Abstract
The 2013–2016 West African epidemic caused by the Ebola virus was of unprecedented magnitude, duration and impact. Here we reconstruct the dispersal, proliferation and decline of Ebola virus throughout the region by analysing 1,610 Ebola virus genomes, which represent over 5% of the known cases. We test the association of geography, climate and demography with viral movement among administrative regions, inferring a classic ‘gravity’ model, with intense dispersal between larger and closer populations. Despite attenuation of international dispersal after border closures, cross-border transmission had already sown the seeds for an international epidemic, rendering these measures ineffective at curbing the epidemic. We address why the epidemic did not spread into neighbouring countries, showing that these countries were susceptible to substantial outbreaks but at lower risk of introductions. Finally, we reveal that this large epidemic was a heterogeneous and spatially dissociated collection of transmission clusters of varying size, duration and connectivity. These insights will help to inform interventions in future epidemics.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
World Health Organization. Ebola Situation Report—10 June 2016http://apps.who.int/iris/bitstream/10665/208883/1/ebolasitrep_10Jun2016_eng.pdf (2016)
Kuhn, J. H. et al. Nomenclature- and database-compatible names for the two Ebola virus variants that emerged in Guinea and the Democratic Republic of the Congo in 2014. Viruses 6, 4760–4799 (2014)
Baize, S. et al. Emergence of Zaire Ebola virus disease in Guinea. N. Engl. J. Med. 371, 1418–1425 (2014)
World Health Organization Regional Office for Africa. Ebola Virus Disease, West Africa (situation as of 25 April 2014)http://www.afro.who.int/en/clusters-a-programmes/dpc/epidemic-a-pandemic-alert-and-response/4121-ebola-virus-disease-west-africa-25-april-2014.html (2014)
Goba, A. et al. An outbreak of Ebola virus disease in the Lassa fever zone. J. Infect. Dis. 214, S110–S121 (2016)
Sack, K., Fink, S., Belluck, P., Nossiter, A. & Berehulak, D. How Ebola roared backhttp://nyti.ms/1wwG5VX (2014)
Gire, S. K. et al. Genomic surveillance elucidates Ebola virus origin and transmission during the 2014 outbreak. Science 345, 1369–1372 (2014)
Dudas, G. & Rambaut, A. Phylogenetic analysis of Guinea 2014 EBOV Ebolavirus outbreak. PLoS Curr. 6, http://dx.doi.org/10.1371/currents.outbreaks.84eefe5ce43ec9dc0bf0670f7b8b417d (2014)
Carroll, M. W. et al. Temporal and spatial analysis of the 2014–2015 Ebola virus outbreak in West Africa. Nature 524, 97–101 (2015)
Quick, J. et al. Real-time, portable genome sequencing for Ebola surveillance. Nature 530, 228–232 (2016)
Blackley, D. J. et al. Reduced evolutionary rate in reemerged Ebola virus transmission chains. Sci. Adv. 2, e1600378 (2016)
Mate, S. E. et al. Molecular evidence of sexual transmission of Ebola virus. N. Engl. J. Med. 373, 2448–2454 (2015)
Simon-Loriere, E. et al. Distinct lineages of Ebola virus in Guinea during the 2014 West African epidemic. Nature 524, 102–104 (2015)
Arias, A . et al. Rapid outbreak sequencing of Ebola virus in Sierra Leone identifies transmission chains linked to sporadic cases. Virus Evol. 2, vew016 (2016)
Park, D. J. et al. Ebola virus epidemiology, transmission, and evolution during seven months in Sierra Leone. Cell 161, 1516–1526 (2015)
