Abstract
Early treatment of acute HIV-1 infection followed by treatment interruptions has shown promise for enhancing immune control of infection1,2,3. A subsequent loss of control, however, allows the correlates of protective immunity to be assessed. Here we show that sudden breakthrough of plasma viraemia occurred after prolonged immune containment in an individual infected with HIV-1 at a time when 25 distinct CD8+ T-cell epitopes in the viral proteins Gag, RT, Integrase, Env, Nef, Vpr, Vif and Rev were being targeted. Sequencing of the virus in plasma and cells showed that superinfection with a second clade-B virus was coincident with the loss of immune control. This sudden increase in viraemia was associated with a decline in half of the CD8+ T-cell responses. The declining CD8+ T-cell responses were coupled with sequence changes relative to the initial virus that resulted in impaired recognition. Our data show that HIV-1 superinfection can occur in the setting of a strong and broadly directed virus-specific CD8+ T-cell response. The lack of cross-protective immunity for closely related HIV-1 strains, despite persistent recognition of multiple CD8 epitopes, has important implications for public health and vaccine development.
Similar content being viewed by others
Main
Increasing evidence suggests that virus-specific CD8+ T-cell responses are important in the control of HIV-1 or SIV replication4,5,6,7,8, and inducing and maintaining these responses are considered to be central for the development of effective HIV-1 vaccines. In the simian-HIV (SHIV) model, induction of strong SHIV-specific CD8+ T-cell responses does not prevent infection after challenge but is associated with persistent control of low levels of viral replication and attenuated disease9,10,11. Although similar vaccine regimens have failed to control more pathogenic and less easily neutralizable SIV strains12,13,14, these studies nevertheless provide optimism that an effective vaccine to prevent HIV-1 disease progression in humans could be developed. Indeed, the augmentation of HIV-1-specific immunity by the early treatment of persons with acute HIV-1 infection, followed by supervised treatment interruptions (STI), has been shown1,2,3. Most individuals treated by this method have been able to control, at least transiently, viraemia after the cessation of treatment at levels that did not require the re-initiation of treatment3. One such individual effectively controlled infection for over 290 d after STI but then experienced a marked increase in plasma viral load (Fig. 1a), offering us the opportunity to investigate the immunological and virological correlates of loss of immune control.
a, HIV-1 plasma viral loads, b, CD4+ T-cell counts; c, Gag-specific lymphoproliferative responses. Time zero represents the first presentation of AC-06 with symptomatic acute HIV-1 infection. At this time, HIV-1 viral loads were 8.8 × 106 RNA copies per ml of plasma (not shown). Shaded areas represent treatment with highly active antiretroviral therapy (HAART). Dotted line indicates 5,000 copies of HIV-1 RNA per ml of plasma.
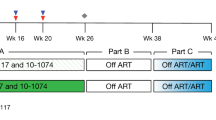
Subject AC-06 underwent STI 546 d after early treatment of acute HIV-1 infection by a previously reported protocol3. The virus rebounded, and within 60 d (day 606 of infection) exceeded 50,000 HIV-1 RNA copies per ml of plasma, necessitating the re-initiation of therapy (Fig. 1a). Therapy was again interrupted at day 715. Although there was a transient peak in viraemia at day 773, viraemia declined spontaneously and his CD4+ T-cell counts remained stable. He then did not meet the criteria for re-initiating therapy until day 1,020 (305 d after stopping therapy), showing prolonged control of viraemia while off therapy.
At this stage, however, he experienced a sudden rapid increase in viraemia along with a marked drop in CD4+ T-cell counts from 998 cells per µl (day 972) to 515 cells per µl before HAART was reinitiated (Fig. 1b). Subsequent STI 4 months later (day 1,149) was associated with an even more rapid loss of control, in which viraemia exceeded 50,000 RNA copies per ml of plasma within 20 d. After another 4 months of highly active antiretroviral therapy (HAART), treatment was again stopped (day 1,312) and HIV-1-viraemia once more rebounded but to lower peak concentrations. Although viraemia never exceeded 50,000 RNA copies per ml of plasma, secondary criteria to restart therapy were met at day 86 owing to viral loads above 5,000 RNA copies per ml for three consecutive weeks. At this stage, subject AC-06 chose to decline further drug therapy, with viral loads ranging from 3,700 to 18,200 RNA copies per ml for 280 d, before increasing to 38,000 RNA copies per ml on day 1,622. During this time, his CD4+ T-cell counts declined progressively.
