Abstract
There is increasing evidence from genome-wide association studies for a strong inherited genetic basis of susceptibility to acute lymphoblastic leukaemia (ALL) in children, yet the effects of protein-coding variants on ALL risk have not been systematically evaluated. Here we show a missense variant in CDKN2A associated with the development of ALL at genome-wide significance (rs3731249, P=9.4 × 10−23, odds ratio=2.23). Functional studies indicate that this hypomorphic variant results in reduced tumour suppressor function of p16INK4A, increases the susceptibility to leukaemic transformation of haematopoietic progenitor cells, and is preferentially retained in ALL tumour cells. Resequencing the CDKN2A–CDKN2B locus in 2,407 childhood ALL cases reveals 19 additional putative functional germline variants. These results provide direct functional evidence for the influence of inherited genetic variation on ALL risk, highlighting the important and complex roles of CDKN2A–CDKN2B tumour suppressors in leukaemogenesis.
Similar content being viewed by others
Introduction
The risk of developing acute lymphoblastic leukaemia (ALL) is highest between 2 and 5 years after birth1,2, with initiating sentinel somatic genomic lesions (for example, chromosomal translocations) detectable at the time of birth in many cases3,4. This early disease onset suggests a strong inherited genetic basis for ALL susceptibility, and recent genome-wide association studies (GWAS) have discovered at least six risk loci: ARID5B, IKZF1, CEBPE, PIP4K2A-BMI1, GATA3 and CDKN2A–CDKN2B5,6,7,8,9,10. These ALL risk genes are directly involved in haematopoietic stem cell function, lymphocyte differentiation and development, and cell cycle regulation11,12,13,14,15, several of which are also commonly targeted by somatic genomic lesions. In particular, the CDKN2A–CDKN2B locus is one of the most frequently deleted genomic regions in childhood ALL with focal copy number loss in both B- and T-cell ALL14,16.
The vast majority of variants examined in previous ALL GWAS are intronic or intergenic. Although it is now evident that non-coding variants related to disease traits are significantly over-represented in regulatory DNA and often function as modulators of local or distal gene transcription17,18, questions also arise whether coding variants within ALL susceptibility genes might confer even greater effects on disease development. Moreover, a large number of low-frequency and rare-coding germline variants have been discovered by exome-sequencing efforts19, but their contributions to ALL pathogenesis have yet to be examined systematically.
In the present study, we perform an exome-focused GWAS to systematically examine the impact of germline-coding variants on the development of ALL in children of European descent, experimentally explore the functional consequences of the genome-wide significant variant in the CDKN2A gene, and comprehensively characterize coding variation at this locus by targeted resequencing.
Results
Exome-focused GWAS of ALL susceptibility
In the discovery GWAS, we genotyped 1,773 children with B-ALL and 10,448 non-ALL controls of European descent20,21 for 247,505 variants using the Illumina Infinium HumanExome array. Three loci with genome-wide significant association signals were observed: ARID5B (10q21.2), IKZF1 (7q12.2) and CDKN2A (9p21.3) (Fig. 1). Non-coding variants rs10821936 in ARID5B and rs4132601 in IKZF1 showed the strongest association (P=9.9 × 10−46 and 4.3 × 10−37, the logistic regression test, respectively; Fig. 1 and Supplementary Table 1), confirming previous GWAS findings from our group and others5,6. No coding variants in ARID5B and IKZF1 were significantly associated with ALL susceptibility. The third genome-wide significant hit was a missense SNP at the CDKN2A locus (rs3731249, P=9.4 × 10−23, the logistic regression test, Fig. 1, Table 1). The T allele at rs3731249 was over-represented in ALL compared with controls (6.8% versus 3.0%, Table 1), with every copy of the allele conferring 2.23-fold increase in disease risk (95% confidence interval 1.90–2.61). The C-to-T nucleotide substitution at rs3731249 (c.C442T) resulted in an alanine-to-threonine change in amino-acid sequence (p.A148T) for tumour suppressor p16INK4A. This variant also locates in the 3′ untranslated region (3′-UTR) of the p14ARF transcript, an alternative open reading frame at this locus encoding a different tumour suppressor. Interestingly, previous GWAS had identified an intronic variant in CDKN2A (rs3731217) to be strongly associated with susceptibility to ALL in populations of European descent9. Genotype correlation between the coding variant rs3731249 and the intronic rs3731217 is exceedingly low (r2<0.01 in Europeans, Supplementary Fig. 1), and multivariate analyses including both SNPs indicated their independent contribution to ALL risk (Supplementary Table 2). In the replication cohort of 409 childhood ALL cases and 1,599 non-ALL controls of European descent in Denmark, the association signal at rs3731249 was validated (P=5.2 × 10−4, odds ratio=1.73 (1.27–2.36), the logistic regression test, Table 1) and this variant also remained significant after adjusting for rs3731217.
