Abstract
Endothelial cells contribute to a subset of cardiac fibroblasts by undergoing endothelial-to-mesenchymal transition, but whether cardiac fibroblasts can adopt an endothelial cell fate and directly contribute to neovascularization after cardiac injury is not known. Here, using genetic fate map techniques, we demonstrate that cardiac fibroblasts rapidly adopt an endothelial-cell-like phenotype after acute ischaemic cardiac injury. Fibroblast-derived endothelial cells exhibit anatomical and functional characteristics of native endothelial cells. We show that the transcription factor p53 regulates such a switch in cardiac fibroblast fate. Loss of p53 in cardiac fibroblasts severely decreases the formation of fibroblast-derived endothelial cells, reduces post-infarct vascular density and worsens cardiac function. Conversely, stimulation of the p53 pathway in cardiac fibroblasts augments mesenchymal-to-endothelial transition, enhances vascularity and improves cardiac function. These observations demonstrate that mesenchymal-to-endothelial transition contributes to neovascularization of the injured heart and represents a potential therapeutic target for enhancing cardiac repair.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Christia, P. et al. Systematic characterization of myocardial inflammation, repair, and remodeling in a mouse model of reperfused myocardial infarction. J. Histochem. Cytochem. 61, 555–570 (2013)
Cohn, J. N., Ferrari, R. & Sharpe, N. Cardiac remodeling—concepts and clinical implications: a consensus paper from an international forum on cardiac remodeling. Behalf of an International Forum on Cardiac Remodeling. J. Am. Coll. Cardiol. 35, 569–582 (2000)
Kocher, A. A. et al. Neovascularization of ischemic myocardium by human bone-marrow-derived angioblasts prevents cardiomyocyte apoptosis, reduces remodeling and improves cardiac function. Nature Med. 7, 430–436 (2001)
Souders, C. A., Bowers, S. L. & Baudino, T. A. Cardiac fibroblast: the renaissance cell. Circ. Res. 105, 1164–1176 (2009)
Zeisberg, E. M. et al. Endothelial-to-mesenchymal transition contributes to cardiac fibrosis. Nature Med. 13, 952–961 (2007)
Chintalgattu, V., Nair, D. M. & Katwa, L. C. Cardiac myofibroblasts: a novel source of vascular endothelial growth factor (VEGF) and its receptors Flt-1 and KDR. J. Mol. Cell. Cardiol. 35, 277–286 (2003)
Zhao, L. & Eghbali-Webb, M. Release of pro- and anti-angiogenic factors by human cardiac fibroblasts: effects on DNA synthesis and protection under hypoxia in human endothelial cells. Biochim. Biophys. Acta 1538, 273–282 (2001)
Qian, L. et al. In vivo reprogramming of murine cardiac fibroblasts into induced cardiomyocytes. Nature 485, 593–598 (2012)
Song, K. et al. Heart repair by reprogramming non-myocytes with cardiac transcription factors. Nature 485, 599–604 (2012)
Duan, J. et al. Wnt1/β-catenin injury response activates the epicardium and cardiac fibroblasts to promote cardiac repair. EMBO J. 31, 429–442 (2012)
Zheng, B., Zhang, Z., Black, C. M., de Crombrugghe, B. & Denton, C. Ligand-dependent genetic recombination in fibroblasts: a potentially powerful technique for investigating gene function in fibrosis. Am. J. Pathol. 160, 1609–1617 (2002)
Liu, S., Thompson, K. & Leask, A. CCN2 expression by fibroblasts is not required for cutaneous tissue repair. Wound Repair Regen. 22, 119–124 (2014)
Madisen, L. et al. A robust and high-throughput Cre reporting and characterization system for the whole mouse brain. Nature Neurosci. 13, 133–140 (2010)
Dejana, E. Endothelial cell-cell junctions: happy together. Nature Rev. Mol. Cell Biol. 5, 261–270 (2004)
Singh, H. et al. Visualization and quantification of cardiac mitochondrial protein clusters with STED microscopy. Mitochondrion 12, 230–236 (2012)
Li, Y. et al. Direct labeling and visualization of blood vessels with lipophilic carbocyanine dye DiI. Nature Protocols 3, 1703–1708 (2008)
Urbich, C. & Dimmeler, S. Endothelial progenitor cells: characterization and role in vascular biology. Circ. Res. 95, 343–353 (2004)
Tomasek, J. J., Gabbiani, G., Hinz, B., Chaponnier, C. & Brown, R. A. Myofibroblasts and mechano-regulation of connective tissue remodelling. Nature Rev. Mol. Cell Biol. 3, 349–363 (2002)
Weber, K. T., Sun, Y., Bhattacharya, S. K., Ahokas, R. A. & Gerling, I. C. Myofibroblast-mediated mechanisms of pathological remodelling of the heart. Nature Rev. Cardiol. 10, 15–26 (2013)
