Abstract
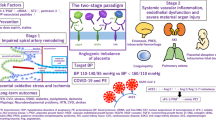
Understanding of the maternal syndrome of pre-eclampsia has greatly improved over the past 5 years. Specifically, the notion has emerged that the placenta is a source of antiangiogenic factors, such as soluble fms-like tyrosine kinase 1, that can progressively impair the mother's vascular and glomerular function throughout pregnancy. This impairment can be harmless during normal pregnancy, but in cases of defective placentation, concentrations of antiangiogenic factors increase to a level that compromises vital vascular functions in the short term and jeopardizes long-term maternal and fetal outcomes. In both pre-eclamptic and healthy pregnancies, the transient imbalance between angiogenic and antiangiogenic factors elicited by pregnancy acts as a 'stress test' for the endothelium, particularly in the glomerular capillary bed. Women who do not pass this test (i.e. those who develop pre-eclampsia or gestational hypertension) should be screened for glomerular disease, and their cardiovascular risk should be carefully monitored throughout life.
Key Points
-
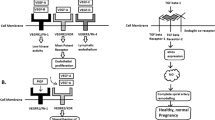
During the final weeks of pregnancy, secretion by the placenta of soluble fms-like tyrosine kinase 1, an inhibitor of vascular endothelial growth factor, increases, and circulating levels of vascular endothelial growth factor decrease
-
Since vascular endothelial growth factor is critical for maintenance of the glomerular environment, the third trimester acts as a 'stress test' for the glomeruli, and glomerular endotheliosis is common at this stage
-
Pregnancy-induced hypertension and pre-eclampsia are linked to early, excessive secretion of soluble fms-like tyrosine kinase 1 and endoglin, another antiangiogenic factor
-
Women with complicated pregnancies should be routinely screened for chronic hypertension and/or glomerulopathy (i.e. albuminuria) 8 weeks after giving birth
-
Follow-up of women with pre-eclampsia should continue for the long term and aim to minimize cardiovascular risk factors (e.g. with lifestyle advice)
-
In cases of severe pre-eclampsia, screening for thrombophilia and antinuclear antibodies might be advisable
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Sibai B et al. (2005) Pre-eclampsia. Lancet 365: 785–799
Maynard SE et al. (2003) Excess placental soluble fms-like tyrosine kinase 1 (sFlt1) may contribute to endothelial dysfunction, hypertension, and proteinuria in preeclampsia. J Clin Invest 111: 649–658
Mignini LE (2006) Mapping the theories of preeclampsia: the need for systematic reviews of mechanisms of the disease. Am J Obstet Gynecol 194: 317–321
Luttun A and Carmeliet P (2003) Soluble VEGF receptor Flt1: the elusive preeclampsia factor discovered? J Clin Invest 111: 600–602
Schaffer NK et al. (1943) Uric acid clearance in normal pregnancy and pre-eclampsia. J Clin Invest 22: 201–206
Groopman J (online 24 June 2006) The preeclampsia puzzle: making sense of a mysterious pregnancy disorder. The New Yorker [http://www.newyorker.com/archive/2006/07/24/060724fa_fact] (accessed 6 June 2008)
Chaiworapongsa T et al. (2004) Evidence supporting a role for blockade of the vascular endothelial growth factor system in the pathophysiology of preeclampsia. Young Investigator Award. Am J Obstet Gynecol 190: 1541–1547
Hertig A et al. (2004) Maternal serum sFlt1 concentration is an early and reliable predictive marker of preeclampsia. Clin Chem 50: 1702–1703
McKeeman GC et al. (2004) Soluble vascular endothelial growth factor receptor-1 (sFlt-1) is increased throughout gestation in patients who have preeclampsia develop. Am J Obstet Gynecol 191: 1240–1246
Shibata E et al. (2005) Soluble fms-like tyrosine kinase 1 is increased in preeclampsia but not in normotensive pregnancies with small-for-gestational-age neonates: relationship to circulating placental growth factor. J Clin Endocrinol Metab 90: 4895–4903
