Abstract
Sepsis caused by Gram-positive bacterial pathogens is a major fatal disease but its molecular basis remains elusive. Toll-like receptor 2 (TLR2) has been implicated in the orchestration of inflammation and sepsis but its role appears to vary for different pathogen species and clones. Accordingly, Staphylococcus aureus clinical isolates differ substantially in their capacity to activate TLR2. Here we show that strong TLR2 stimulation depends on high-level production of phenol-soluble modulin (PSM) peptides in response to the global virulence activator Agr. PSMs are required for mobilizing lipoproteins, the TLR2 agonists, from the staphylococcal cytoplasmic membrane. Notably, the course of sepsis caused by PSM-deficient S. aureus is similar in wild-type and TLR2-deficient mice, but TLR2 is required for protection of mice against PSM-producing S. aureus. Thus, a crucial role of TLR2 depends on agonist release by bacterial surfactants. Modulation of this process may lead to new therapeutic strategies against Gram-positive infections.
Similar content being viewed by others
Introduction
Sepsis is a severe syndrome of increasing frequency with a very high mortality rate1. Systemic inflammation initiated by conserved microbe-associated molecular pattern (MAMP) molecules from circulating bacteria can lead to septic shock and organ failure. Toll-like receptor 4 (TLR4) and lipopolysaccharide, its microbial agonist, are long known as major factors in infections and sepsis caused by Gram-negative bacteria2,3. In contrast, TLR2 activates immune cells in response to bacterial lipoproteins and has been considered as a major factor in Gram-positive sepsis4,5. Certain alleles in the TLR2 pathway associate with increased susceptibility and severity of sepsis caused by major Gram-positive pathogens such as Staphylococcus aureus6,7. However, the role of TLR2 in sepsis is much more elusive than that of TLR4 because TLR2 appears to have ambivalent roles and its importance seems to vary for different pathogens for unknown reasons8,9,10. In particular, it has remained elusive under which conditions TLR2 may affect the course of infection and elicit protective or even detrimental responses5,11,12. These unsolved questions have impeded the use of TLR2 as a target for immunomodulatory drugs12,13.
A major percentage of bacteremia and sepsis cases is caused by S. aureus and these infections are often particularly difficult to treat because of the enormous burden of antibiotic resistance in methicillin-resistant S. aureus (MRSA)14. The extraordinary capacity of S. aureus to cause massive inflammation and withstand host defense can be attributed to the release of pro-inflammatory MAMPs and leukocyte-damaging toxins15,16. TLR2-activating lipoproteins, major staphylococcal MAMPs, are attached to bacterial membranes via a diacylglycerol moiety, which is connected to an N-terminal cysteine residue of the lipoprotein via a thioether bond by the lipoprotein diacylglyceryl transferase (Lgt)17. In addition, many bacteria modify the lipoprotein N-terminus with a third fatty acid18. Many lipoproteins from Gram-positive bacteria are components of ABC importers such as the staphylococcal siderophor uptake system SitC and are upregulated under nutrient-limited conditions19,20. Inactivation of lgt abrogates the post-translational modification of pre-lipoproteins and the capacity of S. aureus to stimulate TLR221. In addition to MAMPs a large inventory of toxins compromizing the function of leukocytes or other host cells contribute to the aggressive behaviour of S. aureus22.
Most of the S. aureus virulence factors are controlled by the quorum-sensing regulatory Agr system, which is specific for staphylococci23. AgrA, the DNA-binding regulator of the Agr system controls directly expression of phenol-soluble modulin (PSM) peptides, which shape S. aureus infections in several ways24,25. S. aureus usually produces four co-transcribed short PSMα peptides (20–22 amino acids), two longer PSMβ peptides, and the PSMα-related δ-toxin, which is encoded in RNAIII of the Agr system26. PSMs are α-helical and have surfactant-like properties, which are responsible for the potent cytolytic activity of PSMs towards leukocytes and other host cells24. Whereas this activity depends on high (micromolar) concentrations PSMs can stimulate and activate leukocytes in the nanomolar range because they bind to the G-protein coupled formylpeptide receptor 2 (FPR2) thereby representing chemotactic MAMPs27,28. Staphylococcal species and strains differ largely in the levels of PSM expression, which appears to affect the virulence of the producing strain29. However, how important PSMs may be for the induction of inflammation in the context of other MAMPs such as lipoproteins has remained unknown.
Here we analyse how staphylococcal strains differ in their capacity to activate TLR2 and report that PSMs are crucial for the proinflammatory potential of S. aureus because they are required for the release of lipoproteins from bacterial cytoplasmic membranes. Accordingly, PSMs have a strong impact on the severity of sepsis, and TLR2 has an important role in systemic S. aureus infections only for PSM-producing strains.
Results
TLR2 activation depends on an active Agr system
S. aureus strains differ in their ability to stimulate TLR2. Some strains are almost unable to trigger TLR2 even in the presence of lipoproteins suggesting that other factors besides lipoproteins must have a role5,11. Accordingly, we have recently found that S. aureus strain SA113 and its isogenic lipoprotein-deficient mutant (Δlgt) did not differ much in their capacities to cause sepsis in wild-type and TLR2-deficient mice11. In order to elucidate if and under which conditions TLR2 may be crucial in staphylococcal infections we compared different Gram-positive pathogens including several S. aureus strains for their capacity to stimulate TLR2. In line with our previous finding11, SA113 extracellular factors in culture filtrates elicited only very weak interleukin (IL)-8 release in TLR2-transfected human embryonic kidney 293 (HEK-TLR2) cells (Fig. 1a). Similar observations were made with other Gram-positive pathogens such as enterococci, Streptococcus pyogenes and Listeria monocytogenes. When different MRSA strains were compared for their capacity to stimulate IL-8, it became obvious that hospital-associated MRSA (HA-MRSA) such as strains COL, Mu50 and N315 behaved like SA113 while highly pathogenic community-associated MRSA (CA-MRSA) such as USA300 and USA400 (ref. 30) induced secretion of approximately tenfold higher amounts of IL-8, indicating that strong TLR2 stimulation is not a constant species-specific phenomenon but differs profoundly between individual strains and may be associated with high staphylococcal virulence (Fig. 1b). Since CA-MRSA are distinguished from hospital-associated MRSA and SA113 by particularly strong activity of the global virulence regulator Agr31, we compared the TLR2-stimulating capacities of CA-MRSA wild-type and isogenic Agr mutants. The function or dysfunction of the Agr -system in the various strains was confirmed by quantitative real-time PCR (qRT–PCR) of the Agr-dependent RNAIII (Fig. 1i, Supplementary Fig. 1). Of note, inactivation of Agr in USA300 and USA400 resulted in drastically reduced capacities to induce IL-8 release in HEK-TLR2 cells or human polymorphonuclear neutrophil granulocytes (PMN) and tumour-necrosis factor (TNF)-α, IL-6 and IL-1β release in human peripheral blood mononuclear cells (PBMC), which demonstrated that the capacity of S. aureus to stimulate TLR2 depends heavily on an active Agr system (Fig. 1b-f, Supplementary Fig. 2). USA300 extracellular factors in culture filtrates stimulated HEK-TLR2 cells in a dose-dependent manner with no cytotoxic side effects at the used concentrations (Fig. 1g,h). In contrast, HEK cells not expressing TLR2 did not respond to USA300 culture filtrates confirming that the Agr-dependent IL-8 release in HEK-TLR2 cells depends on TLR2 (Supplementary Fig. 3c).
