Abstract
The need for an effective noninvasive tool to ablate spinal lesions reflects the limitations of traditional surgical and radiotherapeutic approaches. Open surgery is invasive and carries a risk of neurological injury and vertebral column dysfunction. Conventional radiotherapy often has poor clinical efficacy and a risk of neurologic complications. Spinal radiosurgery has been developed to overcome these limitations. This technique consists of precise delivery of high-dose radiation to a spinal target. To spare the delicate and radiation-sensitive spinal cord and to avoid potentially devastating neurological complications, it is essential that the radiation dose decreases rapidly outside of the target. This is accomplished by use of advanced, image-guidance technology, treatment planning software, and robotics. Preliminary data indicate that this approach can achieve high rates of tumor control of spinal and paraspinal lesions and durable reduction of associated vertebral pain without neurological complications. Although spinal radiosurgery is not yet widely practiced, the benefits of this new therapeutic approach are likely to encourage its widespread adoption in coming years.
Key Points
-
The accurate, tightly focused delivery of radiation to spinal lesions is possible by frameless robotic radiosurgical technologies such as CyberKnife® and Novalis® Shaped Beam
-
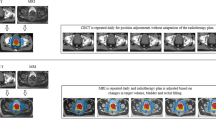
Image guidance is the key to spinal radiosurgery; X-ray images are registered to images derived from preoperative CTs, and the computations required to align the images provide the coordinates for lesion targeting
-
A range of pathologies have been treated with spinal radiosurgery, including metastatic lesions, primary malignant and benign lesions, and arteriovenous malformations
-
Spinal radiosurgery provides durable pain relief and local tumor control while maintaining physical and mental quality of life
-
Spinal radiosurgery is associated with a low rate of complications; no neurological complications were observed in the largest series to date (500 lesions)
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Fuentes S et al. (2006) Brainstem metastases: management using gamma knife radiosurgery. Neurosurgery 58: 37–42
Hadjipanayis CG et al. (2001) Stereotactic radiosurgery for motor cortex region arteriovenous malformations. Neurosurgery 48: 70–76
Hasegawa T et al. (2005) Stereotactic radiosurgery for vestibular schwannomas: analysis of 317 patients followed more than 5 years. Neurosurgery 57: 257–265
Heppner PA et al. (2005) Gamma knife surgery for low-grade gliomas. Neurosurgery 57: 1132–1139
Kobayashi T et al. (2005) Long-term results of gamma knife surgery for the treatment of craniopharyngioma in 98 consecutive cases. J Neurosurg 103: 482–488
Kondziolka D et al. (2002) Stereotactic radiosurgery for the treatment of trigeminal neuralgia. Clin J Pain 18: 42–47
Laws ER et al. (2004) Stereotactic radiosurgery for pituitary adenomas: a review of the literature. J Neurooncol 69: 257–272
Lunsford LD et al. (1991) Stereotactic radiosurgery for arteriovenous malformations of the brain. J Neurosurg 75: 512–524
Lunsford LD et al. (2005) Radiosurgery of vestibular schwannomas: summary of experience in 829 cases. J Neurosurg 102 (Suppl): S195–S199
McDermott MW et al. (2005) Radiosurgery in metastatic brain cancer. Neurosurgery 57 (Suppl): S45–S53
Pollock BE et al. (2005) Results of stereotactic radiosurgery for patients with imaging defined cavernous sinus meningiomas. Int J Radiat Oncol Biol Phys 62: 1427–1431
Regis J et al. (2004) Gamma knife surgery for epilepsy related to hypothalamic hamartomas. Acta Neurochir Suppl 91: 33–50
