Abstract
Cancer incidence is rising and this global challenge is further exacerbated by tumour resistance to available medicines. A promising approach to meet the need for improved cancer treatment is drug repurposing. Here we highlight the potential for repurposing disulfiram (also known by the trade name Antabuse), an old alcohol-aversion drug that has been shown to be effective against diverse cancer types in preclinical studies. Our nationwide epidemiological study reveals that patients who continuously used disulfiram have a lower risk of death from cancer compared to those who stopped using the drug at their diagnosis. Moreover, we identify the ditiocarb–copper complex as the metabolite of disulfiram that is responsible for its anti-cancer effects, and provide methods to detect preferential accumulation of the complex in tumours and candidate biomarkers to analyse its effect on cells and tissues. Finally, our functional and biophysical analyses reveal the molecular target of disulfiram’s tumour-suppressing effects as NPL4, an adaptor of p97 (also known as VCP) segregase, which is essential for the turnover of proteins involved in multiple regulatory and stress-response pathways in cells.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Collins, F. S. Mining for therapeutic gold. Nat. Rev. Drug Discov. 10, 397 (2011)
Pantziarka, P. et al. The repurposing drugs in oncology (ReDO) project. Ecancermedicalscience 8, 442 (2014)
Iljin, K. et al. High-throughput cell-based screening of 4910 known drugs and drug-like small molecules identifies disulfiram as an inhibitor of prostate cancer cell growth. Clin. Cancer Res. 15, 6070–6078 (2009)
Cvek, B. Nonprofit drugs as the salvation of the world’s healthcare systems: the case of Antabuse (disulfiram). Drug Discov. Today 17, 409–412 (2012)
Shen, M. L., Johnson, K. L., Mays, D. C., Lipsky, J. J. & Naylor, S. Determination of in vivo adducts of disulfiram with mitochondrial aldehyde dehydrogenase. Biochem. Pharmacol. 61, 537–545 (2001)
Chen, D., Cui, Q. C., Yang, H. & Dou, Q. P. Disulfiram, a clinically used anti-alcoholism drug and copper-binding agent, induces apoptotic cell death in breast cancer cultures and xenografts via inhibition of the proteasome activity. Cancer Res. 66, 10425–10433 (2006)
Zha, J. et al. Disulfiram targeting lymphoid malignant cell lines via ROS–JNK activation as well as Nrf2 and NF-κB pathway inhibition. J. Transl. Med. 12, 163 (2014)
Safi, R. et al. Copper signaling axis as a target for prostate cancer therapeutics. Cancer Res. 74, 5819–5831 (2014)
Liu, P. et al. Liposome encapsulated disulfiram inhibits NFκB pathway and targets breast cancer stem cells in vitro and in vivo. Oncotarget 5, 7471–7485 (2014)
Dufour, P. et al. Sodium dithiocarb as adjuvant immunotherapy for high risk breast cancer: a randomized study. Biotherapy 6, 9–12 (1993)
Yip, N. C. et al. Disulfiram modulated ROS–MAPK and NFκB pathways and targeted breast cancer cells with cancer stem cell-like properties. Br. J. Cancer 104, 1564–1574 (2011)
Lövborg, H. et al. Inhibition of proteasome activity, nuclear factor-κB translocation and cell survival by the antialcoholism drug disulfiram. Int. J. Cancer 118, 1577–1580 (2006)
Allensworth, J. L. et al. Disulfiram (DSF) acts as a copper ionophore to induce copper-dependent oxidative stress and mediate anti-tumor efficacy in inflammatory breast cancer. Mol. Oncol. 9, 1155–1168 (2015)
Nechushtan, H. et al. A phase IIb trial assessing the addition of disulfiram to chemotherapy for the treatment of metastatic non-small cell lung cancer. Oncologist 20, 366–367 (2015)