Culture filtrates of S. aureus strains with strong Agr activity but not with weakly active or no Agr have potent capacities to induce either IL-8 in HEK-TLR2 cells (a,b) and in PMN (c), or TNF-α, IL-6 and IL-1β in PBMCs (d–f). The synthetic lipopeptide Pam2CSK4 and TSB medium were used as positive and negative controls, respectively. Expression of TLR2 in HEK cells leads to dose-dependent IL-8 induction by USA300 culture filtrates (g). Culture filtrates are not cytotoxic to HEK cells at indicated dilutions used for stimulation (h). Agr activity of S. aureus strains was measured by qRT–PCR of RNAIII expression (i). Data represent means +/− s.e.m. of at least three independent experiments. *P<0.05, **P<0.01, ***P<0.001; ****P<0.0001 significantly different versus USA300 wild-type (b–f) as calculated by Student’s t test.
PSM peptides are necessary for S. aureus TLR2 stimulation
Because Agr has a particular impact on expression of pro-inflammatory PSM peptides25 the impact of PSM genes on the TLR2-stimulating capacity of S. aureus was analysed. A USA300 mutant lacking each of the three PSM gene clusters encoding PSMα, PSMβ, and δ-toxin/Hld peptides32 behaved like Agr or lgt mutants with hardly detectable capacities to induce IL-8. PSMα peptides, the most cytolytic PSMs24, had the most pronounced impact on TLR2 activation, whereas inactivation of PSMβ peptides or δ-toxin did not affect the response of HEK-TLR2 to S. aureus. (Fig. 2a). Recombinant expression of the four PSMα peptides in Agr-deficient S. aureus strains such as SA113 and N315 or the PSMα-deficient USA300 Δα mutant led to markedly increased IL-8 induction in HEK-TLR2 cells confirming that PSMα peptide expression is crucial for TLR2 stimulation by S. aureus culture filtrates (Fig. 2b). Complementation of PSM- and lipopeptide-deficient mutants with plasmid-encoded copies of the deleted genes showed that both are required for TLR2-stimulating activity (Fig. 2c–e). Similar observations were made with IL-8, TNF-α, IL-6 and IL-1β induction in human PMNs and PBMCs, with MIP-2, mTNFα or mIL-6 induction in mouse macrophages, or with IL-8 induction in HEK-TLR1/2 or HEK-TLR2/6, indicating that Agr-regulated PSMs may have essential roles in TLR2-dependent S. aureus cytokine induction and inflammation (Figs 3 and 4, Supplementary Fig. 3).
Inactivation of PSMα genes in S. aureus USA300 has a similar impact on IL-8 induction in HEK-TLR2 cells as deletion of the lipoprotein diacylglyceryl transferase gene (lgt) (a) and this phenotype can be complemented by recombinant expression of the PSMα cluster (b). Stimulation of HEK-TLR2 with live S. aureus leads to decreased IL-8 induction by the PSM mutant compared with USA300 wild-type, which can be restored by PSMα expression (c). The capacity of S. aureus Δlgt to stimulate IL-8 release in HEK-TLR2 cells can be restored by transformation with an lgt-expressing plasmid (d). A USA300 mutant lacking PSMs and Lgt requires complementation with both, PSM genes and lgt to regain TLR2-stimulating activity (e). The synthetic lipopeptide Pam2CSK4 and TSB medium were used as positive and negative controls, respectively. Data represent means +/− s.e.m. of at least three independent experiments. ***P<0.001; ****P<0.0001 significantly different versus USA300 wild-type (a,c,d), pTXΔα1-4 versus empty plasmid (b), or as indicated (e) as calculated by Student’s t test.
Absence of PSMα or lgt genes abrogates the capacity of S. aureus to stimulate TNF-α, IL-6 or IL-1β (a–c) and a USA300 mutant lacking PSMs plus Lgt requires complementation with both, PSM genes and lgt to regain the capacity to stimulate the release of these cytokines in human PBMCs (d–e) or IL-8 by human PMNs (f). Data represent means +/− s.e.m. of at least three independent experiments. *P<0.05, **P<0.01; ***P<0.001; ****P<0.0001; significantly different versus USA300 wild-type (a–c) or as indicated (d–f) as calculated by Student’s t-test.
BM-ϕ from TLR2−/− mice do not secrete MIP-2, mTNFα or mIL-6 in response to USA300 or the synthetic lipopeptide Pam2CSK4 but respond to LPS stimulation (a–c). Expression of both, PSMα and lipopeptides, is necessary to induce MIP-2, mTNFα and mIL-6 in BM- ϕ derived from wild-type mice (d–l). Data represent means +/− s.e.m. of at least three independent experiments. ****P<0.0001, significantly different versus USA300 wild-type (d–l) as calculated by Student’s t-test.
