Abstract
Studies of the human microbiome have revealed that even healthy individuals differ remarkably in the microbes that occupy habitats such as the gut, skin and vagina. Much of this diversity remains unexplained, although diet, environment, host genetics and early microbial exposure have all been implicated. Accordingly, to characterize the ecology of human-associated microbial communities, the Human Microbiome Project has analysed the largest cohort and set of distinct, clinically relevant body habitats so far. We found the diversity and abundance of each habitat’s signature microbes to vary widely even among healthy subjects, with strong niche specialization both within and among individuals. The project encountered an estimated 81–99% of the genera, enzyme families and community configurations occupied by the healthy Western microbiome. Metagenomic carriage of metabolic pathways was stable among individuals despite variation in community structure, and ethnic/racial background proved to be one of the strongest associations of both pathways and microbes with clinical metadata. These results thus delineate the range of structural and functional configurations normal in the microbial communities of a healthy population, enabling future characterization of the epidemiology, ecology and translational applications of the human microbiome.
Similar content being viewed by others
Main
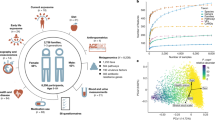
A total of 4,788 specimens from 242 screened and phenotyped adults1 (129 males, 113 females) were available for this study, representing the majority of the target Human Microbiome Project (HMP) cohort of 300 individuals. Adult subjects lacking evidence of disease were recruited based on a lengthy list of exclusion criteria; we will refer to them here as ‘healthy’, as defined by the consortium clinical sampling criteria (K. Aagaard et al., manuscript submitted). Women were sampled at 18 body habitats, men at 15 (excluding three vaginal sites), distributed among five major body areas. Nine specimens were collected from the oral cavity and oropharynx: saliva; buccal mucosa (cheek), keratinized gingiva (gums), palate, tonsils, throat and tongue soft tissues, and supra- and subgingival dental plaque (tooth biofilm above and below the gum). Four skin specimens were collected from the two retroauricular creases (behind each ear) and the two antecubital fossae (inner elbows), and one specimen for the anterior nares (nostrils). A self-collected stool specimen represented the microbiota of the lower gastrointestinal tract, and three vaginal specimens were collected from the vaginal introitus, midpoint and posterior fornix. To evaluate within-subject stability of the microbiome, 131 individuals in these data were sampled at an additional time point (mean 219 days and s.d. 69 days after first sampling, range 35–404 days). After quality control, these specimens were used for 16S rRNA gene analysis via 454 pyrosequencing (abbreviated henceforth as 16S profiling, mean 5,408 and s.d. 4,605 filtered sequences per sample); to assess function, 681 samples were sequenced using paired-end Illumina shotgun metagenomic reads (mean 2.9 gigabases (Gb) and s.d. 2.1 Gb per sample)1. More details on data generation are provided in related HMP publications1 and in Supplementary Methods.
Microbial diversity of healthy humans
The diversity of microbes within a given body habitat can be defined as the number and abundance distribution of distinct types of organisms, which has been linked to several human diseases: low diversity in the gut to obesity and inflammatory bowel disease2,3, for example, and high diversity in the vagina to bacterial vaginosis4. For this large study involving microbiome samples collected from healthy volunteers at two distinct geographic locations in the United States, we have defined the microbial communities at each body habitat, encountering 81–99% of predicted genera and saturating the range of overall community configurations (Fig. 1, Supplementary Fig. 1 and Supplementary Table 1; see also Fig. 4). Oral and stool communities were especially diverse in terms of community membership, expanding prior observations5, and vaginal sites harboured particularly simple communities (Fig. 1a). This study established that these patterns of alpha diversity (within samples) differed markedly from comparisons between samples from the same habitat among subjects (beta diversity, Fig. 1b). For example, the saliva had among the highest median alpha diversities of operational taxonomic units (OTUs, roughly species level classification, see http://hmpdacc.org/HMQCP), but one of the lowest beta diversities—so although each individual’s saliva was ecologically rich, members of the population shared similar organisms. Conversely, the antecubital fossae (skin) had the highest beta diversity but were intermediate in alpha diversity. The vagina had the lowest alpha diversity, with quite low beta diversity at the genus level but very high among OTUs due to the presence of distinct Lactobacillus spp. (Fig. 1b). The primary patterns of variation in community structure followed the major body habitat groups (oral, skin, gut and vaginal), defining as a result the complete range of population-wide between-subject variation in human microbiome habitats (Fig. 1c). Within-subject variation over time was consistently lower than between-subject variation, both in organismal composition and in metabolic function (Fig. 1d). The uniqueness of each individual’s microbial community thus seems to be stable over time (relative to the population as a whole), which may be another feature of the human microbiome specifically associated with health.
