Abstract
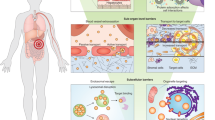
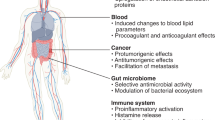
Biological barriers to drug transport prevent successful accumulation of nanotherapeutics specifically at diseased sites, limiting efficacious responses in disease processes ranging from cancer to inflammation. Although substantial research efforts have aimed to incorporate multiple functionalities and moieties within the overall nanoparticle design, many of these strategies fail to adequately address these barriers. Obstacles, such as nonspecific distribution and inadequate accumulation of therapeutics, remain formidable challenges to drug developers. A reimagining of conventional nanoparticles is needed to successfully negotiate these impediments to drug delivery. Site-specific delivery of therapeutics will remain a distant reality unless nanocarrier design takes into account the majority, if not all, of the biological barriers that a particle encounters upon intravenous administration. By successively addressing each of these barriers, innovative design features can be rationally incorporated that will create a new generation of nanotherapeutics, realizing a paradigmatic shift in nanoparticle-based drug delivery.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Kola, I. & Landis, J. Can the pharmaceutical industry reduce attrition rates? Nat. Rev. Drug Discov. 3, 711–716 (2004).
Torchilin, V.P. Recent advances with liposomes as pharmaceutical carriers. Nat. Rev. Drug Discov. 4, 145–160 (2005).
Matsumura, Y. & Maeda, H. A new concept for macromolecular therapeutics in cancer chemotherapy: mechanism of tumoritropic accumulation of proteins and the antitumor agent smancs. Cancer Res. 46, 6387–6392 (1986). A seminal work on the EPR effect in cancer that essentially laid the foundation for the use of nanotherapeutics, including liposomes and polymer-drug conjugates, as treatment modalities.
Maeda, H., Nakamura, H. & Fang, J. The EPR effect for macromolecular drug delivery to solid tumors: Improvement of tumor uptake, lowering of systemic toxicity, and distinct tumor imaging in vivo. Adv. Drug Deliv. Rev. 65, 71–79 (2013).
Azzopardi, E.A., Ferguson, E.L. & Thomas, D.W. The enhanced permeability retention effect: a new paradigm for drug targeting in infection. J. Antimicrob. Chemother. 68, 257–274 (2013).
Marti, C.N. et al. Endothelial dysfunction, arterial stiffness, and heart failure. J. Am. Coll. Cardiol. 60, 1455–1469 (2012).
Zhang, L. et al. Nanoparticles in medicine: therapeutic applications and developments. Clin. Pharmacol. Ther. 83, 761–769 (2008).
Safra, T. et al. Pegylated liposomal doxorubicin (doxil): reduced clinical cardiotoxicity in patients reaching or exceeding cumulative doses of 500 mg/m2. Ann. Oncol. 11, 1029–1033 (2000).
Barenholz, Y. Doxil(R)–the first FDA-approved nano-drug: lessons learned. J. Control. Release 160, 117–134 (2012).
Hawkins, M.J., Soon-Shiong, P. & Desai, N. Protein nanoparticles as drug carriers in clinical medicine. Adv. Drug Deliv. Rev. 60, 876–885 (2008).
Gradishar, W.J. et al. Phase III trial of nanoparticle albumin-bound paclitaxel compared with polyethylated castor oil-based paclitaxel in women with breast cancer. J. Clin. Oncol. 23, 7794–7803 (2005).
O'Brien, M.E. et al. Reduced cardiotoxicity and comparable efficacy in a phase III trial of pegylated liposomal doxorubicin HCl (CAELYX/Doxil) versus conventional doxorubicin for first-line treatment of metastatic breast cancer. Ann. Oncol. 15, 440–449 (2004).
Ferrari, M. Frontiers in cancer nanomedicine: directing mass transport through biological barriers. Trends Biotechnol. 28, 181–188 (2010).
