Abstract
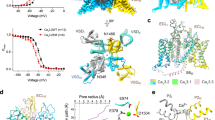
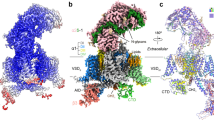
Two voltage-gated calcium channel subtypes—CaV1.2 and CaV1.3—underlie the major L-type Ca2+ currents in the mammalian central nervous system. Owing to their high sequence homology, the two channel subtypes share similar pharmacological properties, and at high doses classic calcium channel blockers, such as dihydropyridines, phenylalkylamines and benzothiazepines, do not discriminate between the two channel subtypes. Recent progress in treating Parkinson’s disease (PD) was marked by the discovery of synthetic compound 8, which was reported to be a highly selective inhibitor of the CaV1.3 L-type calcium channels (LTCC). However, despite a previously reported IC50 of ~24 μM, in our hands inhibition of the full-length CaV1.342 by compound 8 at 50 μM reaches a maximum of 45%. Moreover, we find that the selectivity of compound 8 towards CaV1.3 relative to CaV1.2B15 channels is greatly influenced by the β-subunit type and its splice isoform variants.
Similar content being viewed by others
Introduction
Parkinson’s disease (PD) is a movement disorder arising from the degeneration of dopaminergic neurons in the substantia nigra pars compacta (SNc). Although mutations of several genes have been associated with PD1, 95% of PD cases are idiopathic. The over-reliance of CaV1.3 current for pacemaking in the adult SNc neurons was reported to aggravate mitochondrial oxidative stress2, and consequently enhance the susceptibility of these neurons towards toxins such as MPTP (1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine) and rotenone3. Significantly, pharmacological blockade or genetic deletion of CaV1.3 channels confers protection against toxin induced neuronal damage3. Interestingly, population studies also revealed significant reduction in the risk of developing PD among hypertensive subjects receiving dihydropyridines (DHPs), classical blockers of L-type calcium channels4,5.
Voltage-gated calcium channels CaV1.2 and CaV1.3 underlie the majority of L-type calcium currents in the central nervous system. While CaV1.3 channels contribute only 20% of the total L-type currents in the central nervous system, the use of non-selective DHPs that also inhibits CaV1.2 channels could have profound neuro-physiological consequences6. In addition, neuronal transcripts of CaV1.3 channels display extensive alternative splicing patterns, generating splice variants with different biophysical and pharmacological properties7,8,9. The CaV1.342a splice variant with a truncated C terminus displayed attenuated sensitivity towards DHP as compared with the long-form CaV1.342 channels8. Tissue-selective expression of various CaV1.3 splice variants would therefore require different dosages for effective inhibition of the CaV1.3 currents.
Recently, Kang et al.10 reported the identification of 1-(3-chlorophenethyl)-3-cyclopentylpyrimidine-2,4,6(1H,3H,5H)-trione, also known as compound 8 as a pharmacological blocker highly selective for CaV1.3 (IC50=24.3±0.7 μM) over CaV1.2 channels. In the current study, we evaluated compound 8 for its activity against different CaV1.3 channel splice isoforms. Unexpectedly, initial heterologous expression in human embryonic kidney 293 (HEK293) cells co-transfected with β2a-subunit revealed that compound 8 inhibited CaV1.2 more than either CaV1.342 or CaV1.342a channels. Replacing β2a-subunit with β1-, β3- or β4-subunit on the other hand yielded results that showed modest selective inhibition of compound 8 against CaV1.342 over CaV1.2B15 channels. However, there was clearly no selective inhibition of compound 8 against CaV1.342a and CaV1.2 channels in the presence of anyone of the other three β-subunits. Based on the existing data, we conclude that the CaV1.3-selective inhibition by compound 8 is modest and is highly dependent on the composition of the CaV1.3 splice variant in association with a particular type of β-subunit.
Results
Compound 8 is not selective against CaV1.3 with β2a-subunit
Compounds 1, 8 and PYT (1,3-bis(4-chlorophenethyl)pyrimidine-2,4,6(1H, 3H, 5H)-trione; Fig. 1) were synthesized according to the procedure reported by Kang. et al.10 but with slight modifications (see Methods section). It has been reported that the newly discovered compound 8 inhibited ~30 and 60% of CaV1.3 current at concentrations of 5 and 50 μM, respectively, whereas CaV1.2 channels were weakly responsive as 50 μM of compound 8 inhibited only close to 10% of its peak current10.