a, Alpha diversity within subjects by body habitat, grouped by area, as measured using the relative inverse Simpson index of genus-level phylotypes (cyan), 16S rRNA gene OTUs (blue), shotgun metagenomic reads matched to reference genomes (orange), functional modules (dark orange), and enzyme families (yellow). The mouth generally shows high within-subject diversity and the vagina low diversity, with other habitats intermediate; variation among individuals often exceeds variation among body habitats. b, Bray–Curtis beta diversity among subjects by body habitat, colours as for a. Skin differs most between subjects, with oral habitats and vaginal genera more stable. Although alpha- and beta-diversity are not directly comparable, changes in structure among communities (a) occupy a wider dynamic range than do changes within communities among individuals (b). c, Principal coordinates plot showing variation among samples demonstrates that primary clustering is by body area, with the oral, gastrointestinal, skin and urogenital habitats separate; the nares habitat bridges oral and skin habitats. d, Repeated samples from the same subject (blue) are more similar than microbiomes from different subjects (red). Technical replicates (grey) are in turn more similar; these patterns are consistent for all body habitats and for both phylogenetic and metabolic community composition. See previously described sample counts1 for all comparisons.
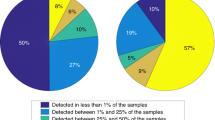
No taxa were observed to be universally present among all body habitats and individuals at the sequencing depth employed here, unlike several pathways (Fig. 2 and Supplementary Fig. 2, see below), although several clades demonstrated broad prevalence and relatively abundant carriage patterns6,7. Instead, as suggested by individually focused studies2,3,5,8,9, each body habitat in almost every subject was characterized by one or a few signature taxa making up the plurality of the community (Fig. 3). Signature clades at the genus level formed on average anywhere from 17% to 84% of their respective body habitats, completely absent in some communities (0% at this level of detection) and representing the entire population (100%) in others. Notably, less dominant taxa were also highly personalized, both among individuals and body habitats; in the oral cavity, for example, most habitats are dominated by Streptococcus, but these are followed in abundance by Haemophilus in the buccal mucosa, Actinomyces in the supragingival plaque, and Prevotella in the immediately adjacent (but low oxygen) subgingival plaque10.
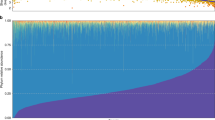
a, b, Vertical bars represent microbiome samples by body habitat in the seven locations with both shotgun and 16S data; bars indicate relative abundances colored by microbial phyla from binned OTUs (a) and metabolic modules (b). Legend indicates most abundant phyla/pathways by average within one or more body habitats; RC, retroauricular crease. A plurality of most communities’ memberships consists of a single dominant phylum (and often genus; see Supplementary Fig. 2), but this is universal neither to all body habitats nor to all individuals. Conversely, most metabolic pathways are evenly distributed and prevalent across both individuals and body habitats.
a–c, Prevalence (intensity, colour denoting phylum/class) and abundance when present (size) of clades in the healthy microbiome. The most abundant metagenomically-identified species (a), 16S-identified genera (b) and PATRIC12 pathogens (metagenomic) (c) are shown. d, e, The population size and sequencing depths of the HMP have well defined the microbiome at all assayed body sites, as assessed by saturation of added community metabolic configurations (rarefaction of minimum Bray–Curtis beta-diversity of metagenomic enzyme class abundances to nearest neighbour, inter-quartile range over 100 samples) (d) and phylogenetic configurations (minimum 16S OTU weighted UniFrac distance to nearest neighbour) (e).
Additional taxonomic detail of the human microbiome was provided by identifying unique marker sequences in metagenomic data11 (Fig. 3a) to complement 16S profiling (Fig. 3b). These two profiles were typically in close agreement (Supplementary Fig. 3), with the former in some cases offering more specific information on members of signature genera differentially present within habitats (for example, vaginal Prevotella amnii and gut Prevotella copri) or among individuals (for example, vaginal Lactobacillus spp.) One application of this specificity was to confirm the absence of NIAID (National Institute of Allergy and Infectious Diseases) class A–C pathogens above 0.1% abundance (aside from Staphylococcus aureus and Escherichia coli) from the healthy microbiome, but the near-ubiquity and broad distribution of opportunistic ‘pathogens’ as defined by PATRIC12. Canonical pathogens including Vibrio cholerae, Mycobacterium avium, Campylobacter jejuni and Salmonella enterica were not detected at this level of sensitivity. Helicobacter pylori was found in only two stool samples, both at <0.01%, and E. coli was present at >0.1% abundance in 15% of stool microbiomes (>0% abundance in 61%). Similar species-level observations were obtained for a small subset of stool samples with 454 pyrosequencing metagenomics data using PhylOTU13,14. In total 56 of 327 PATRIC pathogens were detected in the healthy microbiome (at >1% prevalence of >0.1% abundance, Supplementary Table 2), all opportunistic and, strikingly, typically prevalent both among hosts and habitats. The latter is in contrast to many of the most abundant signature taxa, which were usually more habitat-specific and variable among hosts (Fig. 3a, b). This overall absence of particularly detrimental microbes supports the hypothesis that even given this cohort’s high diversity, the microbiota tend to occupy a range of configurations in health distinct from many of the disease perturbations studied to date3,15.