Association between genotype and ALL was evaluated for 35,802 SNPs in 1,773 ALL cases and 10,448 non-ALL controls. P-values (the logistic regression test, −log10 P, y axis) were plotted against respective chromosomal position of each SNP (x axis). Gene, symbols were indicated for 3 loci achieving genome-wide significance threshold (P<5 × 10−8, dashed blue line): ARID5B (10q21.2), IKZF1 (7p12.2) and CDKN2A (9p21.3). Blue dots indicated SNPs within 2M bp of the top ALL susceptibility variants at the ARID5B (rs10821936) and IKZF1(rs4132601) loci, the red dots indicated SNPs in the 2M-bp region around the novel ALL risk variant rs3731249 in CDKN2A.
Functional characterization of the rs3731249 variant
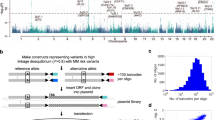
To experimentally evaluate the effects of rs3731249 on ALL leukaemogenesis, we directly compared the effect of wildtype versus variant allele p16INK4A (p.148A versus p.148 T) on BCR–ABL1-mediated leukaemic transformation in vitro. We chose mouse haematopoietic progenitor Ba/f3 cell line because it is inherently p16Ink4a-defective due to methylation at the Ink4a-Arf locus22, and ectopic expression of BCR-ABL1 in Ba/f3 cells efficiently induces exogenous cytokine (interleukin 3 (IL3))-independent proliferation. Over-expression of wild-type p16INK4A(p.148A) significantly inhibited leukaemic transformation by BCR–ABL1 (Fig. 2a, Supplementary Fig. 2), consistent with its role as a critical tumour suppressor in ALL. In contrast, Ba/f3 cells overexpressing variant p16INK4A(p.148 T) were significantly more susceptible to BCR–ABL1 transformation measured by IL3-independent growth, suggesting that the p.148 T variant is likely hypomorphic with reduced tumour suppressor function. In Ba/f3 cells transfected with both variant and wild-type p16INK4A, the relative ratio of the p.148 T (variant) to p.148A (wildtype) transcript increased substantially upon BCR–ABL1-mediated transformation (Supplementary Fig. 3), consistent with the increased leukaemia risk conferred by the variant allele at rs3731249. To further examine the potential susceptibility to ALL conferred by the rs3731249 in patients, we compared the genotype distribution in RNA and DNA from primary leukaemic blasts and matched germline samples from children with ALL (Fig. 2b). Of 15 cases with the heterozygous germline genotype at this SNP, six exhibited somatic deletion of one copy of CDKN2A, all of which retained the risk allele in tumour cells. Even in cases not affected by somatic copy number loss at this locus, the variant p16INK4A(c.442 T) was preferentially transcribed relative to wildtype (c.442C), with allele-biased expression ranging from 61 to 100%, Fig. 2b). Altogether, these results pointed to the possibility that cells carrying the hypomorphic risk allele at rs3731249 might have been enriched during leukaemogenesis.
(a) Mouse haematopoietic progenitor cell Ba/f3 overexpressing wildtype, variant p16INK4A, or transfected with control vector was transduced with leukaemia oncogenic BCR–ABL1 fusion gene. Cell proliferation in the absence of cytokine IL3 was measured daily as an indicator of leukaemic transformation. Ectopic expression of p16INK4A (p.148 T, green) significantly potentiated leukaemic transformation by BCR–ABL1, compared with cells expressing wild-type p16INK4A (p.148A, blue), consistent with the association of this allele with susceptibility to ALL. Data represent the mean of three replicates±s.e.m. (b) Allele-specific expression of p16INK4A in ALL blasts was determined by comparing the number of sequence reads for transcripts containing C or T alleles at rs3731249 (p16INK4Ap.148A versus p16INK4Ap.148 T), in 15 childhood ALL cases with heterozygous genotype in the germline DNA at this SNP. Each dot represents an ALL case (red indicates cases with somatic deletion (loss of heterozygosity) and blue indicates cases without copy number change in tumour) and the line of identity indicates equal expression of both alleles. P-value was estimated by paired t-test based on the number of sequence reads for each allele.