Regis J et al. (2004) Gamma knife surgery in mesial temporal lobe epilepsy: a prospective multicenter study. Epilepsia 45: 504–515
Sheehan JP et al. (2005) Stereotactic radiosurgery for pituitary adenomas: an intermediate review of its safety, efficacy, and role in the neurosurgical treatment armamentarium. J Neurosurg 102: 678–691
Yamamoto Y et al. (1995) Interim report on the radiosurgical treatment of cerebral arteriovenous malformations: the influence of size, dose, time, and technical factors on obliteration rate. J Neurosurg 83: 832–837
Ryu SI et al. (2001) Image-guided hypo-fractionated stereotactic radiosurgery to spinal lesions. Neurosurgery 49: 838–846
Bhatnagar AK et al. (2005) CyberKnife frameless radiosurgery for the treatment of extracranial benign tumors. Technol Cancer Res Treat 4: 571–576
Gerszten PC et al. (2005) Stereotactic radiosurgery for spinal metastases from renal cell carcinoma. J Neurosurg Spine 3: 288–295
Gerszten PC et al. (2006) Radiosurgery for the treatment of spinal melanoma metastases. Stereotact Funct Neurosurg 83: 213–221
Gerszten PC et al. (2005) Single-fraction radiosurgery for the treatment of spinal breast metastases. Cancer 104: 2244–2254
Gerszten PC et al. (2003) Evaluation of CyberKnife frameless real-time image-guided stereotactic radiosurgery for spinal lesions. Stereotact Funct Neurosurg 81: 84–89
Gerszten PC et al. (2003) CyberKnife frameless single-fraction stereotactic radiosurgery for benign tumors of the spine. Neurosurg Focus 14: e16
Gerszten PC et al. (2004) CyberKnife frameless stereotactic radiosurgery for spinal lesions: clinical experience in 125 cases. Neurosurgery 55: 89–98
Gerszten PC et al. (2003) CyberKnife frameless single-fraction stereotactic radiosurgery for tumors of the sacrum. Neurosurg Focus 15: e7
Gerszten PC et al. (2005) Combination kyphoplasty and spinal radiosurgery: a new treatment paradigm for pathological fractures. J Neurosurg Spine 3: 296–301
Benzil DL et al. (2004) Safety and efficacy of stereotactic radiosurgery for tumors of the spine. J Neurosurg 101 (Suppl 3): S413–S418
De Salles AA et al. (2004) Spinal lesions treated with Novalis shaped beam intensity-modulated radiosurgery and stereotactic radiotherapy. J Neurosurg 101 (Suppl 3): S435–S440
Rock JP et al. (2006) Postoperative radiosurgery for malignant spinal tumors. Neurosurgery 58: 891–898
Rock JP et al. (2004) Novalis radiosurgery for metastatic spine tumors. Neurosurg Clin N Am 15: 503–509
Ryu S et al. (2003) Image-guided and intensity-modulated radiosurgery for patients with spinal metastasis. Cancer 97: 2013–2018
Bilsky MH et al. (2004) Intensity-modulated stereotactic radiotherapy of paraspinal tumors: a preliminary report. Neurosurgery 54: 823–830
Hamilton AJ et al. (1995) Preliminary clinical experience with linear accelerator-based spinal stereotactic radiosurgery. Neurosurgery 36: 311–319
Yamada Y et al. (2005) Multifractionated image-guided and stereotactic intensity-modulated radiotherapy of paraspinal tumors: a preliminary report. Int J Radiat Oncol Biol Phys 62: 53–61
Yamada Y et al. (2006) Image-guided intensity-modulated radiation therapy of spine tumors. Curr Neurol Neurosci Rep 6: 207–211
Gerszten PC et al. (2007) Radiosurgery for spinal metastases: clinical experience in 500 cases from a single institution. Spine 32: 193–199
Leksell L (1951) The stereotaxic method and radiosurgery of the brain. Acta Chir Scand 102: 316–319
Colombo F et al. (1989) Linear accelerator radiosurgery of cerebral arteriovenous malformations. Neurosurgery 24: 833–840
Colombo F et al. (1994) Linear accelerator radiosurgery of cerebral arteriovenous malformations: an update. Neurosurgery 34: 14–20