Carriage of specific microbes
Inter-individual variation in the microbiome proved to be specific, functionally relevant and personalized. One example of this is illustrated by the Streptococcus spp. of the oral cavity. The genus dominates the oropharynx16, with different species abundant within each sampled body habitat (see http://hmpdacc.org/HMSMCP) and, even at the species level, marked differences in carriage within each habitat among individuals (Fig. 4a). As the ratio of pan- to core-genomes is high in many human-associated microbes17, this variation in abundance could be due to selective pressures acting on pathways differentially present among Streptococcus species or strains (Fig. 4b). Indeed, we observed extensive strain-level genomic variation within microbial species in this population, enriched for host-specific structural variants around genomic islands (Fig. 4c). Even with respect to the single Streptococcus mitis strain B6, gene losses associated with these events were common, for example differentially eliminating S. mitis carriage of the V-type ATPase or choline binding proteins cbp6 and cbp12 among subsets of the host population (Fig. 4d). These losses were easily observable by comparison to reference isolate genomes, and these initial findings indicate that microbial strain- and host-specific gene gains and polymorphisms may be similarly ubiquitous.
Metagenomic reads from 127 tongue samples spanning 90 subjects were processed with MetaPhlAn to determine relative abundances for each species. a, Relative abundances of 11 distinct Streptococcus spp. In addition to variation in broader clades (see Fig. 2), individual species within a single habitat demonstrate a wide range of compositional variation. Inset illustrates average tongue sample composition. b, Metabolic modules present/absent (grey/white) in KEGG24 reference genomes of tongue streptococci denote selected areas of strain-specific functional differentiation. cpnt, component. c, Comparative genomic coverage for the single Streptococcus mitis B6 strain. Grey dots are median reads per kilobase per million reads (RPKM) for 1-kb windows, grey bars are the 25th to 75th percentiles across all samples, red line the LOWESS-smoothed average. Red bars at the bottom highlight predicted genomic islands27. Large, discrete, and highly variable islands are commonly under-represented. d, Two islands are highlighted, V (V-type H+ ATPase subunits I, K, E, C, F, A and B) and CH (choline-binding proteins cbp6 and cbp12), indicating functional cohesion of strain-specific gene loss within individual human hosts.
Other examples of functionally relevant inter-individual variation at the species and strain levels occurred throughout the microbiome. In the gut, Bacteroides fragilis has been shown to prime T-cell responses in animal models via the capsular polysaccharide A18, and in the HMP stool samples this taxon was carried at a level of at least 0.1% in 16% of samples (over 1% abundance in 3%). Bacteroides thetaiotaomicron has been studied for its effect on host gastrointestinal metabolism19 and was likewise common at 46% prevalence. On the skin, S. aureus, of particular interest as the cause of methicillin-resistant S. aureus (MRSA) infections, had 29% nasal and 4% skin carriage rates, roughly as expected20. Close phylogenetic relatives such as Staphylococcus epidermidis (itself considered commensal) were, in contrast, universal on the skin and present in 93% of nares samples, and at the opposite extreme Pseudomonas aeruginosa (a representative Gram-negative skin pathogen) was completely absent from both body habitats (0% at this level of detection). These and the data above suggest that the carriage pattern of some species in the human microbiome may be analogous to genetic traits, where recessive alleles of modest risk are maintained in a population. In the case of the human microbiome, high-risk pathogens remain absent, whereas species that pose a modest degree of risk also seem to be stably maintained in this ecological niche.
Finally, microorganisms within and among body habitats exhibited relationships suggestive of driving physical factors such as oxygen, moisture and pH, host immunological factors, and microbial interactions such as mutualism or competition21 (Supplementary Fig. 4). Both overall community similarity and microbial co-occurrence and co-exclusion across the human microbiome grouped the 18 body habitats together into four clusters corresponding to the five target body areas (Supplementary Fig. 4a, b). There was little distinction among different vaginal sites, with Lactobacillus spp. dominating all three and correlating in abundance. However, Lactobacillus varied inversely with the Actinobacteria and Bacteroidetes (see Supplementary Fig. 4c and Figs 2 and 3), as also observed in a previous cohort9. Gut microbiota relationships primarily comprised inverse associations with the Bacteroides, which ranged from dominant in some subjects to a minority in others who carried a greater diversity of Firmicutes. A similar progression was evident in the skin communities, dominated by one of Staphylococcus (phylum Firmicutes), Propionibacterium, or Corynebacterium (both phylum Actinobacteria), with a continuum of oral organisms (for example, Streptococcus) appearing in nares communities (Supplementary Fig. 4c). These observations suggest that microbial community structure in these individuals may sometimes occupy discrete configurations and under other circumstances vary continuously, a topic addressed in more detail by several HMP investigations (ref. 6 and unpublished results). An individual’s location within such configurations is indicative of current microbial carriage (including pathogens) and of the community’s ability to resist future pathogen acquisition or dysbiosis; it may thus prove to be associated with disease susceptibility or other phenotypic characteristics.
