Abstract
Ring chromosomes are structural aberrations commonly associated with birth defects, mental disabilities and growth retardation1,2. Rings form after fusion of the long and short arms of a chromosome, and are sometimes associated with large terminal deletions2. Owing to the severity of these large aberrations that can affect multiple contiguous genes, no possible therapeutic strategies for ring chromosome disorders have been proposed. During cell division, ring chromosomes can exhibit unstable behaviour leading to continuous production of aneuploid progeny with low viability and high cellular death rate3,4,5,6,7,8,9. The overall consequences of this chromosomal instability have been largely unexplored in experimental model systems. Here we generated human induced pluripotent stem cells (iPSCs)10,11,12 from patient fibroblasts containing ring chromosomes with large deletions and found that reprogrammed cells lost the abnormal chromosome and duplicated the wild-type homologue through the compensatory uniparental disomy (UPD) mechanism. The karyotypically normal iPSCs with isodisomy for the corrected chromosome outgrew co-existing aneuploid populations, enabling rapid and efficient isolation of patient-derived iPSCs devoid of the original chromosomal aberration. Our results suggest a fundamentally different function for cellular reprogramming as a means of ‘chromosome therapy’13 to reverse combined loss-of-function across many genes in cells with large-scale aberrations involving ring structures. In addition, our work provides an experimentally tractable human cellular system for studying mechanisms of chromosomal number control, which is of critical relevance to human development and disease.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Cote, G. B. et al. The cytogenetic and clinical implications of a ring chromosome 2. Ann. Genet. 24, 231–235 (1981)
Kosztolányi, G. Does “ring syndrome” exist? An analysis of 207 case reports on patients with a ring autosome. Hum. Genet. 75, 174–179 (1987)
McClintock, B. The production of homozygous deficient tissues with mutant characteristics by means of the aberrant mitotic behavior of ring-shaped chromosomes. Genetics 23, 315–376 (1938)
Kistenmacher, M. L. & Punnett, H. H. Comparative behavior of ring chromosomes. Am. J. Hum. Genet. 22, 304–318 (1970)
Tommerup, N. & Lothe, R. Constitutional ring chromosomes and tumor suppressor genes. J. Med. Genetik 29, 879–882 (1992)
Jobanputra, V. et al. Changes in an inherited ring (22) due to meiotic recombination? Implications for genetic counseling. Am. J. Med. Genet. A. 149A, 1310–1314 (2009)
Mantzouratau, A. et al. Meiotic and mitotic behaviour of a ring/deleted chromosome 22 in human embryos determined by preimplantation genetic diagnosis for a maternal carrier. Mol. Cytogenet. 2, 3 (2009)
Sodré, C. P. et al. Ring chromosome instability evaluation in six patients with autosomal rings. Genet. Mol. Res. 9, 134–143 (2010)
Zhang, H. Z. et al. Unique genomic structure and distinct mitotic behavior of ring chromosome 21 in two unrelated cases. Cytogenet. Genome Res. 136, 180–187 (2012)
Takahashi, K. et al. Induction of Pluripotent Stem Cells from Adult Human Fibroblasts by Defined Factors. Cell 131, 861–872 (2007)
Yu, J. et al. Induced pluripotent stem cell lines derived from human somatic cells. Science 318, 1917–1920 (2007)
Park, I. H. et al. Reprogramming of human somatic cells to pluripotency with defined factors. Nature 451, 141–146 (2008)
Jiang, J. et al. Translating dosage compensation to trisomy 21. Nature 500, 296–300 (2013)
Dobyns, W. B. et al. Miller-Dieker syndrome: lissencephaly and monosomy 17p. J. Pediatr. 102, 552–558 (1983)
Cardoso, C. et al. Refinement of a 400-kb critical region allows genotypic differentiation between isolated lissencephaly, Miller-Dieker syndrome, and other phenotypes secondary to deletions of 17p13.3. Am. J. Hum. Genet. 72, 918–930 (2003)