We have recently discovered that alternative splicing at the C terminus regulated the sensitivity of CaV1.3 channels towards DHPs; while the long-form CaV1.342 channel exhibited high sensitivity towards DHP; truncation of the C terminus immediately after the IQ domain via alternate use of exon 42a yielded the less sensitive CaV1.342a channel8. To determine whether the compound 8 may also have differential effects on different C-terminal splice forms, we first tested the sensitivity of rat CaV1.342 and CaV1.342a. In the presence of β2a contransfected with the CaV1.3 channels, the channel isoforms displayed very little run-down with repeated 1 s square pulse depolarization to test potential of 10 mV from a holding potential of −70 mV at the frequency of 0.05 Hz (Figs 2b and 3b). Surprisingly, 5 μM of compound 8 failed to significantly inhibit the peak Ca2+ current (ICa) of either CaV1.342 or CaV1.342a (Figs 2 and 3) as compared with the untreated controls. Moreover, 50 μM of compound 8 only inhibited 29.51±3.01 and 23.57±2.14% of the peak ICa of CaV1.342 or CaV1.342a, respectively (Figs 2 and 3). In addition, CaV1.342 channels were blocked to a similar level with compound 8 obtained from an additional source (Supplementary Fig. 1). In comparison, 78.85±2.63% of CaV1.342 current and 68.14±3.43% of CaV1.342a current could be robustly inhibited by 5 μM of nimodipine (Figs 2 and 3). As compound 8 has been reported to have little effect on CaV1.2 current, we tested its inhibition on the rat CaV1.2B15 channels11. As compared with the CaV1.3, a slightly enhanced run-down effect (10.14±3.98%) was observed for CaV1.2B15 channels (Fig. 4b). However, 34.97±4.39 and 44.03±4.67% of CaV1.2B15 current could be inhibited by 5 and 50 μM of compound 8, respectively, indicating a stronger inhibitory effect of compound 8 on CaV1.2 than CaV1.3 channels. As expected, 80.66±2.82% of CaV1.2B15 current was blocked by 5 μM nimodipine (Fig. 4).
(a) Representative traces of CaV1.342 currents recorded by single 1 s square pulse to test potential of 10 mV from holding potential of −70 mV for 25 sweeps with sweep interval of 20 s. Only the first three untreated (black) and last three treated (red) traces are shown for each treatment groups. Displayed are the first 100 ms of each recording trace. (b) Averaged diary plot of effects of either control, 5 μM 8, 50 μM 8 or 5 μM Nimo on CaV1.342 peak currents. The number of cells analysed are indicated in the parenthesis. The drugs were added after the three stable sweeps. (c) Population data of the % peak current inhibition at the 25th sweep normalized against the first sweep conferred by either 5 μM 8, 50 μM 8 or 5 μM Nimo as compared with the control. NS, non-significant. ***P<0.001 (Student’s unpaired t-test). Alternatively, P<0.001 among all the treatment groups (one-way analysis of variance and Bonferroni’s test). The number of cells analysed is indicated in b. The data for each condition were collected from two to three transfections.
(a) Representative traces of CaV1.342a currents, format as in Fig. 2a. (b) Averaged diary plot of effects either control, 5 μM 8, 50 μM 8 or 5 μM Nimo on CaV1.342a peak currents, format as in Fig. 2b. (c) Population data of the % peak current inhibition at the 25th sweep normalized against the first sweep conferred by either 5 μM 8, 50 μM 8 or 5 μM Nimo as compared with the control. NS, non-significant. ***P<0.001 (Student’s unpaired t-test). Alternatively, P<0.001 among all the treatment groups (one-way analysis of variance and Bonferroni’s test). The number of cells analysed is indicated in b. The data for each condition were collected from two to three transfections.
(a) Representative traces of CaV1.2B15 currents, format as in Fig. 2a. (b) Averaged diary plot of effects of either control, 5 μM 8, 50 μM 8 or 5 μM Nimo on CaV1.2B15 peak currents, format as in Fig. 2b. (c) Population data of the % peak current inhibition at the 25th sweep normalized against the first sweep conferred by either 5 μM 8, 50 μM 8 or 5 μM Nimo as compared with the control. ***P<0.001. (Student’s unpaired t-test) Alternatively, P<0.001 among all the treatment groups (one-way analysis of variance and Bonferroni’s test). The number of cells analysed is indicated in b. The data for each condition were collected from two to three transfections.