Jin, M. et al. Alcohol drinking and all cancer mortality: a meta-analysis. Ann. Oncol. 24, 807–816 (2013)
Li, Y. et al. Copper improves the anti-angiogenic activity of disulfiram through the EGFR/Src/VEGF pathway in gliomas. Cancer Lett. 369, 86–96 (2015)
Suzuki, Y. et al. The origin of an EPR signal observed in dithiocarbamate-loaded tissues. Copper(ii)-dithiocarbamate complexes account for the narrow hyperfine lines. Biochim. Biophys. Acta 1335, 242–245 (1997)
Kepp, O., Galluzzi, L., Lipinski, M., Yuan, J. & Kroemer, G. Cell death assays for drug discovery. Nat. Rev. Drug Discov. 10, 221–237 (2011)
Doil, C. et al. RNF168 binds and amplifies ubiquitin conjugates on damaged chromosomes to allow accumulation of repair proteins. Cell 136, 435–446 (2009)
Li, J. M., Wu, H., Zhang, W., Blackburn, M. R. & Jin, J. The p97–UFD1L–NPL4 protein complex mediates cytokine-induced IκBα proteolysis. Mol. Cell. Biol. 34, 335–347 (2014)
Chou, T. F. & Deshaies, R. J. Quantitative cell-based protein degradation assays to identify and classify drugs that target the ubiquitin–proteasome system. J. Biol. Chem. 286, 16546–16554 (2011)
Kisselev, A. F. & Goldberg, A. L. Monitoring activity and inhibition of 26S proteasomes with fluorogenic peptide substrates. Methods Enzymol. 398, 364–378 (2005)
Asher, G ., Lotem, J ., Cohen, B ., Sachs, L. & Shaul, Y. Regulation of p53 stability and p53-dependent apoptosis by NADH quinone oxidoreductase 1. Proc. Natl Acad. Sci. USA 98, 1188–1193 (2001)
Asher, G ., Tsvetkov, P ., Kahana, C. & Shaul, Y. A mechanism of ubiquitin-independent proteasomal degradation of the tumor suppressors p53 and p73. Genes Dev. 19, 316–321 (2005)
Verma, R. et al. Role of Rpn11 metalloprotease in deubiquitination and degradation by the 26S proteasome. Science 298, 611–615 (2002)
Dai, R. M. & Li, C. C. Valosin-containing protein is a multi-ubiquitin chain-targeting factor required in ubiquitin–proteasome degradation. Nat. Cell Biol. 3, 740–744 (2001)
Alexandru, G . et al. UBXD7 binds multiple ubiquitin ligases and implicates p97 in HIF1α turnover. Cell 134, 804–816 (2008)
Chou, T. F. et al. Reversible inhibitor of p97, DBeQ, impairs both ubiquitin-dependent and autophagic protein clearance pathways. Proc. Natl Acad. Sci. USA 108, 4834–4839 (2011)
Riemer, A. et al. The p97–Ufd1–Npl4 ATPase complex ensures robustness of the G2/M checkpoint by facilitating CDC25A degradation. Cell Cycle 13, 919–927 (2014)
Radhakrishnan, S. K., den Besten, W. & Deshaies, R. J. p97-dependent retrotranslocation and proteolytic processing govern formation of active Nrf1 upon proteasome inhibition. eLife 3, e01856 (2014)
Meyer, H., Bug, M. & Bremer, S. Emerging functions of the VCP/p97 AAA-ATPase in the ubiquitin system. Nat. Cell Biol. 14, 117–123 (2012)
Magnaghi, P. et al. Covalent and allosteric inhibitors of the ATPase VCP/p97 induce cancer cell death. Nat. Chem. Biol. 9, 548–556 (2013)
Samali, A., Fitzgerald, U., Deegan, S. & Gupta, S. Methods for monitoring endoplasmic reticulum stress and the unfolded protein response. Int. J. Cell Biol. 2010, 830307 (2010)
Auner, H. W. et al. Combined inhibition of p97 and the proteasome causes lethal disruption of the secretory apparatus in multiple myeloma cells. PLoS ONE 8, e74415 (2013)
Soriano, G. P. et al. Proteasome inhibitor-adapted myeloma cells are largely independent from proteasome activity and show complex proteomic changes, in particular in redox and energy metabolism. Leukemia 30, 2198–2207 (2016)
Lass, A., McConnell, E., Fleck, K., Palamarchuk, A. & Wójcik, C. Analysis of Npl4 deletion mutants in mammalian cells unravels new Ufd1-interacting motifs and suggests a regulatory role of Npl4 in ERAD. Exp. Cell Res. 314, 2715–2723 (2008)
