Abstract
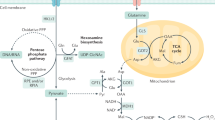
Pancreatic ductal adenocarcinoma (PDAC) is an aggressive disease characterized by an intense fibrotic stromal response and deregulated metabolism1,2,3,4. The role of the stroma in PDAC biology is complex and it has been shown to play critical roles that differ depending on the biological context5,6,7,8,9,10. The stromal reaction also impairs the vasculature, leading to a highly hypoxic, nutrient-poor environment4,11,12. As such, these tumours must alter how they capture and use nutrients to support their metabolic needs11,13. Here we show that stroma-associated pancreatic stellate cells (PSCs) are critical for PDAC metabolism through the secretion of non-essential amino acids (NEAA). Specifically, we uncover a previously undescribed role for alanine, which outcompetes glucose and glutamine-derived carbon in PDAC to fuel the tricarboxylic acid (TCA) cycle, and thus NEAA and lipid biosynthesis. This shift in fuel source decreases the tumour’s dependence on glucose and serum-derived nutrients, which are limited in the pancreatic tumour microenvironment4,11. Moreover, we demonstrate that alanine secretion by PSCs is dependent on PSC autophagy, a process that is stimulated by cancer cells. Thus, our results demonstrate a novel metabolic interaction between PSCs and cancer cells, in which PSC-derived alanine acts as an alternative carbon source. This finding highlights a previously unappreciated metabolic network within pancreatic tumours in which diverse fuel sources are used to promote growth in an austere tumour microenvironment.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
Change history
05 October 2016
An Erratum to this paper has been published: https://doi.org/10.1038/nature19851
References
Hidalgo, M. Pancreatic cancer. N. Engl. J. Med. 362, 1605–1617 (2010)
Sousa, C. M. & Kimmelman, A. C. The complex landscape of pancreatic cancer metabolism. Carcinogenesis 35, 1441–1450 (2014)
Whatcott, C. J. et al. Desmoplasia in primary tumors and metastatic lesions of pancreatic cancer. Clin. Cancer Res. 21, 3561–3568 (2015)
Feig, C. et al. The pancreas cancer microenvironment. Clin. Cancer Res. 18, 4266–4276 (2012)
Erkan, M. et al. StellaTUM: current consensus and discussion on pancreatic stellate cell research. Gut 61, 172–178 (2012)
Gore, J. & Korc, M. Pancreatic cancer stroma: friend or foe? Cancer Cell 25, 711–712 (2014)
Apte, M. V & Wilson, J. S. Dangerous liaisons: pancreatic stellate cells and pancreatic cancer cells. J. Gastroenterol. Hepatol. 27 (Suppl 2), 69–74 (2012)
Özdemir, B. C. et al. Depletion of carcinoma-associated fibroblasts and fibrosis induces immunosuppression and accelerates pancreas cancer with reduced survival. Cancer Cell 25, 719–734 (2014)
Rhim, A. D. et al. Stromal elements act to restrain, rather than support, pancreatic ductal adenocarcinoma. Cancer Cell 25, 735–747 (2014)
Feig, C. et al. Targeting CXCL12 from FAP-expressing carcinoma-associated fibroblasts synergizes with anti-PD-L1 immunotherapy in pancreatic cancer. Proc. Natl Acad. Sci. USA 110, 20212–20217 (2013)
Kamphorst, J. J. et al. Human pancreatic cancer tumors are nutrient poor and tumor cells actively scavenge extracellular protein. Cancer Res. 75, 544–553 (2015)
Olive, K. P. et al. Inhibition of Hedgehog signaling enhances delivery of chemotherapy in a mouse model of pancreatic cancer. Science 324, 1457–1461 (2009)
Commisso, C. et al. Macropinocytosis of protein is an amino acid supply route in Ras-transformed cells. Nature 497, 633–637 (2013)
Son, J. et al. Glutamine supports pancreatic cancer growth through a KRAS-regulated metabolic pathway. Nature 496, 101–105 (2013)
Ying, H. et al. Oncogenic Kras maintains pancreatic tumors through regulation of anabolic glucose metabolism. Cell 149, 656–670 (2012)
Hwang, R. F. et al. Cancer-associated stromal fibroblasts promote pancreatic tumor progression. Cancer Res. 68, 918–926 (2008)
Yuan, M., Breitkopf, S. B., Yang, X. & Asara, J. M. A positive/negative ion–switching, targeted mass spectrometry–based metabolomics platform for bodily fluids, cells, and fresh and fixed tissue. Nat. Protocols 7, 872–881 (2012)
Yang, A. et al. Autophagy is critical for pancreatic tumor growth and progression in tumors with p53 alterations. Cancer Discov. 4, 905–913 (2014)