Targeted resequencing of CDKN2A and CDKN2B in childhood ALL
To comprehensively identify putative functional ALL susceptibility variants at this locus, we resequenced the coding region of the CDKN2A and CDKN2B genes in germline DNA from 2,407 childhood ALL cases (1,450 of which were also included in the discovery GWAS). In addition to rs3731249, we observed another 13 germline exonic variants in tumour suppressors p16INK4A and p14ARF encoded by the CDKN2A gene, 12 of which result in amino-acid sequence changes (Fig. 3, Supplementary Table 3). These missense variants were all singletons, except for the p.D125H variant in p16INK4A and the p.A121T variant in p14ARF observed in two and five cases, respectively. Five variants were predicted to be damaging based on combined annotation dependent depletion23 (CADD score>13, Supplementary Table 3), and we did not observe germline insertions or deletions in CDKN2A in our ALL cohort. Comparing with 4,300 European American individuals from the NHLBI GO Exome Sequencing Project (ESP), there was a trend for a higher burden of rare missense variants in relative to controls the CDKN2A gene (p16INK4A and p14ARF) in children with ALL (0.71% versus 0.23%, P=0.0045, Fisher’s exact test, Fig. 3). In addition, we identified six germline-coding variants in the adjacent CDKN2B gene in this cohort of children with ALL, although there was no significant over-representation compared with European controls in the ESP cohort (0.83% versus 0.79%, Fig. 3).
CDKN2A and CDKN2B genes were sequenced using Illumina HiSeq platform following capture-based enrichment of this genomic region in 2,407 ALL cases of European descent. Variants in non-ALL controls were based on publicly available data from the individuals of European descent within the NHLBI Exome Sequencing Project (N=4,300). Exonic variants are classified as silent or missense (grey or purple solid circles) and are mapped to three distinct open reading frames at this locus: p16INK4A, p14ARF and p15INK4B, for ALL cases (red vertical lines) and non-ALL controls (blue vertical lines), and functional domains are indicated by colour based on Pfam annotation. Each circle represents a unique individual carrying the indicated variant (heterozygous or homozygous), except for variants recurring in more than 10 individuals for which the number in the circle indicates the exact frequency of the observed variant.
Discussion
Encoding three tumour suppressor proteins (p16INK4A, p14ARF and p15INK4B), the CDKN2A–CDKN2B locus at 9p21 is promiscuously associated with tumorigenesis and commonly targeted by somatic mutation, deletion and/or hypermethylation in various cancers. p16INK4A and p15INK4B are highly homologous inhibitors of cyclin-dependent kinase and function mainly as master regulators of cell cycle entry via the Rb-E2F signalling axis24. Although also encoded by the CDKN2A gene, p14ARF utilizes a completely different reading frame with distinct tumour suppression functions by inhibiting MDM2 and activating p5325. Suppressed during normal haematopoiesis, p16INK4A and p14ARF expression is activated on oncogenic stimuli (for example, constitutive expression of BCR-ABL1 fusion) to trigger cell cycle exit (senescence) or apoptosis as a means of eliminating oncogene-stressed cells26. In fact, the CDKN2A–CDKN2B locus is either bi- or monoallelicly deleted in 64% of BCR–ABL1-positive ALL cases and in 32–72% of T- or B-ALL cases without the BCR-ABL1 translocation, suggesting positive selection for cells with defective p16INK4A, p14ARF and p15INK4B (or some combinations thereof) during leukaemogenesis.
The previously reported ALL susceptibility variant rs3731217 is located in a non-coding region downstream of exon 1β (specific for p14ARF), but distal to exon 1α (specific for p16INK4A) of the CDKN2A gene. The germline genotype at this SNP was not associated with overall CDKN2A expression in lymphoblastoid cell lines9 but transcript-specific analyses may be needed to definitively determine the effects of this variant on p14ARF versus p16INK4A expression. In contrast, the genome-wide significant variant rs3731249 in our current GWAS localizes to exon 2 of CDKN2A. While this exon is shared by both p16INK4A and p14ARF, the C-to-T nucleotide transition causes a missense change for the p16INK4A open reading frame but is in the UTR of the p14ARF, therefore, likely to have a more direct effect on the former. This hypothesis is supported by the fact that haematopoietic progenitor cells (Ba/f3) expressing variant p16INK4A were substantially more susceptible to BCR–ABL1-mediated leukaemic transformation compared with cells with the wild-type protein (Fig. 2a), pointing to rs3731249 as a possible functional variant directly contributing to the association with ALL risk. The structural basis of the hypomorphic effects of the p.A148T variant is unclear, since this residue is not directly involved in binding to CDK4 or CDK627. However, there was evidence that the variant p16INK4A (p.148 T) is preferentially retained in the nucleus compared with the wild-type p16INK4A (p.148A), compromising its ability to inhibit CDKs in the cytoplasm28,29. The relative contribution of p16INK4A versus p14ARF to ALL pathogenesis is not unequivocal because somatic deletions at this locus almost always lead to the loss of both genes. Although the rs3731249 variant also results in sequence changes of the 3′-UTR of the p14ARF transcript, bioinformatic prediction did not identify any potential effects on mRNA stability or microRNA binding and no difference was observed in reporter gene transcription under the influence of 3′-UTR containing either the wildtype or variant allele at rs3731249 (Supplementary Fig. 4), suggesting minimal effects of this variant on p14ARF transcription. Finally, rs3731249 is also observed in non-European populations, for example, there was a trend for a higher frequency of the risk allele in African American children with ALL than that in individuals from this racial background in the NHLBI ESP cohort (0.58% in 260 ALL cases versus 0.38% in 2,203 controls), although a much larger sample size is needed to rigorously examine the statistical significance of such differences. It should be noted that we and others previously showed that the non-coding ALL risk variants (rs17756311 and rs3731217) at this locus had much stronger effects in European Americans than in other race/ethnic groups7,30, suggesting potential racial differences in genetic susceptibility to ALL.
