Abstract
Cancer cells exploit the expression of the programmed death-1 (PD-1) ligand 1 (PD-L1) to subvert T-cell-mediated immunosurveillance1,2. The success of therapies that disrupt PD-L1-mediated tumour tolerance has highlighted the need to understand the molecular regulation of PD-L1 expression1. Here we identify the uncharacterized protein CMTM6 as a critical regulator of PD-L1 in a broad range of cancer cells, by using a genome-wide CRISPR–Cas9 screen. CMTM6 is a ubiquitously expressed protein that binds PD-L1 and maintains its cell surface expression. CMTM6 is not required for PD-L1 maturation but co-localizes with PD-L1 at the plasma membrane and in recycling endosomes, where it prevents PD-L1 from being targeted for lysosome-mediated degradation. Using a quantitative approach to profile the entire plasma membrane proteome, we find that CMTM6 displays specificity for PD-L1. Notably, CMTM6 depletion decreases PD-L1 without compromising cell surface expression of MHC class I. CMTM6 depletion, via the reduction of PD-L1, significantly alleviates the suppression of tumour-specific T cell activity in vitro and in vivo. These findings provide insights into the biology of PD-L1 regulation, identify a previously unrecognized master regulator of this critical immune checkpoint and highlight a potential therapeutic target to overcome immune evasion by tumour cells.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
Accession codes
References
Sharma, P. & Allison, J. P. The future of immune checkpoint therapy. Science 348, 56–61 (2015)
Boussiotis, V. A. Molecular and biochemical aspects of the PD-1 checkpoint pathway. N. Engl. J. Med. 375, 1767–1778 (2016)
Green, M. R. et al. Integrative analysis reveals selective 9p24.1 amplification, increased PD-1 ligand expression, and further induction via JAK2 in nodular sclerosing Hodgkin lymphoma and primary mediastinal large B-cell lymphoma. Blood 116, 3268–3277 (2010)
Kataoka, K. et al. Aberrant PD-L1 expression through 3′-UTR disruption in multiple cancers. Nature 534, 402–406 (2016)
Morgens, D. W. et al. Genome-scale measurement of off-target activity using Cas9 toxicity in high-throughput screens. Nat. Commun. 8, 15178 (2017)
Han, W. et al. Identification of eight genes encoding chemokine-like factor superfamily members 1–8 (CKLFSF1–8) by in silico cloning and experimental validation. Genomics 81, 609–617 (2003)
Sánchez-Pulido, L., Martín-Belmonte, F., Valencia, A. & Alonso, M. A. MARVEL: a conserved domain involved in membrane apposition events. Trends Biochem. Sci. 27, 599–601 (2002)
Weekes, M. P. et al. Latency-associated degradation of the MRP1 drug transporter during latent human cytomegalovirus infection. Science 340, 199–202 (2013)
Matheson, N. J. et al. Cell surface proteomic map of HIV infection reveals antagonism of amino acid metabolism by Vpu and Nef. Cell Host Microbe 18, 409–423 (2015)
Grant, B. D. & Donaldson, J. G. Pathways and mechanisms of endocytic recycling. Nat. Rev. Mol. Cell Biol. 10, 597–608 (2009)
van Weert, A. W., Geuze, H. J., Groothuis, B. & Stoorvogel, W. Primaquine interferes with membrane recycling from endosomes to the plasma membrane through a direct interaction with endosomes which does not involve neutralisation of endosomal pH nor osmotic swelling of endosomes. Eur. J. Cell Biol. 79, 394–399 (2000)
Arjonen, A., Alanko, J., Veltel, S. & Ivaska, J. Distinct recycling of active and inactive β1 integrins. Traffic 13, 610–625 (2012)
Tumeh, P. C. et al. PD-1 blockade induces responses by inhibiting adaptive immune resistance. Nature 515, 568–571 (2014)
Homet Moreno, B., Parisi, G., Robert, L. & Ribas, A. Anti-PD-1 therapy in melanoma. Semin. Oncol. 42, 466–473 (2015)
Li, C. W. et al. Glycosylation and stabilization of programmed death ligand-1 suppresses T-cell activity. Nat. Commun. 7, 12632 (2016)
Behren, A. et al. The Ludwig institute for cancer research Melbourne melanoma cell line panel. Pigment Cell Melanoma Res. 26, 597–600 (2013)
Woods, K. & Cebon, J. Tumor-specific T-cell help is associated with improved survival in melanoma. Clin. Cancer Res. 19, 4021–4023 (2013)
Boutros, C. et al. Safety profiles of anti-CTLA-4 and anti-PD-1 antibodies alone and in combination. Nat. Rev. Clin. Oncol. 13, 473–486 (2016)
Mahoney, K. M., Rennert, P. D. & Freeman, G. J. Combination cancer immunotherapy and new immunomodulatory targets. Nat. Rev. Drug Discov. 14, 561–584 (2015)
Acknowledgements
M.L.B. is supported by a Cancer Research UK Fellowship, Addenbrooke’s Charitable Trust award and NIHR fellowship. M.A.D. is supported by a Senior Leukaemia Foundation Australia Fellowship and work in the Dawson laboratory is supported by the NHMRC (Grants 1085015, 1106444 and 1106447) Cancer Council Victoria and Leukaemia Foundation Australia. P.J.L. is supported by a Wellcome Trust PRF (101835/Z/13/Z) and work in the Lehner laboratory is supported by NHSBT, NIHR Cambridge BRC, a Wellcome Trust Strategic Award to CIMR, and the Addenbrooke’s Charitable Trust.