Yang, S. et al. Pancreatic cancers require autophagy for tumor growth. Genes Dev. 25, 717–729 (2011)
Zhao, H. et al. Tumor microenvironment derived exosomes pleiotropically modulate cancer cell metabolism. eLife 5, e10250 (2016)
Sonveaux, P. et al. Targeting lactate-fueled respiration selectively kills hypoxic tumor cells in mice. J. Clin. Invest. 118, 3930–3942 (2008)
Tape, C. J. et al. Oncogenic KRAS regulates tumor cell signaling via stromal reciprocation. Cell 165, 910–920 (2016)
Serrao, E. M. et al. MRI with hyperpolarised [1-13C] pyruvate detects advanced pancreatic preneoplasia prior to invasive disease in a mouse model. Gut http://dx.doi.org/10.1136/gutjnl-2015-310114 (2015)
Trinquier, G. & Sanejouand, Y. H. Which effective property of amino acids is best preserved by the genetic code? Protein Eng. 11, 153–169 (1998)
Sherman, M. H. et al. Vitamin D receptor-mediated stromal reprogramming suppresses pancreatitis and enhances pancreatic cancer therapy. Cell 159, 80–93 (2014)
Ouyang, H. et al. Immortal human pancreatic duct epithelial cell lines with near normal genotype and phenotype. Am. J. Pathol. 157, 1623–1631 (2000)
Metallo, C. M. et al. Reductive glutamine metabolism by IDH1 mediates lipogenesis under hypoxia. Nature 481, 380–384 (2012)
Fernandez, C. A., Des Rosiers, C., Previs, S. F., David, F. & Brunengraber, H. Correction of 13C mass isotopomer distributions for natural stable isotope abundance. J. Mass Spectrom. 31, 255–262 (1996)
Sastra, S. A. & Olive, K. P. Quantification of murine pancreatic tumors by high-resolution ultrasound. Methods Mol. Biol. 980, 249–266 (2013)
Acknowledgements
We thank Kimmelman laboratory members for reading the manuscript, A. Yang for help with orthotopic injections, M. Yuan and S. Breitkopf for technical support with mass spectrometry, E. Sicinska for resected PDAC specimens, and the Dana-Farber/Harvard Cancer Center Rodent Histopathology Core for assistance with tissue processing. DFHCC is supported in part by NIH 5P30CA06516. A.C.K. is supported by NIH grant GM095567, NCI grants R01CA157490, R01CA188048, ACS Research Scholar Grant (RSG-13-298-01-TBG), and the Lustgarten Foundation. C.A.L. is supported by a PanCAN-AACR Pathway to Leadership award and a Dale F. Frey award from the Damon Runyon Cancer Research Foundation (DFS-09-14). Metabolomics studies performed at the University of Michigan were supported by NIH grant DK097153. L.C.C. was supported by P01CA117969, PanCAN-AACR and the Lustgarten Foundation. J.M.A. was supported by P30CA006516 and P01CA120964. R.M.E. is an investigator of the Howard Hughes Medical Institute and March of Dimes Chair in Molecular and Developmental Biology at the Salk Institute, and is supported in part by grants from The Lustgarten Foundation and a Stand Up to Cancer Dream Team Translational Cancer Research Grant, a Program of the Entertainment Industry Foundation (SU2C-AACR-DT0509).
Author information
Authors and Affiliations
Contributions
C.M.S. performed or participated in the conception and performance of all experiments. D.E.B. and X.W. participated in tissue culture imaging and animal studies. C.J.H. conducted kinetic metabolite release, capture and quantification metabolomics studies with support from D.K. L.Z. performed the associated metabolomics and fatty acid analyses. J.M.A. supervised the metabolite tracing metabolomics experiments as a core service. M.H.S., D.K., R.F.H, A.K.W. and H.Y. provided essential reagents. R.M.E. and L.C.C. provided intellectual feedback and support. C.M.S., C.A.L. and A.C.K. conceived the project, planned and guided the research, and wrote the paper.
Corresponding authors
Ethics declarations
Competing interests
L.C.C. owns equity in, receives compensation from, and serves on the Board of Directors and Scientific Advisory Board of Agios Pharmaceuticals. Agios Pharmaceuticals is identifying metabolic pathways of cancer cells and developing drugs to inhibit such enzymes to disrupt tumour cell growth and survival. The remaining authors have no competing financial interests to declare.
Additional information
Reviewer Information
Nature thanks J. Debnath and the other anonymous reviewer(s) for their contribution to the peer review of this work.
Extended data figures and tables
Extended Data Figure 1 Pancreatic stellate cells secrete metabolites that PDAC utilize to fuel their metabolism.