PSM peptides mobilize lipopeptides to stimulate TLR2
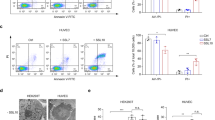
Since TLR2 stimulation is thought to be caused predominantly by bacterial lipoproteins it was analysed how PSMs and lipoproteins may play together in the induction of proinflammatory responses. The TLR2-activating capacity of Agr-positive S. aureus was fully dependent on lipoprotein MAMPs because inactivation of the lipoprotein-diacylglyceryl transferase gene (lgt) completely abrogated cytokine induction in human PBMCs, mouse macrophages, HEK-TLR2, HEK-TLR1/2 and HEK-TLR2/6 (Fig. 3, Fig. 4g–l, Fig. 2a,d, Supplementary Fig. 3). Synthetic PSMs did not stimulate HEK-TLR2 indicating that PSMs are no TLR2 agonists but may have essential roles in the expression, stability or release of lipoproteins (Fig. 5a). Of note, PSMs were only necessary for IL-8 induction when bacterial extracellular factors were used. In contrast, cell lysates of PSM-deficient USA300 mutants were equally active as those of USA300 wild-type (Fig. 5b) suggesting that even PSM mutants contain substantial amounts of TLR2 ligands but do not release them. In order to evaluate this assumption the major S. aureus lipoprotein SitC19,33 was quantified in USA300 wild-type and PSM mutants by western blotting. Of note, similar amounts of SitC were found cell-associated in wild-type and mutant strain while the amounts were drastically reduced in culture supernatants of the PSM mutant (Fig. 5c). Moreover, the entire exoprotein profile was substantially altered and particularly smaller protein bands corresponding to the predicted mass of many lipoproteins (∼20–40 kDa, Supplementary Data 1) were largely absent in the PSM and Agr mutants (Fig. 5d–f). Detailed label-free proteome analysis confirmed that the amounts of most lipoproteins were markedly reduced in culture filtrates of the PSMα and Agr mutants compared with the wild-type (Fig. 5g,h). All these data provided evidence for a crucial role of PSMs, which are known to have surfactant-like properties26, in the release of membrane-embedded lipoproteins to the extracellular space.
Synthetic PSMs do not stimulate IL-8 secretion by untransfected or TLR2-transfected HEK cells (a). PSMs do not affect the capacity of S. aureus USA300 cell lysates to induce IL-8 in HEK-TLR2 (b) but are required for efficient release of the major lipoprotein SitC with a C-terminal His tag as shown by western blotting of equal amounts of culture filtrates of USA300 wild-type, Δα, and Δα,β,hld (c, Supplementary Fig. 7). Inactivation of Agr or absence of PSMs leads to drastically altered Coomassie Blue-stained exoprotein patterns and reduced protein content in culture filtrates (d,e). Amounts of cytoplasmic proteins are also strongly reduced in USA300 PSM and Agr mutant exoproteomes compared with the wild-type strain (f). In contrast, signal peptide-bearing secreted proteins are not affected by deletion of PSMα peptides but the amount of this group of proteins is reduced in culture filtrates of the Agr mutant, probably because Agr controls expression of many major extracellular proteins. Overall amounts of most S. aureus lipoproteins and the lipoprotein SitC are reduced in culture filtrates of Agr and PSM mutants (g,h). Data in (a), (b) and (f) represent means +/− s.e.m. of at least three independent experiments. ***P<0.001, ****P<0.0001, significantly different for HEK versus HEK-TLR2 (a) and mutants versus USA300 wild-type (b,f) as calculated by Student’s t test.
PSM-producing staphylococci are not inhibited by PSMs because they express the PSM-exporting Pmt efflux pump34. Nevertheless, it is tempting to assume that PSMs alter the properties of the staphylococcal cytoplasmic membrane in a way that promotes the release of lipoproteins. In order to study if exogenous PSMs can also mobilize lipoproteins S. aureus PSM mutants were incubated with synthetic PSMs. Indeed, supernatants of PSMα-treated PSM mutants contained strongly increased levels of SitC and exhibited potent TLR2-stimulating activity (Fig. 6a,b). In line with the assumption that PSMs may partially permeabilize the cytoplasmic membrane many cytoplasmic proteins were also much more abundant in culture filtrates of PSMα-expressing S. aureus compared with Agr or PSM-deficient mutants, whereas the levels of signal peptides-bearing secreted proteins remained largely unaltered in the wild-type compared with the PSM mutant. In contrast, the Agr mutant produced less extracellular proteins than the PSM mutant because many secreted proteins are Agr-regulated34 (Fig. 5f, Supplementary Data 1). Major toxins such as Hla, Pvl and LukAB had no impact on the overall protein amount and had no major impact on TLR2-dependent cytokine release (Supplementary Fig. 4). Nevertheless, PSM-producing S. aureus were not affected in their growth behaviour, viability or microscopic appearance (Supplementary Fig. 5), which confirms previous results24,34 and indicates that the PSM-mediated modulation of the cytoplasmic membrane has no detrimental impact on S. aureus cellular integrity.
Incubation of S. aureus USA300 PSM mutants with synthetic PSMα peptides leads to a strong increase in free His-tagged SitC detectable in western blots of culture filtrates (a, Supplementary Fig. 7) and restores the capacity of PSM mutant culture filtrates to stimulate IL-8 production in HEK-TLR2 cells (b). The synthetic lipopeptide Pam2CSK4 and TSB medium or (dimethylsulphoxide) DMSO at concentrations used to dissolve synthetic PSMs were used as positive and negative controls, respectively. Data in (b) represent means +/− s.e.m. of at least three independent experiments. **P<0.01; ****P<0.0001, significantly different versus USA300 Δα (b) as calculated by Student’s t test.
TLR2 is crucial for protection against PSM-producing S. aureus
The finding that PSMs are crucial for TLR2-dependent cytokine induction in cell culture raised the question if PSMs contribute to TLR2 activation in vivo. Intravenous injection of C57BL/6 mice with S. aureus USA300 led to induction of proinflammatory cytokines and USA300 wild-type caused stronger inflammation than the PSM mutant (Supplementary Fig. 6). USA300 PSM or Agr mutants had lethal consequence only in a small minority of mice and mortality was similar in wild-type and TLR2-deficient mice, indicating that TLR2 does not contribute much to clearing systemic infection caused by PSM-deficient S. aureus (Fig. 7a,b). In contrast, USA300 wild-type was more virulent than PSM or Agr mutants, most probably as a consequence of PSM- and Agr-dependent cytotoxicity. Moreover, inactivation of TLR2 led to increased mortality in USA300 wild-type infected mice with no surviving animals 4 days after infection (Fig. 7c). Thus, TLR2 has a vital role in protection against infections caused by S. aureus that produce PSMs (Fig. 8).
TLR2 has only a minor impact on survival of mice infected with Agr or PSM-deficient S. aureus USA300 (a,b) but protects mice infected with USA300 wild-type (c). The FPR2 receptor has no major impact on the course of systemic S. aureus infection. Mice were infected with 1 × 107 CFU of USA300 wild-type (18 non-transgenic, 8 TLR2−/−, 10 FPR2−/− C57BL/6 animals), with USA300 Δα,β,hld (8 non-transgenic, 8 TLR2−/−, 10 FPR2−/− C57BL/6 animals), or USA300 Δagr (10 non-transgenic, 12 TLR2−/− C57BL/6 animals). Survival curves were monitored for statistical significance versus wild-type mice by the log-rank test.