Microbiome metabolism and function
As the first study to include both marker gene and metagenomic data across body habitats from a large human population, we additionally assessed the ecology of microbial metabolic and functional pathways in these communities. We reconstructed the relative abundances of pathways in community metagenomes22, which were much more constant and evenly diverse than were organismal abundances (Fig. 2b, see also Fig. 1), confirming this as an ecological property of the entire human microbiome2. We were likewise able to determine for the first time that taxonomic and functional alpha diversity across microbial communities significantly correlate (Spearman of inverse Simpson’s r = 0.60, P = 3.6 × 10−67, n = 661), the latter within a more proscribed range of community configurations (Supplementary Fig. 5).
Unlike microbial taxa, several pathways were ubiquitous among individuals and body habitats. The most abundant of these ‘core’ pathways include the ribosome and translational machinery, nucleotide charging and ATP synthesis, and glycolysis, and reflect the basics of host-associated microbial life. Also in contrast to taxa, few pathways were highly variable among subjects within any body habitat; exceptions included the Sec (orally, pathway relative abundance s.d. = 0.0052; total mean of oral standard deviations = 0.0011 with s.d. = 0.0016) and Tat (globally, pathway s.d. = 0.0055; mean of global standard deviations = 0.0023 with s.d. = 0.0033) secretion systems, indicating a high degree of host–microbe and microbe–microbe interactions in the healthy human microbiota. This high variability was particularly present in the oral cavity; for phosphate, mono- and di-saccharide, and amino acid transport in the mucosa; and also for lipopolysaccharide biosynthesis and spermidine/putrescine synthesis and transport on the plaque and tongue (http://hmpdacc.org/HMMRC). The stability and high metagenomic abundance of this housekeeping ‘core’ contrasts with the greater variability and lower abundance of niche-specific functionality in rare but consistently present pathways; for example, spermidine biosynthesis, methionine degradation and hydrogen sulphide production, all examples highly prevalent in gastrointestinal body sites (non-zero in >92% of samples) but at very low abundance (median relative abundance < 0.0052). This ‘long tail’ of low-abundance genes and pathways also probably encodes much of the uncharacterized biomolecular function and metabolism of these metagenomes, the expression levels of which remain to be explored in future metatranscriptomic studies.
Protein families showed diversity and prevalence trends similar to those of full pathways, ranging from maxima of only ∼16,000 unique families per community in the vagina to almost 400,000 in the oral cavity (Fig. 1a, b; http://hmpdacc.org/HMGI). A remarkable fraction of these families were indeed functionally uncharacterized, including those detected by read mapping, with a minimum in the oral cavity (mean 58% s.d. 6.8%) and maximum in the nares (mean 77% s.d. 11%). Likewise, many genes annotated from assemblies could not be assigned a metabolic function, with a minimum in the vagina (mean 78% s.d. 3.4%) and maximum in the gut (mean 86% s.d. 0.9%). The latter range did not differ substantially by body habitat and is in close agreement with previous comprehensive gene catalogues of the gut metagenome3. Taken together with the microbial variation observed above throughout the human microbiome, functional variation among individuals might indicate pathways of particular importance in maintaining community structure in the face of personalized immune, environmental or dietary exposures among these subjects. Determining the functions of uncharacterized core and variable protein families will be especially essential in understanding role of the microbiota in health and disease.
Correlations with host phenotype
We finally examined relationships associating both clades and metabolism in the microbiota with host properties such as age, gender, body mass index (BMI), and other available clinical metadata (Fig. 5 and Supplementary Table 3). Using a sparse multivariate model, 960 microbial, enzymatic or pathway abundances were significantly associated with one or more of 15 subject phenotype and sample metadata features. A wide variety of taxa, gene families and metabolic pathways were differentially distributed with subject ethnicity at every body habitat (Fig. 5a), representing the phenotype with the greatest number (266 at false discovery rate (FDR) q < 0.2) of total associations with the microbiome. Vaginal pH has also been observed to correlate with microbiome composition9, and we detected in this population both the expected reduction in Lactobacillus at high pH and a corresponding increase in metabolic diversity (Fig. 5b). Intriguingly, and not previously observed, subject age was most associated with a collection of highly differential metagenomically encoded pathways on the skin (Fig. 5c), as well as shifts in skin clades including retroauricular Firmicutes (P = 1.0 × 10−4, q = 0.033). The examples of associations with ethnicity and vaginal pH are among the strongest associations with the microbiome, however, and most correlates (for example, with subject BMI, Fig. 5d) are more representatively modest. This lower degree of correlation held for most available biometrics (gender, temperature, blood pressure, etc.), with even the most significant associations possessing generally low effect sizes and considerable unexplained variance. We conclude that most variation in the human microbiome is not well explained by these phenotypic metadata, and other potentially important factors such as short- and long-term diet, daily cycles, founder effects such as mode of delivery, and host genetics should be considered in future analyses.
a–d, The pathway and clade abundances most significantly associated (all FDR q < 0.2) using a multivariate linear model with subject race or ethnicity (a), vaginal posterior fornix pH (b), subject age (c) and BMI (d). Scatter plots of samples are shown with lines indicating best simple linear fit. Race/ethnicity and vaginal pH are particularly strong associations; age and BMI are more representative of typically modest phenotypic associations (Supplementary Table 3), suggesting that variation in the healthy microbiota may correspond to other host or environmental factors.