a–c, Conditioned medium (CM) from human pancreatic stellate cell (PSC) lines (hPSC#1 and hPSC#2) increases oxygen consumption (OCR) in multiple PDAC cell lines: a, Tu8902, b, MiaPaCa2 and c, Panc-1. Data are represented as per cent increase in OCR in cells treated with conditioned medium versus cells treated with fresh DMEM containing 10% serum. Error bars represent the s.e.m. of n = 5 for a and n = 3 for b, c, except hPSC#1-conditioned medium in b where n = 4, from independent experiments. One-way ANOVA was performed. a, ***P = 0.0004 for hPSC#1 versus control, P = 0.0018 for hPSC#2 versus control; b, ***P < 0.0001; c, *P = 0.0293. d, e, Extracellular acidification rate (ECAR) is not significantly altered in 8988T cells when treated with conditioned medium from different cell lines. A representative Seahorse trace is shown in d. Error bars show s.d. of 6 independent wells from a representative tracing from 6 independent experiments (depicted in e). e, Results using conditioned medium from multiple PDAC and PSC lines including primary hPSCs. Error bars represent the s.e.m of n = 3 for MiaPaCa2, IMR-90, primary hPSC#1 and #2, and n = 6 for 8988T conditioned medium and hPSC#1, in independent experiments. f, g, Conditioned medium from hPSC#1 and hPSC#2 harvested in serum-free conditions retains the capacity to increase OCR in 8988T (f) and Tu8902 (g) cell lines. Data are represented as per cent increase in OCR in cells treated with conditioned medium versus cells treated with fresh DMEM without serum. Error bars represent the s.e.m of 3 independent experiments. 1-way ANOVA. f, ***P < 0.0001; g, ***P = 0.0005 for hPSC#1 versus control, P < 0.0001 for hPSC#2 versus control. h, Characterization of PSCs (primary hPSC #1 and #2 and hPSC#1 and #2) by RT–qPCR. Primary PSCs from tumours display an activated stellate cell signature in a similar fashion to that of the hPSC lines, as evidenced by the high levels of expression of the activated fibroblast marker, smooth muscle actin (αSMA), and the stellate cell marker, desmin. mRNA levels are represented as fold change compared to 8988T cells. IMR90 (human fibroblasts derived from lung tissue) and human PSCs derived from disease-free pancreata (primary hPSC N) are included as controls. Note: the transfer of normal PSCs to the tissue culture setting also leads to activation. Expression levels are normalized to β-actin. Error bars represent the s.d. of triplicate wells. i, Activated hPSCs are devoid of lipid droplets, an indicator of the activated state, as illustrated using oil red O staining. Tu8902 is included as a positive staining control. j, Conditioned medium from hPSCs does not alter OCR of non-transformed pancreatic ductal cells (HPDE). Error bars represent the s.d. of quintuplicate wells from a representative experiment (of 3 independent experiments). One-way ANOVA: P > 0.9. k–m, The ability of hPSC-conditioned medium to increase PDAC OCR is retained after boiling at 100 °C for 15 min in both Tu8902 (k) and MiaPaCa2 (l) as well as after three consecutive freeze (−80 °C, 10 min)-thaw (60 °C, 10 min) cycles in 8988T, as depicted in m. Error bars represent the s.d. of 4 independent wells from representative experiments (of 3 experiments). One-way ANOVA. k, *P = 0.0004 for hPSC#1 boiled conditioned medium versus control, P = 0.0001 for hPSC#1-conditioned medium versus control; l, ***P = 0.0002 for hPSC boiled versus control, P < 0.0001 for hPSC versus control; m, *P = 0.0011. n, The factor secreted by hPSCs that increases PDAC OCR is retained in the <3-kDa fraction of hPSC-conditioned medium. Error bars represent the s.e.m of 3 independent experiments. One-way ANOVA. *P = 0.0175, ***P = 0.0007 for hPSC versus control, P = 0.0015 for <3kDa versus control.
Extended Data Figure 2 Alanine is secreted by pancreatic stellate cells and consumed by PDAC cells.
a, Schematic of the metabolomic experiments depicted in Fig. 1d. b, The amino acids alanine, glutamate, proline and asparagine are differentially secreted by PSCs and consumed by PDAC cells. The alanine data here are also presented in Fig. 1d. Error bars represent the s.d. of n = 3 technical replicates from independently prepared samples from individual wells. t-tests were performed, for alanine: *P = 0.0176, **P = 0.0097; for glutamate, *P = 0.0108, ***P = 0.0024; for proline, *P = 0.0013 for hPSC#1 conditioned medium versus 8988T-conditioned medium, P = 0.0024 for double-conditioned medium versus 8988T-conditioned medium; for asparagine, *P = 0.0125. c, A mixture of non-essential amino acids (1 mM of NEAA: alanine, asparagine, aspartate, glutamate, proline and serine) increases MiaPaCa2 OCR in a similar fashion to PSC-conditioned medium. Among these NEAAs, only alanine can increase PDAC OCR to an extent comparable to the NEAA mixture. Data are normalized to cells treated with fresh DMEM with 10% serum. Error bars represent the s.e.m of 3 experiments. ***P < 0.0001. d, Profile of the U-13C-glucose and U-13C-glutamine derived NEAA secretome of hPSCs. Error bars represent the