Bertrand, N., Wu, J., Xu, X., Kamaly, N. & Farokhzad, O.C. Cancer nanotechnology: the impact of passive and active targeting in the era of modern cancer biology. Adv. Drug Deliv. Rev. 66, 2–25 (2014).
Mura, S., Nicolas, J. & Couvreur, P. Stimuli-responsive nanocarriers for drug delivery. Nat. Mater. 12, 991–1003 (2013).
Park, K. Facing the truth about nanotechnology in drug delivery. ACS Nano 7, 7442–7447 (2013).
Venditto, V.J. & Szoka, F.C. Cancer nanomedicines: so many papers and so few drugs!. Adv. Drug Deliv. Rev. 65, 80–88 (2013).
Patel, H.M. & Moghimi, S.M. Serum-mediated recognition of liposomes by phagocytic cells of the reticuloendothelial system - The concept of tissue specificity. Adv. Drug Deliv. Rev. 32, 45–60 (1998).
Tenzer, S. et al. Rapid formation of plasma protein corona critically affects nanoparticle pathophysiology. Nat. Nanotechnol. 8, 772–781 (2013).
Nel, A.E. et al. Understanding biophysicochemical interactions at the nano-bio interface. Nat. Mater. 8, 543–557 (2009). One of the most comprehensive reviews on the subject of nanoparticle protein coronas and implications on nanoparticle fate.
Sahay, G., Alakhova, D.Y. & Kabanov, A.V. Endocytosis of nanomedicines. J. Control. Release 145, 182–195 (2010).
Salvati, A. et al. Transferrin-functionalized nanoparticles lose their targeting capabilities when a biomolecule corona adsorbs on the surface. Nat. Nanotechnol. 8, 137–143 (2013). Excellent study highlighting the dynamic nature of nanoparticles following protein corona formation, and the detrimental effects this has on active targeting strategies.
Docter, D. et al. Quantitative profiling of the protein coronas that form around nanoparticles. Nat. Protoc. 9, 2030–2044 (2014).
Röcker, C., Potzl, M., Zhang, F., Parak, W.J. & Nienhaus, G.U. A quantitative fluorescence study of protein monolayer formation on colloidal nanoparticles. Nat. Nanotechnol. 4, 577–580 (2009).
Harris, J.M. & Chess, R.B. Effect of pegylation on pharmaceuticals. Nat. Rev. Drug Discov. 2, 214–221 (2003).
Hamilton, A. et al. EORTC 10968: a phase I clinical and pharmacokinetic study of polyethylene glycol liposomal doxorubicin (Caelyx, Doxil) at a 6-week interval in patients with metastatic breast cancer. European Organization for Research and Treatment of Cancer. Ann. Oncol. 13, 910–918 (2002).
Guo, S.T. & Huang, L. Nanoparticles escaping RES and endosome: challenges for siRNA delivery for cancer therapy. J. Nanomater. 2011, 742895 (2011).
Li, S.D. & Huang, L. Nanoparticles evading the reticuloendothelial system: role of the supported bilayer. Biochim. Biophys. Acta 1788, 2259–2266 (2009).
Rodriguez, P.L. et al. Minimal “Self” peptides that inhibit phagocytic clearance and enhance delivery of nanoparticles. Science 339, 971–975 (2013). An excellent study involving nanoparticle 'camouflaging' or 'biomimicry' for evasion of the MPS, highlighting consequent enhanced tumor accumulation and efficacy.
Parodi, A. et al. Synthetic nanoparticles functionalized with biomimetic leukocyte membranes possess cell-like functions. Nat. Nanotechnol. 8, 61–68 (2013).
Hu, C.M. et al. Erythrocyte membrane-camouflaged polymeric nanoparticles as a biomimetic delivery platform. Proc. Natl. Acad. Sci. USA 108, 10980–10985 (2011).
Kreuter, J. et al. Apolipoprotein-mediated transport of nanoparticle-bound drugs across the blood-brain barrier. J. Drug Target. 10, 317–325 (2002).