Kugelman, J. R. et al. Monitoring of Ebola virus Makona evolution through establishment of advanced genomic capability in Liberia. Emerg. Infect. Dis. 21, 1135–1143 (2015)
Ladner, J. T. et al. Evolution and spread of Ebola virus in Liberia, 2014–2015. Cell Host Microbe 18, 659–669 (2015)
Lemey, P. et al. Unifying viral genetics and human transportation data to predict the global transmission dynamics of human influenza H3N2. PLoS Pathog. 10, e1003932 (2014)
Viboud, C. et al. Synchrony, waves, and spatial hierarchies in the spread of influenza. Science 312, 447–451 (2006)
Truscott, J. & Ferguson, N. M. Evaluating the adequacy of gravity models as a description of human mobility for epidemic modelling. PLOS Comput. Biol. 8, e1002699 (2012)
Yang, W. et al. Transmission network of the 2014–2015 Ebola epidemic in Sierra Leone. J. R. Soc. Interface 12, 20150536 (2015)
Fischer, R. et al. Ebola virus stability on surfaces and in fluids in simulated outbreak environments. Emerg. Infect. Dis. 21, 1243–1246 (2015)
Bausch, D. G. & Schwarz, L. Outbreak of Ebola virus disease in Guinea: where ecology meets economy. PLoS Negl. Trop. Dis. 8, e3056 (2014)
Chan, M. Ebola virus disease in West Africa—no early end to the outbreak. N. Engl. J. Med. 371, 1183–1185 (2014)
Wesolowski, A. et al. Commentary: containing the Ebola outbreak—the potential and challenge of mobile network data. PLoS Curr. 6, http://dx.doi.org/10.1371/currents.outbreaks.0177e7fcf52217b8b634376e2f3efc5e (2014)
Goodfellow, I., Reusken, C. & Koopmans, M. Laboratory support during and after the Ebola virus endgame: towards a sustained laboratory infrastructure. Euro Surveill. 20, 21074 (2015)
World Health Organization. Ebola Response Roadmap Situation Report Update—12 November 2014http://apps.who.int/iris/bitstream/10665/141468/1/roadmapsitrep_12Nov2014_eng.pdf (2014)
Folarin, O. A. et al. Ebola virus epidemiology and evolution in Nigeria. J. Infect. Dis. 214, S102–S109 (2016)
Abdoulaye, B. et al. Experience on the management of the first imported Ebola virus disease case in Senegal. Pan Afr. Med. J. 22, 6 (2015)
Whitmer, S. L. M. et al. Preliminary evaluation of the effect of investigational Ebola virus disease treatments on viral genome sequences. J. Infect. Dis. 214, S333–S341 (2016)
Xia, Y., Bjørnstad, O. N. & Grenfell, B. T. Measles metapopulation dynamics: a gravity model for epidemiological coupling and dynamics. Am. Nat. 164, 267–281 (2004)
Ferrari, M. J. et al. The dynamics of measles in sub-Saharan Africa. Nature 451, 679–684 (2008)
WHO Ebola Response Team. Ebola virus disease in West Africa — the first 9 months of the epidemic and forward projections. N. Engl. J. Med. 371, 1481–1495 (2014)
Gardy, J., Loman, N. J. & Rambaut, A. Real-time digital pathogen surveillance — the time is now. Genome Biol. 16, 155 (2015)
Yozwiak, N. L., Schaffner, S. F. & Sabeti, P. C. Data sharing: make outbreak research open access. Nature 518, 477–479 (2015)
Woolhouse, M. E. J., Rambaut, A. & Kellam, P. Lessons from Ebola: improving infectious disease surveillance to inform outbreak management. Sci. Transl. Med. 7, 307rv5 (2015)
Stadler, T., Kühnert, D., Rasmussen, D. A. & du Plessis, L. Insights into the early epidemic spread of Ebola in Sierra Leone provided by viral sequence data. PLoS Curr. 6, http://dx.doi.org/10.1371/currents.outbreaks.02bc6d927ecee7bbd33532ec8ba6a25f (2014)
