Abstract
Inflammation in HIV infection is predictive of non-AIDS morbidity and death1, higher set point plasma virus load2 and virus acquisition3; thus, therapeutic agents are in development to reduce its causes and consequences. However, inflammation may simultaneously confer both detrimental and beneficial effects. This dichotomy is particularly applicable to type I interferons (IFN-I) which, while contributing to innate control of infection4,5,6,7,8,9,10, also provide target cells for the virus during acute infection, impair CD4 T-cell recovery, and are associated with disease progression6,7,11,12,13,14,15,16,17,18,19. Here we manipulated IFN-I signalling in rhesus macaques (Macaca mulatta) during simian immunodeficiency virus (SIV) transmission and acute infection with two complementary in vivo interventions. We show that blockade of the IFN-I receptor caused reduced antiviral gene expression, increased SIV reservoir size and accelerated CD4 T-cell depletion with progression to AIDS despite decreased T-cell activation. In contrast, IFN-α2a administration initially upregulated expression of antiviral genes and prevented systemic infection. However, continued IFN-α2a treatment induced IFN-I desensitization and decreased antiviral gene expression, enabling infection with increased SIV reservoir size and accelerated CD4 T-cell loss. Thus, the timing of IFN-induced innate responses in acute SIV infection profoundly affects overall disease course and outweighs the detrimental consequences of increased immune activation. Yet, the clinical consequences of manipulation of IFN signalling are difficult to predict in vivo and therapeutic interventions in human studies should be approached with caution.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
Accession codes
Primary accessions
Gene Expression Omnibus
Data deposits
Gene expression data are available at the Gene Expression Omnibus under accession codes GSM1298835 through GSM1299037.
References
Hunt, P. W. et al. Gut epithelial barrier dysfunction and innate immune activation predict mortality in treated HIV infection. J. Infect. Dis. http://dx.doi.org/10.1093/infdis/jiu238 (21 April 2014)
Roberts, L. et al. Genital tract inflammation during early HIV-1 infection predicts higher plasma viral load set point in women. J. Infect. Dis. 205, 194–203 (2012)
Naranbhai, V. et al. Innate immune activation enhances HIV acquisition in women, diminishing the effectiveness of tenofovir microbicide gel. J. Infect. Dis. 206, 993–1001 (2012)
Schoggins, J. W. et al. A diverse range of gene products are effectors of the type I interferon antiviral response. Nature 472, 481–485 (2011)
Schoggins, J. W. et al. Pan-viral specificity of IFN-induced genes reveals new roles for cGAS in innate immunity. Nature 505, 691–695 (2013)
Gonzalez-Navajas, J. M., Lee, J., David, M. & Raz, E. Immunomodulatory functions of type I interferons. Nature Rev. Immunol. 12, 125–135 (2012)
Lane, H. C. et al. Anti-retroviral effects of interferon-α in AIDS-associated Kaposi’s sarcoma. Lancet 332, 1218–1222 (1988)
Manion, M. et al. Interferon-alpha administration enhances CD8+ T cell activation in HIV infection. PLoS ONE 7, e30306 (2012)
Azzoni, L. et al. Pegylated Interferon alfa-2a monotherapy results in suppression of HIV type 1 replication and decreased cell-associated HIV DNA integration. J. Infect. Dis. 207, 213–222 (2013)
Feld, J. J. & Hoofnagle, J. H. Mechanism of action of interferon and ribavirin in treatment of hepatitis C. Nature 436, 967–972 (2005)
Stacey, A. R. et al. Induction of a striking systemic cytokine cascade prior to peak viremia in acute human immunodeficiency virus type 1 infection, in contrast to more modest and delayed responses in acute hepatitis B and C virus infections. J. Virol. 83, 3719–3733 (2009)
Fraietta, J. A. et al. Type I interferon upregulates Bak and contributes to T cell loss during human immunodeficiency virus (HIV) infection. PLoS Pathog. 9, e1003658 (2013)