We subsequently identified additional coding variants in p16INK4A, p14ARF and p15INK4B by resequencing, most of which were low frequency or rare. While there was a modest over-representation of potentially damaging coding variants in ALL cases compared with controls (Fig. 3), our data do not suggest that rare variants contribute substantially to the associations with ALL susceptibility observed at this locus. It should also be noted that the vast majority of coding variants within the CDKN2A gene affects only one of the two tumour suppressors (either p16INK4A or p14ARF). Interestingly, rs199888003 is the only variant that is located in the coding region of both p16INK4A and p14ARF, resulting in an alanine-to-threonine change in p14ARF (p.A121T) with synonymous effect on p16INK4A. This is also the most frequent germline missense variant in p14ARF in our cohort and was over-represented in ALL compared with non-ALL controls (0.21% versus 0.046%, respectively, Fig. 3). This substitution of threonine in p14ARF adds a possible glycosylation and phosphorylation site and also introduces a phosphoprotein-binding FHA domain implicated in DNA damage response and cell cycling31. Future studies are warranted to determine the exact consequences of this variant on p14ARF functions. To systemically evaluate the contribution of low frequency and rare-coding variants to ALL risk, we also performed genome-wide gene-level burden test but did not observe any genome-wide significant associations (Supplementary Table 4). Of the six known ALL risk loci, we noted two coding variants in CEBPE (rs141903485 and rs146580935, Supplementary Table 5) nominally associated with ALL susceptibility.
In conclusion, we comprehensively evaluated exonic genetic variations for association with ALL susceptibility and identified novel coding risk variants at the CDKN2A–CDKN2B locus that may directly affect tumour suppressor functions and potentiate leukaemic transformation. These results provided functional evidence for the influence of inherited genetic variants on ALL leukaemogenesis, further indicating that a continuum of genetic variations in both host and tumour genomes contribute to malignant transformation and cancer risk.
Methods
Subjects and samples
The discovery GWAS consisted of 1,773 childhood B-ALL cases and 10,448 non-ALL controls of European descent (>90% European genetic ancestry as estimated using STRUCTURE32,33). ALL cases were from the Children’s Oncology Group (COG) AALL0232 study (N=1,277)8, the COG P9906 protocol (N=115)34 and St Jude Total Therapy XIIIB and XV protocols (N=381)5. Unrelated individuals of European descent from the Atherosclerosis Risk in Communities (ARIC) study20,21 were used as non-ALL controls because the prevalence of adult survivors of childhood ALL is less than 1 in 10,000 in the US. The replication series included 409 children with ALL from NOPHO ALL92, ALL2000 and ALL2008 protocols35 and 1,599 unrelated non-ALL controls from Danish Childhood Obesity Biobank study (clinicaltrials.gov: NCT00928473) in Holbæk and at random schools in Zealand, Denmark. ALL cases were selected only on the basis of sample availability, and we did not observe any statistically significant differences in demographic or clinical features of children included versus not included in this genetic study. We elected to focus on individuals of European descent to minimize population stratification36.
Germline DNA for cases was extracted from peripheral blood or bone marrow samples obtained during clinical remission (<5% ALL blasts by morphology). This study was approved by the Institutional Review Board at St Jude Children’s Research Hospital and COG member institutions and the Ethics Committee at the Danish Data Protection Agency, Region Zealand and the University Hospital Rigshospitalet, Denmark. Informed consent was obtained from parents, guardians, or patients, as appropriate.
Genotyping and quality control
SNP genotyping was performed in germline DNA using the Illumina Infinium HumanExome Array v1.0 in the discovery GWAS, and using Illumina HumanCoreExome chip for the replication series. Genotype calls (coded as 0, 1, and 2 for AA, AB and BB genotypes) were determined using the Illumina GenomeStudio Software. For the ALL cases, samples for which genotype was ascertained at <98% of SNPs on the array were deemed to have failed and were excluded from the analyses. Quality control procedures were performed for both samples and SNPs on the basis of call rate, minor allele frequency (MAF), and Hardy Weinberg equilibrium (Supplementary Fig. 5). Detailed quality control for the non-ALL controls from the ARIC study was performed at the University of Texas Health Science Center following established protocols21.