Zhou, B. et al. Adult mouse epicardium modulates myocardial injury by secreting paracrine factors. J. Clin. Invest. 121, 1894–1904 (2011)
Acharya, A. et al. The bHLH transcription factor Tcf21 is required for lineage-specific EMT of cardiac fibroblast progenitors. Development 139, 2139–2149 (2012)
Lin, S. L., Kisseleva, T., Brenner, D. A. & Duffield, J. S. Pericytes and perivascular fibroblasts are the primary source of collagen-producing cells in obstructive fibrosis of the kidney. Am. J. Pathol. 173, 1617–1627 (2008)
Melo, L. G. et al. Molecular and cell-based therapies for protection, rescue, and repair of ischemic myocardium: reasons for cautious optimism. Circulation 109, 2386–2393 (2004)
Sharpless, N. E. & DePinho, R. A. p53: good cop/bad cop. Cell 110, 9–12 (2002)
Hong, H. et al. Suppression of induced pluripotent stem cell generation by the p53-p21 pathway. Nature 460, 1132–1135 (2009)
Chang, C. J. et al. p53 regulates epithelial-mesenchymal transition and stem cell properties through modulating miRNAs. Nature Cell Biol. 13, 317–323 (2011)
Hasan, N. M., Adams, G. E. & Joiner, M. C. Effect of serum starvation on expression and phosphorylation of PKC-alpha and p53 in V79 cells: implications for cell death. Int. J. Cancer 80, 400–405 (1999)
Shi, Y. et al. Starvation-induced activation of ATM/Chk2/p53 signaling sensitizes cancer cells to cisplatin. BMC Cancer 12, 571 (2012)
Komarov, P. G. et al. A chemical inhibitor of p53 that protects mice from the side effects of cancer therapy. Science 285, 1733–1737 (1999)
Marino, S., Vooijs, M., van Der Gulden, H., Jonkers, J. & Berns, A. Induction of medulloblastomas in p53-null mutant mice by somatic inactivation of Rb in the external granular layer cells of the cerebellum. Genes Dev. 14, 994–1004 (2000)
Issaeva, N. et al. Small molecule RITA binds to p53, blocks p53-HDM-2 interaction and activates p53 function in tumors. Nature Med. 10, 1321–1328 (2004)
Bruhl, T. et al. Homeobox A9 transcriptionally regulates the EphB4 receptor to modulate endothelial cell migration and tube formation. Circ. Res. 94, 743–751 (2004)
Boudreau, N., Andrews, C., Srebrow, A., Ravanpay, A. & Cheresh, D. A. Induction of the angiogenic phenotype by Hox D3. J. Cell Biol. 139, 257–264 (1997)
Fazel, S. et al. Cardioprotective c-kit+ cells are from the bone marrow and regulate the myocardial balance of angiogenic cytokines. J. Clin. Invest. 116, 1865–1877 (2006)
Economopoulou, M. et al. Histone H2AX is integral to hypoxia-driven neovascularization. Nature Med. 15, 553–558 (2009)
Bishopric, N. H. et al. Hypoxia-activated apoptosis of cardiac myocytes requires reoxygenation or a pH shift and is independent of p53. J. Clin. Invest. 104, 239–252 (1999)
Bolte, S. & Cordelieres, F. P. A guided tour into subcellular colocalization analysis in light microscopy. J. Microsc. 224, 213–232 (2006)
McDonald, J. H. & Dunn, K. W. Statistical tests for measures of colocalization in biological microscopy. J. Microsc. 252, 295–302 (2013)
Agocha, A. E. & Eghbali-Webb, M. A simple method for preparation of cultured cardiac fibroblasts from adult human ventricular tissue. Mol. Cell. Biochem. 172, 195–198 (1997)
Nagelkerke, J. F., Barto, K. P. & van Berkel, T. J. In vivo and in vitro uptake and degradation of acetylated low density lipoprotein by rat liver endothelial, Kupffer, and parenchymal cells. J. Biol. Chem. 258, 12221–12227 (1983)
Acknowledgements
We thank the Michael Hooker Confocal Microscopy and the Histology Research Core facilities at UNC, Chapel Hill. We thank the confocal and advanced light microscopy facilities in the Division of Molecular Medicine and California Nanosystems Institute at UCLA, Histology facilities at Brain Research Institute & Pathology and Laboratory Medicine, UCLA, Broad Stem Cell Research Center UCLA flow cytometry laboratories and the Vector core facility at UCLA for technical assistance. We thank K. Caron, V. Bauch, J. Taylor, C. Otey at UNC, Chapel Hill and J. Lusis at UCLA for scientific suggestions and discussion. This work was supported by grants from the National Institutes of Health (NIH R01HL102190) to A. Deb. Super-resolution studies and ChIP studies were supported by NIH grant HL088640 to E.S. and NIH grant HL105699 to T.V. E. Ubil was supported in part by a pre-doctoral grant from the American Heart Association. This work was initiated when A.D. was at the University of North Carolina, Chapel Hill and completed at the University of California, Los Angeles.