Tsatsaris V et al. (2003) Overexpression of the soluble vascular endothelial growth factor receptor in preeclamptic patients: pathophysiological consequences. J Clin Endocrinol Metab 88: 5555–5563
Wathen KA et al. (2006) Maternal serum-soluble vascular endothelial growth factor receptor-1 in early pregnancy ending in preeclampsia or intrauterine growth retardation. J Clin Endocrinol Metab 91: 180–184
Levine RJ et al. (2004) Circulating angiogenic factors and the risk of preeclampsia. N Engl J Med 350: 672–683
Berkane N et al. (2008) Hypertensive disorders of pregnancy: future perspectives. A French point of view. Curr Opin Obstet Gynecol 20: 107–109
Sugimoto H et al. (2003) Neutralization of circulating vascular endothelial growth factor (VEGF) by anti-VEGF antibodies and soluble VEGF receptor 1 (sFlt-1) induces proteinuria. J Biol Chem 278: 12605–12608
Eremina V et al. (2003) Glomerular-specific alterations of VEGF-A expression lead to distinct congenital and acquired renal diseases. J Clin Invest 111: 707–716
Ostendorf T et al. (1999) VEGF(165) mediates glomerular endothelial repair. J Clin Invest 104: 913–923
Berkane N et al. (2007) Angiogenic factors in preeclampsia: so complex, so simple? Nephrol Dial Transplant 22: 2753–2756
Shimizu A et al. (2004) Vascular endothelial growth factor165 resolves glomerular inflammation and accelerates glomerular capillary repair in rat anti-glomerular basement membrane glomerulonephritis. J Am Soc Nephrol 15: 2655–2665
Kabbinavar F et al. (2003) Phase II, randomized trial comparing bevacizumab plus fluorouracil (FU)/leucovorin (LV) with FU/LV alone in patients with metastatic colorectal cancer. J Clin Oncol 21: 60–65
Eremina V et al. (2008) VEGF inhibition and renal thrombotic microangiopathy. N Engl J Med 358: 1129–1136
Ferrara N and Kerbel RS (2005) Angiogenesis as a therapeutic target. Nature 438: 967–974
Yoshimatsu J et al. (2006) Relationship between urinary albumin and serum soluble fms-like tyrosine kinase 1 (sFlt-1) in normal pregnancy. Eur J Obstet Gynecol Reprod Biol 128: 204–208
Strevens H et al. (2003) Glomerular endotheliosis in normal pregnancy and pre-eclampsia. BJOG 110: 831–836
Murakami S et al. (2000) Renal disease in women with severe preeclampsia or gestational proteinuria. Obstet Gynecol 96: 945–949
Levine RJ et al. (2006) Soluble endoglin and other circulating antiangiogenic factors in preeclampsia. N Engl J Med 355: 992–1005
Lopez-Espinoza I et al. (1986) Urinary albumin excretion in pregnancy. BJOG 93: 176–181
Misiani R et al. (1991) Urinary albumin excretion in normal pregnancy and pregnancy-induced hypertension. Nephron 59: 416–422
Hladunewich MA et al. (2008) Course of preeclamptic glomerular injury after delivery. Am J Physiol Renal Physiol 294: F614–F620
Bar J et al. (1999) Microalbuminuria after pregnancy complicated by pre-eclampsia. Nephrol Dial Transplant 14: 1129–1132
Nisell H et al. (1995) Blood pressure and renal function seven years after pregnancy complicated by hypertension. BJOG 102: 876–881
Vikse BE et al. (2006) Adverse perinatal outcome and later kidney biopsy in the mother. J Am Soc Nephrol 17: 837–845
Sibai BM et al. (1986) Severe preeclampsia-eclampsia in young primigravid women: subsequent pregnancy outcome and remote prognosis. Am J Obstet Gynecol 155: 1011–1016
Pouta A et al. (2004) Manifestations of metabolic syndrome after hypertensive pregnancy. Hypertension 43: 825–831
Irgens HU et al. (2001) Long term mortality of mothers and fathers after pre-eclampsia: population based cohort study. BMJ 323: 1213–1217
Ray JG et al. (2005) Cardiovascular health after maternal placental syndromes (CHAMPS): population-based retrospective cohort study. Lancet 366: 1797–1803
Wilson BJ et al. (2003) Hypertensive diseases of pregnancy and risk of hypertension and stroke in later life: results from cohort study. BMJ 326: 845
Smith GC et al. (2001) Pregnancy complications and maternal risk of ischaemic heart disease: a retrospective cohort study of 129,290 births. Lancet 357: 2002–2006