Flickinger JC et al. (1996) A dose-response analysis of arteriovenous malformation obliteration after radiosurgery. Int J Radiat Oncol Biol Phys 36: 873–879
Friedman WA et al. (2003) Analysis of factors predictive of success or complications in arteriovenous malformation radiosurgery. Neurosurgery 52: 296–307
Ulfarsson E et al. (2002) Gamma knife radiosurgery for craniopharyngiomas: long-term results in the first Swedish patients. J Neurosurg 97: 613–622
Abramson N et al. (1976) Short-course radiation therapy in the treatment of head and neck tumors. Radiology 118: 175–178
Fitzgerald RH Jr et al. (1982) Chronic radiation myelitis. Radiology 144: 609–612
Madden FJ et al. (1979) Split course radiation in inoperable carcinoma of the bronchus. Eur J Cancer 15: 1175–1177
Guthrie RT et al. (1973) Comparative analysis of two regimens of split course radiation in carcinoma of the lung. Am J Roentgenol Radium Ther Nucl Med 117: 605–608
Schultheiss TE et al. (1995) Radiation response of the central nervous system. Int J Radiat Oncol Biol Phys 31: 1093–1112
Adler JR Jr et al. (1997) The Cyberknife: a frameless robotic system for radiosurgery. Stereotact Funct Neurosurg 69: 124–128
Adler JR et al. (1996) Preliminary clinical experience with the CyberKnife: image-guided stereotactic radiosurgery. In Radiosurgery 1995, 316–326 (Eds Alexander III E, et al.) Basel, Switzerland: Karger
Yu C et al. (2004) An anthropomorphic phantom study of the accuracy of Cyberknife spinal radiosurgery. Neurosurgery 55: 1138–1149
Ho AK et al. (2007) A study of the accuracy of Cyberknife spinal radiosurgery using skeletal structure tracking. Neurosurgery 60: 147–156
Muacevic A et al. (2006) Technical description, phantom accuracy, and clinical feasibility for fiducial-free frameless real-time image-guided spinal radiosurgery. J Neurosurg Spine 5: 303–312
Yan H et al. (2003) A phantom study on the positioning accuracy of the Novalis Body system. Med Phys 30: 3052–3060
Mahan SL et al. (2005) Evaluation of image-guided helical tomotherapy for the retreatment of spinal metastasis. Int J Radiat Oncol Biol Phys 63: 1576–1583
Yu C et al. (2003) Dosimetric comparison of CyberKnife with other radiosurgical modalities for an ellipsoidal target. Neurosurgery 53: 1155–1162
Murphy MJ et al. (2000) Image-guided radiosurgery for the spine and pancreas. Comput Aided Surg 5: 278–288
Shiu AS et al. (2003) Near simultaneous computed tomography image-guided stereotactic spinal radiotherapy: an emerging paradigm for achieving true stereotaxy. Int J Radiat Oncol Biol Phys 57: 605–613
Yenice KM et al. (2003) CT image-guided intensity-modulated therapy for paraspinal tumors using stereotactic immobilization. Int J Radiat Oncol Biol Phys 55: 583–593
Sinclair J et al. (2006) Multisession CyberKnife radiosurgery for intramedullary spinal cord arteriovenous malformations. Neurosurgery 58: 1081–1089
Friedman WA et al. (1996) The risk of hemorrhage after radiosurgery for arteriovenous malformations. J Neurosurg 84: 912–919
Maruyama K et al. (2005) The risk of hemorrhage after radiosurgery for cerebral arteriovenous malformations. N Engl J Med 352: 146–153
Maruyama K et al. (2004) Stereotactic radiosurgery for brainstem arteriovenous malformations: factors affecting outcome. J Neurosurg 100: 407–413
Dodd RL et al. (2006) CyberKnife radiosurgery for benign intradural extramedullary spinal tumors. Neurosurgery 58: 674–685
Jacobs WB et al. (2001) Evaluation and treatment of spinal metastases: an overview. Neurosurg Focus 11: e10
Helweg-Larsen S (1996) Clinical outcome in metastatic spinal cord compression: a prospective study of 153 patients. Acta Neurol Scand 94: 269–275