PSM lipopeptides cause general inflammation via TLR2 (left) while PSM gradients lead to local recruitment of leukocytes via FPR2 (right)28.
The FPR2 receptor can sense PSM peptides and elicit neutrophil chemotaxis27,28. FPR2-deficient mice were included in the infection model to assess if FPR2 may contribute to PSM-dependent aggravation of sepsis, but wild-type and FPR2-deficient mice did not differ in sepsis. This indicates that FPR2 may be important for leukocyte recruitment in local infection as reported previously27 but has no major impact on systemic infection. Taken together, these data confirm that TLR2 is important in S. aureus infections but its capacity to contribute to host defense depends on the mobilization of lipoproteins by PSMs.
Discussion
Our study demonstrates that the capacity of pattern recognition receptors to respond to MAMPs does not only depend on MAMP production but also on mechanisms mobilizing them. These may be human molecules such as lipopolysaccharide-binding protein and CD14 for lipopolysaccharide (LPS) release and TLR4 stimulation35 or, as in the case of PSMs, bacterial molecules. PSMs are also crucial toxins disrupting eukaryotic membranes at very high concentrations24,26. They may be indispensable for highly pathogenic S. aureus, which may use PSMs for coping with immune cells infiltrating upon strong activation of innate immunity via TLR2 or other pathways. It is interesting to note that PSMα2 and PSMα3, the most cytotoxic PSMs24, also had the most pronounced capacity to release lipoproteins from S. aureus. Thus, disrupting human cell membranes and promoting the release of bacterial lipoproteins may depend on the same surfactant-like properties of PSMs.
PSM peptides have previously been reported to have some TLR2-stimulating activity36, but this study has used PSMs purified from staphylococcal culture supernatants, which may have been contaminated by residual lipoproteins. In contrast, we demonstrate that synthetic PSMs have no such activity. Only staphylococci produce PSMs and high amounts are found in highly pathogenic strains such as CA-MRSA26,29. Accordingly, TLR2 may have a major role in defense against highly pathogenic S. aureus and only a minor role against opportunistic pathogens. This notion is in agreement with the low capacities of enterococci and L. monocytogenes to stimulate HEK-TLR2. S. aureus strains causing chronic infections such as osteomyelitis often acquire Agr mutations37 probably as a means to avoid strong TLR2-dependent inflammation. Many S. aureus strains produce the SSL3 protein, a potent inhibitor of TLR2 (refs 38, 39), which may have similar consequences as the mutation of Agr albeit without affecting the activity of virulence factors other than TLR2 agonists and PSMs.
Modulation of inflammation is a crucial strategy to treat bacterial infections, either by dampening overwhelming inflammation, for example, in sepsis or by stimulating host defense in chronic infections, which often fail to initiate an appropriate immune response40,41. S. aureus sepsis is always associated with exuberant, systemic inflammation14,15 and protective immune-modulatory intervention strategies are urgently needed. Our study will be important for assessing in which types of Gram-positive infections immunomodulatory interventions should be helpful. In addition to directly targeting TLR2, new types of drugs may help to either block PSM release to prevent exuberant inflammation or support lipoprotein release in chronic infections. Along this line the S. aureus PSM exporter Pmt has been recognized as an attractive antibiotic target34. Moreover, agents with surfactant-like properties such as membrane-damaging antibiotics and disinfectants may help to mobilize TLR2 ligands in infections caused, for example, by S. aureus Agr mutants. PSMs are only found in staphylococci but the concept of MAMP release by surfactant–like molecules may be relevant also for other pathogens, for example, by the rhamnolipids of Pseudomonas aeruginosa42. Modulating the expression or treatment with surfactant-like agents may open new avenues for therapeutic interventions.
Methods
Bacterial cultivation and preparation of crude lysates
Bacterial strains (Supplementary Table 1) were maintained on sheep-blood tryptic soy agar plates. Haemolysis and RNAIII expression were monitored to confirm functional Agr systems and toxin production in S. aureus. All bacteria were grown in tryptic soy broth (TSB, Gram-positives) or lysogeny broth (E. coli) supplemented with appropriate antibiotics (Supplementary Table 2) if necessary in flasks on a shaker at 37 °C. In order to induce SitC expression in S. aureus USA300 pTXSitC-His, bacteria were cultivated in TSB without glucose containing 0.5% xylose. Bacterial culture supernatants were obtained by centrifugation of overnight cultures and filtered through 0.2-μm pore size filters. All steps were performed at 4 °C or on ice. Twenty-four-well plates were used for small culture volumes of bacteria when adding synthetic PSM peptides to release lipoproteins. Bacterial lysates were performed using the FastPrep-24 cell disintegrator (MP Biomedicals). To this end 500 μl glass beads (150–212 μm, Sigma) were mixed with 500 μl heat-inactivated (70 °C, 30 min) bacteria (OD600=28) in lysis buffer (20 mM Tris/HCl, 0.1 M NaCl, pH 8). FastPrep speed was set to 5 and bacteria were lysed by three runs for 30 s. To determine the colony forming units (CFU)-to- optical density relation of bacterial strains TSB was inoculated with overnight cultures at an OD600 of 0.1 and the ODs were monitored at hourly intervals until the stationary growth phase was reached (growth curves). The CFU was determined with optical density adjusted overnight cultures by plating on TSB plates. To determine the ratio between live and dead cells the LIVE/DEAD BacLight Bacterial Viability Kit (Molecular Probes) was used as described by the manufacturer’s instructions.