Abel, K. et al. The relationship between simian immunodeficiency virus RNA levels and the mRNA levels of α/β interferons (IFN-alpha/beta) and IFN-α/β-inducible Mx in lymphoid tissues of rhesus macaques during acute and chronic infection. J. Virol. 76, 8433–8445 (2002)
Teijaro, J. R. et al. Persistent LCMV infection is controlled by blockade of type I interferon signaling. Science 340, 207–211 (2013)
Wilson, E. B. et al. Blockade of chronic type I interferon signaling to control persistent LCMV infection. Science 340, 202–207 (2013)
Li, Q. et al. Glycerol monolaurate prevents mucosal SIV transmission. Nature 458, 1034–1038 (2009)
Haas, D. W. et al. A randomized trial of interferon alpha therapy for HIV type 1 infection. AIDS Res. Hum. Retroviruses 16, 183–190 (2000)
Fernandez, S. et al. CD4+ T-cell deficiency in HIV patients responding to antiretroviral therapy is associated with increased expression of interferon-stimulated genes in CD4+ T cells. J. Infect. Dis. 204, 1927–1935 (2011)
Levin, D. et al. Multifaceted activities of type I interferon are revealed by a receptor antagonist. Sci. Signal. 7, ra50 (2014)
Goujon, C. et al. Human MX2 is an interferon-induced post-entry inhibitor of HIV-1 infection. Nature 502, 559–562 (2013)
Honda, K. et al. IRF-7 is the master regulator of type-I interferon-dependent immune responses. Nature 434, 772–777 (2005)
Barouch, D. H. et al. Vaccine protection against acquisition of neutralization-resistant SIV challenges in rhesus monkeys. Nature 482, 89–93 (2012)
Carrington, M. & Alter, G. Innate immune control of HIV. Cold Spring Harb. Perspect. Med. 2, a007070 (2012)
Asmuth, D. M. et al. Pegylated interferon-α 2a treatment of chronic SIV-infected macaques. J. Med. Primatol. 37, 26–30 (2008)
Litvak, V. et al. A FOXO3–IRF7 gene regulatory circuit limits inflammatory sequelae of antiviral responses. Nature 490, 421–425 (2012)
Schellekens, H. et al. The effect of recombinant human interferon αB/D compared to interferon α2b on SIV infection in rhesus macaques. Antiviral Res. 32, 1–8 (1996)
Waggoner, S. N., Daniels, K. A. & Welsh, R. M. Therapeutic depletion of natural killer cells controls persistent infection. J. Virol. 88, 1953–1960 (2014)
Parrish, N. F. et al. Phenotypic properties of transmitted founder HIV-1. Proc. Natl Acad. Sci. USA 110, 6626–6633 (2013)
Fenton-May, A. E. et al. Relative resistance of HIV-1 founder viruses to control by interferon-alpha. Retrovirology 10, 146 (2013)
McElrath, M. J. et al. Comprehensive assessment of HIV target cells in the distal human gut suggests increasing HIV susceptibility toward the anus. J. Acquir. Immune Defic. Syndr. 63, 263–271 (2013)
Vanderford, T. H. et al. Treatment of SIV-infected sooty mangabeys with a type-I IFN agonist results in decreased virus replication without inducing hyperimmune activation. Blood 119, 5750–5757 (2012)
Dobin, A. et al. STAR: ultrafast universal RNA-seq aligner. Bioinformatics 29, 15–21 (2013)
Trapnell, C. et al. Differential analysis of gene regulation at transcript resolution with RNA-seq. Nature Biotechnol. 31, 46–53 (2013)
Brenchley, J. M. et al. Differential infection patterns of CD4+ T cells and lymphoid tissue viral burden distinguish progressive and nonprogressive lentiviral infections. Blood 120, 4172–4181 (2012)
Acknowledgements
We would like to acknowledge A. Zimin for his work in creating the MuSuRCA rhesus assembly, C. Miller for the gift of 6 rhesus macaques and Y. Peleg and S. Albeck at the Israel Structure Proteomic Center and G. Jona from Weizmann Institute Biological services for helping with protein production and purification; A. Roque and N. Haining for initial work on the pilot study; N. Modi, D. Ambrozak, R. Koup, M. Ghosh, I. Srivastava, R. Schwartz, F. Villinger, K. Zoon, J. Bekisz, K. Ghneim, A. Filali, R. Sekaly, L. Mach and L. Shen for their assistance on the current project; and A. Somasunderam for additional support. This project was supported by NIH Intramural Funding, federal funds from NCI/NIH Contract HHSN261200800001E, NIH R24 RR017444, NIH AI-076174, I-CORE Program of the Planning and Budgeting Committee and the Israel Science Foundation grant No. 1775/12.