We performed principal component analysis of cases and controls in the discovery GWAS to characterize population substructure (Supplementary Fig. 6).
Genome-wide analyses
In the discovery GWAS, the association of each SNP individually with ALL susceptibility was tested by comparing the genotype frequency between ALL cases and non-ALL controls in logistic regression models, after adjusting for top 10 principal components to control for population stratification. A quantile–quantile (Q–Q) plot was constructed and there was only minimal inflation at the upper tail of the distribution (λ=1.08, Supplementary Fig. 7). In the replication studies, we evaluated the novel genome-wide significant variant rs3731249, using the same logistic regression models. Multivariate logistic regression model including both rs3731217 and rs3731249 were tested to determine independent association signals at the CDKN2A locus in both discovery and replication series.
We also performed gene-level analyses to evaluate the aggregated effects of low-frequency variants on ALL susceptibility, using the SKAT test37. Missense, stop codon-altering and splice-site variants with MAF<5% were included. In total, 12,687 genes with at least two variants were tested.
R (version 3.0) statistical software was used for all analyses unless indicated otherwise.
CDKN2A–CDKN2B resequencing and rare variant analyses
Germline DNA from 2,407 children with ALL was used to create individual Illumina dual-indexed libraries. These libraries were pooled in sets of 96 and hybridized with a custom version of the Roche NimbleGen SeqCap EZ custom probes to capture the CDKN2A–CDKN2B region on 9p21. Quantitative PCR was used to determine the appropriate capture product titre necessary to efficiently populate an Illumina HiSeq 2000 flowcell for paired-end 2 × 101 bp sequencing. Each sequence pool of 96 samples was demultiplexed, with coverages of >20 × depth across >90% of the targeted regions for nearly all samples. Sequence reads in FASTQ format were mapped and aligned using the Burrows–Wheeler Aligner, and genetic variants were called using the GATK pipeline version 3.1 (ref. 38). We compared the proportion of rare variant-carriers in ALL subjects (either homozygous or heterozygous) versus that in individuals of European descent in the ESP cohort (non-ALL controls), focusing on variants with MAF<1%. Statistical significance of the difference was estimated using Fisher’s exact test.
CDKN2A sequencing was also performed in matched germline and diagnostic ALL tumour DNA by Complete Genomics for all cases with available materials, and in tumour RNA by RNA-seq. Details regarding sequencing, data analysis and coverage are available at ftp://caftpd.nci.nih.gov/pub/dcc_target/ALL/Phase_II/sequence/WGS/CGI_TARGET_Pipeline_README.pdf, or as previously described39 (European Genome Phenome archive: EGAS00001000654).
Leukaemic transformation assay in Ba/f3 cells
The full-length CDKN2A was purchased from GE Healthcare. The p.A148T variant (rs3731249) was introduced by site-directed mutagenesis (forward primer: 5′-TGCCCGCATAGATGCCACGGAAGGTCCCTCAGA-3′, reverse primer: 5′-TCTGAGGGACCTTCCGTGGCATCTATGCGGGCA-3′) and cloned into the cL20c-IRES–GFP lentiviral vector, and lentiviral supernatants containing cL20c–p16INK4Ap.148A–IRES–GFP or cL20c–p16INK4Ap.148 T–IRES–GFP were produced by transient transfection of 293 T cells (American Type Culture Collection) using calcium phosphate. The MSCV (Babe MCS)–BCR–ABL1–Luc2 construct was a gift from Dr Charles Sherr at St Jude Children’s Research Hospital22 and retroviral particles were produced using 293 T cells. Ba/f3 cells (gift from Dr Omar Abdel-Wahab at the Memorial Sloan Kettering Cancer Center) were maintained in medium supplemented with 10 ng ml−1 recombinant mouse IL3. Ba/f3 cells were transduced with lentiviral supernatants with wild-type or variant p16INK4A(Supplementary Fig. 8). GFP-positive cells were sorted 48 h after transduction and maintained in IL3 medium for another 24 h before transfected by BCR–ABL1 retroviral supernatants. Forty-eight hours later, cells were washed three times and grown in the absence of cytokine. Cell growth and viability were monitored daily by Trypan blue using a TC10 automated cell counter (BIO-RAD). Each experiment was performed three times.
For immunoblotting assays, Ba/f3 cells were washed and resuspended in lysis buffer (10 × PBS with 0.5 M EDTA, 10% NP-40 and 50% glycerol) with protease inhibitors and phosphatase inhibitors. Lysates were sonicated six times and centrifuged at 13,000 g for 10 min at 4 °C. Supernatants were quantified for protein concentration by BCA kit, electrophoresed, and transferred to nitrocellulose membranes. Membranes were probed with 1: 1,000 anti-p16INK4A antibody (Abcam, ab81278), with α-tubulin as a loading control (1: 1,000 anti-tubulin antibody, Sigma-Aldrich, T5618).
