Abstract
The repair and regeneration of tissues using endogenous stem cells represents an ultimate goal in regenerative medicine. To our knowledge, human lens regeneration has not yet been demonstrated. Currently, the only treatment for cataracts, the leading cause of blindness worldwide, is to extract the cataractous lens and implant an artificial intraocular lens. However, this procedure poses notable risks of complications. Here we isolate lens epithelial stem/progenitor cells (LECs) in mammals and show that Pax6 and Bmi1 are required for LEC renewal. We design a surgical method of cataract removal that preserves endogenous LECs and achieves functional lens regeneration in rabbits and macaques, as well as in human infants with cataracts. Our method differs conceptually from current practice, as it preserves endogenous LECs and their natural environment maximally, and regenerates lenses with visual function. Our approach demonstrates a novel treatment strategy for cataracts and provides a new paradigm for tissue regeneration using endogenous stem cells.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Barbosa-Sabanero, K. et al. Lens and retina regeneration: new perspectives from model organisms. Biochem. J. 447, 321–334 (2012)
Tsonis, P. A. & Del Rio-Tsonis, K. Lens and retina regeneration: transdifferentiation, stem cells and clinical applications. Exp. Eye Res. 78, 161–172 (2004)
Gwon, A. Lens regeneration in mammals: a review. Surv. Ophthalmol. 51, 51–62 (2006)
Gwon, A. E., Gruber, L. J. & Mundwiler, K. E. A histologic study of lens regeneration in aphakic rabbits. Invest. Ophthalmol. Vis. Sci. 31, 540–547 (1990)
Stevens, G. A. et al. Global prevalence of vision impairment and blindness: magnitude and temporal trends, 1990–2010. Ophthalmology 120, 2377–2384 (2013)
Lois, N., Taylor, J., McKinnon, A. D. & Forrester, J. V. Posterior capsule opacification in mice. Arch. Ophthalmol. 123, 71–77 (2005)
Visser, N., Bauer, N. J. & Nuijts, R. M. Toric intraocular lenses: historical overview, patient selection, IOL calculation, surgical techniques, clinical outcomes, and complications. J. Cataract Refract. Surg. 39, 624–637 (2013)
Mamalis, N., Davis, B., Nilson, C. D., Hickman, M. S. & Leboyer, R. M. Complications of foldable intraocular lenses requiring explantation or secondary intervention – 2003 survey update. J. Cataract Refract. Surg. 30, 2209–2218 (2004)
Jacobi, P. C., Dietlein, T. S. & Konen, W. Multifocal intraocular lens implantation in pediatric cataract surgery. Ophthalmology 108, 1375–1380 (2001)
Bothun, E. D. et al. One-year strabismus outcomes in the Infant Aphakia Treatment Study. Ophthalmology 120, 1227–1231 (2013)
Infant Aphakia Treatment Study Group. A randomized clinical trial comparing contact lens with intraocular lens correction of monocular aphakia during infancy: grating acuity and adverse events at age 1 year. Arch. Ophthalmol. 128, 810–818 (2010)
Beebe, D. C., Holekamp, N. M. & Shui, Y. B. Oxidative damage and the prevention of age-related cataracts. Ophthalmic Res. 44, 155–165 (2010)
Park, I. K. et al. Bmi-1 is required for maintenance of adult self-renewing haematopoietic stem cells. Nature 423, 302–305 (2003)
Lessard, J. & Sauvageau, G. Bmi-1 determines the proliferative capacity of normal and leukaemic stem cells. Nature 423, 255–260 (2003)
Molofsky, A. V. et al. Bmi-1 dependence distinguishes neural stem cell self-renewal from progenitor proliferation. Nature 425, 962–967 (2003)
Tsonis, P. A. Animal models in eye research . 1st edn, (Academic Press, 2008)
Gogate, P., Kalua, K. & Courtright, P. Blindness in childhood in developing countries: time for a reassessment? PLoS Med. 6, e1000177 (2009)
Wilson, M. E., Saunders, R. A. & Trivedi, R. H. Pediatric Ophthalmology: Current Thought and A Practical Guide . (Springer-Verlag, Berlin, 2009)
You, C. et al. Visual impairment and delay in presentation for surgery in chinese pediatric patients with cataract. Ophthalmology 118, 17–23 (2011)
Wilson, M. E., Trivedi, R. H. & Pandey, S. K. Pediatric Cataract Surgery: Techniques, Complications, and Management . (Lippincott Williams & Wilkins, 2005)