Author information
Authors and Affiliations
Contributions
N.G.S. designed and coordinated the study, developed and performed experiments, interpreted the data and prepared the manuscript. S.E.B. analysed and interpreted the sequencing data, generated figures and contributed to manuscript preparation. J.D.E. contributed to study design and developed and performed in situ hybridization and immunohistochemistry assays. R.T.R.Z. processed samples, performed flow cytometry and analysis, performed qRT–PCR and generated the sequencing libraries. G.K.T. analysed and interpreted the sequencing data and generated figures. E.B. developed the library generation protocol and supervised library generation. D.L. and G.Y. synthesized the IFN-1ant. S.W. generated sequencing libraries and assisted in analysis of the sequencing data. K.N.M. assisted with sample processing, performed flow cytometry assays, and assessed plasma for neutralizing activity. G.Q.d.P. evaluated circulating SIV for IFN resistance. B.J.H. designed, performed and analysed qRT–PCR assays. J.K.T. processed samples and performed ELISAs. E.R. assisted with sample processing and performed flow cytometry assays. S.D. assisted with sequencing analysis. E.C. assisted with sample processing and performed flow cytometry assays. J.P.T. performed SIV inoculations and coordinated the study at Bioqual. G.Si. established the Non-Human Primate Sequencing Core and facilitated sequencing analysis and contributed to data interpretation. M.N. assisted with statistical analyses. R.B.N. generated the MuSuRCA Macaca mulatta assembly. B.F.K. sequenced the transmitted/founder variants. S.R. contributed to study design and followed the rhesus macaques clinically. J.A.L. contributed to IFN-1ant design and assisted with analysis. J.D.L. contributed to study design, assessment for IFN-resistant viruses and manuscript preparation. G.Sc. contributed to study design, IFN-1ant design and production and assisted with analysis. D.C.D. designed and supervised the study, interpreted the data and prepared the manuscript.
Corresponding author
Ethics declarations
Competing interests
The type I interferon receptor antagonist used in this study and related type I interferon antagonists are covered in the Patent Application PCT/US2009/056366 held by J.A.L. and G.Sc.
Extended data figures and tables
Extended Data Figure 1 Dose escalation study for IFN-1ant and experimental schema.
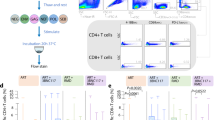
a–d, Effects of three times weekly IFN-1ant dosing on the frequency of CD4 T cells (a), CCR5+ CD4 T cells (b), CCR5+ CD8 T cells (c) and Ki67+ CD8 T cells (d) in 2 rhesus macaques. Dose was 50 μg in week 1, 200 μg in week 2, 500 μg in week 3 and 800 μg in week 4. Vertical dotted lines indicate the days a new dose was started. Black lines connect time points 4 days after the first dose. Grey shading indicates treatment period. e, Six macaques received 4 weeks of IFN-1ant intramuscularly starting at day 0 and were challenged intrarectally with 1 ml of a 1:25 dilution of SIVMAC251 (stock concentration 3 × 108 SIV RNA copies ml−1) at day 0 and followed until developing end-stage AIDS. Nine macaques were treated with 4 weeks of placebo saline intramuscularly starting at day 0 and challenged intrarectally with SIVMAC251 at day 0 and followed. Six macaques were injected weekly with IFN-α2a starting 1 week before the first challenge and through 4 w.p.i. Macaques required 2, 3 or 5 challenges to acquire systemic infection. Thus, macaques received 6, 7 or 9 doses of IFN-α2a. Macaques were necropsied at 12 w.p.i. per protocol.
Extended Data Figure 2 Effects of IFN-1ant on IFN-stimulated genes and virus burden.
a, b, MX1 (a) and OAS2 (b) expression by qRT–PCR during acute SIV infection in IFN-1ant (red, n = 6) and placebo (blue, n = 9) macaques. P values were calculated by Mann–Whitney U test. c, ISGs in PBMCs in IFN-1ant and placebo macaques. P values represent the comparison between IFN-1ant (n = 6) and placebo (n = 9) macaque FPKMs at 7 d.p.i. d, e, SAMHD1 (d) and APOBEC3G (e) expression in the lymph nodes in IFN-1ant (n = 6) and placebo (n = 9) macaques. P values were calculated by Mann–Whitney U test. f, g, Plasma SIV RNA levels at 12 w.p.i. (f) or at peak (g) stratified by the day that MX1 or OAS2 expression peaked in PBMCs in IFN-1ant (n = 6) and placebo (n = 9) macaques. VL, viral load. P values were calculated by Mann–Whitney U test. h, SIV gag levels in PBMCs stratified by the day that MX1 or OAS2 expression peaked in PBMCs in IFN-1ant (n = 6) and placebo (n = 6) macaques. P values were calculated by Mann–Whitney U test. For all panels, IFN-1ant-treated macaques are represented in red, placebo-treated macaques in blue.