RNA isolation
For qRT–PCR 25-ml cultures were inoculated with a preculture to an OD600 of 0.05 and grown for 6 h. Cells were immediately harvested and RNA stabilized by addition of 2 × vol. RNAprotect bacteria reagent (Quiagen). After centrifugation the supernatant was removed, and the pellet was quickly frozen with liquid N2.Then the pellets were resuspended in 1 ml TRIZOL solution (Invitrogen—Life Technologies Corporation, Darmstadt, Germany) and lysed with 0.3 ml zirconia-silica beads (Karl Roth GmbH, Karlsruhe, Germany; 0.1-mm diameter) in a high-speed benchtop homogenizer (FastPrep-24, MP Biomedicals, Germany). The lysed samples were mixed with 200 μl chloroform followed by centrifugation for 15 min at 4 °C and 15 000 r.p.m. The clear layer was transferred to a new tube and mixed with 500 μl isopropanol. After a further centrifugation and two washing steps with ethanol the RNA was carefully resuspended in RNAse-free water. To get rid of DNA contamination 5 μg ml−1 of each sample was mixed with 2 μl DNAse I (DNase Treatment and Removal kit, Ambion, Life Technologies) and 1 μl recombinant RNasin ribonuclease inhibitor (Promega, Madison, WI, USA) and incubated for 30 min at room temperature. Then DNAse was inactivated by adding inactivation reagent (DNase Treatment and Removal kit, Ambion, Life Technologies and RNA concentration was analysed.
qRT–PCR
For relative quantification standards of the gyrase gene gyrB and for RNAIII were generated from pooled RNA with the primers for gyrB forward: 5′-CAAATGATCACAGCATTTGGTACAG-3′ and reverse: 5′-CGGCATCAGTCATAATGACGAT-3′ or RNAIII forward: 5′-GTGATGGAAAATAGTTGATGAGTTGTTT-3′ and reverse: 5′-GAATTTGTTCACTGTGTCGATAATCC-3′, respectively, as described in ref. 31. qRT–PCR was performed using the QuantStudio 3 instrument (Applied Biosystems, Thermo Fisher Scientific) in combination with the Power SYBR Green RNA-to-CT 1 Step Kit (Applied Biosystems). Master mixes were prepared according to the manufacturer’s instructions.
Stimulation of cell lines
HEK cells stably transfected with the human TLR2, TLR1/2, TLR2/6 genes or un-transfected HEK cells were purchased from Invivogen. HEK-TLR2 cells were cultivated in 75-cm2 culture flasks using 20 ml of growth medium (Dulbecco's modified eagle medium (DMEM), 10% fetal calf serum (FCS), 100 μg ml−1 normocin, and 10 μg ml−1blasticidin). Un-transfected HEK cells were cultivated in DMEM, 10% FCS, 20 mM L-glutamine, and 1,000 u ml−1penicillin/streptomycin. Cells were seeded into 24-well cell culture plates and cultivated until confluence was reached. Growth medium was then replaced by medium without FCS containing appropriately diluted stimuli. Culture filtrates were used at 0.25% (TSB), 2% (TSB with 0.5% xylose and lacking glucose) or 5% (IMDM) final concentration according to bacterial densities reached in the various media. Diluted culture filtrates exerted no toxicity towards HEK cells as analysed with the Cytotoxicity Detection Kit (Roche Applied Sciences). No stimulatory activity was detected in non-inoculated media at corresponding dilutions. Protein concentrations of crude lysates were determined with the Bradford assay (BioRad) and 100 ng ml−1 per lysate were used for stimulation. For stimulation with live bacteria 1 × 106 CFU S. aureus from overnight cultures grown in TSB were added per well and incubated with HEK cells for 18 h at 37 °C and 5% CO2 to allow expression and release of PSMs and lipoproteins. Subsequently bacterial growth was stopped by adding 200 μg ml−1 gentamicin to avoid overgrowth and cytotoxicity and incubation was continued for another 16 h. The synthetic lipopeptide Pam2CSK4 (1 ng ml−1 in stimulation medium) and cell culture medium with TSB concentrations corresponding to diluted culture filtrates were used as positive and negative controls, respectively. Formylated PSM peptides (PSMα1, PSMα2, PSMα3 and PSMα4) with the recently published sequences24 were synthesized at the Interfaculty Institute of Cell Biology (Department of Immunology, University of Tübingen). After stimulation supernatants were collected by centrifugation for 10 min at 250 × g and stored at −20 °C before use. Cytokines were measured using ELISA kits (R&D Systems) according to the manufacturer's instructions.
Stimulation of primary cells
Human PMNs and PBMCs were isolated from fresh human blood of healthy volunteers by standard Ficoll/Histopaque gradient centrifugation as described recently27 and stimulated with diluted bacterial culture filtrates (1.5% for TSB culture filtrates) or crude bacterial lysates (100 ng ml−1 protein) in 96-well plates. 5 × 105 PMNs or PBMCs were seeded in cell culture medium (very low endotoxin-Roswell Park Memorial Institute Medium (RPMI) 1640, 2 mM sodium pyruvate, 2 mM L-glutamine, 100 u ml−1 penicillin/streptomycin, 10 mM 4-(2-hydroxyethyl)-1-piperazineethanesulfonic acid (HEPES)) and incubated for 5 h at 37 °C and 5% CO2. Primary bone marrow-derived macrophages (BM-Φ) were generated from 12-week-old female and male C57BL6J wild-type (Harlan Laboratories) or isogenic TLR2−/−43 mice as described previously44. Briefly, femora and tibiae were flushed with cold PBS. Obtained cells were cultivated in medium (DMEM, 10% FCS, 5% human serum albumin (HSA), 1% penicillin/streptomycin, 1% glutamine, 0.5% sodium pyruvate and 20% supernatant of L929 cells producing macrophage colony-stimulating factor for differentiation) for 7 days in 15-cm uncoated cell culture dishes and subsequently resuspended in ice-cold PBS on ice. BM-ϕ were seeded at a density of 0.25 × 106 per ml in 24-well plates and allowed to adhere overnight followed by stimulation with culture filtrates (2%) diluted in stimulation medium (DMEM, 10% FCS, 1% glutamine, 0.5% sodium pyruvate, 1% penicillin/streptomycin) for 24 h. Cytokines were measured as described above.
Deletion of lgt in S. aureus USA300 LAC
For deletion of the lgt gene in USA300 LAC the flanking regions of the lgt gene were amplified by PCR using primer with added restriction sites for EcoRI/SacI (N-terminal) and SacI/BglII (C-terminal) (Supplementary Table 3). The plasmid pBASE6 was digested with EcoRI and BglII and ligated with the flanking regions of lgt. After amplification of pBASE6-Δlgt in E. coli DH5α and S. aureus RN4220, the plasmid was used to transform USA300 and the lgt gene was deleted by homologous recombination as described previously45.