Vorácˇková, I., Suchanová, S., Ulbrich, P., Diehl, W. E. & Ruml, T. Purification of proteins containing zinc finger domains using immobilized metal ion affinity chromatography. Protein Expr. Purif. 79, 88–95 (2011)
Holdgate, G. et al. Biophysical methods in drug discovery from small molecule to pharmaceutical. Methods Mol. Biol. 1008, 327–355 (2013)
Lomenick, B. et al. Target identification using drug affinity responsive target stability (DARTS). Proc. Natl Acad. Sci. USA 106, 21984–21989 (2009)
Becker, L. A. et al. Therapeutic reduction of ataxin-2 extends lifespan and reduces pathology in TDP-43 mice. Nature 544, 367–371 (2017)
Guo, L. et al. A cellular system that degrades misfolded proteins and protects against neurodegeneration. Mol. Cell 55, 15–30 (2014)
Kim, Y. E., Hipp, M. S., Bracher, A., Hayer-Hartl, M. & Hartl, F. U. Molecular chaperone functions in protein folding and proteostasis. Annu. Rev. Biochem. 82, 323–355 (2013)
Dai, C. & Sampson, S. B. HSF1: guardian of proteostasis in cancer. Trends Cell Biol. 26, 17–28 (2016)
Cvek, B. Targeting malignancies with disulfiram (Antabuse): multidrug resistance, angiogenesis, and proteasome. Curr. Cancer Drug Targets 11, 332–337 (2011)
Deshaies, R. J. Proteotoxic crisis, the ubiquitin–proteasome system, and cancer therapy. BMC Biol. 12, 94 (2014)
Anderson, D. J . et al. Targeting the AAA ATPase p97 as an approach to treat cancer through disruption of protein homeostasis. Cancer Cell 28, 653–665 (2015)
Cui, Y. et al. High expression of valosin-containing protein predicts poor prognosis in patients with breast carcinoma. Tumour Biol. 36, 9919–9927 (2015)
Yamamoto, S. et al. Expression of valosin-containing protein in colorectal carcinomas as a predictor for disease recurrence and prognosis. Clin. Cancer Res. 10, 651–657 (2004)
Tsujimoto, Y. et al. Elevated expression of valosin-containing protein (p97) is associated with poor prognosis of prostate cancer. Clin. Cancer Res. 10, 3007–3012 (2004)
Thygesen, L. C., Daasnes, C., Thaulow, I. & Brønnum-Hansen, H. Introduction to Danish (nationwide) registers on health and social issues: structure, access, legislation, and archiving. Scand. J. Public Health 39 (Suppl), 12–16 (2011)
Rosenbaum, P. R. & Rubin, D. B. The central role of the propensity score in observational studies for causal effects. Biometrika 70, 41–55 (1983)
R Core Team . R: A language and environment for statistical computing. R Foundation for Statistical Computinghttps://www.R-project.org/ R v.3.2.3 (2015-12-10) (R Foundation for Statistical Computing, 2016)
Cvek, B., Milacic, V., Taraba, J. & Dou, Q. P. Ni(ii), Cu(ii), and Zn(ii) diethyldithiocarbamate complexes show various activities against the proteasome in breast cancer cells. J. Med. Chem. 51, 6256–6258 (2008)
Acknowledgements
We thank J. Škvor, M. Zadinová, J. Vecˇerka and D. Doležal for help with animal experiments, Jana Vrbkova for statistical analysis, D. Fridecky and T. Adam for help with HPLC, I. Protivankova and M. Grønvig Nielsen for technical assistance. This work was supported by grants from the Kellner Family Foundation, Czech National Program of Sustainability, Grant Agency of the Czech Republic, MEYS CR project Czech-BioImaging, the Czech Health Research Council, of the Danish Cancer Society, the Danish National Research Foundation (project CARD), the Danish Council for Independent Research, the Novo Nordisk Foundation, the Czech Cancer League, the Swedish Research Council, Cancerfonden of Sweden, the European Commission (EATRIS), the Czech Ministry of Education, youth and sports (OPVKCZ), Cancer Research Czech Republic and the Howard Hughes Medical Institute.