Extended Data Figure 3 Effects of IFN-1ant on CD4 T cells and on immune activation.
a, b, CD4/CD8 T-cell ratio in peripheral blood (a) and lymph node (LN) (b) in IFN-1ant (Ant, n = 6) and placebo (Plac, n = 9) macaques. Shading indicates treatment period. Error bars indicate range. Red vertical line indicates day 0 of systemic SIV infection. For all panels, horizontal bars indicate median values, and P values at different time points within treatment groups were calculated by Wilcoxon matched pairs signed rank test and between groups by Mann–Whitney U test. c–f, T-cell activation in lymph nodes (c–f) in CD4 (c, d) and CD8 (e, f) T cells as represented by the frequency of Ki67+ (c, e) or HLA-DR+ (d, f) cells in IFN-1ant (n = 6) and placebo (n = 9) macaques. g, Frequency of circulating CD16+ or CD56+CD3−CD14− NK cells in IFN-1ant (n = 6) and placebo (n = 9) macaques. h, Frequency of circulating CD16+ NK cells in IFN-1ant (n = 6) and placebo (n = 9) macaques. i, Frequency of circulating CD56+ NK cells in IFN-1ant (n = 6) and placebo (n = 9) macaques. For all panels, IFN-1ant-treated macaques are represented in red, placebo-treated macaques in blue.
Extended Data Figure 4 IFN-1ant alters innate and adaptive immune signalling.
a, Selected pathways significantly affected by IFN-I blockade. P values were calculated by Fisher’s exact test with the Benjamini–Hochberg multiple testing correction. b, Expression of genes involved in pattern recognition receptor signalling of IFN-1ant-treated macaques (n = 6) compared to placebo (n = 9) at 7 d.p.i. Upregulation compared to pre-infection is represented by red, no change by white, downregulation by blue. P values represent the comparison between IFN-1ant and placebo macaques at 7 d.p.i. c, Selected genes in pattern recognition receptor signalling pathways. Upregulation at 7 d.p.i. is represented by red, downregulation by green.
Extended Data Figure 5 Effects of IFN-1ant on T-cell function and phenotype.
a–e, SIV-specific responses in peripheral blood at 4 and >12 w.p.i. in IFN-1ant (Ant, n = 6) and placebo (Plac, n = 6) macaques by frequency of IFN-γ+ (a), TNF+ (b), perforin+ (c), granzyme B+ (d) and CD107+ (e) CD8 T cells. T-cell exhaustion in peripheral blood and lymph nodes (LN) at >16 w.p.i. based on frequency of PD-1+ CD4 (f) and CD8 (h) T cells and ICOS+ (g) CD8 T cells. For all panels, P values at different time points within treatment groups were calculated by Wilcoxon matched pairs signed rank test and between groups by Mann–Whitney U test. IFN-1ant-treated macaques are represented in red, placebo-treated macaques in blue.
Extended Data Figure 6 IFN-α2a treatment transiently induces ISGs and subsequently induces the IFN-repressor FOXO3a but does not induce neutralizing anti-IFN antibodies.
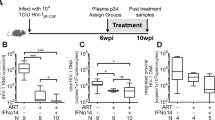
a–d, MX1 (a, c) and OAS2 (b, d) expression during the duration of IFN-α2a treatment in the IFN-α2a group alone (a, b) and during infection in the IFN-α2a (n = 6) and placebo (n = 9) groups (c, d). P values were calculated by Wilcoxon matched pairs signed rank test. e, Percentage of in vitro IFN antiviral activity inhibited by plasma from IFN-α2a (n = 6) and placebo (n = 3) macaques. f, Expression of FOXO3a and FOXO3a-bound genes in SIV-uninfected macaques (n = 3) treated with 21 days of IFN-α2a. Large circles indicate statistically significant (P<0.05) changes from pre-IFN-α2a treatment calculated by Wilcoxon matched pairs signed rank test. Small circles indicate no statistically significant change from pre-IFN-α2a treatment. g, Expression of IFN-α-regulatory genes in IFN-α2a (n = 6) and placebo (n = 9) macaques. P values represent the comparison between FPKMs of IFN-α2a (n = 6) and placebo (n = 9) macaques at 7 d.p.i. h, Expression of FOXO3a-bound genes in IFN-α2a (green, n = 6) and placebo (blue, n = 9) macaques at 7 d.p.i.