For quantitative reverse transcription-PCR (qRT–PCR), total RNA was extracted using the RNeasy Micro kit (Qiagen) according to the manufacturer’s protocol. Total RNA (500 ng) was reverse transcribed into cDNA using oligoT primers and the SuperScript III reverse transcriptase kit (Invitrogen). Quantitative real-time PCR was performed by using ABI Prism 7900HT detection system (Applied Biosystems) with Faststart SYBR Green master mix (Roche). Relative expression was calculated as a ratio of BCR-ABL1 to Hprt. Primer sequences of BCR–ABL1 and Hprt were as follows: BCR-ABL1 (forward: 5′-CTGGCCCAACGATGGCGA-3′; reverse: 5′-CACTCAGACCCTGAGGCTCAA-3′); Hprt (forward: 5′-GAGCAATGATCTTGATCTTC-3′; reverse: 5′-TTCCTTCTTGGGTATGGAAT-3′).
To co-express rs3731249 variant and wild-type p16INK4A, Ba/f3 cells were transduced with equal molar cL20c–p16INK4Ap.148A–IRES–GFP and cL20c–p16INK4Ap.148 T–IRES–iYFP lentivirus and cells successfully transfected with both were selected by flow cytometry sorting for GFP/YFP double positivity. BCR-ABL1-mediated transformation was performed as described above. Genomic DNA and RNA samples were collected at day 0, 2, 4 and 5 after IL3 removal. p.148A and p.148 T transcript in RNA was quantified using allele-specific Taqman genotyping assay and normalized to allele ratio in matched DNA samples at respective time points. Each experiment was performed three times and each sample was assayed in triplicate.
Luciferase reporter assays
The p14INK4A–3′-UTR vector (3′-UTR for Human NM_058195.2 was placed downstream of luciferase reporter gene on the pEZX-MT01 backbone) was purchased from GeneCopoeia and the T variant at rs3731249 was introduced by site-directed mutagenesis (forward primer: 5′-CCATGCCCGCATAGATGCCGTGGAAGGTCCCTCAGACATCC-3′; reverse primer: 5′-GGATGTCTGAGGGACCTTCCACGGCATCTATGCGGGCATGG-3′). For reporter gene assay, 2.5 × 104 293 T cells cultured in 96-well plate were transiently transfected with 100 ng empty vector, variant, or wild-type p14INK4A 3′UTR constructs using Lipofectamine 2000 (Invitrogen). Firefly luciferase activities were measured 24 h later using the Dual Luciferase Assay (Promega). The results were normalized against Renilla luciferase. Each reporter construct transfection was replicated at least three times, and each sample was assayed in triplicate.
Additional information
Accession codes. The RNA-seq data have been deposited in European Genome Phenome archive under the accession codes EGAS00001000654.
How to cite this article: Xu, H. et al. Inherited coding variants at the CDKN2A locus influence susceptibility to acute lymphoblastic leukaemia in children. Nat. Commun. 6:7553 doi: 10.1038/ncomms8553 (2015).
References
Greaves, M. Infection, immune responses and the aetiology of childhood leukaemia. Nat. Rev. Cancer 6, 193–203 (2006).
Hjalgrim, L. L. et al. Age- and sex-specific incidence of childhood leukemia by immunophenotype in the Nordic countries. J. Natl Cancer Inst. 95, 1539–1544 (2003).
Greaves, M. F. & Wiemels, J. Origins of chromosome translocations in childhood leukaemia. Nat. Rev. Cancer 3, 639–649 (2003).
Greaves, M. F., Maia, A. T., Wiemels, J. L. & Ford, A. M. Leukemia in twins: lessons in natural history. Blood 102, 2321–2333 (2003).
Trevino, L. R. et al. Germline genomic variants associated with childhood acute lymphoblastic leukemia. Nat. Genet. 41, 1001–1005 (2009).
Papaemmanuil, E. et al. Loci on 7p12.2, 10q21.2 and 14q11.2 are associated with risk of childhood acute lymphoblastic leukemia. Nat. Genet. 41, 1006–1010 (2009).
Xu, H. et al. Novel susceptibility variants at 10p12.31-12.2 for childhood acute lymphoblastic leukemia in ethnically diverse populations. J. Natl Cancer Inst. 105, 733–742 (2013).
Perez-Andreu, V. et al. Inherited GATA3 variants are associated with Ph-like childhood acute lymphoblastic leukemia and risk of relapse. Nat. Genet. 45, 1494–1498 (2013).
Sherborne, A. L. et al. Variation in CDKN2A at 9p21.3 influences childhood acute lymphoblastic leukemia risk. Nat. Genet. 42, 492–494 (2010).