Author information
Authors and Affiliations
Contributions
M.L.B., P.J.L. and M.A.D. designed the research and interpreted data. M.A.D. and M.L.B. wrote the manuscript with assistance from P.J.L., Y-C.C. and E.Y.N.L. M.L.B., C.E.S., Y.-C.C., E.Y.N.L., C.C.B., S.S., and O.G. performed experiments and analysed data directly supervised by M.A.D. M.L.B. performed the CRISPR screen assisted by S.B. and J.C.W. performed the plasma membrane profiling supervised by P.J.L. K.W. and A.B. performed T cell assays supervised by J.C. P.A.B. and M.A.H. performed the mouse experiments. D.W.M. and M.C.B. designed and generated the CRISPR sgRNA library. P.J.N., P.K.D., S-J.D., I.V. and J.A.T. provided critical reagents and aided in manuscript preparation.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Additional information
Reviewer Information Nature thanks S. Ogawa, A. Ribas and the other anonymous reviewer(s) for their contribution to the peer review of this work.
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data figures and tables
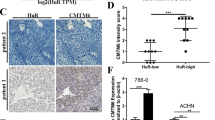
Extended Data Figure 1 A CRISPR–Cas9 screen in the pancreatic cancer cell line BxPC-3 identifies CMTM6 as a principal regulator of PD-L1 expression.
a, PD-L1 is expressed at the cell surface in BxPC-3 cells and upregulated following treatment with IFNγ. Cell surface PD-L1 was analysed by flow cytometry following incubation with or without IFNγ 500 IU ml−1 for 48 h. b, BxPC-3 cells stably expressing Cas9 were mutagenized by infection with a pooled lentiviral gRNA library and rare PD-L1low cells enriched by two successive rounds of FACS sorting for mCherry-positive (containing sgRNA vector) PD-L1low cells. FACS plots depict sorted and unsorted mutagenized populations stained for PD-L1 (top panel) and MHC class I control (bottom panel). c, Total cellular PD-L1 levels are markedly reduced following shRNA-mediated depletion of CMTM6 in both IFNγ-treated and non-IFNγ-treated cells. Immunoblot for PD-L1, CMTM6 and HSP60 control in MDA-MB-231 cells transduced with shRNAs targeting CMTM6 or control shRNA. d, Reduced cell surface PD-L1 following shRNA-mediated depletion of CMTM6 in BxPC-3 cells.
Extended Data Figure 2 Downregulation of cell surface PD-L1 following effective RNA interference (RNAi)-mediated depletion of CMTM6.
a, Efficiency of CMTM6 depletion was assessed by quantitative reverse-transcription PCR (qRT–PCR) in cells transduced with shRNAs targeting CMTM6 or a non-targeting control shRNA. The mean and s.e.m. of 3 technical replicates are shown. b, RNAi-mediated depletion of CMTM6 reduces cell surface PD-L1 expression both in the presence and absence of IFNγ stimulation. Cell surface PD-L1 was analysed by flow cytometry in the indicated cell lines transduced with lentiviral vectors encoding shRNAs targeting CMTM6 or control shRNA (left). The adjacent bar chart (right) shows fold change in cell surface PD-L1 fluorescence intensity following CMTM6 depletion (mean and s.e.m.). BxPC-3, HCC-827 and A375 cells were pre-treated with IFNγ 500 IU ml−1 for 48 h before analysis. Experiments were performed at least twice in each cell type.
Extended Data Figure 3 CRISPR–Cas9-mediated knockout of CMTM6 reduces cell surface PD-L1 expression in a broad range of cancer cells.