Conclusions
This extensive sampling of the human microbiome across many subjects and body habitats provides an initial characterization of the normal microbiota of healthy adults in a Western population. The large sample size and consistent sampling of many sites from the same individuals allows for the first time an understanding of the relationships among microbes, and between the microbiome and clinical parameters, that underpin the basis for individual variation—variation that may ultimately be critical for understanding microbiome-based disorders. Clinical studies of the microbiome will be able to leverage the resulting extensive catalogues of taxa, pathways and genes1, although they must also still include carefully matched internal controls. The uniqueness of each individual’s microbiome even in this reference population argues for future studies to consider prospective within-subjects designs where possible. The HMP’s unique combination of organismal and functional data across body habitats, encompassing both 16S and metagenomic profiling, together with detailed characterization of each subject, has allowed us and subsequent studies to move beyond the observation of variability in the human microbiome to ask how and why these microbial communities vary so extensively.
Many details remain for further work to fill in, building on this reference study. How do early colonization and lifelong change vary among body habitats? Do epidemiological patterns of transmission of beneficial or harmless microbes mirror patterns of transmission of pathogens? Which co-occurrences among microbes reflect shared response to the environment, as opposed to competitive or mutualistic interactions? How large a role does host immunity or genetics play in shaping patterns of diversity, and how do the patterns observed in this North American population compare to those around the world? Future studies building on the gene and organism catalogues established by the Human Microbiome Project, including increasingly detailed investigations of metatranscriptomes and metaproteomes, will help to unravel these open questions and allow us to more fully understand the links between the human microbiome, health and disease.
Methods Summary
Microbiome samples were collected from up to 18 body sites at one or two time points from 242 individuals clinically screened for absence of disease (K. Aagaard et al., manuscript submitted). Samples were subjected to 16S ribosomal RNA gene pyrosequencing (454 Life Sciences), and a subset were shotgun-sequenced for metagenomics using the Illumina GAIIx platform1. 16S data processing and diversity estimates were performed using QIIME23, and metagenomic data were taxonomically profiled using MetaPhlAn11, metabolically profiled by HUMAnN22, and assembled for gene annotation and clustering into a unique catalogue1. Potential pathogens were identified using the PATRIC database12, isolate reference genome annotations drawn from KEGG24, and reference genome mapping performed by BWA25 to a reduced set of genomes to which short reads could be matched26. Microbial associations were assessed by similarity measures accounting for compositionality21, and phenotypic association testing was performed in R. All data and additional protocol details are available at http://hmpdacc.org. Full methods accompany this paper in the Supplementary Information.
References
The Human Microbiome Project Consortium. A framework for human microbiome research. Nature http://dx.doi.org/10.1038/nature11209 (this issue)
Turnbaugh, P. J. et al. A core gut microbiome in obese and lean twins. Nature 457, 480–484 (2009)
Qin, J. et al. A human gut microbial gene catalogue established by metagenomic sequencing. Nature 464, 59–65 (2010)
Fredricks, D. N., Fiedler, T. L. & Marrazzo, J. M. Molecular identification of bacteria associated with bacterial vaginosis. N. Engl. J. Med. 353, 1899–1911 (2005)
Costello, E. K. et al. Bacterial community variation in human body habitats across space and time. Science 326, 1694–1697 (2009)
Huse, S., Ye, Y., Zhou, Y. & Fodor, A. A core human microbiome as viewed through 16s rRNA sequences clusters. PLoS ONE http://dx.doi.org/10.1371/journal.pone.0034242 (14 June 2012)
Li, K., Bihan, M., Yooseph, S. & Methe, B. A. Analyses of the microbial diversity across the human microbiome. PLoS ONE http://dx.doi.org/10.1371/journal.pone.0032118 (14 June 2012)
Grice, E. A. et al. Topographical and temporal diversity of the human skin microbiome. Science 324, 1190–1192 (2009)
Ravel, J. et al. Vaginal microbiome of reproductive-age women. Proc. Natl Acad. Sci. USA 108 (Suppl 1). 4680–4687 (2011)
Segata, N. et al. Composition of the adult digestive tract microbiome based on seven mouth surfaces, tonsils, throat and stool samples. Genome Biol. 13, R42 (2012)
Segata, N. et al. Efficient metagenomic microbial community profiling using unique clade-specific marker genes. Nature Methods http://dx.doi.org/10.1038/nmeth.2066 (2012)
Gillespie, J. J. et al. PATRIC: the comprehensive bacterial bioinformatics resource with a focus on human pathogenic species. Infect. Immun. 79, 4286–4298 (2011)
Sharpton, T. J. et al. PhylOTU: a high-throughput procedure quantifies microbial community diversity and resolves novel taxa from metagenomic data. PLoS Comput. Biol. 7, e1001061 (2011)