s.d. of n = 3 technical replicates from independently prepared samples from individual wells. e, PSCs were labelled to saturation with U-13C-glucose and U-13C-glutamine. Alanine was the only labelled metabolite that showed a statistically significant increase in the PSC-conditioned medium (compared to 8988T-conditioned medium) and a decrease in the double conditioned medium (PSC-conditioned medium added to 8998T cells). Error bars, s.d. of n = 3 technical replicates from independently prepared samples from individual wells. A two-tailed t-test was performed, ***P < 0.0001. f, Alanine standard curve as determined by LC–MS/MS. Data points for conditioned medium from hPSC (green diamond), 8988T (red triangle) and Tu8902 (red square) are displayed on the alanine standard curve. These data are presented in Fig. 1f in μM per 106 cells. Error bars represent the s.d. of n = 3 technical replicates from independently prepared samples from individual wells. t-test, ***P < 0.0001. g, h, Alanine is secreted by PSCs in the presence (g) or absence (h) of serum. Error bars represent the s.d. of n = 3 technical replicates from independently prepared samples from individual wells. t-test performed; g, ***P < 0.0001 for control versus hPSC#1, P = 0.0007 for control versus hPSC#2; h, ***P = 0.0003 for control versus hPSC#1, P = 0.0004 for control versus hPSC#2. i, The rate of PSC Ala secretion into conditioned medium was determined over a 72-h period using LC–MS; error bars represent s.d. of n = 4 technical replicates from independently prepared samples from individual wells. j, k, The levels of amino acids (j) and lactate (k) in complete medium conditioned by hPSC#1 were monitored over a 72-h period. Alanine was the most relatively secreted metabolite and surpassed even lactate. Metabolite levels are normalized to time 0 (fresh DMEM with 10% dialysed serum). Error bars represent the s.d. of n = 4 technical replicates from independently prepared samples from individual wells. Two-way ANOVA was performed; ***P < 0.0001. The same data are used for alanine and presented in curves in i–k. l, Alanine was the most avidly consumed amino acid by 8988T cells treated with hPSC#1-conditioned medium. Error bars represent the s.d. of n = 4 technical replicates from independently prepared samples from individual wells. Two-way ANOVA was performed; ***P < 0.0001 for the last time-point.
Extended Data Figure 3 Alanine secreted by stellate cells is used by PDAC to fuel biosynthetic reactions.
a–c, Knockdown of GPT1 or GPT2 in PDAC cells (a) significantly attenuates the ability of hPSC-conditioned medium to increase OCR in Tu8902 cells (b). This observation was repeated with conditioned medium from an independent hPSC line in 8988T cells (c). Error bars represent the s.e.m of 3 independent experiments. One-way ANOVA; b, *P = 0.0134; c, *P = 0.0129. d–j, Metabolic tracing studies using U-13C-Ala and U-13C-pyruvate (Pyr) (f–h). d, Metabolic tracing studies using U-13C-Ala in 8988T cells. Error bars, s.d. of n = 3. Two-way ANOVA was performed: for alanine, ***P < 0.0001; for lactate, ***P = 0.0001, **P = 0.0086. e, Intracellular accumulation and labelling of alanine in Tu8902 cells treated with 1 mM alanine. Two-way ANOVA was performed: ***P < 0.0001. f–h, Intracellular accumulation and labelling of alanine in 8988T cells treated with 1 mM pyruvate or 1 mM alanine grown in media containing different glucose (Glc) concentrations (0.5, 10, 25 mM). Error bars represent s.d. of n = 3. i, j, U-13C-Ala does not contribute to glycolysis or gluconeogenesis as seen for the metabolites glucose 6-phosphate (G6P), fructose 6-phosphate (F6P), fructose bis-phosphate (FBP), glyceraldehyde 3-phosphate (Ga3P), 3-phosphoglycerate (3PG), and phosphoenolpyruvate (PEP) in 8988T (i) or Tu8902 (j) PDAC cell lines. Label can be incorporated in lactate (Lac) independent of glycolysis. Error bars represent s.d. of n = 3. k, 1 mM alanine does not significantly increase basal extra cellular acidification rate (ECAR) of 8988T cells. Error bars represent s.d. of 6 replicates. Data presented for a representative experiment (of 3 experiments), P = 0.6082. l, m, Alanine does not alter the NAD+/NADH ratio in 8988T cells to the same extent as pyruvate in medium containing either 0.5 mM (l) or 25 mM (m) extracellular glucose. 10 mM pyruvate and 10 mM lactate were included as controls; error bars represent s.e.m of n = 4 (l) or n = 3 (m) independent experiments. t-test performed; l, *P = 0.0205; m, *P = 0.0291. n–q, Alanine contributes minimally to lactate in both Tu8902 (n) and 8988T (o–q) cells, and independently of glucose concentrations in medium, as seen by tracing of U-13C-Ala: 0.5 mM (o), 10 mM (p) or 25 mM (q) glucose. Pyruvate labels ~50% of the lactate pool in 8988T cells (o–q) independent of the glucose concentration in the medium. Error bars represent the s.d. of n = 3. d–j, n–o, n = 3 technical replicates from independently prepared samples from individual wells
Extended Data Figure 4 Alanine fuels the TCA cycle in 8988T PDAC cells.