Tong, Y.-G. et al. Genetic diversity and evolutionary dynamics of Ebola virus in Sierra Leone. Nature 524, 93–96 (2015)
Diallo, B. et al. Resurgence of Ebola virus disease in Guinea linked to a survivor with virus persistence in seminal fluid for more than 500 days. Clin. Infect. Dis. 63, 1353–1356 (2016)
Rowe, A. K. et al. Clinical, virologic, and immunologic follow-up of convalescent Ebola hemorrhagic fever patients and their household contacts, Kikwit, Democratic Republic of the Congo. J. Infect. Dis. 179, S28–S35 (1999)
Katoh, K., Misawa, K., Kuma, K. & Miyata, T. MAFFT: a novel method for rapid multiple sequence alignment based on fast Fourier transform. Nucleic Acids Res. 30, 3059–3066 (2002)
Gélinas, J.-F., Clerzius, G., Shaw, E. & Gatignol, A. Enhancement of replication of RNA viruses by ADAR1 via RNA editing and inhibition of RNA-activated protein kinase. J. Virol. 85, 8460–8466 (2011)
Bass, B. L. & Weintraub, H. An unwinding activity that covalently modifies its double-stranded RNA substrate. Cell 55, 1089–1098 (1988)
Cattaneo, R. et al. Biased hypermutation and other genetic changes in defective measles viruses in human brain infections. Cell 55, 255–265 (1988)
Rueda, P., García-Barreno, B. & Melero, J. A. Loss of conserved cysteine residues in the attachment (G) glycoprotein of two human respiratory syncytial virus escape mutants that contain multiple A–G substitutions (hypermutations). Virology 198, 653–662 (1994)
Carpenter, J. A., Keegan, L. P., Wilfert, L., O’Connell, M. A. & Jiggins, F. M. Evidence for ADAR-induced hypermutation of the Drosophila sigma virus (Rhabdoviridae). BMC Genet. 10, 75 (2009)
Smits, S. L. et al. Genotypic anomaly in Ebola virus strains circulating in Magazine Wharf area, Freetown, Sierra Leone, 2015. Euro Surveill. 20, 30035 (2015)
Hasegawa, M., Kishino, H. & Yano, T. Dating of the human–ape splitting by a molecular clock of mitochondrial DNA. J. Mol. Evol. 22, 160–174 (1985)
Yang, Z. Maximum likelihood phylogenetic estimation from DNA sequences with variable rates over sites: approximate methods. J. Mol. Evol. 39, 306–314 (1994)
Drummond, A. J., Ho, S. Y. W., Phillips, M. J. & Rambaut, A. Relaxed phylogenetics and dating with confidence. PLoS Biol. 4, e88 (2006)
Gill, M. S. et al. Improving Bayesian population dynamics inference: a coalescent-based model for multiple loci. Mol. Biol. Evol. 30, 713–724 (2013)
Ferreira, M. A. R. & Suchard, M. A. Bayesian analysis of elapsed times in continuous-time Markov chains. Can. J. Stat. 36, 355–368 (2008)
Lemey, P ., Suchard, M. & Rambaut, A. Reconstructing the initial global spread of a human influenza pandemic: a Bayesian spatial-temporal model for the global spread of H1N1pdm. PLoS Curr. 1, RRN1031 (2009)
Drummond, A. J., Suchard, M. A., Xie, D. & Rambaut, A. Bayesian phylogenetics with BEAUti and the BEAST 1.7. Mol. Biol. Evol. 29, 1969–1973 (2012)
Edwards, C. J. et al. Ancient hybridization and an Irish origin for the modern polar bear matriline. Curr. Biol. 21, 1251–1258 (2011)
Minin, V. N. & Suchard, M. A. Fast, accurate and simulation-free stochastic mapping. Phil. Trans. R. Soc. B 363, 3985–3995 (2008)
Bielejec, F., Lemey, P., Baele, G., Rambaut, A. & Suchard, M. A. Inferring heterogeneous evolutionary processes through time: from sequence substitution to phylogeography. Syst. Biol. 63, 493–504 (2014)