In addition, we evaluated the inhibitory activities of PYT and compound 1 against CaV1.3 and CaV1.2 channels10. Kang et al.10 reported that PYT was the original scaffold that displayed an eightfold selectivity for CaV1.3, whereas compound 1 was one of the PYT analogues that was 28 times more selective for CaV1.3 channels. However, in our experiments, 5 μM of PYT and compound 1 did not significantly inhibit the peak ICa of CaV1.342 (Supplementary Fig. 2). In addition, 5 μM of PYT inhibited 19.90±2.59% of CaV1.342a current, whereas 5 μM of compound 1 had no effect on CaV1.342a channels (Supplementary Fig. 3). In comparison, PYT and compound 1 also appeared to be more selective for CaV1.2B15 showing 43.52±4.83% and 31.69±4.83% inhibition, respectively, (Supplementary Fig. 4). The effect could not be a result of current run-down as little current decay was observed for the untreated CaV1.2 current upon prolonged pulses, and the current density of the recorded cells under all treatment groups were not significantly different in the study (Supplementary Fig. 5).
Furthermore, we noted that the use of the original rat CaV1.342 (ref. 12) (Genbank accession no. AF370010) by Kang et al.10 contained three mutations, including G244S, A1104V and V2123A, that have been shown to drastically alter both the biophysical and pharmacological properties of the channel9,13,14. To test whether the use of uncorrected CaV1.342 channel, named here as CaV1.342_UC, could account for the lack of selectivity of compound 8 against CaV1.3 channels in the presence of β2a-subunit, we measured the sensitivity of CaV1.342_UC to either 5 and 50 μM compound 8 or 5 μM nimodipine with instead shorter 100 ms depolarizing pulse that was used by Kang et al.10 While 5 μM compound 8 has little effect on CaV1.342_UC channels as compared with control treatment, only 15.75±3.25% of the peak current could be inhibited by 50 μM compound 8, and expectedly 73.10±3.48% of the current was blocked by 5 μM nimodipine (Fig. 5). Hence, it was consistent that in the presence of β2a-subunit, CaV1.2 displayed higher sensitivity to compound 8 as compared with CaV1.3 channels.
(a) Representative traces of uncorrected CaV1.242_UC currents, format as in Fig. 2a. The current was recorded by single square pulse from holding of −70 to 10 mV for over 100 ms with sweep interval of 20 s. (b) Averaged diary plot of effects of either control, 5 μM 8, 50 μM 8 or 5 μM Nimo on CaV1.342_UC peak currents, format as in Fig. 2b. (c) Population data of the % peak current inhibition at the 28th sweep normalized against the first sweep conferred by either 5 μM 8, 50 μM 8 or 5 μM Nimo as compared with the control. *P<0.05, ***P<0.001 (Student’s unpaired t-test). Alternatively, P<0.001 among all the treatment groups (one-way analysis of variance and Bonferroni’s test). The number of cells analysed is indicated in b. The data for each condition were collected from two to three transfections.
β-subunit influences compound 8 selectivity
Although it has been shown that the presence of different β-subunits did not overtly affect the sensitivity of L-type channels towards DHP15, the use of different β-subunits such as β3 in Kang et al.10 and β2a in the current study might account for the opposite selectivity of compound 8 on CaV1.2 and CaV1.3 channels observed in these two studies. To test this possibility, we first measured the effect of 50 μM compound 8 on CaV1.342, CaV1.342_UC, CaV1.2B15 and CaV1.342a channels co-transfected with β3-subunit. Interestingly, while ~40% of the peak ICa of CaV1.342 and the uncorrected CaV1.342_UC were similarly inhibited by 50 μM compound 8, CaV1.2B15 and CaV1.342a channels displayed a slightly but significantly weaker sensitivity in comparison with CaV1.342 channels as 23.47±2.60 and 29.05±2.48% of respective peak currents were inhibited (Fig. 6 and Supplementary Fig. 6). Additional experiments done using either β1- and β4-subunits produced results that demonstrated enhanced inhibitory effect of compound 8 on CaV1.342 as compared with CaV1.342_UC, CaV1.2B15 and CaV1.342a channels. However, CaV1.2B15 and CaV1.342a channels were inhibited to similar level by 50 μM compound 8 in the presence of β1-, β3- and β4-subunits (Fig. 6 and Supplementary Fig. 6). Significantly, in the presence of β2a, CaV1.2B15 still displayed higher sensitivity as compared with CaV1.342, CaV1.342_UC and CaV1.342a, even when the currents were repeatedly recorded with a shorter100-ms depolarizing square pulse (Fig. 6 and Supplementary Fig. 6). Finally, we performed analysis of the correlation of the % of inhibition with the current density for each of the CaV1.342, CaV1.342_UC, CaV1.2B15, and CaV1.342a channels. Only weak correlations were observed as indicated by the following R2 values: 0.0121 for CaV1.342, 0.0859 for CaV1.342_UC, 0.2439 for CaV1.2B15 and 0.2047 for CaV1.342a. Therefore, the inhibitory effect of compound 8 on the CaV1.2 and CaV1.3 channels are not influenced by the amplitudes of the currents. (Supplementary Fig. 7).
