Abstract
Maternal immune activation has been highlighted as a factor that might increase the risk and severity of autism spectrum disorder (ASD) in children. Preclinical animal evidence shows that immune activation in mothers during pregnancy causes ASD-like behavioural traits in offspring. To this point, there has been no investigation of whether immune system activation in human mothers during pregnancy is associated with more severe symptoms in children with ASD. In this study, data from an existing ASD cohort (N=220) were analysed to investigate whether immune conditions in the mother were associated with greater severity of autism-related symptoms. Results showed that children whose mothers reported a history of immune activation (allergies and asthma) had significantly higher scores on the Social Responsiveness Scale (SRS; P=0.016), suggesting more severe social impairment symptoms in these children. This increasing severity of social impairment symptoms was further shown on the SRS cognition (P=0.007) and mannerisms (P=0.002) subscales. While immune history was associated with an increase in the severity of social impairment symptoms, history of autoimmune conditions in the mother did not have any effect in this cohort. To the best of our knowledge, this study is the first to show an association between immune activation history in the mother and increased ASD symptom severity in children with ASD. These findings support the idea of an immune system-mediated subtype in ASD, where the immune history of the mother may be an important factor.
Similar content being viewed by others
Introduction
Autism spectrum disorder (ASD) represents a group of neurodevelopmental disorders characterised by impairment in reciprocal social interaction and communication, along with restricted and repetitive behaviours and interests. In 2010, a worldwide prevalence of ASD was estimated at 1 in 132 individuals,1 but more recently the US Centers for Disease Control and Prevention indicated a prevalence of 1 in 68.2 Autism is associated with substantial physical and mental health problems across the lifespan3,4 which places a large financial, social and personal burden on individuals, families and society.5 There are no single known causes of ASD; it is believed to be caused by a complicated interplay between genetic, epigenetic and environmental factors.6 Similarly, the clinical presentation, developmental course and treatment outcomes of ASD are heterogeneous,7,8 posing challenges for diagnosis and treatment.
In recent years, research has developed to suggest the immune system plays an important role in the pathophysiology of ASD.9,10,11,12 Maternal immune activation (MIA), resulting from either genetic or environmental causes, has been highlighted as a factor that can increase the risk of ASD.13,14,15,16 MIA is broadly defined as an active immune response during pregnancy. MIA can be considered from two perspectives: externally triggered or autoimmune. MIA in response to infections, particularly when associated with fever or hospitalisation, has been shown to increase the risk of delivering a child with ASD.17,18,19 Similar findings have also been reported for asthma and severe allergies during pregnancy, which are also externally triggered.20 Maternal history of autoimmune disorders has also been associated with increased incidence in the diagnosis of ASD,15,21,22 providing further support for the notion that maternal immune response, especially during gestation, is an important factor in the aetiology of ASD.
External immune insults and autoimmune conditions can both produce an immune response in the mother, mediated by cytokines, chemokines, inflammatory cells and antibodies, resulting in an altered immune system environment for the fetus. Preclinical animal models have already shown that immune activation during pregnancy causes ASD-like phenotypes in offspring, which supports the MIA hypothesis,14,23,24 although the molecular mechanisms through which MIA increases the risk of ASD are still largely unknown.
It has been suggested that prenatal exposure to cytokines and chemokines may alter the expression of genes associated with the development and regulation of the central nervous system and immune system.25,26 Additionally, MIA may compromise the ability of the placenta to regulate the maternal–fetal immune interface, causing an increase in fetal cytokine levels and disrupting the development of the fetal central nervous system and immune system.25,27,28 Many studies have shown that a proportion of individuals with ASD have elevated levels of pro-inflammatory cytokines and chemokines, which aid in the recruitment of inflammatory cells, while anti-inflammatory cytokine levels are reduced.29,30 This state of chronic inflammation has also been correlated with an increase in ASD symptom severity,29,31,32 indicating a possible link between the immune system and the observed ASD phenotype.
Furthermore, some mothers of children with ASD show antibody reactivity to fetal proteins, raising the possibility that these antibodies interfere with development of the fetus and contribute to ASD symptoms.33,34,35 Although a family history of autoimmune disease has been associated with an increased risk of ASD,15,22 it is not yet clear whether autoimmune disease in the mother is related to the generation of these detrimental antibodies in the mother or to ASD symptom severity in the child.