Chang EL et al. (2004) Phase I clinical evaluation of near-simultaneous computed tomographic image-guided stereotactic body radiotherapy for spinal metastases. Int J Radiat Oncol Biol Phys 59: 1288–1294
Degen JW et al. (2005) CyberKnife stereotactic radiosurgical treatment of spinal tumors for pain control and quality of life. J Neurosurg Spine 2: 540–549
Milker-Zabel S et al. (2003) Clinical results of retreatment of vertebral bone metastases by stereotactic conformal radiotherapy and intensity-modulated radiotherapy. Int J Radiat Oncol Biol Phys 55: 162–167
Gerszten PC et al. (2006) Radiosurgery for the treatment of spinal lung metastases. Cancer 107: 2653–2661
Jin JY et al. (2007) Technical and clinical experience with spine radiosurgery: a new technology for management of localized spine metastases. Technol Cancer Res Treat 6: 127–133
Ryu S et al. (2007) Partial volume tolerance of the spinal cord and complications of single-dose radiosurgery. Cancer 109: 628–636
Ryu S et al. (2004) Patterns of failure after single-dose radiosurgery for spinal metastasis. J Neurosurg 101 (Suppl 3): 402–405
Timmerman RD et al. (2006) Stereotactic body radiation therapy: a treatment in need of basic biological research. Cancer J 12: 19–20
Timmerman R et al. (2006) Excessive toxicity when treating central tumors in a phase II study of stereotactic body radiation therapy for medically inoperable early-stage lung cancer. J Clin Oncol 24: 4833–4839
Blomgren H et al. (1995) Stereotactic high dose fraction radiation therapy of extracranial tumors using an accelerator: clinical experience of the first thirty-one patients. Acta Oncol 34: 861–870
Le QT et al. (2006) Results of a phase I dose-escalation study using single-fraction stereotactic radiotherapy for lung tumors. J Thorac Oncol 1: 802–809
Choi JY (2005) Experimental treatment of hepatocellular carcinoma. Korean J Gastroenterol 45: 271–276
Kavanagh BD et al. (2006) Interim analysis of a prospective phase I/II trial of SBRT for liver metastases. Acta Oncol 45: 848–855
Koong AC et al. (2004) Phase I study of stereotactic radiosurgery in patients with locally advanced pancreatic cancer. Int J Radiat Oncol Biol Phys 58: 1017–1021
Hara W et al. (2006) Hypofractionated stereotactic radiotherapy for prostate cancer: early results. Int J Radiat Oncol Biol Phys 66 (Suppl): S324–S325
Madsen BL et al. (2007) Stereotactic hypofractionated accurate radiotherapy of the prostate (SHARP), 33.5 Gy in five fractions for localized disease: first clinical trial results. Int J Radiat Oncol Biol Phys 67: 1099–1105
Gerszten PC et al. (2002) Feasibility of frameless single-fraction stereotactic radiosurgery for spinal lesions. Neurosurg Focus 13: e2
Rock J et al. (2002) Radiosurgical treatment for Ewing's sarcoma of the lumbar spine: case report. Spine 27: E471–E475
Ryu SI et al. (2003) Stereotactic radiosurgery for hemangiomas and ependymomas of the spinal cord. Neurosurg Focus 15: e10
Acknowledgements
The authors wish to thank Professor G Cantore for his unwavering support and Dr D Schaal for his invaluable editorial assistance.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
P Romanelli has worked occasionally as a consultant for Accuray Incorporated during the past 3 years. JR Adler Jr is a shareholder and is on the Board of Directors of Accuray Incorporated.
Supplementary information
Supplementary Table 1
Studies of high-dose stereotactic radiosurgery for spinal lesions. (DOC 100 kb)
Rights and permissions
About this article
Cite this article
Romanelli, P., Adler, J. Technology Insight: image-guided robotic radiosurgery—a new approach for noninvasive ablation of spinal lesions. Nat Rev Clin Oncol 5, 405–414 (2008). https://doi.org/10.1038/ncponc1131
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ncponc1131