(a) Averaged diary plot of effects of 50 μM 8 on CaV1.342 peak currents in the presence of β1-, β2a-, β3- and β4-subunit. The current was recorded by single square pulse from holding of −70 to 10 mV for over 100 ms with sweep interval of 20 s. (b–d) Averaged diary plot of effects of 50 μM 8 on the peak currents of CaV1.342_UC, CaV1.2B15 and CaV1.342a, respectively, in the presence of different β-subunits, format as in a. (e) Comparison of the % peak current inhibition at the 28th sweep normalized against the first sweep conferred by 50 μM 8 for CaV1.342, CaV1.342_UC, CaV1.2B15, CaV1.342a in the presence of different β-subunits. Within each β-subunit, the % inhibitions of CaV1.342_UC, CaV1.2B15, CaV1.342a were compared with that of CaV1.342. NS, non-significant, *P<0.05, **P<0.01, ***P<0.001 (Student’s unpaired t-test). Alternatively, P<0.001 within each group (one-way analysis of variance and Bonferroni’s test). The number of cells analysed is indicated in b–d. The data for each condition were collected from two to three transfections.
Discussion
PD is a debilitating movement disorder currently with no cure. The constant Ca2+ influx via the CaV1.3 channels enhances mitochondrial oxidative stress that could contribute towards the pathogenesis of PD. The presence of other possible pacemaking current underlied by hyperpolarization-activated and cyclic nucleotide-gated cation (HCN) channel suggested that it might be feasible to block CaV1.3 current without grossly affecting the normal physiological functions of SNc neurons3. The availability of a CaV1.3 channel-specific antagonist that could eventually replace non-selective L-type blockers such as DHPs would therefore be ideal for the therapeutic management of PD.
In contrast to the IC50 of 24.3 ±0.7 μM as determined using patch-clamp electrophysiology by Kang et al.10, our initial data with β2a-subunits revealed that the percentage inhibition of compound 8 on Cav1.3 channels at 50 μM was only 30% while at 5 μM no significant inhibition was observed. In contrast to the published report, the inhibition of Cav1.2 channels at 50 and 5 μM were 44% and 35%, respectively, indicating selectivity of compound 8 against Cav1.2 channels.
The initial failure to observe any selectivity of compound 8 in inhibiting CaV1.3 channels led us to investigate the effect of compound 8 with other β-subunits. However, while the CaV1.342 current was indeed more sensitive than Cav1.2 in the presence of β1-, β3- and β4-subunits, only 35–45% of the its peak currents could be blocked by 50 μM compound 8, and the percentage of inhibition on CaV1.2B15 channels was a modest 10–15% less as compared with CaV1.342 channels.
To complicate the story further, the short-form CaV1.342a channels displayed similar level of sensitivity as compared with CaV1.2B15 channels with either β1-, β3- or β4-subunit co-transfected. The CaV1.342a splice variant accounts for ~30% of the total CaV1.3 transcripts in the substantial nigra region7. While the roles of different CaV1.3 splice variants in neurodegeneration of SNc neurons in the pathogenesis of PD awaits further clarification, the larger current density and more hyperpolarized-shifted I-V relationship implied a greater involvement of CaV1.342a current in driving the pacemaking acitivity in the SNc neurons as compared with the full-length CaV1.342 channels8.