Acknowledgements
The authors acknowledge support from: European Union Seventh Framework 278433-PREDEMICS (P.L., A.R.) and ERC 260864 (P.L., A.R., M.A.S.) European Union Horizon 2020 643476-COMPARE (M.P.G.K., A.R.), 634650-VIROGENESIS (P.L., M.P.G.K.), 666100-EVIDENT and European Commission IFS/2011/272-372, EMLab (S.G.), National Institutes of Health R01 AI107034, R01 AI117011 and R01 HG006139 and National Science Foundation IIS 1251151 and DMS 1264153 (M.A.S.), NIH AI081982, AI082119, AI082805 AI088843, AI104216, AI104621, AI115754, HSN272200900049C, HHSN272201400048C (R.F.G.), NIH R35 GM119774-01 (T.B.) National Health & Medical Research Council (Australia) (E.C.H.). The Research Foundation - Flanders G0D5117N (G.B., P.L.), Work in Liberia was funded by the Defense Threat Reduction Agency, the Global Emerging Infections System and the Targeted Acquisition of Reference Materials Augmenting Capabilities (TARMAC) Initiative agencies from the US Department of Defense (G.Pa.), Bill and Melinda Gates Foundation OPP1106427, 1032350, OPP1134076, Wellcome Trust 106866/Z/15/Z, Clinton Health Access Initiative (A.J.T.), National Institute for Health Research Health Protection Research Unit in Emerging and Zoonotic Infections (J.A.H.), Key Research and Development Program from the Ministry of Science and Technology of China 2016YFC1200800 (D.L.), National Natural Science Foundation of China 81590760 and 81321063 (G.F.G.), Mahan Post-doctoral fellowship Fred Hutchinson Cancer Research Center (G.D.), National Institute of Allergy and Infectious Disease U19AI110818, 5R01AI114855-03, United States Agency for International Development OAA-G-15-00001 and the Bill and Melinda Gates Foundation OPP1123407 (P.C.S.), NIH 1U01HG007480-01 and the World Bank ACE019 (C.T.H.), PEW Biomedical Scholarship, NIH UL1TR001114, and NIAID contract HHSN272201400048C (K.G.A.). J.H.K., an employee of Tunnell Government Services, Inc., is a subcontractor under Battelle Memorial Institute’s prime contract with the NIAID (contract HHSN272200700016I). Colour-blind-friendly colour palettes were designed by C. Brewer, Pennsylvania State University (http://colorbrewer2.org). Matplotlib (http://matplotlib.org) was used extensively throughout this article for data visualisation. We acknowledge support from NVIDIA Corporation with the donation of parallel computing resources used for this research. Finally, we recognize the contributions made by our colleagues who died from Ebola virus disease whilst fighting the epidemic.
Author information
Authors and Affiliations
Contributions
G.D., L.M.C., T.B., C.F., M.A.S., P.L. and A.R. designed the study. G.D., L.M.C., T.B., A.J.T., G.B., P.L. and A.R. performed the analysis. G.D., T.B., M.A.S, P.L. and A.R. wrote the manuscript. L.M.C., A.J.T., G.B., N.R.F., J.T.L., M.C., S.F.S., K.G.A., M.W.C., R.F.G., I.G., E.C.H., P.K., M.P.G.K., J.H.K., S.T.N., G.Pa., O.G.P., P.C.S. and U.S. edited the manuscript. The other authors were critical for the coordination, collection, processing of virus samples or the sequencing and bioinformatics of virus genomes. All authors read and approved the contents of the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Additional information
Reviewer Information Nature thanks R. Biek, C. Viboud, M. Worobey and the other anonymous reviewer(s) for their contribution to the peer review of this work.