Author information
Authors and Affiliations
Contributions
Z.S., M.Mis., B.C., R.J.D. and J.Barte. conceived the study. Z.S. and M.Mis. performed most biochemical and microscopy experiments and wrote the manuscript. D.M. established the expression cell lines and performed most cytotoxicity tests. T.O., P.D. and I.V. performed the HPLC experiments. K.K.A., S.F. and J.O. performed the epidemiological analyses. J.Bartk. performed the immunohistochemical analyses. J.V. and P.D. performed DARTS experiments. P.M. performed cell death analyses. Z.T. performed cytotoxicity tests and heat-shock response analyses. A.K. performed cytotoxicity tests. A.M. designed and performed phlebotomies of patients treated with Antabuse. M.Mic. performed the ITC. J.G. performed FACS analyses, cell death assays and cell sorting. J.S. performed 20S proteasome assays. J.L. performed 26S proteasome assays. M.K. and C.D. performed the cytotoxicity experiments on myeloid- and patient-derived cell lines. P.P., J.M. and M.H. performed mouse experiments. J.Barte., B.C., Q.P.D. and R.J.D. helped to design the experiments, interpreted the data and wrote/edited the manuscript. All authors approved the manuscript.
Corresponding authors
Ethics declarations
Competing interests
R.J.D. is a founder of and consultant for Cleave Biosciences. The other authors declare no competing financial interests.
Additional information
Reviewer Information Nature thanks P. Brossart and the other anonymous reviewer(s) for their contribution to the peer review of this work.
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data figures and tables
Extended Data Figure 1 Epidemiological and pre-clinical data of the anti-cancer effects of DSF.
a, Summary of hazard ratios (HR) and 95% confidence intervals (CI) for cancer-specific mortality among Danish patients with cancer, comparing continuing and previous users of DSF for selected types of cancer (for statistical analysis and definitions of DSF exposure categories, see Methods). b, Photographs of subcutaneously growing human MDA-MB-231 tumours extracted from mice at day 32.c, Time-course diagram of mouse weight. n = 8 animals per group. d, Model of CuET formation during metabolic processing of orally administered DSF in the human body. e, Examples of mass-spectrometry spectra of CuET expressed as peaks of 4 MRM transitions in mouse serum after CuET spikes, compared to orally applied DSF (50 mg kg−1). Data are representative of two independent experiments. f, Pharmacokinetic analysis of CuET levels in mouse serum after orally applied DSF (50 mg kg−1). n = 2 animals per time point. g, Effect of DTC and CuET on MDA-MB-231 cells analysed by colony formation assay. n = 3 independent experiments. h, Time-course diagram of weight in CuET- and vehicle-treated mice. n = 10 animals per group. i, Extended time-course diagram of weight in CuET- and vehicle-treated mice. n = 10 animals per group. Data are mean ± s.d. (c, h, i) or linked means (g).
Extended Data Figure 2 CuET is the major anti-cancer metabolite of DSF.
a, CuET cytotoxicity measured by a colony-formation assay in human cell lines derived from breast, lung, colon and prostate carcinomas. Data are mean ± s.d. of three independent experiments (breast) or presented individually for two independent biological experiments for each cell line (lung, colon and prostate). b, IC50 values from two independent biological experiments documenting differential CuET-induced cytotoxicity across a panel of cancer and non-cancerous cell lines (48 h treatment). c, Analysis of annexin V signal in AMO-1 cells exposed to toxic doses of NMS873 (5 μM, 16 h) or CuET (100 nM, 16 h) and in U2OS cell exposed to toxic doses of NMS873 (10 μM, 16 h) or CuET (1 μM, 16 h). d, Analysis of caspase 3/7 activity in selected cell lines after apoptosis induction by NMS873 (AMO-1: 6 h, 5 μM; Capan1: 16 h, 10 μM; U2OS: 16 h, 10 μM; MDA-MB-231: 24 h, 10 μM) or CuET (AMO-1: 16 h, 100 nM; Capan1: 16 h, 250 nM; U2OS: 16 h, 1 μM; MDA-MB-231: 24 h, 1 μM). e, Absence of cleaved PARP1 after a toxic dose of CuET in U2OS cells, compared to etoposide treatment as a positive control. f, Analysis of cytochrome c (in red) release from mitochondria in U2OS cells during cell death induced by the positive control staurosporin (STS, 1 μM) compared to cell death induced by CuET (1 μM). Blue, DAPI. Scale bar, 10μm. c–f, Data are representative of two independent biological experiments.
Extended Data Figure 3 CuET-induced proteasome inhibition-like response is not due to proteasome inhibition.