Wylie, K. M. et al. Novel bacterial taxa in the human microbiome. PLoS ONE http://dx.doi.org/10.1371/journal.pone.003529 (14 June 2012)
Sokol, H. et al. Faecalibacterium prausnitzii is an anti-inflammatory commensal bacterium identified by gut microbiota analysis of Crohn disease patients. Proc. Natl Acad. Sci. USA 105, 16731–16736 (2008)
Aas, J. A., Paster, B. J., Stokes, L. N., Olsen, I. & Dewhirst, F. E. Defining the normal bacterial flora of the oral cavity. J. Clin. Microbiol. 43, 5721–5732 (2005)
Medini, D. et al. Microbiology in the post-genomic era. Nature Rev. Microbiol. 6, 419–430 (2008)
Mazmanian, S. K., Round, J. L. & Kasper, D. L. A microbial symbiosis factor prevents intestinal inflammatory disease. Nature 453, 620–625 (2008)
Goodman, A. L. et al. Identifying genetic determinants needed to establish a human gut symbiont in its habitat. Cell Host Microbe 6, 279–289 (2009)
Kuehnert, M. J. et al. Prevalence of Staphylococcus aureus nasal colonization in the United States, 2001–2002. J. Infect. Dis. 193, 172–179 (2006)
Faust, K. et al. Microbial co-occurrence relationships in the human microbiome. PLoS Comput. Biol. (in the press)
Abubucker, S. et al. Metabolic reconstruction for metagenomic data and its application to the human microbiome. PLoS Comput. Biol. http://dx.doi.org/10.1371/journal.pcbi.1002358 (14 June 2012)
Caporaso, J. G. et al. QIIME allows analysis of high-throughput community sequencing data. Nature Methods 7, 335–336 (2010)
Kanehisa, M., Goto, S., Furumichi, M., Tanabe, M. & Hirakawa, M. KEGG for representation and analysis of molecular networks involving diseases and drugs. Nucleic Acids Res. 38, D355–D360 (2010)
Li, H. & Durbin, R. Fast and accurate long-read alignment with Burrows–Wheeler transform. Bioinformatics 26, 589–595 (2010)
Giannoukos, G. et al. Efficient and robust RNA-seq process for cultured bacteria and complex community transcriptomes. Genome Biol. 13, R23 (2012)
Langille, M. G. & Brinkman, F. S. IslandViewer: an integrated interface for computational identification and visualization of genomic islands. Bioinformatics 25, 664–665 (2009)
Acknowledgements
The Consortium would like to thank our external scientific advisory board: R. Blumberg, J. Davies, R. Holt, P. Ossorio, F. Ouellette, G. Schoolnik and A. Williamson. We would also like to thank our collaborators throughout the International Human Microbiome Consortium, particularly the investigators of the MetaHIT project, for advancing human microbiome research. Data repository management was provided by the National Center for Biotechnology Information and the Intramural Research Program of the NIH National Library of Medicine. We appreciate the participation of the individuals from the Saint Louis, Missouri, and Houston, Texas areas who made this study possible. This research was supported in part by National Institutes of Health grants U54HG004969 to B.W.B.; U54HG003273 to R.A.G.; U54HG004973 to R.A.G., S.K.H. and J.F.P.; U54HG003067 to E.S.Lander; U54AI084844 to K.E.N.; N01AI30071 to R.L.Strausberg; U54HG004968 to G.M.W.; U01HG004866 to O.R.W.; U54HG003079 to R.K.W.; R01HG005969 to C.H.; R01HG004872 to R.K.; R01HG004885 to M.P.; R01HG005975 to P.D.S.; R01HG004908 to Y.Y.; R01HG004900 to M.K.Cho and P. Sankar; R01HG005171 to D.E.H.; R01HG004853 to A.L.M.; R01HG004856 to R.R.; R01HG004877 to R.R.S. and R.F.; R01HG005172 to P. Spicer.; R01HG004857 to M.P.; R01HG004906 to T.M.S.; R21HG005811 to E.A.V.; M.J.B. was supported by UH2AR057506; G.A.B. was supported by UH2AI083263 and UH3AI083263 (G.A.B., C. N. Cornelissen, L. K. Eaves and J. F. Strauss); S.M.H. was supported by UH3DK083993 (V. B. Young, E. B. Chang, F. Meyer, T. M. S., M. L. Sogin, J. M. Tiedje); K.P.R. was supported by UH2DK083990 (J. V.); J.A.S. and H.H.K. were supported by UH2AR057504 and UH3AR057504 (J.A.S.); DP2OD001500 to K.M.A.; N01HG62088 to the Coriell Institute for Medical Research; U01DE016937 to F.E.D.; S.K.H. was supported by RC1DE0202098 and R01DE021574 (S.K.H. and H. Li); J.I. was supported by R21CA139193 (J.I. and D. S. Michaud); K.P.L. was supported by P30DE020751 (D. J. Smith); Army Research Office grant W911NF-11-1-0473 to C.H.; National Science Foundation grants NSF DBI-1053486 to C.H. and NSF IIS-0812111 to M.P.; The Office of Science of the US Department of Energy under Contract No. DE-AC02-05CH11231 for P.S. C.; LANL Laboratory-Directed Research and Development grant 20100034DR and the US Defense Threat Reduction Agency grants B104153I and B084531I to P.S.C.; Research Foundation - Flanders (FWO) grant to K.F. and J.Raes; R.K. is an HHMI Early Career Scientist; Gordon & Betty Moore Foundation funding and institutional funding from the J. David Gladstone Institutes to K.S.P.; A.M.S. was supported by fellowships provided by the Rackham Graduate School and the NIH Molecular Mechanisms in Microbial Pathogenesis Training Grant T32AI007528; a Crohn’s and Colitis Foundation of Canada Grant in Aid of Research to E.A.V.; 2010 IBM Faculty Award to K.C.W.; analysis of the HMP data was performed using National Energy Research Scientific Computing resources, the BluBioU Computational Resource at Rice University.