Zheng, Q. et al. Vitreous surgery for macular hole-related retinal detachment after phacoemulsification cataract extraction: 10-year retrospective review. Eye (Lond.) 26, 1058–1064 (2012)
Zhou, M., Leiberman, J., Xu, J. & Lavker, R. M. A hierarchy of proliferative cells exists in mouse lens epithelium: implications for lens maintenance. Invest. Ophthalmol. Vis. Sci. 47, 2997–3003 (2006)
Plager, D. A. et al. Complications, adverse events, and additional intraocular surgery 1 year after cataract surgery in the Infant Aphakia Treatment Study. Ophthalmology 118, 2330–2334 (2011)
Nihalani, B. R. & VanderVeen, D. K. Technological advances in pediatric cataract surgery. Semin. Ophthalmol. 25, 271–274 (2010)
Gwon, A., Gruber, L. J. & Mantras, C. Restoring lens capsule integrity enhances lens regeneration in New Zealand albino rabbits and cats. J. Cataract Refract. Surg. 19, 735–746 (1993)
Rowan, S. et al. Notch signaling regulates growth and differentiation in the mammalian lens. Dev. Biol. 321, 111–122 (2008)
Mich, J. K. et al. Prospective identification of functionally distinct stem cells and neurosphere-initiating cells in adult mouse forebrain. Elife 3, e02669 (2014)
Tronche, F. et al. Disruption of the glucocorticoid receptor gene in the nervous system results in reduced anxiety. Nature Genet. 23, 99–103 (1999)
Gabriel, G. M. & Mutti, D. O. Evaluation of infant accommodation using retinoscopy and photoretinoscopy. Optom. Vis. Sci. 86, 208–215 (2009)
Hainline, L., Riddell, P., Grose-Fifer, J. & Abramov, I. Development of accommodation and convergence in infancy. Behav. Brain Res. 49, 33–50 (1992)
Banks, M. S. The development of visual accommodation during early infancy. Child Dev. 51, 646–666 (1980)
Acknowledgements
We thank E. Yeh, L. Xi, J. Shelton, A. Pineda and R. Ufret-Vincenty for technical assistance. This study was funded by 973 Program (2015CB964600, 2014CB964900, 2013CB967504); a Major International Joint Research Project (No. 81320108008); 863 Program (2014AA021604), NSFC (No. 81270981); the State Key Laboratory of Ophthalmology, Zhongshan Ophthalmic Center, Sun Yat-sen University; Research to Prevent Blindness and the Howard Hughes Medical Institute.
Author information
Authors and Affiliations
Contributions
H.L., S.H., Z.L., S.C., .X.L., L.L., B.C., Y.W. and Y.L. conducted the clinical trial; H.O., Jie Z., Y.Z., J.C., H.C. and S.P. performed mouse LEC lineage tracing experiments; H.O., J.Z., G.C., G.L., Y.X., S.P., Jin Z., M.J., A.Q., F.S., X.L., R.H., W.S. and D.C. performed LEC characterization and differentiation experiments; D.G., C.H., F.W., Z.S. and J.H. analysed clinical trial data; H.O., M.K., D.S-K., C.C., M.J., Y.W., W.S., D.C., S.Z., L.Z. and S.C. performed gene expression studies and analysed data; R.A.J.S. and S.J.M. performed and analysed the experiments related to BMI-1 function in mouse lens epithelium. Y.L, R.M. and K.Z. designed the study and wrote the paper. All authors discussed the results and commented on the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Extended data figures and tables
Extended Data Figure 1 Surgical methods and lens regeneration for congenital cataract.
a, b, Slit-lamp photography of ‘doughnut-like’ lens regeneration at different time points after treatment using the current surgical method. Two years after surgery (a), the transparent regenerated lens tissue contained the sealed capsular opening with an opaque white scar at the centre. The regions between the dashed circles indicated by the red arrows are the regenerated lens tissues. Four years after surgery (b), the capsular opening was constricted compared to that seen at two years post-surgery, indicating continued growth of the regenerated lens. There was also the complication of iridolenticular synechiae. c, Schematic diagrams of the current surgical method for paediatric cataracts: the currently practiced paediatric ACCC creates an opening 6 mm in diameter at the centre of the anterior capsule, removing the LECs underneath it and leaving a relatively large wound area of 28 mm2. The scars formed often cause postoperative VAO. Additionally, PCCC and anterior vitrectomy are commonly performed at follow-up visits.
Extended Data Figure 2 BrdU pulse labelling of human LECs.