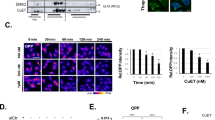
a, Kinetics of poly-Ub protein accumulation in U2OS cells treated with CuET or the proteasome inhibitor BTZ. b, CuET treatment (1.5 h) induces rapid deubiquitylation of ubiquitylated histone H2A (uH2A) similarly to proteasome inhibitors BTZ or MG132 in U2OS cells. c, CuET treatment (1.5 h) induces rapid cytoplasmic accumulation of poly-ubiquitylated proteins (FK2 antibody staining) in U2OS cells, similar to BTZ and MG132 treatment. Scale bar, 10μm. d, e, 20S proteasome activity is not inhibited by CuET as examined in live MDA-MB-231 cells (d) or in lysates from MDA-MB-231 cells (e). Data are mean ± s.d. of four independent experiments. f, CuET treatment (1 μM, 6 h) does not cause accumulation of p53 in the presence of dicoumarol (300 μM) in MCF7 cells. g, In vitro 26S proteasome function measured as RPN11 deubiquitylation activity, is not inhibited by CuET; 1,10-phenanthroline (1,10-OPT) served as a positive control. Data are representative of two (a–c, f) or three (g) independent experiments.
Extended Data Figure 4 CuET inhibits the p97 pathway and induces cellular UPR.
a, MG132-treated cells (5 μM, 6 h) accumulate both forms of NRF1 (120-kDa and 110-kDa bands, top and bottom arrows, respectively), whereas CuET-treated cells (1 μM, 6 h) accumulate only the non-cleaved 120-kDa form. b, Inhibition of the NRF1 cleavage process (appearance of the lower band) by CuET and NMS873 (a p97 inhibitor; 5 μM) in mouse NIH3T3 cells co-treated with the proteasome inhibitor MG132 (5 μM for 6 h). c, Time-course example images from a FRAP experiment, for which the quantitative analysis is shown in Fig. 2g (U2OS cells, blue boxes mark areas before bleaching, arrows after bleaching). d, U2OS cells pre-extracted with Triton X-100 and stained for poly-Ub(K48). The antibody signal intensities for cells treated with DMSO, BTZ (1 μM), NMS873 (10 μM) and CuET (1 μM) are analysed by microscopy-based cytometry and plotted below. e, Western blot analysis of accumulated poly-Ub proteins in the ultracentrifugation-separated microsomal fraction from U2OS cells treated with mock, CuET (1 μM), NMS873 (10 μM) or BTZ (1 μM) for 3 h. f, UPR in U2OS and MDA-MB-231 cell lines induced by 6-h treatment with CuET (various concentrations) or positive controls (5 μM NMS873, 2 μg ml−1 tunicamycin, 1 μM thapsigargin) is shown by increased levels of XBP1s, ATF4 and p-eIF2α. a–f, Data are representative of two independent experiments.
Extended Data Figure 5 CuET kills BTZ-resistant cells.
a, BTZ-adapted (BTZres), CFZ-adapted (CFZres) and non-adapted AMO-1 human myeloma cells are equally sensitive to treatment with CuET. b, BTZ-adapted, CFZ-adapted and non-adapted ARH77 human plasmocytoma cells are equally sensitive to treatment with CuET. c, BTZ-adapted and non-adapted RPMI8226 human myeloma cells are equally sensitive to treatment with CuET. d, Human myeloma cells derived from a patient with BTZ-resistant myeloma show CuET sensitivity comparable to myeloma cells derived from a patient with BTZ-sensitive myeloma. Data are means linked of three independent experiments (a–c) or data are from two independent experiments (d).
Extended Data Figure 6 CuET targets NPL4, causing immobilization and nuclear clustering of NPL4.
a, CuET (1 μM) does not inhibit ATPase activity of p97. NMS873 (5 μM) was used as a positive control. Data are mean ± s.d. from four independent experiments. b, Western blotting analysis showing levels of ectopic p97–GFP, NPL4–GFP and UFD1–GFP in stable U2OS-derived cell lines used for the CuET-treatment rescue and cluster formation experiments. c, Ectopic expression of NPL4–GFP alleviates CuET-induced (125 nM, 4 h) accumulation of poly-Ub proteins in U2OS cells. d, Distribution of NPL4 nuclear clusters relative to chromatin in cells treated with CuET (1 μM, 2 h). Scale bars, 2 μm. e, Schematic representation of site-directed mutagenesis within the amino acid sequence of the putative zinc finger domain of NPL4. f, ITC curve showing the lack of CuET binding to purified NPL4(MUT) protein. g, DARTS analysis of recombinant NPL4 proteins shows that differential pronase-mediated proteolysis after CuET addition is apparent for NPL4(WT) but not for NPL4(MUT); detected by either silver-stained SDS–PAGE (the most prominent differential bands are marked by red dots) or by blotting with an anti-NPL4 polyclonal antibody. h, Viability of cells expressing doxycycline-inducible NPL4(MUT)–GFP, treated with CuET for 48 h. Data are from three independent experiments, means are linked. i, Accumulation of K48-ubiquitinated proteins and activation of UPR in cells expressing the doxycycline-inducible NPL4(MUT)–GFP. b–d, f, g, i, Data are representative of two independent experiments.