Considered together, the developing research suggests the potential of an immune-mediated subtype in ASD that may be driven by alterations in cytokine, chemokine or antibody levels in the mother and/or child. In many cases, these immune system aberrations are a result of MIA, which may be externally triggered or due to an autoimmune disease. This raises the possibility that a history of MIA in mothers of children with ASD may be related to increased severity of ASD symptoms. To our knowledge, no study has examined whether MIA is associated with poorer outcomes for children with ASD. In this study, we use an existing ASD cohort with collected data from parents about immune history. We aim to test whether having an immune or autoimmune-driven MIA is associated with increased severity of ASD symptoms for the child.
Materials and methods
The cohort used for this study were participants in the Western Australian Autism Biological Registry (WAABR), located at the Telethon Kids Institute in Perth, Western Australia.36 Ethics approval for the WAABR was granted by the Human Ethics Committee at Princess Margaret Hospital for Children in Perth, Western Australia. Participants were recruited between the period of January 2011 and September 2014 through newspaper advertisements and flyers, distributed among local clinicians and service providers. The study included participants with a DSM-IV clinical diagnosis of Autistic Disorder (autism), Asperger’s Syndrome or Pervasive Developmental Disorder-Not Otherwise Specified (PDDNOS). Informed consent to be a part of the WAABR was provided by the primary caregiver of the participant.
ASD phenotype
The Autism Diagnostic Observation Schedule-Generic (ADOS-G) was administered to each participant by research accredited professionals. The ADOS-G is a standardised, semistructured assessment which uses simple activities and questions that are designed to prompt and observe the communicative, social and stereotyped behaviours which are relevant to the diagnosis of ASD.37 For each participant, the ADOS-G raw scores and total scores were converted to the updated ADOS-2 calibrated severity score, as this score is less influenced by child characteristics.38,39,40 The ADOS calibrated severity scores are based on a scale on 1–10, where 1 represents minimal evidence of ASD-related symptoms and 10 denotes a high severity of symptoms. A primary caregiver also completed the Social Responsiveness Scale (SRS), which is a 65-item rating scale that measures social interaction, language, and repetitive/restricted behaviours and interests in the child.41 The SRS provides a total score, as well as separate scores for five subscales: awareness, cognition, communication, motivation and mannerisms. Higher SRS scores indicate heightened severity of ASD-related social impairment.
Demographics and maternal medical history
A primary caregiver completed a family history questionnaire, which included participant demographics such as age, gender, head circumference, height and weight. It also included a section addressing the medical history of the biological mother, where details regarding any diagnosed illnesses or chronic conditions were reported, along with age of any diagnosis.
Results
Data were analysed from 220 children in the registry who completed the ADOS assessment and whose primary caregiver completed the family history questionnaire and SRS assessment. The SRS total scores (T scores; M=88.06, Mdn=88, s.d.=15.25) and ADOS calibrated severity scores (M=5.96, Mdn=6, s.d.=2.45) were used as measures of ASD symptom severity. Demographics of the child with ASD and the biological mother are provided in Table 1. The children were separated into categories based on maternal medical history. Children whose mothers reported a history of chronic immune activation were placed in the immune category. Allergies and asthma were the only reported chronic immune conditions in this cohort. Children whose mothers reported a diagnosis of any autoimmune conditions were grouped together in the autoimmune category. In this cohort, the reported autoimmune conditions included type 1 diabetes (N=7), optic neuritis (N=1), rheumatoid arthritis (N=4), coeliac disease (N=1), eczema/psoriasis (N=2), sarcoidosis (N=1), systemic lupus erythematosus (N=1) and thyroid problems (N=16), with three mothers reporting more than one autoimmune condition. As there were eight children whose mother reported both immune history (asthma or allergies) and autoimmune history (previous list), these two groups were analysed separately against the non-immune history category.
After checking the data for normality, T-tests were run to compare each medical history category against the demographic variables. Results showed that there we no significant differences in the demographics between mothers with an immune activation history (allergies or asthma) and those without. However, mothers with a history of autoimmune activation were older in age than those without (t(216)=3.53, P=0.001).