SitC release and detection
Bacterial cultures expressing SitC-His under xylose induction were adjusted to densities of OD600=0.1, supplemented with 200 μg ml−1 PSMα peptides and cultivated for appropriate times in 24-well plates under agitation at 37 °C. Culture filtrates were obtained by centrifugation for stimulation of HEK cells as described above or for detection of SitC-His by western blotting. The protein concentration of culture filtrates was determined by Bradford assay (BioRad) and a volume corresponding to 25 μg protein of USA300 wild-type and the same volume from mutant strains were concentrated with 10 μl Strataclean Resin beads (Agilent Technologies). After washing with 1 ml PBS, beads were resuspended in twofold loading dye (Pierce), boiled at 99 °C for 10 min, cooled down on ice, and loaded on SDS-HEPES polyacrylamide gels (12%, Gel Pierce). Ten microlitres of PageRuler (Thermo) was used as molecular weight marker. SDS-PAGE was performed according to the manufacturer’s instructions (Pierce). Proteins were either visualized by Coomassie blue staining or transferred from SDS gels to a nitrocellulose membranes for western blotting. The membrane was blocked for 30 min with Pierce blocking solution and washed twice with Tris-buffered saline and Tween and one time with Tris-buffered saline. The first antibody (mouse anti-5His-IgG from QIAGEN, 0.2 mg ml−1 stock solution diluted 1:10,000) was applied for 60 min in blocking solution. After washing the second antibody (goat anti-maus-IgG-HRP from Merck Millipore, 0.2 mg ml−1 stock solution diluted 1:30,000) in Tris-buffered saline with 10% skim milk powder was added for 60 min. The membrane was then washed again. For visualization of the SitC-His bands on the membrane the western blotting luminol reagent (Santa Cruz) was applied and chemiluminescence was detected on an x-ray film.
Transmission electron microscopy
Transmission electron microscopy analysis was performed as described earlier34. Briefly, bacterial cultures grown in TSB medium were harvested at late exponential growth phase (6 h). The cells were fixed overnight at 4 °C by 2.5% glutaraldehyde in 0.1 M sodium cacodylate and rinsed three times with 0.1 M sodium cacodylate. Samples were further fixed with 0.5% osmium tetroxide/0.8% potassium ferricyanide in 0.1 M sodium cacodylate and then with 1% tannic acid. The fixed samples were dehydrated by washing with ethanol and then transferred to acetone. After embedding into epon/araldite and polymerization, thin sections were cut and stained with 4% samarium acetate and Reynold’s lead citrate. The sections were viewed at 80 kV on a Tecnai BT Spirit transmission electron microscope (FEI) and digital images were acquired with a Hamamatsu ORCA HR camera system (Advanced Microscopy Techniques).
Quantitative label-free proteomics
Three biological replicates of USA300 wild-type or mutant culture filtrates grown overnight in TSB were analysed. The same protein amount measured by Bradford assay in culture filtrates of the various strains was used for exoprotein precipitation with 10% ice-cold trichloroacetic acid overnight at 4 °C. After centrifugation at 13,200 r.p.m. at 4 °C for 15 min the supernatants were discarded and precipitated proteins were air dried. For nanoliquid chromatography–mass spectrometry/mass spectrometry analysis dried proteins were dissolved in a buffer containing 6 M urea, 2 M thiourea, 10 mM Tris at pH 8.0 and digested in solution with trypsin as described previously46. Peptide mixtures were then separated on an EasyLC nano- high-performance liquid chromatography (Proxeon Biosystems) coupled to an Linear Trap Quadrupole (LTQ) Orbitrap Elite mass spectrometer (Thermo Fisher Scientific) as described elsewhere46 with the following modifications: Peptides were eluted with an 87-min segmented gradient of 5–33–90% high-performance liquid chromatography solvent B (80% acetonitrile in 0.5% acetic acid). Each sample was run in technical triplicates. Acquired mass spectrometry spectra were processed with the MaxQuant software package version 1.2.2.9 (ref. 47) with integrated Andromeda search engine48 as described previously46. Database searches were performed against a target decoy S. aureus USA300 database obtained from Uniprot, containing 5,295 protein entries and 248 commonly observed contaminants. The label-free algorithm was enabled as was the ‘match between runs’ option49. Label-free quantification (LFQ) protein intensities from the MaxQuant data output were used for relative protein quantification. Different volumes of culture filtrates needed for precipitation of equal amounts of proteins were considered when calculating the original protein contents from determined LFQ intensities. Detected proteins were sorted by their subcellular localization using the software PSORTb v.3.0 (www.psort.org). The database of lipopeptide prediction PRED-LIPO was used to identify lipoproteins (S. aureus USA300 predicted 63: www.bioinformatics.biol.uoa.gr/PRED-LIPO-results/). Culture filtrates were compared for total protein content (∑LFQ of all proteins) and composition sorted by subcellular localization (∑LFQ of each subcellular localization). Differences of single proteins between mutants are listed in Supplementary Data 1.
Mouse bacteremia model
TSB medium was inoculated with S. aureus strains from a pre-culture and grown to mid-exponential growth phase (2–3 h). Bacteria were harvested, washed and diluted in sterile PBS. CFU were determined by diluting and plating on TSB plates. Six-week old female C57BL/6 wild-type mice purchased from Harlan Laboratories, C57BL/6 TLR2−/−43, or C57BL/6 FPR2−/−50 mice were challenged with 1 × 107 live bacteria in 0.2 ml PBS injected into the tail vein as described recently43. Survival and disease progression was monitored over 14 days. Blood was collected from some mice 6 and 17 h after infection. Cytokine/chemokine levels in blood serum were determined following the manufacturer’s instructions with a custom-made Luminex assay including magnetic beads for the measurement of CXCL2 (MIP-2), IL-1β, IL-6 and TNFα (R&D Systems, Minneapolis, MN, USA). The samples were analysed on a Bio-Plex MAGPIX Multiplex Reader (Bio-Rad Laboratories, Munich, Germany) with Bio-Plex Manager MP Software (Bio-Rad) and ELISA (R&D Systems, Minneapolis, MN, USA).
Statistics
Statistical analysis was performed using Graph Pad Prism 5.0. Unpaired two-tailed Student’s t-test was used to compare two groups unless otherwise noted. Survival of mouse strains was compared with the log-rank test. Data represent mean and s.d. or s.e.m. as indicated.
Ethic statements
Human PMNs and PBMCs were isolated from venous blood of healthy volunteers in accordance with protocols approved by the Institutional Review Board for Human Subjects at the University of Tübingen. Informed written consent was obtained from all volunteers. Animal experiments were performed according to German law with permission of the responsible authorities (H3/12 und H3/13, Regierungspräsidium Tübingen).