Sica, A. & Bronte, V. Altered macrophage differentiation and immune dysfunction in tumor development. J. Clin. Invest. 117, 1155–1166 (2007).
Woollard, K.J. & Geissmann, F. Monocytes in atherosclerosis: subsets and functions. Nat. Rev. Cardiol. 7, 77–86 (2010).
Prapainop, K., Witter, D.P. & Wentworth, P. Jr. A chemical approach for cell-specific targeting of nanomaterials: small-molecule-initiated misfolding of nanoparticle corona proteins. J. Am. Chem. Soc. 134, 4100–4103 (2012).
Decuzzi, P., Pasqualini, R., Arap, W. & Ferrari, M. Intravascular delivery of particulate systems: does geometry really matter? Pharm. Res. 26, 235–243 (2009).
Arvizo, R.R. et al. Modulating pharmacokinetics, tumor uptake and biodistribution by engineered nanoparticles. PLoS ONE 6, e24374 (2011).
Yao, C. et al. Highly biocompatible zwitterionic phospholipids coated upconversion nanoparticles for efficient bioimaging. Anal. Chem. 86, 9749–9757 (2014).
Decuzzi, P., Lee, S., Bhushan, B. & Ferrari, M. A theoretical model for the margination of particles within blood vessels. Ann. Biomed. Eng. 33, 179–190 (2005).
Tan, J., Shah, S., Thomas, A., Ou-Yang, H.D. & Liu, Y. The influence of size, shape and vessel geometry on nanoparticle distribution. Microfluid. Nanofluidics 14, 77–87 (2013).
Shah, S., Liu, Y., Hu, W. & Gao, J. Modeling particle shape-dependent dynamics in nanomedicine. J. Nanosci. Nanotechnol. 11, 919–928 (2011).
Alexiou, C. et al. Locoregional cancer treatment with magnetic drug targeting. Cancer Res. 60, 6641–6648 (2000).
Gentile, F. et al. The effect of shape on the margination dynamics of non-neutrally buoyant particles in two-dimensional shear flows. J. Biomech. 41, 2312–2318 (2008).
Tasciotti, E. et al. Mesoporous silicon particles as a multistage delivery system for imaging and therapeutic applications. Nat. Nanotechnol. 3, 151–157 (2008).
Chiappini, C. et al. Tailored porous silicon microparticles: fabrication and properties. ChemPhysChem 11, 1029–1035 (2010).
van de Ven, A.L. et al. Rapid tumoritropic accumulation of systemically injected plateloid particles and their biodistribution. J. Control. Release 158, 148–155 (2012).
Tanaka, T. et al. Sustained small interfering RNA delivery by mesoporous silicon particles. Cancer Res. 70, 3687–3696 (2010).
Chen, X. et al. XBP1 promotes triple-negative breast cancer by controlling the HIF1alpha pathway. Nature 508, 103–107 (2014).
Dave, B. et al. Targeting RPL39 and MLF2 reduces tumor initiation and metastasis in breast cancer by inhibiting nitric oxide synthase signaling. Proc. Natl. Acad. Sci. USA 111, 8838–8843 (2014).
von Maltzahn, G. et al. Nanoparticles that communicate in vivo to amplify tumour targeting. Nat. Mater. 10, 545–552 (2011). An inventive approach for targeting of nanoparticles involving 'biological communication' between different injectable constructs for enhanced uptake into tumors.
Murphy, E.A. et al. Nanoparticle-mediated drug delivery to tumor vasculature suppresses metastasis. Proc. Natl. Acad. Sci. USA 105, 9343–9348 (2008).
Thurston, G. et al. Cationic liposomes target angiogenic endothelial cells in tumors and chronic inflammation in mice. J. Clin. Invest. 101, 1401–1413 (1998). An interesting study demonstrating the potential of using surface charge of nanoparticles, in this case cationic liposomes, as a means to target therapeutics to angiogenic tumor vasculature by means of enhanced endothelial cell uptake.