a, Whole mount of a human lens capsule showing BrdU+ cells (brown) by enzymatic immunohistology and diaminobenzidine staining. b, High-magnification images of human donor lenses showing BrdU+ LECs. c, Bar graph showing quantification of BrdU+ cells. There was an age-dependent decrease in the number of BrdU+ cells (8 months, 39.9 ± 8.1; 30 years, 20.3 ± 7.3 and 40 years, 5.9 ± 2.9; 8 months versus 40 years, *P < 0.05). Six randomly chosen fields of each capsule were used for analysis, four samples in each group, (n = 24 fields, chosen over four samples). d, High-magnification images of whole-mount staining of human lens capsules with or without injury showed a marked increase in the number of BrdU+ cells after injury. e, Bar graph showing quantification of BrdU+ cells. The contralateral eyes from the respective donors were used as controls. There was a significant increase in number of BrdU+ cells. No injury, 1.5 ± 1.2; after injury, 18.4 ± 4.2; fold change after injury, 11.3 ± 2.5; *P < 0.05. Six randomly chosen fields within the germinative zone of each capsule were used for analysis, five samples in each group (n = 30 fields, chosen over five samples). Data shown as means ± s.d. f, Cultured human fetal LECs were positive for BMI-1 (green, right upper panel); co-staining of PAX6 (red) and Ki67 (green), middle panels; co-staining of SOX2 (red) and Ki67 (green), lower panels. g, Co-staining of PAX6 (red) and SOX2 (green) of human fetal LECs. All scale bars, 100 μm.
Extended Data Figure 3 Conditional deletion of Bmi-1 led to decrease in Pax6+ and Sox2+ cells and cataract formation.
A, Loss of Bmi-1 reduced the Pax6+ and Sox2+ LECs population. a, Representative images of haematoxylin and eosin-stained lens sections from Bmi1fl/fl control mice and Nestin-cre;Bmi1fl/fl mice. b, Representative images of Bmi-1 (red) staining in LECs. c, Pax6 (red) and Sox2 (green) immunostaining. d, Percentage of Pax6+ (Bmi1fl/fl, 88.5 ± 2.9%; Nestin-cre;Bmi1fl/fl, 2.4 ± 2.3%) and Sox2+ (Bmi1fl/fl, 82.7 ± 3.9%; Nestin-cre;Bmi1fl/fl, 4.9 ± 1.5%) cells (n = 5 mice; 5 sections counted per mice, for a total of 25 sections across 5 mice), *P < 0.001. Data are shown as mean ± s.d. B, Conditional deletion of Bmi1 led to reduced LEC proliferation. The percentage of BrdU+ LECs per eye is shown (2M: Bmi1fl/fl, 2.6 ± 0.9%; Nestin-cre;Bmi1fl/fl, 3.0 ± 0.4%; n = 4 mice. 7M: Bmi1fl/fl, 1.5 ± 0.2%; Nestin-cre;Bmi1fl/fl, 0.6 ± 0.4%; n = 6 mice. 12M: Bmi1fl/fl, 1.8 ± 0.6%; Nestin-cre;Bmi1fl/fl, 0.2 ± 0.2%; n = 8 mice), two sections counted per eye. Statistical significance was assessed using a two-tailed Student’s t-test. *P < 0.05. Data are shown as mean ± s.d. C, Nestin (green) staining is shown in E13.5, E18.5, and 2-month-old wild-type mice. All scale bars, 100 μm. D, Representative images of lenses from Nestin-cre;Bmi1fl/fl and Bmi1fl/fl control mice. a, Cataracts are evident in 7- and 12-month-old Nestin-cre;Bmi1fl/fl mice (arrow). b, Deletion of Bmi-1 at 6 weeks of age with Nestn-creER did not recapitulate the cataract phenotype 10 months after tamoxifen treatment. Haematoxylin and eosin-stained sections of the same eyes are also shown. All scale bars, 100 μm.
Extended Data Figure 4 Loss of BMI-1 decreased the proliferative ability of LECs.
a, Phase-contrast photographs of human LECs (upper panels) and quantification of Ki67+ proliferating human fetal LECs upon BMI1 knockdown (shBMI1) compared to controls (two shRNAs gave similar results; n = 5, P < 0.05). Data shown as mean ± s.d. Blue indicates DAPI staining. b, Loss of BMI-1 did not significantly affect expression of LEC or lens fibre cell makers in LECs. BMI1 was reduced by 3.3-fold (all n = 3, P < 0.05); gene expression changes of LEC markers were: 1.3-fold increase (PAX6), 1.1-fold increase (SOX2), 1.3-fold increase (C-MAF) and 1.1-fold increase (E-cadherin); gene expression changes of differentiated lens fibre cell markers were: 1.6-fold increase (Filensin), 0.9 fold increase (CP49) and 1.4-fold decrease (CRYBA2). Two different shRNAs gave similar results; n = 5, P < 0.05. Data shown as mean ± s.d.