Lawlor DA et al. (2005) Birth weight is inversely associated with incident coronary heart disease and stroke among individuals born in the 1950s: findings from the Aberdeen Children of the 1950s prospective cohort study. Circulation 112: 1414–1418
Sibai BM (1996) Treatment of hypertension in pregnant women. N Engl J Med 335: 257–265
Higgins JR and de Swiet M (2001) Blood-pressure measurement and classification in pregnancy. Lancet 357: 131–135
Salahuddin S et al. (2007) Diagnostic utility of soluble fms-like tyrosine kinase 1 and soluble endoglin in hypertensive diseases of pregnancy. Am J Obstet Gynecol 197: 28.e1–28.e6
He H et al. (1999) Vascular endothelial growth factor signals endothelial cell production of nitric oxide and prostacyclin through flk-1/KDR activation of c-Src. J Biol Chem 274: 25130–25135
Venkatesha S et al. (2006) Soluble endoglin contributes to the pathogenesis of preeclampsia. Nat Med 12: 642–649
Hertig A et al. (2007) Soluble endoglin levels during normotensive and hypertensive pregnancies. Eur J Obstet Gynecol Reprod Biol [10.1016/j.ejogrb.2007.09.007]
Villar J et al. (2006) Preeclampsia, gestational hypertension and intrauterine growth restriction, related or independent conditions? Am J Obstet Gynecol 194: 921–931
Fisher KA et al. (1981) Hypertension in pregnancy: clinical-pathological correlations and remote prognosis. Medicine (Baltimore) 60: 267–276
Alfirevic Z et al. (2002) How strong is the association between maternal thrombophilia and adverse pregnancy outcome? A systematic review. Eur J Obstet Gynecol Reprod Biol 101: 6–14
Kupferminc MJ (2003) Thrombophilia and pregnancy. Reprod Biol Endocrinol 1: 111
Johansen M et al. (1999) Trophoblast deportation in human pregnancy—its relevance for pre-eclampsia. Placenta 20: 531–539
Germain SJ et al. (2007) Systemic inflammatory priming in normal pregnancy and preeclampsia: the role of circulating syncytiotrophoblast microparticles. J Immunol 178: 5949–5956
Lin J and August P (2005) Genetic thrombophilias and preeclampsia: a meta-analysis. Obstet Gynecol 105: 182–192
Zhou CC et al. (2008) Autoantibody from women with preeclampsia induces soluble Fms-like tyrosine kinase-1 production via angiotensin type 1 receptor and calcineurin/nuclear factor of activated T-cells signaling. Hypertension 51: 1010–1019
Wallukat G et al. (1999) Patients with preeclampsia develop agonistic autoantibodies against the angiotensin AT1 receptor. J Clin Invest 103: 945–952
Karumanchi SA and Lindheimer MD (2008) Preeclampsia pathogenesis: “triple a rating”-autoantibodies and antiangiogenic factors. Hypertension 51: 991–992
Subramanya A et al. (2005) Steroid-responsive idiopathic glomerular capillary endotheliosis: case report and literature review. Am J Kidney Dis 45: 1090–1095
Matthiesen LS et al. (1999) A prospective study on the occurrence of autoantibodies in low-risk pregnancies. Eur J Obstet Gynecol Reprod Biol 83: 21–26
Kanasaki K et al. (2008) Deficiency in catechol-O-methyltransferase and 2-methoxyoestradiol is associated with pre-eclampsia. Nature [10.1038/nature06951]
Qazi U et al. (2008) Soluble fms-like tyrosine kinase associated with preeclampsia in pregnancy in systemic lupus erythematosus. J Rheumatol 35: 631–634
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
About this article
Cite this article
Hertig, A., Watnick, S., Strevens, H. et al. How should women with pre-eclampsia be followed up? New insights from mechanistic studies. Nat Rev Nephrol 4, 503–509 (2008). https://doi.org/10.1038/ncpneph0880
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ncpneph0880
This article is cited by
-
Post-partum trend in blood pressure levels, renal function and proteinuria in women with severe preeclampsia and eclampsia in Sub-Saharan Africa: A 6-months cohort study
BMC Pregnancy and Childbirth (2014)
-
Insuffisance rénale aiguë et prééclampsie
Réanimation (2013)
-
Women with a history of preeclampsia should be monitored for the onset and progression of chronic kidney disease
Nature Clinical Practice Nephrology (2009)