Flow cytometry analysis of cell surface PD-L1 in cells transduced with different sgRNAs targeting CMTM6 compared to parental Cas9-expressing cells. Cell lines depicted are melanoma (A375 and WM-852), triple-negative breast cancer (MDA-MB-231), non-small cell lung cancer (HCC-827) and pancreatic cancer (BxPC-3). All cells were pre-treated with IFNγ 500 IU ml−1 for 48 h before analysis. Selected representative histograms are presented in Fig. 1e.
Extended Data Figure 4 CMTM6 selectively regulates both constitutive and interferon-induced PD-L1 without compromising tumour cell MHC class I expression.
a, Cell surface MHC class I expression is unaffected by shRNA-mediated depletion of CMTM6. Flow cytometry analysis of surface MHC class I and PD-L1 in MDA-MB-231 and A375 cells transduced with shRNAs targeting CMTM6 or control shRNA. Cells were pre-treated with IFNγ 500 IU ml−1 for 48 h before analysis. b, CMTM6 knockout leads to loss of both constitutive and IFNγ-induced PD-L1 expression. Flow cytometry analysis of cell surface PD-L1 in Cas9-expressing MDA-MB-231 cells transduced with sgRNA targeting either PD-L1, JAK2 or CMTM6 (red) compared to parental Cas9-expressing cells (blue). PD-L1 expression is reduced in both the presence and absence of IFNγ stimulation following knockout of CMTM6. In contrast, knockout of the IFNγ pathway component JAK2 leads to selective loss of IFNγ induced upregulation of PD-L1 with no effect on constitutive PD-L1 expression.
Extended Data Figure 5 CMTM6 is not regulated by IFNγ and co-localizes with PD-L1 at the cell surface in both the presence and absence of IFNγ stimulation.
a, CMTM6 regulates cell surface and total PD-L1 levels in a dose-dependent manner. Single-cell clones isolated from WM-852 cells transduced with Cas9 and an sgRNA-targeting CMTM6 were analysed by flow cytometry for surface PD-L1 and immunoblot for total PD-L1 and CMTM6 following incubation with 500 IU ml–1 IFNγ for 48 h. b, qRT–PCR analysis of relative CMTM6 mRNA expression in the indicated cell lines incubated with or without IFNγ 500 IU ml−1 for 48 h before analysis. The data were obtained in control shRNA-expressing cells depicted in Extended Data Fig. 2a. Graphs show mean and s.e.m. of two biological replicates (MDA-MB-231 and HCC-827) or three technical replicates (BxPC-3). c, To confirm specific staining of endogenous CMTM6 by the anti-CMTM6 antibody, CMTM6-knockout MDA-MB-231 cells were labelled with CFSE before mixing with wild-type MDA-MB-231 cells, fixed and immunostained for CMTM6. Scale bar, 10 μm. d, MDA-MB-231 cells treated with IFNγ 500 IU ml−1 for 48 h were fixed, immunostained for CMTM6 and PD-L1 and analysed by confocal microscopy. Scale bar, 10 μm.
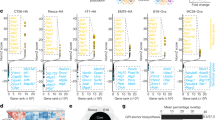
Extended Data Figure 6 CMTM6 shows functional specificity for PD-L1.
a, b, CMTM6 specifically regulates PD-L1, with no effect on cell surface PD-L2 levels in THP-1 cells. THP-1 cells expressing Cas9 and transduced with CMTM6 sgRNA were treated with IFNγ 500 IU ml−1 and TNFα 20 ng ml−1 for 24 h as indicated before staining of cell surface PD-L1 and PD-L2 and analysis by flow cytometry. c, Mass spectrometry analysis identifies PD-L1 as a principal interaction partner of CMTM6. CMTM6 was immunoprecipitated from digitonin lysates of IFNγ-treated MDA-MB-231 cells, and CMTM6-knockout cells as a control. Immunoprecipitates were analysed by mass spectrometry. Table represents all CMTM6 interaction partners identified by at least three unique peptides and absent from the control immunoprecipitation from CMTM6-knockout cells. d, Increased degradation of EndoH-resistant PD-L1 species in the absence of CMTM6. IFNγ-treated CMTM6-knockout or parental Cas9-expressing WM-852 cells were pulse-labelled with 35S-methionine/cysteine for 30 min before chase incubation at 37 °C. PD-L1 was immunoprecipitated from detergent lysates at the indicated times. e, f, IFNγ 500 IU ml−1 was added to CMTM6-knockout and parental Cas9-expressing WM-852 cells and samples taken at the indicated time-points for analysis by flow cytometry. A representative example of an experiment done in biological triplicate is shown. g, Lysates of CMTM6-knockout cells incubated with IFNγ for the indicated times were treated with or without EndoH before SDS–PAGE analysis and immunoblot to assess modification of N-linked glycans on PD-L1 as a marker of passage through the Golgi.