Author information
Authors and Affiliations
Contributions
E.U. and J.D. performed experiments, obtained and analysed data and did statistical analysis. I.C.L.P., Y.W. and E.S. performed super-resolution microscopy experiments. I.C.L.P., S.S. and J.H. performed flow cytometry and in vitro experiments. M.R.-G. and T.M.V. performed ChIP experiments. F.B. did western blotting. M.R. and Y.L. performed animal surgeries and echocardiograms. A.D. conceptualized the project, performed statistical analysis, supervised the work and wrote the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Extended data figures and tables
Extended Data Figure 1 Phenotypic characterization of tdTomato-labelled cells in hearts of Col1a2-CreERT:R26RtdTomato mice.
a–c, Hearts were digested to obtain a non-myocyte population and subjected to flow cytometry to determine expression of DDR2 (b) and vimentin (c). Panel a serves as a control with no primary antibody added (number in each quadrant represents fraction of total population of cells). d, e, Immunofluorescent staining on sham-injured hearts of Col1a2-CreERT:R26RtdTomato mice to determine expression of DDR2 (d) (green) and vimentin (e) (green) in tdTomato-labelled cells (red) with merged image (right; arrowheads point to tdTomato-labelled cells staining for DDR2 or vimentin). Scale bar, 10 μm. f–h, Non-myocyte cells from the heart were subjected to flow cytometry to determine expression of VECAD (f), CD31 (g) or c-Kit (h) (number in each quadrant represents fraction of total population of cells). i–k, Immunofluorescent staining for α-smooth muscle actin (i), CD68 (j) or podoplanin (k) was performed on frozen heart sections prepared from 8-week-old sham-injured Col1a2-CreERT:R26RtdTomato mice after tamoxifen injections and co-localization analysis performed to determine the number of labelled cardiac fibroblasts expressing α-smooth muscle actin (99.4% negative for α-SMA, 1,500 cells examined), CD68 (100% negative for CD68, 1,000 cells examined) or podoplanin (arrowheads). Scale bar: i–k, 10 μm. l, m, STED super-resolution microscopy demonstrating tdTomato-labelled cells (arrows) not expressing NG2 (l) (green, arrows, STED channel) or CD146 (m) (green, arrows, STED channel). Scale bar, 10 μm.
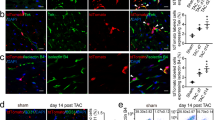
Extended Data Figure 2 Expression of VECAD in fibroblast-derived endothelial cells that take up DiO and expression of α-smooth muscle actin and VECAD in tdTomato-labelled cells.
a, Col1a2-CreERT:R26RtdTomato mice were subjected to ischaemic injury, injected with DiO 7 days after cardiac injury and then harvested. High magnification of a wall of a blood vessel in the injured region demonstrates luminal cells staining for DiO (green, arrowheads), VECAD (blue, arrowheads), tdTomato (red, arrowheads) and merged image demonstrating co-localization of all three fluorophores (filled arrowheads); open arrowhead points to VECAD+DiO+ cell that does not bear the tdTomato label. Scale bar, 10 μm. b–f, Expression of α-smooth muscle actin and VECAD in tdTomato-labelled cells. b–e, Tamoxifen-injected Col1a2-CreERT:R26RtdTomato mice underwent ischaemia reperfusion injury and hearts were harvested 3 days after injury and immunofluorescent staining performed for α-smooth muscle actin and VECAD. Section shows tdTomato-labelled cardiac fibroblasts (b), VECAD (c), α-smooth muscle actin expressing cells (d) and merged image (e) showing co-localization of fluorophores. Arrowheads show labelled cardiac fibroblasts expressing α-smooth muscle actin and arrow shows a labelled cardiac fibroblast expressing VECAD but not smooth muscle actin. Scale bar: b–e, 10 μm. f, Fraction of labelled cardiac fibroblasts that are α-smooth muscle actin+ and VECAD+ or VECAD− (mean ± s.e.m., *P < 0.05, n = 3).
