Abstract
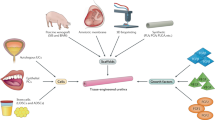
Patients suffering from diseased or injured organs may be treated with transplanted organs. Engineered tissue has a variety of potential applications throughout urology, from reconstruction of the urethra or bladder following trauma or surgery, to growing reproductive organs for individuals with congenital malformations. In this review, Anthony Atala discusses the different techniques and materials employed in tissue regeneration and tissue engineering, and their urologic applications.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Chen F et al. (1999) Acellular collagen matrix as a possible “off the shelf” biomaterial for urethral repair. Urology 54: 407–410
Dahms SE et al. (1998) Composition and biomechanical properties of the bladder acellular matrix graft: comparative analysis in rat, pig and human. Br J Urol 82: 411–419
Piechota HJ et al. (1998) In vitro functional properties of the rat bladder regenerated by the bladder acellular matrix graft. J Urol 159: 1717–1724
Yoo JJ et al. (1998) Bladder augmentation using allogenic bladder submucosa seeded with cells. Urology 51: 221–225
Kim B and Mooney DJ (1998) Development of biocompatible synthetic extracellular matrices for tissue engineering. Trends Biotechnol 16: 224–230
Bergsma JE et al. (1995) In vivo degradation and biocompatibility study of in vitro pre-degraded as-polymerized polyactide particles. Biomaterials 16: 267–274
Hynes RO (1992) Integrins: versatility, modulation, and signaling in cell adhesion. Cell 69: 11–25
Deuel TF (1997) Growth factors. In: Principles of Tissue Engineering 133–149 (Eds Lanzer RP et al.) New York: Academic Press
Pariente JL et al. (2001) In vitro biocompatibility assessment of naturally derived and synthetic biomaterials using normal human urothelial cells. J Biomed Mater Res 55: 33–39
Pariente JL et al. (2002) In vitro biocompatibility evaluation of naturally derived and synthetic biomaterials using normal human bladder smooth muscle cells. J Urol 167: 1867–1871
Li ST (1995) Biologic biomaterials: tissue-derived biomaterials (collagen). In: The Biomedical Engineering Handbook, 627–647 Vol 1(Ed Bronzino JD) Boca Raton, FL: CRC Press
Silver FH and Pins G (1992) Cell growth on collagen: a review of tissue engineering using scaffolds containing extracellular matrix. J Long Term Eff Med Implants 2: 67–80
Sams AE and Nixon AJ (1995) Chondrocyte-laden collagen scaffolds for resurfacing extensive articular cartilage defects. Osteoarthritis Cartilage 3: 47–59
Smidsrod O and Skjak-Braek G (1990) Alginate as immobilization matrix for cells. Trends Biotechnol 8: 71–80
Lim F and Sun AM (1980) Microencapsulated islets as bioartificial endocrine pancreas. Science 210: 908–910
Gilding DK (1981) Biodegradable polymers. In: Biocompatibility of Clinical Implant Materials, 209–232 (Ed Williams DF) Boca Raton, FL: CRC Press
Freed LE et al. (1994) Biodegradable polymer scaffolds for tissue engineering. Biotechnology (NY) 12: 689–693
Mikos AG et al. (1994) Preparation and characterization of poly(L-lactic acid) foams. Polymer 35: 1068–1077
Harris LD et al. (1998) Open pore biodegradable matrices formed with gas foaming. J Biomed Mater Res 42: 396–402
Peppas NA and Langer R (1994) New challenges in biomaterials. Science 263: 1715–1720
Bazeed MA et al. (1983) New treatment for urethral strictures. Urology 21: 53–57
Atala A et al. (1992) Formation of urothelial structures in vivo from dissociated cells attached to biodegradable polymer scaffolds in vitro. J Urol 148: 658–662
Olsen L et al. (1992) Urethral reconstruction with a new synthetic absorbable device. An experimental study. Scand J Urol Nephrol 26: 323–326