Migliorini, G. et al. Variation at 10p12.2 and 10p14 influences risk of childhood B-cell acute lymphoblastic leukemia and phenotype. Blood 122, 3298–3307 (2013).
Akasaka, T. et al. Five members of the CEBP transcription factor family are targeted by recurrent IGH translocations in B-cell precursor acute lymphoblastic leukemia (BCP-ALL). Blood 109, 3451–3461 (2007).
Novershtern, N. et al. Densely interconnected transcriptional circuits control cell states in human hematopoiesis. Cell 144, 296–309 (2011).
Lahoud, M. H. et al. Gene targeting of Desrt, a novel ARID class DNA-binding protein, causes growth retardation and abnormal development of reproductive organs. Genome Res. 11, 1327–1334 (2001).
Mullighan, C. G. et al. Deletion of IKZF1 and prognosis in acute lymphoblastic leukemia. N. Engl. J. Med. 360, 470–480 (2009).
Yagi, R., Zhu, J. & Paul, W. E. An updated view on transcription factor GATA3-mediated regulation of Th1 and Th2 cell differentiation. Int. Immunol. 23, 415–420 (2011).
Mullighan, C. G. et al. Genome-wide analysis of genetic alterations in acute lymphoblastic leukaemia. Nature 446, 758–764 (2007).
ENCODE Project Consortium. An integrated encyclopedia of DNA elements in the human genome. Nature 489, 57–74 (2012).
Maurano, M. T. et al. Systematic localization of common disease-associated variation in regulatory DNA. Science 337, 1190–1195 (2012).
Tennessen, J. A. et al. Evolution and functional impact of rare coding variation from deep sequencing of human exomes. Science 337, 64–69 (2012).
The Atherosclerosis Risk in Communities (ARIC) Study: design and objectives. The ARIC investigators. Am. J. Epidemiol. 129, 687–702 (1989).
Grove, M. L. et al. Best practices and joint calling of the HumanExome BeadChip: the CHARGE Consortium. PLoS ONE 8, e68095 (2013).
Williams, R. T., Roussel, M. F. & Sherr, C. J. Arf gene loss enhances oncogenicity and limits imatinib response in mouse models of Bcr-Abl-induced acute lymphoblastic leukemia. Proc. Natl Acad. Sci. USA 103, 6688–6693 (2006).
Kircher, M. et al. A general framework for estimating the relative pathogenicity of human genetic variants. Nat. Genet. 46, 310–315 (2014).
Krug, U., Ganser, A. & Koeffler, H. P. Tumor suppressor genes in normal and malignant hematopoiesis. Oncogene 21, 3475–3495 (2002).
Sherr, C. J. et al. p53-Dependent and -independent functions of the Arf tumor suppressor. Cold Spring Harb. Symp. Quant. Biol. 70, 129–137 (2005).
Williams, R. T. & Sherr, C. J. The INK4-ARF (CDKN2A/B) locus in hematopoiesis and BCR-ABL-induced leukemias. Cold Spring Harb. Symp. Quant. Biol. 73, 461–467 (2008).
Russo, A. A., Tong, L., Lee, J. O., Jeffrey, P. D. & Pavletich, N. P. Structural basis for inhibition of the cyclin-dependent kinase Cdk6 by the tumour suppressor p16INK4a. Nature 395, 237–243 (1998).
Walker, G. J., Gabrielli, B. G., Castellano, M. & Hayward, N. K. Functional reassessment of P16 variants using a transfection-based assay. Int. J. Cancer 82, 305–312 (1999).
Lilischkis, R., Sarcevic, B., Kennedy, C., Warlters, A. & Sutherland, R. L. Cancer-associated mis-sense and deletion mutations impair p16INK4 CDK inhibitory activity. Int. J. Cancer 66, 249–254 (1996).
Chokkalingam, A. P. et al. Genetic variants in ARID5B and CEBPE are childhood ALL susceptibility loci in Hispanics. Cancer Causes Control 24, 1789–1795 (2013).
Durocher, D., Smerdon, S. J., Yaffe, M. B. & Jackson, S. P. The FHA domain in DNA repair and checkpoint signaling. Cold Spring Harb. Symp. Quant. Biol. 65, 423–431 (2000).
Pritchard, J. K., Stephens, M. & Donnelly, P. Inference of population structure using multilocus genotype data. Genetics 155, 945–959 (2000).
Yang, J. J. et al. Ancestry and pharmacogenomics of relapse in acute lymphoblastic leukemia. Nat. Genet. 43, 237–241 (2011).
Harvey, R. C. et al. Rearrangement of CRLF2 is associated with mutation of JAK kinases, alteration of IKZF1, Hispanic/Latino ethnicity, and a poor outcome in pediatric B-progenitor acute lymphoblastic leukemia. Blood 115, 5312–5321 (2010).