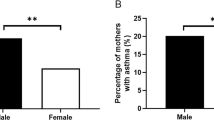
We then conducted multivariate ANOVAs for each category to examine the relationship between MIA history and outcome measures of the SRS and ADOS. There was no significant influence of autoimmune history on SRS total scores or ADOS calibrated severity scores (F(2, 202)=2.36, P=0.09), even when mother’s age was included as a covariate. No further analysis was conducted regarding the influence of autoimmune history. For the immune history category (allergies or asthma), a one-way multivariate ANOVA examining the effect of immune status on both SRS total scores and ADOS calibrated severity scores revealed a significant effect (F(2, 202)=3.27, P=0.041). Follow-up ANOVAs revealed a significant influence of immune status on SRS total scores (F(1, 207)=5.88, P=0.016), meaning that children of mothers with a history of immune activation showed higher SRS total scores (Figure 1). Subscale analysis of the SRS showed that a history of immune activation was associated with higher SRS scores, particularly on the cognition (P=0.007) and mannerisms (P=0.002) treatment subscales (Figure 1). There was, however, no influence of immune status on ADOS calibrated severity scores (F(1,212)=0.10, P>0.05). All of these analyses remained similarly significant when the three mothers who were not diagnosed with an immune condition until after pregnancy were removed.
Mean (+s.e.m.) Social Responsiveness Scale (SRS) T scores of the immune and non-immune categories. Children whose mothers were in the immune category show higher SRS total scores (P=0.016), specifically on cognition (P=0.007) and mannerisms (P=0.002) subscales, but not on awareness, communication or motivation.
Discussion
We believe this is the first study that has explored the relationship between maternal immune history and severity of autism symptoms in a well-characterised cohort of children with ASD. Specifically, we examined whether a history of immune activation in mothers of children with autism, driven by either an immune condition (allergies or asthma) or autoimmune condition, would be associated with an increase in severity of ASD symptoms in the child. Results showed that a positive immune history (allergies or asthma) was associated with increased severity of social symptoms in child. A history of autoimmune conditions in the mother did not influence autism symptom severity in this cohort, although we cannot rule out that this was due to a large number of mothers being diagnosed with autoimmune problems post-pregnancy. Our results provide further support of a relationship between a history of immune activation in the mother and caregiver rated severity of ASD-related symptoms in the child.
Preclinical animal models have shown that immune activation during pregnancy results in offspring displaying autism like symptoms, such as abnormal communication, decreased sociability and repetitive/restricted behaviours.14 These models have demonstrated that the type, severity and timing of the immune insult can influence the observed ASD-like phenotype24 and that MIA can lead to permanent immune dysregulation in offspring.23 In humans, it has been shown that MIA increases the risk of children being born with ASD.13,14,15,17,18,19,22 For instance, asthma and allergies during pregnancy have been associated with a twofold elevated risk of ASD.20 Our results build upon the existing literature by showing an association between MIA (caused by asthma and allergies) and ASD symptom severity in children with ASD. Children of mothers who reported a history of immune activation had significantly higher SRS total scores, meaning that they show more severe caregiver reported social deficits. Specifically, they had higher scores on the cognition and mannerisms subscales, suggesting that they have more difficulty understanding social situations and display more restricted behaviours or unusual interests. Interestingly, this association of maternal immune history was not seen on the ADOS calibrated severity scores. The ADOS is, however, primarily a diagnostic measure that has poor capacity for differentiating both severity and change.42,43
Our study extends the MIA hypothesis and indicates that MIA may contribute to increasing the severity of autism symptoms in the child. This may be caused by prenatal exposure to cytokines, chemokines or antibodies which interfere with the development and regulation of the fetal central nervous system.25,27,44 Furthermore, immune activation in the mother may have been associated with immune system dysregulation in the child,23 leading heightened inflammation to increase ASD symptom severity.29,31,32 Immune profiles of the mothers and children in the immune category now need to be examined in order to determine whether maternal immune history and increased symptom severity are correlated with elevated levels of pro-inflammatory cytokines in the mother and/or child. We also note that the scope of the MIA hypothesis may include all types of maternal immune responses, including infections and fevers,17,18,19,20 asthma and allergies,20 as well as autoimmune diseases.15,21,22 The interplay between these various immune responses, in terms of type, timing and molecular pathways, may be a crucial part of characterising the immune system-mediated subtype in ASD.