a, 1 mM U-13C-Ala labelling of 8988T cells for 24 h shows incorporation of alanine carbon into the TCA cycle metabolites citrate (Cit), isocitrate (Iso), fumarate (Fum), malate (Mal) and NEAAs, aspartate and glutamate, derived thereof. These data are presented in Fig. 2 as fractional labelling (Fig. 2e) and as the percentage of the citrate pool incorporating the label (Fig. 2f). M0 refers to an unlabelled metabolite with no heavy carbons (unlabelled isotopomer, 12C), M1 is an isotopomer with one heavy (13C) carbon that can be in any position in the molecule, M2 is a metabolite with any two heavy carbons (13C), M3 with 3 and so on. The maximal M for a given species represents the fully 13C labelled isotopomer (for example, for citrate that has a 6-carbon skeleton, it would be M6). In the schematic illustration, U-13C-Ala is represented as three red balls, each depicting a labelled carbon atom. This is converted into U-13C-Pyr (M3) and shuttled into the mitochondria. The conversion of U-13C-Pyr to Ac-CoA results in the loss of one carbon as CO2. Ac-CoA is then added to oxaloacetate (OAA) to form 2-13C labelled citrate (M2). This citrate traverses around the TCA cycle and is metabolized into the other TCA cycle metabolites. The carbon labelling patterns are indicated with red (labelled) and white (unlabelled) balls. αKG, α-ketoglutarate; Succ, succinate. b–e, Contribution of alanine and pyruvate to TCA cycle metabolites citrate (b), isocitrate (c), fumarate (d) and malate (e) as shown by U-13C-Ala and U-13C-Pyr tracing in 8988T cells in medium containing 10 mM glucose and 2 mM glutamine. f–k, Contribution of alanine to TCA cycle metabolites citrate (f), isocitrate (g), fumarate (h) and malate (i) as well as the NEAAs Glu (j) and Asp (k) is independent of glucose concentration in the medium, as shown by U-13C-Ala tracing in medium containing 0.5 mM, 10 mM or 25 mM glucose. Data are presented as total ion currents; error bars represent the s.d. of n = 3 technical replicates from independently prepared samples from individual wells. The raw data for b–k are presented in Supplementary Information Fig. 2a–j.
Extended Data Figure 5 Alanine carbon contributes to the TCA cycle in multiple PDAC cell lines.
a–d, 1 mM U-13C-Ala labelling of Tu8902 (a), MiaPaCa2 (b), Panc-1 (c) and mPanc96 (d) cells show incorporation of alanine carbon into the TCA cycle metabolites citrate, isocitrate, malate and fumarate and the NEAAs Asp and Glu. Data are presented as total ion currents; error bars represent the s.d. of n = 3 technical replicates from independently prepared samples from individual wells. These data are presented in Fig. 2f as the percentage of the citrate pool incorporating label.
Extended Data Figure 6 Alanine relieves the demand of PDAC cells on glucose and glutamine carbon so that it can fuel other biosynthetic processes.
a, The addition of alanine to PDAC cells labelled with U-13C-glucose significantly increases the unlabelled citrate, with a corresponding reduction in the labelled (M2) citrate. A t-test was performed; ***P = 0.0009, *P = 0.0169. b–c, Alanine is a meaningful source of carbon for the de novo biosynthesis of the free fatty acids palmitate (b) and stearate (c) in two PDAC cell lines. The sum of the isotopomers from these data are presented in Fig. 2g, h. d–g, The addition of alanine to PDAC cells labelled with U-13C-glucose reduces glucose carbon incorporation into palmitate in 8988T (d) and Tu8902 (e) cells as well as into stearate in both 8988T (f) and Tu8902 (g) PDAC cells. This is shown by a decrease in highly enriched species (M14, M16 for palmitate and M16, M18 for stearate) and an increase in less enriched species (M6, M8, M10 for palmitate and M6, M8, M10, M12 for stearate). h, U-13C-glucose tracing studies illustrate that alanine drives glucose carbon into the serine biosynthetic pathway, as demonstrated by significant increases in fully labelled (M3), glucose-derived 3-phosphoglycerate (3PG), 3-phosphoserine (p-Ser), serine (Ser), and M2 glycine. A t-test was performed; *P = 0.0355 for 3PG (Ala) versus control; ***P = 0.0041 for p-Ser (Ala) versus control; *P = 0.0172 for Ser (Ala) versus control; *P = 0.0123 for Gly (Ala) versus control. i, j, Alanine increases serine biosynthetic pathway activity, as seen for changes in the precursors 3PG and p-Ser. This effect is enhanced in cells grown under low glucose (0.5 mM) conditions (j). A t-test was performed; i, *P = 0.0355, ***P = 0.0041; j, ***P = 0.0005 for 3PG Ala versus mock, P < 0.0001 for pSer Ala versus mock. k, l, Alanine alters the contribution of glutamine carbon to the TCA cycle as seen by changes in the U-13C-Gln-derived fractional labelling of the TCA metabolites citrate, isocitrate, fumarate and malate upon addition of 1 mM alanine in 8988T (k) and Tu8902 (l) PDAC cell lines. Data are presented as relative metabolite for a, per cent labelling for b–g, k, l, and total ion currents for h–j. Error bars represent the s.d. of n = 3 (a, h–l) and n = 4 (b–g) technical replicates from independently prepared samples from individual wells. The raw data for k, l are presented in Supplementary Information Fig. 2k, l.