Wynshaw-Boris, A. et al. Lissencephaly: mechanistic insights from animal models and potential therapeutic strategies. Semin. Cell Dev. Biol. 21, 823–830 (2010)
Okita, K. et al. A more efficient method to generate integration-free human iPS cells. Nature Methods 8, 409–412 (2011)
Robinson, W. P. Mechanisms leading to uniparental disomy and their clinical consequences. Bioessays 22, 452–459 (2000)
Speevak, M. D. et al. Molecular characterization of an inherited ring (19) demonstrating ring opening. Am. J. Med. Genet. A. 121A, 141–145 (2003)
Hussein, S. M. et al. Genome damage in induced pluripotent stem cells: assessing the mechanisms and their consequences. Bioessays 35, 152–162 (2013)
Moynahan, M. E. & Jasin, M. Mitotic homologous recombination maintains genomic stability and suppresses tumorigenesis. Nature Rev. Mol. Cell Biol. 11, 196–207 (2010)
Draper, J. S. et al. Recurrent gain of chromosomes17q and 12 in cultured human embryonic stem cells. Nature Biotechnol. 22, 53–54 (2004)
Baker, D. E. et al. Adaptation to culture of human embryonic stem cells and oncogenesis in vivo. Nature Biotechnol. 25, 207–215 (2007)
Spits, C. et al. Recurrent chromosomal abnormalities in human embryonic stem cells. Nature Biotechnol. 26, 1361–1363 (2008)
Azuhata, T. et al. The inhibitor of apoptosis protein survivin is associated with high-risk behavior of neuroblastoma. J. Pediatr. Surg. 36, 1785–1791 (2001)
Damelin, M. et al. Decatenation checkpoint deficiency in stem and progenitor cells. Cancer Cell 8, 479–484 (2005)
Wilton, L. Preimplantation genetic diagnosis for aneuploidy screening in early human embryos: a review. Prenat. Diagn. 22, 512–518 (2002)
Vanneste, E. et al. Chromosome instability is common in human cleavage-stage embryos. Nature Med. 15, 577–583 (2009)
Petersen, M. B. et al. Uniparental isodisomy due to duplication of chromosome 21 occurring in somatic cells monosomic for chromosome 21. Genomics 13, 269–274 (1992)
Bartsch, O. et al. “Compensatory” uniparental disomy of chromosome 21 in two cases. J. Med. Genet. 31, 534–540 (1994)
Matsumoto, Y. et al. Induced pluripotent stem cells from patients with human fibrodysplasia ossificans progressiva show increased mineralization and cartilage formation. Orphanet J. Rare Dis. 8, 190–204 (2013)
Pfaffl, M. W. A new mathematical model for relative quantification in real-time RT-PCR. Nucleic Acids Res. 29, e45 (2001)
Hoffmann, T. J. et al. Next generation genome-wide association tool: design and coverage of a high-throughput European-optimized SNP array. Genomics 98, 79–89 (2011)
R: A language and environment for statistical computing. http://www.R-project.org. (R Foundation for Statistical Computing, 2008)
Bolstad, B. M. et al. A comparison of Normalization methods for high density oligonucleotide array data based on variance and bias. Bioinformatics 19, 185–193 (2003)
Weiss, L. A. et al. Association between microdeletion and microduplication at 16p11.2 and autism. N. Engl. J. Med. 358, 667–675 (2008)
Colella, S. et al. QuantiSNP: an objective Bayes hidden-Markov model to detect and accurately map copy number variation using SNP genotyping data. Nucleic Acids Res. 35, 2013–2025 (2007)
Meisner, L. F. & Johnson, J. A. Protocols for cytogenetic studies of human embryonic stem cells. Methods 45, 133–141 (2008)
Acknowledgements