Kropp BP et al. (1998) Rabbit urethral regeneration using small intestinal submucosa onlay grafts. Urology 52: 138–142
Sievert KD et al. (2000) Homologous acellular matrix graft for urethral reconstruction in the rabbit: histological and functional evaluation. J Urol 163: 1958–1965
Yoo JJ et al. (1999) Autologous engineered cartilage rods for penile reconstruction. J Urol 162: 1119–1121
El-Kassaby AW et al. (2003) Urethral stricture repair with an off-the-shelf collagen matrix. J Urol 169: 170–173
De Filippo RE et al. (2002) Total penile urethral replacement with autologous cell-seeded collagen matrices [abstract]. J Urol 167 (Suppl): 152–153
De Filippo RE et al. (2002) Urethral replacement using cell seeded tubularized collagen matrices. J Urol 168: 1789–1793
Atala A et al. (1993) Implantation in vivo and retrieval of artificial structures consisting of rabbit and human urothelium and human bladder muscle. J Urol 150: 608–612
Oberpenning F et al. (1999) De novo reconstitution of a functional mammalian urinary bladder by tissue engineering. Nat Biotechnol 17: 149–155
Kershen RT et al. (2002) Reconstitution of human corpus cavernosum smooth muscle in vitro and in vivo. Tissue Eng 8: 515–524
Kwon TG et al. (2002) Autologous penile corpora cavernosa replacement using tissue engineering techniques. J Urol 168: 1754–1758
Wang T et al. (2003) Creation of an engineered uterus for surgical reconstruction [abstract 391]. In Proceedings of the American Academy of Pediatrics Annual Meeting: November 1–5; New Orleans, LA. Elk Grove Village, IL: American Academy of Pediatrics
De Filippo RE et al. (2003) Engineering of vaginal tissue in vivo. Tissue Eng 9: 301–306
De Filippo RE et al. (2003) Engineering of vaginal tissue for total reconstruction. J Urol 169 (Suppl): 1057
Lanza RP et al. (2002) Generation of histocompatible tissues using nuclear transplantation. Nat Biotechnol 20: 689–696
Evans MJ et al. (1999) Mitochondrial DNA genotypes in nuclear transfer-derived cloned sheep. Nat Genet 23: 90–93
Hiendleder S et al. (1999) Transmitochondrial differences and varying levels of heteroplasmy in nuclear transfer cloned cattle. Mol Reprod Dev 54: 24–31
Steinborn R et al. (2000) Mitochondrial DNA heteroplasmy in cloned cattle produced by fetal and adult cell cloning. Nat Genet 25: 255–257
Auchincloss H and Bonventre JV (2002) Transplanting cloned cells into therapeutic promise. Nat Biotechnol 20: 665–666
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The author declares no competing financial interests.
Glossary
- HYPOSPADIAS
-
Congenital defect in males where the urethral opening is on the underside of the penis or the perineum, rather than on the glans
- EPISPADIAS
-
Congenital defect more common in males, where the upper wall of the urethra is absent
- CAVERNOSOGRAPHY
-
An imaging technique whereby the corpus cavernosum is visualized by radiography
- CAVERNOSOMETRY
-
A way of measuring vascular pressure within the corpus cavernosum, it can be used with dynamic infusion to give a visual representation
- ENZYME-LINKED IMMUNOSPOT (ELISPOT) ASSAY
-
This is a technique for analyzing immunological functions in blood and lymphocytes
Rights and permissions
About this article
Cite this article
Atala, A. Technology Insight: applications of tissue engineering and biological substitutes in urology. Nat Rev Urol 2, 143–149 (2005). https://doi.org/10.1038/ncpuro0121
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1038/ncpuro0121
This article is cited by
-
Autologous urothelial cells transplantation onto a prefabricated capsular stent for tissue engineered ureteral reconstruction
Journal of Materials Science: Materials in Medicine (2012)