Abstract
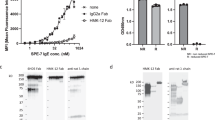
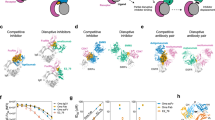
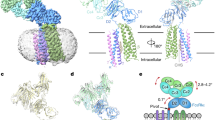
IgE antibodies bind the high-affinity IgE Fc receptor (FcεRI), found primarily on mast cells and basophils, and trigger inflammatory cascades of the allergic response1,2. Inhibitors of IgE–FcεRI binding have been identified and an anti-IgE therapeutic antibody (omalizumab) is used to treat severe allergic asthma3,4. However, preformed IgE–FcεRI complexes that prime cells before allergen exposure dissociate extremely slowly5 and cannot be disrupted by strictly competitive inhibitors. IgE-Fc conformational flexibility indicated that inhibition could be mediated by allosteric or other non-classical mechanisms6,7,8. Here we demonstrate that an engineered protein inhibitor, DARPin E2_79 (refs 9, 10, 11), acts through a non-classical inhibition mechanism, not only blocking IgE–FcεRI interactions, but actively stimulating the dissociation of preformed ligand–receptor complexes. The structure of the E2_79–IgE-Fc3-4 complex predicts the presence of two non-equivalent E2_79 sites in the asymmetric IgE–FcεRI complex, with site 1 distant from the receptor and site 2 exhibiting partial steric overlap. Although the structure is indicative of an allosteric inhibition mechanism, mutational studies and quantitative kinetic modelling indicate that E2_79 acts through a facilitated dissociation mechanism at site 2 alone. These results demonstrate that high-affinity IgE–FcεRI complexes can be actively dissociated to block the allergic response and suggest that protein–protein complexes may be more generally amenable to active disruption by macromolecular inhibitors.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
Change history
22 November 2012
This article was originally incorrectly listed under Planetary Sciences. The subject terms have since been corrected.
References
Kraft, S. & Kinet, J. P. New developments in FcεRI regulation, function and inhibition. Nature Rev. Immunol. 7, 365–378 (2007)
Gould, H. J. & Sutton, B. J. IgE in allergy and asthma today. Nature Rev. Immunol. 8, 205–217 (2008)
D’Amato, G., Bucchioni, E., Oldani, V. & Canonica, W. Treating moderate-to-severe allergic asthma with a recombinant humanized anti-IgE monoclonal antibody (Omalizumab). Treat. Respir. Med. 5, 393–398 (2006)
Chang, T. W. The pharmacological basis of anti-IgE therapy. Nature Biotechnol. 18, 157–162 (2000)
Holdom, M. D. et al. Conformational changes in IgE contribute to its uniquely slow dissociation rate from receptor FcεRI. Nature Struct. Mol. Biol. 18, 571–576 (2011)
Dhaliwal, B. et al. Crystal structure of IgE bound to its B-cell receptor CD23 reveals a mechanism of reciprocal allosteric inhibition with high affinity receptor FcεRI. Proc. Natl Acad. Sci. USA 109, 12686–12691 (2012)
Wurzburg, B. A. & Jardetzky, T. S. Conformational flexibility in immunoglobulin E-Fc3–4 revealed in multiple crystal forms. J. Mol. Biol. 393, 176–190 (2009)
Wurzburg, B. A., Garman, S. C. & Jardetzky, T. S. Structure of the human IgE-Fc Cε3-Cε4 reveals conformational flexibility in the antibody effector domains. Immunity 13, 375–385 (2000)
Eggel, A., Baumann, M. J., Amstutz, P., Stadler, B. M. & Vogel, M. DARPins as bispecific receptor antagonists analyzed for immunoglobulin E receptor blockage. J. Mol. Biol. 393, 598–607 (2009)
Baumann, M. J., Eggel, A., Amstutz, P., Stadler, B. M. & Vogel, M. DARPins against a functional IgE epitope. Immunol. Lett. 133, 78–84 (2010)
Eggel, A. et al. Inhibition of ongoing allergic reactions using a novel anti-IgE DARPin-Fc fusion protein. Allergy 66, 961–968 (2011)
Garman, S. C., Wurzburg, B. A., Tarchevskaya, S. S., Kinet, J. P. & Jardetzky, T. S. Structure of the Fc fragment of human IgE bound to its high-affinity receptor FcεRIα. Nature 406, 259–266 (2000)
Basu, M. et al. Purification and characterization of human recombinant IgE-Fc fragments that bind to the human high affinity IgE receptor. J. Biol. Chem. 268, 13118–13127 (1993)
Wang, B. et al. Epidermal Langerhans cells from normal human skin bind monomeric IgE via FcεRI. J. Exp. Med. 175, 1353–1365 (1992)
Mirkina, I., Schweighoffer, T. & Kricek, F. Inhibition of human cord blood-derived mast cell responses by anti-FcεRI mAb 15/1 versus anti-IgE Omalizumab. Immunol. Lett. 109, 120–128 (2007)
Mendonsa, S. D. & Bowser, M. T. In vitro selection of high-affinity DNA ligands for human IgE using capillary electrophoresis. Anal. Chem. 76, 5387–5392 (2004)
Wiegand, T. W. et al. High-affinity oligonucleotide ligands to human IgE inhibit binding to Fcε receptor I. J. Immunol. 157, 221–230 (1996)