Data availability
The mass spectrometry proteomics data have been deposited to the ProteomeXchange Consortium via the PRIDE51 partner repository with the dataset identifier PXD004283. These data were further processed and are provided as source data for figure 5f–h with the article (Supplementary Data 1). The authors declare that the data supporting the findings of this study are available within the article and its supplementary information files.
Additional information
How to cite this article: Hanzelmann, D. et al. Toll-like receptor 2 activation depends on lipopeptide shedding by bacterial surfactants. Nat. Commun. 7:12304 doi: 10.1038/ncomms12304 (2016).
References
Angus, D. C. & van der Poll, T. Severe sepsis and septic shock. N. Engl. J. Med. 369, 840–851 (2013).
Plociennikowska, A., Hromada-Judycka, A., Borzecka, K. & Kwiatkowska, K. Co-operation of TLR4 and raft proteins in LPS-induced pro-inflammatory signaling. Cell. Mol. Life Sci. 72, 557–581 (2015).
Kawai, T. & Akira, S. The role of pattern-recognition receptors in innate immunity: update on Toll-like receptors. Nat. Immunol. 11, 373–384 (2010).
Hashimoto, M. et al. Not lipoteichoic acid but lipoproteins appear to be the dominant immunobiologically active compounds in Staphylococcus aureus. J. Immunol. 177, 3162–3169 (2006).
Takeuchi, O., Hoshino, K. & Akira, S. Cutting edge: TLR2-deficient and MyD88-deficient mice are highly susceptible to Staphylococcus aureus infection. J. Immunol. 165, 5392–5396 (2000).
Nachtigall, I. et al. Polymorphisms of the toll-like receptor 2 and 4 genes are associated with faster progression and a more severe course of sepsis in critically ill patients. J. Int. Med. Res. 42, 93–110 (2014).
Stappers, M. H. et al. TLR1, TLR2, and TLR6 gene polymorphisms are associated with increased susceptibility to complicated skin and skin structure infections. J. Infect. Dis. 210, 311–318 (2014).
Lachance, C., Segura, M., Gerber, P. P., Xu, J. & Gottschalk, M. Toll-like receptor 2-independent host innate immune response against an epidemic strain of Streptococcus suis that causes a toxic shock-like syndrome in humans. PLoS ONE 8, e65031 (2013).
Edelson, B. T. & Unanue, E. R. MyD88-dependent but Toll-like receptor 2-independent innate immunity to Listeria: no role for either in macrophage listericidal activity. J. Immunol. 169, 3869–3875 (2002).
Loof, T. G., Goldmann, O. & Medina, E. Immune recognition of Streptococcus pyogenes by dendritic cells. Infect. Immun. 76, 2785–2792 (2008).
Schmaler, M. et al. Lipoproteins in Staphylococcus aureus mediate inflammation by TLR2 and iron-dependent growth in vivo. J. Immunol. 182, 7110–7118 (2009).
Peres, A. G. et al. Uncoupling of pro- and anti-inflammatory properties of Staphylococcus aureus. Infect. Immun. 83, 1587–1597 (2015).
Basto, A. P. & Leitao, A. Targeting TLR2 for vaccine development. J. Immunol. Res. 2014, 619410 (2014).
Tong, S. Y., Davis, J. S., Eichenberger, E., Holland, T. L. & Fowler, V. G. Jr Staphylococcus aureus infections: epidemiology, pathophysiology, clinical manifestations, and management. Clin. Microbiol. Rev. 28, 603–661 (2015).
Thammavongsa, V., Kim, H. K., Missiakas, D. & Schneewind, O. Staphylococcal manipulation of host immune responses. Nat. Rev. Microbiol. 13, 529–543 (2015).
Spaan, A. N., Surewaard, B. G., Nijland, R. & van Strijp, J. A. Neutrophils versus Staphylococcus aureus: a biological tug of war. Annu. Rev. Microbiol. 67, 629–650 (2013).
Nakayama, H., Kurokawa, K. & Lee, B. L. Lipoproteins in bacteria: structures and biosynthetic pathways. FEBS J. 279, 4247–4268 (2012).
Buddelmeijer, N. The molecular mechanism of bacterial lipoprotein modification--how, when and why? FEMS Microbiol. Rev. 39, 246–261 (2015).
Muller, P. et al. The Staphylococcus aureus lipoprotein SitC colocalizes with Toll-like receptor 2 (TLR2) in murine keratinocytes and elicits intracellular TLR2 accumulation. Infect. Immun. 78, 4243–4250 (2010).
Sheldon, J. R. & Heinrichs, D. E. The iron-regulated staphylococcal lipoproteins. Front. Cell. Infect. Microbiol. 2, 41 (2012).
Stoll, H., Dengjel, J., Nerz, C. & Gotz, F. Staphylococcus aureus deficient in lipidation of prelipoproteins is attenuated in growth and immune activation. Infect. Immun. 73, 2411–2423 (2005).
Otto, M. Staphylococcus aureus toxins. Curr. Opin. Microbiol. 17, 32–37 (2014).
Singh, R. & Ray, P. Quorum sensing-mediated regulation of staphylococcal virulence and antibiotic resistance. Future Microbiol. 9, 669–681 (2014).
Wang, R. et al. Identification of novel cytolytic peptides as key virulence determinants for community-associated MRSA. Nat. Med. 13, 1510–1514 (2007).
Queck, S. Y. et al. RNAIII-independent target gene control by the agr quorum-sensing system: insight into the evolution of virulence regulation in Staphylococcus aureus. Mol. Cell. 32, 150–158 (2008).
Peschel, A. & Otto, M. Phenol-soluble modulins and staphylococcal infection. Nat. Rev. Microbiol. 11, 667–673 (2013).
Kretschmer, D. et al. Human formyl peptide receptor 2 senses highly pathogenic Staphylococcus aureus. Cell Host Microbe 7, 463–473 (2010).
Bloes, D. A., Kretschmer, D. & Peschel, A. Enemy attraction: bacterial agonists for leukocyte chemotaxis receptors. Nat. Rev. Microbiol. 13, 95–104 (2015).
Rautenberg, M., Joo, H. S., Otto, M. & Peschel, A. Neutrophil responses to staphylococcal pathogens and commensals via the formyl peptide receptor 2 relates to phenol-soluble modulin release and virulence. FASEB J. 25, 1254–1263 (2011).
Chambers, H. F. Community-associated MRSA--resistance and virulence converge. N. Engl. J. Med. 352, 1485–1487 (2005).
Cheung, G. Y., Wang, R., Khan, B. A., Sturdevant, D. E. & Otto, M. Role of the accessory gene regulator agr in community-associated methicillin-resistant Staphylococcus aureus pathogenesis. Infect. Immun. 79, 1927–1935 (2011).