Yokoi, K. et al. Serum biomarkers for personalization of nanotherapeutics-based therapy in different tumor and organ microenvironments. Cancer Lett. 345, 48–55 (2014).
Yokoi, K. et al. Capillary-wall collagen as a biophysical marker of nanotherapeutic permeability into the tumor microenvironment. Cancer Res. 74, 4239–4246 (2014).
Heldin, C.H., Rubin, K., Pietras, K. & Ostman, A. High interstitial fluid pressure - an obstacle in cancer therapy. Nat. Rev. Cancer 4, 806–813 (2004).
Chauhan, V.P. et al. Normalization of tumour blood vessels improves the delivery of nanomedicines in a size-dependent manner. Nat. Nanotechnol. 7, 383–388 (2012).
Jain, R.K. Normalizing tumor microenvironment to treat cancer: bench to bedside to biomarkers. J. Clin. Oncol. 31, 2205–2218 (2013).
Jain, R.K. & Stylianopoulos, T. Delivering nanomedicine to solid tumors. Nat. Rev. Clin. Oncol. 7, 653–664 (2010).
Monsky, W.L. et al. Augmentation of transvascular transport of macromolecules and nanoparticles in tumors using vascular endothelial growth factor. Cancer Res. 59, 4129–4135 (1999).
Diop-Frimpong, B., Chauhan, V.P., Krane, S., Boucher, Y. & Jain, R.K. Losartan inhibits collagen I synthesis and improves the distribution and efficacy of nanotherapeutics in tumors. Proc. Natl. Acad. Sci. USA 108, 2909–2914 (2011).
Miller, C.R., Bondurant, B., McLean, S.D., McGovern, K.A. & O'Brien, D.F. Liposome-cell interactions in vitro: effect of liposome surface charge on the binding and endocytosis of conventional and sterically stabilized liposomes. Biochemistry 37, 12875–12883 (1998).
Gratton, S.E. et al. The effect of particle design on cellular internalization pathways. Proc. Natl. Acad. Sci. USA 105, 11613–11618 (2008).
Osaka, T., Nakanishi, T., Shanmugam, S., Takahama, S. & Zhang, H. Effect of surface charge of magnetite nanoparticles on their internalization into breast cancer and umbilical vein endothelial cells. Colloids Surf. B Biointerfaces 71, 325–330 (2009).
Serda, R.E. et al. The association of silicon microparticles with endothelial cells in drug delivery to the vasculature. Biomaterials 30, 2440–2448 (2009).
Lee, Y. et al. A protein nanocarrier from charge-conversion polymer in response to endosomal pH. J. Am. Chem. Soc. 129, 5362–5363 (2007).
Yuan, Y.Y. et al. Surface charge switchable nanoparticles based on zwitterionic polymer for enhanced drug delivery to tumor. Adv. Mater. 24, 5476–5480 (2012). A highly innovative approach towards site-specific, externally stimulated nanoparticle surface charge conversion that permits for prolonged circulation and heightened tumor cell internalization: a perfect example of design considerations that take into account different barriers to nanoparticle drug delivery.
Le Roy, C. & Wrana, J.L. Clathrin- and non-clathrin-mediated endocytic regulation of cell signalling. Nat. Rev. Mol. Cell Biol. 6, 112–126 (2005).
Gould, G.W. & Lippincott-Schwartz, J. New roles for endosomes: from vesicular carriers to multi-purpose platforms. Nat. Rev. Mol. Cell Biol. 10, 287–292 (2009).
Luo, D. & Saltzman, W.M. Synthetic DNA delivery systems. Nat. Biotechnol. 18, 33–37 (2000).
Bareford, L.M. & Swaan, P.W. Endocytic mechanisms for targeted drug delivery. Adv. Drug Deliv. Rev. 59, 748–758 (2007).
Martens, T.F., Remaut, K., Demeester, J., De Smedt, S.C. & Braeckmans, K. Intracellular delivery of nanomaterials: how to catch endosomal escape in the act. Nano Today 9, 344–364 (2014).