Extended Data Figure 7 Stellate cell autophagy is required to support PDAC cell metabolism through the secretion of alanine.
a, PSCs immunostained for LC3-II display basal autophagy in standard culture conditions as shown by the presence of autophagosomes represented by LC3 puncta (green). Nuclei are counterstained with DAPI (blue). b, Representative images of autophagic puncta in control (shGFP) or autophagy impaired (shATG5 and shATG7) PSCs using an LC3 tandem fluorescence (GFP–RFP) reporter. Knockdown of ATG5 or ATG7 significantly decreases autophagosome formation. c, Quantification of autophagy in PSCs. Error bars represent the s.e.m of n = 13 for shGFP; n = 12 for shATG5#1, shATG7#1 and #2; n = 10 for shATG5#2. Two-way ANOVA: **P = 0.0067 for shGFP versus shATG5#1, ***P = 0.0009 for shGFP versus shATG5#2, ***P < 0.0001 for shGFP versus shATG7#1 or #2. d, PDAC-conditioned medium increases autophagy in hPSC cells, as determined using an LC3 tandem fluorescence (GFP–RFP) reporter. The relative abundance of autolysosomes and autophagosomes (red and yellow puncta, respectively) is a measure of flux; data are quantified in Fig. 3c. e, f, Western blot demonstrating knockdown of ATG5 and ATG7 using two independent shRNAs in hPSC#1 (e) and hPSC#2 (f). A decrease in autophagy is shown by a decrease in LC3-II (lower band). g, Suppression of PSC autophagy by ATG5 or ATG7 knockdown attenuates the ability of PSC- (hPSC#2)-conditioned medium to increase PDAC OCR. Error bars represent the s.d. of quadruplicate wells from a representative experiment (of 3 experiments). One-way ANOVA; ***P = 0.0006. h, Suppression of PSC autophagy by ATG5 or ATG7 knockdown attenuates the ability of PSC- (hPSC#1)-conditioned medium to increase PDAC OCR in serum-free conditions and this phenotype can be rescued by addition of 1 mM exogenous alanine. Data are normalized to cells treated with serum-free DMEM. Error bars represent the s.e.m of n = 4 for 8988T, 1mM Ala, shGFP groups; n = 3 for shATG5#2, shATG7#1, shATG5#2 + Ala, shATG7#1 + Ala and shGFP + Ala groups in independent experiments. One-way ANOVA; ***P = 0.0004 for control versus 1 mM Ala, P = 0.0003 for control versus hPSC, P < 0.0001 for control versus hPSC shATG5 #2 + Ala, P = 0.0002 for control versus hPSC shATG7 #1 + Ala, P < 0.0001 for control versus hPSC + Ala. i, ATG5 or ATG7 knockdown in hPSCs decreases intracellular alanine concentrations compared to shGFP controls. Error bars, s.d. of n = 3 technical replicates from independently prepared samples from individual wells. One-way ANOVA: *** P = 0.0020 for hPSC-shGFP versus hPSC-shATG5; P = 0.0040 for hPSC-shGFP versus hPSC-shATG7. j, In serum-free conditions, ATG5 or ATG7 knockdown in hPSCs also decreases the secretion of alanine relative to shGFP controls. Error bars represent s.d. of n = 3 technical replicates from independently prepared samples from individual wells. t-test; *P = 0.0428 for hPSC versus hPSC-shATG5, P = 0.0477 for hPSC versus hPSC-shATG7. k–m, Autophagy inhibition by ATG5 or ATG7 knockdown (e, f, l) or chloroquine (CQ) treatment (10 μM) decreases alanine levels in conditioned medium from hPSC#2 (k) and mouse PSC (m) as compared to shGFP or mock-treated controls. Error bars represent s.d. of n = 3 technical replicates from independently prepared samples from individual wells. t-test; k, *P = 0.0213 for shGFP versus shATG7, P = 0.02061 for shGFP versus CQ; m, ***P < 0.0001 for shGFP versus shATG5, P = 0.0003 for shGFP versus shATG7, P = 0.0001 for shGFP versus CQ. n, Autophagy inhibition has a modest impact on PSC proliferation. Data are plotted as relative cell proliferation in arbitrary units (a.u.). Error bars, s.d. of 4 independent wells from a representative experiment (of 4 experiments). One-way ANOVA; P values for the last time point are as follows: *P = 0.0103 for shGFP versus shATG5#1, *P = 0.0124 for shGFP vs shATG5#2, P = 0.6657 for shGFP versus shATG7#1, ***P < 0.0001 for shGFP vs shATG7#2. o, p, Autophagy inhibition does not significantly impact hPSC (o) or mPSC (p) viability following growth for 48 h in serum-free conditions, as shown by a trypan-blue exclusion assay. Error bars represent s.e.m of n = 3 independent experiments.