Joo, H. S., Cheung, G. Y. & Otto, M. Antimicrobial activity of community-associated methicillin-resistant Staphylococcus aureus is caused by phenol-soluble modulin derivatives. J. Biol. Chem. 286, 8933–8940 (2011).
Diep, B. A. et al. Identifying potential therapeutic targets of methicillin-resistant Staphylococcus aureus through in vivo proteomic analysis. J. Infect. Dis. 209, 1533–1541 (2014).
Chatterjee, S. S. et al. Essential Staphylococcus aureus toxin export system. Nat. Med. 19, 364–367 (2013).
Vesy, C. J., Kitchens, R. L., Wolfbauer, G., Albers, J. J. & Munford, R. S. Lipopolysaccharide-binding protein and phospholipid transfer protein release lipopolysaccharides from gram-negative bacterial membranes. Infect. Immun. 68, 2410–2417 (2000).
Hajjar, A. M. et al. Cutting edge: functional interactions between toll-like receptor (TLR) 2 and TLR1 or TLR6 in response to phenol-soluble modulin. J. Immunol. 166, 15–19 (2001).
Valour, F. et al. Delta-toxin production deficiency in Staphylococcus aureus: a diagnostic marker of bone and joint infection chronicity linked with osteoblast invasion and biofilm formation. Clin. Microbiol. Infect. 21, 568.e1–568.e11 (2015).
Bardoel, B. W. et al. Evasion of toll-like receptor 2 activation by staphylococcal superantigen-like protein 3. J. Mol. Med. (Berl) 90, 1109–1120 (2012).
Koymans, K. J. et al. Structural basis for inhibition of TLR2 by staphylococcal superantigen-like protein 3 (SSL3). Proc. Natl Acad. Sci. USA 112, 11018–11023 (2015).
Hengge, U. R., Benninghoff, B., Ruzicka, T. & Goos, M. Topical immunomodulators--progress towards treating inflammation, infection, and cancer. Lancet Infect. Dis. 1, 189–198 (2001).
Savva, A. & Roger, T. Targeting toll-like receptors: promising therapeutic strategies for the management of sepsis-associated pathology and infectious diseases. Front. Immunol. 4, 387 (2013).
Kim, L. H., Jung, Y., Yu, H. W., Chae, K. J. & Kim, I. S. Physicochemical interactions between rhamnolipids and pseudomonas aeruginosa biofilm layers. Environ. Sci. Technol. 49, 3718–3726 (2015).
Wooten, R. M. et al. Toll-like receptor 2 is required for innate, but not acquired, host defense to Borrelia burgdorferi. J. Immunol. 168, 348–355 (2002).
Siegfried, A. et al. IFIT2 is an effector protein of type I IFN-mediated amplification of lipopolysaccharide (LPS)-induced TNF-alpha secretion and LPS-induced endotoxin shock. J. Immunol. 191, 3913–3921 (2013).
Geiger, T. et al. The stringent response of Staphylococcus aureus and its impact on survival after phagocytosis through the induction of intracellular PSMs expression. PLoS Pathog. 8, e1003016 (2012).
Carpy, A. et al. Absolute proteome and phosphoproteome dynamics during the cell cycle of Schizosaccharomyces pombe (Fission Yeast). Mol. Cell. Proteomics 13, 1925–1936 (2014).
Cox, J. & Mann, M. MaxQuant enables high peptide identification rates, individualized p.p.b.-range mass accuracies and proteome-wide protein quantification. Nat. Biotechnol. 26, 1367–1372 (2008).
Cox, J. et al. Andromeda: a peptide search engine integrated into the MaxQuant environment. J. Proteome. Res. 10, 1794–1805 (2011).
Luber, C. A. et al. Quantitative proteomics reveals subset-specific viral recognition in dendritic cells. Immunity 32, 279–289 (2010).
Chen, K. et al. A critical role for the g protein-coupled receptor mFPR2 in airway inflammation and immune responses. J. Immunol. 184, 3331–3335 (2010).
Vizcaino, J. A. et al. 2016 update of the PRIDE database and its related tools. Nucleic Acids Res 44, D447–456 (2016).
Acknowledgements
We thank Nele Nikola, Cordula Gekeler, Irina Droste-Borel, Silke Wahl and Johannes Madlung for technical support, and Ji Ming Wang for providing C57BL/6 FPR2−/− mice. This study was supported by grants from the German Research Council SFB685 to S.S. and A.P, SFB766 to B.M., C.W., F.G., and A.P, TRR34 to C.W., F.G., D.K., and A.P., and PE805/5-1, to A.P.; by the Fortüne Program of the Medical Faculty, University of Tübingen (to D.K.), the German Center for Infectious Diseases Research (DZIF) to D.K. and A.P.; and the Intramural Research Program of the National Institute of Allergy and Infectious Diseases, National Institutes of Health (to M.O.)
Author information
Authors and Affiliations
Contributions
S.S. synthesized PSM peptides, M.F.-W., B.M. and D.H. performed label-free quantitative proteomics, D.K. performed qRT–PCR, T.H. performed Luminex assay, H.-S.J. and M.O. performed TEM analysis, D.K. and D.H performed animal infection experiments, F.G. and C.W. provided strains and plasmids, D.H. performed all other experiments, D.K. and A.P. supervised the experiments and D.H., D.K. and A.P. prepared the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Supplementary Information
Supplementary Figures 1-7, Supplementary Tables 1-3 and Supplementary References (PDF 349 kb)
Supplementary Data 1
Quantitative label-free proteomics. Three biological replicates of USA300 wild-type, PSM and Agr mutant culture filtrates were analysed for protein content and composition. Label-free quantification (LFQ) protein intensities are listed for detected proteins of each culture filtrate (sheet: quantitative label-free). Proteins were sorted for their subcellular localization. ∑LFQ of each protein was compared between wild-type and mutants (sheets: cytoplasmic, membrane, cell wall, extracellular, unknown and lipopeptides). Culture filtrates were compared for composition sorted by subcellular localization (∑LFQ of each subcellular localization) (sheet: ∑LFQ). (XLSX 336 kb)
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Hanzelmann, D., Joo, HS., Franz-Wachtel, M. et al. Toll-like receptor 2 activation depends on lipopeptide shedding by bacterial surfactants. Nat Commun 7, 12304 (2016). https://doi.org/10.1038/ncomms12304
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/ncomms12304
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.