The authors wish to thank N. Larocque and S. Fisher for access to the University of California San Francisco (UCSF) Human Embryonic Stem Cell Shared Research and Training Facility. We thank P. Tesar and Z. Nevin for comments on the manuscript; D. Srivastava and B. Conklin for advice; H. Belinson, A. Pollen and T. Nowakowski for helpful discussions; S. Hirotsune for LIS1 antibody; K. Essex for administrative support; and the Gladstone Stem Cell, Histology and Microscopy, and Bioinformatics Cores for technical support. The research was made possible by support from a NIH/NIGMS postdoctoral training grant in medical genetics (grant number GM007085-32) and a postdoctoral training fellowship from the California Institute for Regenerative Medicine (grant number TG2-01153) to M.B.; from the Uehara Memorial Foundation and USCF’s Program for Breakthrough Biomedical Research to Y.H.; from the NIAMS/NIH (K08 AR056299) and the UCSF Department of Medicine to E.C.H.; and from the NHLBI/NIH (UO1HL098179), the Leading Project of MEXT (Japan), the Funding Program for World-Leading Innovative R&D on Science and Technology (FIRST Program) of the JSPS (Japan), Grants-in-Aid for Scientific Research of the JSPS and MEXT (Japan), the Program for Promotion of Fundamental Studies in Health Sciences of NIBIO (Japan), the L. K. Whittier Foundation, and the Roddenberry Foundation to S.Y. The Gladstone Institutes received support from a National Center for Research Resources Grant RR18928. S.Y. is a member without salary of the scientific advisory boards of iPierian, iPS Academia Japan, Megakaryon Corporation and HEALIOS K.K. Japan. The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript. The contents of this publication are solely the responsibility of the authors and do not necessarily represent the official views of CIRM or any other agency of the State of California.
Author information
Authors and Affiliations
Contributions
M.B. conceived and designed the study, generated and characterized MDS iPSC lines, performed experiments, analysed data, created the figures and wrote the manuscript. Y.H. helped to generate MDS iPSC lines, generated and characterized wild-type and r(13) iPSC lines, designed the study, performed experiments and analysed data. G.D. and L.A.W. performed SNP array genotyping and CNV calling analyses for MDS samples. E.C.H., S.S. and K.M.T. provided technical support for various experiments. A.R.K. provided advice, access to equipment and laboratory space for M.B. S.Y. supervised the study, provided advice, laboratory space and financial support. A.W.-B. supervised the study, provided advice, helped with design and interpretation, and provided laboratory space and financial support. A.W.-B., Y.H., S.Y., A.R.K., E.C.H. and L.A.W. edited the manuscript. All authors read and approved the final version of the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Extended data figures and tables
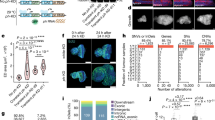
Extended Data Figure 1 Karyotypes of MDS cells used in this study.
a, b, Representative karyotypes of MDS1r(17) fibroblasts (a) and two independent iPSC clones from each of the three MDS patients (b). Magnifications of chromosome 17 pairs (dotted squares) are shown in Fig. 2a for MDS1r(17) cells (boxes 1–3) and to the right of panel (a) for MDS2 and MDS3 iPSCs (boxes 4–7). c, Summary of karyotype data from G-banding analyses of MDS fibroblasts and iPSC clones 1 and 2 (n = 20 each).
Extended Data Figure 2 Expression of pluripotency markers in iPSCs.
a–j, Immunocytochemistry of MDS (a–d) and r(13)-derived (e–j) iPSCs with the antibodies indicated.
Extended Data Figure 3 No evidence of episomal factor integration in iPSCs.
qPCR from genomic DNA using primers specific for exogenous KLF4, SOX2, OCT4, L-MYC and LIN28, as described previously17. a, b, Relative levels of episomal factors in MDS fibroblasts on day 15 after electroporation with epiY4 mixture17 (positive control), WT and MDS iPSCs (passages 20–25), as well as WT human embryonic stem cell line HSF-1 (negative control) (n = 1). c, d, Episomal factor copy number per cell in r(13) fibroblasts electroporated with epiY4 mixture (positive control) and iPSCs (n = 1).