We carried out comprehensive evaluation of the virus-specific immune responses to define the correlates of this loss of immune control. Gag-specific CD4+ T-cell proliferative responses were detected after early treatment3,15,16 and were present during the period of control during the second STI, but they declined with the sudden increase in viraemia (Fig. 1c). Although impairment of HIV-1-specific T-helper cell (TH) responses by continuing low-level viral replication17 before the rebound of viraemia cannot be excluded by these data, they suggest that a sudden loss of Gag-specific TH responses did not precede the observed loss of viral control in this individual. Similarly, only weak neutralizing antibody responses (titres ranging from <4 to 8 reciprocal plasma dilutions) against autologous virus were present during the second STI at the time of viral control.
Because animal model data suggest that CD8+ T-cell responses are essential for immune control in AIDS virus infections5,7,18, we measured longitudinally the maintenance of virus-specific CD8+ T-cell responses using an interferon-γ (IFN-γ) Elispot assay and 504 clade-B overlapping peptides spanning all expressed HIV-1 proteins. HIV-1-specific CD8+ T-cell responses were enhanced and broadened with re-exposure to antigen during the first and second STIs (see also ref. 19), ultimately targeting 25 distinct cytotoxic T lymphocyte (CTL) epitopes with a total of 27,470 spot-forming cells (SFCs) per 106 peripheral blood mononuclear cells (PBMCs) at the end of the second STI (Fig. 2a, b). In addition to IFN-γ secretion after antigenic stimulation, these epitope-specific CD8+ T cells also demonstrated epitope-specific cytotoxic activity (data not shown). But this pattern of enhancement of epitope-specific responses present during the first two STIs changed markedly during the third STI. Although a subset of epitope-specific CD8+ T-cell responses was maintained or expanded further, for the first time some established responses declined (Fig. 2c), leaving a reduced magnitude of 18,250 SFCs per 106 PBMCs (P = 0.01, versus the second STI).
Responses to individual epitopes are shown before and at the end of each STI (a, 1st STI; b, 2nd STI; c, 3rd STI) and are presented as spot-forming cells (SFCs) per million peripheral blood mononuclear cells (PBMCs). The duration of STI is indicated in months. All epitope-specific responses increased until the third STI, during which more than half of the responses declined.
To investigate the relationship between sequence variation within targeted epitopes and loss of immune control18, we sequenced regions in HIV-1 gag using PBMC samples derived from the time of acute infection (day 18) and the third STI (day 1,170). Although sequence changes were identified in three of the seven epitopes located within HIV-1 gag, there was an even greater number of amino acid changes in the flanking regions that did not contain targeted CD8+ T-cell epitopes (Fig. 3a). Phylogenetic analysis of autologous gag sequences from these time points (day 18 acute infection, and day 1,170 3rd STI) indicated that a distinct and unrelated second strain of HIV-1 had emerged (Fig. 3b). Additional sequencing of virus derived from intermediate time points during the first STI (day 606) and the second STI (day 1,021) confirmed these results, which were verified by an independent investigator (data not shown). These data showed that the early samples (day 18 and day 606) represented one strain of HIV-1 (referred to as virus A), whereas later samples (day 1,021 and day 1,170) represented a distinct second strain of HIV-1 (referred to as virus B) that became detectable during the end of the second STI and persisted during the third and fourth STI.