Author information
Authors and Affiliations
Consortia
Contributions
Principal investigators: B.W.B., R.A.G., S.K.H., B.A.M., K.E.N., J.F.P., G.M.W., O.W., R.K.W. Manuscript preparation: D.G., C.H., R.K., O.W. Funding agency management: C.C.B., T.B., V.R.B., J.L.C., S.C., C.D., V.D.F., C.G., M.Y.G., R.D.L., J.M., P.M., J.P., L.M.P., J.A.S., L.W., C.W., K.A.W. Project leadership: S.A., J.H.B., B.W.B., A.T.C., H.H.C., A.M.E., M.G.F., R.S.F., D.G., M.G.G., K.H., S.K.H., C.H., E.A.L., R.M., V.M., J.C.M., B.A.M., M.M., D.M.M., K.E.N., J.F.P., E.J.S., J.V., G.M.W., O.W., A.M.W., K.C.W., J.R.W., S.K.Y., Q.Z. Analysis preparation for manuscript: J.C.C., K.F., D.G., A.G., K.H.H., C.H., R.K., D.K., H.H.K., O.K., K.P.L., R.E.L., J.R., J.F.S., P.D.S., N.S. Data release: L.A., T.B., I.A.C., K.C., H.H.C., N.J.D., D.J.D., A.M.E., V.M.F., L.F., J.M.G., S.G., S.K.H., M.E.H., C.J., V.J., C.K., A.A.M., V.M.M., T.M., M.M., D.M.M., J.O., K.P., J.F.P., C.P., X.Q., R.K.S., N.S., I.S., E.J.S., D.V.W., O.W., K.W., K.C.W., C.Y., B.P.Y., Q.Z. Methods and research development: S.A., H.M.A., M.B., D.M.C., A.M.E., R.L.E., M.F., S.F., M.G.F., D.C.F., D.G., G.G., B.J.H., S.K.H., M.E.H., W.A.K., N.L., K.L., V.M., E.R.M., B.A.M., M.M., D.M.M., C.N., J.F.P., M.E.P., X.Q., M.C.R., C.R., E.J.S., S.M.S., D.G.T., D.V.W., G.M.W., Y.W., K.M.W., S.Y., B.P.Y., S.K.Y., Q.Z. DNA sequence production: S.A., E.A., T.A., T.B., C.J.B., D.A.B., K.D.D., S.P.D., A.M.E., R.L.E., C.N.F., S.F., C.C.F., L.L.F., R.S.F., B.H., S.K.H., M.E.H., V.J., C.L.K., S.L.L., N.L., L.L., D.M.M., I.N., C.N., M.O., J.F.P., X.Q., J.G.R., Y.R., M.C.R., D.V.W., Y.W., B.P.Y., Y.Z. Clinical sample collection: K.M.A., M.A.C., W.M.D., L.L.F., N.G., H.A.H., E.L.H., J.A.K., W.A.K., T.M., A.L.M., P.M., S.M.P., J.F.P., G.A.S., J.V., M.A.W., G.M.W. Body site experts: K.M.A., E.A.V., G.A., L.B., M.J.B., C.C.D., F.E.D., L.F., J.I., J.A.K., S.K.H., H.H.K., K.P.L., P.J.M., J. Ravel, T.M.S., J.A.S., J.D.S., J.V. Ethical, legal and social implications: R.M.F., D.E.H., W.A.K., N.B.K., C.M.L., A.L.M., R.R., P. Sankar, R.R.S., P. Spicer, L.Z. Strain management: E.A.V., J.H.B., I.A.C., K.C., S.W.C., H.H.C., T.Z.D., A.S.D., A.M.E., M.G.F., M.G.G., S.K.H., V.J., N.C.K., S.L.L., L.L., K.L., E.A.L., V.M.M., B.A.M., D.M.M., K.E.N., I.N., I.P., L.S., E.J.S., C.M.T., M.T., D.V.W., G.M.W., A.M.W., Y.W., K.M.W., B.P.Y., L.Z., Y.Z. 16S data analysis: K.M.A., E.J.A., G.L.A., C.A.A., M.B., B.W.B., J.P.B., G.A.B., S.R.C., S.C., J.C., T.Z.D., F.E.D., E.D., A.M.E., R.C.E., K.F., M.F., A.A.F., J.F., H.G., D.G., B.J.H., T.A.H., S.M.H., C.H., J.I., J.K.J., S.T.K., S.K.H., R.K., H.H.K., O.K., P.S.L., R.E.L., K.L., C.A.L., D.M., B.A.M., K.A.M., M.M., M.P., J.F.P., M.P., K.S.P., X.Q., J. Raes, K.P.R., M.C.R., B.R., J.F.S., P.D.S., T.M.S., N.S., J.A.S., W.D.S., T.J.S., C.S.S., E.J.S., R.M.T., J.V., T.A.V., Z.W., D.V.W., G.M.W., J.R.W., K.M.W., Y.Y., S.Y., Y.Z. Shotgun data