Extended Data Figure 8 Stellate cell metabolite secretion can support PDAC growth under nutrient-limiting conditions.
a, hPSC-conditioned medium does not significantly affect proliferation of 8988T cells grown in complete medium (25 mM glucose, 4 mM Gln, 10% serum). Alanine supplementation contributes modestly to PDAC growth in complete medium. Error bars represent the s.d. of 6 replicate wells from a representative experiment (of 4 experiments). One-way ANOVA; **P = 0.0079. b, c, hPSC #2 or hPSC #3-conditioned medium can sustain in vitro proliferation over 48 h for 8988T (b) and Tu8902 (c) cells, as compared to PDAC-conditioned medium. Data are normalized to growth in serum-free DMEM and complete serum medium is included as a positive control. Error bars represent s.e.m of n = 4 experiments for b and s.d. of quadruplicate wells from a representative experiment (of 3 experiments) for c. One-way ANOVA; b, ***P < 0.0001; c, **P = 0.0091, ***P < 0.0001. d, hPSC-conditioned medium facilitates proliferation of 8988T cells grown in low glucose (0.5 mM) medium. Conditioned medium from hPSCs in which autophagy is inhibited loses the ability to support PDAC growth. Supplementation of medium with exogenous alanine rescues PDAC proliferation under low glucose conditions in a manner akin to the positive control, 10 mM glucose-containing medium. Error bars represent the s.e.m of 4 independent experiments. One-way ANOVA; *P = 0.0420 for GFP versus control, P = 0.0158 for complete medium versus control; **P = 0.0054. e–g, hPSC#1-conditioned medium increases PDAC proliferation in MiaPaCa2 (e), Tu8902 (f) and 8988T (g) cells in serum-free medium. Conditioned medium from hPSCs in which autophagy is inhibited is less effective at maintaining PDAC proliferation. Alanine increases PDAC proliferation under serum-free conditions, and it can rescue the proliferation-inducing capacity of autophagy-deficient hPSC-conditioned medium (g). The addition of 10% serum is included as a positive control. Error bars represent the s.e.m of 8 independent experiments for e, f and 3 independent experiments for g. One-way ANOVA; e, ***P = 0.0011 for shGFP versus control, ***P = 0.0013 for 1 mM alanine versus control, ***P = 0.0001 for complete medium versus control; f, ***P = 0.0007 for shGFP versus control, **P = 0.0042 for alanine versus control, ***P < 0.0001 for complete medium versus control; g, ***P < 0.0001. h, i, Mouse PSC-conditioned medium increases proliferation in 8988T (h) and MiaPaCa2 (i) PDAC cell lines over 48 h in serum-free conditions. This effect is impaired when the conditioned medium is collected from mouse PSCs in which autophagy is inhibited. Error bars represent s.e.m of n = 3 experiments. One-way ANOVA; h, ***P = 0.0002 for shGFP versus control, ***P < 0.0001 for complete medium versus control; i, *P = 0.0108, ***P = 0.0002. j–l, PDAC proliferation under low glucose (0.5 mM) conditions can be rescued by 1 mM alanine or pyruvate, but not by 1 mM lactate in 8988T (j), Tu8902 (k) and MiaPaCa2 (l) PDAC cell lines. Error bars represent the s.d. of quadruplicate wells from a representative experiment (of 4 experiments). One-way ANOVA; j, ***P = 0.0013, **P = 0.0085 for 1 mM alanine versus control, P = 0.0070 for 10 mM glucose versus control; k, *P = 0.0323 for 1 mM alanine versus control, ***P = 0.0044 for 1 mM pyruvate versus control, ***P = 0.0010 for 10mM glucose versus control; l, **P = 0.0060 for 1 mM alanine versus control, ***P = 0.0008 for 1 mM pyruvate versus control, ***P = 0.0018 for 10 mM glucose media versus control. m, 8988T PDAC cells depleted for GPT1 and grown in serum-free medium do not proliferate in response to hPSC-conditioned medium or alanine, relative to control shGFP or GPT2-depleted cells. Data are represented as fold-change over 48 h and complete medium is included as a positive control. Error bars represent s.e.m. from 3 independent experiments. Two-way ANOVA; for shGFP, ***P < 0.0001 for control versus hPSC#1, ***P = 0.0060 for control versus alanine, ***P < 0.0001 for control versus complete medium; for shGPT1 #1, ***P = 0.0005; for shGPT1 #2, ***P < 0.0001, *P = 0.0493; for shGPT2 #1, ***P < 0.0001; for shGPT2 #2, ***P = 0.0004 for control versus hPSC#1, ***P < 0.0001 for others.
Extended Data Figure 9 Subcutaneous PDAC xenograft tumour growth is supported by autophagy-competent pancreatic stellate cells.