a, Gag sequences from subject AC-06 show high amino acid diversity. Consensus sequences were derived from several clones (minimum 4, mean 8) spanning each of the individual PCR fragments of the HIV-1 gag open reading frame. The sequences shown reflect the predominant viral populations present at day 18 and day 1,170. Boxes indicate the seven HLA-A03- or B07-restricted Gag epitopes targeted by this subject. b, HIV gag sequences from subject AC-06 during acute (day 18) and chronic (day 1,170) infection cluster independently. Sequences from 17 HIV-1 infected persons from the Boston area were aligned27. The neighbour-joining phylogenetic tree indicates that two distinct viruses are present in subject AC-06 at these different times after infection (bootstrap values >60 are shown). Numbers in parentheses indicate the number of sequences included for each subject and where available the number of acute (ac) or chronic (ch) stage sequences included. Scale bar indicates the genetic distance along the branches. c, Virus B predominates in plasma of subject AC-06 on day 1,005. Specific PCR primers for virus A and virus B were generated based on unique nucleotide substitutions present in the two viruses in a region of gag. RT–PCR was carried out on plasma viral RNA isolated throughout infection. Consensus clade-B-specific primers successfully amplify products at all time points, verifying sample integrity. Only virus-A-specific primers amplify product from plasma samples taken during the first 972 d of infection; by contrast, only virus-B-specific primers amplify product from samples taken from day 1,005 onwards.
Overall, the sequences of virus A and virus B were significantly different, showing 12% heterogeneity in amino acid sequence (on the basis of >80% sequence coverage of whole HIV genomes). BLAST searches of the HIV database also confirmed the uniqueness of both viruses. By contrast, viruses A and B themselves were found to vary only minimally (<0.3% amino acid heterogeneity) over time between day 18 and day 606 (virus A) and between day 1,021 and day 1,170 (virus B). Similarly, the viral diversity observed to develop in other subjects undergoing STIs over a similar time frame was also significantly more limited (data not shown). Thus, the sequence variations observed between virus A and virus B were not the result of viral evolution in several targeted CD8+ T-cell epitopes, but rather the emergence of a new HIV-1 clade-B strain in the study subject at a time when the initial virus was well controlled. An additional maximum likelihood phylogenetic analysis showed that it is highly unlikely that virus A and virus B arose from the same lineage within the context of the Boston cohort (see Supplementary Fig. 1). In addition, there was no evidence for recombination between virus A and virus B in subject AC-06 (data not shown). Both strains were most closely related to HIV-1 clade-B sequences and possessed an R5 phenotype as determined by their differential infection in U87-CD4-CCR5, U87-CD4-CXCR4 and MT2 cells (ref. 20 and data not shown).
The above data suggest that either dual infection with viruses A and B occurred during the primary HIV-1 infection or there was subsequent superinfection with virus B. Review of medical records indicated that subject AC-06 experienced symptoms including fever, lymphadenopathy and night sweats in the month preceding the first detection of virus B. In addition, this subject reported an unprotected sexual risk exposure with an anonymous partner 4–8 weeks before the beginning of symptoms. The clinical data were thus consistent with exposure to another virus. To define further the time of infection with virus B, virus-specific nested polymerase chain reaction (PCR) primer sets corresponding to unique gag nucleotide sequences were used to track both viruses throughout infection (see Supplementary Table I). Nested PCR with reverse transcription (RT–PCR) of plasma virus showed that virus A was the only detectable virus at the time of acute infection (day 4), during the first STI (day 606), and throughout most of the second STI (until day 972). In marked contrast, after the sudden increase in viraemia (day 1,005, Fig. 1a), the only virus detected in plasma was virus B (Fig. 3c). We carried out a similar analysis on viral DNA derived from PBMCs. Primers specific for virus A successfully amplified products from PBMC samples taken throughout infection, albeit less consistently from later time points when virus B predominated in plasma (data not shown). By contrast, primers specific for virus B successfully amplified products only from PBMC samples taken after day 1,021 (data not shown). Thus, the clinical and PCR data are most consistent with superinfection rather than with dual infection at the time of primary infection.
We next compared the sequence integrity of the CD8+ T-cell epitopes that were targeted before emergence of virus B to assess the impact of viral variability on immune recognition. Autologous sequences of virus A and virus B were amplified successfully for all regions except portions of env and nef, for which high sequence diversity limited amplification with the available primers (Supplementary Fig. 2 and Table II). Sixteen of the twenty-five epitopes were sequenced, as well as three new epitopes targeted for the first time after emergence of virus B. Recognition of autologous epitopes was assessed using PBMCs from several time points before and after emergence of virus B (Table 1) using an IFN-γ Elispot assay.