In summary, the newly reported compound 8 is not a potent blocker of CaV1.3 channels as compared with the classical L-type blockers such as the DHPs. The selectivity of compound 8 on CaV1.342 over CaV1.2B15 channels could be influenced strongly by the presence of various β-subunits and the compound 8 was not selective for CaV1.342a over CaV1.2B15 channels in the presence of β1-, β3- or β4-subunit. Instead, in the presence of β2a, compound 8 strongly inhibits CaV1.2B15 channels over all the CaV1.3 splice variants tested. Given the differential distribution of β-subunits and the varied expression levels of Cav1.3 channel variants across various neuronal types, brain regions and organs, the use of compound 8 as a CaV1.3-selective antagonist needs to be further clarified. Nonetheless, the quest for discovering a highly selective and potent compound targeting CaV1.3 channels is a highly worthwhile goal.
Methods
General synthesis information
All commercially available reagents were bought from Sigma-Aldrich and Alfa Aesar, and used without further purification. Thin layer chromatography was performed using pre-coated plate (Merck silica gel 60, F254) and visualized with ultraviolet (UV) light. Flash column chromatography was carried out on Merck silica gel (230–400 mesh). 1H and 13C nuclear magnetic resonance (NMR) spectrums were recorded on Bruker ACF300 (300 MHz) or AMX 500 (500 MHz) spectrometer at 298 K, respectively. All J values are reported in Hz and chemical shift (δ) reported in p.p.m. relative to tetramethylsilane. Abbreviations for signal multiplicities are as follow: singlet (s), doublet (d), triplet (t) and multiplet (m). Mass spectra were determined by electrospray ionization (ESI) on Finnigan TSQ 7000. High-performance liquid chromatography was performed using a Shimadzu LCMS-IT-TOF system with a Phenomenex Luma C18 column (50 × 3.0 mm, 5 μm) using acetonitrile and 0.1% trifluoroacetic acid in water. The mobile phase has a flow rate of 5 ml min−1 with gradient flow of acetonitrile increasing from 5 to 90%. UV/visible detector was set at a wavelength of 254 nm.
General synthetic procedure for compounds 1, 8 and PYT
Compounds 1, 8 and PYT were synthesized according to the procedure reported by Kang. et al.10 but with slight modifications (Scheme 1). In brief, a solution of isocyanate (1 mmol) in dichloromethane (10 ml), the respective amine (1 mmol) was added and allowed to stir at room temperature overnight. The mixture was then diluted with dichloromethane (8 ml) and malonyl chloride (1.1 mmol) was added dropwise to the mixture at room temperature under vigorous stirring. Upon reaction completion (monitored by thin layer chromatography), the reaction mixture was concentrated and purified via flash column chromatography using hexane: ethyl acetate(3:1) as eluent to afford the final product. Compounds 1, 8 and PYT were characterized via 1H and 13C NMR, mass spectrometry (ESI) and melting point determination (Supplementary Figs 8,9 and 10). The characterization data were comparable to those reported by Kang et al.10 Furthermore, the purity of each compound was determined by HPLC (Supplementary Figs 11 and 12), and the compounds were found to have a purity value of over 98%.
1-(4-chlorophenethyl)-3-cyclohexylpyrimidine-2,4,6(1H,3H,5H)-trione (1)
White powder; 1H NMR spectrum (CDCl3, 300 MHz): δ 7.21(d, J=8.4 Hz, 2H), 7.12(d, J=8.4 Hz, 2H), 4.54(m, 1H), 3.99(m, 2H) 3.55(s, 1H), 2.81(m, 2H), 2.17(m, 2H), 1.79(m, 2H), 1.58(m, 3H), 1.32(m, 3H); 13C NMR (CDCl3, 75 MHz): δ 164.59, 164.41, 150.92, 136.16, 132.33, 130.13, 128.48, 55.12, 42.50, 40.02, 33.15, 28.88, 26.11, 24.93; melting point: 146.6–147.5 °C (146–148 °C; ref. 11); HRMS(ESI) calculated for C18H21ClN2O3[M-H]-: 347.1168; found, 347.1168.