processing and alignments: C.J.B., J.C.C., E.D., D.G., A.G., M.E.H., H.J., D.K., K.C.K., C.L.K., Y.L., J.C.M., B.A.M., M.M., D.M.M., J.O., J.F.P., X.Q., J.G.R., R.K.S., N.U.S., I.S., E.J.S., G.G.S., S.M.S., J.W., Z.W., G.M.W., O.W., K.C.W., T.W., S.K.Y., L.Z. Assembly: H.M.A., C.J.B., P.S.C., L.C., Y.D., S.P.D., M.G.F., M.E.H., H.J., S.K., B.L., Y.L., C.L., J.C.M., J.M.M., J.R.M., P.J.M., M.M., J.F.P., M.P., M.E.P., X.Q., M.R., R.K.S., M.S., D.D.S., G.G.S., S.M.S., C.M.T., T.J.T., W.W., G.M.W., K.C.W., L.Y., Y.Y., S.K.Y., L.Z. Annotation: O.O.A., V.B., C.J.B., I.A.C., A.T.C., K.C., H.H.C., A.S.D., M.G.G., J.M.G., J.G., A.G., S.G., B.J.H., K.H., S.K.H., C.H., H.J., N.C.K., R.M., V.M.M., K.M., T.M., M.M., J.O., K.P., M.P., X.Q., N.S., E.J.S., G.G.S., S.M.S., M.T., G.M.W., K.C.W., J.R.W., C.Y., S.K.Y., Q.Z., L.Z., W.G.S. Metabolic reconstruction: S.A., B.L.C., J.G., C.H., J.I., B.A.M., M.M., B.R., A.M.S., N.S., M.T., G.M.W., S.Y., Q.Z., J.D.Z.
Corresponding author
Ethics declarations
Competing interests
The author declare no competing financial interests.
Additional information
All data used in this study is available fromtheHuman Microbiome Project Data Analysis and Coordination Center at http://hmpdacc.org and from the NCBI.
Supplementary information
Supplementary Information
This file contains Supplementary Methods, a Supplementary Discussion, Supplementary Figures 1-5, Supplementary Table 1 and Supplementary References - see Contents for more details. This file was replaced on 26 June 2012 to correct the caption for Supplementary Figure 4. (PDF 2750 kb)
Supplementary Tables
This zipped file contains Supplementary Tables 2 and 3. (ZIP 96 kb)
Rights and permissions
This article is distributed under the terms of the Creative Commons Attribution-Non-Commercial-Share Alike licence (http://creativecommons.org/licenses/by-nc-sa/3.0/).
About this article
Cite this article
The Human Microbiome Project Consortium. Structure, function and diversity of the healthy human microbiome. Nature 486, 207–214 (2012). https://doi.org/10.1038/nature11234
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nature11234
This article is cited by
-
Ocular mucosal homeostasis of teleost fish provides insight into the coevolution between microbiome and mucosal immunity
Microbiome (2024)
-
Fine-scale geographic difference of the endangered Big-headed Turtle (Platysternon megacephalum) fecal microbiota, and comparison with the syntopic Beale’s Eyed Turtle (Sacalia bealei)
BMC Microbiology (2024)
-
Gut microbial ecology and exposome of a healthy Pakistani cohort
Gut Pathogens (2024)
-
Metagenomic analysis of Mesolithic chewed pitch reveals poor oral health among stone age individuals
Scientific Reports (2024)
-
Mock community taxonomic classification performance of publicly available shotgun metagenomics pipelines
Scientific Data (2024)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.