This study was conducted retrospectively in an existing cohort and relied on accurate caregiver report in terms of the SRS and medical history of the mother. The ADOS provided a measure of observed ASD symptom severity, but the influence of maternal immune history was not significant on this outcome measure. While the sample size of the immune and non-immune categories was large, the autoimmune category was much smaller. Within the autoimmune category, only 16 mothers were diagnosed prior to pregnancy and it remains unclear how many of these who reported thyroid problems were specifically related to autoimmunity. It is possible that the 14 mothers who were diagnosed post-pregnancy and possible thyroid cases that were not autoimmune conditions influenced the nonsignificant result in this category. This study needs to be repeated in a larger cohort with equal numbers in each category and more objective immune activation details and records regarding specific medical conditions. Future prospective studies collectively examining externally triggered immune activation and autoimmune conditions are now required to shed further light on the nature of the relationship between immune history and symptom severity.
In conclusion, this study is the first to show a relationship between immune history in the mother and increased severity of social symptoms in children with ASD. While we were not able to determine a causative relationship, this study suggests that children with ASD who are born to mothers with an immune activation history (in this case, asthma or allergies) present with more severe social deficits than those born to mothers without an immune history. Findings support the role of an immune system-mediated subtype in ASD, which may be driven by MIA and changes in levels immune markers. Identification of such a subtype in ASD will enable more streamlined diagnosis and management in clinical environments. It supports investigation of biomarkers in this subgroup and presents novel targets for immune-modulating pharmacotherapies. Further studies, using a prospective, longitudinal approach and larger cohorts are needed to elucidate the interplay between MIA, immune profiles and ASD symptom severity to further understand the role of mother’s immune history status in ASD.
References
Baxter AJ, Brugha TS, Erskine HE, Scheurer RW, Vos T, Scott JG. The epidemiology and global burden of autism spectrum disorders. Psychol Med 2015; 45: 601–613.
Christensen DL, Baio J, Braun KVN, Bilder D, Charles J, Constantino JN et al. Prevalence and characteristics of autism spectrum disorder among children aged 8 years. Morbidity and Mortality Weekly Report 2016; 65: 1–23.
Simonoff E, Psych FRC, Pickles A, Charman T, Chandler S, Loucas T et al. Psychiatric disorders in children with autism spectrum disorders: prevalence, comorbidity, and associated factors in a population-derived sample. J Am Acad Child Adolesc Psychiatry 2008; 47: 921–929.
Zafeiriou DI, Ververi A, Vargiami E. Childhood autism and associated comorbidities. Brain Dev 2007; 29: 257–272.
Kogan MD, Strickland BB, Blumberg SJ, Singh GK, Perrin JM, Van Dyck PC. A national profile of the health care experiences and family impact of autism spectrum disorder among children in the United States, 2005–2006. Pediatrics 2008; 122: e1149–e1158.
Persico AM, Bourgeron T. Searching for ways out of the autism maze: genetic, epigenetic and environmental clues. Trends Neurosci 2006; 29: 349–358.
Howlin P, Goode S, Hutton J, Rutter M. Adult outcome for children with autism. J Child Psychol Psychiatry 2004; 45: 212–229.
Szatmari P, Georgiades S, Duku E, Bennett TA, Bryson S, Fombonne E et al. Developmental trajectories of symptom severity and adaptive functioning in an inception cohort of preschool children with autism spectrum disorder. JAMA Psychiatry 2015; 72: 276–283.
Meltzer A, Van de Water J. The role of the immune system in autism spectrum disorder. Neuropsychopharmacology 2017; 42: 284–298.
Ashwood P, Wills S, Van De Water J. The immune response in autism: a new frontier for autism research. J Leukoc Biol 2006; 80: 1–15.
McDougle CJ, Landino SM, Vahabzadeh A, O’Rourke J, Zurcher NR, Finger BC et al. Toward an immune-mediated subtype of autism spectrum disorder. Brain Res 2015; 1617: 72–92.
Noriega DB, Savelkoul HFJ. Immune dysregulation in autism spectrum disorder. Eur J Pediatr 2014; 173: 33–43.
Estes ML, McAllister AK. Maternal immune activation: implications for neuropsychiatric disorders. Science 2016; 353: 772–777.