Extended Data Figure 3 tdTomato expression in hearts of vehicle-injected Col1a2-CreERT:R26RtdTomato mice and immunostaining for Col1 and VECAD in tamoxifen-injected Col1a2-CreERT:R26RtdTomato mice after cardiac injury.
a–c, Oil-injected Col1a2-CreERT:R26RtdTomato mice underwent ischaemia reperfusion injury and 3 days after injury, hearts were harvested and sectioned. Area of injury (white lines) was stained with Alexa488-labelled wheat germ agglutinin (a) (WGA, stains cell membranes), rare tdTomato-expressing cells in same field (b) (arrowhead) and merged image (c) showing the presence of rare labelled cells in the injury region (arrowhead) (28 labelled cells out of 38,000 cells counted (0.07%), n = 3 mice). Scale bar: 100 µm. d, e, Col1a2-Cre:R26RtdTomato mice (injected with tamoxifen as described in text) were subjected to ischaemic cardiac injury and hearts harvested 3 days post injury and stained for Col1 and VECAD. d, Region of injury demonstrating a VECAD-expressing cell (blue, arrow) staining positive for Col1 (green) but negative for the tdTomato label (merged arrow). Arrowheads in merged panel show tdTomato-labelled cells expressing VECAD but not Col1. Scale bar, 10 μm. e, tdTomato-labelled cells expressing VECAD (arrowheads) that do not stain for Col1 (green) with merged image showing tdTomato+VECAD+ cells not staining with the Col1 antibody. Out of 225 cells counted (n = 3 mice), we did not observe a single tdTomato+VECAD+ cell to stain for Col1. Conversely, not a single VECAD+Col1+ cell exhibited tdTomato fluorescence. Scale bar, 10 μm.
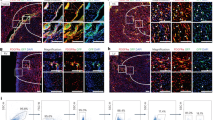
Extended Data Figure 4 VECAD and Cre immunostaining in heart sections of Col1a2-Cre:R26RtdTomato:Col1-GFP mice 3 days after injury.
a, b, Col1a2-Cre:R26RtdTomato:Col1-GFP mice were subjected to ischaemic cardiac injury and hearts harvested at 3 days post injury and stained for VECAD. a, tdTomato-labelled cells (red, arrowheads) expressing VECAD (blue, arrowheads) but not GFP (green), with merged image demonstrating co-localization of tdTomato and VECAD but not GFP (arrowheads). Scale bar, 10 μm. b, High magnification of a blood vessel (asterisk) outlined by VECAD staining (blue) demonstrating rare cell that co-localizes all three fluorophores (tdTomato+VECAD+GFP+, white, arrowhead). Arrows point to tdTomato-positive cells expressing VECAD but not GFP. Scale bar, 10 μm. c–f, Immunostaining for Cre protein on hearts of Col1a2-Cre:R26RtdTomato:Col1-GFP mice harvested 3 days following ischaemic injury to detect Cre expression in the nucleus of tdTomato-labelled cells expressing VECAD. tdTomato-labelled cells (c) in area of injury (arrowheads) expressing VECAD (d) (arrowheads), merged image showing co-localization of fluorophores (e) (arrowheads) and nuclei stained for DAPI and Cre (f) demonstrating absence of any detectable nuclear Cre protein. Scale bar, 10 μm. g–i, Positive control demonstrating section of heart of Wt-1Cre transgenic mouse heart 3 days after injury with region of injury stained for DAPI (g), Cre (h) (red) and merged image (i) demonstrating numerous cells in the injury region expressing nuclear Cre (arrowheads). Scale bar, 10 μm. j–m, Cre immunostaining in tdTomato-labelled cells expressing GFP. Area in region of injury with nuclei stained for DAPI (j), tdTomato expression (k) (arrowhead), GFP expression (arrowhead) (l) and merged image (DAPI, Cre and GFP) (m) showing Cre staining (red channel) localized to the cytoplasm of GFP-expressing cell (arrowhead). Scale bar, 10 μm.
