Abstract
Inherited alleles account for most of the genetic risk for schizophrenia. However, new (de novo) mutations, in the form of large chromosomal copy number changes, occur in a small fraction of cases and disproportionally disrupt genes encoding postsynaptic proteins. Here we show that small de novo mutations, affecting one or a few nucleotides, are overrepresented among glutamatergic postsynaptic proteins comprising activity-regulated cytoskeleton-associated protein (ARC) and N-methyl-d-aspartate receptor (NMDAR) complexes. Mutations are additionally enriched in proteins that interact with these complexes to modulate synaptic strength, namely proteins regulating actin filament dynamics and those whose messenger RNAs are targets of fragile X mental retardation protein (FMRP). Genes affected by mutations in schizophrenia overlap those mutated in autism and intellectual disability, as do mutation-enriched synaptic pathways. Aligning our findings with a parallel case–control study, we demonstrate reproducible insights into aetiological mechanisms for schizophrenia and reveal pathophysiology shared with other neurodevelopmental disorders.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
Accession codes
Data deposits
Data included in this manuscript have been deposited at dbGaP under accession number phs000687.v1.p1 and is available for download at http://www.ncbi.nlm.nih.gov/projects/gap/cgi-bin/study.cgi?study_id=phs000687.v1.p1.
Change history
12 February 2014
The link in reference 15 was incorrect and has been fixed.
References
Sullivan, P. F., Daly, M. J. & O’Donovan, M. Genetic architectures of psychiatric disorders: the emerging picture and its implications. Nature Rev. Genet. 13, 537–551 (2012)
Bundy, H., Stahl, D. & MacCabe, J. H. A systematic review and meta-analysis of the fertility of patients with schizophrenia and their unaffected relatives. Acta Psychiatr. Scand. 123, 98–106 (2011)
McClellan, J. M., Susser, E. & King, M.-C. Schizophrenia: a common disease caused by multiple rare alleles. Br. J. Psychiatry 190, 194–199 (2007)
Malhotra, D. & Sebat, J. Genetics: Fish heads and human disease. Nature 485, 318–319 (2012)
Rees, E., Moskvina, V., Owen, M. J., O’Donovan, M. C. & Kirov, G. De novo rates and selection of schizophrenia-associated copy number variants. Biol. Psychiatry 70, 1109–1114 (2011)
Neale, B. M. et al. Patterns and rates of exonic de novo mutations in autism spectrum disorders. Nature 485, 242–245 (2012)
O’Roak, B. J. et al. Sporadic autism exomes reveal a highly interconnected protein network of de novo mutations. Nature 485, 246–250 (2012)
Sanders, S. J. et al. De novo mutations revealed by whole-exome sequencing are strongly associated with autism. Nature 485, 237–241 (2012)
Iossifov, I. et al. De novo gene disruptions in children on the autistic spectrum. Neuron 74, 285–299 (2012)
Rauch, A. et al. Range of genetic mutations associated with severe non-syndromic sporadic intellectual disability: an exome sequencing study. Lancet 380, 1674–1682 (2012)
de Ligt, J. et al. Diagnostic exome sequencing in persons with severe intellectual disability. N. Engl. J. Med. 367, 1921–1929 (2012)
Girard, S. L. et al. Increased exonic de novo mutation rate in individuals with schizophrenia. Nature Genet. 43, 860–863 (2011)
Xu, B. et al. De novo gene mutations highlight patterns of genetic and neural complexity in schizophrenia. Nature Genet. 44, 1365–1369 (2012)
Gulsuner, S. et al. Spatial and temporal mapping of de novo mutations in schizophrenia to a fetal prefrontal cortical network. Cell 154, 518–529 (2013)
Purcell, S. M. et al. A polygenic burden of rare disruptive mutations in schizophrenia. Nature http://dx.doi.org/10.1038/nature12975 (22 January 2014)
Kong, A. et al. Rate of de novo mutations and the importance of father’s age to disease risk. Nature 488, 471–475 (2012)
Mesholam-Gately, R. I., Giuliano, A. J., Goff, K. P. & Faraone, S. V & Seidman, L. J. Neurocognition in first-episode schizophrenia: a meta-analytic review. Neuropsychology 23, 315–336 (2009)
Glessner, J. T. et al. Strong synaptic transmission impact by copy number variations in schizophrenia. Proc. Natl Acad. Sci. USA 107, 10584–10589 (2010)
Malhotra, D. et al. High frequencies of de novo CNVs in bipolar disorder and schizophrenia. Neuron 72, 951–963 (2011)
Kirov, G. et al. De novo CNV analysis implicates specific abnormalities of postsynaptic signalling complexes in the pathogenesis of schizophrenia. Mol. Psychiatry 17, 142–153 (2012)
Darnell, J. C. et al. FMRP stalls ribosomal translocation on mRNAs linked to synaptic function and autism. Cell 146, 247–261 (2011)