Extended Data Figure 7 Cellular localization of PD-L1.
a, Loss of CMTM6 leads to selective destabilization of PD-L1 with no effect on the stability of cell surface MHC class I. IFNγ-treated CMTM6-knockout and Cas9 control WM-852 cells were labelled as described in Fig. 3b with APC-conjugated antibodies specific for either PD-L1 or MHC class I on ice before incubation at 37 °C. Samples taken at the indicated time-points were analysed by flow cytometry. Experiment performed twice. b, MDA-MB-231 cells were fixed, immunostained for PD-L1 together with a marker of the ER (CANX), Golgi (GM130 and TGN46), early endosome (EEA1) or late endosome/lysosome (LAMP1) before analysis by confocal microscopy. Scale bar, 10 μm.
Extended Data Figure 8 PD-L1 endocytosis and recycling assays.
a, Internalization assay (relates to data presented in Fig. 3g). Cells were labelled with unconjugated PD-L1-specific antibodies at 4 °C. After washing off unbound antibody, cells were incubated at 37 °C to allow PD-L1 internalization. Remaining cell surface antibody-labelled PD-L1 was detected with an AF647-conjugated anti-mouse secondary antibody and analysed by flow cytometry. b, Recycling assay 1. Cell surface PD-L1 in IFNγ-treated CMTM6-knockout and Cas9 control WM-852 cells was labelled with an unconjugated PD-L1-specific antibody and allowed to internalize for 30 min at 37 °C as described in a. Remaining cell-surface bound antibody was stripped by washing in pH 2.5 buffer and cells were either kept on ice (post-strip baseline) or re-incubated at 37 °C for the indicated times. Recycled PD-L1 was detected with an AF647-conjugated anti-mouse secondary antibody. c, Recycling assay 2 (relates to data presented in Fig. 3h). Cells were labelled with an AF488-conjugated PD-L1-specific antibody, washed and incubated at 37 °C to allow endocytosis. Remaining cell surface AF488 was quenched by incubation with an AF488-specific antibody for 1 h on ice before reincubation at 37 °C to allow recycling of antibody-labelled PD-L1. Samples were split and incubated with or without an AF488-specific antibody for 1 h on ice to re-quench cell surface AF488. Recycled PD-L1 was detected by the reappearance of cell surface ‘quenchable’ AF488 signal. After normalization for incomplete quenching at baseline by subtracting the ‘quenchable’ AF488 fluorescence at time zero, the fluorescence intensity of recycled PD-L1 at each time-point was compared to that of the total internalised PD-L1 after the endocytosis step to calculate the proportion of PD-L1 recycled.
Extended Data Figure 9 PD-L1 is targeted for degradation in the lysosome following depletion of CMTM6.
a, b, PD-L1 is targeted for lysosome-dependent degradation in the absence of CMTM6. IFNγ-treated CMTM6-knockout and Cas9 control WM-852 cells were labelled with APC-conjugated PD-L1-specific antibody as in Fig. 3b. Cells were chased at 37 °C in the presence or absence of either 50 nM concanamycin-A, 50 μM chloroquine or 400 nM bafilomycin A1 (two experiments (mean, s.e.m.)). c, IFNγ-treated CMTM6-knockout and Cas9 control WM-852 cells were incubated with con-A, chloroquine or bafilomycin-A1 for 16 h before analysis by immunoblot. d, Following inhibition of lysosomal degradation PD-L1 remains sequestered intracellularly in the absence of CMTM6. MDA-MB-231 cells expressing shRNAs targeting CMTM6 or control shRNA were incubated with 50 nM concanamycin-A (conA) for 16 h before flow cytometry analysis for cell surface PD-L1. e, Jurkat cells co-cultured with a CMTM6-knockout tumour show enhanced Il-2 secretion. Jurkat cells were pre-activated overnight with PMA and PHA and co-cultured with PD-L1-knockout, CMTM6-knockout or control vector expressing WM-852 Cas9 cells pre-treated with 500 IU ml−1 IFNγ for 24 h to upregulate PD-L1 expression. IL-2 levels in the culture supernatant were measured by cytometric bead array after 48 h and 72 h co-culture of Jurkat cells and tumour. Graphs show percent change in Il-2 secretion compared to control cell co-culture (mean and s.e.m. of experimental duplicates). f–h, Reduction in cell surface PD-L1 following knockout or knockdown of CMTM6 in NY-ESO-1 expressing melanoma cell lines used in T cell co-culture assays. All cells were treated with IFNγ before flow cytometry analysis for cell surface PD-L1. f, A375 cells stably expressing Cas9 were transduced with two different sgRNA-targeting CMTM6 and CMTM6-knockout clones were isolated by dilution cloning. g, Patient-derived melanoma cell line LM-MEL-44 was transduced with CMTM6 targeting or control shRNA. h, Patient-derived melanoma cell line LM-MEL-53 was sequentially transduced with Cas9 and either one of two different sgRNAs targeting CMTM6, an sgRNA-targeting PD-L1 or a control vector.