Extended Data Figure 7 Effects of IFN-α2a on IFN-stimulated and antiviral genes.
a, ISGs in PBMCs in IFN-α2a (n = 6) and placebo (n = 9) macaques. Red indicates upregulation, yellow indicates no change and blue indicates downregulation relative to pre-infection. b, Expression of ISGs in macaques treated with IFN-α2a (n = 6) or placebo (n = 9). P values indicate differentially expressed genes at 10 d.p.i. c–h, Expression of TRIM22 (c, d), MX2 (e, f) and IRF7 (g, h) in SIV-uninfected macaques (n = 3) treated with weekly IFN-α2a for 3 weeks in PBMCs (c, e, g) and lymph nodes and rectum (d, f, h). Day 0 reflects baseline. Numbers indicate days since first IFN-α2a administration. Error bars indicate range. P values were calculated by Wilcoxon matched pairs signed rank test.
Extended Data Figure 8 Effects of IFN-α2a on SIV control.
a, Number of transmitted/founder (T/F) variants in placebo (n = 9), IFN-1ant (n = 6) and IFN-α2a (n = 6) macaques. P value was calculated by Mann–Whitney U test. b, Antiviral protein production in lymph nodes (LN) by immunohistochemistry at 4 w.p.i. in IFN-α2a (n = 6) and placebo (n = 6) macaques. P value was calculated by Mann–Whitney U test. c, CD56+ NK-cell frequency on the day of challenge stratified by whether the macaque resisted or was susceptible to systemic infection that day. Each IFN-α2a macaque (n = 6) is indicated by a different colour. Circles indicate that the macaque was resistant to infection with the next challenge and triangles indicate that the macaque was susceptible to infection with the next challenge. P value was calculated by Mann–Whitney U test. d, Correlation between the number of challenges required to achieve systemic infection and rectal CD16+ NK-cell frequency in each macaque (n = 6) at 4 w.p.i. r indicates the Spearman’s rank correlation coefficient. P value indicates the significance of the correlation. e, Plasma SIV RNA levels in macaques treated with IFN-α2a (n = 6) or placebo (n = 9) saline. Shading reflects treatment period. Red vertical line indicates day 0 of systemic SIV infection. f–i, Frequency of IFN-γ+ (f), TNF+ (g), granzyme B+ (h) and perforin+ (i) CD8 T cells at 4 and ≥12 w.p.i. in IFN-α2a (n = 6) and placebo (n = 6) macaques. j, Frequency of circulating CD16+CD56− NK cells in IFN-α2a (n = 6) and placebo (n = 9) macaques. P values at different time points within treatment groups were calculated by Wilcoxon matched pairs signed rank test and between groups by Mann–Whitney U test.
Extended Data Figure 9 Effects of IFN-α2a on T-cell activation.
a–h, Frequency of peripheral blood (a–d) and lymph node (LN) (e–h) CD4 (a, c, e, g) and CD8 (b, d, f, h) memory T cells expressing HLA-DR (a, b, e, f) or Ki67 (c, d, g, h) in IFN-α2a (IFN, n = 6) and placebo (Plac, n = 9) macaques. Shading indicates treatment period. Error bars indicate range. a–d, Red vertical line indicates day 0 of systemic SIV infection. P values represent the comparison between groups of the AUC (0-4 w.p.i.). e–h, Horizontal bars indicate median values. P values were calculated by Mann–Whitney U test.
Extended Data Figure 10 Effects of IFN-α2a on gene expression.
a, Selected pathways significantly affected by IFN-α2a treatment. P values were calculated by Fisher’s exact test with the Benjamini–Hochberg multiple testing correction. b, Expression of genes downstream of IL-6 signalling. Upregulation relative to before IFN-α2a or placebo treatment and SIV infection is represented by red, no change by white, downregulation by blue. P values represent the comparison between IFN-α2a (n = 6) and placebo (n = 9) macaques at 7 d.p.i. c, Selected genes in apoptosis signalling pathways. Significant upregulation at 7 d.p.i. is represented by red, downregulation by green.
Supplementary information
Supplementary Information
This file contains Supplementary Results and Supplementary Figure 1. (PDF 879 kb)
Rights and permissions
About this article
Cite this article
Sandler, N., Bosinger, S., Estes, J. et al. Type I interferon responses in rhesus macaques prevent SIV infection and slow disease progression. Nature 511, 601–605 (2014). https://doi.org/10.1038/nature13554
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nature13554
This article is cited by
-
Evolution of enhanced innate immune suppression by SARS-CoV-2 Omicron subvariants
Nature Microbiology (2024)
-
HIV-2/SIV Vpx antagonises NF-κB activation by targeting p65
Retrovirology (2022)
-
Innate immune regulation in HIV latency models
Retrovirology (2022)
-
Expression of type I interferon-associated genes at antiretroviral therapy interruption predicts HIV virological rebound
Scientific Reports (2022)
-
Evasion of cGAS and TRIM5 defines pandemic HIV
Nature Microbiology (2022)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.