Malkova NV, Yu CZ, Hsiao EY, Moore MJ, Patterson PH. Maternal immune activation yields offspring displaying mouse versions of the three core symptoms of autism. Brain Behav Immun 2012; 26: 607–616.
Chen S, Zhong X, Jiang L, Zheng X, Xiong Y, Ma S et al. Maternal autoimmune diseases and the risk of autism spectrum disorders in offspring: a systematic review and meta-analysis. Behav Brain Res 2016; 296: 61–69.
Jiang H-Y, Xu L-L, Shao L, Xia R-M, Yu Z-H, Ling Z-X et al. Maternal infection during pregnancy and risk of autism spectrum disorders: a systematic review and meta-analysis. Brain Behav Immun 2016; 58: 165–172.
Zerbo O, Qian Y, Yoshida C, Grether JK, Van de Water J, Croen LA. Maternal infection during pregnancy and autism spectrum disorders. J Autism Dev Disord 2015; 45: 4015–4025.
Zerbo O, Iosif A-M, Walker C, Ozonoff S, Hansen RL. Is maternal influenza or fever during pregnancy associated with autism or developmental delays? Results from the CHARGE (CHildhood Autism Risks from Genetics and Environment) study. J Autism Dev Disord 2013; 43: 25–33.
Hornig M, Bresnahan M, Che X, Schultz A, Ukaigwe J, Eddy M et al. Prenatal fever and autism risk. Mol Psychiatry 2017;: 1–8.
Croen LA, Grether JK, Yoshida CK, Odouli R, Van de Water J. Maternal autoimmune diseases, asthma and allergies, and childhood autism spectrum disorders. Arch Pediatr Adolesc Med 2005; 159: 151–157.
Gesundheit B, Rosenzweig JP, Naor D, Lerer B, Zachor DA, Procházka V et al. Immunological and autoimmune considerations of autism spectrum disorders. J Autoimmun 2013; 44: 1–7.
Atladottir HO, Pedersen MG, Scient C, Thorsen P, Mortensen PB, Deleuran B et al. Association of family history of autoimmune diseases and autism spectrum disorders. Pediatrics 2009; 124: 687–694.
Hsiao EY, McBride SW, Chow J, Mazmanian SK, Patterson PH. Modeling an autism risk factor in mice leads to permanent immune dysregulation. Proc Natl Acad Sci USA 2012; 109: 12776–12781.
Careaga M, Murai T, Bauman MD. Maternal immune activation and autism spectrum disorder: from rodents to nonhuman and human primates. Biol Psychiatry 2016; 81: 391–401.
Parker-Athill EC, Tan J. Maternal immune activation and autism spectrum disorder: interleukin-6 signaling as a key mechanistic pathway. Neurosignals 2011; 18: 113–128.
Deverman BE, Patterson PH. Cytokines and CNS development. Neuron 2009; 64: 61–78.
Garay PA, Hsiao EY, Patterson PH, McAllister AK. Maternal immune activation causes age- and region-specific changes in brain cytokines in offspring throughout development. Brain Behav Immun 2013; 31: 54–68.
Masi A, Glozier N, Dale R, Guastella A. The immune system, cytokines, and biomarkers in autism spectrum disorder. Neurosci Bull 2017; 33: 194–204.
Krakowiak P, Goines PE, Tancredi DJ, Ashwood P, Hansen RL, Hertz-Picciotto I et al. Neonatal cytokine profiles associated with autism spectrum disorder. Biol Psychiatry 2015; 81: 442–451.
Masi A, Quintana DS, Glozier N, Lloyd AR, Hickie IB, Guastella AJ. Cytokine aberrations in autism spectrum disorder: a systematic review and meta-analysis. Mol Psychiatry 2015; 20: 440–446.
Ashwood P, Krakowiak P, Hertz-Picciotto I, Hansen R, Pessah I, Van de Water J. Elevated plasma cytokines in autism spectrum disorders provide evidence of immune dysfunction and are associated with impaired behavioral outcome. Brain Behav Immun 2011; 25: 40–45.
Ashwood P, Krakowiak P, Hertz-Picciotto I, Hansen R, Pessah IN, Van de Water J. Associations of impaired behaviors with elevated plasma chemokines in autism spectrum disorders. J Neuroimmunol 2011; 232: 196–199.