1-(3-chlorophenethyl)-3-cyclopentylpyrimidine-2,4,6(1H, 3H, 5H)-trione (8)
White solid; 1H NMR spectrum (CDCl3, 500 MHz): δ 7.23-7.18(m, 3H), 7.12(d, J= 4.14 Hz, 1H), 5.12(m, 1H), 4.05(m, 2H), 3.60(s, 2H), 2.86(m, 2H), 1.92(m, 4H), 1.84(m, 2H), 1.57(m, 2H); 13C NMR spectrum (CDCl3, 125 MHz): δ 164.68, 164.40, 150.79, 139.77, 134.18, 129.72, 128.96, 127.03, 126.81, 54.24, 42.48, 40.00, 33.55, 28.59, 25.42; melting point: 131.3-131.8 °C (131-132 °C; ref. 11); HRMS(ESI) calculated for C17H19ClN2O3[M-H]-: 333.1011; found, 333.1007.
1,3-bis(4-chlorophenethyl)pyrimidine-2,4,6(1H, 3H, 5H)-trione (PYT)
White powder; 1H NMR (CDCl3, 500 MHz): δ 7.28(d, J=8.15 Hz, 4H), 7.17(d, J=8.1 Hz, 4H), 4.06(t, J=7.7 Hz, 4H), 3.60(s, 2H) 2.84(t, J=7.95 Hz, 4H); 13C NMR (CDCl3, 125 MHz): δ 164.18, 150.98, 136.07, 132.57, 130.23, 128.67, 42.77, 39.46, 33.26; melting point: 171.8-172.9 °C; HRMS(ESI) calculated for C20H18Cl2N2O3[M-H]-:403.0622; found, 403.0612.
Electrophysiological recordings and data analysis
Whole-cell patch-clamp electrophysiological recordings were used to characterize the recombinant rat CaV1.342 and of CaV1.342a channels8, and rat CaV1.2B15 channel9. ICa currents were recorded from transiently transfected mammalian HEK293 cells at room temperature with calcium phosphate method16,17. Outward IK currents were blocked by Cs+ in the internal and external solutions. Cells were transiently transfected with the respective CaV1.3 and CaV1.2 constructs with rat β2a-subunit and rat α2δ-subunit using standard calcium phosphate transfection method. For whole-cell patch-clamp recording, the internal solution (patch-pipette solution) contained the following (in mM): 138 Cs-MeSO3, 5 CsCl, 5.0 EGTA, 10 HEPES and 1 MgCl2, and 2 mg ml−1 Mg–ATP, pH 7.3 (adjusted with CsOH), and 290 mOsm with glucose. The external solution contained the following (in mM): 109 NaCl, 10 CaCl2, 1 MgCl2, 20 CsCl and 10 HEPES, (pH adjusted to 7.4 with CsOH and osmolality to 290 glucose). Pipettes of resistance 1.5–2 MΩ were used. Whole-cell currents, obtained under voltage clamp with an Axopatch 200B amplifier (Molecular Devices, Union City, CA), were filtered at 1–5 kHz and sampled at 5–50 kHz, and the series resistance was typically <5 MΩ after >80% compensation. A P/4 protocol was used to subtract on-line the leak and capacitive transients.
The currents were recorded by single square pulse from holding of −70 to 10 mV for over 1 s or 100 ms with sweep interval of 20 s. Data were acquired using the software pClamp9 (Molecular Devices), and analysed and fitted using GraphPad Prism V software (San Diego, CA) and Microsoft (Seattle, WA) Excel. Data are expressed as mean values±s.e.m.
Drug preparation
Stock solutions were prepared by dissolving compound PYT, 1, 8 and nimodipine (RBI) in DMSO to make a 100-mM stock solution and stored at −20 °C in the dark. Respective concentrations were freshly prepared in the bath solution from stock, and perfused (1 ml per min) into the whole recording chamber by gravity during current recording. The cell selected for patch-clamp recording were positioned as close to the outlet as possible. The external solutions were protected from light throughout the experiment.
Additional information
How to cite this article: Huang, H. et al. Modest CaV1.342-selective inhibition by compound 8 is β-subunit dependent. Nat. Commun. 5:4481 doi: 10.1038/ncomms5481 (2014).
References
Lesage, S. & Brice, A. Parkinson's disease: from monogenic forms to genetic susceptibility factors. Hum. Mol. Genet. 18, R48–R59 (2009).
Guzman, J. N. et al. Oxidant stress evoked by pacemaking in dopaminergic neurons is attenuated by DJ-1. Nature 468, 696–700 (2010).
Chan, C. S. et al. 'Rejuvenation' protects neurons in mouse models of Parkinson's disease. Nature 447, 1081–1086 (2007).