For 9 of the 16 sequenced epitopes targeted at the time of loss of immune control, either the epitope sequence was conserved completely (7 epitopes) or the virus B variant differed but was equally well recognized by CD8+ T cells derived from early and late time points (two epitopes), as assessed through peptide titration Elispot assays (ref. 21 and Supplementary Fig. 3). CD8+ T-cell responses to eight of these nine epitopes persisted after emergence of virus B (Table 1). The exception was a declining HLA-A3-restricted response to p17 Gag (KIRLRPGGK); this sequence was identical in both viruses, but virus B had an arginine to threonine mutation at position C + 2 that may have impaired antigen processing22.
For 7 of the 16 epitopes evaluated by sequence analysis, there were sequence changes in the CD8+ T-cell epitopes that were associated with declining CD8+ T-cell responses (Table 1) and decreased recognition by the established immune response (Supplementary Fig. 3). Indeed, comparison of the variability observed within each of these 16 sequenced epitopes to clade-B sequences present in the Los Alamos database showed a similar trend, with those epitopes conserved between virus A and virus B showing a greater degree of conservation than those that varied. Sequence data were not obtained for nine epitopes, for which five responses declined and four persisted (data not shown). Notably, the immunodominant CD8+ T-cell epitope GPGHKARVL in p24 Gag was present in both viruses, indicating that maintained responses against this epitope were not sufficient to prevent emergence of virus B9,18.
Optimal CD4+ T-cell responses in this individual have not been defined and thus the impact that this viral diversity has on maintenance of HIV-specific CD4+ T-cell responses is unknown. After emergence of virus B, however, Gag-specific CD4+ T-cell proliferative responses did rebound to significant levels, suggesting persistent cross-recognition. Notably, a marked decline in Gag-specific CD4 proliferative responses and CD4+ T-cell counts was observed during the fourth STI in the setting of increased viral replication (Fig. 1). With respect to humoral responses, as stated previously, only weak neutralizing antibody responses specific to virus A were detectable before superinfection. But these virus-A-specific responses were lost after superinfection with virus B (titre < 4) and were not crossreactive against virus B (Supplementary Table III). After emergence of virus B, virus-B-specific neutralizing antibody responses developed for the first time, with titres reaching 40. But virus B subsequently escaped from these virus-B-specific neutralizing antibody responses (titre < 4). These data show that neutralizing antibodies to virus B were lacking at the time of superinfection but were produced later, potentially contributing to viral evolution and neutralization escape.
In addition to a loss of immune responses at the time of emergence of virus B, at least three new CD8+ T-cell responses within HIV-1 Gag and Env were detectable for the first time after superinfection, including two previously described CD8 epitopes and one newly described epitope in HIV-1 Gag. Fine mapping of the new response showed that it was directed against an HLA-B7-restricted epitope (YPLASLRSL). Comparison of virus A and B sequences in this region indicated that the insertion of a proline at position 3 of this epitope (YPPLASLRSL) in virus A resulted in a variant that apparently had prevented the initial presentation of this region to the immune system (Fig. 3a and Supplementary Fig. 3). A response to this region was detectable for the first time when virus B predominated (Table 1). Similarly, for two additional epitopes that were recognized for the first time with emergence of virus B, the autologous variants of virus B were recognized at lower peptide concentrations than were the virus A variants (Supplementary Fig. 3). Thus, new CD8+ T-cell responses were capable of being induced in the setting of chronic persistent viral infection.