Schmiegelow, K. et al. Long-term results of NOPHO ALL-92 and ALL-2000 studies of childhood acute lymphoblastic leukemia. Leukemia 24, 345–354 (2010).
Mathieson, I. & McVean, G. Differential confounding of rare and common variants in spatially structured populations. Nat. Genet. 44, 243–246 (2012).
Wu, M. C. et al. Rare-variant association testing for sequencing data with the sequence kernel association test. Am. J. Hum. Genet. 89, 82–93 (2011).
DePristo, M. A. et al. A framework for variation discovery and genotyping using next-generation DNA sequencing data. Nat. Genet. 43, 491–498 (2011).
Roberts, K. G. et al. Targetable kinase-activating lesions in Ph-like acute lymphoblastic leukemia. N. Engl. J. Med. 371, 1005–1015 (2014).
Acknowledgements
We thank the patients and parents who participated in the clinical protocols included in this study and the clinicians and research staff at participating institutions. J.J.Y. is supported by the American Society of Hematology Scholar Award and by the Order of St. Francis Foundation. H.Z. is a St Baldrick’s International Scholar. V.P.A is supported by the Spanish Ministry of Education Fellowship Grant and by the St Jude Children’s Research Hospital Academic Programs Special Fellowship. C.G.M. is a Pew Scholar in the Biomedical Sciences and a St Baldrick’s Scholar. We thank M. Shriver (Pennsylvania State University) for sharing SNP genotype data of the Native American references and K. Nielsen (The Technical University of Denmark) for assistance with analysing the Danish dataset. This work was supported by the National Institutes of Health (grant numbers CA156449, CA21765, CA36401, CA98543, CA114766, CA98413, CA140729, CA176063, GM097119 and GM92666, HHSN261200800001E), the American Lebanese Syrian Associated Charities (ALSAC), the Danish Council for Strategic Research (TARGET (0603-00484B), BIOCHILD (0603-00457B)), the Region Zealand Health Scientific Research Foundation, Danish National Research Foundation, Danish Childhood Cancer Foundation, and Swedish Childhood Cancer Foundation. The Atherosclerosis Risk in Communities (ARIC) study is carried out as a collaborative study supported by the National Heart, Lung, and Blood Institute contracts (HHSN268201100005C, HHSN268201100006C, HHSN268201100007C, HHSN268201100008C, HHSN268201100009C, HHSN268201100010C, HHSN268201100011C and HHSN268201100012C). Funding support for ‘Building on GWAS for NHLBI-diseases: the U.S. CHARGE consortium’ was provided by the NIH through the American Recovery and Reinvestment Act of 2009 (ARRA) (5RC2HL102419). The authors also thank the staff and participants of the ARIC study for their important contributions.
Author information
Authors and Affiliations
Contributions
J.J.Y. is the principal investigator of this study and has full access to all of the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis. H.X., W.Y., M.Q., R.Y., R.G. and V.P.A. performed data analysis, H.Z., H.X. and X.Z. performed the experiments. J.J.Y., H.X, H.Z. and M.Q. wrote the manuscript. R.Y., A.C.M., M.D., J.M.G-F., P.J.L., G.N., Y.L., E.R., E.L., W.P-B., W.L.C., N.W., R.W., T.H., J.H., E.M., R.F., C.P., J.Z., C.G.M., W.E.E, S.P.H., R.G., K.S., M.L.L. and M.V.R. contributed reagents, materials and/or data. J.J.Y., H.X., H.Z., W.Y., M.Q., V.P.A., R.Y., R.G., R. W. and K. S. interpreted the data and the research findings. All of the co-authors reviewed the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Supplementary Information
Supplementary Figures 1-8 and Supplementary Tables 1-5 (PDF 1183 kb)
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Xu, H., Zhang, H., Yang, W. et al. Inherited coding variants at the CDKN2A locus influence susceptibility to acute lymphoblastic leukaemia in children. Nat Commun 6, 7553 (2015). https://doi.org/10.1038/ncomms8553
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/ncomms8553
This article is cited by
-
Investigation of inherited noncoding genetic variation impacting the pharmacogenomics of childhood acute lymphoblastic leukemia treatment
Nature Communications (2024)
-
Association of CDKN2A/B mutations, PD-1, and PD-L1 with the risk of acute lymphoblastic leukemia in children
Journal of Cancer Research and Clinical Oncology (2023)
-
Association of IKZF1 and CDKN2A gene polymorphisms with childhood acute lymphoblastic leukemia: a high-resolution melting analysis
BMC Medical Genomics (2022)
-
Distinct germline genetic susceptibility profiles identified for common non-Hodgkin lymphoma subtypes
Leukemia (2022)
-
A causal mechanism for childhood acute lymphoblastic leukaemia
Nature Reviews Cancer (2018)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.