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data figures and tables
Extended Data Figure 1 Distribution and correlation of EVD cases and EBOV sequences.
a, Administrative regions within Guinea (green), Sierra Leone (blue) and Liberia (red); shading is proportional to the cumulative number of known and suspected EVD cases in each region. Darkest shades represent 784 cases for Guinea (Macenta prefecture); 3,219 cases for Sierra Leone (Western Area urban district); and 2,925 cases for Liberia (Montserrado county); hatching indicate regions without reported EVD cases. Circle diameters are proportional to the number of EBOV genomes available from that region over the entire EVD epidemic with the largest circle representing 152 sequences. Crosses mark regions for which no sequences are available. Circles and crosses are positioned at population centroids within each region. b, A plot of number of EBOV genomes sampled against the known and suspected cumulative EVD case numbers. Regions in Guinea are denoted in green, Sierra Leone in blue and Liberia in red. Spearman correlation coefficient: 0.93.
Extended Data Figure 2 Dispersal of virus lineages over time.
Virus dispersal between administrative regions estimated using the GLM phylogeography model (see Methods). The arcs are between population centroids of each region, show directionality from the thin end to the thick end and are coloured in a scale denoting time from December 2013 in blue to October 2015 in yellow. Countries are coloured with Liberia in red, Guinea in green and Sierra Leone in blue.
Extended Data Figure 3 Inference of GLM predictors in a ‘real-time’ context.
For the dataset constructed from EBOV genome sequences derived from samples taken up until October 2014 (blue), the same 5 spatial EBOV movement predictors were given categorical support (inclusion probabilities = 1.0) as for the full dataset (red). Likewise, the coefficients for these predictors are consistent in their sign and magnitude.
Extended Data Figure 4 The effect of borders on EBOV migration rates between regions.
Posterior densities for the migration rates between locations that share a geographical border and those that do not share borders for international migrations and national migrations. Where two regions share a border (right y axis), national migrations are only marginally more frequent than international migrations showing that both types of borders are porous to short local movement. Where the two regions are not adjacent (left y axis), international migrations are much rarer than national migrations.
Extended Data Figure 5 Summarized international migration history of the epidemic.
a, b, All viral movement events between countries (Guinea, green; Sierra Leone, blue; Liberia, red) are shown split by whether they are between regions that are geographically distant (a) or regions that share the international border (b). Curved lines indicate median (intermediate colour intensity), and 95% highest posterior density intervals (lightest and darkest colour intensities) for the number of migrations that are inferred to have taken place between countries.
Extended Data Figure 6 Comparison of predicted and observed numbers of introductions and case numbers.
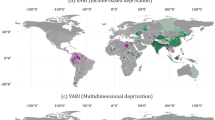
a, b, Left, scatter plots show inferred introduction numbers (a) or observed case numbers (b), coloured by region as in Extended Data Fig. 1. Administrative regions that did not report any cases are indicated with empty circles on the scatter plot. Right, administrative regions on the map are coloured by the residuals (as observed/predicted) of the scatter plot. Regions are coloured grey where 0.5 < observed/predicted < 2.0 and transition into red or blue colours for overestimation or underestimation, respectively.
Extended Data Figure 7 Region-specific introductions, cluster sizes and persistence.
Each row summarizes independent introductions and the sizes (as numbers of sequences) of resulting outbreak clusters. Clusters are coloured by their inferred region of origin (colours are the same as in Extended Data Fig. 1). The horizontal lines represent the persistence of each cluster from the time of introduction to the last sampled case (individual tips have persistence 0). The areas of the circles in the middle of the lines are proportional to the number of sequenced cases in the cluster. The areas of the circles next to the labels on the left represent the population sizes of each administrative region. Vertical lines within each cell indicate the dates of declared border closures by each of the three countries: 11 June 2014 in Sierra Leone (blue), 27 July 2014 in Liberia (red) and 09 August 2014 in Guinea (green).
Extended Data Figure 8 Kernel density estimates for inferred epidemiological statistics.