Extended Data Figure 5 Flow cytometry for endothelial progenitor markers on non-myocyte cells harvested from uninjured hearts of Col1a2-CreERT:R26RtdTomato mice and bone marrow cells isolated from the same animal.
a, b, Hearts of mice were digested, myocytes discarded and the entire non-myocyte population without any further selection was subjected to flow cytometry. Expression of tdTomato and CD45 and Flk-1 (APC fluorophore) (a) and CD133, CD34 and combined expression of CD34 and Flk-1 in non-myocyte population (b). c–f, Bone marrow cells were isolated from Col1a2-CreERT:R26RtdTomato mice and without further culture subjected to flow cytometry. Expression of tdTomato and CD45 (c), Flk-1 (d), CD133 (e), and CD34 and combined expression of Flk1 and CD34 (f) in bone marrow cells. g, Expression of tdTomato in bone-marrow-derived mesenchymal stem-cell colonies (black arrowhead points to rare tdTomato-positive cell; white arrowheads point to mesenchymal stem cells). Scale bar, 50 μm.
Extended Data Figure 6 Mesenchymal–endothelial transition in FSP1-Cre:R26RtdTomato mice.
a, b, FSP1-Cre:R26RtdTomato mice were subjected to sham (a) or ischaemia-reperfusion (b) cardiac injury. Hearts were harvested 3 days after injury and stained for endothelial marker VECAD or isolectin. Injury region demonstrated tdTomato-labelled cells expressing VECAD or isolectin (arrowheads, n = 4). Scale bar, 10 μm. c, Quantification of labelled fibroblasts that express VECAD or isolectin in sham-injured animals and in the injury border zone (mean ± s.e.m., *P < 0.01, n = 4).
Extended Data Figure 7 Effect of serum starvation on p53 levels and effects of pifithrin-α and RITA on tube formation of serum-fed cardiac fibroblasts.
a, Western blot for p53 in cardiac fibroblasts subjected to serum starvation for 24, 48 and 72 h (representative sample from n = 3). b, Densitometric quantification of western blot (mean ± s.e.m., *P < 0.05 compared to cells in 10% serum). c, Effect on tube formation after adding pifithrin-α or RITA to cardiac fibroblasts grown in 10% serum. Scale bar, 250 μm. d, Quantification of tube formation (mean ± s.e.m., *P < 0.05, n = 3).
Extended Data Figure 8 Effect of adding TGF-β to serum-starved cardiac fibroblasts, or adding TGF-β, serum or pifithrin-α on tubes that have already formed.
a, b, Tube formation of cardiac fibroblasts subjected to serum starvation in the absence (a) or presence (b) of TGF-β. (TGF-β was added at the onset of serum starvation.) Scale bar, 250 μm. c–f, Effect of adding TGF-β or serum to tubes that had already formed. c, e, Twenty-four hours after serum starvation (after tubes had already formed), PBS was added to tubes shown in c and e and photographs taken after another 24 h. d, f, After tubes had already formed (24 h of serum starvation), TGF-β (d) or serum (f) was added and photographs taken after another 24 h (note clumping of cells and regression of tubes in d and f). Scale bar: c–f, 250 μm. g, Effect of adding TGF-β or serum to tubes that had already formed, expressed as a percentage decrease in tube length. h–n, Effect of adding pifithrin-α to serum-starved cardiac fibroblasts that had already formed tubes. h, k, Tube formation in cardiac fibroblasts serum starved for 24 h. Scale bar, 250 μm. i, j, PBS was then added to cardiac fibroblasts shown in h and photographs were taken after another 24 h (i) or 48 h (j) of serum starvation. Scale bar, 250 μm. l, m, Pifithrin-α was added to cardiac fibroblasts shown in k and photographs were taken after another 24 h (l) or 48 h (m) of serum starvation in the presence of pifithrin-α. Scale bar, 250 μm. n, Tube length in j and m was expressed as a per cent change from their respective control (h and k) (mean ± s.e.m., *P < 0.05 compared to control, n = 3).