Extended Data Figure 4 Embryoid-body differentiation from MDS iPSCs.
a–c, Immunocytochemistry showing expression of endoderm-derived cells positive for AFP (a), mesoderm-derived cells positive for SMA (b), and ectoderm-derived cells positive for TUJ1 (c) generated in vitro using the embryoid-body method with MDS1r(17), MDS2 and MDS3 iPSCs.
Extended Data Figure 5 Teratoma formation from MDS iPSCs.
a–c, Histological sections from 6.5–11-week teratomas developed in the testis of SCID mice following injection with MDS1r(17), MDS2 and MDS3 iPSCs. Haematoxylin and eosin (H&E) staining reveals characteristic tissues from the mesoderm (a), endoderm (b) and ectoderm (c). d, List of MDS iPSC lines that were injected and teratoma efficiency.
Extended Data Figure 6 Cell morphology and chromosome distribution of additional MDS1r(17) iPSC clones.
a–c, Cell morphology of well growing MDS1r(17) clones 3 and 6 at passage 5 on Matrigel (a), compared to the morphology of poorly growing clones 4 and 5 at passage 4 on SNL feeders (b, approximate colony borders indicated in white) and passage 5 on Matrigel (c). d, examples of metaphase spreads observed in MDS1r(17) clones. e, Quantification of cell populations in MDS1r(17) clones 3–6 with various chromosome compositions shown in (d).
Extended Data Figure 7 Karyotypes of r(13) cells and morphology of corrected iPSC clones.
a–c, Representative karyotypes of GM00285 fibroblasts (a) and corrected GM00285 iPSC clones 1 and 3 (b, c). d, e, Representative karyotypes of GM05563 fibroblasts (d) and corrected GM05563 iPSC clone 1 (e). f–h, Representative morphologies of corrected iPSC clones derived from r(13) fibroblasts cultured in feeder-free conditions.
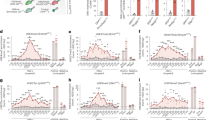
Extended Data Figure 8 Rescue of r(13)-associated deletions in corrected iPSC clones through compensatory uniparental disomy.
a–e, Total copy number of SNPs across chromosome 13 in r(13) GM00285 fibroblasts (a), GM05563 fibroblasts (b), karyotypically normal GM00285 iPSC clones 1 (c) and clone 3 (d), and GM05563 iPSC clone 1 (e). The areas shaded in pink represent the deletions. f, g, Frequency of heterozygous (blue) or homozygous (red) SNPs in r(13) fibroblasts and karyotypically normal iPSC clones for chromosome 13 (f) and chromosome 12 (g). The corrected iPSC clones are completely homozygous for chromosome 13, supporting the compensatory UPD mechanism.
Extended Data Figure 9 Embryoid-body differentiation from ring(13)-derived iPSCs.
a–c, immunocytochemistry showing expression of endoderm-derived cells positive for AFP (a), mesoderm-derived cells positive for SMA (b) and ectoderm-derived cells positive for MAP2 (c) generated in vitro using the embryoid-body method with corrected iPSC clones GM00285-1, GM00285-3 and GM05563-1.
Rights and permissions
About this article
Cite this article
Bershteyn, M., Hayashi, Y., Desachy, G. et al. Cell-autonomous correction of ring chromosomes in human induced pluripotent stem cells. Nature 507, 99–103 (2014). https://doi.org/10.1038/nature12923
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nature12923
This article is cited by
-
Risk assessment of assisted reproductive technology and parental age at childbirth for the development of uniparental disomy-mediated imprinting disorders caused by aneuploid gametes
Clinical Epigenetics (2023)
-
Complex biology of constitutional ring chromosomes structure and (in)stability revealed by somatic cell reprogramming
Scientific Reports (2021)
-
From contemplation to classification of chromosomal mosaicism in human preimplantation embryos
Journal of Assisted Reproduction and Genetics (2021)
-
Autonomous trisomic rescue of Down syndrome cells
Laboratory Investigation (2019)
-
Highly efficient methods to obtain homogeneous dorsal neural progenitor cells from human and mouse embryonic stem cells and induced pluripotent stem cells
Stem Cell Research & Therapy (2018)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.