Malenka, R. C. & Nicoll, R. A. NMDA-receptor-dependent synaptic plasticity: multiple forms and mechanisms. Trends Neurosci. 16, 521–527 (1993)
Bramham, C. R. et al. The Arc of synaptic memory. Exp. Brain Res. 200, 125–140 (2010)
Korb, E. & Finkbeiner, S. Arc in synaptic plasticity: from gene to behavior. Trends Neurosci. 34, 591–598 (2011)
Shepherd, J. D. & Bear, M. F. New views of Arc, a master regulator of synaptic plasticity. Nature Neurosci. 14, 279–284 (2011)
Mikuni, T. et al. Arc/Arg3.1 Is a postsynaptic mediator of activity-dependent synapse elimination in the developing cerebellum. Neuron 78, 1024–1035 (2013)
Feinberg, I. Schizophrenia: caused by a fault in programmed synaptic elimination during adolescence? J. Psychiatr. Res. 17, 319–334 (1982)
Darnell, J. C. & Klann, E. The translation of translational control by FMRP: therapeutic targets for FXS. Nature Neurosci. 16, 1530–1536 (2013)
Ashburner, M. et al. Gene ontology: tool for the unification of biology. The Gene Ontology Consortium. Nature Genet. 25 25–29 (2000)
Gilman, S. R. et al. Rare de novo variants associated with autism implicate a large functional network of genes involved in formation and function of synapses. Neuron 70, 898–907 (2011)
Golzio, C. et al. KCTD13 is a major driver of mirrored neuroanatomical phenotypes of the 16p11.2 copy number variant. Nature 485, 363–367 (2012)
Steinberg, S. et al. Common variants at VRK2 and TCF4 conferring risk of schizophrenia. Hum. Mol. Genet. 20, 4076–4081 (2011)
von Eichborn, J. et al. SynSysNet: integration of experimental data on synaptic protein-protein interactions with drug-target relations. Nucleic Acids Res. 41, D834–D840 (2013)
Aoto, J., Martinelli, D. C., Malenka, R. C., Tabuchi, K. & Südhof, T. C. Presynaptic neurexin-3 alternative splicing trans-synaptically controls postsynaptic AMPA receptor trafficking. Cell 154, 75–88 (2013)
Williams, N. M. et al. Rare chromosomal deletions and duplications in attention-deficit hyperactivity disorder: a genome-wide analysis. Lancet 376, 1401–1408 (2010)
Girirajan, S. et al. Phenotypic heterogeneity of genomic disorders and rare copy-number variants. N. Engl. J. Med. 367, 1321–1331 (2012)
Owen, M. J., O’Donovan, M. C., Thapar, A. & Craddock, N. Neurodevelopmental hypothesis of schizophrenia. Br. J. Psychiatry 198, 173–175 (2011)
Nozawa, R.-S. et al. Human POGZ modulates dissociation of HP1α from mitotic chromosome arms through Aurora B activation. Nature Cell Biol. 12, 719–727 (2010)
Buxbaum, J. D. et al. The autism sequencing consortium: large-scale, high-throughput sequencing in autism spectrum disorders. Neuron 76, 1052–1056 (2012)
Craddock, N. & Owen, M. J. The Kraepelinian dichotomy – going, going...but still not gone. Br. J. Psychiatry 196, 92–95 (2010)
Insel, T. R. Transforming diagnosis. NIMH Director’s Blog http://www.nimh.nih.gov/about/director/2013/transforming-diagnosis.shtml (29 April 2013)
Pocklington, A. J., Armstrong, J. D. & Grant, S. G. N. Organization of brain complexity–synapse proteome form and function. Brief. Funct. Genomics Proteomics 5, 66–73 (2006)
Coba, M. P. et al. TNiK is required for postsynaptic and nuclear signaling pathways and cognitive function. J. Neurosci. 32, 13987–13999 (2012)
Ruderfer, D. M. et al. A family-based study of common polygenic variation and risk of schizophrenia. Mol. Psychiatry 16, 887–888 (2011)
Acknowledgements
Work in Cardiff was supported by Medical Research Council (MRC) Centre (G0800509) and Program Grants (G0801418), the European Community’s Seventh Framework Programme (HEALTH-F2-2010-241909 (Project EU-GEI)), and NIMH (2 P50 MH066392-05A1). Work at the Icahn School of Medicine at Mount Sinai was supported by the Friedman Brain Institute, the Institute for Genomics and Multiscale Biology (including computational resources and staff expertise provided by the Department of Scientific Computing), and National Institutes of Health grants R01HG005827 (S.M.P.), R01MH099126 (S.M.P.), and R01MH071681 (P.S.). Work at the Broad Institute was funded by Fidelity Foundations, the Sylvan Herman Foundation, philanthropic gifts from K. and E. Dauten, and the Stanley Medical Research Institute. Work at the Wellcome Trust Sanger Institute was supported by The Wellcome Trust (grant numbers WT089062 and WT098051) and also by the European Commission FP7 project gEUVADIS no. 261123 (P.P.). We would like to thank M. Daly, B. Neale and K. Samocha for discussions and providing unpublished autism data. We would also like to acknowledge M. DePristo, S. Gabriel, T. J. Fennel, K. Shakir, C. Tolonen and H. Shah for their help in generating and processing the various data sets.