Extended Data Figure 9 RITA decreases inflammatory infiltrate after cardiac injury, does not increase apoptosis in myocytes and does not enhance mesenchymal–endothelial transition in Col1a2-CreERT:R26RtdTomato:p53CKO mice.
a–d, Sections of hearts harvested at 3 days after cardiac injury were stained for the monocyte/macrophage marker CD68 (green, arrowheads) in Col1a2-CreERT:R26RtdTomato (a), Col1a2-CreERT:R26RtdTomato:p53CKO (b) and RITA-injected Col1a2-CreERT:R26RtdTomato (c) mice. Scale bar, 10 μm. d, Quantification of the number of CD68 cells per high-power field in the injury region (mean ± s.e.m., *P < 0.05 versus Col1a2-CreERT:R26RtdTomato, **P < 0.05 versus Col1a2-CreERT:R26RtdTomato, n = 3). e–g, p53 expression in myocytes after cardiac injury and effect of RITA on apoptosis in injury region. e, f, Col1a2-CreERT:R26RtdTomato mice were subjected to ischaemic cardiac injury, hearts harvested at 3 days and sections stained for p53 and the cardiomyocyte marker troponin. e, p53 (green, arrowheads) staining is observed in tdTomato-expressing cells (red, arrowheads) but not in cardiomyocytes (blue); merged image shows arrowheads pointing to tdTomato-labelled cells expressing p53. Scale bar, 10 μm. f, Higher magnification in injury region demonstrating tdTomato cells (arrowheads) expressing p53 (merged, yellow, arrowheads); p53 staining is not visible in cardiomyocytes (blue). Scale bar, 10 μm. g, TUNEL staining and quantification to determine p53+ apoptotic cells after RITA injection (arrowheads point to p53+TUNEL+ cells in Col1a2-CreERT:R26RtdTomato mice (left panel) and RITA-injected Col1a2-CreERT:R26RtdTomato mice (right panel); inset shows p53+TUNEL+ cell in higher magnification (data shown as mean ± s.e.m., ns, not significant, n = 3). Hearts in both cases were examined 3 days after injury. Scale bar, 10 μm. h, i, Effect of RITA on mesenchymal–endothelial transition in Col1a2-CreERT:R26RtdTomato:p53CKO mice after cardiac injury. h, tdTomato-labelled cardiac fibroblasts expressing VECAD in Col1a2-CreERT:R26RtdTomato mice treated with RITA or vehicle and Col1a2-CreERT:R26RtdTomato:p53CKO mice treated with RITA or vehicle. Scale bar, 10 μm. i, Quantification of the percentage of labelled fibroblasts undergoing mesenchymal–endothelial transition for each treatment group (mean ± s.e.m., *P < 0.05, n.s., not significant, n = 4 mice per group).
Extended Data Figure 10 γH2AX expression in cells expressing p53 after ischaemic cardiac injury.
Col1a2-CreERT:R26RtdTomato mice were subjected to ischaemic cardiac injury and immunostaining performed for γH2AX and p53. a, Immunostaining for p53 (green), γH2AX (red) and DAPI (blue) in region of injury (arrowheads point to nuclei co-expressing γH2AX and p53). Scale bar, 10 μm. b, Immunostaining for p53 (green), γH2AX (blue) and tdTomato (red) to determine co-expression of p53 and γH2AX in tdTomato-labelled cells. Arrowheads point to tdTomato-positive cells co-expressing γH2AX and p53. Scale bar, 10 μm. c, Quantification of the fraction of tdTomato+p53+ cells expressing γH2AX (mean ± s.e.m., *P < 0.01, n = 3).
Rights and permissions
About this article
Cite this article
Ubil, E., Duan, J., Pillai, I. et al. Mesenchymal–endothelial transition contributes to cardiac neovascularization. Nature 514, 585–590 (2014). https://doi.org/10.1038/nature13839
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nature13839
This article is cited by
-
miR-92a-3p promotes pulmonary fibrosis progression by regulating KLF2-mediated endothelial-to-mesenchymal transition
Cytotechnology (2024)
-
Investigation of SAMD1 ablation in mice
Scientific Reports (2023)
-
Oct4 cooperates with c-Myc to improve mesenchymal-to-endothelial transition and myocardial repair of cardiac-resident mesenchymal stem cells
Stem Cell Research & Therapy (2022)
-
Loss of KDM5B ameliorates pathological cardiac fibrosis and dysfunction by epigenetically enhancing ATF3 expression
Experimental & Molecular Medicine (2022)
-
Dusp6 deficiency attenuates neutrophil-mediated cardiac damage in the acute inflammatory phase of myocardial infarction
Nature Communications (2022)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.