Our studies in a single individual indicate that virus-specific CD8+ T-cell responses that control replication of one strain of HIV-1 may not be sufficiently potent to prevent superinfection with a second virus of the same clade. It must be emphasized, however, that superinfection in an individual already infected with HIV-1 may be different from infection in a person with healthy immune system. In line with studies showing superinfection with a different HIV-1 clade23,24, our results provide a potential explanation for the emergence of a growing number of recombinant viruses worldwide25. In the case described here, although there was only roughly 12% difference in overall sequence, at least half of the targeted CD8 epitopes were not shared between the two viruses, both of which were acquired in North America. Although the immunodominant CD8+ T-cell epitope was conserved in both viruses, control of virus B was not achieved until additional epitopes were targeted, which suggests that subdominant responses have a role in immune control. Our study does show the ability of the immune system to generate CD8+ T-cell responses against epitopes that have not been previously presented, which indicates that therapeutic immunization in chronic infection may be possible. Further detailed dissection of immune responses in persons who control viraemia and then lose this control should provide important insights regarding the breadth, magnitude and phenotype of HIV-1-specific immune responses that may be necessary to provide broad, cross-protective immunity.
Methods
Subjects
Individual AC-06 presented with symptomatic acute infection, defined by detectable amounts of plasma HIV-1 RNA (8.8 × 106 copies per ml) and negative antibodies (HIV-1/HIV-2 ELISA and HIV-1 western blot). The CD4+ T-cell count at presentation was 551 cells per mm3, and HAART (d4T, 3TC and Nelfinavir) was initiated 4 d later. After 546 d of therapy, he underwent three cycles of STI with the plan to restart therapy if viral load exceeded 5,000 copies of HIV-1 RNA per ml of plasma for three consecutive weeks or 50,000 RNA copies per ml at one time. The fourth STI was off protocol.
IFN-γ Elispot assay
We quantified HIV-1-specific CD8+ T-cell responses by Elispot assay as described21, using overlapping peptides (peptides with 15–18 residues, overlapping by 10 amino acids) spanning the whole expressed HIV-1 clade-B sequence. Peptides corresponding to optimal clade-B CTL epitopes26 and the autologous virus sequences were also tested. PBMCs were plated at 50,000–100,000 cells per well with peptides at a final concentration of 10-5 M in 96-well plates and processed as described21. One hundred thousand PBMCs were incubated with media alone (negative control) or phytohaemoagglutinin (positive control). The number of specific IFN-γ secreting T-cells was counted by direct visualization, calculated by subtracting the negative control value and expressed as spot-forming cells (SFC) per 106 input cells. Negative controls were always less than 30 SFC per 106 input cells. A response was considered positive if it was equal to or greater than 50 SFC per 106 and at least three times greater than mean background activity. The CD8+ T-cell dependence of all responses was confirmed by CD4+ T-cell/CD8+ T-cell depletion/enrichment studies21 using MACS magnetic beads (Miltenyi Biotech). Fine-mapping of epitopes and comparison of recognition of the autologous epitope variants of virus A and virus B were done as described21.
HIV-1-specific TH cell assays
We carried out lymphocyte proliferation assays using baculovirus-derived HIV-1 Gag protein as described3. Briefly, PBMCs were incubated with protein (5 µg ml-1) for 6 d and then pulsed with [3H]thymidine at 1.0 µCi per well for 6 h.
Sequencing of autologous virus
Viral DNA was isolated from PBMCs (5 × 106 cells) and viral RNA was extracted from plasma samples and reverse-transcribed as described8. A set of seven external primer pairs amplified the whole HIV-1 genome (see Supplementary Fig. 2, Supplementary Table II and ref. 8). Primers were designed on the basis of alignments of over 100 clade-B sequences from the HIV Sequence Database (http://hiv-web.lanl.gov). PCR cycling conditions were as follows: 94 °C for 2 min, 35–50 cycles of 30 s at 94 °C, 30 s at 56 °C, 2 min at 72 °C and a final extension of 68 °C for 20 min. RT–PCR cycling conditions were as follows: 50 °C for 60 min, 95 °C for 15 min and cycling conditions as noted above. We used 44 internal primer pairs in nested PCR reactions to yield clonable fragments. The extension times were shortened to 1 min in the nested PCR reactions. PCR fragments were then gel-purified and cloned by TOPO TA (Invitrogen). Plasmid DNA was isolated by ‘miniprep’ using QiaPrep Turbo Miniprep (Qiagen) and sequenced bidirectionally on an ABI 3100 PRISM automated sequencer (Applied Biosystems). Sequencher (Gene Codes Corp.) and MacVector 4.1 (Oxford Molecular) were used to edit and align sequences. We sequenced a minimum of four clones for each region of the genome at each time point. Neighbour-joining trees were constructed using the Phylip Phylogeny Inference Package Version 3.5c (ref. 27).