Wasungu, L. & Hoekstra, D. Cationic lipids, lipoplexes and intracellular delivery of genes. J. Control. Release 116, 255–264 (2006).
Chou, L.Y., Ming, K. & Chan, W.C. Strategies for the intracellular delivery of nanoparticles. Chem. Soc. Rev. 40, 233–245 (2011).
Dauty, E., Remy, J.S., Zuber, G. & Behr, J.P. Intracellular delivery of nanometric DNA particles via the folate receptor. Bioconjug. Chem. 13, 831–839 (2002).
Gradishar, W.J. Albumin-bound paclitaxel: a next-generation taxane. Expert Opin. Pharmacother. 7, 1041–1053 (2006).
Ibrahim, N.K. et al. Multicenter phase II trial of ABI-007, an albumin-bound paclitaxel, in women with metastatic breast cancer. J. Clin. Oncol. 23, 6019–6026 (2005). Clinical trial of nanoparticle albumin-bound paclitaxel in metastatic breast cancer patients, highlighting not only the therapeutic potential of paclitaxel, but its benefits with regards to reduced side effects compared to the conventional formulation containing Cremophor EL.
Szakács, G., Paterson, J.K., Ludwig, J.A., Booth-Genthe, C. & Gottesman, M.M. Targeting multidrug resistance in cancer. Nat. Rev. Drug Discov. 5, 219–234 (2006).
Rees, D.C., Johnson, E. & Lewinson, O. ABC transporters: the power to change. Nat. Rev. Mol. Cell Biol. 10, 218–227 (2009).
Aller, S.G. et al. Structure of P-glycoprotein reveals a molecular basis for poly-specific drug binding. Science 323, 1718–1722 (2009).
Gottesman, M.M., Fojo, T. & Bates, S.E. Multidrug resistance in cancer: role of ATP-dependent transporters. Nat. Rev. Cancer 2, 48–58 (2002).
Fletcher, J.I., Haber, M., Henderson, M.J. & Norris, M.D. ABC transporters in cancer: more than just drug efflux pumps. Nat. Rev. Cancer 10, 147–156 (2010).
Dean, M., Fojo, T. & Bates, S. Tumour stem cells and drug resistance. Nat. Rev. Cancer 5, 275–284 (2005).
Wu, J. et al. Reversal of multidrug resistance by transferrin-conjugated liposomes co-encapsulating doxorubicin and verapamil. J. Pharm. Pharm. Sci. 10, 350–357 (2007).
Wong, H.L., Bendayan, R., Rauth, A.M. & Wu, X.Y. Simultaneous delivery of doxorubicin and GG918 (Elacridar) by new polymer-lipid hybrid nanoparticles (PLN) for enhanced treatment of multidrug-resistant breast cancer. J. Control. Release 116, 275–284 (2006).
Patel, N.R., Rathi, A., Mongayt, D. & Torchilin, V.P. Reversal of multidrug resistance by co-delivery of tariquidar (XR9576) and paclitaxel using long-circulating liposomes. Int. J. Pharm. 416, 296–299 (2011).
Xiong, X.B. & Lavasanifar, A. Traceable multifunctional micellar nanocarriers for cancer-targeted co-delivery of MDR-1 siRNA and doxorubicin. ACS Nano 5, 5202–5213 (2011).
Batrakova, E.V. & Kabanov, A.V. Pluronic block copolymers: evolution of drug delivery concept from inert nanocarriers to biological response modifiers. J. Control. Release 130, 98–106 (2008).
Sosnik, A. Reversal of multidrug resistance by the inhibition of ATP-binding cassette pumps employing “Generally Recognized As Safe” (GRAS) nanopharmaceuticals: A review. Adv. Drug Deliv. Rev. 65, 1828–1851 (2013).
Lee, Y., Park, S.Y., Mok, H. & Park, T.G. Synthesis, characterization, antitumor activity of pluronic mimicking copolymer micelles conjugated with doxorubicin via acid-cleavable linkage. Bioconjug. Chem. 19, 525–531 (2008).