Ascherio, A. & Tanner, C. M. Use of antihypertensives and the risk of Parkinson disease. Neurology 72, 578–579 (2009).
Ritz, B. et al. L-type calcium channel blockers and Parkinson disease in Denmark. Ann. Neurol. 67, 600–606 (2010).
Sinnegger-Brauns, M. J. et al. Isoform-specific regulation of mood behavior and pancreatic beta cell and cardiovascular function by L-type Ca 2+ channels. J. Clin. Invest. 113, 1430–1439 (2004).
Bock, G. et al. Functional properties of a newly identified C-terminal splice variant of Cav1.3 L-type Ca2+ channels. J. Biol. Chem. 286, 42736–42748 (2011).
Huang, H., Yu, D. & Soong, T. W. C-terminal alternative splicing of CaV1.3 channels distinctively modulates their dihydropyridine sensitivity. Mol. Pharmacol. 84, 643–653 (2013).
Tan, B. Z. et al. Functional characterization of alternative splicing in the C terminus of L-type CaV1.3 channels. J. Biol. Chem. 286, 42725–42735 (2011).
Kang, S. et al. CaV1.3-selective L-type calcium channel antagonists as potential new therapeutics for Parkinson's disease. Nat. Commun. 3, 1146 (2012).
Tang, Z. Z., Hong, X., Wang, J. & Soong, T. W. Signature combinatorial splicing profiles of rat cardiac- and smooth-muscle Cav1.2 channels with distinct biophysical properties. Cell Calcium 41, 417–428 (2007).
Xu, W. & Lipscombe, D. Neuronal Ca(V)1.3alpha(1) L-type channels activate at relatively hyperpolarized membrane potentials and are incompletely inhibited by dihydropyridines. J. Neurosci. 21, 5944–5951 (2001).
Huang, H. et al. RNA editing of the IQ domain in Ca(v)1.3 channels modulates their Ca(2)(+)-dependent inactivation. Neuron 73, 304–316 (2012).
Lieb, A., Scharinger, A., Sartori, S., Sinnegger-Brauns, M. J. & Striessnig, J. Structural determinants of CaV1.3 L-type calcium channel gating. Channels (Austin) 6, 197–205 (2012).
Berjukow, S., Marksteiner, R., Gapp, F., Sinnegger, M. J. & Hering, S. Molecular mechanism of calcium channel block by isradipine. Role of a drug-induced inactivated channel conformation. J. Biol. Chem. 275, 22114–22120 (2000).
Patil, P. G., Brody, D. L. & Yue, D. T. Preferential closed-state inactivation of neuronal calcium channels. Neuron 20, 1027–1038 (1998).
Peterson, B. Z., DeMaria, C. D., Adelman, J. P. & Yue, D. T. Calmodulin is the Ca2+ sensor for Ca2+ -dependent inactivation of L-type calcium channels. Neuron 22, 549–558 (1999).
Acknowledgements
We would like to thank Dr Joerg Striessnig (Medical School, University of Innsbruck, Austria) for the additional source of compound 8. The work is supported by Singapore Biomedical Research Council and the National Medical Research Council.
Author information
Authors and Affiliations
Contributions
H.H. designed and performed the patch-clamp experiments and wrote the initial draft of the manuscript; C.Y.N synthesized all compounds; Y.D. and J.Z. participated in the patch-clamp experiment; and Y.L and T.W.S supervised the experiments and edited the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Supplementary Information
Supplementary Figures 1-12 (PDF 1047 kb)
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-sa/4.0/
About this article
Cite this article
Huang, H., Ng, C., Yu, D. et al. Modest CaV1.342-selective inhibition by compound 8 is β-subunit dependent. Nat Commun 5, 4481 (2014). https://doi.org/10.1038/ncomms5481
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/ncomms5481
This article is cited by
-
Selective blockade of Cav1.2 (α1C) versus Cav1.3 (α1D) L-type calcium channels by the black mamba toxin calciseptine
Nature Communications (2024)
-
Structural basis for pore blockade of human voltage-gated calcium channel Cav1.3 by motion sickness drug cinnarizine
Cell Research (2022)
-
Targeting voltage-gated calcium channels in neurological and psychiatric diseases
Nature Reviews Drug Discovery (2016)
-
Regulation of aldosterone secretion by Cav1.3
Scientific Reports (2016)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.