Design of specific primers for virus A and virus B
We designed primers specific for virus A and virus B by taking advantage of unique nucleotide substitutions present in each virus in a particular region of Gag (Supplementary Table I). The RT and RT–PCR conditions using these specific primers were the same as those used for the clade-B consensus primers.
Neutralization assays
We measured neutralizing antibodies in human plasma as described20. Titres are reported as the reciprocal plasma dilution that resulted in an 80% reduction in p24 synthesis. Viruses were isolated by PBMC co-culture as described20 and used as original co-culture supernatants in the neutralization assay. All plasma samples were heat-inactivated at 56 °C for 1 h before use.
Statistical analysis
Statistical analysis and graphical presentation was done using SigmaPlot 5.0 (SPSS Inc.). The reported significance (P values) of the results is based on two-tailed t-tests.
References
Lisziewicz, J. et al. Control of HIV despite the discontinuation of antiretroviral therapy. N. Engl. J. Med. 340, 1683–1684 (1999)
Ortiz, G. M. et al. HIV-1-specific immune responses in subjects who temporarily contain virus replication after discontinuation of highly active antiretroviral therapy. J. Clin. Invest. 104, R13–R18 (1999)
Rosenberg, E. S. et al. Immune control of HIV-1 after early treatment of acute infection. Nature 407, 523–526 (2000)
Borrow, P., Lewicki, H., Hahn, B. H., Shaw, G. M. & Oldstone, M. B. Virus-specific CD8+ cytotoxic T-lymphocyte activity associated with control of viremia in primary human immunodeficiency virus type 1 infection. J. Virol. 68, 6103–6110 (1994)
Jin, X. et al. Dramatic rise in plasma viremia after CD8+ T cell depletion in simian immunodeficiency virus-infected macaques. J. Exp. Med. 189, 991–998 (1999)
Koup, R. A. et al. Temporal association of cellular immune responses with the initial control of viremia in primary human immunodeficiency virus type 1 syndrome. J. Virol. 68, 4650–4655 (1994)
Schmitz, J. E. et al. Control of viremia in simian immunodeficiency virus infection by CD8+ lymphocytes. Science 283, 857–860 (1999)
Allen, T. M. et al. Tat-specific cytotoxic T lymphocytes select for SIV escape variants during resolution of primary viraemia. Nature 407, 386–390 (2000)
Barouch, D. H. et al. Control of viremia and prevention of clinical AIDS in rhesus monkeys by cytokine-augmented DNA vaccination. Science 290, 486–492 (2000)
Amara, R. R. et al. Control of a mucosal challenge and prevention of AIDS by a multiprotein DNA/MVA vaccine. Science 292, 69–74 (2001)
Shiver, J. W. et al. Replication-incompetent adenoviral vaccine vector elicits effective anti-immunodeficiency-virus immunity. Nature 415, 331–335 (2002)
Hanke, T. et al. Effective induction of simian immunodeficiency virus-specific cytotoxic T lymphocytes in macaques by using a multiepitope gene and DNA prime- modified vaccinia virus Ankara boost vaccination regimen. J. Virol. 73, 7524–7532 (1999)
Allen, T. M. et al. Tat-vaccinated macaques do not control simian immunodeficiency virus SIVmac239 replication. J. Virol. 76, 4108–4112 (2002)
Feinberg, M. B. & Moore, J. P. AIDS vaccine models: challenging challenge viruses. Nature Med. 8, 207–210 (2002)
Malhotra, U. et al. Effect of combination antiretroviral therapy on T-cell immunity in acute human immunodeficiency virus type 1 infection. J. Infect. Dis. 181, 121–131 (2000)
Oxenius, A. et al. Early highly active antiretroviral therapy for acute HIV-1 infection preserves immune function of CD8+ and CD4+ T lymphocytes. Proc. Natl Acad. Sci. USA 97, 3382–3387 (2000)
Douek, D. C. et al. HIV preferentially infects HIV-specific CD4+ T cells. Nature 417, 95–98 (2002)