Zheng, L. et al. Fine epitope mapping of humanized anti-IgE monoclonal antibody omalizumab. Biochem. Biophys. Res. Commun. 375, 619–622 (2008)
Wright, J. D. & Lim, C. Prediction of an anti-IgE binding site on IgE. Protein Eng. 11, 421–427 (1998)
Wurzburg, B. A. et al. An engineered disulfide bond reversibly traps the IgE-Fc3-4 in a closed, non-receptor binding conformation. J. Biol. Chem. http://dx.doi.org/10.1074/jbc.M112.407502 (2012)
Prinz, H. & Striessnig, J. Ligand-induced accelerated dissociation of (+)-cis-diltiazem from L-type Ca2+ channels is simply explained by competition for individual attachment points. J. Biol. Chem. 268, 18580–18585 (1993)
Gutfreund, H. Kinetics for the Life Sciences. Receptors, Transmitters and Catalysts (Cambridge Univ. Press, 1995)
Hoops, S. et al. COPASI—a COmplex PAthway SImulator. Bioinformatics 22, 3067–3074 (2006)
He, M. M. et al. Small-molecule inhibition of TNF-α. Science 310, 1022–1025 (2005)
Wells, J. A. & McClendon, C. L. Reaching for high-hanging fruit in drug discovery at protein-protein interfaces. Nature 450, 1001–1009 (2007)
Wang, C. C. et al. Negative and positive site-site interactions, and their modulation by pH, insulin analogs, and monoclonal antibodies, are preserved in the purified insulin receptor. Proc. Natl Acad. Sci. USA 85, 8400–8404 (1988)
Lowenthal, J. W. et al. High and low affinity IL 2 receptors: analysis by IL 2 dissociation rate and reactivity with monoclonal anti-receptor antibody PC61. J. Immunol. 135, 3988–3994 (1985)
Boulain, J. C. & Menez, A. Neurotoxin-specific immunoglobulins accelerate dissociation of the neurotoxin-acetylcholine receptor complex. Science 217, 732–733 (1982)
Garman, S. C., Kinet, J. P. & Jardetzky, T. S. Crystal structure of the human high-affinity IgE receptor. Cell 95, 951–961 (1998)
Otwinowski, Z. & Minor, W. Processing of X-ray diffraction data collected in oscillation mode. in Methods Enzymol. Vol. 276 (eds Carter, J. C. W. & Sweet, R. M. ) 307–326 (Academic, 1997)
McCoy, A. J. et al. Phaser crystallographic software. J. Appl. Crystallogr. 40, 658–674 (2007)
Emsley, P. & Cowtan, K. Coot: model-building tools for molecular graphics. Acta Crystallogr. D 60, 2126–2132 (2004)
Chen, V. B. et al. MolProbity: all-atom structure validation for macromolecular crystallography. Acta Crystallogr. D 66, 12–21 (2010)
Laskowski, R. A., Rullmannn, J. A., MacArthur, M. W., Kaptein, R. & Thornton, J. M. AQUA and PROCHECK-NMR: programs for checking the quality of protein structures solved by NMR. J. Biomol. NMR 8, 477–486 (1996)
Acknowledgements
We thank B. Wurzburg and other past and present members of the Jardetzky Laboratory. This research was supported in part by an NIH research grant (AI-18939) and an American Asthma Foundation Senior Investigator Award as well as the Swiss National Science Foundation grant number 310030_127350 to T.S.J. We also thank C. A. Dahinden and B. M. Stadler and members of their groups for valuable discussions. Furthermore, we thank M. J. Baumann for technical support and Molecular Partners AG, especially P. Amstutz, M. T. Stumpp, P. Forrer and D. Steiner, for placing DARPin libraries at our disposal and providing scientific support.
Author information
Authors and Affiliations
Contributions
B.K., A.E., S.S.T. and T.S.J. designed and performed experiments. B.K., A.E., S.S.T., H.P. and T.S.J. analysed data. B.K., S.S.T., A.E., M.V. and T.S.J. contributed reagents. B.K., S.S.T., A.E., M.V., H.P. and T.S.J. discussed/commented on results and edited the manuscript. B.K., A.E. and T.S.J. wrote the manuscript and Supplementary Information, and prepared the figures.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Supplementary Information
This file contains Supplementary Figures 1-3 and Supplementary Tables 1-4. (PDF 999 kb)
Rights and permissions
About this article
Cite this article
Kim, B., Eggel, A., Tarchevskaya, S. et al. Accelerated disassembly of IgE–receptor complexes by a disruptive macromolecular inhibitor. Nature 491, 613–617 (2012). https://doi.org/10.1038/nature11546
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nature11546
This article is cited by
-
Understanding human mast cells: lesson from therapies for allergic and non-allergic diseases
Nature Reviews Immunology (2022)
-
The mechanistic and functional profile of the therapeutic anti-IgE antibody ligelizumab differs from omalizumab
Nature Communications (2020)
-
Tailoring the component of protein corona via simple chemistry
Nature Communications (2019)
-
IL-3 but not monomeric IgE regulates FcεRI levels and cell survival in primary human basophils
Cell Death & Disease (2018)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.