Extended Data Figure 7 Immobilized NPL4 forms insoluble protein aggregates.
a, NPL4–GFP aggregates induced by CuET treatment (1 μM, 3 h) do not co-localize with nuclear speckles (stained by SC-35 antibody) or nucleoli (visible as a DAPI− nuclear signal). b, NPL4–GFP nuclear aggregates induced by CuET (1 μM, 3 h) are excluded from chromatin in early prometaphase U2OS cells. c, Co-localization of spontaneous NPL4(MUT)–GFP aggregates with SUMO2/3, poly-UB(K48) and TDP43 in pre-extracted U2OS cells. d, NPL4–GFP aggregates are formed independently of ubiquitylation, as shown in CuET-treated (1 μM, 3 h) cells pre-treated with a chemical UBA1 inhibitor (MLN7243, 10 μM, 1 h). The lack of cellular FK2 staining of ubiquitylated proteins validates the efficacy of the MLN7243 inhibitor. e, Co-localization of FK2 signal with the spontaneous NPL4(MUT)–GFP aggregates in pre-extracted U2OS cells. f, Analysis of p97 in CuET-induced (1 μM, 3 h) NPL4–GFP aggregates in pre-extracted U2OS cells. g, Analysis of p97 in spontaneous NPL4(MUT)–GFP aggregates in pre-extracted U2OS cells. a–g, Data are representative of two independent biological experiments.
Extended Data Figure 8 NPL4 aggregation immobilizes the p97 binding partner and induces a global cellular HSR.
a, Immobilization of selected proteins in Triton X-100-resistant pellet fractions of CuET-treated (1 μM, 3 h) U2OS cells. b, Immobilization of selected proteins in Triton X-100-resistant pellet fractions from U2OS cells expressing doxycycline-inducible NPL4(MUT)–GFP (48 h after induction). c, CuET dose-dependent immobilization of p97 in Triton X-100 pre-extracted MDA-MB-231 cells (3 h). Scale bar, 10μm. d, Immunohistochemical staining showing non-extractable p97 in MDA-MB-231 xenografts from mice treated with DSF or DSF and CuGlu, compared to vehicle. Scale bar, 50μm. e, HSR after CuET (8 h treatment) is shown by various HSR markers detected by western blotting of U2OS cell extracts. f, HSR markers in U2OS cells expressing doxycycline-inducible NPL4(MUT)–GFP (24 h after induction). a–f, Data are representative of two independent biological experiments.
Supplementary information
Supplementary Figure 1
This file contains the uncropped gels and gating strategy example. (PDF 2563 kb)
Rights and permissions
About this article
Cite this article
Skrott, Z., Mistrik, M., Andersen, K. et al. Alcohol-abuse drug disulfiram targets cancer via p97 segregase adaptor NPL4. Nature 552, 194–199 (2017). https://doi.org/10.1038/nature25016
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nature25016
This article is cited by
-
Augmenting MEK inhibitor efficacy in BRAF wild-type melanoma: synergistic effects of disulfiram combination therapy
Journal of Experimental & Clinical Cancer Research (2024)
-
LIFU/MMP-2 dual-responsive release of repurposed drug disulfiram from nanodroplets for inhibiting vasculogenic mimicry and lung metastasis in triple-negative breast cancer
Journal of Nanobiotechnology (2024)
-
Mechanistic insights and the clinical prospects of targeted therapies for glioblastoma: a comprehensive review
Experimental Hematology & Oncology (2024)
-
Cuproptosis: unveiling a new frontier in cancer biology and therapeutics
Cell Communication and Signaling (2024)
-
Drug repurposing for cancer therapy
Signal Transduction and Targeted Therapy (2024)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.