Tian, Y., Bromberg, L., Lin, S.N., Hatton, T.A. & Tam, K.C. Complexation and release of doxorubicin from its complexes with pluronic P85-b-poly(acrylic acid) block copolymers. J. Control. Release 121, 137–145 (2007).
Longmire, M., Choyke, P.L. & Kobayashi, H. Clearance properties of nano-sized particles and molecules as imaging agents: considerations and caveats. Nanomedicine (Lond.) 3, 703–717 (2008).
Black, K.C. et al. Radioactive 198Au-doped nanostructures with different shapes for in vivo analyses of their biodistribution, tumor uptake, and intratumoral distribution. ACS Nano 8, 4385–4394 (2014).
Xiao, K. et al. The effect of surface charge on in vivo biodistribution of PEG-oligocholic acid based micellar nanoparticles. Biomaterials 32, 3435–3446 (2011).
Sheridan, C. Gene therapy finds its niche. Nat. Biotechnol. 29, 121–128 (2011).
Kay, M.A., Glorioso, J.C. & Naldini, L. Viral vectors for gene therapy: the art of turning infectious agents into vehicles of therapeutics. Nat. Med. 7, 33–40 (2001).
Levine, R.M., Pearce, T.R., Adil, M. & Kokkoli, E. Preparation and characterization of liposome-encapsulated plasmid DNA for gene delivery. Langmuir 29, 9208–9215 (2013).
Dobson, J. Gene therapy progress and prospects: magnetic nanoparticle-based gene delivery. Gene Ther. 13, 283–287 (2006).
Pissuwan, D., Niidome, T. & Cortie, M.B. The forthcoming applications of gold nanoparticles in drug and gene delivery systems. J. Control. Release 149, 65–71 (2011).
Lechardeur, D. et al. Metabolic instability of plasmid DNA in the cytosol: a potential barrier to gene transfer. Gene Ther. 6, 482–497 (1999).
Anderson, D.J. & Hetzer, M.W. Nuclear envelope formation by chromatin-mediated reorganization of the endoplasmic reticulum. Nat. Cell Biol. 9, 1160–1166 (2007).
Raices, M. & D'Angelo, M.A. Nuclear pore complex composition: a new regulator of tissue-specific and developmental functions. Nat. Rev. Mol. Cell Biol. 13, 687–699 (2012).
Hu, Y., Haynes, M.T., Wang, Y., Liu, F. & Huang, L. A highly efficient synthetic vector: nonhydrodynamic delivery of DNA to hepatocyte nuclei in vivo. ACS Nano 7, 5376–5384 (2013).
Choi, H.S. et al. Renal clearance of quantum dots. Nat. Biotechnol. 25, 1165–1170 (2007).
Braet, F. et al. Contribution of high-resolution correlative imaging techniques in the study of the liver sieve in three-dimensions. Microsc. Res. Tech. 70, 230–242 (2007).
Chen, L.T. & Weiss, L. The role of the sinus wall in the passage of erythrocytes through the spleen. Blood 41, 529–537 (1973).
Hobbs, S.K. et al. Regulation of transport pathways in tumor vessels: role of tumor type and microenvironment. Proc. Natl. Acad. Sci. USA 95, 4607–4612 (1998).
Cabral, H. et al. Accumulation of sub-100 nm polymeric micelles in poorly permeable tumours depends on size. Nat. Nanotechnol. 6, 815–823 (2011). Excellent study that highlights the effect of nanoparticle size on accumulation and penetration of nanoparticles in hypovascular tumors.
Maeda, H., Wu, J., Sawa, T., Matsumura, Y. & Hori, K. Tumor vascular permeability and the EPR effect in macromolecular therapeutics: a review. J. Control. Release 65, 271–284 (2000).
Geng, Y. et al. Shape effects of filaments versus spherical particles in flow and drug delivery. Nat. Nanotechnol. 2, 249–255 (2007).