Extended Data Figure 10 CMTM6 regulates tumour-specific T cell activity by regulating PD-L1 levels.
a, Schematic overview of T cell and tumour co-culture assays to evaluate PD-L1-dependent inhibition of T cell activity. b, Increased PD-1 expression on NY-ESO-192–100 HLA-CW3-restricted T lymphocytes following 24 h co-culture with LM-MEL-53 melanoma. Staining with APC-conjugated anti-PD-1 antibody is completely blocked following addition of anti-PD-1 antibody nivolumab (BMS) at a saturating concentration (10 μg ml−1). c–g, CMTM6 regulates the anti-tumour activity of NY-ESO-1 antigen-specific T lymphocytes. c–e, NY-ESO-192–100 HLA-CW3-restricted or NY-ESO-1157–165 HLA-A2-restricted CTLs were incubated with the indicated melanoma cells at an effector:target ratio of 1:1 (c, e) or 1:2 (d) for 24–48 h at 37 °C, then washed off. CTL-mediated tumour lysis was determined by MTS assay and normalized to control wells with no CTLs. f, g, Enhanced T cell activation following co-culture with a CMTM6-depleted cancer cells. f, NY-ESO-192-100 HLA-CW3-restricted T lymphocytes were cultured with CMTM6 sgRNA, PD-L1 sgRNA or control vector transduced LM-MEL-53 melanoma cells stably expressing Cas9 for 24 h before incubation with brefeldin A for 6 h and intracellular staining for TNFα. Where indicated, 10 μg ml–1 nivolumab (anti-PD-1 antibody) was added to the co-cultures. Graphs show triplicates (mean + s.e.m.). *P < 0.05, unpaired two-tailed t-test (c–f). g, Supernatants from 3 day co-cultures of NY-ESO-192–100 CTLs and control vector or CMTM6 sgRNA transduced LM-MEL-53 cells were analysed by multiplex bead immunoassay (Luminex). Chemokines detected at increased levels following inclusion of 10 μg ml−1 nivolumab (anti-PD-1 antibody) in the co-cultures are shown. Graphs show triplicates (mean + s.e.m.). *P < 0.05, unpaired two-tailed t-test with Holm–Sidak correction for multiple testing. h, Efficiency of CMTM6 depletion was assessed by qRT–PCR in B16-OVA cells transduced with shRNA targeting CMTM6 or a non-targeting control shRNA. i, j, Growth of CMTM6-deficient and control shRNA expressing B16-OVA tumours injected subcutaneously in C57BL/6 mice. Data are from two independent experiments. Where indicated, mice were treated with anti-CTLA-4 or isotype control antibody from day 4 after tumour cell injection.
Supplementary information
Supplementary Information
This file contains the uncropped gels and a representative example of FACs gating strategy. (PDF 372 kb)
Supplementary Data
This file contains Supplementary Table 1. (XLSX 125 kb)
Supplementary Data
This file contains Supplementary Table 2. (XLSX 1975 kb)
Rights and permissions
About this article
Cite this article
Burr, M., Sparbier, C., Chan, YC. et al. CMTM6 maintains the expression of PD-L1 and regulates anti-tumour immunity. Nature 549, 101–105 (2017). https://doi.org/10.1038/nature23643
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nature23643
This article is cited by
-
TMEM160 promotes tumor immune evasion and radiotherapy resistance via PD-L1 binding in colorectal cancer
Cell Communication and Signaling (2024)
-
Mutual regulation of PD-L1 immunosuppression between tumor-associated macrophages and tumor cells: a critical role for exosomes
Cell Communication and Signaling (2024)
-
Exercise accelerates recruitment of CD8+ T cell to promotes anti-tumor immunity in lung cancer via epinephrine
BMC Cancer (2024)
-
Emerging therapeutic frontiers in cancer: insights into posttranslational modifications of PD-1/PD-L1 and regulatory pathways
Experimental Hematology & Oncology (2024)
-
Carnosine regulation of intracellular pH homeostasis promotes lysosome-dependent tumor immunoevasion
Nature Immunology (2024)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.