Barouch, D. H. et al. Eventual AIDS vaccine failure in a rhesus monkey by viral escape from cytotoxic T lymphocytes. Nature 415, 335–339 (2002)
Yu, X. G. et al. Consistent patterns in the development and immunodominance of human immunodeficiency virus type 1 (HIV-1)-specific CD8+ T-cell responses following acute HIV-1 infection. J. Virol. 76, 8690–8701 (2002)
Montefiori, D. C., Hill, T. S., Vo, H. T., Walker, B. D. & Rosenberg, E. S. Neutralizing antibodies associated with viremia control in a subset of individuals after treatment of acute human immunodeficiency virus type 1 infection. J. Virol. 75, 10200–10207 (2001)
Altfeld, M. A. et al. Identification of dominant optimal HLA-B60- and HLA-B61-restricted cytotoxic T-lymphocyte (CTL) epitopes: rapid characterization of CTL responses by enzyme-linked immunospot assay. J. Virol. 74, 8541–8549 (2000)
Del Val, M., Schlicht, H. J., Ruppert, T., Reddehase, M. J. & Koszinowski, U. H. Efficient processing of an antigenic sequence for presentation by MHC class I molecules depends on its neighbouring residues in the protein. Cell 66, 1145–1153 (1991)
Ramos, A. et al. Intersubtype human immunodeficiency virus type 1 superinfection following seroconversion to primary infection in two injection drug users. J. Virol. 76, 7444–7452 (2002)
Jost, S. et al. A patient with HIV-1 superinfection. N. Engl. J. Med. 347, 731–736 (2002)
McCutchan, F. E. Understanding the genetic diversity of HIV-1. Aids 14, S31–S44 (2000)
Brander, C., Goulder, P. J. R., et al. HIV Molecular Database (ed. Korber, B. T. M.) I1–I20 (Los Alamos National Laboratory, Los Alamos, NM, 1999)
Felsenstein, J. PHYLIP—Phylogeny Inference Package Version 3.5c, (Dept. Genetics, Univ. Washington, Seattle, 1989)
Acknowledgements
We thank the Advanced Computing Laboratory at the Los Alamos National Lab for providing time on the Nirvana supercomputer for the maximum likelihood phylogenetic analysis, and Tanmoy Bhattacharya for his advice. This study was supported by the Doris Duke Charitable Foundation (M.A., E.S.R.,B.D.W.), the NIH (M.A., E.S.R., B.D.W.), the Foundation for AIDS & Immune Research (M.A.), and the Partners/Fenway/Shattuck Center for AIDS Research (T.A., X.G.Y.). B.D.W. is the recipient of a Doris Duke Distinguished Clinical Scientist Award; B.T.K. and P.J.R.G. are recipients of the Elizabeth Glaser Scientist Award.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare that they have no competing financial interests.
Supplementary information
Rights and permissions
About this article
Cite this article
Altfeld, M., Allen, T., Yu, X. et al. HIV-1 superinfection despite broad CD8+ T-cell responses containing replication of the primary virus. Nature 420, 434–439 (2002). https://doi.org/10.1038/nature01200
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1038/nature01200
This article is cited by
-
Distinct mechanisms of long-term virologic control in two HIV-infected individuals after treatment interruption of anti-retroviral therapy
Nature Medicine (2021)
-
Killed whole-HIV vaccine; employing a well established strategy for antiviral vaccines
AIDS Research and Therapy (2017)
-
HIV integration sites in latently infected cell lines: evidence of ongoing replication
Retrovirology (2017)
-
Immunological and virological characteristics of human immunodeficiency virus type 1 superinfection: implications in vaccine design
Frontiers of Medicine (2017)
-
Promise and problems associated with the use of recombinant AAV for the delivery of anti-HIV antibodies
Molecular Therapy - Methods & Clinical Development (2016)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.