Author information
Authors and Affiliations
Contributions
The project was led in Cardiff by M.C.O.D. and M.J.O., in Mount Sinai by S.M.P. and P.S., at the Broad by S.A.M. and J.L.M., and at the Sanger by A.P.; H.J.W., J.L.M., K.C., J.S.J., D.D.B., M.M. and S.A.R. were responsible for sample processing and data management. M.F., H.J.W., P.G., D.M.R., D.H.K., G.K., E.R. and S.D. processed NGS data, annotated and validated mutations. L.G., N.C., I.H., S.D., H.J.W. and S.A.R. undertook validation of mutations and additional lab work. A.J.P., M.F., D.H.K., S.M.P. and P.H. co-ordinated/undertook the main bioinformatics/statistical analyses. E.R., D.M.R., E.B., P.P., E.H. and P.R. performed additional analyses. S.G.G. contributed additional insights into synaptic biology. Sample recruitment was led by G.K. and V.M.; The main findings were interpreted by M.C.O.D., M.F., M.J.O., P.H., G.K., E.M.S., S.A.M., D.H.K., A.J.P., A.P., S.M.P. and P.S. who drafted the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Extended data figures and tables
Extended Data Figure 1 Comparison of sequencing metrics for putative de novo calls and parental singletons.
a–e, Putative de novo calls (child heterozygous, both parents homozygous reference; N parent-proband trios = 623) were compared with variants observed in only a single parent (“singletons”), in terms of depth of all reads at the variant site (a), fraction of reads with the alternate allele (AB = allele balance) (b), mapping quality of the reads at the site (MQ) (c), the likelihood of the heterozygous genotype (PL = Phred-scaled likelihood) (d), and the number of other samples in the present study with a non-reference allele at that site (AAC = alternate allele count) (e). Distributions were calculated for putative de novo variants (red), or grouped by sites of putatively recurrent de novo mutations (orange) when relevant, transmitted singletons (green), and non-transmitted singletons (blue).
Extended Data Figure 2 Metrics for de novo variants across cohorts and trios.
a, Rates of recurrence of validated de novo mutations for tri-nucleotide sequences. For each of 96 possible tri-nucleotide base contexts of single-base mutations (accounting for strand symmetry by reverse complementarity), the number of observed de novo SNV is plotted (sorted by this count). Mutation counts are sub-divided into those not found in external data (red), those found in dbSNP (build 137, green), those found in controls (N = 2543) in the parallel exome sequencing study15 (cyan), and those found both in dbSNP and that study (purple). b, Comparison of on-target heterozygous SNV and indel call rate with putative de novo mutation calls. For each proband (N = 623), the number of heterozygous SNV and indel calls is compared with the number of putative de novo mutations (child heterozygous, both parents homozygous reference). Probands are coloured by sequencing centre (see Supplementary Information for differences in exome capture), and six trios are noticeable outliers from all others (marked by ‘×’) in terms of number of putative de novo mutations. c, Variation in sequencing coverage between and across trios and sequencing centres. For each trio (N = 623), the number of bases covered by 10 reads or more for each member (marked by ‘×’) and the joint coverage9 in all three members (marked by points) are plotted at corresponding horizontal points; trios are sorted in increasing order of joint coverage and coloured by sequencing centre (see Supplementary Information). The intersection of each exome capture with the RefSeq coding sequence is marked by respective dotted lines.
Extended Data Figure 3 De novo mutation counts and rates.
a, The observed distribution of number of validated RefSeq-coding (see Supplementary Information) de novo mutations found for each trio (N = 617) is compared with that expected from a Poisson distribution with a rate equal to the observed mean number of de novo mutations (λ = 1.032). b, Deleterious mutation rate inversely correlates with academic performance. Individuals were grouped according to their final school grade (3–6, corresponding to D, C, B, A in the US system, http://www.fulbright.bg/en/p-Educational-System-of-Bulgaria-18/), and the proportion of individuals with one or more de novo loss-of-function mutations is plotted. N, number of individuals in each group. See Supplementary Information for details on linear regression performed to evaluate association; note that 19 samples were removed from this analysis for missing parental age or school grade information, leaving a total of 598 trios.