Champion, J.A. & Mitragotri, S. Role of target geometry in phagocytosis. Proc. Natl. Acad. Sci. USA 103, 4930–4934 (2006). Seminal work on the effect of particle geometry on macrophage uptake, demonstrating that the architectural design parameter of curvature drives phagocytosis.
Champion, J.A. & Mitragotri, S. Shape induced inhibition of phagocytosis of polymer particles. Pharm. Res. 26, 244–249 (2009).
Christian, D.A. et al. Flexible filaments for in vivo imaging and delivery: persistent circulation of filomicelles opens the dosage window for sustained tumor shrinkage. Mol. Pharm. 6, 1343–1352 (2009).
Park, J.H. et al. Systematic surface engineering of magnetic nanoworms for in vivo tumor targeting. Small 5, 694–700 (2009).
Alexis, F., Pridgen, E., Molnar, L.K. & Farokhzad, O.C. Factors affecting the clearance and biodistribution of polymeric nanoparticles. Mol. Pharm. 5, 505–515 (2008).
Yamamoto, Y., Nagasaki, Y., Kato, Y., Sugiyama, Y. & Kataoka, K. Long-circulating poly(ethylene glycol)-poly(d,l-lactide) block copolymer micelles with modulated surface charge. J. Control. Release 77, 27–38 (2001).
Moghimi, S.M., Hunter, A.C. & Murray, J.C. Long-circulating and target-specific nanoparticles: theory to practice. Pharmacol. Rev. 53, 283–318 (2001).
Zhang, L. et al. Softer zwitterionic nanogels for longer circulation and lower splenic accumulation. ACS Nano 6, 6681–6686 (2012).
Merkel, T.J. et al. The effect of particle size on the biodistribution of low-modulus hydrogel PRINT particles. J. Control. Release 162, 37–44 (2012).
Cui, J. et al. Super-soft hydrogel particles with tunable elasticity in a microfluidic blood capillary model. Adv. Mater. 26, 7295–7299 (2014).
Attia, A.B.E. et al. The effect of kinetic stability on biodistribution and anti-tumor efficacy of drug-loaded biodegradable polymeric micelles. Biomaterials 34, 3132–3140 (2013).
van Nostrum, C.F. Covalently cross-linked amphiphilic block copolymer micelles. Soft Matter 7, 3246–3259 (2011).
Acknowledgements
M.F. is grateful for the Ernest Cockrell Jr. Distinguished Endowed Chair in the Department of Nanomedicine at the Houston Methodist Research Institute. The authors acknowledge financial support from Department of Defense grant W81XWH-12-1-0414, and US National Institutes of Health grants NIH U54CA143837 and NIH U54CA151668. E.B. is grateful for the support of the Susan G. Komen Breast Cancer Foundation (grant KG101394). The authors are grateful for the assistance of F.E. Cara, V. Segura-Ibarra and Suhong Wu in manuscript preparation. M.G. Landry is acknowledged for manuscript schematics.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
About this article
Cite this article
Blanco, E., Shen, H. & Ferrari, M. Principles of nanoparticle design for overcoming biological barriers to drug delivery. Nat Biotechnol 33, 941–951 (2015). https://doi.org/10.1038/nbt.3330
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nbt.3330
This article is cited by
-
Breaking through the basement membrane barrier to improve nanotherapeutic delivery to tumours
Nature Nanotechnology (2024)
-
Small interfering RNA (siRNA) as a potential gene silencing strategy for diabetes and associated complications: challenges and future perspectives
Journal of Diabetes & Metabolic Disorders (2024)
-
Nanotechnology-driven improvisation of red algae-derived carrageenan for industrial and bio-medical applications
World Journal of Microbiology and Biotechnology (2024)
-
M2-type macrophage membrane-mediated delivery of Carvedilol nanocomplex for acute liver failure treatment and remodeling inflammatory microenvironment
Nano Research (2024)
-
Multi-channel Small Animal Drug Metabolism Real-Time Monitoring Fluorescence System
Molecular Imaging and Biology (2024)