From top to bottom, distance travelled (distance between population centroids, in kilometres); number of introductions that each location experienced; cluster size (number of sequences collected in a location as a result of a single introduction); cluster persistence (days from the common ancestor of a cluster to its last descendent, single tips have persistence of 0. Left, analysis for Sierra Leone (blue), Liberia (red) and Guinea (green). Right, analysis for before October 2014 (grey) and after October 2014 (orange). Points with vertical lines connected to the x axis indicate the 50% and 95% quantiles of the parameter density estimates. Within Sierra Leone, Liberia and Guinea, 50% of all migrations occurred over distances of around 100 km and persisted for around 25 days. Exceptions were for Sierra Leone, which experienced more introductions per location (around 12) than Guinea and Liberia (around 4); and Guinea, where migrations tended to occur over larger distances owing to the size of the country and whose cluster sizes following introductions tended to be lower (3 sequences versus Liberia and Sierra Leone, which had 5 sequences each). Between the first (grey) and second (orange) years of the epidemic there were considerable reductions in cluster persistence, cluster sizes and distances travelled by viruses, whereas dispersal intensity remained largely the same.
Extended Data Figure 9 Relationship between cluster size, introductions or persistence and population size.
a, The mean number of introductions into each location against (log) population sizes. The Western Area (in Sierra Leone) received the most introductions, whereas Conakry and Montserrado were closer to the average. The association between population size and the number of introductions was not very strong (R2 = 0.28, Pearson correlation = 0.54, Spearman correlation = 0.57). b, The mean cluster size for each location plotted against (log) population sizes. The association is weaker than for a (R2 = 0.11, Pearson correlation = 0.35, Spearman correlation = 0.57). c, The mean persistence times (per cluster, in days) against population sizes. A similarly weak association is observed as in b (R2 = 0.12, Pearson correlation = 0.37, Spearman correlation = 0.36). All computations were based on a sample of 10,000 trees from the posterior distribution.
Supplementary information
Supplementary Table
This file contains Supplementary Table 1. (PDF 40 kb)
Video 1: Reconstructed history of the West African Ebola virus epidemic
Map of the three most affected countries - Guinea, Liberia and Sierra Leone - is shown on the left. Colours indicate country - Guinea is green, Liberia is red and Sierra Leone is blue. Weekly incidence of EVD cases is indicated by shading of administrative divisions (darker shades correspond to more cases, on a logarithmic scale) within each country. Cases are linearly interpolated between successive reporting weeks. Inferred movements of Ebola virus are indicated with tapered projectiles, coloured by its origin country (Guinea in green, Sierra Leone in blue, Liberia in red) if lineage is crossing an international border and black otherwise. Red circles at population centroids of each administrative division indicate the number of lineages estimated to be present within the location. Phylogenetic tree in the upper right shows the relationships between sampled Ebola lineages, with branches coloured by location (lighter shades indicate locations further west within each country). Migrations inferred between any two locations in the tree are animated on the map on the left. Plot on the lower right shows the sum of weekly cases reported for each administrative division, for each individual country (Guinea in green, Sierra Leone in blue, Liberia in red). Weekly cases for individual administrative divisions are animated as changes in administrative division's colour on the map on the left. (MP4 11204 kb)
Rights and permissions
About this article
Cite this article
Dudas, G., Carvalho, L., Bedford, T. et al. Virus genomes reveal factors that spread and sustained the Ebola epidemic. Nature 544, 309–315 (2017). https://doi.org/10.1038/nature22040
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nature22040
This article is cited by
-
Evaluating the performance of Plasmodium falciparum genetic metrics for inferring National Malaria Control Programme reported incidence in Senegal
Malaria Journal (2024)
-
A topology-marginal composite likelihood via a generalized phylogenetic pruning algorithm
Algorithms for Molecular Biology (2023)
-
Genomic epidemiology offers high resolution estimates of serial intervals for COVID-19
Nature Communications (2023)
-
The episodic resurgence of highly pathogenic avian influenza H5 virus
Nature (2023)
-
Outbreak.info genomic reports: scalable and dynamic surveillance of SARS-CoV-2 variants and mutations
Nature Methods (2023)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.