de la Recherche Scientifique (all to M.V.) and the Manton Center for Orphan Disease Research at Children's Hospital Boston (94824-01 to K.K.). The study was performed within the EuroBoNeT, a European Commission-granted Network of Excellence for studying the pathology and genetics of bone tumors (018814).
Author information
Authors and Affiliations
Contributions
The study was designed, written and reviewed by T.C.P. and J.V.M.G.B. Mutation analysis was designed and performed by T.C.P., M.A.J.H.v.R., J.V.M.G.B., K.S., T.v.W. and R.v.E. Immunohistochemistry was conducted and evaluated by T.C.P., M.A.J.H.v.R. and J.V.M.G.B. T.C.P., S.L.J.V., J.G.v.O. and D.M. contributed tissue microarrays. Expression profiling was designed and performed by A.-M.C.-J., T.C.P., J.V.M.G.B. and J.O. and analyzed by J.O. and M.L.K. Methylation profiling was designed by A.-M.C.-J., J.V.M.G.B. and L.S., performed by P.d.A., and the results analyzed by P.d.A. and P.J.F. K.H.N., S.D., L.S., B.T., B.L.-A., M.S.-J., R.S., N.L., L.-G.K., C.G., M.V., L.M.B. and K.C.K. each contributed frozen or paraffin-embedded tissues for multiple subjects with Ollier disease or Maffucci syndrome and acquired data for these individuals. The manuscript was approved by all authors.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Supplementary Text and Figures
Supplementary Figures 1 and 2 and Supplementary Tables 1, 2 and 4–6 (PDF 21614 kb)
Supplementary Table 3
Differentially methylated sites in enchondromas with and without IDH1 mutation at Sanger sequencing (XLS 391 kb)
Rights and permissions
About this article
Cite this article
Pansuriya, T., van Eijk, R., d'Adamo, P. et al. Somatic mosaic IDH1 and IDH2 mutations are associated with enchondroma and spindle cell hemangioma in Ollier disease and Maffucci syndrome. Nat Genet 43, 1256–1261 (2011). https://doi.org/10.1038/ng.1004
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ng.1004
This article is cited by
-
A single-cell atlas of conventional central chondrosarcoma reveals the role of endoplasmic reticulum stress in malignant transformation
Communications Biology (2024)
-
Prevalence and characteristics of benign cartilaginous tumours of the shoulder joint. An MRI-based study
Skeletal Radiology (2024)
-
IDH mutations in G2-3 conventional central bone chondrosarcoma: a mono institutional experience
BMC Cancer (2023)
-
Quantitative multiple fragment monitoring with enhanced in-source fragmentation/annotation mass spectrometry
Nature Protocols (2023)
-
GANT-61 induces cell cycle resting and autophagy by down-regulating RNAP III signal pathway and tRNA-Gly-CCC synthesis to combate chondrosarcoma
Cell Death & Disease (2023)