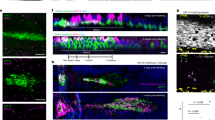
Extended Data Figure 5 Higher expression levels of Bmi1, Sox2 and Ki67 in Pax6+ LECs.
a, Pax6–GFP+ LECs were observed at the germinative zone. Left panel, a section of lens of a Pax6P0-3.9-GFPcre mouse at P1. Middle and right panels, higher magnification of the framed area in the left panel. Blue indicates DAPI staining. b, Upper panel, bright-field photograph showing flat-mount preparation of a lens capsule of a Pax6P0-3.9-GFPcre mouse at 6 months; lens capsule materials between two red circles were dissected to enrich Pax6–GFP+ LECs. Lower panel, fluorescence image of GFP+ LECs from the framed area in the upper panel. AC, anterior capsule; PC, posterior capsule. c, Comparison of gene expression levels in Pax6–GFP+ LECs versus GFP− LECs in anterior lens capsule in 6-month-old mice, increased expression of the following genes were observed: 10.1-fold in Pax6 (P < 0.005), 8.2-fold in Ki67 (P < 0.05), 4.3-fold in Bmi1 (P < 0.05), and 2.6-fold in Sox2 (P < 0.05), all n = 5. Data shown as mean ± s.d.
Extended Data Figure 6 Lens regeneration surgery in rabbits.
a, A 3.2-mm keratome was used to make a limbus tunnel incision at the 11–12 o’clock position into the anterior chamber. b, The capsular opening was created by a capsulorhexis needle. c, A 1–2 mm diameter anterior capsulotomy was performed using the anterior continuous curvilinear capsulorhexis (ACCC) technique near the capsular opening area (yellow arrow). d, A blunt needle was used to inject balanced salt solution for hydrodissection of the cortex from the anterior capsule. e, The cortex was removed using a phacoemulsification device. f, The remaining cortex was removed using irrigation and aspiration. h, An elbow I/A handle was used to clear the equatorial cortex. i, j, The limbus wound was sutured with an interrupted 10-0 nylon suture. The wound was found to be watertight.
Extended Data Figure 7 Lens regeneration in rabbits.
a, Haematoxylin and eosin staining of regenerated lenses at different time points after surgery. At postoperative day 1, a monolayer of LECs between the anterior and posterior capsules was visible (arrowheads). At postoperative day 4, LECs proliferated and covered the posterior capsule. At postoperative day 7, LECs in the posterior capsule began to elongate and differentiate. b, At postoperative day 28, LECs in the posterior capsule further elongated, forming primary lens fibres. c, Transparency and shape of regenerated lenses in rabbits. Upper panel, slit-lamp photography of a regenerated lens at different time points after surgery. Lower panel, schematic diagram of slit-lamp photographs in the upper panel. At day 1 after surgery, the capsular opening was clearly seen in the peripheral anterior capsule, and the area of LEC loss during surgery is indicated. At 7 weeks after surgery, loss of LECs led to adhesion between the anterior and the posterior capsule and inhibition of lens regeneration in this area.
Extended Data Figure 8 Human lens regeneration.
a, A clinical trial consort flowchart. b, Comparison of visual acuity mean response profiles in two groups. A non-parallel pattern of mean responses between two groups was observed largely due to the vision loss at 3 months before laser surgery in the control group (left panel), whereas a parallel pattern of mean responses between two groups was observed using time points including 3 months after laser surgery (right panel); n = 25 control, n = 12 experimental. Data are shown as mean ± s.d. c, Lens thickness increased after surgery. Pentacam showed that 3 months after surgery, the regenerating lens tissue grew from the periphery of the capsular bag to the centre. The sealed capsular bag was only partially filled, appearing spindle-shaped on cross-sectional scan. The fundus was clearly visible on ophthalmoscopy. Arrowheads indicate the regenerated lens structure. d, Six months after surgery, the capsular bag was filled with regenerated lens tissue and appeared biconvex on cross-sectional scan by Pentacam. The anterior–posterior capsular adhesion disappeared. The fundus could be seen clearly using an ophthalmoscope with an 18-dioptre lens. e, Minimally invasive capsulorhexis preserved LECs for lens regeneration in human infants. Top panel, slit-lamp exam demonstrating human infant’s eye visual axis transparency 6 months after minimally invasive surgery compared to baseline (before cataract surgery). Bottom panel, retro-illumination demonstrating the reduced size of the capsulorhexis (white arrowheads).
Supplementary information
Supplementary Information
This file contains Supplementary Figure 1, which contains original gel pictures used in Figure 2, and Supplementary Table 1, which shows the sequences of primers used for real-time PCR. (PDF 222 kb)
Rights and permissions
About this article
Cite this article
Lin, H., Ouyang, H., Zhu, J. et al. Lens regeneration using endogenous stem cells with gain of visual function. Nature 531, 323–328 (2016). https://doi.org/10.1038/nature17181
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nature17181
This article is cited by
-
Next-generation nanomaterials: advancing ocular anti-inflammatory drug therapy
Journal of Nanobiotechnology (2023)
-
Nicotinamide improves in vitro lens regeneration in a mouse capsular bag model
Stem Cell Research & Therapy (2022)
-
Malfunction of airway basal stem cells plays a crucial role in pathophysiology of tracheobronchopathia osteoplastica
Nature Communications (2022)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.