Extended Data Figure 4 Enrichment of de novo SNVs, indels and CNVs in genes encoding postsynaptic complexes at glutamatergic synapses.
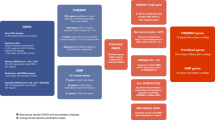
a, Number of de novo mutations (N cases = 617) in postsynaptic complexes in current study (and genes affected) are shown alongside the most conservative estimate of de novo CNV enrichment from ref. 20 (N cases studied = 662). NS, nonsynonymous, LoF, loss-of-function, PSD, postsynaptic density. The NMDAR complex gene set was derived a priori from a published proteomics data set42. To avoid investigator bias, we did not add additional members post hoc, thus omitting genes with de novo mutations and important NMDAR functions; these include GRIN2A, which encodes a subunit of the NMDA receptor itself, and AKAP9, which directly anchors protein complexes involved in signalling at NMDA receptors43. P < 0.05 are marked in bold as are genes hit by mutations in the current study and by de novo CNVs in ref. 20. b–g, 95% credible intervals (CI) for fold-enrichment statistics of de novo mutations in postsynaptic gene sets (corresponding to enrichments in a, above, and as marked) were calculated from the posterior distributions of fold-enrichment (O/E, observed to expected) statistic values for individuals in this study. Point estimates of O/E are given in Table 3, and correspond to the distribution modes here. The 95% CI is marked by red vertical lines, and a null effect size (value of 1) is marked by a grey line. Note that loss-of-function mutations in the large postsynaptic density set are not significantly enriched, and thus the corresponding CI includes an effect size of 1. All posterior distributions were calculated using dnenrich, as described in the Supplementary Information.
Supplementary information
Supplementary Information
This file contains Supplementary Text and additional references. (PDF 761 kb)
Supplementary Table 1
This file contains a list of validated coding de novo mutations discovered in subjects with schizophrenia. For each de novo mutation (single-nucleotide or insertion/deletion variant) discovered in a proband with schizophrenia in this study, listed are basic details, including genomic coordinates (hg19), reference and de novo alleles, functional impact in genes overlapped (see Supplementary Text), number of total alternate alleles called at that locus in this sample (N=623 trios, including parental genotypes), sequencing metrics for the genotypes (in the proband, father, and mother), the phased parent-of-origin when known, and family history (first-degree relatives). (XLSX 170 kb)
Supplementary Table 2
The file contains a compiled list of published de novo mutations in unaffected controls and individuals with neuropsychiatric illness. Sheet 1 shows de novo mutations analyzed alongside the schizophrenia mutations in this study, counts of individuals and RefSeq-coding mutations from published study sources, neuropsychiatric phenotype, and first author of study source are given. ASD = autism spectrum disorders, CONTROL = individual from unaffected family, ID = intellectual disability, SZ = schizophrenia, SIB = unaffected sibling of proband (from families with sequenced “quads” = father, mother, child with ASD or SZ, unaffected sibling). Sheet 2 shows that for the studies and sample sizes listed in the sheet 1, all published de novo mutations were collated and uniformly annotated. Note that only those annotated as RefSeq-coding by Plink/Seq (see Supplementary Text) are listed here. Columns are as described in Table S1. (XLSX 259 kb)
PowerPoint slides
Rights and permissions
About this article
Cite this article
Fromer, M., Pocklington, A., Kavanagh, D. et al. De novo mutations in schizophrenia implicate synaptic networks. Nature 506, 179–184 (2014). https://doi.org/10.1038/nature12929
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nature12929
This article is cited by
-
Differential functional consequences of GRIN2A mutations associated with schizophrenia and neurodevelopmental disorders
Scientific Reports (2024)
-
Morphological and transcriptomic analyses of stem cell-derived cortical neurons reveal mechanisms underlying synaptic dysfunction in schizophrenia
Genome Medicine (2023)
-
Non-synaptic function of the autism spectrum disorder-associated gene SYNGAP1 in cortical neurogenesis
Nature Neuroscience (2023)
-
Deep exome sequencing identifies enrichment of deleterious mosaic variants in neurodevelopmental disorder genes and mitochondrial tRNA regions in bipolar disorder
Molecular Psychiatry (2023)
-
Common and rare variant associations with latent traits underlying depression, bipolar disorder, and schizophrenia
Translational Psychiatry (2023)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.