Braunschweig D, Krakowiak P, Duncanson P, Boyce R, Hansen RL, Ashwood P et al. Autism-specific maternal autoantibodies recognize critical proteins in developing brain. Transl Psychiatry 2013; 3: e277.
Braunschweig D, Ashwood P, Krakowiak P, Hertz-Picciotto I, Hansen R, Croen L et al. Autism: maternally derived antibodies specific for fetal brain proteins. Neurotoxicology 2008; 29: 226–231.
Croen LA, Braunschweig D, Haapanen L, Yoshida CK, Fireman B, Grether JK et al. Maternal mid-pregnancy autoantibodies to fetal brain protein: the early markers for autism study. Biol Psychiatry 2008; 64: 583–588.
Taylor LJ, Maybery MT, Wray J, Ravine D, Hunt A, Whitehouse AJO. Are there differences in the behavioural phenotypes of autism spectrum disorder probands from simplex and multiplex families? Res Autism Spectr Disord 2015; 11: 56–62.
Lord C, Risi S, Lambrecht L, Edwin H, Cook J, Leventhal BL et al. The Autism Diagnostic Observation Schedule—Generic: a standard measure of social and communication deficits associated with the spectrum of autism. J Autism Dev Disord 2000; 30: 205–223.
Gotham K, Pickles A, Lord C. Standardizing ADOS scores for a measure of severity in autism spectrum disorders. J Autism Dev Disord 2009; 36: 693–705.
Hus V, Lord C. The Autism Diagnostic Observation Schedule, Module 4: revised algorithm and standardized severity scores. J Autism Dev Disord 2014; 44: 1996–2012.
Shumway S, Farmer C, Thurm A, Joseph L, Black D. The ADOS calibrated severity score: relationship to phenotypic variables and stability over time. Autism Res 2012; 5: 267–276.
Constantino JN, Davis SA, Todd RD, Schindler MK, Gross MM, Brophy SL et al. Validation of a brief quantitative measure of autistic traits: comparison of the Social Responsiveness Scale with the Autism Diagnostic Interview-Revised. J Autism Dev Disord 2003; 33: 427–433.
Duvekot J, van der Ende J, Verhulst FC, Greaves-Lord K. The screening accuracy of the parent and teacher-reported Social Responsiveness Scale (SRS): comparison with the 3Di and ADOS. J Autism Dev Disord 2015; 45: 1658–1672.
Aldridge FJ, Gibbs VM, Schmidhofer K, Williams M. Investigating the clinical usefulness of the Social Responsiveness Scale (SRS) in a tertiary level, autism spectrum disorder specific assessment clinic. J Autism Dev Disord 2012; 42: 294–300.
Smith SEP, Li J, Garbett K, Mirnics K, Patterson PH. Maternal immune activation alters fetal brain development through interleukin-6. J Neurosci 2007; 27: 10695–10702.
Acknowledgments
We acknowledge a National Health and Medical Research Council Career Development Fellowship (APP1061922) and a Project Grant (APP1043664) to AJG, a NHMRC Australian Fellowship (APP511921) to IBH and a Senior Research Fellowship (APP1077966) to AJOW.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare no conflict of interest.
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License. The images or other third party material in this article are included in the article's Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/4.0/
About this article
Cite this article
Patel, S., Masi, A., Dale, R.C. et al. Social impairments in autism spectrum disorder are related to maternal immune history profile. Mol Psychiatry 23, 1794–1797 (2018). https://doi.org/10.1038/mp.2017.201
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/mp.2017.201
This article is cited by
-
Abnormal neutrophil-to-lymphocyte ratio in children with autism spectrum disorder and history of maternal immune activation
Scientific Reports (2023)
-
Maternal immune activation during pregnancy is associated with more difficulties in socio-adaptive behaviors in autism spectrum disorder
Scientific Reports (2023)
-
Signalling pathways in autism spectrum disorder: mechanisms and therapeutic implications
Signal Transduction and Targeted Therapy (2022)
-
Eczema and related atopic diseases are associated with increased symptom severity in children with autism spectrum disorder
Translational Psychiatry (2022)
-
Maternal immune conditions are increased in males with autism spectrum disorders and are associated with behavioural and emotional but not cognitive co-morbidity
Translational Psychiatry (2020)