a, Immunoblot for ATG5 and ATG7 knock-down in hPSC#1 cells infected before subcutaneous co-injection. LC3-II shows the inhibition of autophagy in these cells. b, Tumour growth is enhanced following co-injection of hPSCs with 8988T PDAC cells. This affect is significantly attenuated when autophagy is suppressed in the hPSCs during the initial phases of tumour growth. Error bars represent the s.e.m for 10 tumours per condition at each time point. t-tests were performed for each time point; *P < 0.05. c–e, Co-injection of MiaPaCa-2 PDAC cells with PSCs significantly enhances early tumour growth, analysed at 25 days post-injection (c) and decreases tumour-free survival (d). This effect is significantly attenuated when autophagy is suppressed in the PSCs. e, Tumour growth kinetics. Error bars represent the s.e.m. of 10 tumours per condition per time point, except for the PSC-shGFP control, for which only 5 animals were injected. c, One-way ANOVA, **P = 0.0099, ***P = 0.0020; d, log-rank Mantel-Cox test, *P = 0.0450, **P = 0.00174, ***P < 0.0001; e, t-tests for each time point, *P < 0.05. f, Representative sections for endpoint analysis from tumours for each experimental group stained with trichrome (top, blue) or α-smooth muscle actin (αSMA) (bottom, brown). Minimal residual intra-tumour collagen deposition and stromal content remains at endpoint. The asterisk in the αSMA staining images indicates a vessel and serves as a positive control. g–i, Early time-point analysis of MiaPaCa2 cells co-injected with RFP-labelled hPSCs in nude mouse flanks; tumours removed at 2 weeks post-injection. g, Representative sections of tumours stained with mCherry, a lineage label for the injected PSCs, illustrating minimal stromal content even at early time points. h, RFP immunoblot quantification as a marker of remaining RFP-labelled stellate cells injected. Four tumours originating from MiaPaCa2 cells co-injected with control shGFP-hPSCs, three tumours from MiaPaCa2 cells co-injected with shATG5-hPSCs and two tumours from MiaPaCa2 cells co-injected with shATG7-hPSCs were quantified. Error bars represent the s.d. of 2–4 lanes quantified per condition, as indicated. t-test; n.s., P = 0.5982 for shGFP versus shATG5, P > 0.9999 for shGFP versus shATG7. i, RFP immunoblot as a marker of remaining RFP-labelled stellate cells injected. Quantification shown in h. The full blot containing all nine samples is presented in Supplementary Fig. 1e.
Extended Data Figure 10 Orthotopic PDAC xenograft tumour growth is supported by autophagy-competent pancreatic stellate cells.
a, Representative high-resolution ultrasound images of the pancreata of nude mice 4 weeks after intra-pancreatic injection with MiaPaCa2 cells alone or with control shGFP or autophagy-impaired shATG5 or shATG7 hPSCs. hPSC-only injections are included as negative controls. Skin and spleen (Sp) are indicated as spatial references; tumours are outlined in red; prospective tumours that did not meet threshold at the time of imaging are outlined in orange. b, c, Co-injection of MiaPaCa-2 PDAC cells with PSCs in the pancreata of nude mice significantly enhances early tumour growth at 21 days post-injection (b) and decreases tumour-free survival (c) in this orthotopic xenograft model. Again, this effect is significantly attenuated when autophagy is suppressed in the PSCs. Error bars, s.e.m. of 5 tumours per condition per time point. b, One-way ANOVA; *P = 0.0283, ***P = 0.0010; c, log-rank Mantel-Cox test; *P = 0.0278 for MiaPaCa2 + hPSC#1-shGFP versus MiaPaCa2 + hPSC#1-shATG5, *P = 0.0288, ***P = 0.0017 for MiaPaCa2 + hPSC#1-shGFP versus MiaPaCa2. d, Tumour growth kinetics following co-injection of MiaPaCa2 PDAC cells with hPSCs show enhanced tumour growth. This affect is significantly attenuated when autophagy is suppressed in the hPSCs during the initial phases of tumour growth. Error bars represent the s.e.m. of tumours from 5 animals measured per condition at each time point. t-tests for each time point; *P < 0.05. e, Representative endpoint sections of tumours 5 weeks post-injection stained with αSMA, a marker of PSCs, and the lineage label mCherry. Together, these stains illustrate that minimal stromal content remains at endpoint.
Supplementary information
Supplementary Figures
This file contains Supplementary Figures 1 and 2. (PDF 1529 kb)
Supplementary Data
This file contains the statistical information for Figures 1-4 and Extended Data Figures 1-3 and 6-10. (PDF 1809 kb)
Supplementary Tables
This file contains Supplementary Tables 1-4. (XLSX 31 kb)
Rights and permissions
About this article
Cite this article
Sousa, C., Biancur, D., Wang, X. et al. Pancreatic stellate cells support tumour metabolism through autophagic alanine secretion. Nature 536, 479–483 (2016). https://doi.org/10.1038/nature19084
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nature19084
This article is cited by
-
Nutrient restriction-activated Fra-2 promotes tumor progression via IGF1R in miR-15a downmodulated pancreatic ductal adenocarcinoma
Signal Transduction and Targeted Therapy (2024)
-
Targeting paraptosis in cancer: opportunities and challenges
Cancer Gene Therapy (2024)
-
Lysosomes as coordinators of cellular catabolism, metabolic signalling and organ physiology
Nature Reviews Molecular Cell Biology (2024)
-
The dual role of autophagy in HPV-positive head and neck squamous cell carcinoma: a systematic review
Journal of Cancer Research and Clinical Oncology (2024)
-
Cancer-associated fibroblast-derived acetate promotes pancreatic cancer development by altering polyamine metabolism via the ACSS2–SP1–SAT1 axis
Nature Cell Biology (2024)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.